Abstract
Objectives
N-Acetyl cysteine (NAC), a well-known antioxidant molecule, has been used to modulate oxidative stress and inflammation. However, no studies have examined the effect of NAC in regenerative endodontic procedures (REPs). Therefore, the aim of this study was to investigate the effects of NAC on cell survival, mitochondrial reactive oxygen species (mtROS) production, and inflammatory and mitochondria-related gene expression on lipopolysaccharide (LPS)-treated apical papilla cells (APCs).
Materials and methods
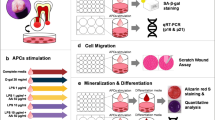
To assess the NAC concentration, 5 and 10 mM NAC were administered to LPS-treated APCs. Cell proliferation was measured at 24, 48, and 72 h by using AlamarBlue® assay. The 5-mM concentration was further analyzed using different treatment durations: 10 min, 24 h, and the entire study period. The mtROS production was quantified using MitoSOX™ Red and MitoTracker™ Green. RT-PCR was used to detect the expression of IL-6 and TNF-α inflammatory genes and mitochondrial morphology–related genes (Mfn-2/Drp-1 and Bcl-2/Bax) at 6 and 24 h. The statistical significance level was set at 0.05.
Results
Five-millimolar NAC promoted the highest LPS-treated APC proliferation. The use of 24-h NAC stimulated cell proliferation, whereas the entire-period NAC application (> 48 h) significantly reduced the cell number. The mtROS levels were slightly altered after NAC induction. Ten-minute NAC treatment downregulated the IL-6 and TNF-α expression, whereas the expression of Bcl-2/Bax and Mfn-2/Drp-1 ratios was upregulated at 6 h.
Conclusions
Under the LPS-induced inflammatory condition, NAC stimulated APC survival and decreased inflammation. Ten-minute NAC treatment was sufficient to reduce the level of inflammation and maintain the mitochondrial dynamics.
Clinical relevance
Ten-minute NAC application is sufficient to reduce the level of inflammation and maintain the mitochondrial dynamics. Therefore, NAC may be considered as a potential adjunctive irrigation solution in REPs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Regenerative endodontic procedures (REPs) have been defined as biologically based procedures designed to regenerate a fully functional pulp–dentin complex by using the tissue engineering concept [1,2,3]. This technique has recently gained interest as a new alternative treatment technique for treating necrotic immature permanent teeth with apical periodontitis because it influences root development [4, 5]. The treatment procedures of REPs involve two main clinical steps, namely, disinfection and regeneration steps. In the regeneration step, bleeding is created inside the root canal by intentionally stimulating the apical tissues [6, 7]. The evoked-bleeding step from the apical papilla tissues leads to a significant influx of stem cells from the apical papilla into the root canal systems [6,7,8,9]. These cells are incorporated with the natural scaffold and play vital roles in tissue regeneration. Given that one of the main causes of pulpal necrosis is bacterial infection, disease progression leads to the activation of pathological cascades [10]. Therefore, it is essential to control those situations that potentially distress the stem cells at the tooth apex.
Lipopolysaccharide (LPS), a common imitator used for the induction of inflammation, activates various signaling pathways, resulting in pro-inflammatory cytokine production [11, 12]. During the progression of the inflammatory process, intracellular reactive oxygen species (ROS) is upregulated, resulting in mitochondrial dynamic changes and leading to cell apoptosis if uncontrolled [13,14,15]. Hence, the control of mitochondrial dynamics would allow cells to survive during inflammation [16, 17].
N-Acetyl cysteine (NAC), a free radical scavenger, has been generally used to treat oxidative stress–related diseases [18], reduce excessive ROS production, and regulate cell proliferation, differentiation, and apoptosis [19,20,21,22,23,24,25]. Various studies in the dental field have investigated the effects of NAC [19, 26,27,28,29,30]. Most of those studies examined the neutralizing effects of NAC on different types of materials. NAC improves cell survival and proliferation [19, 26, 31,32,33,34,35]. It also exhibits anti-inflammatory effect by suppressing the activation of pro-inflammatory cytokine production and immune response [36,37,38]. Moreover, the use of NAC as an intracanal medicament and root canal irrigating solution exhibits antimicrobial effects against both planktonic bacteria and bacteria in biofilms [20, 23, 25]. However, no studies have examined the effects of NAC in REPs, in particular the effects of NAC on apical papilla cells (APCs) under inflammatory conditions. Therefore, this study examined the effects of NAC on inflammation-induced APCs, in terms of cell survival, mtROS production, inflammatory cytokine production, and mitochondrial dynamics.
Materials and methods
Primary human APC culture
All procedures were in accordance with the ethical standards by the Human Experimentation Committee, Faculty of Dentistry, Chiang Mai University, Chiang Mai, Thailand. APCs, obtained from apical papilla tissues of non-carious immature mandibular third molars from 16- to 20-year-old patients (N = 3), were gently separated and digested in a solution of Collagenase I (Gibco/Invitrogen, Gaithersburg, MD, USA) and Dispase II (Sigma-Aldrich, St. Louis, MO, USA) for 45 min at 37 °C. APCs were cultured in complete alpha-minimum essential medium (⍺-MEM) (Sigma-Aldrich) containing 10% fetal bovine serum (Sigma-Aldrich), 1% penicillin–streptomycin (Sigma-Aldrich), and 100 μmol/L l-ascorbic acid (Sigma-Aldrich) at a 37 °C humidified atmosphere of 95% air and 5% CO2. Cells from the second to third passages were used. All experiments were conducted in triplicate.
