Abstract
Background
Although the Tampa Scale for Kinesiophobia (TSK) is useful for measuring fear of movement in patients with musculoskeletal pain, no psychometrically validated Japanese version is available. We evaluated the reliability and validity of the Japanese version of the TSK-J (original 17-item version and shorter 11-item version).
Methods
The data subset used in this psychometric testing was derived from a survey previously conducted to collect information on musculoskeletal pain due to motor vehicle accident. For reliability, internal consistency was assessed via Cronbach’s alpha coefficient. For concurrent validity, Pearson correlation coefficients of the TSK-J with the pain catastrophizing scale (PCS), euroqol 5 dimension (EQ-5D), and numerical rating scales (NRSs) for pain in the neck and back were calculated. For known-group validity, the relationship between variables (e.g., depression, somatic symptoms, treatment period) and the TSK-J score was examined.
Results
Data from 956 persons who had suffered from a motor vehicle accident were used in this analysis. For reliability, internal consistency was demonstrated, with Cronbach’s alpha statistics of 0.850 (TSK-J17) and 0.919 (TSK-J11). For concurrent validity, significantly strong correlations were demonstrated between the TSK-J versions and PCS total score and subscales (r = 0.602–0.680). For known-group validity, as hypothesized, significantly higher TSK-J scores were observed in persons with depressive mood, somatic symptoms, and longer treatment period.
Conclusions
The present analysis showed that the Japanese versions of the TSK-J17 and TSK-J11 were psychometrically reliable and valid for detecting fear of movement in the Japanese population suffering from neck to back pain due to a motor vehicle accident.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A high level of musculoskeletal pain may evoke the perception of fear of future pain. People may avoid movements or physical activities due to exaggerated fears that pain will result in additional functional restriction [1]. Avoidance of physical activities based on fear of movement (Kinesiophobia) leads to further avoidance [2]. Furthermore, avoidance of pain-inducing activities can result in a reduction of muscle strength and flexibility, which may partly contribute to a delay in recovery. This repeating cycle of fear of movement and avoidance behaviors may perpetuate the chronicity of the condition, resulting in disability. The contributing role of fear avoidance beliefs in the development of long-term disability has been widely recognized [3], and a low level of fear avoidance was reported to be the most useful item for predicting an earlier recovery in patients with acute low back pain [4]. Catastrophizing and somatic symptoms are additional major factors associated with chronicity in patients with whiplash injury [5].
The Tampa Scale of Kinesiophobia (TSK), a 17-item self-reported measure originally developed to discriminate between non-excessive fear and phobia among patients with chronic musculoskeletal pain (Miller RP, Kori SH, Todd DD. The Tampa Scale. Unpublished report 1991), is widely used to assess pain-related fear of movement or re-injury in patients with musculoskeletal complaints. The TSK employs a 4-point Likert scale, with scoring options ranging from 1 (strongly disagree) to 4 (strongly agree). A total score is calculated following inversion of the individual scores of items 4, 8, 12, and 16. The total score of the original 17-item version ranges between 17 and 68, with a higher score indicating a higher degree of Kinesiophobia. The TSK was developed in English, and has thus far been translated into various languages. The psychometric properties of both the original English version and other language versions have been assessed in several patient populations, including patients with chronic musculoskeletal pain [6], low back pain (LBP) [7, 8], whiplash injury pain [9], shoulder pain [10], temporomandibular disorder [11], sciatica [12], and fibromyalgia [13]. Based on the results of exploratory or confirmatory factor analysis in these studies, several factor-structured models with a different number of items (e.g., 17, 13, 12, or 11) have been proposed. Among these versions, an 11-item version that excluded the six psychometrically poor items (4, 8, 9, 12, 14, and 16) is the most widely-used short version. This 11-item version was reported to possess psychometric properties that are similar to the original TSK, and offers the advantage of brevity [14].
