Abstract
The modulation of N-methyl-D-aspartate receptor (NMDAR) and l-arginine/nitric oxide (NO) pathway is a therapeutic strategy for treating depression and neurologic disorders that involves excitotoxicity. Literature data have reported that creatine exhibits antidepressant and neuroprotective effects, but the implication of NMDAR and l-arginine/nitric oxide (NO) pathway in these effects is not established. This study evaluated the influence of pharmacological agents that modulate NMDAR/l-arginine-NO pathway in the anti-immobility effect of creatine in the tail suspension test (TST) in mice. The NOx levels and cellular viability in hippocampal and cerebrocortical slices of creatine-treated mice were also evaluated. The anti-immobility effect of creatine (10 mg/kg, po) in the TST was abolished by NMDA (0.1 pmol/mouse, icv), d-serine (30 µg/mouse, icv, glycine-site NMDAR agonist), arcaine (1 mg/kg, ip, polyamine site NMDAR antagonist), l-arginine (750 mg/kg, ip, NO precursor), SNAP (25 μg/mouse, icv, NO donor), L-NAME (175 mg/kg, ip, non-selective NOS inhibitor) or 7-nitroindazole (50 mg/kg, ip, neuronal NOS inhibitor), but not by DNQX (2.5 µg/mouse, icv, AMPA receptor antagonist). The combined administration of sub-effective doses of creatine (0.01 mg/kg, po) and NMDAR antagonists MK-801 (0.001 mg/kg, po) or ketamine (0.1 mg/kg, ip) reduced immobility time in the TST. Creatine (10 mg/kg, po) increased cellular viability in hippocampal and cerebrocortical slices and enhanced hippocampal and cerebrocortical NO x levels, an effect potentiated by l-arginine or SNAP and abolished by 7-nitroindazole or L-NAME. In conclusion, the anti-immobility effect of creatine in the TST involves NMDAR inhibition and enhancement of NO levels accompanied by an increase in neural viability.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glutamate has been implicated in the pathogenesis of depressive disorders (Sanacora et al. 2008; Skolnick 1999). A post-mortem study found increased levels of glutamate in the frontal cortex of patients with major depression (Hashimoto et al. 2007). Evidence indicates that the N-methyl-D-aspartate receptor (NMDAR) complex is particularly involved in the pathophysiology of depression, since preclinical and clinical studies have indicated that compounds that reduce transmission at NMDAR exhibit antidepressant properties (Berman et al. 2000; Cunha et al. 2008; Zomkowski et al. 2010, 2012). Changes in NMDAR have been also demonstrated in the frontal cortex of suicide victims (Nowak et al. 1995). Noteworthy, the NMDAR antagonist ketamine produces a rapid and sustained antidepressant effect in animal models and in patients that suffer from treatment-resistant major depression (Berman et al. 2000; Li et al. 2011), in consonance with the proposition that NMDAR antagonists may be novel strategies for the treatment of depression (Skolnick 1999). The faster antidepressant-like effect of ketamine has been attributed to NMDA and AMPA receptor modulation (Duman et al. 2012; Zhou et al. 2014).
In response to activation of glutamate receptors (NMDA, AMPA or Kainate) or voltage-gated Ca2+ channels, nitric oxide (NO) is synthesized from l-arginine by nitric oxide synthase (NOS) (Contestabile 2000; Esplugues 2002; Yamamoto et al. 2004). Several studies indicate that l-arginine/NO pathway is also involved in the pathophysiology of depression. Plasma nitrate concentrations and expression of neuronal nitric oxide synthase in the hippocampus were reported to be significantly higher in depressed patients, suggesting that NO production is increased in depression (Oliveira et al. 2008; Suzuki et al. 2001). In line with this, several studies have shown that NOS inhibitors exert antidepressant-like effects in animal models (da Silva et al. 2000; Harkin et al. 1999, 2003; Heiberg et al. 2002; Joca and Guimarães 2006; Volke et al. 2003). However, an antidepressant-like action was also observed with the administration of the substrate for NOS, l-arginine (da Silva et al. 2000; Inan et al. 2004; Spiacci et al. 2008), suggesting that NO may have a dual role in the modulation of depression.
A growing number of reports have provided evidence for the importance of the creatine kinase/phosphocreatine system in the pathophysiology of depression: (1) brain phosphocreatine, detected by phosphorus-31 magnetic resonance spectroscopy, was shown to be decreased in severely depressed patients (Kato et al. 1992); (2) an inverse correlation between Hamilton Depression Rating Scale scores and white matter creatine levels was shown (Dager et al. 2004); (3) single prolonged stress and forced swimming stress decreased creatine concentrations in the rat prefrontal cortex (Herring et al. 2008; Kim et al. 2010; Knox et al. 2010); (4) learned helplessness, a well-validated animal model of depression, decreased the expression of hippocampal creatine transporter (Lugenbiel et al. 2010); (5) the acute administration of the fast-acting antidepressant ketamine increased creatine kinase activity in rats (Assis et al. 2009); (6) clinical trials show that creatine augmentation in antidepressant treatment-resistant patients may be a promising therapeutic approach that exhibits more rapid and efficacious responses (Kondo et al. 2011; Lyoo et al. 2012); (7) creatine administration in mice produced an anti-immobility effect in the tail suspension test (TST) and forced swimming test (FST), two widely used tests for screening antidepressants (Allen et al. 2010, Cunha et al. 2012, 2013a, b).
The mechanisms underlying the neuroprotective and antidepressant actions may be different, although antidepressant agents commonly exhibit neuroprotective properties. The link between these two effects may be the inhibition of NMDAR and the modulation of NO production.
Taking into account the involvement of NMDAR and l-arginine-NO pathway in the pathogenesis of depression and the importance of these molecular targets for the efficacy of antidepressants (Dhir and Kulkarni 2007; Krass et al. 2011; Zomkowski et al. 2010, 2012), this study investigated whether the anti-immobility effect of creatine in the TST is mediated by a modulation of NMDAR and NO pathway and also assessed the ability of creatine to enhance cellular viability and to counteract glutamate excitotoxicity.
Materials and methods
Animals
Female Swiss mice (30–40 g) and female Wistar rats (210–230 g) were housed in groups of fourteen (mice) or five (rats) per plastic cage under controlled conditions of light (from 07:00 to 19:00 h) and temperature (21 ± 1 °C). Animals were allowed free access to standard laboratory food and tap water, and to adapt to the laboratory environment for at least 1-week before the behavioral studies. For behavioral analysis, each experimental group consisted of 8–11 animals. For the biochemical measurements, each experimental group consisted of 4–6 samples. Animals were randomly distributed into the experimental groups. All manipulations were carried out between 14:00 and 17:00 h. All procedures in this study were performed in accordance with the National Institute of Health Guide for the Care and Use of Laboratory Animals and approved by the Ethics Committee of the Institution (CEUA/UFSC). All efforts were made to minimize animals suffering and to reduce the number of animals used in the experiments.
Drugs
The following drugs were used: 6,7-dinitroquinoxaline-2,3-dione (DNQX, 2.5 µg/mouse, icv), 7-nitroindazole (50 mg/kg, ip), arcaine (1 mg/kg, ip), creatine monohydrate (0.01 or 10 mg/kg, po), d-serine (30 µg/mouse, icv), fluoxetine (10 mg/kg, po), ketamine (0.1–1 mg/kg, ip), l-arginine (750 mg/kg, ip), NG-nitro-l-arginine methyl ester (L-NAME, 175 mg/kg, ip), MK-801 (0.001 mg/kg, po), N-methyl-D-aspartate (NMDA, 0.1 pmol/mouse, icv), S-nitroso-N-acetyl-penicillamine (SNAP, 25 µg/mouse, icv), (Sigma Chemical Co, St Louis, MO, USA). Table 1 summarizes the drugs used in the experimental protocols.
All drugs were dissolved in saline, except 7-nitroindazole that was dissolved in saline with 1 % Tween 80. Drugs were administered by intraperitoneal (ip) route in a constant volume of 10 ml/kg body weight, except NMDA and SNAP which were administered by intracerebroventricular (icv) route and creatine and MK-801 that was administered per os (po) by gavage.