AlamarBlue® cell proliferation analysis
APCs, at a density of 1 × 103 cells per well in 96-well plates, were seeded. Then, 20 μg/mL LPS (L4391, Sigma-Aldrich) was added for 24 h followed by NAC (A7250, Sigma-Aldrich). These concentrations were selected according to the results of our pilot study (data not shown). Cell proliferation was measured and calculated using AlamarBlue® Assay (Bio-Rad Laboratories Inc., Hercules, CA, USA) at 24, 48, and 72 h.
Two main experimental studies were assigned to evaluate the various concentrations and durations of NAC treatment.
Part A. Concentration of NAC treatment
Five experimental groups were assigned as follows:
-
1
Control: APCs cultured in regular complete media
-
2
LPS: APCs cultured in 20 μg/mL LPS-containing regular complete media
-
3
LPS/media: APCs cultured in 20 μg/mL LPS-containing regular complete media for 24 h and changed into regular complete media
-
4
LPS/5 mM NAC: APCs cultured in 20 μg/mL LPS-containing regular complete media for 24 h and changed into regular complete media with 5 mM NAC supplement
-
5
LPS/10 mM NAC: Similar to the previous group, but 10 mM NAC supplement was applied.
Part B. Duration of NAC treatment
The experimental groups were designed similar to those in Part A, except that NAC at only 5 mM was selected. Exposure times at 10 min, 24 h, and entire culture periods were selected. The 10-min application was based on the possibility for use as the root canal irrigating solution in clinical application. In the groups in which NAC was administered for a short period, the complete medium was immediately replaced at the specified time and continuously cultured. Cell proliferation was measured at 24, 48, and 72 h (Fig. 1A).
Six experimental groups were assigned as follows:
-
1
Control: APCs cultured in regular complete media
-
2
LPS: APCs cultured in 20 μg/mL LPS-containing regular complete media
-
3
LPS/media: APCs cultured in 20 μg/mL LPS-containing regular complete media for 24 h and replaced with regular complete media for the remainder of the study period
-
4
LPS/NAC10min: APCs cultured in 20 μg/mL LPS-containing regular complete media for 24 h and replaced with 5 mM NAC-containing regular complete media for 10 min
-
5
LPS/NAC24h: APCs cultured in 20 μg/mL LPS-containing regular complete media for 24 h and replaced with 5 mM NAC-containing regular complete media for 24 h
-
6
LPS/NAC: APCs cultured in 20 μg/mL LPS-containing regular complete media for 24 h and replaced with 5 mM NAC-containing regular complete media for the remainder of the study period
Mitochondrial ROS production analysis
The samples assigned in Part B were analyzed for ROS production and RT-PCR at 6 and 24 h after stimulation (Fig. 1B). ROS production in mitochondria (mtROS) was measured using the Mitosox™ Red–based and MitoTracker™ Green indicators (Thermo Fisher Scientific, Waltham, MA). Briefly, APCs at a concentration of 2 × 105 cells/well were cultured in a 96-well plate. After 6- and 24-h incubation, the cells were washed and incubated with 100-μL buffer containing 25 nM MitoTracker™ Green for 20 min at 37 °C and 100 μL of 5 μM Mitosox™ Red for 10 min. The cells were again washed, and their fluorescence intensity was measured with a microplate reader (CLARIOstar Plus microplate reader, BMG LABTECH, Ortenberg, Germany), using wavelengths at 510/580 nm and 490/516 nm. The ratio of MitoSOX™ Red to MitoTracker™ Green was calculated to evaluate the ROS per mitochondrion. Mitochondrial distribution imaging was examined under a fluorescence microscope (Olympus, Tokyo, Japan).
Real-time polymerase chain reaction
APCs were seeded and treated in 6-well plates at a concentration of 3 × 105 cells/well. After 6- and 24-h incubation, total RNA (Nucleospin RNA II extraction kit, Macherey-Nagel, Duren, Germany) was extracted and reversed transcripted using the ReverTra Ace kit (Τoyobo Co., Ltd., Osaka, Japan). Gene expression analyses were performed in triplicate samples with SYBR Green (Takara, Otsu, Japan) by using a LightCycler 480 Real-Time PCR system (Roche Applied Science, Rotkreuz, Switzerland). The condition of RT-PCR was 45 cycles of denaturing at 95 °C for 10 s, annealing at 60 °C for 20 s, and extension at 72 °C for 40 s. The primers for amplification of IL-6, TNF-α, Mfn, Drp-1, Bax, and Bcl-2 were designed based on published sequences as follows: GAPDH (forward) ACC ACA GTC CAT GCC ATC AC, (reverse) TCC ACC ACC CTG TTG CTG TA; IL-6 (forward) ACA GCC ACT CAC CTC TTC AG, (reverse) CCA TCT TTT TCA GCC ATC TTT; TNF-α (forward) CCC GAG TGA CAA GCC TGT AG, (reverse) GAT GGC AGA GAG GAG GTT GAC; Mfn (forward) ATG CAT CCC CAC TTA AGC AC, (reverse) CCA GAG GGC AGA ACT TTG TC; Drp-1 (forward) ACC CGG AGA CCT CTC ATT CT, (reverse) TGA CAA CGT TGG GTG AAA AA; Bax (forward) CCA GCT CTG AGC AGA TCA TG, (reverse) TGC TGG CAA AGT AGA AAA GG; Bcl-2 (forward) GAC TTC GCC GAG ATG TCC AG, (reverse) CAG GTG CCG GTT CAG GTA CT. Quantification of each mRNA was normalized with the housekeeping enzyme GAPDH. The 2−ΔΔCT method was used to determine the mRNA levels.
Statistical analysis
All experiments were conducted in triplicate and statistically analyzed using one-way ANOVA and either Tukey’s or Dunnett’s T3 test by using SPSS 23.0 software (SPSS Inc., Chicago, IL). The difference between experimental groups was considered to be statistically significant at P < .05.
