Abstract
The aim of this study was to assess the push-out bond strengths of self-adhesive resin cements to epoxy resin-based fiber posts after challenging by thermocycling. Thirty-six single-rooted premolars were endodontically treated, and the post-spaces were drilled to receive RelyX Fiber posts #1. Three self-adhesive resin cements (RelyX Unicem, G-Cem, and Breeze) were used for luting fiber posts. The bonded specimens were either stored for 1 month in a moist field (37°C) or submitted to thermocycling (5,000 times) prior to push-out test. The maximum force required to dislodge the post via an apical–coronal direction was recorded (megapascal). The data were statistically analyzed with two-way ANOVA and Tukey tests (p < 0.05). The factors “luting cement” and “thermocycling” significantly influenced bond strengths. The initial push-out values of RelyX Unicem and Breeze were higher than those of G-Cem. After thermocycling, the bond strength of G-Cem increased and no differences were found between groups. RelyX Unicem and Breeze bond strengths were not affected by the thermal challenge. Thermal cycling and cement type differently influence the bond strengths of self-adhesive resin cements. Self-adhesive cements can represent an option for luting fiber posts into root canal
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Fiber posts are routinely used in dental practice for increasing the retentive strength of postendodontic restorations in the cases of massive coronal destruction [1–3]. Due to their passive retention into root canals, the dislocation resistance of fiber posts is mainly ascribed to the luting agents and cementation techniques [4, 5]. Resin-based luting materials are preferred for fiber post cementation, as an increase in post retention and higher fracture resistance are expected when compared to conventional cements [6, 7].
Post debondings have been indicated as the most unfavorable situations for post-restored teeth [1, 8]; in this context, the use of different resin cements can influence the results [9, 10]. Self-adhesive cements represent a subgroup of resin cements and are characterized by one-step, simple, and standardized adhesive procedures. These one-step cements do not require pre-conditioning of the post-space walls. Due to the variability of the substrate, bonding to intra-radicular dentin has been considered a challenge. Simplifying luting procedures would be helpful in overcoming some technical problems observed with multi-step cements systems [9], such as the difficult control of moisture and/or the chemical incompatibility between simplified adhesives and dual-cured methacrylate-based resin cements [11–14]. Self-adhesive composite cements exhibited similar push-out bond strength values [4, 15] and higher displacement resistance [16, 17] when compared to resin cements that rely on multi-step adhesive systems.
The bond strength of dental biomaterials can be quantitatively assessed with the push-out test. The push-out test has been considered appropriate for measuring the bond strength inside the root canal, as the shear movements are created parallel to the cement/dentin and cement/post interfaces and seems to procure similar stresses to those occurring in clinical conditions [18, 19]. A push-out design combined to dynamic stresses (i.e., thermocycling) allows for a better understanding of dental materials properties in vitro. Thermal cycling is conventionally used to simulate the thermal changes occurring in the oral cavity during eating, drinking, or breathing which may concur in stressing the adhesive interfaces [20–22]. A previous investigation tested the effect of 5,000 thermal cycles on the bond strength of RelyX Unicem in the endodontic space [23]. However, little information is present regarding the bonding ability of other auto-adhesive luting agents employed for the cementation of fiber posts inside the root canal [24]. Self-adhesive cements possess different chemical compositions that can differentiate their bonding mechanism and a comparison between differently branded luting materials is warranted.
Therefore, the present laboratory study was conducted to evaluate the influence of thermal cycling and cement type on the bond strength of translucent glass fiber posts luted with different self-adhesive resin cements. The null hypothesis tested was that thermal cycling and the type of cement do not affect the bond strength of the tested self-adhesive resin cements when luting fiber posts into root canals.
