Abstract
Growth hormone (GH) deficiency causes decreased bone mineral density and osteoporosis, predisposing to fractures. We investigated the mechanism of action of GH on bone modeling and remodeling in hypophysectomized (HX) female rats. Thirty female Sprague–Dawley rats at age 2 months were divided into three groups with 10 rats each: control (CON) group, HX group, and HX + GH (3 mg/kg daily SC) group, for a 4-week study. Hypophysectomy resulted in cessation of bone growth and decrease in cancellous bone mass. Periosteal bone formation decreased and bone turnover rate of endocortical and trabecular surfaces increased as compared to the CON group. GH administration for 4 weeks restored weight gain and bone growth and mitigated decrease in bone density after hypophysectomy. However, trabecular bone mass in the proximal tibial metaphysis remained lower in group HX + GH than in group CON. Dynamic histomorphometric analysis showed that bone modeling of periosteal bone formation and growth plate elongation was significantly higher in group HX + GH than in group HX. New bone formed beneath the growth plate was predominately woven bone in group CON and group HX + GH. Bone remodeling and modeling–remodeling mixed modes in the endocortical and PTM sites were enhanced by GH administration; both bone formation and resorption activities were significantly higher than in group HX. In conclusion, GH administration to HX rats reactivated modeling activities in modeling predominant sites and increased new bone formation. GH administration also increases remodeling activities in remodeling predominant sites, giving limited net gain in the bone mass.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Childhood-onset growth hormone (GH) deficiency (GHD), as well as adult-onset GHD, exhibits significant reductions in cortical thickness, cortical cross-sectional area, and overall cortical content associated with the smaller bone size [1, 2]. Cancellous bone volume (BV), mineralizing surface (MS), and trabecular thickness are also decreased in patients with GHD when compared with sex- and age-matched healthy controls [1–3]. Histomorphometric analysis of bone in HX rats and humans with GHD showed higher eroded bone surface (BS), with decreased bone formation rate (BFR) and decreased mineralization [4–6], thus resulting in reduced bone mineral density (BMD) [7] and increased risk of fractures [8].
Numerous studies have assessed the effect of GH on bone density and body composition in children and adults with GHD. Both GH and insulin-like growth factor (IGF)-1 have well-recognized roles in bone elongation and skeletal maturation in vitro and in vivo [1, 9, 10]. GH replacement in animals and in the clinical setting suggests a short-term increase in bone turnover and long-term increase in BMD [11–14]. However, a direct role of GH for mineral accrual and bone density is still not fully understood.
Bone modeling is active in childhood and adolescent stages, occurring mainly in the primary spongiosa and periosteal surface of the cortex during growth stages by independent action of osteoblasts and osteoclasts, whereas bone remodeling predominates when bone is reaching maturity stages. Bone remodeling takes place by the teamed action of osteoclasts and osteoblasts, mainly in the secondary spongiosa and endocortical surfaces, and the balance of formation and resorption determines the preservation or loss of the bone [15, 16]. GH plays an important role in the whole process of both modeling and remodeling activities to maintain bone mineral density (BMD) [17–19]. However, the mechanism of action of GH on bone modeling and remodeling at the levels of the cancellous and cortical bone has not been studied in detail thus far.
The aim of this study was to evaluate the mechanism of action of GH on bone modeling and remodeling at different sites in the cortical and trabecular bone.
Understanding this mechanism may be essential for the application of GH in combined therapies with antiresorptive agents to fully reestablish the bone mineral content (BMC) and BMD of conditions such as childhood-onset and adult-onset GHD where GH treatment alone is not able to restore bone health.