Results
Effects of NAC concentration and exposure time on LPS-treated APC proliferation
The freshly extracted apical papilla cells showed a fibroblast-like morphology. The cells initially started to form multiple sporadic clusters containing small spindle-shaped cells. After 7 days, the cells arranged in a monolayer were observed.
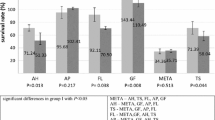
For the experimental results, the LPS/5 mM NAC and LPS/10 mM NAC groups showed the highest cell proliferation at 24 h (P < .05). Cell proliferation in the control, LPS, and LPS/media groups increased for up to 72 h. At 48 h, the LPS/10 mM NAC group showed the lowest cell proliferation (P < .05). At 72 h, both groups using 5 mM and 10 mM NAC had significantly lower cell proliferation compared with the control group (P < .05) (Fig. 2a). Therefore, NAC at the concentration of 5 mM was selected for further studies.
Cell proliferation of LPS-treated APCs in response to different concentrations of NAC at different time points (a). The LPS/5 mM NAC and LPS/10 mM NAC groups showed the highest cell proliferation at 24 h. The LPS/10 mM NAC group showed the lowest cell proliferation at 48 h. Both the LPS/5 mM NAC and LPS/10 mM NAC groups showed the lowest cell proliferation at 72 h. Cell proliferation of LPS-treated APCs in response to different treatment durations of NAC at different time points (b). At 48 and 72 h, the LPS/NAC24h group showed the highest cell proliferation, whereas the LPS/NAC group showed the lowest cell proliferation. *P < .05 compared with the control group. Statistical analyses were performed using one-way ANOVA and either Tukey’s or Dunnett’s T3 test
The proliferation of LPS-treated APCs after exposure to 5 mM of NAC for 10 min, 24 h, and the entire study period was evaluated. At 24 h, no differences in cell proliferation were observed among the groups. At 48 and 72 h, the LPS/NAC (entire period) group exhibited the lowest cell proliferation (P < .05), whereas the highest cell proliferation was observed in the LPS/NAC24h group (P < .05) (Fig. 2b). At all time periods, the exposure of NAC for 10 min did not distress the cell proliferation.
Mitochondrial ROS production of LPS-treated APCs after NAC treatment
The mitochondrial ROS level was significantly increased in the LPS group at both periods when compared with the control group (P < .05). At 6 h, the ROS level was notably reduced in the LPS/media and LPS/NAC groups compared with the LPS group (P < .05). At 24 h, most of the groups showed a comparable ROS level compared with the control, except the LPS group (Fig. 3A). For the fluorescent images, a high intensity of MitoSOX™ Red was observed in the LPS group (Fig. 3B). Mitochondria were diffusely distributed (Fig. 3C).
Bar graphs represent the ROS production per mitochondrion at 6 and 24 h (A). Representative images of MitoSOX™ Red staining of mitochondrial superoxide (B). The fluorescence images of MitoSOX™ Red in red and MitoTracker™ GREEN in green; the nuclear DAPI stain is in blue (C). Scale bars = 50 μm. Data are presented as mean ± SD. Statistical analyses were performed using one-way ANOVA and Tukey’s test. a, b, and c represent significant differences between groups. a indicates the highest average and c indicates the lowest at each time point (P < .05)
Expression of inflammatory markers and mitochondrial morphology–related genes of LPS-treated APCs after NAC treatment
IL-6 and TNF-α
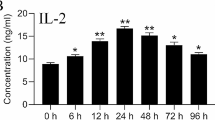
A marked upregulation of IL-6 expression was observed in the LPS group at both periods (P < .05) (Fig. 4a). Positive trends in TNF-α expression were also observed in the LPS group (Fig. 4b). In all treatment groups involving the removal of LPS, the expression of both inflammatory markers was reduced when compared with the LPS group at both time points. Significant reductions in TNF-α and IL-6 were noted in the LPS/NAC10min group at 6 h (P < .05).
The effects of NAC on inflammatory markers (a, b), apoptotic markers (c), and mitochondrial morphology–related markers (d). Untreated APCs served as the normal control for comparison of relative gene expression in all samples. Data are presented as mean ± SD. Statistical analyses were performed using one-way ANOVA and Dunnett’s T3 test. A, B, and C represent significant differences between groups at 6 h; A indicates the highest average and C indicates the lowest. a, b, and c represent significant differences between groups at 24 h; a indicates the highest average and c indicates the lowest (P < .05)
Bcl-2/Bax and Mfn-2/Drp-1
To explore the anti-apoptotic/pro-apoptotic property, the ratio of the Bcl-2/Bax gene was evaluated. At 6 h, the expression was significantly upregulated in most of the groups when compared with the control group. A marked increase was observed in the LPS/NAC and LPS/NAC10min groups (P < .05) (Fig. 4c). Conversely, at 24 h, the expression levels were downregulated in most of the groups, except that the LPS/NAC10min group showed significant constant upregulation compared with the other groups involving the removal of LPS (P < .05).
To measure the mitochondrial dynamics (fusion/fission), the ratio of the Mfn-2/Drp-1 gene was examined. At 6 h, the expression was significantly reduced in the LPS group (P < .05), whereas it was increased in the other groups (Fig. 4d). By contrast, at 24 h, all groups had similar trends, showing the downregulation of these genes when compared with the control.
Discussion
This study evaluated the influence of NAC supplementation on APCs under an inflammatory-induced condition from various aspects, including cell survival, genes regulating pro-inflammatory cytokine production, and mitochondrial dynamics. NAC promoted proliferation of LPS-treated APCs when used at 5 mM for 24 h. Ten-minute application of NAC maintained the survival of the cells comparable with the control. Longer application of NAC (> 24 h) generated deteriorating effects on cell survival. NAC helped retain the mtROS level of LPS-treated APCs at the same level as in the control group. Besides, 10-min NAC application decreased the levels of IL-6 and TNF-α gene expression in LPS-treated APCs. The expression of Bcl-2 and Mfn-2 genes were upregulated in the presence of NAC at 6-h observation.