Icv administration
The icv injections were performed by a ‘‘free hand’’ method performed and validated in our research group (Moretti et al. 2012; Kaster et al. 2012). Icv administration was performed using a microsyringe (25 μl, Hamilton) connected to a 26-gauge stainless-steel needle that was inserted perpendicularly 2 mm deep through the skull according to the procedure described by Laursen and Belknap (1986). Briefly, mice were lightly anesthetized with ether (i.e. just that necessary for loss of the postural reflex) and then gently restrained by hand for icv injections. The sterilization of the injection site was carried out using gauze embedded in 70 % ethanol. The needle was inserted unilaterally 1 mm into the midline point equidistant from each eye, at an equal distance between the eyes and the ears and perpendicular to the plane of the skull. A volume of 5 μl of sterile saline (vehicle) or drugs (dissolved in sterile saline) was injected directly into the left lateral ventricle, at the following coordinates from bregma taken from the atlas of Franklin and Paxinos (1997): anterioposterior (AP) = −0.1 mm; mediolateral (ML) = 1 mm; and dorsoventral (DV) = −3 mm. Mice exhibited normal behavior within 1 min after injection. After completion of the experiments, all animals were decapitated and their brains were examined freshly (Moretti et al. 2012). Mice presenting misplacement of the injection site or any sign of cerebral hemorrhage were excluded from the statistical analysis (overall less than 5 % of the total animals used).
Experimental design
Involvement of NMDA receptors in the anti-immobility effect of creatine treatment in mice submitted to TST
Taking into account that the minimum effective dose of creatine that produced a reduction in the immobility time in the TST (at the significance level of p < 0.01) was 10 mg/kg, po and the sub-effective dose was 0.01 mg/kg, po (Cunha et al. 2012), these doses were used in the present study. Notably, these doses of creatine did not exert psychostimulant effects in the open-field test (Cunha et al. 2012). In the experiments designed to verify the involvement of the NMDAR modulation in the mechanism underlying the anti-immobility effect of creatine in the TST, mice were treated with creatine (10 mg/kg, po) or vehicle. After 45 min, NMDA (0.1 pmol/mouse, icv), d-serine (30 µg/mouse, icv, agonist of the glycine site on the NMDAR) or vehicle was administered. Fifteen minutes later, mice were submitted to the TST or open-field test. The experimental protocols for NMDA and d-serine administrations were selected on the basis of previous results from our laboratory (Bettio et al. 2012; Ludka et al. 2013; Kaster et al. 2012; Moretti et al. 2011; Rieger et al. 2014; Zeni et al. 2011; Zomkowski et al. 2010, 2012) and others (Wlaz et al. 2011).
To investigate the possible involvement of the polyamine site at NMDAR in the anti-immobility effect of creatine in the TST, mice were treated with arcaine (1 mg/kg, ip, an antagonist at the polyamine site of NMDAR). After 30 min, they received either creatine (10 mg/kg) or vehicle. Mice were submitted to behavioral testing 30 min later. The dose and protocol of administration of arcaine used were selected based on a study by Zomkowski et al. (2006).
To investigate the possible synergistic effect in the TST obtained by the combined administration of sub-effective doses of creatine and MK-801, mice were treated with a sub-effective dose of MK-801 (0.001 mg/kg, po, NMDAR antagonist) and, immediately after, a sub-effective dose of either creatine (0.01 mg/kg, po) or vehicle was administered. Mice were submitted to behavioral testing 60 min later. The dose of MK-801 was chosen based on previous studies (Bettio et al. 2012; Kaster et al. 2012; Ludka et al. 2013; Moretti et al. 2012; Zeni et al. 2011; Zomkowski et al. 2012). In another set of experiments, mice were administered with creatine (0.01 mg/kg, po) or vehicle. After 30 min, ketamine (0.1 mg/kg, ip, NMDAR antagonist) or vehicle was administered. Mice were submitted to behavioral testing 30 min later. The dose and time point of ketamine administration were selected on the basis of previous results from our laboratory (Mantovani et al. 2003; Bettio et al. 2012; Ludka et al. 2013) and others (Cruz et al. 2009; Iijima et al. 2012).
Involvement of AMPA receptors in the anti-immobility effect of creatine administration in mouse TST
The influence of AMPA receptors in the anti-immobility effect of creatine in the TST was investigated. Forty five minutes after creatine (10 mg/kg, po), fluoxetine (10 mg/kg, po, conventional antidepressant), or vehicle administrations, mice received DNQX (2.5 µg/mouse, icv, AMPA receptor antagonist). After 15 min, mice were submitted to behavioral testing. In another set of experiments, 15 min after the administration of ketamine (1 mg/kg, ip, positive control), mice received DNQX (2.5 µg/mouse, icv) and a further 15 min was elapsed to the behavioral testing. The doses of the fluoxetine and DNQX used were selected based on previous studies (Cunha et al. 2008; Sharp et al. 1995).
Involvement of l-arginine/nitric oxide pathway in anti-immobility effect of creatine treatment in the TST
To measure hippocampal and cerebrocortical NO x levels, creatine (10 mg/kg, po, an effective dose in the TST) or vehicle was administered to mice 60 min before decapitation. Ketamine (1 mg/kg, ip, effective dose in the TST), administered 30 min before decapitation, was used as a positive control. To investigate the possible involvement of the l-arginine-NO pathway in the anti-immobility effect of creatine in TST, 30 min after creatine administration (10 mg/kg, po), mice received l-arginine (750 mg/kg, ip, a precursor of NO), L-NAME (175 mg/kg, ip, non-selective NOS inhibitor), 7-nitroindazole (50 mg/kg, ip, neuronal NOS inhibitor), or vehicle. Mice were submitted to behavioral testing 30 min later. In another set of experiments, 45 min after the administration of creatine (10 mg/kg, po), mice were injected with SNAP or vehicle, and a further 15 min elapsed before animals was submitted to behavioral testing. In an independent experiment, mice were administered with the nitrergic modulators and creatine using the same administration protocols described above and, thereafter, the animals were decapitated for measurement of NO x levels. The doses and time points for l-arginine (Bettio et al. 2012; Ludka et al. 2013; Zeni et al. 2011; Zomkowski et al. 2012), SNAP (Brocardo et al. 2008; Kaster et al. 2005; Zomkowski et al. 2012), 7-nitroindazole and L-NAME (Bettio et al. 2012; da Silva et al. 2000; Harkin et al. 1999) administrations were selected on the basis of previous studies.
Effect of creatine treatment on hippocampal and cerebrocortical cellular viability
To evaluate the effect of creatine on ex vivo hippocampal and cerebrocortical cellular viability, creatine (10 mg/kg, po) or vehicle was administered to mice and 60 min later they were killed. After that, forebrains were rapidly removed from the skull and placed into ice-cold Krebs bicarbonate buffer (KRB), containing (in mM): NaCl 122, KCl 3, CaCl2 1.3, NaHCO3 25, MgSO4 1.2, KH2PO4 0.4, d-glucose 10, pre-bubbled with 95 % O2/5 % CO2 up to pH 7.4. The hippocampi or cerebral cortices were quickly dissected and sectioned into transverse slices of 400 µm thick using a tissue chopper (McIlwain Tissue Chopper, The Micle Laboratory Engineering Company). After the preincubation time (30 min in KRB), the medium was withdrawn and replaced by a nutritive culture medium composed of 50 % KRB, 50 % Dulbecco’s modified Eagle’s medium (DMEM, Gibco), 20 mM HEPES and 100 μg/ml gentamicin, at 37 °C in a CO2 atmosphere (Molz et al. 2008) and slices were maintained for an additional 4 h period to evaluate cellular viability.
Effect of creatine treatment on glutamate-induced neurotoxicity in hippocampal slices
To assess the ability of creatine treatment to counteract the excitotoxicity elicited by an in vitro challenge with glutamate, creatine (10 mg/kg, po) or vehicle was administered to mice and 60 min later the hippocampi were sectioned into 400 µm slices. After the stabilization period (30 min), slices were incubated with glutamate (Sigma, St. Louis, MO; 10 mM, in KRB buffer) or KRB buffer for 60 min. After this period, the medium was withdrawn and replaced by a nutritive culture medium, described above, at 37 °C in a CO2 atmosphere and slices were maintained for an additional 4-h period to evaluate cellular viability.