Materials and methods
Treatment of animals
Twenty female Sprague–Dawley rats, hypophysectomized at 8 weeks of age by the vender (Hilltop Lab Animals, Scottdale, PA, USA), were shipped to the Animal Facility of the Winthrop-University Hospital 3 days after the surgery, with 10 additional rats that served as the age-matched controls (CON). One week after the rats were received and adapted to the environment, the HX rats were randomized by stratified weight method into two groups of 10 rats each: HX and HX + GH. Recombinant human GH, supplied by Genentech (Vacaville, CA, USA), was administered SC daily at a dosage of 3 mg/kg (0.666 mg/0.2 ml), 5 days a week (Monday–Friday). The dose of GH was determined in accordance with previously published data [20, 21]. Throughout the experiment, all HX rats, with and without GH, were supplemented daily with hydrocortisone in the form of sodium succinate (100 μg/100 g BW) and thyroxine at 2 μg/100 g, SC. They were also given 3% sucrose water ad libitum to maintain their blood glucose levels whereas all pituitary-intact CON rats were given normal tap water and a standard pelleted chow diet ad libitum. The body weight of the rats was monitored weekly; the total experimental period was 4 weeks. Whether HX was successfully performed was confirmed at the end of the study by observing no gain in body weight and a significant reduction in longitudinal growth rate (LGR/day) of the proximal tibial metaphysis (PTM). The study was carried out at Winthrop-University Hospital, and the animals were maintained according to the National Institutes of Health (NIH) Guidelines for Care and Use of Laboratory Animals. All the animal protocols were approved by the Laboratory Animal Care Committee of Winthrop-University Hospital.
Preparation of specimens
All the rats were labeled with 10 mg/kg calcein (Sigma Chemical, St. Louis, MO, USA) injected intramuscularly 10 days and 3 days before they were killed. The femurs were used for the measurement of bone area, BMC, and BMD, as described below. The tibiae were used for measuring bone length and static and dynamic bone histomorphometric analyses. The undecalcified PTM and tibial diaphysis with the fibular junction were processed and embedded in methyl methacrylate (EM Science, Gibbstown, NJ, USA). Pairs of serial cross sections of the tibial diaphysis just proximal to the tibia–fibula junction, and pairs of serial frontal sections of the PTM, were sectioned at 6-μm thickness using a microtome (Leica RM2155; Leica, Nussloch, Germany). Villanueva stain was used for static and dynamic histomorphometric and polarized light analyses. The toluidine blue-stained sections were used to view cement lines, osteoblasts, and wall thickness, and Goldner’s trichrome-stained sections were used to measure tissue area, bone area, osteoid area, osteoclast number (OcN), and BS.
Bone histomorphometric analysis of the tibia
A digitizing morphometric system was used to measure bone histomorphometric parameters, as described previously [21, 22]. The measured parameters for cancellous bone included total tissue volume (TV), BV, BS, single- and double-labeled surfaces (sLS and dLS, respectively), interlabel width, osteoid area, and OcN. These data were used to calculate percent cancellous bone volume (BV/TV), MS/BS [(sLS/2 + dLS)/BS], mineral apposition rate (MAR), BFR/BS, osteoid/BV, and OcN/BS, in accordance with the standard nomenclature proposed by Parfitt et al. [23]. In the present study, the region of cancellous bone measured was 0–1.0 mm distal to the lower margin of the growth plate as zone 1 and 1–4.0 mm distal to the lower margin of the growth plate as zone 2 in the PTM. In addition to the measurement of these parameters, interlabel width beneath the growth plate was used to calculate longitudinal growth rate (LGR/day). The measured parameters for cortical bone were total tissue area (Tt Ar), marrow area (Ma Ar), periosteal and endocortical BS, sLS, dLS, eroded surface (ES), and interlabel width. These data were used to calculate cortical area (Ct Ar), Ct Ar (%), and periosteal and endocortical MS/BS [(sLS/2 + dLS)/BS], MAR, BFR/BS, and ES/BS (%).
Active bone-forming, calcein-labeled osteons on trabecular and endocortical surfaces were studied using polarized light for collagen orientation and transmitted light for cement line stains according to the method described previously [24]. Only those trabecular structural units containing either calcein label or osteoblast surfaces as evidence for active bone formation at the time of sacrifice were analyzed. Modeling and remodeling analyses were performed on the trabecular and endocortical areas containing either calcein label or osteoblast surfaces as evidence for active bone formation at the time of sacrifice were analyzed (Fig. 1). The osteons were classified according to the presence of smooth (modeling) or scalloped (remodeling) cement lines as described previously [24, 25]. A remodeling site was defined by the presence of a scalloped cement line with interrupted collagen fibers indicating that formation followed previous bone resorption or osteoclastic activity [24]. A bone formation site was also scored as remodeling when fluorochrome labeling started from an arrest line that was part of an incompletely filled remodeling unit. A modeling site was defined as the sites with smooth cement lines, showing evidence that no osteoclastic bone resorption preceded bone formation. The modeling unit was further assessed under polarized light to ensure that collagen fibers in the whole unit followed the same orientation as those of the adjacent bone tissue. Bone-forming units with the presence of short scalloped and long smooth cement lines were classified as prolonged remodeling sites or mixed remodeling–modeling (Mixed-M-R) hemiosteons. The percentage of each type of the hemiosteons from the total numbers of formation osteons was calculated. Those osteons with disoriented collagen fibers as examined under polarized light were considered as woven bone whereas the osteons with oriented fibers were measured as lamellar bone.
