Abstract
Background
Although patellar instability can be treated with several surgical procedures, the appropriate surgical treatment for patellar instability with patella alta has not yet been investigated. The objective of this study is to find out whether three-dimensional transfer of the tibial tuberosity elicits good knee functionality with improved patella alta and prevents further patellar dislocation.
Methods
Twelve knees (10 patients) underwent surgery for patellar instability with patella alta from 2007 to 2011. The surgery performed was a three-dimensional transfer for the anteromedial distalization of the tibial tuberosity. Predisposing anatomical factors for patellar instability were evaluated preoperatively; femorotibial angle (FTA), patella alta (IS ratio), trochlear dysplasia (sulcus angle) and tilting angle (lateral tilt). The function of the knee was assessed before and after surgery by Lysholm and Kujala score.
Results
Before surgery, the IS ratio was 1.34 ± 0.13, lateral tilt was 22.4° ± 6.5°, and the sulcus angle was 151.7° ± 8.3°, indicating patella alta, laterality, and trochlear dysplasia. After surgery, the IS ratio and lateral tilt significantly improved to 0.95 ± 0.13, and 10.6° ± 3.4°, respectively. FTA and sulcus angle were not altered. Lysholm and Kujala score improved from 63.8 to 94.7 and 67.0 to 94.1 points, respectively. Most patients displayed good outcomes except for one patient who suffered re-dislocation by hitting their knee on the floor, 2.5 years after surgery.
Conclusion
Three-dimensional tibial tuberosity transfer was shown to correct the patella position and result in a good clinical outcome. This method is introduced as an alternative surgery for patellar instability with patella alta.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patellar dislocation is frequently affected by acute and chronic injury. Acute dislocation is mainly caused by traumatic high-energy injuries, whereas chronic dislocation is caused by recurrent patellar dislocation, which contributes to multifactorial problems such as patellar shape [1], patella alta [2, 3], patellar tilt [4], trochlear dysplasia [5], and an excessive tibial tubercle–trochlear groove (TT–TG) distance [6, 7].
Several surgical procedures and outcomes for patellar instability have already been reported. Since Hauser [8] reported the surgical treatment of patellar dislocation by transferring the tibial tuberosity, Elmslie-Trillat [9], and Fulkerson [10] procedures were reported with some modification of distal realignment. Most of these procedures were reported to have a good outcome [11, 12], however, some later progressed to osteoarthritic change at the patellofemoral (PF) joint [13], especially after the distalization of tibial tuberosity by Hauser’s procedure [14]. Recently, medial patellofemoral ligament (MPFL) reconstruction has been more commonly performed because of the anatomical reconstruction with low surgical invasion [15–17]. Although most of the MPFL reconstructions reported good outcomes [16], there were still some cases that retained patellar instability [18], and it is hard to resolve the problems associated with patella alta using MPFL reconstruction [19].
Patella alta is characterized by proximal location, as indicated by an Insall–Salvati [20] patella height ratio (IS ratio) over 1.2. Patella alta is associated with maximal PF contact force [21], adverse cartilage adaptations, PF pain, and instability [22]. As a result, it frequently induces knee osteoarthritis (OA) [23, 24]. It is recommended that the surgical procedure is selected on the basis of cause and effect, though appropriate surgical treatment for patellar instability with patella alta has still to be investigated.
In this study, we focus on patellar instability with patella alta and introduce a three-dimensional transfer, which is an anteromedial distalization of the tibial tuberosity, and assess the outcome of this procedure.
Materials and methods
This study was performed according to a protocol approved by the Institutional Review Board of Osaka Medical College (No. 1125). All subjects provided their informed consent to participate in this study. A retrospective study was conducted for 12 knees (10 patients; 8 women, 2 men), which underwent surgical treatment for patellar instability with patella alta from 2007 to 2011. The average age was 20.2 years (range 16–43 years) and the mean follow-up was 3.2 years (range 1.1–5.5 years). The indication of this surgery was that patients who had experienced patellar dislocation several times and continued the complaint of patellar instability with patella alta with a IS ratio over 1.2.