Various concerns have been raised in the field of regenerative endodontics [7]. The main purpose of regenerative endodontics is to promote consistent best treatment outcomes. One of the major approaches is the modification of procedures related to the cell-based tissue engineering perspective. Apical papilla tissues have been of interest since they are potentially renewable sources of stem cells located around the root of immature teeth [9]. Clinically, in necrotic immature teeth requiring REPs, most of the teeth become necrotic because of negative insults, particularly infection, mainly from gram-negative anaerobic bacteria, followed by inflammation. Therefore, in this study, the APCs were initially induced by bacterial LPS to create a clinically relevant environment. Studies have reported that LPS induced ROS production in various cell types, including human dental pulp cells, periodontal ligament fibroblast, and gingival fibroblast cells, which in turn triggered the impairment of cellular functions [24, 39,40,41]. The pathological levels of ROS inhibit cell proliferation and differentiation and, finally, induce apoptosis [42, 43]. Therefore, it would be beneficial to control the situation after the cells are confronted with inflammation.
NAC, an antioxidant widely used in medicine, is one of the most interesting materials that possess the potential to modulate oxidative stress under a variety of conditions [11, 40, 41, 44,45,46]. In the dental field, NAC helps to reduce the cytotoxic effects of dental materials by inhibiting cell apoptosis, regulating cell proliferation and differentiation, and controlling the synthesis of intracellular ROS [26, 28, 47]. Several studies have reported the anti-inflammatory effect of NAC in dental cells under oxidative stress conditions [11, 24, 37]. Moreover, NAC showed greater efficacy in biofilm cell removal and killing than saturated calcium hydroxide solution and 2% chlorhexidine solution [25]. NAC used as a root canal irrigating solution showed greater inhibition of Enterococcus faecalis and Streptococcus mutans compared with 5.25% sodium hypochlorite and 2% chlorhexidine [23]. Therefore, the adoption of NAC into REPs would offer some benefits since it could control the inflammation and improve the mitochondria function while also reducing bacterial contamination.
The results show that the application of 5 mM NAC controlled the proliferation of LPS-treated APCs. The use of NAC either for 10 min or 24 h maintained and even stimulated cell proliferation. These findings are consistent with those of previous studies reporting NAC-stimulated cell survival and inhibited cell apoptosis [16, 19, 28, 44, 46], for which several mechanisms have been proposed, including the induction of the NF-κB pathway [19], the reduction of oxidative stress [16, 28, 44, 46], and the inhibition of the intrinsic mitochondrial pathway [16, 28, 44, 46]. However, prolonged exposure to NAC (> 48 h) exhibited a deteriorating effect on the proliferation of LPS-treated APCs in our study. The reasons may be due to the alteration of the intracellular redox status and the inhibition of the MAPK pathway [48]. Therefore, the duration of NAC treatment is critical.
With regard to the antioxidant effect of NAC, several studies have reported significant ROS reduction after NAC application in the dental field [11, 40, 41, 44,45,46]. However, in our study, we focused only on the mtROS since mitochondria are a major source of ROS production. Surprisingly, the application of NAC did not alter the level of mtROS. Only the removal of LPS significantly reduced the mtROS level. We speculate that the reduction in mtROS does not depend directly on the anti-oxidative effect of NAC itself [45, 49]. Another role of NAC in GSH replenishment might be a concern [50].
For inflammatory marker expression, LPS activates various signaling pathways, such as NF-κB, MAPK, and p53, resulting in pro-inflammatory cytokine production [24, 37, 51, 52]. In our study, the expression of IL-6 and TNF-α genes were upregulated in the presence of LPS, whereas the expression were markedly reduced when LPS was removed. These findings endorse the bacterial disinfection step as an early phase of regenerative treatment because the reduction of inflammatory cytokine overexpression offers benefits for cell survival and wound healing. Focusing on the supplementation of NAC, a significant reduction in TNF-α and IL-6 was observed in the LPS/NAC10min group. This finding is consistent with that of a previous study revealing the effect of short-term treatment with a low concentration of NAC on inflammatory cytokine reduction [51]. In that study, the long duration of NAC treatment was also tested and revealed that it reversed the level of inflammation as a result of a different activation pathway (via the MAPK, rather than the p53-dependent pathway) [51]. Similar to our results, the considerable increase in IL-6 expression was detected in cells with a prolonged period of NAC treatment. Therefore, short-term NAC treatment (10 min) was more effective than long-term (24 h) treatment in reducing pro-inflammatory cytokines. However, the mechanisms involved in the anti-inflammatory effect of NAC remain unclear. It is possible that the elevation of p53 expression, after NAC stimulation, subsequently inhibits the proinflammatory cytokine expression [51]. Moreover, its antioxidant activity, its ability to modify signaling molecules, and its ability to inhibit cell death are other supportive rationales [11, 19]. However, there are various inflammation-related genes, for example, NADPH Oxidase 4 (NOX4), IL-1β, prostaglandin E-2 (PGE-2), and matrix metalloproteinase-2 (MMP-2), which play important roles in inflammation [53,54,55,56]. Future studies are required to investigate the effect of other pro-inflammatory genes.