Modeling and remodeling-dependent bone gain in proximal tibial metaphysis (a1, a2, a3) and endocortical surface (b1, b2). Micrographs of metaphysical trabecular (a) and endocortical (b) bone with Villanueva osteochrome bone staining under epifluorescent light (a1, b1), Goldner trichrome staining (a2), and under polarized light (a3, b2). White arrows, calcein-labeled surfaces; black arrows, osteoblast cells; blue-black arrows, cement line with scalloped surface; red arrows, cement line with smooth surface. Note osteoblast and osteoprogenitor cells lying on the surface of modeling- and remodeling-active bone sites
Femoral bone area, BMC, and BMD
Bone area, BMC, and BMD of the whole right femur were determined by dual-energy X-ray absorptiometry (DXA) using a Hologic QDR-4500 Plus (Hologic, Bedford, MA, USA). The instrument was adapted for an ultraresolution mode, with a line spacing of 0.0254 cm, resolution of 0.0127 cm, and collimation of 0.9 cm diameter. BMC and bone area were measured, and BMD of this area was calculated by dividing BMC by bone area. The coefficient of variation of these measurements at our laboratory was less than 1.0% [22].
Statistical analysis
All the data were expressed as means and standard deviation (SD). Multiple comparisons of data among the groups were performed by analysis of variance (ANOVA) with the Turkey–Kramer test. All statistical analyses were performed using the Prism-5.0 program on a Hewlett Packard computer. A significance level of P < 0.05 was used for all the comparisons.
Results
Body weight, tibial length, femoral density, and static histomorphometry of the tibial shaft and proximal tibial metaphysis
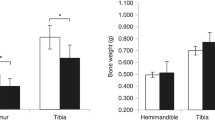
Table 1 shows that although the CON young animals were growing during the experimental period, HX resulted in a cessation of weight gain, bone lengthening, and bone size in area, and a decrease in femoral BMC and BMD. GH administration resulted in a significant increase in body weight, tibial bone length, and femoral bone area to levels not significantly different from those of the age-matched CON group. Although BMC and BMD of the GH-treated group were increased as compared to the HX group, the levels were still lower than that of the CON group. The total area of the tibial shaft cross section of the GH-treated group was not different from that of the CON rats, but the Ma Ar was lower; thus, the Ct Ar in percentage was significantly higher than that of the CON and HX groups.
In the metaphysis of the proximal tibia, we measured 0–1 mm and 1–4 mm beneath the growth plate as zone 1 and zone 2, respectively, in comparison (see Table 1). The BV/TV (%) of the HX was significantly lower than that of the CON in both zone 1 and zone 2, respectively. Column A of Fig. 2 illustrates the distribution of trabecular bone in the PTM of the CON, HX, and HX + GH rats, respectively.
Proximal tibial metaphysis and micrographs of the metaphysis beneath the growth plate from control group (CON) (a1, b1, c1), hypophysectomized (HX) (a2, b2, c2), and HX + GH (growth hormone) (a3, b3, c3) animals. a1, a2, and a3 were stained with Krutsay’s Von Kossa method; micrographs of the metaphysis beneath the growth plate b1, b2, and b3 were stained with Villanueva Osteochrome bone stain for fluorescent labeling; c1, c2, and c3 were examined under visible light with a polaroid filter. White arrows, growth plate; green arrows, calcein-labeled surfaces; black arrows, lamellar bones; blue-black arrows, woven bones; PTM, proximal tibial metaphysis. Note that the trabecular bone density was significantly lower in the HX than that of the CON group; bone was predominantly polarized lamellar bone. GH administration resulted in increased growth plate width and newly woven bone formation
Under fluorescent and polaroid light, in examination of the same field (columns B and C of Fig. 2) it is possible to measure bone mineralized surface and distinguish the woven and lamellar bone formed. Examining the percent of lamellar and woven bones of the HX group, 80.8% (5.92%/7.33%) was lamellar bone, and only 19.2% was woven bone in zone 1 (see Table 1), whereas in the CON group, only 31.6% (13.8%/43.61%) of the bone was lamellar bone, but 68.4% of the bone was woven bone in zone 1. Although GH treatment resulted in a significant increase in the BV/TV of zone 1 as compared to the HX group, the increase was primarily woven bone (16.56%/23.56% = 70.26%). Nevertheless, the total BV/TV of zone 1 in the HX + GH group was lower than that of the CON group. The bone in zone 2 of the three experimental groups was primarily lamellar bone, and the BV/TV of both HX groups with or without GH treatment (9.74% and 5.74%, respectively) was lower than that of the intact animals (29.47%). GH treatment resulted in a trend to increase, but not a statistically significant increase, in the bone mass in zone 2 as compared to the HX group.