In previous work, Matsudaira et al. translated the original English version into Japanese and linguistically validated it, with the aim of introducing the TSK in Japan [15]. In this study, we evaluated the reliability and validity of the Japanese version of the TSK [both the 17-item original version (TSK-J17) and the 11-item shorter version (TSK-J11)] in people with spinal pain due to a motor vehicle accident, including neck pain as a whiplash-associated disorder and LBP.
Methods
Study population
To assess the psychometric properties of the TSK-J, we used a data subset derived from an online survey we had previously conducted in 2012 to collect information on musculoskeletal disorders related to a motor vehicle accident among the general Japanese population. Potential participants were recruited through an Internet panel provided by an Internet research company, including approximately 1.8 million individuals aged from 20 to 79 years as research volunteers. The company’s volunteers were consistent with the general Japanese population, and were stratified by sex and age. From these volunteers, 1,063,083 individuals were randomly selected, contacted by e-mail, and invited to complete an online questionnaire regarding a motor vehicle accident experienced in the past 12 months (first survey). Among these individuals, 227,853 were considered effective users, as the research company was unable to exclude non-users from invitations for technical reasons. The first survey was closed when the number of participants reached 127,956 [mean (SD) age 47.7 (10.8), male 63.6 %]. For this reason, the response rate was not relevant to this survey. Of these, 1,639 (1.3 %) individuals who responded that they had suffered from whiplash injury and/or LBP due to a motor vehicle accident in the past 12 months were screened and again invited to complete the online questionnaire (second survey), in order to investigate the impact of the motor vehicle accident on the physical and psychosocial aspects of their lives. Responses from 974 individuals (response rate 59.4 %) were obtained. After excluding data from 18 individuals due to inconsistent responses, data from 956 individuals was included into the analysis. Note that participants received points for online shopping as an incentive for participating in the survey. Double registration was prevented by checking e-mail address duplication and by blocking access to the questionnaire once a responder had completed the survey.
The TSK-J was translated and linguistically validated, according to the general cross-cultural adaptation process: (1) forward-translation (English to Japanese), (2) back-translation (Japanese to English), and 3) cognitive debriefing. Cognitive debriefing interviews of 6 Japanese adult respondents (three male, three female) were conducted to assess their comprehension of the questions and response scales.
This survey was approved by the medical/ethics review board of the Japan Labor Health and Welfare Organization. Personally identifiable information, including name, phone number, and permanent address, were not collected. Due to the nature of this study (an online survey), no written informed consent was obtained; however, receiving an answered questionnaire was considered evidence of consent.
Measures
Whiplash injury and LBP
Whiplash neck injury (cervical sprain and traumatic cervical syndrome) was defined as an injury in the neck, upper back, and shoulder area due to a motor vehicle accident. LBP was defined as pain localized between the costal margin and the inferior gluteal folds that persisted for more than a day at any time, based on the consensus approach for back pain definition proposed by Dionne et al. [16]. Pain associated only with menstrual periods, pregnancy, or during the course of a feverish illness was excluded. A diagram of affected areas by a whiplash injury and LBP was provided within the questionnaire.
The degree of the experienced pain associated with the whiplash injury or LBP was assessed using an 11-point numerical rating scale (NRS). Scores ranged from 0 (no pain) to 10 (worst pain imaginable), with a higher score indicating greater pain.
Catastrophizing
Pain catastrophizing, which is a maladaptive perception of pain, is an important predictor of future disability. Catastrophizing was assessed by the Japanese version of the pain catastrophizing scale (PCS) [17], a 13-item scale used to measure negative attitudes toward pain, involving rumination, helplessness, and magnification. The reliability and validity of the Japanese version were previously confirmed [17]. The total PCS score ranges from 0 (no catastrophizing) to 52 (severe catastrophizing).
Depressive mood
The presence of depressive mood was assessed using the mental health (MH) domain of the short-form health survey with 36 questions (SF-36) [18].
Somatic symptoms
Somatization was assessed using a subset of items from the brief symptom inventory (BSI). The Japanese version of the BSI-somatization scale was linguistically validated [19]. Seven somatic symptoms (faintness or dizziness, pains in the heart or chest, nausea or upset stomach, breathing difficulty, numbness or tingling in parts of the body, feeling weak in parts of the body, and hot or cold spells) were assessed on a 5-point scale (0, not at all; 1, a little bit; 2, moderate; 3, quite a bit; and 4, extreme).