Preoperative assessment
Predisposing anatomical factors for recurrent patellar dislocation were evaluated preoperatively, including valgus knee alignment via the femorotibial angle (FTA), patella alta (IS ratio) [20], and trochlear dysplasia (sulcus angle) with Merchant view [25] by X-ray. Lateral patellar displacement (tilting angle) and TT–TG distance were evaluated by CT images. PF joint space was measured at the center of medial and lateral facet and was used to calculate PT index [26]. The relationship between the measurements of anatomical features and postoperative patellar instability, which was defined by the patellar redislocation or residual apprehension after surgery was assessed. The clinical outcome was evaluated by Lysholm and Kujala [27] score before and at the end of the follow-up.
Surgical procedure
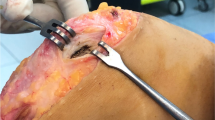
The surgery performed was a three-dimensional, anteromedial and distal transfer of the tibial tuberosity. An 8-cm longitudinal skin incision was made from the insertion of the patella to the lower end of the tibial tuberosity (Fig. 1a, b). Kirschner wires were inserted 20°–30° from the anteromedial to the posterolateral of tibia as a guide for osteotomy at the tibial tuberosity (Fig. 1c). The transferred tibial tuberosity, was about 45 mm long and about 15 mm wide. The bone fragment was detached from the distal tibial tuberosity to be transferred 10–15 mm by anteromedial distalization. The size and shape of the detached bone depended on the distance the tibial tuberosity was to be transferred. To correct the patellar instability with patella alta, the distance of distal transfer was calculated for correcting the IS ratio to 1.0, and the distance of medial transfer was decided to normalize the TT–TG distance to 10–15 mm based on the CT measurements. Usually, the distance of anterior transfer was decided after medial and distal transfers had been performed (Fig. 1d, e). The bone fragment from the distal end of the tibial tuberosity was placed at the side of the replaced tuberosity to stabilize the transferred position. Finally, the tibial tuberosity was fixed with two cannulated cancellous screws 5.0 mm in diameter (Fig. 1f). Lateral release and medial plication for proximal realignment was added (Fig. 1g). The transfer of the tibial tuberosity was assessed with CT after surgery. Medialization was measured with a coronal view, distalization used a sagittal view, and ventralization used an axial view (Fig. 2). All cases were performed arthroscopy to determine the cartilage degeneration when the screws at tibia tuberosity were removed almost 1 year after initial surgery.
Surgical procedure for three-dimensional transfer of tibial tuberosity. a, b An 8-cm longitudinal skin incision from the tibial tuberosity to the distal edge of the anterior tibia is performed. c–e Kirschner wires were inserted to 20°–30° as a guide for osteotomy at the tibial tuberosity, from anterior medial to posterior lateral. f Tibial tuberosity (45 × 15 mm) transferred via anteromedial distalization. Bone fragment from the distal end of transferred tibial tuberosity was placed to stabilize the position. The tibial tuberosity was fixed with two cannulated cancellous screws 5.0 mm in diameter. g Lateral release and medial plication for proximal realignment
Rehabilitation
Weight-bearing was permitted with a knee extension brace for the first 3 weeks after surgery. Exercising the knee’s range of motion started as follows; aggressive quadriceps and hamstrings muscle exercises were added after 8 weeks or later, while running and full sports activities were permitted after 3 and 6 months, respectively.
Statistical analysis
Statistically significant differences were determined with a paired T test before and after surgery. The results are given as mean ± SD. P values <0.05 were considered significant.