Dynamic histomorphometry of trabecular bone in zones 1 and 2 of the proximal tibia metaphysis
As compared to the CON group, HX resulted in a cessation of the longitudinal growth rate (LGR) and GH administration resulted in a reactivation of the LGR (Table 2). This finding is also illustrated by the cancellous bone distribution and double labeling beneath the growth plate in columns A and B of Fig. 2. As expected, HX resulted in a decrease in the BFR in both zone 1 and zone 2, and GH administration resulted in an increase of the BFR in both zone areas. The percentage of lamellar bone under modeling and remodeling was examined under polarized light, cement line, and calcein labeling of the adjacent sections (a1, a2, and a3 of Fig. 1 and column C of Fig. 2). Table 2 shows that there was 78.5% ± 6.38% of the lamellar bone under modeling, and 9.35% ± 2.45% and 12.2% ± 3.07% under remodeling and Mixed-M-R, respectively, in zone 1 of the CON animals. Hypophysectomy resulted in a decrease in the modeling activity (8.42% ± 1.87% vs. 78.5% ± 6.38%), and activity was relatively high in both remodeling (61.4% ± 4.24% vs. 9.35% ± 2.45%) and Mixed-M-R (30.2% ± 3.55% vs. 12.2% ± 3.07%) percentages as compared to the CON group. GH administration to the HX rats resulted in a significant increase in the percent of modeling (83.7% ± 7.93% vs. 8.42% ± 1.87%) and a decrease in the remodeling (13.7% ± 2.11% vs. 61.4% ± 4.24%) and Mixed-M-R (2.61% ± 1.84% vs. 30.2% ± 3.55%) percentages in comparison with the HX group. Lamellar bone was predominant in percentage in zone 2 area among the three experimental groups under remodeling; however, the percentage of bone under remodeling was significantly higher in the HX group (91.4% ± 7.38%) than that of the CON group (63.2% ± 3.98%). Conversely, percent of bone under modeling was significantly lower in the HX than in the CON groups. GH administration to the HX rats resulted in an increase in modeling (8.3% ± 4.68% vs. 1.425 ± 1.74%), thereby decreasing remodeling percentages (76.8% ± 5.87% vs. 91.4% ± 7.38%) as compared to the HX group. The percentage of stained osteoid bone in zone 2 was decreased to undetectable in the HX group, and the osteoclast cell surface (%) was significantly higher than that of the CON group; GH administration to the HX rats resulted in an increase in both the osteoid and osteoclast cell-surface percentage in the zone 2 area.
Dynamic histomorphometry of the tibial shaft at periosteal and endocortical surfaces of the cross section proximal to the tibia–fibula junction
Table 3 shows the dynamic histomorphometry of the periosteal and endocortical BS. Hypophysectomy resulted in a significant decrease of the periosteal bone mineral surface (16.2% ± 9.1% vs. 75.8% ± 9.7%), MAR (1.02% ± 0.19% vs. 2.78% ± 0.28%), and BFR (17.2% ± 11.2% vs. 210% ± 39.3%), and an increase in the endocortical bone mineral surface (62.6% ± 16.9% vs. 38.3% ± 12.1%), MAR (1.81% ± 0.25% vs. 1.45% ± 0.21%), BFR (113.9% ± 32.3% vs. 56.7% ± 23.1%), and the eroded surface (12.1% ± 3.28% vs. 6.5% ± 2.39%) as compared to the CON group. As expected, GH administration resulted in a significant increase in the periosteal bone formation parameters (288% ± 64.5% vs. 17.2% ± 11.2%) as compared to the HX group. The endocortical BFR and erosion surface (%) of the HX + GH group remained higher than that of the CON and was not different from the respective HX group. Under polaroid and cement line examination, most of the endocortical surfaces were under remodeling among the three experimental groups; however, hypophysectomy resulted in a cessation of the modeling and a decrease in the mixed modeling and remodeling (%). GH administration reactivated the modeling activity of the HX rats, and the increased level was higher than that of the CON group.