Materials and methods
Specimen preparation
Thirty-six extracted, single-rooted human premolars stored in 0.5% chloramine T solution at 4°C were collected after the informed consent of the donors was obtained. Exclusion criteria were presence of caries, cracks, or resorptions on the root. The crown of each tooth was removed 1 mm above the CEJ by means of a slow-speed diamond saw (Isomet; Buehler, Lake Bluff, IL, USA) under copious water cooling. Working length was established at 1 mm from the root apex. Cleaning and shaping of the root canal were performed with Protaper Ni-Ti rotatory instruments (size S1, S2, S3. Dentsply Maillefer, Ballaigues, Switzerland) following the crown-down technique. Irrigations with 2.5% sodium hypochlorite were performed between the instrumentations. The roots were dried with paper points, filled with gutta-percha cones (Coltène/Whaledent, Langenau, Germany) and cemented with a resin sealer (AH Plus Jet; Dentsply DeTrey, Konstanz, Germany) according to the lateral condensation technique. The canal access was sealed with a temporary restorative material (Fuji VII; GC Corporation, Tokyo, Japan; batch no. 0410221) and stored in a laboratory incubator (100% relative humidity; 37°C). After 24 h, the coronal seal was abraded by means of #240 SiC paper under water cooling, and the gutta-percha was removed with a pre-shaping drill (Dentsply DeTrey), leaving a 5-mm-long apical seal. A 10-mm-deep post-space was prepared with a universal drill (3 M ESPE, Seefeld, Germany) to match the size of the corresponding epoxy resin-based RelyX Fiber Post (#1; 3 M ESPE; Lot: 02363200603). The post was tried-in the prepared post-space and then cut with a bur mounted on a water-coolant handpiece to the selected coronal length. Three self-adhesive materials were employed for fiber post cementation (n = 12): (1) RelyX Unicem (3 M ESPE), (2) G-Cem (GC Corporation, Tokyo, Japan), and (3) Breeze (Pentron Clinical Technologies, Wallingford, CT, USA).
Each material was handled according to manufacturer’s instructions. Application modes, chemical composition, and batch numbers of the materials investigated are presented in Table 1.
Self-adhesive cements polymerized in a dual-cure mode. Immediately, 2 s of light curing allowed the removal of the extruding cement with a spatula. After the first 5 min of auto-cure, during which the post was seated to full depth in the prepared spaces using finger pressure, additional 40 s of light polymerization through the top of the translucent fiber post was performed (Astralis 7; Ivoclar-Vivadent, Schaan, Liechtenstein; output 500 mW/cm2). A core buildup was created with a resin composite core material (CoreX; Dentsply DeTrey; Konstanz, Germany; batch no. 0703000080). All bonded specimens were stored for 1 month in a flower sponge slightly moist with deionized water in a laboratory stove at 37°C and relative humidity.
Prior to push-out test, half of the specimens (n = 18) were additionally thermocycled for 5,000 cycles in deionized water from 5°C to 50°C. The dwelling time at each temperature was 30 s in each bath; the transport time between the water baths was 2 s.
Push-out bond strength test
The coronal portion of each root containing the fiber post was sectioned perpendicular to the long axis with a low-speed diamond saw (Isomet; thickness 0.1 mm) under water cooling to create 1.00 ± 0.05-mm-thick slices. The apical side of each slice was marketed with an indelible marker, and the slice was then placed on the universal test machine. The cylindrical plunger of the testing machine (Triax 50; Controls, Milan, Italy) dislodged, via an apical–coronal direction, each inverted, truncated fiber post from the root dentin. A load (cross-head speed 0.5 mm/min until failure) was then applied to the post surface that resulted in shear stresses along the cement/dentin–cement/post interfaces. The retentive strength of the post fragment (megapascal) was calculated by dividing the load at failure (Newton) by the interfacial area of the post segment (S L). The formula used for measuring the troncoconical area was as follows:
In which π was equal to 3.14, R and r were the coronal and the apical post radius, respectively, and h the root slice thickness. The diameters of the post and the thickness of the slice were individually measured using a digital caliper with 0.01 mm accuracy (Orteam; Milan, Italy). Failure modes were evaluated by a single operator under a stereomicroscope (Olympus SZ-CTV; Olympus, Tokyo, Japan) at ×40 magnification and classified as cohesive (within the cement, C), adhesive (between the post and the cement, AP, or at the cement/root dentin level, AD), or mixed (adhesive and cohesive fractures occurred simultaneously, M).
Statistical analysis
The normal and equal distributions of the push-out bond strength data were first checked and verified by the Kolmogorov–Smirnov and Levene’s test, respectively. A two-way ANOVA was executed to determine the effect of the type of cement, thermocycling, and interactions (p < 0.05). Mean bond strengths of the three cements were analyzed with the Tukey test for post hoc multiple comparisons (p < 0.05). Calculations were handled by the SPSS 15.0 software (SPSS; Chicago, IL, USA).
Results
Bond strength was significantly influenced by the luting material (F = 14.640; p < 0.0005) and thermocycling (F = 18.205; p < 0.0005); interactions were also significant (F = 3.836; p = 0.001). Mean push-out bond strengths and standard deviations (SD) of the tested cements (megapascal) are shown in Table 2.