General health status
The euroqol 5 dimension (EQ-5D) [20], which is a generic measure of health status that provides a simple descriptive profile and a single index value, was included in the questionnaire. The EQ-5D is a universally used tool to describe respondent’s perception of his/her own health status. The index score derived from conversion of all responses ranges from −0.11 to 1.00, with a score of 1 denoting “perfect health” and a score of 0 denoting “death”.
Data analysis
Demographic and clinical characteristics of the participants were summarized with descriptive statistics. Psychometric properties were assessed with respect to both versions: TSK-J17 and TSK-J11 (Table 1). With regard to internal consistency, the homogeneity of the items in the TSK-J versions was evaluated using Cronbach’s alpha statistics. A Cronbach’s alpha coefficient of 0.7 or higher is required to claim that the TSK-J versions are internally consistent [21]. Concurrent validity was evaluated using the Pearson correlation coefficient with the PCS, EQ-5D, and pain NRS. Note that the Pearson correlation coefficient was used because the TSK employed a 4-point (1–4) Likert scale, under the assumption of an equally spaced distance between response choices. According to the criterion for correlation strength in the psychometric validation proposed by Cohen, the correlation coefficient was judged as follows: 0.1, weak correlation; 0.3, medium correlation; and 0.5, strong correlation [22]. For the known-group validity, relationships between selected variables and the subscale scores were examined using the t test or one-way analysis of variance (ANOVA). If one-way ANOVA showed there was a significant difference between groups, all pairwise comparisons between groups were conducted. Multiplicity of statistical tests was adjusted by the Tukey–Kramer method. We hypothesized that persons who met the following attributes would obtain higher TSK-J scores: (1) individuals with depressive mood, (2) individuals with more somatic symptoms, and (3) individuals with longer treatment periods. If an individual obtained a score of 52 or lower on the SF-36 Mental Health scale, he/she was considered to exhibit a “depressive mood” (score range 0–100, with lower scores indicating more psychological distress) [23]. With regard to somatic symptoms, if an individual answered ‘moderate’, ‘quite a bit’, or ‘extremely’ on a selected item of the BSI-somatization subscale, he/she was considered to have the somatic symptom described in the item. The number of somatic symptoms was divided into three categories: no symptom, one symptom, and two or more symptoms. The treatment period was divided into three categories: 3 months or less, 3–6 months, and 6 months or longer.
All statistical tests were two-tailed, and the level of significance was set at 0.05. Statistical calculations were performed using SAS version 9.3 (SAS Institute, Cary, NC, USA).
Results
Characteristics of participants
Data from a total of 956 Japanese individuals who experienced a motor vehicle accident and an accompanying subsequent whiplash injury and/or LBP in the past 12 months were included in this analysis. The characteristics of the participants are shown in Table 2. The mean (SD) age was 45.4 (10.4) years; 71.0 % were male. The mean scores obtained on the TSK-J17 and the TSK-J11 were 41.1 (7.7) and 23.2 (6.6), respectively. Neither floor nor ceiling effect was observed. The mean total score for the PCS was 24.0 (11.8). The mean score for the MH domain of the SF-36 was 56.9 (19.7), and scores of 52 or lower were observed in 43.9 % (n = 420) of individuals. The mean EQ-5D score was 0.82 (0.18). The mean NRSs for whiplash injury and LBP were 6.1 (2.5) and 4.8 (2.9), respectively. Absence of work or housework due to whiplash injury or LBP was observed in 66.4 % (n = 635) of individuals. Of these, 36.9 % (n = 234) had to miss work more than once per week.
Reliability
Cronbach’s alpha coefficient was 0.850 for the TSK-J17 and 0.919 for the TSK-J11, indicating sufficient internal consistency.