Discussion
The main purpose of this study was to investigate the effect of GH administration on bone modeling and remodeling on different sites of the long bones under growth hormone deficiency using hypophysectomized rats as an animal model. Our study confirms the previous findings that GH administration to HX rats activated both bone formation and resorption [4, 5]. As a result of activation of bone formation in modeling sites, GH administration increases bone elongation, new bone formation, and cortical expansion. However, in remodeling sites the activation of both formation and resorption after GH administration results in increased bone turnover rat, and therefore the net gain in bone mass in those sites is limited.
It is well known that GHD subjects have lower BMC and BMD, as seen in HX rats [20, 21]. The decrease in BV seen after HX is believed to be caused by suppressed new bone formation in addition to decreased trabecular number and thickness, with or without an increase in the bone resorption. Because intestinal calcium absorption has been shown to be decreased and serum calcium is lower after HX as compared to that of intact control animals [26], calcium in bone acts as a reservoir to be released to maintain constant serum calcium levels. The finding of relatively rapid decrease in trabecular BV and trabecular thickness in the proximal tibia after HX as compared to the decrease in cortical bone mass in the tibial shaft supports the fact that bone response to calcium demand is more rapid in cancellous than in cortical bone. It has been reported that when individuals go into negative calcium balance, 40–60% of trabecular calcium is lost, with much less lost in the form of cortical bone calcium, and calcium supplementation alone or in combination with vitamin D cannot suppress trabecular bone loss sufficiently as compared to the loss in cortical bone [27]. Nevertheless, the change in microarchitecture of trabecular and cortical bone results in increased bone vulnerability to fractures.
It is well understood that GH treatment of HX animals is able to increase serum levels of 1,25-dihydroxyvitamin D, parathyroid hormone (PTH) sensitivity, and calcium absorption efficiency [28]. Thereby, the anabolic effect of GH on calcium metabolism is established. However, GH treatment causes a different response to bone growth, modeling, and remodeling in trabecular as compared to cortical bone, but the mechanism of action has not been well described. Several studies in animals and humans postulate that long-term GH treatment to GHD subjects results in a greater effect on cortical than on trabecular bone, supporting the suggestion that there is a differential effect of GH on bone modeling and remodeling activities at different cortical and trabecular bone sites [20, 29–31]. Typically, bone growth and modeling improve new bone formation on the chondrocytes beneath the growth plate and primary spongiosa of the cancellous bone, whereas cortical bone modeling increases periosteal surface expansion without prior resorption. Bone remodeling either conserves or removes the bone in the cancellous bone and in the endocortical bone in contact with the marrow cavity. When the subjects are in growth stages, most of the trabecular bone in the primary spongiosa is longitudinally oriented and it contains newly synthesized woven bone, whereas in secondary spongiosa the majority of trabecular bone has been remodeled, as evidenced by the fact that the main content was lamellar bone. Because there is no clear separation to distinguish primary and secondary spongiosa areas in PTM, in the current study we arbitrarily separated PTM into zones 1 and 2 to illustrate the effect of HX and GH treatment on bone modeling and remodeling and the effect on primary and secondary bone turnover. Presumably, the majority of the primary spongiosa was covered in 0–1 mm beneath the growth plate as zone 1 and the majority of secondary spongiosa was covered in 1–4 mm as zone 2.
Our data for zones 1 and 2 show that the bone mass of the HX rat was lower than that of the age-matched controls and that the bone was predominantly lamellar bone over woven bone, indicating that GHD during the growth stage not only causes cessation of new bone formation from the growth plate elongation, but also the remaining bones were under remodeling with low bone formation relative to a high resorption activity, thus causing a net decrease in the bone mass. On the other hand, the new bone beneath the growth plate after GH treatment visualized in the current study as woven bone and the lamellar bone with adjacent smooth cement line under polarized light indicates that GH treatment restores the modeling activity of the trabecular bone and causes a net gain in the bone mass in this modeling site.