Initially, the push-out bond strengths of RelyX Unicem and Breeze were statistically comparable and higher than those exhibited by G-Cem. Thermocycling did not affect the bond strengths of RelyX Unicem and Breeze. After the thermal challenge, increased push-out values were registered for G-Cem when compared to the initial group, and no differences were then found among the tested groups.
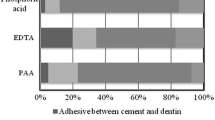
The most frequently recorded modes of failure were adhesives at the cement/dentin interfaces (Table 3). Debonded specimens between cement and fiber posts were also recorded both in the initial and in the thermocycled groups. Cohesive failures within the cement were only registered for RelyX Unicem prior to thermocycling. Mixed failures were observed for RelyX Unicem and G-Cem before being thermally challenged.
Discussion
The present investigation dealt with the push-out bond strengths of three differently branded self-adhesive resin cements used to lute fiber posts into root canal. The tested materials were selected as they possess different chemical composition that would differentiate their bonding mechanism [25]. Additionally, RelyX Unicem was the most investigated self-adhesive luting agent, while little information is present in literature regarding the bonding performances of Breeze and G-Cem before and after being thermally challenged. The null hypothesis was rejected as bond strengths were influenced by the type of cement and thermocycling.
The push-out test is a practical method to test the multiple variables that can affect the retention of posts, resulting in shear stresses at the cement/dentin and cement/fiber post interfaces. The push-out design is considered more reliable than the microtensile technique for testing the bond strength inside the root canal. Lower incidence of premature failures has been reported when using the push-out test instead of the microtensile method [18, 26]. Due to the substantial premature failures registered when self-adhesive cements were used on dentin and tested with a microtensile test [27, 28], the push-out technique was used in the present investigation.
Quasistatic evaluations seemed to not be enough for a complete understanding of dental material properties, and in this context, dynamic stresses become of great importance. Although in vivo studies are the ultimate testing stages, laboratory tests and aging simulations are important sources for reproducing intra-oral conditions [18, 29, 30]. Thermocycling test is conventionally used to simulate the thermal changes and water exposure that may occur in the oral cavity during eating, drinking, or even breathing [21]. The ISO TR 11450 [31] reports that 500 thermocycles in water (5°C and 55°C) are an appropriate method to test thermal stability of a dental material. To date, concerns still arise on the ability of the test to simulate intra-oral aging. In the present study, the measurements of push-out bond strengths were performed prior and after thermal cycling. The challenging parameters applied in the investigation are in accordance with previous studies [23, 32, 33]. Bitter et al. reported higher push-out bond strengths with RelyX Unicem, after being submitted to 5,000 thermal cycles [23]. An important difference is that in the present study, the roots were not isolated in order to directly expose the bonded interfaces to the different temperatures.
No differences in push-out values were encountered for RelyX Unicem and Breeze before or after being thermally challenged. An increase in bond strength was previously reported for RelyX Unicem when used for luting fiber posts or ceramic restorations [34, 35]. Although the authors admit that this finding is difficult to explain, it was speculated that the thermal stress occurring during the laboratory test would enhance the chemical polymerization of the materials, promoting their complete setting reactions [23, 34, 35]. In the present study, the roots were not embedded in acrylic resins and no isolation was created around the bonded interfaces. The direct exposure of the root to the different temperatures may have promoted weak adhesive–dentin interfaces counting for the differences registered between the investigations. Some questions arise on the degree of monomer conversion of self-adhesive cements when used in an auto-cure mode, as an incomplete polymerization is expected and it will jeopardize bond strength [36, 37]. If so, dual-curing self-adhesive cements have become imperative for achieving reliable bonding. Conversely, Mazzoni et al. reported inferior bond strengths of RelyX Unicem when compared to resin cements that rely on multi-step adhesive systems and after being thermally challenged for 40,000 cycles revealing an increase of silver nitrate deposition at the cement/dentin interface [38]. Limited demineralization/infiltration into dentin was previously observed for several self-adhesive cements, and no hybrid layers were observed at the adhesive interfaces [39, 40]. The lack of an effective hybrid layer and the high viscosity of the materials resulted in the lowest bond strength of selected self-adhesive cements [26, 40], renewing concerns regarding the effective sealing ability of self-adhesive cements. Future studies are warranted to fully investigate on this topic.