Effect of in vitro creatine incubation on hippocampal slices of mice or rats challenged with glutamate
To assess the ability of creatine (in vitro) to counteract glutamate toxicity, hippocampi from mice or rats were dissected and sectioned into transverse slices of 400 µm thick. After the stabilization period (30 min), the slices were incubated with glutamate (10 mM) or KRB buffer for 60 min. Creatine at concentrations 2.5, 5 or 10 mM was added to the slices in the presence or absence of glutamate. After this period, the medium was withdrawn and replaced by the nutritive culture medium described above and slices were maintained for an additional 4-h period to evaluate cellular viability.
Behavioral tests
Tail suspension test (TST)
The total duration of immobility induced by tail suspension was measured according to the method described by Steru et al. (1985). Briefly, mice both acoustically and visually isolated were suspended 50 cm above the floor by adhesive tape placed approximately 1 cm from the tip of the tail. Immobility time was recorded in a 6-min period by an observer blind to the drug treatment. Effective antidepressant treatments decrease immobility time of mice (Steru et al. 1985).
Open-field test
To assess the possible effects of creatine and/or the pharmacologic agents on locomotor activity, mice were subjected to the open-field paradigm (Cunha et al. 2008). Mice were individually placed in a wooden box (40 × 60 × 50 cm) with the floor divided into 12 equal rectangles (13.3 × 15 cm). The number of rectangles crossed by the animal with its four paws (crossing) was registered in a 6-min session and was considered as indicative of locomotor activity. Although the evaluation in the open-field paradigm is simple, non-automated method for assessing locomotor activity, it is able to detect either hyperlocomotion (Machado et al. 2012; Rodrigues et al. 2005) or hypolocomotion (Cunha et al. 2008; Rosa et al. 2003).
Biochemical measurements
NO x analysis
NO is unstable and quickly oxidized to nitrate and nitrite after production. Then, NO metabolites were determined using the NO x analysis, a modified method described by Hevel and Marletta (1994). Briefly, homogenates from cerebral cortex or hippocampus (pool of three hippocampi) were mixed with 25 % trichloroacetic acid and centrifuged at 1,800g for 10 min. The supernatant was immediately neutralized with 2 M potassium bicarbonate. Nitrate was measured as nitrite after enzymatic conversion by nitrate reductase by a colorimetric assay based on the Griess color reaction (Ludka et al. 2013; Zomkowski et al. 2012). A standard curve was performed using sodium nitrite (0–80 μM). Results were expressed as percentage of control (100 %).
Evaluation of cellular viability
In hippocampal or cerebral cortex slices, cellular viability was determined through the ability of cells to reduce the formazan salt 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) (Mosmann 1983). Hippocampal or cortical slices were incubated with MTT (0.5 mg/ml) in KRB for 30 min at 37 °C. The tetrazolium ring of MTT can be cleaved by active dehydrogenases to produce a precipitated formazan. The formazan produced was solubilized by adding 200 µl dimethylsulfoxide (DMSO), resulting in a colored compound whose optical density was measured in an ELISA reader (540 nm).
Protein measurement
Protein content was evaluated according to the Lowry method (Lowry et al. 1951) using bovine serum albumin (Sigma Chemical Co.) as standard.
Statistical analysis
Kolmogorov–Smirnov test was used to evaluate the normality assumption of behavioral and biochemical data. All variables in the present study showed a normal distribution. Comparisons between experimental and control groups were performed by Student’s t test (effect of creatine or ketamine on hippocampal and cerebrocortical NO x levels and effect of creatine on cellular viability of hippocampal and cerebrocortical slices) or two-way ANOVA (behavioral analysis). Post-hoc Tukey’s HSD test was used when the F values of ANOVA were significant. A value of p < 0.05 was considered to be significant.
Results
Effect of NMDA, d-serine or arcaine on anti-immobility effect of creatine in TST
Figure 1d shows that the treatment of mice with NMDA (0.1 pmol/mouse, icv) was able to abolish the anti-immobility effect of creatine (10 mg/kg, po) in the TST in mice. Two-way ANOVA revealed significant differences for creatine treatment [F(1,30) = 5.82, p < 0.01], NMDA treatment [F(1,30) = 8.38, p < 0.01] and creatine × NMDA interaction [F(1,30) = 15.85, p < 0.01]. NMDA administration alone or in combination with creatine did not significantly affect ambulation in the open-field test (p > 0.05, data not shown).
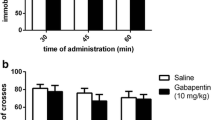
Activation of NMDA receptors abolishes the anti-immobility effect of creatine. Timeline of NMDA (a), d-serine (b) and arcaine (c) administrations to reverse the anti-immobility effect of creatine. Effect of treatments of mice with NMDA (0.1 pmol/mouse, icv), d-serine (30 µg/mouse, icv) or arcaine (1 mg/kg, ip) on the anti-immobility effect of creatine (10 mg/kg, po) in the TST (d, e and f, respectively). Each column represents the mean + SEM. *p < 0.05, **p < 0.01 compared with the vehicle-treated control; # p < 0.05, ## p < 0.01, as compared to same group treated with vehicle (creatine/vehicle)
Similarly Fig. 1e shows that the treatment of mice with d-serine (30 µg/mouse, icv) abolished the anti-immobility effect of creatine (10 mg/kg, po) in the TST. Two-way ANOVA revealed significant differences for the creatine treatment [F(1,33) = 11.92, p < 0.01], d-serine [F(1,33) = 5.19, p < 0.05] and creatine × d-serine interaction [F(1,33) = 4.65, p < 0.05]. d-serine administration alone or in combination with creatine did not affect the ambulation in the open-field test (p > 0.05, data not shown).
Arcaine administration (1 mg/kg, ip) reversed the anti-immobility effect of creatine in the TST (Fig. 1f). The two-way ANOVA revealed significant differences for the creatine treatment [F(1,26) = 6.27, p < 0.05] and arcaine × creatine interaction [F(1,33) = 4.69, p < 0.05], but not a main effect of arcaine treatment [F(1,33) = 1.63, p = 0.21]. Arcaine administration alone or in combination with creatine did not affect ambulation in the open-field test (p > 0.05, data not shown).
Effect of combined treatment with sub-effective doses of the NMDA antagonists MK-801 or ketamine and creatine in the TST.
Figure 2c shows that combined administration of sub-effective doses of MK-801 (0.001 mg/kg, po) and creatine (0.01 mg/kg, po) caused an anti-immobility effect in the TST, but the administration of creatine or MK-801 alone did not reduce immobility time in the TST. Two-way ANOVA revealed significant differences for the creatine treatment [F(1,32) = 4.82, p < 0.01], MK-801 treatment [F(1,32) = 8.68, p < 0.01] and creatine × MK-801 interaction [F(1,32) = 6.07, p < 0.01]. Creatine administration alone or in combination with MK-801 did not affect ambulation in the open-field test (p > 0.05, data not shown).
A sub-effective dose of creatine produces an anti-immobility effect in the TST when combined with sub-effective doses of NMDA receptor antagonists. Timeline of experimental protocol of mice treated with creatine in combination with MK-801 (a) or ketamine (b). Effects of sub-effective doses of creatine (0.01 mg/kg, po) in combination with MK-801 (0.001 mg/kg, po, an NMDAR antagonist) or ketamine (0.1 mg/kg, ip, an NMDAR antagonist) on the immobility time in the TST (c and d, respectively). Each column represents the mean + SEM. **p < 0.01 compared with the vehicle-treated control
Combined administration of sub-effective doses of ketamine (0.1 mg/kg, ip) and creatine (0.01 mg/kg, po) produced synergistic anti-immobility effect in the TST (Fig. 2d). Two-way ANOVA revealed significant differences for creatine treatment [F(1,33) = 18.40, p < 0.01] and creatine × ketamine interaction [F(1,33) = 4.81, p < 0.05], but not a main effect of ketamine treatment [F(1,33) = 1.56, p = 0.22]. Ketamine administration alone or in combination with creatine did not significantly alter the ambulation in the open-field test (p > 0.05, data not shown).