Concurrent validity
The correlations of the TSK-J versions with the PCS, EQ-5D, and whiplash and LBP NRSs were calculated to examine concurrent validity. Both the TSK-J17 and TSK-J11 correlated strongly with the PCS total score, rumination, helplessness, and magnification subscales (r = 0.674, 0.616, 0.607, and 0.613 for the TSK-J17, respectively; r = 0.680, 0.635, 0.602, and 0.610 for the TSK-J11, respectively; P < 0.0001, for all) (Table 3).
Both the TSK-J17 and TSK-J11 negatively correlated moderately with the EQ-5D (r = −0.583 and −0.570, respectively; p < 0.0001). Both the TSK-J17 and TSK-J11 correlated moderately with the NRS for whiplash injury pain (r = 0.380 and 0.394, respectively; p < 0.0001) and NRS for LBP (r = 0.393 and 0.401, respectively; p < 0.0001).
Known-group validity
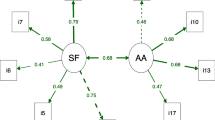
The relationship between variables that may affect the TSK-J score was examined. As hypothesized, significantly higher TSK-J scores were observed in persons with depressive mood, more somatic symptom(s), and longer treatment periods (Fig. 1). for depressive mood, the TSK-J17 score was 38.3 (6.7) for the less depressive group and 44.7 (6.5) for the more depressive group (p < 0.0001). The TSK-J11 score was 21.0 (6.0) for the less depressive group and 26.0 (6.2) for the more depressive group (p < 0.0001).
With respect to the number of somatic symptoms, persons who had more somatic symptoms had significantly higher TSK-J scores. The TSK-J17 scores in persons with no somatic symptom, one somatic symptom, and two or more somatic symptoms were 35.3 (6.1), 38.7 (6.0), and 43.7 (7.3), respectively, with significant differences between groups (p < 0.0001 for all). The corresponding TSK-J11 scores were 18.0 (5.8), 21.3 (5.2), and 25.4 (5.8), respectively, with significant differences between groups (p < 0.0001 for all).
Individuals with a longer treatment period had significantly higher TSK-J scores. The TSK-J17 scores in persons with treatment periods shorter than 3 months, 3–6 months, and 6 months or longer were 37.6, 41.7, and 46.0, respectively. The corresponding TSK-J11 scores were 20.3, 23.8, and 26.9, respectively, with significant differences between groups (p < 0.0001 for all).
Discussion
Matsudaira et al. proposed a linguistically-validated Japanese version of the TSK [15], the linguistic validity of which was established by ensuring the conceptual equivalence between the original and its translation by following a standardized method for developing a translated questionnaire [24]. In the present study, we assessed its psychometric properties with regard to 956 Japanese individuals who had whiplash injury pain or LBP due to a motor vehicle accident. Based on the results for internal consistency, concurrent validity, and known-group validity, the Japanese version of the TSK-J17 and TSK-J11 is considered to be reliable and valid as a measure for assessing fear of movement for (re)injury.
As an index to assess reliability, a highly sufficient internal consistency, with a Cronbach’s alpha statistic of 0.850 for the TSK-J17 and 0.919 for the TSK-J11, was demonstrated. Although a direct comparison is not appropriate due to the different characteristics of the adopted study populations, the Cronbach’s alpha coefficients obtained in this study are higher, relative to results obtained from the psychometric testing of other language versions of the TSK-17 or -11, including the Persian (TSK-17; α = 0.77–0.78 in acute chronic pain) [25], Chinese (TSK-17; α = 0.67 in chronic pain) [26], Brazilian/Portuguese (TSK-17; α = 0.82 in acute/subacute and chronic LBP) [27], German (TSK-11; α = 0.73 in LBP) [12], Swedish (TSK-11; α = 0.74–0.87 in chronic pain) [28], and Dutch (TSK-11; α = 0.68–0.80 in acute and chronic LBP) [8] versions. Reasons remain unknown about the higher Cronbach’s alpha coefficients obtained in this study; however, as the Cronbach’s alpha is an indicator of the internal consistency of items, the results may indicate that the Japanese version was translated more successfully compared to other language versions. As another result to be noted, the TSK-J11 had higher alpha statistic than the TSK-J17 in this study. In general, a superior Cronbach’s alpha statistic is obtained with inclusion of an increasing number of questions in the questionnaire. In this respect, the TSK-J11 presented not only the advantage of shorter length, but also that of higher internal consistency, which describes the extent to which all of the items in the test measure the same concept or construct, and hence is connected to the level of inter-relatedness of the items in the test.