Conversely, the results of zone 2 showed only a moderate gain in the bone mass in association with a relatively high bone formation and resorption activities after GH treatment in comparison to the HX group without the treatment. This finding demonstrates that even though GH administration increases bone modeling activity, it also activates the secondary bone remodeling activity rate. This result provides evidence and strongly supports the recent findings of that a longer period of treatment is required to exhibit the beneficial effect of GH on improving bone mass and bone density in GHD subjects [11–13].
As expected, GHD results in cessation of cortical growth in length and circumferential expansion, increases the marrow cavity, and decreases BMC and BMD [20, 32], and GH treatment to the HX rats is able to restore the growth and periosteal expansion [29, 30]. The current finding that GH administration increases bone modeling activity in both periosteal and endocortical sites and increased cortical thickness with moderate decrease in the marrow cavity demonstrates that GH increases bone modeling activity on the remodeling-predominant site of endocortical surface. This action is particularly important on improving bone strength because the diameter and the thickness of the cortex have a dramatic impact on the biomechanical integrity of the bone [15]. This difference in modeling and remodeling effects of GH on cortical bone as compared to trabecular bone could explain why GH has a greater effect on cortical than on trabecular bone. The current data of modeling and remodeling suggest that the decrease in BMD in GHD is not only the result of decrease in modeling-induced new bone formation but also a result of bone loss from increased imbalance in remodeling activity. On the other hand, the increase in bone mass after GH administration is the result of increase in bone modeling gain in size and mass in periosteal and endocortical sites of cortical bone.
Hypophysectomy results in deficiency not only of growth hormone but also of other pituitary hormones that have a direct effect on gonadal hormones influencing bone metabolism. It has been demonstrated that the preventive effect of estrogen on cancellous bone loss in ovariectomized rats is diminished after HX [33, 34]. When GH and/or estrogen are administered to the HX rats with or without ovariectomy, the beneficial effects are additive but minimal [33, 35]. Furthermore, the combined intervention of GH and testosterone on aged orchioectomized rats also exhibited an additive but not statistically significant effect on preventing osteopenia [36]. Therefore, it is believed that the effect of sex steroid hormones on bone metabolism is pituitary dependent.
Although GH increases cancellous bone modeling and growth plate new bone formation, it also increases trabecular bone remodeling-induced bone turnover and ameliorates the net gain in mass. To improve this disadvantage, a combination therapy of GH with an antiresorptive agent or with another anabolic agent, such as PTH, has been recommended. Biermasz et al. [37], Mosekilde et al. [38], Iwamoto et al. [39], and Guevarra et al. [40] proved that combined treatment of recombinant human growth hormone (rhGH) and alendronate, rhGH and vitamin K, or rhGH and PTH, respectively, causes positive effects at the level of cortical but also trabecular bone as compared to GH treatment alone. Those findings suggest that GH causes a gain in bone mass mainly at the cortical site of the bones, whereas antiresorptive agents or another anabolic agent are needed to fully reestablish the bone mass at the level of the trabecular bone [38, 40, 41]. Understanding the mechanism of GH in modeling and remodeling in the bone will facilitate future clinical applications of GH in combination with other agents to fully reestablish the pathological bone loss seen in conditions such as childhood- and adult-onset GHD and to improve BMD by rebuilding more bone, therefore causing a positive impact in bone health.
In conclusion, GH administration to HX rats activates bone modeling activities and results in new bone formation; however, the activation of remodeling results in increased bone turnover rate and loss in bone mass. Therefore, the combination of bone modeling and remodeling resulted in limited net gain in bone mass. Understanding the mechanism and the sites of GH in modeling and remodeling in the bone will facilitate future clinical applications of GH with other combined therapies in improving bone metabolism.