Scarce information is present in literature regarding the bonding ability of Breeze as fiber post cementing agent. When compared to another self-adhesive cement and a glass-ionomer cement, Breeze showed the highest dislodgement force after being stored in water for 30 days [17]. Breeze is composed of a mixture of hydrophilic components (i.e., BisGMA and HEMA) and hydrophobic monomers (i.e., TEGDMA). The latter molecule furnishes the material hydrophobic characteristics necessary to withstand the moisture condition of dentin when submitted to thermal challenging and prevent excessive water sorption that would jeopardize the polymerization reaction of the material. This may have accounted for the lack of differences recorded for Breeze prior and after being aged. However, further studies are required to better define the bonding performance of Breeze.
G-Cem previously showed the worse push-out values when used for luting fiber posts in comparison to RelyX Unicem and multi-step resin cements [10]. Although the auto-adhesion mechanism of G-Cem follows a glass-ionomer technology (G-Cem technical information, GC Corp.), its high viscosity has been responsible of the scarce interaction with the adhesive substrates [10]. However, bond strength of G-Cem increased after thermal challenging. Thermal changes will cause expansion/contraction stresses within the material [22, 41], which may affect the adhesive stability, but the cement expansion will also create frictions along the root canals that are thought to improve its mechanical retention [42]. After setting, G-Cem showed a porous appearance at the adhesive interface [27]. The pores would function as stresses–absorbers that would prevent the premature degradation of the adhesive interfaces [43]. It remains to be proved if prolonged expansion/contraction phenomena would result in crack formations within the cement bulk hence diminishing the mechanical properties of the material and if the pores present in the material would resist to prolonged cycles and mechanical occlusal loading and their resistance to degradation when submitted to chemical solutions (i.e., sodium hypochlorite).
The importance of using the cement/post combination recommended by each manufacturer has been previously emphasized [9, 38]. Glass, quartz, zirconium, and/or titanium posts differ in terms of structure, composition, and mechanical properties that can influence their bonding mechanism as well as affect their responses to chemo/mechanical treatments. In the present investigation, only one type of post was used, which is made of glass fibers (60–70 vol.%) embedded in an epoxy resin (RelyX Fiber Post technical pamphlet, 3 M ESPE). Although no differences were found between cements after thermocycling, the bonding performance of self-adhesive cements to other differently branded fiber posts should also be evaluated.
The most frequently registered modes of failures were adhesives between cement and dentin, followed by adhesive at the cement/post interface both prior to and after thermocycling (Table 3). The self-adhesive cement–dentin joint represents the weakest point of the one-step cements. Although self-adhesive cements do not require any pre-treatment of the bonding substrate, their retention was increased once the post-space cavity was roughened, resulting in micromechanical grooves formations were the cement could flow and establish an improved bonding [15]. Doubts also exist on the efficacy of pre-treating fiber posts in the attempt to increase the retention of the auto-adhesive cements/fiber post bonds, such as with silane agents [44]. Due to the limited chemical interaction established between self-adhesive cements and fiber posts, chemomechanical post surface treatments could be proposed to increase the surface area available for bonding and enhance microretentions [45].
In general, bond strength of dual-cure self-adhesive luting agents is not compromised by physiologic thermal stresses. Although further studies are desirable to define the overall bonding process of the different self-adhesive luting agents, a combination of chemical adhesion and mechanical retention seemed to characterize the adhesion mechanism of these simplified cements.
Conclusions
Within the limits of this study, it can be concluded that self-adhesive cement type and thermal cycling influence the bond strengths to fiber posts into root canal. Push-out bond strength values of G-Cem increased after the thermal challenge.