Compared with previous studies [25, 29], both the TSK-J17 and TSK-J11 scores showed a stronger positive association with PCS, with a Pearson correlation coefficient above 0.6 for the PCS total and domain scores. There were also moderate associations with pain NRS in the affected area (0.380–0.401). The results were similar in TSK-J17 and TSK-J11. The obtained result of higher correlations with PCS, compared to NRSs may reflect that an individual’s psychological perception toward pain, rather than degree of pain itself, may contribute to the development of a fear avoidance belief. For known-group validity, as hypothesized, relevance was exhibited between the TSK-J score and the variables that might affect the scores, including the presence of depressive mood, presence of somatic symptom(s), and duration of the treatment period. It should be noted that these results do not necessarily imply a causal relationship between fear avoidance belief and the variables.
Fear avoidance behavior was reported to be an important risk factor for chronicity of pain and subsequent disability. In recent guidelines for the management of non-specific acute LBP, continuing normal daily activities is recommended and bed rest is discouraged [30]. To help reduce pain-related fear, it is important not to focus on imaging findings that could lead to the development of fear avoidance behavior in patients, but to instruct them that pain is a common condition and is self-manageable, along with gradual exposure to activities. For this reason, detecting patient fear avoidance beliefs and encouraging them to change their beliefs and behaviors is of vital importance in the management of musculoskeletal pain, to achieve a better outcome. The TSK-J enables clinicians to detect a patient’s fear avoidance beliefs, and helps to establish an effective management program to prevent chronic pain on an individual basis. In this study, the results of concurrent validity and known-group validity were similar for the TSK-J17 and TSK-J11; however, Cronbach’s alpha coefficient was higher for the TSK-J11. This result may partly support the sufficiency of using the TSK-J11, in place of the TSK-J17. Moreover, due to its fewer number of questions, the TSK-J11 is more convenient for use in clinical settings, enabling shorter response times and a lower psychological burden on the patients.
There are several study limitations that should be noted. Our results were obtained in individuals who suffered from a motor vehicle accident; accordingly, findings may not be generalizable to other populations. For instance, suffering from a motor vehicle accident may have had a strong psychological impact on the painful experience of these individuals, possibly enhancing the development of fear avoidance beliefs. In addition, the use of an Internet panel to recruit participants could have contributed to a selection bias, although the large sample size collected, throughout the nation is a major strength of this study. Our strategy of using the Internet may invite criticism regarding the representativeness of the sample; however, taking into account both cost and feasibility, we decided to recruit participants via the Internet. As another limitation, it should be noted that factor structure was not analyzed in this study. The original TSK-J17 and the TSK-J11 are frequently used versions; however, we are concerned that different factor solutions were proposed in different language versions and differently targeted populations, potentially making it difficult to compare international data derived from different translated versions. In addition, test–retest reliability over certain time intervals remains unknown. Responsiveness cannot be assessed in the present study due to the cross-sectional nature of the data. Accordingly, future studies are necessary to address these issues.
In conclusion, the present psychometric analyses demonstrated that the Japanese version of the TSK is psychometrically reliable and valid as a measure of fear for movement in a Japanese population who had whiplash injury pain and/or LBP due to a motor vehicle accident. As the TSK-J11, a shorter version of the TSK-J17, showed better internal reliability and similar construction and known-group validity compared to the 17-item version, it may be more useful in routine clinical care, given a limited time for assessment.
References
Leeuw M, Goossens ME, Linton SJ, Crombez G, Boersma K, Vlaeyen JW. The fear-avoidance model of musculoskeletal pain: current state of scientific evidence. J Behav Med. 2007;30(1):77–94.