Results
The average transfer of tibial tuberosity in this surgical procedure was 5.6 ± 1.9 (3.6–9.0) mm anterior, 8.7 ± 0.5 (8.1–9.1) mm medial and 10.6 ± 3.4 (6.7–13.1) mm distal, respectively (Fig. 2). The average FTA was 176.7 (175.0–179.0) degrees before surgery and 176.4 (173.0–179.0) degrees after surgery (P = 0.73). Before surgery, the average IS ratio was 1.34 ± 0.13 (1.21–1.65) and the tilting angle was 22.4 ± 6.5 (15.0–36.5) degrees, which showed patella alta and lateral subluxation. The preoperative sulcus angle was 151.7 ± 8.3 (141.5–168.0) degrees, with trochlear groove dysplasia and the postoperative sulcus angle was 150.1 ± 8.5 (140.5–167.5) degrees, which was not significantly improved (P = 0.74). After surgery, the IS ratio, which was the distance to the patella ligament attachment before surgery, improved to 0.95 ± 0.13 (0.79–1.16, P < 0.01) and the tilting angle to 10.6 ± 3.4 (6.0–17.5) degrees (P = 0.001). TT–TG was significantly improved from 17.2 ± 1.2 (15.2–18.8) to 10.1 ± 1.8 (8.8–13.9) mm after surgery (P < 0.01). No patient noticed patellar apprehension after surgery, and the Lysholm and Kujala scores changed from 63.8 (36–80) to 94.7 (75–100), and 67.0 (43–78) to 94.1 (77–100), respectively (P < 0.01) (Table 1). Re-dislocation happened in one patient who hit his knee on the floor while dancing, 2.5 years after surgery, although no patellar instability was detected from initial surgery to this injury. It was treated with MPFL reconstruction. Subsequently, no additional dislocation or patellar instability was observed.
PF joint space was decreased in the medial joint space (P = 0.014), suggesting the improvement of patellar instability, whereas no significant difference was detected in the lateral, indicating not to progress the PF pressure after surgery (Fig. 3). The PT index improved from 2.4 to 1.4. Moreover, no arthritic change at the PF joint was observed by arthroscopy when the screws were removed almost 1 year after initial surgery.
Discussion
Patella alta is recognized one of the risk factors for recurrent patellar dislocation and many surgical procedures have been reported to improve patellar instability.
In 1992, MPFL reconstruction was first reported for the treatment of recurrent dislocation of the patella [17], and good, long-term outcomes resulted from anatomical reconstruction [15, 16]. Recently, MPFL reconstruction has become common for patellar instability treatment, although the outcome is not always good due to the uncertain tension of reconstructed MPFL in cases of patella alta [19, 28]. Additionally, MPFL repair for recurrent patellar dislocation has a significantly higher rate of failure for patella alta patients [19] and a distal tibial tubercle transfer is recommended for decreasing the IS ratio when patella alta is found [29].
The distal realignment technique has been reported from early times. Since Hauser [8] reported the surgical treatment of patellar dislocation by transferring the tibial tuberosity to a distal realignment in 1938, Elmslie-Trillat [9], Fulkerson [10], and other surgeons reported that each new technique achieved a good outcome for preventing patellar dislocation. Although the Hauser procedure, which was the medial and distal transfer of the tibial tuberosity, had the advantage of correcting patella height, it was reported to have a high incidence of PF OA [14]. Later, excellent outcomes from the Elmslie-Trillat procedure [30, 31], which was a pure medial transfer of the tibial tuberosity, was reported as a useful procedure without incidence of OA [11]. However, PF arthritic change had developed during long-term follow-up [13]. The Fulkerson procedure was also reported as having excellent results by anteromedialization of the tibial tuberosity for recurrent patellar dislocation. However, Tsuda et al. [32] pointed out that patella alta was the predictor of postoperative patellar instability after the Fulkerson procedure, and they concluded that the Fulkerson procedure should not be indicated for recurrent patellar dislocation with severe patella alta. These reports suggest that distal transfer of the tibial tuberosity might be critical in cases of patella alta to correct the PF alignment.
The main purpose of this three-dimensional transfer of the tibial tuberosity is to correct the patella at anatomical position. This procedure resulted in appropriate radiographic change, not only correcting the patella height (IS ratio), but also the TT–TG distance, resulting in a good clinical score. Furthermore, the medial joint space of the PF was significantly decreased and was similar to the lateral joint space. This indicates patellar instability was improved after this procedure. Additionally, the PT index, which was <1.6, got within normal range after surgery. Although distalization in this surgery involves the possibility of more pressure applied on the PF joint, as in Hauser’s procedure, this surgery did not induce PF arthritic change, according to arthroscopic findings 1 year after initial surgery. This was because this surgery was performed only for patellar instability with patella alta patients and induced anterior transfer that Hauser’s procedure did not. When the IS ratio is <1.2, distalization is not performed and the Elmslie-Trillat procedure is usually indicated instead in our hospital. Re-dislocation happened in one patient who had no patellar instability before his knee hit the floor. This re-dislocation might not have happened if the patella had not suffered such a traumatic high-energy injury.