Effect of the DNQX on the anti-immobility effect of creatine in the TST
Results depicted in Fig. 3 show that the anti-immobility effect of creatine (10 mg/kg, po) or fluoxetine (10 mg/kg, po) was not prevented by pretreatment of mice with the AMPA receptor antagonist DNQX (2.5 µg/mouse, icv) in the TST (p > 0.05, Fig. 3d, e, respectively). The number of crossings in open-field test was not altered by DNQX, creatine or fluoxetine treatments (p > 0.05, data not shown). Conversely, administration of DNQX abolished the anti-immobility effect of ketamine in the TST (Fig. 3f). Two-way ANOVA revealed significant differences for ketamine treatment [F(1,24) = 4.70, p < 0.05] and ketamine × DNQX interaction [F(1,24) = 4.95, p < 0.05], but not a main effect of DNQX treatment [F(1,24) = 1.64, p = 0.21]. Ketamine administration alone or in combination with DNQX did not affect ambulation in the open-field test (p > 0.05, data not shown).
DNQX, an AMPA receptor antagonist, abolishes the anti-immobility effect of ketamine, but not of creatine or fluoxetine. Timeline of reversal protocol of the anti-immobility effect of creatine, fluoxetine or ketamine by DNQX (a, b and c, respectively). Effects of treatments of mice with DNQX (2.5 µg/mouse, icv) and creatine (10 mg/kg, po), fluoxetine (10 mg/kg, po) or ketamine (1 mg/kg, ip) on the immobility time in the TST (d, e and f, respectively). Each column represents the mean + SEM. *p < 0.05, **p < 0.01 compared with the vehicle-treated control; # p < 0.05, ## p < 0.01, as compared to same group treated with vehicle (creatine/vehicle)
Effect of creatine treatment on NO x levels in hippocampus and cerebral cortex
NO x measurement was performed in hippocampus and cerebral cortex of mice treated with creatine at dose of 10 mg/kg (po) or vehicle 60 before decapitation (Fig. 4). Creatine at dose of 10 mg/kg significantly increased NO x levels in hippocampus and cerebral cortex of mice (46.3 and 43.6 %, respectively), as compared with control group [T Test: t(10) = −2.92; p < 0.05; t(14) = −3.63; p < 0.01, respectively]. Ketamine, used as a positive control, also increased NO x levels in the hippocampus and cerebral cortex [116.2 and 93.2 %, respectively, t test: t(9) = 2.30; p < 0.05 and t(21) = 2.30; p < 0.05, respectively]. Considering that the effect of creatine on NO x levels was similar in both brain structures, the next experiments that investigate the influence of NO modulators on the creatine-induced increase in NO x levels were performed in cerebral cortex due to the higher amount of tissue available to the assays.
Creatine, similar to ketamine, increases NO x levels in hippocampus and cerebral cortex. Effect of treatment with creatine (10 mg/kg, po) or ketamine (1 mg/kg, ip, an NMDAR antagonist) on the NOx levels in the hippocampus and cerebral cortex of mice. Each column represents the mean + SEM. *p < 0.05 compared with the vehicle-treated control. The NO x levels in the control group (100 %) was 13.20 µM nitrite/mg protein (hippocampus) and 22.3 µM nitrite/mg protein (cerebral cortex)
Effect of l-arginine, SNAP or 7-nitroindazole on the anti-immobility effect of creatine in the TST, and on cerebrocortical NO x levels
Taking into account that NO modulation may affect either behavioral responses of creatine in the TST or its ability to enhance NO x levels, the next set of the experiments evaluated the influence of the NO enhancers l-arginine and SNAP and the NOS inhibitors L-NAME and 7-nitroindazole on the effect of creatine in the TST and on NO x levels in the cerebral cortex. Figure 5c shows that treatment of mice with l-arginine (750 mg/kg, ip) abolished the anti-immobility effect of creatine (10 mg/kg, po) in TST. Two-way ANOVA revealed significant differences for creatine treatment [F(1,23) = 23.48, p < 0.01], l-arginine treatment [F(1,23) = 5.17, p < 0.05] and creatine × l-arginine interaction [F(1,23) = 5.11, p < 0.05]. l-arginine administration alone or in combination with creatine did not affect the ambulation in the open-field (p > 0.05, data not shown). Additionally, Fig. 5e shows that the treatment of mice with l-arginine (750 mg/kg, ip), at dose that per se produced an enhancement on NO x levels, was able to potentiate the creatine-induced increase in NO x levels. Two-way ANOVA analysis revealed significant differences for the creatine treatment [F(1,24) = 43.02, p < 0.01] and l-arginine treatment [F(1,24) = 17.17, p < 0.01], but not creatine × l-arginine interaction [F(1,24) = 0.37, p = 0.55].
Influence of treatment with l-arginine or SNAP on the effect of creatine in the TST, open-field test and NO x levels. Timeline of reversal protocol of the anti-immobility effect of creatine by l-arginine (a) and SNAP (b). Effect of treatment of mice with l-arginine (750 mg/kg, ip, a precursor of NO) or SNAP (25 µg/mouse, icv, a NO donor) on the immobility time in the TST (c and d, respectively) and on NO x levels in the cerebral cortex (e and f, respectively). Each column represents the mean + SEM. **p < 0.01 compared with the vehicle-treated control; # p < 0.05, ## p < 0.01 as compared to group pretreated with creatine and treated with vehicle; $$ p < 0.01 as compared to group pretreated with vehicle and treated with l-arginine. The NO x level in the control group (100 %) was 7.64 µM nitrite/mg protein (g) and 7.82 µM nitrite/mg protein (h)
Figure 5d shows that treatment of mice with the NO donor SNAP (25 µg/mouse, icv) was able to abolish the anti-immobility effect of creatine (10 mg/kg, po) in the TST. Two-way ANOVA revealed significant differences for creatine treatment [F(1,24) = 5.47, p < 0.05], SNAP treatment [F(1,24) = 7.60, p < 0.05] and creatine × SNAP interaction [F(1,24) = 5.81, p < 0.05]. SNAP administration alone or in combination with creatine did not affect ambulation in the open-field (p > 0.05, data not shown). Moreover, Fig. 5f shows that treatment of mice with SNAP, which per se produced an enhancement on NO x levels, enhanced the effect of creatine (10 mg/kg, po) on NO x levels. Two-way ANOVA revealed significant differences for SNAP treatment [F(1,26) = 13.90, p < 0.01] and creatine × SNAP interaction [F(1,26) = 7.47, p < 0.05], but not a main effect for creatine treatment [F(1,26) = 0.50, p = 0.49].
Administration of a non-selective NOS inhibitor, namely L-NAME (175 mg/kg, ip), prevented the anti-immobility effect of creatine in the TST (Fig. 6b). Two-way ANOVA revealed significant differences for creatine treatment [F(1,32) = 4.44, p < 0.05], L-NAME treatment [F(1,32) = 20.22, p < 0.01] and L-NAME × creatine interaction [F(1,32) = 18.24, p < 0.01]. L-NAME administration alone or in combination with creatine did not affect ambulation in the open-field (p > 0.05, data not shown). Figure 6d shows that treatment of mice with L-NAME abolished the increase in cerebrocortical NO x levels induced by creatine administration (10 mg/kg, po). Two-way ANOVA revealed significant differences for creatine treatment [F(1,28) = 16.86, p < 0.01] and L-NAME treatment [F(1,28) = 30.31, p < 0.01], but not for creatine × L-NAME interaction [F(1,28) = 0.15, p = 0.70].