Vowles KE, Gross RT. Work-related beliefs about injury and physical capability for work in individuals with chronic pain. Pain. 2003;101(3):291–8.
Fritz JM, George SZ, Delitto A. The role of fear-avoidance beliefs in acute low back pain: relationships with current and future disability and work status. Pain. 2001;94(1):7–15.
Chou R, Shekelle P. Will this patient develop persistent disabling low back pain? JAMA. 2010;303(13):1295–302.
Walton DM, Pretty J, MacDermid JC, Teasell RW. Risk factors for persistent problems following whiplash injury: results of a systematic review and meta-analysis. J Orthop Sports Phys Ther. 2009;39(5):334–50.
Koho P, Aho S, Kautiainen H, Pohjolainen T, Hurri H. Test-retest reliability and comparability of paper and computer questionnaires for the Finnish version of the Tampa Scale of Kinesiophobia. Physiotherapy. 2014;100(4):356–62.
Rusu AC, Kreddig N, Hallner D, Hülsebusch J, Hasenbring MI. Fear of movement/(Re)injury in low back pain: confirmatory validation of a German version of the Tampa Scale for Kinesiophobia. BMC Musculoskelet Disord. 2014;19(15):280.
Swinkels-Meewisse EJ, Swinkels RA, Verbeek AL, Vlaeyen JW, Oostendorp RA. Psychometric properties of the Tampa Scale for kinesiophobia and the fear-avoidance beliefs questionnaire in acute low back pain. Man Ther. 2003;8(1):29–36.
Bunketorp L, Carlsson J, Kowalski J, Stener-Victorin E. Evaluating the reliability of multi-item scales: a non-parametric approach to the ordered categorical structure of data collected with the Swedish version of the Tampa Scale for Kinesiophobia and the Self-Efficacy Scale. J Rehabil Med. 2005;37(5):330–4.
Mintken PE, Cleland JA, Whitman JM, George SZ. Psychometric properties of the fear-avoidance beliefs questionnaire and Tampa Scale of Kinesiophobia in patients with shoulder pain. Arch Phys Med Rehabil. 2010;91(7):1128–36.
Visscher CM, Ohrbach R, van Wijk AJ, Wilkosz M, Naeije M. The Tampa Scale for Kinesiophobia for temporomandibular disorders (TSK-TMD). Pain. 2010;150(3):492–500.
Haugen AJ, Grøvle L, Keller A, Grotle M. Cross-cultural adaptation and validation of the Norwegian version of the Tampa scale for kinesiophobia. Spine (Phila Pa 1976). 2008;33(17):E595–601.
Burwinkle T, Robinson JP, Turk DC. Fear of movement: factor structure of the tampa scale of kinesiophobia in patients with fibromyalgia syndrome. J Pain. 2005;6(6):384–91.
Woby SR, Roach NK, Urmston M, Watson PJ. Psychometric properties of the TSK-11: a shortened version of the Tampa Scale for Kinesiophobia. Pain. 2005;117(1–2):137–44.
Matsudaira K, Inuzuka K, Kikuchi N, Sakae C, Arisaka M, Isomura T. Development of a Japanese version of the Tampa Scale for Kinesiophobia (TSK-J): translation and linguistic validation. Seikei Geka (Orthop surg). 2013;48(1):13–9 (in Japanese).
Dionne CE, Dunn KM, Croft PR, Nachemson AL, Buchbinder R, Walker BF, Wyatt M, Cassidy JD, Rossignol M, Leboeuf-Yde C, Hartvigsen J, Leino-Arjas P, Latza U, Reis S, Gil Del Real MT, Kovacs FM, Oberg B, Cedraschi C, Bouter LM, Koes BW, Picavet HS, van Tulder MW, Burton K, Foster NE, Macfarlane GJ, Thomas E, Underwood M, Waddell G, Shekelle P, Volinn E, Von Korff M. A consensus approach toward the standardization of back pain definitions for use in prevalence studies. Spine (Phila Pa 1976). 2008;33(1):95–103.