This study involves some limitations. One is the short follow-up period of 3.1 years. However, most re-dislocation occurred within the first 2 years after surgery [33], and we considered that the period in this study was enough to assess the clinical outcome. The other is the lack of a control group because there is no gold standard surgery for patellar instability. In this series, we evaluated the outcome using several radiographical assessments and clinical scores, which are generally accepted in the orthopedic scene. However, further research and follow-up would be indispensable over time.
In conclusion, even though no gold standard for the treatment of patellar instability with patella alta is recognized, this proximal and three-dimensional tibial transferring procedure might be useful for patellar instability with patella alta.
References
Panni AS, Cerciello S, Maffulli N, Di Cesare M, Servien E, Neyret P. Patellar shape can be a predisposing factor in patellar instability. Knee Surg Sports Traumatol Arthrosc. 2011;19:663–70.
Ward SR, Terk MR, Powers CM. Patella alta: association with patellofemoral alignment and changes in contact area during weight-bearing. J Bone Joint Surg Am. 2007;89:1749–55.
Juliusson R, Markhede G. A modified Hauser procedure for recurrent dislocation of the patella. A long-term follow-up study with special reference to osteoarthritis. Arch Orthop Trauma Surg. 1984;103:42–6.
Laurin CA, Lévesque HP, Dussault R, Labelle H, Peides JP. The abnormal lateral patellofemoral angle: a diagnostic roentgenographic sign of recurrent patellar subluxation. J Bone Joint Surg Am. 1978;60:55–60.
Balcarek P, Jung K, Ammon J, Walde TA, Frosch S, Schüttrumpf JP, Stürmer KM, Frosch KH. Anatomy of lateral patellar instability: trochlear dysplasia and tibial tubercle–trochlear groove distance is more pronounced in women who dislocate the patella. Am J Sports Med. 2010;38:2320–7.
Servien E, Verdonk PC, Neyret P. Tibial tuberosity transfer for episodic patellar dislocation. Sports Med Arthrosc. 2007;15:61–7.
Monk AP, Doll HA, Gibbons CLMH, Ostlere S, Beard DJ, Gill HS, Murray DW. The patho-anatomy of patellofemoral subluxation. J Bone Joint Surg Br. 2011;93:1341–7.
Hauser EDW. Total tendon transplant for slipping patella: a new operation for recurrent dislocation of the patella. 1938. Clin Orthop Relat Res. 2006;452:7–16.
Cox JS. Evaluation of the Roux-Elmslie-Trillat procedure for knee extensor realignment. Am J Sports Med. 1982;10:303–10.
Fulkerson JP. Anteromedialization of the tibial tuberosity for patellofemoral malalignment. Clin Orthop Relat Res. 1983;177:176–81.
Endres S, Wilke A. A 10 year follow-up study after Roux-Elmslie-Trillat treatment for cases of patellar instability. BMC Musculoskelet Disord. 2011;12:48.
Akgün U, Nuran R, Karahan M. Modified Fulkerson osteotomy in recurrent patellofemoral dislocations. Acta Orthop Traumatol Turc. 2010;44:27–35.
Nakagawa K, Wada Y, Minamide M, Tsuchiya A, Moriya H. Deterioration of long-term clinical results after the Elmslie-Trillat procedure for dislocation of the patella. J Bone Joint Surg Br. 2002;84:861–4.
Hampson WG, Hill P. Late results of transfer of the tibial tubercle for recurrent dislocation of the patella. J Bone Joint Surg Br. 1975;57:209–13.
Nomura E. Classification of lesions of the medial patello-femoral ligament in patellar dislocation. Int Orthop. 1999;23:260–3.
Nomura E, Inoue M, Kobayashi S. Long-term follow-up and knee osteoarthritis change after medial patellofemoral ligament reconstruction for recurrent patellar dislocation. Am J Sports Med. 2007;35:1851–8.