Influence of NOS inhibitors on the effect of creatine in the TST, open-field test and NOx levels. Timeline of experimental protocol for drug administrations and behavioral tests (a). Effect of treatment of mice with 7-nitroindazole (50 mg/kg, ip, a neuronal nitric oxide synthase inhibitor) or L-NAME (175 mg/kg, ip, a nitric oxide synthase inhibitor) on the anti-immobility effect of creatine (10 mg/kg, po) in the TST (b and c, respectively) and on cerebrocortical NO x levels (d and e, respectively). Each column represents the mean + SEM. *p < 0.05, **p < 0.01 compared with the vehicle-treated control; # p < 0.05, ## p < 0.01 as compared to group pretreated with creatine and treated with vehicle. The NO x level in the control group (100 %) was 7.96 µM nitrite/mg protein (d) and 7.11 µM nitrite/mg protein (e)
Administration of a nNOS inhibitor 7-nitroindazole (50 mg/kg, ip) prevented the anti-immobility effect of creatine in the TST (Fig. 6c). Two-way ANOVA revealed significant differences for creatine treatment [F(1,26) = 10.67, p < 0.01] and 7-nitroindazole × creatine interaction [F(1,26) = 5.62, p < 0.05], but not a main effect of 7-nitroindazole treatment [F(1,26) = 4.09, p = 0.05]. The administration of 7-nitroindazole alone or in combination with creatine did not affect ambulation in the open-field test (p > 0.05, data not shown). Moreover, Fig. 6e shows that treatment of mice with 7-nitroindazole abolished creatine-induced increase of NO x levels in cerebral cortex. Two-way ANOVA revealed significant differences for creatine treatment [F(1,28) = 11.74, p < 0.01] and creatine × 7-nitroindazole interaction [F(1,28) = 5.31, p < 0.05], but not for 7-nitroindazole treatment [F(1,28) = 0.44, p = 0.51].
Effect of creatine on cellular viability of hippocampal and cerebrocortical slices
Cellular viability analysis was performed in mice administered with creatine at dose of 10 mg/kg or vehicle 60 min before decapitation. Figure 7 shows increased cellular viability (19.6 %) in hippocampal slices obtained from mice treated with creatine as compared with slices obtained from control group (mice administered with vehicle), as revealed by t test: t(16) = −2.40; p < 0.05. Moreover, creatine administration significantly increased cellular viability (11.8 %) in the cerebral cortex as compared with the control group, as revealed by t test: t(15) = 3.84; p < 0.01 (Fig. 7). Considering that the effect of creatine was slightly higher in the hippocampus than in the cerebral cortex, the next experiments that investigated whether creatine could counteract glutamate toxicity were performed in hippocampal slices.
Creatine increases cellular viability in hippocampal and cerebrocortical slices of mice. Effect of the treatment of mice with creatine (10 mg/kg, po) on cellular viability of hippocampal and cerebrocortical slices. Each column represents the mean + SEM. *p < 0.05 as compared to control group treated with vehicle
Effect of creatine on the glutamate-induced neurotoxicity in hippocampal slices
Hippocampal slices obtained from mice administered with creatine at dose of 10 mg/kg or vehicle 60 min before decapitation were submitted to glutamate challenge (10 mM, in vitro) for 1 h. Slices incubated with glutamate presented a reduced cellular viability when compared to control slices. Creatine administration in mice was not able to reverse the glutamate-induced decrease in hippocampal cellular viability (Fig. 8a). The two-way ANOVA revealed significant differences for creatine treatment [F(1,16) = 8.36, p < 0.05], glutamate incubation [F(1,16) = 50.76, p < 0.01] and creatine × glutamate interaction [F(1,16) = 4.67, p < 0.05].
In vitro, but not ex vivo, creatine protects against glutamate-induced decrease in hippocampal cellular viability. Effect of administration of mice with creatine (10 mg/kg, po) on glutamate-induced neurotoxicity in hippocampal slices of mice (a) and the creatine incubation (2.5–10 mM) on the cellular viability of mouse or rat hippocampal slices exposed to glutamate (10 mM) (b and c, respectively). Each column represents the mean + SEM. *p < 0.05 as compared to control group treated with vehicle. **p < 0.01, ***p < 0.001 as compared to control group treated with vehicle. # p < 0.05, ## p < 0.01 as compared to group treated with glutamate
We also investigated the protective effect of in vitro creatine incubation (2.5, 5 and 10 mM) against neurotoxicity induced by glutamate (10 mM) in mice and rats hippocampal slices (Fig. 8b, c, respectively). In vitro incubation of mice hippocampal slices with 5–10 mM creatine was effective to abolish glutamate-induced decrease in cellular viability (Fig. 8b), as revealed by two-way ANOVA (creatine incubation [F(3,34) = 4.09, p < 0.05], glutamate incubation [F(1,34) = 113.20, p < 0.01] and creatine × glutamate interaction [F(3,34) = 6.55, p < 0.01]. Reinforcing the neuroprotective properties of creatine, the results presented in Fig. 8c show that the in vitro incubation of rats hippocampal slices with 2.5, 5 and 10 mM creatine was also effective to abolish glutamate toxicity, as revealed by one-way ANOVA [F(1,4) = 6.06; P < 0.01].
Discussion
This study shows that oral administration of creatine, a substrate of creatine kinase and a precursor of phosphocreatine, has an anti-immobility effect in TST, not influenced by any unspecific locomotor effect, by a mechanism that involves NMDAR and NO modulation.
The NMDAR antagonist ketamine has been shown to elicit a rapid antidepressant action in preclinical and clinical reports (Autry et al. 2011; Berman et al. 2000; Li et al. 2011). Interestingly, a study by Assis et al. (2009) showed that the acute administration of ketamine, besides producing an anti-immobility effect, increased the creatine kinase activity in striatum, cerebral cortex and cerebellum. Memantine, another NMDAR antagonist with anti-immobility effect, also increased creatine kinase activity in prefrontal cortex and hippocampus of rats (Reus et al. 2012). In vitro and in vivo studies have reported that ketamine and MK-801 facilitate recovery of phosphocreatine levels after ischemic or anoxic brain injury, clinical conditions associated with glutamatergic dysfunction (Bielenberg et al. 1987; Haraldseth et al. 1990; Raley and Lipton 1990; Spandou et al. 1999). Interestingly, creatine has been proposed to modulate the glutamatergic system (Andreassen et al. 2001; Bender et al. 2005; Almeida et al. 2006; Royes et al. 2008), but the involvement of the glutamatergic system in the anti-immobility effect of this compound was not previously explored. Therefore, this study investigated the involvement of the NMDAR in the anti-immobility effect of creatine in the TST.
We show that the behavioral response in the TST induced by creatine treatment involves a direct or indirect inhibition of NMDAR, since the treatment of mice with either NMDA or d-serine, a potent co-agonist of synaptic NMDARs (Papouin et al. 2012), caused complete reversal of the anti-immobility effect elicited by creatine. Similar results have been reported for other compounds that exert anti-immobility effects by a mechanism dependent on NMDAR inhibition (Brocardo et al. 2008; Kaster et al. 2012; Ludka et al. 2013; Moretti et al. 2011; Poleszak et al. 2008; Zeni et al. 2011; Zomkowski et al. 2010). Corroborating the hypothesis that creatine modulates the NMDAR, we observed that arcaine, an antagonist of the polyamine site of the NMDAR, abolished the anti-immobility action of creatine. This result suggests that the anti-immobility effect of creatine could be due to its interaction with this modulatory site at NMDAR. In line with this, arcaine abolished the antidepressant-like effect of putrescine, a polyamine with anti-immobility effects in the TST and FST (Zomkowski et al. 2006). Moreover, it has been suggested that creatine could act as an agonist of the polyamine site at the NMDAR since endogenous polyamine spermidine intensifies, while polyamine antagonist, such as arcaine, blocks enhanced spatial learning induced by creatine (Oliveira et al. 2008).
Another finding that reinforces the notion that an NMDAR modulation of glutamatergic system plays a role in the anti-immobility effect of creatine is the synergistic anti-immobility effect observed when sub-effective doses of creatine and MK-801 or ketamine were administered to mice. Accordingly, it has been reported that MK-801 or ketamine produces similar effects when associated with several compounds that display antidepressant properties (Ludka et al. 2013; Moretti et al. 2011; Zeni et al. 2011; Zomkowski et al. 2012). In line with this, a combination of creatine and MK-801 provided protection in an experimental model of anoxia in hippocampal slices (Carter et al. 1995). Considering that dopamine D1 receptor activation is involved in the anti-immobility effect of creatine (Cunha et al. 2012) and that the dopamine D1 receptor agonist SKF38393 could enhance the antidepressant-like effect of non-competitive NMDAR antagonist MK-801 (Yuan et al. 2011), it is possible that the interaction of NMDAR and dopamine D1 receptors could play a role in the anti-immobility effect of creatine.