Apoptosis is an important mechanism in maintaining tissue homeostasis [57]. Bcl-2, an anti-apoptotic protein, has been proved to regulate this process accompanied with Bax, a pro-apoptotic protein [28, 46, 58]. The balance between Bcl-2 and Bax determines cell survival [57, 58]. In our study, after LPS stimulation, the upregulation of the Bcl-2/Bax ratio was observed at 6 h and was abruptly downregulated in some groups, except LPS/NAC10min, at 24 h. A previous study reported high expression of Bcl-2 after LPS exposure as a result of specific induction from immune cells and cytokines [59]. Therefore, the high expression of the Bcl-2/Bax ratio after exposure to LPS at an early time period may have suddenly impeded cell apoptosis. Besides, it is interesting that the application of NAC for a short period sustained the expression of the Bcl-2/Bax ratio, whereas application for the entire study period significantly reduced the Bcl-2/Bax ratio. It is possible that the duration of NAC treatment is a major concern, as also shown by the cytotoxicity of NAC at 48 and 72 h.
Mitochondria are highly dynamic organelles, controlled by coordinated cycles of fusion and fission [60]. Mitochondrial fusion, a process that alleviates mitochondrial stress by merging the contents of two mitochondria, is regulated by mitofusin 2 (Mfn-2) [60]. Mitochondrial fission, a process that allocates mitochondrial content from one mitochondrion into two mitochondria, is regulated by Dynamin-related protein 1 (Drp-1). The decrease in Mfn-2/Drp-1 ratio increases mitochondrial fission, causing mitophagy and physiological adaptation [61, 62], whereas an increase in the Mfn-2/Drp-1 ratio improves the mitochondrial quality. In our study, the lowest expression of the Mfn-2/Drp-1 ratio was observed in the LPS group, whereas in other groups involving LPS removal, it showed gradual increases in expression. In our findings, the removal of LPS, either with or without NAC supplement, strongly promoted an increase in the Mfn-2/Drp-1 ratio at the early stage. The levels were then diminished at 24 h, suggesting that the response was time dependent. However, it is noteworthy that only the removal of infection by replacing it with either regular media or NAC improved the mitochondrial dynamics from the early stage.
Conclusion
Under the LPS-induced inflammatory condition, NAC stimulated APC survival and decreased inflammation. Ten-minute NAC treatment was sufficient to reduce the level of inflammation and maintain the mitochondrial dynamics.
References
Kahler B, Lin LM (2017) A review of regenerative endodontics: current protocols and future directions. J Istanbul Univ Fac Dent 51(3 Suppl 1):41–51
Iwaya SI, Ikawa M, Kubota M (2001) Revascularization of an immature permanent tooth with apical periodontitis and sinus tract. Dent Traumatol 17(4):185–187
Chandki R, Kala M, Banthia P, Banthia R (2012) From stem to roots: tissue engineering in endodontics. J Clin Exp Dent 4(1):e66–e71. https://doi.org/10.4317/jced.50678
Rafter M (2005) Apexification: a review. Dent Traumatol 21(1):1–8. https://doi.org/10.1111/j.1600-9657.2004.00284.x
Banchs F, Trope M (2004) Revascularization of immature permanent teeth with apical periodontitis: new treatment protocol? J Endod 30(4):196–200. https://doi.org/10.1097/00004770-200404000-00003
AAE clinical considerations for a regenerative procedure revised 4/1/2018 (2018) https://www.aae.org/specialty/wpcontent/uploads/sites/2/2018/06/ConsiderationsForRegEndo_AsOfApril2018.pdf. Accessed 26 Jun 2019
Nosrat A, Homayounfar N, Oloomi K (2012) Drawbacks and unfavorable outcomes of regenerative endodontic treatments of necrotic immature teeth: a literature review and report of a case. J Endod 38(10):1428–1434. https://doi.org/10.1016/j.joen.2012.06.025
Lovelace TW, Henry MA, Hargreaves KM, Diogenes A (2011) Evaluation of the delivery of mesenchymal stem cells into the root canal space of necrotic immature teeth after clinical regenerative endodontic procedure. J Endod 37(2):133–138
Huang GT, Sonoyama W, Liu Y, Liu H, Wang S, Shi S (2008) The hidden treasure in apical papilla: the potential role in pulp/dentin regeneration and bioroot engineering. J Endod 34(6):645–651. https://doi.org/10.1016/j.joen.2008.03.001
Dioguardi M, Di Gioia G, Illuzzi G, Arena C, Caponio VCA, Caloro GA, Zhurakivska K, Adipietro I, Troiano G, Lo Muzio L (2019) Inspection of the microbiota in endodontic lesions. Dent J (Basel) 7(2). https://doi.org/10.3390/dj7020047
Kim DY, Jun JH, Lee HL, Woo KM, Ryoo HM, Kim GS, Baek JH, Han SB (2007) N-acetylcysteine prevents LPS-induced pro-inflammatory cytokines and MMP2 production in gingival fibroblasts. Arch Pharm Res 30(10):1283–1292. https://doi.org/10.1007/bf02980269