Ellera Gomes JL. Medial patellofemoral ligament reconstruction for recurrent dislocation of the patella: a preliminary report. YJARS. 1992;8:335–40.
Wagner D, Pfalzer F, Hingelbaum S, Huth J, Mauch F, Bauer G. The influence of risk factors on clinical outcomes following anatomical medial patellofemoral ligament (MPFL) reconstruction using the gracilis tendon. Knee Surg Sports Traumatol Arthrosc. (Published Online First: 27 April 2012).
Arendt EA, Moeller A, Agel J. Clinical outcomes of medial patellofemoral ligament repair in recurrent (chronic) lateral patella dislocations. Knee Surg Sports Traumatol Arthrosc. 2011;19:1909–14.
Insall J, Salvati E. Patella position in the normal knee joint. Radiology. 1971;101:101–4.
Luyckx T, Didden K, Vandenneucker H, Labey L, Innocenti B, Bellemans J. Is there a biomechanical explanation for anterior knee pain in patients with patella alta? Influence of patellar height on patellofemoral contact force, contact area and contact pressure. J Bone Joint Surg Br. 2009;91:344–50.
Redziniak DE, Diduch DR, Mihalko WM, Fulkerson JP, Novicoff WM, Sheibani-Rad S, Saleh KJ. Patellar instability. J Bone Joint Surg Am. 2009;91:2264–75.
Ahlbäck S, Mattsson S. Patella alta and gonarthrosis. Acta Radiol Diagn (Stockh). 1978;19:578–84.
Stefanik JJ, Zhu Y, Zumwalt AC, Gross KD, Clancy M, Lynch JA, Frey Law LA, Lewis CE, Roemer FW, Powers CM, Guermazi A, Felson DT. Association between patella alta and the prevalence and worsening of structural features of patellofemoral joint osteoarthritis: the multicenter osteoarthritis study. Arthritis Care Res (Hoboken). 2010;62:1258–65.
Merchant AC, Mercer RL, Jacobsen RH, Cool CR. Roentgenographic analysis of patellofemoral congruence. J Bone Joint Surg Am. 1974;56:1391–6.
Laurin CA, Dussault R, Lévesque HP. The tangential X-ray investigation of the patellofemoral joint: X-ray technique, diagnostic criteria and their interpretation. Clin Orthop Relat Res. 1979;144:16–26.
Kujala UM, Jaakkola LH, Koskinen SK, Taimela S, Hurme M, Nelimarkka O. Scoring of patellofemoral disorders. YJARS. 1993;9:159–63.
Bollier M, Fulkerson J, Cosgarea A, Tanaka M. Technical failure of medial patellofemoral ligament reconstruction. YJARS. 2011;27:1153–9.
Arendt EA. MPFL reconstruction for PF instability. The soft (tissue) approach. Orthop Traumatol Surg Res. 2009;95:97–100.
Barber FA, McGarry JE. Elmslie–Trillat procedure for the treatment of recurrent patellar instability. Arthrosc J Arthrosc Relat Surg. 2008;24:77–81.
Rillmann P, Dutly A, Kieser C, Berbig R. Modified Elmslie-Trillat procedure for instability of the patella. Knee Surg Sports Traumatol Arthrosc. 1998;6:31–5.
Tsuda E, Ishibashi Y, Yamamoto Y, Maeda S. Incidence and radiologic predictor of postoperative patellar instability after Fulkerson procedure of the tibial tuberosity for recurrent patellar dislocation. Knee Surg Sports Traumatol Arthrosc. 2012;20:2058–66.
Nietosvaara Y, Paukku R, Palmu S, Donell ST. Acute patellar dislocation in children and adolescents. Surgical technique. J Bone Joint Surg Am. 2009;91(Suppl 2 Pt 1):139–45.
Conflict of interest
The authors have no conflicts of interest in the authorship and publication of this contribution.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Otsuki, S., Nakajima, M., Oda, S. et al. Three-dimensional transfer of the tibial tuberosity for patellar instability with patella alta. J Orthop Sci 18, 437–442 (2013). https://doi.org/10.1007/s00776-013-0364-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00776-013-0364-7