The antidepressant response induced by ketamine has been shown to be associated with stimulation of the postsynaptic alpha-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid (AMPA) receptors and BDNF release (Krystal et al. 2013; Moghaddam et al. 1997). We hypothesized that creatine could share with ketamine a similar mechanism of action, activating AMPA receptors in glutamatergic neurons. Interestingly, the AMPA receptor antagonist DNQX abolished the anti-immobility effect of ketamine in the TST, in agreement with literature data that reported a similar effect using NBQX (Koike et al. 2011), but did not affect the anti-immobility effect of creatine or fluoxetine. These results suggest that creatine and fluoxetine produce an anti-immobility effect in the TST by a mechanism independent of AMPA receptor activation, as opposed to ketamine.
Once NMDAR is activated, intracellular calcium levels increase, leading to NO synthesis by nNOS (Esplugues 2002). High concentrations of NO lead to neuronal cell death, whereas lower concentrations are neuroprotective by controlling proliferation and differentiation of mouse neuronal progenitor cells (Baranano and Snyder 2001; Calabrese et al. 2007; Cheng et al. 2003). A dual effect of NO was also suggested regarding mood regulation, since both the NO precursor l-arginine and NOS inhibitors, depending on the doses, may elicit antidepressant-like effects (da Silva et al. 2000; Inan et al. 2004). It is likely that NO exerts beneficial effects on mood, when present at low levels. Interestingly, in the present study, creatine at 10 mg/kg increased the NO x levels in the hippocampus and cerebral cortex of mice. Of note, the administration of ketamine, at a dose that produces an anti-immobility effect in the TST (Ludka et al. 2013), caused a similar increase in the hippocampal and cerebrocortical NO x levels. Therefore, in our study a slight increase in NO levels is associated with antidepressant-like responses. Ketamine also increased NO concentrations in the hippocampus and striatum of rats (Wu et al. 2000) and stimulated the l-arginine/NO pathway via neuronal NOS (Romero et al. 2011). Regarding the modulation of NO, creatine was shown to increase the number of NOS-immunoreactive striatal neurons (Ducray et al. 2006), but was able to abolish the increase in NO levels induced by glutamate in neuronal/glial cells (Juravleva et al. 2003). Future investigations are necessary to understand the detailed mechanisms underlying the modulation of NO levels by creatine.
The increase in NO levels, in turn, may regulate the monoaminergic tonus in the CNS. The experimental treatment with l-arginine or NO donors was reported to induce an augmentation of dopamine release, suggesting that endogenous NO stimulates dopamine activity (Lorrain and Hull 1993). In addition, studies performed in hippocampal slices demonstrate that NO donors increase norepinephrine release (Satoh et al. 1996). Evidence also indicates that NO signaling plays an important role in the mechanism of norepinephrine-induced neuroprotection in both in vivo and in vitro models (Chen and Russo-Neustadt 2007; Lonart et al. 1992). In addition, the NO donor SNAP was reported to increase serotonin levels in the hippocampus, as opposed to the decrease in serotonin induced by NMDA (Segieth et al. 2001). Therefore, it is possible that creatine-induced increase in NO levels with consequent monoaminergic modulation may be associated with its anti-immobility effect in the TST. This hypothesis is consistent with the fact that the behavioral effects in the TST induced by creatine are dependent on the activation of dopamine D1 and D2 receptors, α1-adrenoceptors and 5-HT1A receptors (Cunha et al. 2012, 2013a, b).
Considering that the modulation on NO levels has been reported to be involved in the pathophysiology of depression (da Silva et al. 2000; Inan et al. 2004; Suzuki et al. 2001), we investigated the participation of the l-arginine/NO pathway in the anti-immobility effect of creatine. Our results indicate that NO modulation influences the anti-immobility effect of creatine in the TST, because the treatment of mice with l-arginine or SNAP completely abolished its anti-immobility effect, without altering locomotor activity of mice. These results are in line with previous studies which showed that the anti-immobility effects of several compounds were prevented by l-arginine or SNAP (Brocardo et al. 2008; Kaster et al. 2005; Ludka et al. 2013; Moretti et al. 2011; Zomkowski et al. 2010). A study by Krass et al. (2011) also reported that pretreatment with l-arginine abolished the anti-immobility effect of imipramine, venlafaxine and bupropion in the FST. Noteworthy, in the present study, either l-arginine or SNAP administration potentiated the creatine-induced increase in NO x levels. Therefore, we postulate that a slight increase in NO is related with an anti-immobility effect in the TST, as opposed to a higher increase in NO levels. This is in line with the hypothesis that NO exerts a dual role in the modulation of depression, since the administration of l-arginine significantly reduced the duration of immobility in the FST at low doses (250–500 mg/kg, ip), but not at higher doses (750–1,000 mg/kg) (da Silva et al. 2000). The reduction of immobility time induced by l-arginine was reversed by the NOS inhibitor L-NNA. Conversely, L-NNA, depending on its dose is able to cause an antidepressant-like effect, which can be reversed by l-arginine, administered at a dose that produces no effect in the FST (da Silva et al. 2000). Interestingly, exogenous administration of l-arginine (250–500 mg/kg), at same doses that produce anti-immobility effect, increased neuronal NO signal (Heinzen and Pollack 2002) and DETA/NONOate, a NO donor, produces anti-immobility effect associated with enhancement of NO x levels and hippocampal neurogenesis (Hua et al. 2008). Accordingly, a low dose of L-NAME (100 mg/kg, ip) decreased the immobility time in the FST, whereas high doses (175–300 mg/kg, ip) did not produce any anti-immobility effect in the FST (Harkin et al. 1999).
To further investigate the role of NO in the anti-immobility effect of creatine, in another set of experiments, we evaluated the influence of the administration of the non-selective NOS inhibitor L-NAME and the potent and selective neuronal NOS inhibitor 7-nitroindazole on the effect of creatine in the TST. The ability of these NOS inhibitors to abolish either the anti-immobility effect of the creatine or the creatine-induced increase in NO x levels in cerebral cortex reinforces the hypothesis that the slight creatine-induced increase in NO levels may afford an anti-immobility effect. Interestingly, a study reported that creatine supplementation was able to prevent the reduction on ATP and creatine levels caused by L-NAME administration in rats, suggesting a relationship between NO modulation and creatine effects (Constantin-Teodosiu et al. 1995).
In summary, we provide evidence for a neuromodulatory effect of creatine on NMDAR and on NO levels, although the mechanisms by which creatine interacts with NMDAR require further studies. In line with our results, creatine (10 mM) has been shown to decrease the excitability of hippocampal slices of rats submitted to control or anoxia condition (Parodi et al. 2003) and to produce a direct inhibitory action on the hippocampal NMDAR-mediated calcium response (Genius et al. 2012). Notably, creatine binds to the central benzodiazepine receptor (Kawasaki et al. 2001), an effect that may be associated with NMDAR inhibition. Another possibility that may account for the observed results is that NO could inhibit NMDAR function through a direct action on the receptor-channel complex (Lei et al. 1992; Manzoni et al. 1992), in line with the finding that creatine increased the hippocampal and cerebrocortical NO x levels. Nitrosylation of the NR1 and NR2 subunits of the NMDAR results in functional downregulation of the NMDAR activity, therefore, protecting neurons from excitotoxic insults caused by excessive receptor activation (Choi and Lipton 2000; Lei et al. 1992; Lipton et al. 1998).
Considering that antidepressant and neuroprotective effects may be correlated (Young, 2002; Zeni et al. 2011), in another set of experiments we investigated the effects of the administration of creatine at a dose that produced anti-immobility effect in the TST (10 mg/kg) on the ex vivo cellular viability of hippocampal and cerebrocortical slices of mice, as compared to the slices obtained from mice not treated with creatine. Creatine (10 mg/kg, po) increased cellular viability of hippocampal and cerebrocortical slices, suggesting that the administration of this compound exerts a beneficial effect on the signaling mechanisms that maintain cell survival. In line with our results, creatine increased tyrosine hydroxylase positive cells in ventral mesencephalic organotypic tissue culture (Andres et al. 2005). Interestingly, other ex vivo treatments have been reported to cause similar effects, including ketamine that improved the quality (cellular viability) of neuronal brain slice preparations of neonatal mouse (de Oliveira et al. 2010). Accordingly, NO, which was increased by either creatine or ketamine administration, is required for neuronal survival (Contestabile and Ciani 2004).