Zhang J, Zhang Y, Lv H, Yu Q, Zhou Z, Zhu Q, Wang Z, Cooper PR, Smith AJ, Niu Z, He W (2013) Human stem cells from the apical papilla response to bacterial lipopolysaccharide exposure and anti-inflammatory effects of nuclear factor I C. J Endod 39(11):1416–1422. https://doi.org/10.1016/j.joen.2013.07.018
Li X, Wang X, Zheng M, Luan QX (2016) Mitochondrial reactive oxygen species mediate the lipopolysaccharide-induced pro-inflammatory response in human gingival fibroblasts. Exp Cell Res 347(1):212–221. https://doi.org/10.1016/j.yexcr.2016.08.007
Bullon P, Cordero MD, Quiles JL, Morillo JM, del Carmen Ramirez-Tortosa M, Battino M (2011) Mitochondrial dysfunction promoted by Porphyromonas gingivalis lipopolysaccharide as a possible link between cardiovascular disease and periodontitis. Free Radic Biol Med 50(10):1336–1343. https://doi.org/10.1016/j.freeradbiomed.2011.02.018
Katoh M, Wu B, Nguyen HB, Thai TQ, Yamasaki R, Lu H, Rietsch AM, Zorlu MM, Shinozaki Y, Saitoh Y, Saitoh S, Sakoh T, Ikenaka K, Koizumi S, Ransohoff RM, Ohno N (2017) Polymorphic regulation of mitochondrial fission and fusion modifies phenotypes of microglia in neuroinflammation. Sci Rep 7(1):4942. https://doi.org/10.1038/s41598-017-05232-0
He Y, Gan X, Zhang L, Liu B, Zhu Z, Li T, Zhu J, Chen J, Yu H (2018) CoCl2 induces apoptosis via a ROS-dependent pathway and Drp1-mediated mitochondria fission in periodontal ligament stem cells. Am J Phys Cell Phys 315(3):C389–C397. https://doi.org/10.1152/ajpcell.00248.2017
Chiong M, Cartes-Saavedra B, Norambuena-Soto I, Mondaca-Ruff D, Morales PE, Garcia-Miguel M, Mellado R (2014) Mitochondrial metabolism and the control of vascular smooth muscle cell proliferation. Front Cell Dev Biol 2:72. https://doi.org/10.3389/fcell.2014.00072
Berniakovich I, Laricchia-Robbio L, Izpisua Belmonte JC (2012) N-acetylcysteine protects induced pluripotent stem cells from in vitro stress: impact on differentiation outcome. Int J Dev Biol 56(9):729–735. https://doi.org/10.1387/ijdb.120070ji
Paranjpe A, Cacalano NA, Hume WR, Jewett A (2007) N-acetylcysteine protects dental pulp stromal cells from HEMA-induced apoptosis by inducing differentiation of the cells. Free Radic Biol Med 43(10):1394–1408. https://doi.org/10.1016/j.freeradbiomed.2007.07.011
Ulusoy AT, Kalyoncuoglu E, Reis A, Cehreli ZC (2016) Antibacterial effect of N-acetylcysteine and taurolidine on planktonic and biofilm forms of Enterococcus faecalis. Dent Traumatol 32(3):212–218. https://doi.org/10.1111/edt.12237
Camargo CHR, Gomes LCL, Franca MCM, Bittencourt TS, Valera MC, Camargo SEA, Bottino MC (2019) Incorporating N-acetylcysteine and tricalcium phosphate into epoxy resin-based sealer improved its biocompatibility and adhesiveness to radicular dentine. Dent Mater 35(12):1750–1756. https://doi.org/10.1016/j.dental.2019.09.001
Edlundh-Rose E, Kupershmidt I, Gustafsson AC, Parasassi T, Serafino A, Bracci-Laudiero L, Greco G, Krasnowska EK, Romano MC, Lundeberg T, Nilsson P, Lundeberg J (2005) Gene expression analysis of human epidermal keratinocytes after N-acetyl L-cysteine treatment demonstrates cell cycle arrest and increased differentiation. Pathobiology 72(4):203–212. https://doi.org/10.1159/000086790
Bhasin P, Sharma M, Bindal D, Tomar D, Sarin A, Sharma N (2019) An in vitro evaluation of antimicrobial effects of three different root canal irrigating solutions against Enterococcus faecalis and Streptococcus mutans. J Contemp Dent Pract 20(2):221–225
Zheng R, Tan Y, Gu M, Kang T, Zhang H, Guo L (2019) N-acetyl cysteine inhibits lipopolysaccharide-mediated synthesis of interleukin-1beta and tumor necrosis factor-alpha in human periodontal ligament fibroblast cells through nuclear factor-kappa B signaling. Medicine (Baltimore) 98(40):e17126. https://doi.org/10.1097/MD.0000000000017126
Choi YS, Kim C, Moon JH, Lee JY (2018) Removal and killing of multispecies endodontic biofilms by N-acetylcysteine. Braz J Microbiol 49(1):184–188. https://doi.org/10.1016/j.bjm.2017.04.003
Minamikawa H, Yamada M, Deyama Y, Suzuki K, Kaga M, Yawaka Y, Ogawa T (2011) Effect of N-acetylcysteine on rat dental pulp cells cultured on mineral trioxide aggregate. J Endod 37(5):637–641. https://doi.org/10.1016/j.joen.2011.02.012
Kim NR, Park HC, Kim I, Lim B-S, Yang H-C (2010) In vitro cytocompatibility of N-acetylcysteine–supplemented dentin bonding agents. J Endod 36(11):1844–1850
Jiao Y, Ma S, Wang Y, Li J, Shan L, Liu Q, Liu Y, Song Q, Yu F, Yu H, Liu H, Huang L, Chen J (2016) N-acetyl cysteine depletes reactive oxygen species and prevents dental monomer-induced intrinsic mitochondrial apoptosis in vitro in human dental pulp cells. PLoS One 11(1):e0147858. https://doi.org/10.1371/journal.pone.0147858
Chang M-C, Lin L-D, Wu M-T, Chan C-P, Chang H-H, Lee M-S, Sun T-Y, Jeng P-Y, Yeung S-Y, Lin H-J (2015) Effects of camphorquinone on cytotoxicity, cell cycle regulation and prostaglandin E2 production of dental pulp cells: role of ROS, ATM/Chk2, MEK/ERK and hemeoxygenase-1. PLoS One 10(12):e0143663