Change history
27 July 2019
The following corrections are found in the original publication of the article and corrected as below:
27 July 2019
The following corrections are found in the original publication of the article and corrected as below:
10 November 2021
An Editorial Expression of Concern to this paper has been published: https://doi.org/10.1007/s00774-021-01285-4
References
Ohlsson C, Bengtsson B, Isaksson OGP, Andreassen TT, Slootweg MC (1998) Growth hormone and bone. Endocr Rev 19:55–79
Kosowicz J, Ei Ali Z, Ziomnicka K, Sowinski J (2007) Abnormalities in bone mineral during distribution and bone scintigraphy in patients with childhood onset hypopituitarism. J Clin Densitom 10:332–339
Kann P, Piepkorn B, Schehler B, Andreas J, Lotz J, Prellwitz W, Beyer J (1998) Effect of long-term treatment with GH on bone metabolism, bone mineral density and bone elasticity in GH-deficient adults. Clin Endocrinol 48:561–568
Yeh JK, Chen MM, Aloia JF (1995) Skeletal alterations in hypophysectomized rats. I: A histomorphometric study on tibial cancellous bone. Anat Rec 241:505–512
Chen MM, Yeh JK, Aloia JF (1995) Skeletal alterations in hypophysectomized rats. II: A histomorphometric study on tibial cortical bone. Anat Rec 241:513–518
Bravenboer N, Holzmann P, de Boer H, Blok GJ, Lips P (1996) Histomorphometric analysis of bone mass and bone metabolism in growth hormone deficient adult men. Bone (NY) 18:551–557
Sartorio A, Ortolani S, Conti A, Cherubini R, Galbiati E, Faglia G (1996) Effects of recombinant growth hormone (GH) treatment on bone mineral density and body composition in adults with childhood onset growth hormone deficiency. J Endocrinol Invest 19:524–529
Murray R, Adams JE, Shalet SM (2005) A densitometric and morphometric analysis of the skeleton in adults with varying degrees of growth hormone deficiency. J Clin Endocrinol Metab 91:432–438
Sjogren K, Bohlooly YM, Olsson B, Coschigano K, Tornell J, Mohan S (2000) Disproportional skeletal growth and markedly decreased bone mineral content in growth hormone receptor −/−mice. Biochem Biophys Res Commun 267:603–608
Kim BT, Mosekilde L, Duan Y, Zhang XZ, Tornvig L, Thomsen JS, Seeman E (2003) The structural and hormonal basis of sex differences in peak appendicular bone strength in rats. J Bone Miner Res 18:150–155
Lanes R, Gunczler P, Wesinger JR (1999) Decreased trabecular bone mineral density in children with idiopathic short stature: normalization of bone density and increased bone turnover after one year of GH treatment. Pediatr Res 135:177–181
Lanes R, Gunczler P, Esaa S, Weisinger JR (2002) The effect of short and long term growth hormone treatment on BMD and bone mineral metabolism of pre-pubertal children with ISS: a 3 year study. Clin Endocrinol 57:725–730
Conway GS, Szarras-Czapnik M, Racz K, Keller A, Chanson P, Tauber M, Zacharin M (2009) Treatment for 24 months with recombinant human GH has beneficial effect on bone mineral density in young adults with childhood-onset GH deficiency. Eur J Endocrinol 160:899–907
Monson JP, Drake WM, Carroll PV, Weaver JU, Rodriguez-Arnao J, Savage MO (2002) Influence of growth hormone on accretion of bone mass. Horm Res 58:52–56
Aloia JF (1998) Osteoporosis: the complete guide to prevention and treatment. Odyssey Press, Dover, NH
Nelson DA, Norris SA, Gilsanz V (2006) Childhood and adolescence. In: Primer on the metabolic bone diseases and disorders of mineral metabolism, 6th edn. American Society for Bone and Mineral Research (ASBMR), Washington, DC, pp 55–61
Bex M, Bouillon R (2003) Growth hormone and bone health. Horm Res 60(suppl 13):80–86
Slootweg MC (1993) Growth hormone and bone. Horm Metab Res 25:335–343
Eriksen EF, Kassem M, Langdahl B (1996) Growth hormone, insulin-like growth factors and bone remodeling. Eur J Clin Invest 26:525–534
Chen MM, Yeh JK, Aloia JF (1997) Histologic evidence: Growth hormone completely prevents reduction in cortical bone gain and partially prevents cancellous osteopenia in the tibia of hypophysectomized rats. Anat Rec 249:163–172
Chaudhry AA, Castro-Magana M, Aloia JF, Yeh JK (2009) Differential effects of growth hormone and alpha calcidol on trabecular and cortical bones in hypophysectomized rats. Pediatr Res 65:403–408