References
Schwartz RS, Robbins JW (2004) Post placement and restoration of endodontically treated teeth: a literature review. J Endod 30:289–301
Salameh Z, Ounsi HF, Aboushelib MN, Sadig W, Ferrari M (2008) Fracture resistance and failure patterns of endodontically treated mandibular molars with and without glass fiber post in combination with a zirconia-ceramic crown. J Dent 36:513–519
Bitter K, Noetzel J, Stamm O, Vaudt J, Meyer-Lueckel H, Neumann K, Kielbassa AM (2009) Randomized clinical trial comparing the effects of post placement on failure rate of postendodontic restorations: preliminary results of a mean period of 32 months. J Endod 35:1477–1482
Bitter K, Priehn K, Kielbassa AM (2006) In vitro evaluation of push-out bond strengths of various luting agents to tooth-colored posts. J Prosthet Dent 95:302–310
D’Arcangelo C, D’Amario M, Vadini M, Zazzeroni S, De Angelis F, Caputi S (2008) An evaluation of luting agent application technique effect on fibre post retention. J Dent 36:235–240
Dietschi D, Duc O, Krejci I, Sadan A (2008) Biomechanical considerations for the restoration of endodontically treated teeth: a systematic review. Part II (evaluation of fatigue behavior, interfaces and in vivo studies). Quintessence Int 39:117–129
Rosenstiel SF, Land MF, Crispin BS (1998) Dental luting agents: a review of the current literature. J Prosthet Dent 80:280–301
Ferrari M, Cagidiaco MC, Grandini S, De Sanctis M, Goracci C (2007) Post placamento affects serviva of endodontically treated premolars. J Dent Res 86:729–734
Radovic I, Mazzitelli C, Chieffi N, Ferrari M (2008) Evaluation of the adhesion of fiber posts cemented using different adhesive approach. Eur J Oral Sci 116:557–563
Zicari F, Coutinho E, De Munck J, Poitevin A, Scotti R, Naert I, Van Meerbeek B (2008) Bonding effectiveness and sealing ability of fiber-post bonding. Dent Mater 24:967–977
Carrilho MRO, Carvalho RM, Tay FR, Pashley DH (2004) Effects of storage media on mechanical properties of adhesive systems. Am J Dent 17:104–108
Chersoni S, Acquaviva GL, Prati C, Ferrari M, Grandini S, Pahley DH, Tay FR (2005) In vivo fluid movement through dentin adhesives in endodontically treated teeth. J Dent Res 19:223–227
Pfeifer C, Shih D, Braga RR (2003) Compatibility of dental adhesives and dual-cure cements. Am J Dent 16:235–238
Tay FR, Suh BI, Pashley DH, Prati C, Chuang SF, Li F (2003) Factors contributing to the incompatibility between simplified-step adhesives and self-cured or dual-cured composites. Part II. Single bottle, total-etch adhesive. J Adhes Dent 5:91–105
Balbosh A, Ludwig K, Kern M (2005) Comparison of titanium dowel retention using four different luting agents. J Prosthet Dent 94:227–233
Toman M, Toksavul S, Sarikanat M, Firidonoğlu K, Akin A (2009) The evaluation of displacement resistance of glass FRC posts to root dentine using a thin slice push-out test. Int Endod J 42:802–810
Elsayed ME, El-Mowafy O, Fenton A (2009) Retention of overdenture posts cemented with self-adhesive resin cements. Int J Prosthodont 22:287–289
Goracci C, Tavares AU, Fabianelli A, Monticelli F, Raffaelli O, Cardoso PC, Tay FR, Ferrari M (2004) The adhesion between fiber posts and root canal walls: comparison between microtensile and push-out bond strength measurements. Eur J Oral Sci 112:353–361
Soares CJ, Santana FR, Castro CG, Santos-Filho PCF, Soares PV, Qian F, Armstrong SR (2008) Finite element analysis and bond strength of a glass post to intraradicular dentin: comparison between microtensile and push-out tests. Dent Mater 24:1405–1411
Breschi L, Mazzoni A, Ruggeri A, Cadenaro M, Di Lenarda R, De Stefano DE (2008) Dental adhesion review: aging and stability of the bonded interface. Dent Mater 24:90–101
Gale MS, Darvell BW (1999) Thermal cycling procedures for laboratory testing of dental materials restorations. J Dent 27:89–99
Titley K, Caldwell R, Kulkarni G (2003) Factors that affect the shear bond strength of multiple component and single bottle adhesives to dentin. Am J Dent 16:120–124
Bitter K, Meyer-Lueckel H, Priehn K, Kanjuparambil JP, Neumann K, Kielbassa AM (2006) Effects of luting agent and thermocycling on bond strengths to root canal dentine. Int Endod J 39:809–818