Interestingly, the glutamate-induced reduction on cellular viability of hippocampal slices of mice was not prevented by ex vivo creatine treatment (10 mg/kg, po), suggesting that the anti-immobility effect of creatine is not associated with a protective effect against hippocampal glutamate toxicity. However, creatine incubated in vitro (0.1–10 mM) was reported to protect against glutamate-induced toxicity in cell cultures (Brewer and Wallimann 2000; Genius et al. 2012; Juravleva et al. 2003, 2005). Considering that hippocampal slices offer certain advantages over cell cultures, as the pattern of synaptic connections within the slice is minimally altered and neuron–astrocyte–microglia interactions are preserved (Somjen et al. 1987), in a next set of experiments the in vitro effect of creatine incubation in hippocampal slices was evaluated. To this end, creatine was incubated at relatively high concentrations in rat and mouse hippocampal slices challenged with glutamate. We demonstrated that high creatine concentrations (2.5–10 mM) incubated either in rat or mouse hippocampal slices prevented the toxicity induced by glutamate (10 mM). Opening NMDAR could reduce the membrane potential and lead to a reduced transport rate of creatine into the cytosol. Since creatine transporter works at half maximal rate under physiological conditions (Guerrero-Ontiveros and Wallimann 1998), the reduced transportation rate of creatine may be compensated by an elevated concentration of creatine in the incubation medium.
In conclusion, the present study indicates that modulation of NMDAR and NO levels plays a significant role in the anti-immobility effect of creatine, and reinforces the notion that these are pivotal targets for antidepressant action. Furthermore, the results presented herein show that creatine may also elicit a protective effect against glutamate-induced reduction on hippocampal cellular viability when present at high concentrations in the incubation medium, a result that warrants future studies for the investigation of creatine to counteract glutamatergic excitotoxicity. Under basal conditions, the higher hippocampal cellular viability of slices obtained from mice-treated ex vivo with a dose of creatine that affords anti-immobility effect reinforces the notion that this compound should be further investigated as a promising antidepressant and neuroprotective agent.
Abbreviations
- MTT:
-
3-(4,5-Dimethylthiazol-2-yl-diphenyltetrazolium bromide
- DMEM:
-
Dulbecco’s modified Eagle’s medium
- DMSO:
-
dimethylsulfoxide
- FST:
-
Forced Swimming Test
- Icv :
-
Intracerebroventricular
- Ip :
-
Intraperitoneal
- L-NAME:
-
NG-nitro-l-arginine methyl ester
- NO:
-
Nitric oxide
- NOS:
-
Nitric oxide synthase
- NMDA:
-
N-Methyl-D-aspartate
- NMDAR:
-
N-Methyl-D-aspartate receptor
- Po:
-
Per os
- SNAP:
-
S-nitroso-N-acetyl-penicillamine
- TST:
-
Tail suspension test
References
Allen PJ, D’Anci KE, Kanarek RB, Renshaw PF (2010) Chronic creatine supplementation alters depression-like behavior in rodents in a sex-dependent manner. Neuropsychopharmacology 35:534–546
Almeida LS, Salomons GS, Hogenboom F, Jakobs C, Schoffelmeer AN (2006) Exocytotic release of creatine in rat brain. Synapse 60:118–123
Andreassen OA, Jenkins BG, Dedeoglu A, Ferrante KL, Bogdanov MB, Kaddurah-Daouk R et al (2001) Increases in cortical glutamate concentrations in transgenic amyotrophic lateral sclerosis mice are attenuated by creatine supplementation. J Neurochem 77:383–390
Andres RH, Ducray AD, Perez-Bouza A, Schlattner U, Huber AW, Krebs SH et al (2005) Creatine supplementation improves dopaminergic cell survival and protects against MPP+ toxicity in an organotypic tissue culture system. Cell Transplant 14:537–550
Assis LC, Rezin GT, Comim CM, Valvassori SS, Jeremias IC, Zugno AI et al (2009) Effect of acute administration of ketamine and imipramine on creatine kinase activity in the brain of rats. Revista Brasileira de Psiquiatria 31:247–252
Autry AE, Adachi M, Nosyreva E, Na ES, Los MF, Cheng PF et al (2011) NMDA receptor blockade at rest triggers rapid behavioural antidepressant responses. Nature 475:91–95
Baranano DE, Snyder SH (2001) Neural roles for heme oxygenase: contrasts to nitric oxide synthase. Proc Natl Acad Sci USA 98:10996–11002
Bender A, Auer DP, Merl T, Reilmann R, Saemann P, Yassouridis A et al (2005) Creatine supplementation lowers brain glutamate levels in Huntington’s disease. J Neurol 252:36–41
Berman RM, Cappiello A, Anand A, Oren DA, Heninger GR, Charney DS et al (2000) Antidepressant effects of ketamine in depressed patients. Biol Psychiatry 47:351–354
Bettio LE, Cunha MP, Budni J, Pazini FL, Oliveira A, Colla AR et al (2012) Guanosine produces an antidepressant-like effect through the modulation of NMDA receptors, nitric oxide-cGMP and PI3 K/mTOR pathways. Behav Brain Res 234:137–148
Bielenberg GW, Beck T, Sauer D, Burniol M, Krieglstein J (1987) Effects of cerebroprotective agents on cerebral blood flow and on postischemic energy metabolism in the rat brain. J Cereb Blood Flow Metab 7:480–488
Brewer GJ, Wallimann TW (2000) Protective effect of the energy precursor creatine against toxicity of glutamate and beta-amyloid in rat hippocampal neurons. J Neurochem 74:1968–1978
Brocardo PS, Budni J, Lobato KR, Kaster MP, Rodrigues AL (2008) Antidepressant-like effect of folic acid: involvement of NMDA receptors and l-arginine-nitric oxide-cyclic guanosine monophosphate pathway. Eur J Pharmacol 598:37–42
Calabrese V, Mancuso C, Calvani M, Rizzarelli E, Butterfield DA, Stella AM (2007) Nitric oxide in the central nervous system: neuroprotection versus neurotoxicity. Nat Rev Neurosci 8:766–775
Carter AJ, Muller RE, Pschorn U, Stransky W (1995) Preincubation with creatine enhances levels of creatine phosphate and prevents anoxic damage in rat hippocampal slices. J Neurochem 64:2691–2699
Chen MJ, Russo-Neustadt AA (2007) Nitric oxide signaling participates in norepinephrine-induced activity of neuronal intracellular survival pathways. Life Sci 81:1280–1290
Cheng A, Wang S, Cai J, Rao MS, Mattson MP (2003) Nitric oxide acts in a positive feedback loop with BDNF to regulate neural progenitor cell proliferation and differentiation in the mammalian brain. Dev Biol 258:319–333
Choi YB, Lipton SA (2000) Redox modulation of the NMDA receptor. Cell Mol Life Sci 57:1535–1541
Constantin-Teodosiu D, Greenhaff PL, Gardiner SM, Randall MD, March JE, Bennett T (1995) Attenuation by creatine of myocardial metabolic stress in Brattleboro rats caused by chronic inhibition of nitric oxide synthase. Br J Pharmacol 116:3288–3292
Contestabile A (2000) Roles of NMDA receptor activity and nitric oxide production in brain development. Brain Res Rev 32:476–509
Contestabile A, Ciani E (2004) Role of nitric oxide in the regulation of neuronal proliferation, survival and differentiation. Neurochem Int 45:903–914
Cruz SL, Soberanes-Chávez P, Páez-Martinez N, López-Rubalcava C (2009) Toluene has antidepressant-like actions in two animal models used for the screening of antidepressant drugs. Psychopharmacology 204:279–286