Iwamoto J, Matsumoto H, Takeda T, Sato Y, Liu X, Yeh JK (2008) Effects of vitamin K2 and residronate on bone formation and resorption, osteocyte lacunar system, and porosity in the cortical bone of glucocorticoid-treated rats. Calcif Tissue Int 83:121–128
Parfitt AM, DRezner MK, Glorieux FH, Kanis JA, Malluche H, Meunier PJ, Ott SM, Recker RR (1987) Bone histomorphometry: standardization of nomenclature, symbols and units. J Bone Miner Res 2:595–610
Erben R (1996) Trabecular and endocortical bone surfaces in the rat: modeling or remodeling? Anat Rec 246:39–46
Frost HM (2004) The Utah paradigm of skeletal physiology. International Society of Musculoskeletal and Neuronal Interactions, Athens, Greece, pp 224–241
Yeh JK, Aloia JF (1984) Effect of hypophysectomy and 1, 25 dihydroxy-vitamin D on duodenal calcium absorption. Endocrinology 114:1711–1717
Bronner F (1994) Calcium and osteoporosis. Am J Clin Nutr 60:831–836
Fleet JC, Bruns ME, Hock JM, Wood RJ (1994) Growth hormone and parathyroid hormone stimulate intestinal calcium absorption in aged female rats. Endocrinology 134:1755–1760
Andreassen T, Oxlundi H (2001) The effects of growth hormone on cortical and cancellous bone. J Musculoskel Neuron Interact 2:49–58
Ortoft G, Andreassen TT, Oxlund H (1999) Growth hormone increases cortical and cancellous bone mass in young growing rats with glucocorticoid induced osteopenia. J Bone Miner Res 14:710–721
Bravenboer N, Holzmann PJ, ter Maaten JC, Stuurman LM, Roos JC, Lips P (2005) Effect of long-term growth hormone treatment on bone mass and bone metabolism in growth hormone-deficient men. J Bone Miner Res 2005(20):1778–1784
Yeh JK, Evans JF, Chen MM, Aloia JF (1999) Effect of hypophysectomy on the proliferation and differentiation of rat bone marrow stromal cells. Am J Physiol Endocrinol Metabol 276:E34–E42
Kiddler LS, Schmidt IU, Evans GL, Turner RT (1997) Effects of growth hormone and low dose estrogen on bone growth and turnover in long bones of hypophysectomized rats. Calcif Tissue Int 61:327–335
Yeh JK, Chen MM, Aloia JF (1997) Effects of 17 beta-estradiol administration on cortical and cancellous bone of ovariectomized rats with and without hypophysectomy. Bone (NY) 20:413–420
Yeh JK, Chen MM, Aloia JF (1997) Effects of estrogen and growth hormone on skeleton in the ovariectomized rat with hypophysectomy. Am J Physiol 273:734–742
Prakasam G, Yeh JK, Chen MM, Castro-Magana M, Liang CT, Aloia JF (1999) Effects of growth hormone and testosterone on cortical bone formation and bone density in aged orchiectomized rats. Bone (NY) 24:491–497
Biermasz NR, Hamdy NA, Janssen YJ, Roelfsema F (2001) Additional beneficial effects of alendronate in growth hormone (GH) deficient adults with osteoporosis receiving long term recombinant human GH replacement therapy: a randomized controlled trial. J Clin Endocrinol Metab 86:3079–3085
Mosekilde L, Tornvig L, Thomsen JS, Orhii PB, Banu MJ, Kalu DN (2000) Parathyroid hormone and growth hormone have additive or synergetic effect when used as intervention treatment in ovariectomized rats with established osteopenia. Bone (NY) 26:643–651
Iwamoto J, Takeda T, Sato Y, Yeh JK (2007) Effect of Vitamin K2 and growth hormone on the long bones in hypophysectomized young rats: a bone histomorphometry study. J Bone Miner Metab 25:46–53
Guevarra SM, Yeh JK, Castro-Magana M, Aloia JF (2010) A synergistic effect of parathyroid hormone on trabecular and cortical bone formation in the hypophysectomized rats. Horm Res Pediatr 73:248–257
Wang L, Orhii PB, Kalu DN (2001) Effects of separate and combined therapy with growth hormone and parathyroid hormone on lumbar vertebral bone in aged ovariectomized osteopenic rats. Bone (NY) 28:202–207
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Iglesias, L., Yeh, J.K., Castro-Magana, M. et al. Effects of growth hormone on bone modeling and remodeling in hypophysectomized young female rats: a bone histomorphometric study. J Bone Miner Metab 29, 159–167 (2011). https://doi.org/10.1007/s00774-010-0210-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-010-0210-3