Lee DH, Lim B-S, Lee Y-K, Yang H-C (2007) Mechanisms of root canal sealers cytotoxicity on osteoblastic cell line MC3T3-E1. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 104(5):717–721
Xiong L, Sun J, Hirche C, Yang J, Yang Y, Xia Y, Lehnhardt M, Wang R, Fu X (2012) In vitro N-acetyl-L-cysteine promotes proliferation and suppresses interleukin-8 expression in adipose-derived stem cells. Aesthet Plast Surg 36(5):1260–1265. https://doi.org/10.1007/s00266-012-9960-8
Sun LY, Pang CY, Li DK, Liao CH, Huang WC, Wu CC, Chou YY, Li WW, Chen SY, Liu HW, Chang YJ, Cheng CF (2013) Antioxidants cause rapid expansion of human adipose-derived mesenchymal stem cells via CDK and CDK inhibitor regulation. J Biomed Sci 20:53. https://doi.org/10.1186/1423-0127-20-53
Ali F, Qadir AUR, Fatima N, Wajid N (2017) The effect of N-acetyl cysteine on H2O2 mediated oxidative stress in Whartonʼs jelly derived mesenchymal stem cells. Adv Life Sci 4(4):137–142
Debeljak Martacic J, Borozan S, Radovanovic A, Popadic D, Mojsilovic S, Vucic V, Todorovic V, Kovacevic Filipovic M (2016) N-acetyl-L-cysteine enhances ex-vivo amplification of deciduous teeth dental pulp stem cells. Arch Oral Biol 70:32–38. https://doi.org/10.1016/j.archoralbio.2016.06.002
Ali F, Rafique H, Wajid N (2015) N-acetylcysteine prevents cord derived stem cells from H2O2 induced injury in vitro. EJPMR 2:589–598
Kim E-C, Kim M-K, Leesungbok R, Lee S-W, Ahn S-J (2016) Co–Cr dental alloys induces cytotoxicity and inflammatory responses via activation of Nrf2/antioxidant signaling pathways in human gingival fibroblasts and osteoblasts. Dent Mater 32(11):1394–1405
Guo L, Zhang H, Li W, Zhan D, Wang M (2018) N-acetyl cysteine inhibits lipopolysaccharide-mediated induction of interleukin-6 synthesis in MC3T3-E1 cells through the NF-kB signaling pathway. Arch Oral Biol 93:149–154. https://doi.org/10.1016/j.archoralbio.2018.06.007
Pei Y, Liu H, Yang Y, Yang Y, Jiao Y, Tay FR, Chen J (2018) Biological activities and potential oral applications of n-acetylcysteine: progress and prospects. Oxid Med Cell Longev 2018:2835787. https://doi.org/10.1155/2018/2835787
Kim JC, Lee YH, Yu MK, Lee NH, Park JD, Bhattarai G, Yi HK (2012) Anti-inflammatory mechanism of PPARgamma on LPS-induced pulp cells: role of the ROS removal activity. Arch Oral Biol 57(4):392–400. https://doi.org/10.1016/j.archoralbio.2011.09.009
Golz L, Memmert S, Rath-Deschner B, Jager A, Appel T, Baumgarten G, Gotz W, Frede S (2014) LPS from P. gingivalis and hypoxia increases oxidative stress in periodontal ligament fibroblasts and contributes to periodontitis. Mediat Inflamm 2014:986264–986213. https://doi.org/10.1155/2014/986264
Cheng R, Choudhury D, Liu C, Billet S, Hu T, Bhowmick NA (2015) Gingival fibroblasts resist apoptosis in response to oxidative stress in a model of periodontal diseases. Cell Death Dis 1:15046. https://doi.org/10.1038/cddiscovery.2015.46
Karadzic I, Vucic V, Jokanovic V, Debeljak-Martacic J, Markovic D, Petrovic S, Glibetic M (2015) Effects of novel hydroxyapatite-based 3D biomaterials on proliferation and osteoblastic differentiation of mesenchymal stem cells. J Biomed Mater Res A 103(1):350–357. https://doi.org/10.1002/jbm.a.35180
Xiao Y, Li X, Cui Y, Zhang J, Liu L, Xie X, Hao H, He G, Kander MC, Chen M, Liu Z, Verfaillie CM, Zhu H, Lei M, Liu Z (2014) Hydrogen peroxide inhibits proliferation and endothelial differentiation of bone marrow stem cells partially via reactive oxygen species generation. Life Sci 112(1–2):33–40. https://doi.org/10.1016/j.lfs.2014.07.016
Martacic J, Filipovic MK, Borozan S, Cvetkovic Z, Popovic T, Arsic A, Takic M, Vucic V, Glibetic M (2018) N-acetyl-L-cysteine protects dental tissue stem cells against oxidative stress in vitro. Clin Oral Investig 22(8):2897–2903. https://doi.org/10.1007/s00784-018-2377-2
Diomede F, Marconi GD, Guarnieri S, D'Attilio M, Cavalcanti M, Mariggio MA, Pizzicannella J, Trubiani O (2019) A novel role of ascorbic acid in anti-inflammatory pathway and ROS generation in HEMA treated dental pulp stem cells. Materials (Basel) 13(1). https://doi.org/10.3390/ma13010130
Zhang Y, Xiao J-f, Yang H-f, Cao W-w, Shi H-m, Cun J-f, Tay FR, Ping J, Jiao Y, Xiao Y-h (2020) N-acetyl cysteine as a novel polymethyl methacrylate resin component: protection against cell apoptosis and genotoxicity. Oxid Med Cell Longev 2020:1301736. https://doi.org/10.1155/2019/1301736
Jiao Y, Ma S, Li J, Shan L, Wang Y, Tian M, Yang Y, Sun J, Ban J, Chen J (2015) N-acetyl cysteine (NAC)-directed detoxification of methacryloxylethyl cetyl ammonium chloride (DMAE-CB). PLoS One 10(8):e0135815. https://doi.org/10.1371/journal.pone.0135815