Radovic I, Monticelli F, Goracci C, Vulicevic ZR, Ferrari M (2008) Self-adhesive resin cements: a literature review. J Adhes Dent 10:251–258
Saskalauskaite E, Tam LE, McComb D (2008) Flexural strength, elastic modulus, and pH profile of self-etch resin luting cements. J Prosthodont 17:262–268
Goracci C, Sadek FT, Fabianelli A, Tay FR, Ferrari M (2005) Evaluation of the adhesion of fiber posts to intraradicular dentin. Oper Dent 30:627–635
Cantoro A, Goracci C, Carvalho CA, Coniglio I, Ferrari M (2009) Bonding potential of self-adhesive luting agents used at different temperatures to lute composite onlays. J Dent 37:454–461
Mazzitelli C, Monticelli F, Osorio R, Casucci A, Toledano M, Ferrari M (2008) Effect of simulated pulpal pressure on self-adhesive cements bonding to dentin. Dent Mater 24:1156–1162
Alani AH, Toh CG (1997) Detection of microleakage around dental restorations: a review. Oper Dent 22:173–185
Amaral FLB, Colucci V, Palma-Dibb RG, Corona SAM (2007) Assessment of in vitro methods used to promote adhesive interface degradation: a critical review. J Esthet Restor Dent 19:340–354
International Organization for Standardization (1994) ISO TR11405. Dental materials—guidance on testing of adhesion to tooth structure. International Organization for Standardization, Geneva, pp 1–15
Monticelli F, Osorio R, Tay FR, Sadek FT, Ferrari M (2007) Resistance to thermo-mechanical stress of different coupling agents used as intermediate layer in resin-fiber post bonds. Am J Dent 20:416–420
Ozcan M, Valandro LF (2009) Fracture strength of endodontically-treated teeth restored with post and cores and composite cores only. Oper Dent 34:429–436
Piwowarczyk A, Bender R, Ottl P, Lauer HC (2007) Long-term bond between dual-polymerizing cementing agents and human hard dental tissue. Dent Mater 23:211–217
Reich SM, Wichmann M, Frankenberger R, Zajc D (2005) Effect of surface treatment on the shear bond strength of three resin cements to a machinable feldspatic ceramic. J Biomed Mater Res B Appl Biomater 74B:740–746
Kumbuloglu O, Lassilla LV, User A, Vallittu PK (2004) A study of the physical and chemical properties of four resin composite luting cements. Int J Prosthodont 17:357–363
Vrochari AD, Eliades G, Hellwig E, Wrbas KT (2009) Curing efficiency of four self-etching, self-adhesive resin cements. Dent Mater 25:1104–1108. doi:10.1016/j.dental.2009.02.015
Mazzoni A, Marchesi G, Cadenaro M, Mazzotti G, Di Lenarda R, Ferrari M, Breschi L (2009) Push-out stress for fibre posts luted using different adhesive approaches. Eur J Oral Sci 117:447–453
Monticelli F, Osorio R, Mazzitelli C, Ferrari M, Toledano M (2008) Limited decalcification/diffusion of self-adhesive cements to dentin. J Dent Res 87:974–979
Al-Assaf K, Chakmakchi M, Palaghias G, Karaniko-Kouma A, Eliades G (2007) Interfacial characteristics of adhesive luting resins and composites to dentine. Dent Mater 23:829–839
El Araby AM, Talic YT (2007) The effect of thermocycling on the adhesion of self-etching adhesives on dental enamel and dentin. J Contemp Dent Pract 8:17–24
Cury AH, Goracci C, de Lima Navarro MF, Carvalho RM, Sadek FT, Tay FR, Ferrari M (2006) Effect of hygroscopic expansion on the push-out resistance of glass ionomer-based cements used for the luting of glass fiber posts. J Endod 32:537–540
Monticelli F, Osorio R, Pisani-Proença J, Toledano M (2007) Resistance to degradation of resin–dentin bonds using a one-step HEMA free adhesive. J Dent 35:181–186
Bitter K, Noetzel J, Neumann K, Kielbassa AM (2007) Effect of silanization on bond strengths of fiber posts to various resin cements. Quintessence Int 38:121–128
Wrbas KT, Altenburger MJ, Schirrmeister JF, Bitter K, Kielbassa AM (2007) Effect of adhesive resin cements and post surface silanization on the bond strengths of adhesively inserted fiber posts. J Endod 33:840–843
Acknowledgments
This study was partially supported by grants CICYT/FEDER #MAT 2008-02347\MAT, JA P07-CTS-2568, and JA P08-CTS-3944.
Conflict of interest statement
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mazzitelli, C., Monticelli, F., Toledano, M. et al. Effect of thermal cycling on the bond strength of self-adhesive cements to fiber posts. Clin Oral Invest 16, 909–915 (2012). https://doi.org/10.1007/s00784-011-0576-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-011-0576-1