Matsuoka H, Sakano Y. Assessment of cognitive aspect of pain: development, reliability, and validation of japanese version of pain catastrophizing scale. Shinshin igaku (Japanese Journal of Psychosomatic Medicine). 2007;47(2):95–102 (in Japanese).
Fukuhara S, Bito S, Green J, Hsiao A, Kurokawa K. Translation, adaptation, and validation of the SF-36 Health Survey for use in Japan. J Clin Epidemiol. 1998;51(11):1037–44.
Matsudaira K, Inuzuka K, Kikuchi N, Sakae C, Arisaka M, Isomura T. Development of the Japanese version of the brief symptom inventory-somatization scale: translation and linguistic validation. Seikei Geka (Orthopedic surgery). 2012;63(2):149–53 (in Japanese).
EuroQol Group. EuroQol-a new facility for the measurement of health-related quality of life. Health Policy. 1990;16(3):199–208.
Cronbach LJ. Coefficient alpha and the internal structure of tests. Psychometrika. 1951;16(3):297–334.
Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed. Hillsdale, NJ: Lawrence Erlbaum Associates; 1988.
Yamazaki S, Fukuhara S, Green J. Usefulness of five-item and three-item mental health Inventories to screen for depressive symptoms in the general population of Japan. Health Qual Life Outcomes. 2005;8(3):48.
Devellis RF. Scale development theory and applications. Newbury Park, CA: Sage Publications, Inc.; 1991.
Askary-Ashtiani A, Ebrahimi-Takamejani I, Torkaman G, Amiri M, Mousavi SJ. Reliability and validity of the Persian versions of the fear avoidance beliefs questionnaire and Tampa Scale of Kinesiophobia in patients with neck pain. Spine (Phila Pa 1976). 2014;39(18):E1095–102.
Wong WS, Kwok HY, Luk KD, Chow YF, Mak KH, Tam BK, Wong ET, Fielding R. Fear of movement/(re)injury in Chinese patients with chronic pain: factorial validity of the Chinese version of the Tampa Scale for Kinesiophobia. J Rehabil Med. 2010;42(7):620–9.
de Souza FS, Marinho Cda S, Siqueira FB, Maher CG, Costa LO. Psychometric testing confirms that the Brazilian-Portuguese adaptations, the original versions of the fear-avoidance beliefs questionnaire, and the Tampa Scale of Kinesiophobia have similar measurement properties. Spine (Phila Pa 1976). 2008;33(9):1028–33.
Larsson C, Hansson EE, Sundquist K, Jakobsson U. Psychometric properties of the Tampa Scale of Kinesiophobia (TSK-11) among older people with chronic pain. Physiother Theory Pract. 2014;30(6):421–8.
Hapidou EG, O’Brien MA, Pierrynowski MR, de Las Heras E, Patel M, Patla T. Fear and avoidance of movement in people with chronic pain: psychometric properties of the 11-item Tampa Scale for Kinesiophobia (TSK-11). Physiother Can. 2012 Summer;64(3):235–41.
Koes BW, van Tulder M, Lin CW, Macedo LG, McAuley J, Maher C. An updated overview of clinical guidelines for the management of non-specific low back pain in primary care. Eur Spine J. 2010;19(12):2075–94.
Acknowledgments
This study was supported by grants from JA Kyosai Research Institute and the Japan Labor Health and Welfare Organization.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
NK is a board member of Clinical Study Support, Inc. and received grants to his institution from JA Kyosai Research Institute for this study. KM has no conflict of interests. TS has received grants to his institution from JA Kyosai Research Institute for this study. HO has received grants/grants pending to his institution from Pfizer Inc.
About this article
Cite this article
Kikuchi, N., Matsudaira, K., Sawada, T. et al. Psychometric properties of the Japanese version of the Tampa Scale for Kinesiophobia (TSK-J) in patients with whiplash neck injury pain and/or low back pain. J Orthop Sci 20, 985–992 (2015). https://doi.org/10.1007/s00776-015-0751-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-015-0751-3