Sato N, Ueno T, Kubo K, Suzuki T, Tsukimura N, Att W, Yamada M, Hori N, Maeda H, Ogawa T (2009) N-acetyl cysteine (NAC) inhibits proliferation, collagen gene transcription, and redox stress in rat palatal mucosal cells. Dent Mater 25(12):1532–1540. https://doi.org/10.1016/j.dental.2009.07.006
Valdivieso AG, Dugour AV, Sotomayor V, Clauzure M, Figueroa JM, Santa-Coloma TA (2018) N-acetyl cysteine reverts the proinflammatory state induced by cigarette smoke extract in lung Calu-3 cells. Redox Biol 16:294–302. https://doi.org/10.1016/j.redox.2018.03.006
Cheng G, Zielonka M, Dranka B, Kumar SN, Myers CR, Bennett B, Garces AM, Dias Duarte Machado LG, Thiebaut D, Ouari O, Hardy M, Zielonka J, Kalyanaraman B (2018) Detection of mitochondria-generated reactive oxygen species in cells using multiple probes and methods: potentials, pitfalls, and the future. J Biol Chem 293(26):10363–10380. https://doi.org/10.1074/jbc.RA118.003044
Ohnishi T, Bandow K, Kakimoto K, Kusuyama J, Matsuguchi T (2014) Long-time treatment by low-dose N-acetyl-L-cysteine enhances proinflammatory cytokine expressions in LPS-stimulated macrophages. PLoS One 9(2):e87229. https://doi.org/10.1371/journal.pone.0087229
Jun J-H, Lee H-L, Woo KM, Ryoo H-M, Kim G-S, Baek J-H, Han S-B (2007) N-acetyicysteine prevents lps-lnduced pro-inflammatory cytokines and mmp2 production in gingival fibroblasts. Arch Pharm Res 30(10):1283
Manicone AM, McGuire JK (2008) Matrix metalloproteinases as modulators of inflammation. In: Seminars in cell & developmental biology, vol 1. Elsevier, pp 34–41
Lozhkin A, Vendrov AE, Pan H, Wickline SA, Madamanchi NR, Runge MS (2017) NADPH oxidase 4 regulates vascular inflammation in aging and atherosclerosis. J Mol Cell Cardiol 102:10–21. https://doi.org/10.1016/j.yjmcc.2016.12.004
Ricciotti E, FitzGerald GA (2011) Prostaglandins and inflammation. Arterioscler Thromb Vasc Biol 31(5):986–1000. https://doi.org/10.1161/ATVBAHA.110.207449
Ren K, Torres R (2009) Role of interleukin-1beta during pain and inflammation. Brain Res Rev 60(1):57–64. https://doi.org/10.1016/j.brainresrev.2008.12.020
Yang H, Zhu YT, Cheng R, Shao MY, Fu ZS, Cheng L, Wang FM, Hu T (2010) Lipopolysaccharide-induced dental pulp cell apoptosis and the expression of Bax and Bcl-2 in vitro. Braz J Med Biol Res 43(11):1027–1033. https://doi.org/10.1590/s0100-879x2010007500102
Renault TT, Manon S (2011) Bax: addressed to kill. Biochimie 93(9):1379–1391. https://doi.org/10.1016/j.biochi.2011.05.013
Chand HS, Harris JF, Tesfaigzi Y (2018) IL-13 in LPS-induced inflammation causes Bcl-2 expression to sustain hyperplastic mucous cells. Sci Rep 8(1):436. https://doi.org/10.1038/s41598-017-18884-9
Fu W, Liu Y, Yin H (2019) Mitochondrial dynamics: biogenesis, fission, fusion, and mitophagy in the regulation of stem cell behaviors. Stem Cells Int 2019:9757201–9757215. https://doi.org/10.1155/2019/9757201
Givvimani S, Pushpakumar S, Veeranki S, Tyagi SC (2014) Dysregulation of Mfn2 and Drp-1 proteins in heart failure. Can J Physiol Pharmacol 92(7):583–591. https://doi.org/10.1139/cjpp-2014-0060
Lee JE, Seo BJ, Han MJ, Hong YJ, Hong K, Song H, Lee JW, Do JT (2020) Changes in the expression of mitochondrial morphology-related genes during the differentiation of murine embryonic stem cells. Stem Cells Int 2020:1–12
Acknowledgments
The authors thank the Center of Molecular and Cell Biology of Infectious Diseases Research and Cardiac Electrophysiology Research and Training Center, Chiang Mai University, for the provision of equipment. They also thank Dr. M. Kevin O Carroll, Professor Emeritus of the University of Mississippi School of Dentistry, Oxford, MS, and Faculty Consultant at Chiang Mai University, for his assistance in the preparation of the manuscript.
Funding
The work was supported by a grant from the Faculty of Dentistry of Chiang Mai University.
Author information
Authors and Affiliations
Contributions
Nutcha Jariyamana: validation, formal analysis, investigation, writing—original draft, visualization. Patchanee Chuveera: resources. Anat Dewi: data curation. Warat Leelapornpisid: data curation. Jitjiroj Ittichaicharoen: resources. Siriporn Chattipakorn: supervision. Tanida Srisuwan: conceptualization, methodology, writing—review and editing, project administration.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards by the Human Experimentation Committee, Faculty of Dentistry, Chiang Mai University (No. 13/2019) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jariyamana, N., Chuveera, P., Dewi, A. et al. Effects of N-acetyl cysteine on mitochondrial ROS, mitochondrial dynamics, and inflammation on lipopolysaccharide-treated human apical papilla cells. Clin Oral Invest 25, 3919–3928 (2021). https://doi.org/10.1007/s00784-020-03721-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03721-7