Cunha MP, Machado DG, Bettio LE, Capra JC, Rodrigues AL (2008) Interaction of zinc with antidepressants in the tail suspension test. Prog Neuropsychopharmacol Biol Psychiatry 32:1913–1920
Cunha MP, Machado DG, Capra JC, Jacinto J, Bettio LE, Rodrigues AL (2012) Antidepressant-like effect of creatine in mice involves dopaminergic activation. J Psychopharmacol 26:1489–1501
Cunha MP, Pazini FL, Oliveira A, Bettio LE, Rosa JM, Machado DG et al (2013a) The activation of alpha1-adrenoceptors is implicated in the antidepressant-like effect of creatine in the tail suspension test. Prog Neuropsychopharmacol Biol Psychiatry 44:39–50
Cunha MP, Pazini FL, Oliveira A, Machado DG, Rodrigues AL (2013b) Evidence for the involvement of 5-HT1A receptor in the acute antidepressant-like effect of creatine in mice. Brain Res Bull 95:61–69
da Silva GD, Matteussi AS, dos Santos AR, Calixto JB, Rodrigues AL (2000) Evidence for dual effects of nitric oxide in the forced swimming test and in the tail suspension test in mice. Neuro Rep 11:3699–36702
Dager SR, Friedman SD, Parow A, Demopulos C, Stoll AL, Lyoo IK et al (2004) Brain metabolic alterations in medication-free patients with bipolar disorder. Arch Gen Psychiatry 61:450–458
de Oliveira RB, Graham B, Howlett MC, Gravina FS, Oliveira MW, Imtiaz MS et al (2010) Ketamine anesthesia helps preserve neuronal viability. J Neurosci Methods 189:230–232
Dhir A, Kulkarni SK (2007) Involvement of nitric oxide (NO) signaling pathway in the antidepressant action of bupropion, a dopamine reuptake inhibitor. Eur J Pharmacol 568:177–185
Ducray A, Kipfer S, Huber AW, Andres RH, Seiler RW, Schlattner U et al (2006) Creatine and neurotrophin-4/5 promote survival of nitric oxide synthase-expressing interneurons in striatal cultures. Neurosci Lett 395:57–62
Duman RS, Li N, Liu RJ, Duric V, Aghajanian G (2012) Signaling pathways underlying the rapid antidepressant actions of ketamine. Neuropharmacology 62:35–41
Esplugues JV (2002) NO as a signalling molecule in the nervous system. Br J Pharmacol 135:1079–1095
Franklin KBJ, Paxinos G (1997) The mouse brain in stereotaxic coordinates, 1st edn. Academic Press, San Diego
Genius J, Geiger J, Bender A, Moller HJ, Klopstock T, Rujescu D (2012) Creatine protects against excitoxicity in an in vitro model of neurodegeneration. PLoS One 7:e30554
Guerrero-Ontiveros ML, Wallimann T (1998) Creatine supplementation in health and disease. Effects of chronic creatine ingestion in vivo: down-regulation of the expression of creatine transporter isoforms in skeletal muscle. Mol Cell Biochem 184:427–437
Haraldseth O, Gronas T, Southon TE, Jynge P, Gisvold SE, Unsgard G (1990) The NMDA antagonist MK-801 improved metabolic recovery after 10 minutes global cerebral ischaemia in rats measured with 31 phosphorous magnetic resonance spectroscopy. Acta Neurochir (Wien) 106:32–36
Harkin AJ, Bruce KH, Craft B, Paul IA (1999) Nitric oxide synthase inhibitors have antidepressant-like properties in mice. 1. Acute treatments are active in the forced swim test. Eur J Pharmacol 372:207–213
Harkin A, Connor TJ, Walsh M, St John N, Kelly JP (2003) Serotonergic mediation of the antidepressant-like effects of nitric oxide synthase inhibitors. Neuropharmacology 44:616–623
Hashimoto K, Sawa A, Iyo M (2007) Increased levels of glutamate in brains from patients with mood disorders. Biol Psychiatry 62:1310–1316
Heiberg IL, Wegener G, Rosenberg R (2002) Reduction of cGMP and nitric oxide has antidepressant-like effects in the forced swimming test in rats. Behav Brain Res 134:479–484
Heinzen EL, Pollack GM (2002) Use of an electrochemical nitric oxide sensor to detect neuronal nitric oxide production in conscious, unrestrained rats. J Pharmacol Toxicol Methods 48:139-146
Herring NR, Schaefer TL, Tang PH, Skelton MR, Lucot JP, Gudelsky GA et al (2008) Comparison of time-dependent effects of (+)-methamphetamine or forced swim on monoamines, corticosterone, glucose, creatine, and creatinine in rats. BMC Neurosci 9:49
Hevel JM, Marletta MA (1994) Nitric-oxide synthase assays. Methods Enzymol 233:250–258
Hua Y, Huang XY, Zhou L, Zhou QG, Hu Y, Luo CX et al (2008) DETA/NONOate, a nitric oxide donor, produces antidepressant effects by promoting hippocampal neurogenesis. Psychopharmacology 200:231–242
Iijima M, Fukumoto K, Chaki S (2012) Acute and sustained effects of a metabotropic glutamate 5 receptor antagonist in the novelty-suppressed feeding test. Behav Brain Res 235(2):287–292
Inan SY, Yalcin I, Aksu F (2004) Dual effects of nitric oxide in the mouse forced swimming test: possible contribution of nitric oxide-mediated serotonin release and potassium channel modulation. Pharmacol Biochem Behav 77:457–464
Joca SR, Guimarães FS (2006) Inhibition of neuronal nitric oxide synthase in the rat hippocampus induces antidepressant-like effects. Psychopharmacology 185:298–305
Juravleva E, Barbakadze T, Natsvlishvili N, Kekelidze T, Mikeladze D (2003) Creatine prevents the cytotoxicity of haloperidol by alteration of NO/Ras/NF-κB system. In: Kekelidze T, Holtzman D (eds) Creatine kinase and brain energy metabolism: function and disease. NATO science series: life and behavioral science, vol 343. IOS Press, Amsterdam, pp 113–119
Juravleva E, Barbakadze T, Mikeladze D, Kekelidze T (2005) Creatine enhances survival of glutamate-treated neuronal/glial cells, modulates Ras/NF-kappaB signaling, and increases the generation of reactive oxygen species. J Neurosci Res 79:224–230
Kaster MP, Rosa AO, Santos AR, Rodrigues AL (2005) Involvement of nitric oxide-cGMP pathway in the antidepressant-like effects of adenosine in the forced swimming test. Int J Neuropsychopharmacol 8:601–606
Kaster MP, Machado DG, Santos AR (2012) Rodrigues AL (2012) Involvement of NMDA receptors in the antidepressant-like action of adenosine. Pharmacol Rep 64:706–713
Kato T, Takahashi S, Shioiri T, Inubushi T (1992) Brain phosphorous metabolism in depressive disorders detected by phosphorus-31 magnetic resonance spectroscopy. J Affect Disord 26:223–230
Kawasaki H, Nohtomi A, Nakahara T, Itoh M, Tashiro N (2001) Identification of creatine as an endogenous inhibitor of [3H] flunitrazepam binding. Society for Neuroscience, San Diego
Kim SY, Lee YJ, Kim H, Lee DW, Woo DC, Choi CB et al (2010) Desipramine attenuates forced swim test-induced behavioral and neurochemical alterations in mice: an in vivo (1)H-MRS study at 9.4T. Brain Res 1348:105–113
Knox D, Perrine SA, George SA, Galloway MP, Liberzon I (2010) Single prolonged stress decreases glutamate, glutamine, and creatine concentrations in the rat medial prefrontal cortex. Neurosci Lett 480:16–20
Koike H, Iijima M, Chaki S (2011) Involvement of AMPA receptor in both the rapid and sustained antidepressant-like effects of ketamine in animal models of depression. Behav Brain Res 224:107–111
Kondo DG, Sung YH, Hellem TL, Fiedler KK, Shi X, Jeong EK et al (2011) Open-label adjunctive creatine for female adolescents with SSRI-resistant major depressive disorder: a 31-phosphorus magnetic resonance spectroscopy study. J Affect Disord 135:354–361
Krass M, Wegener G, Vasar E, Volke V (2011) The antidepressant action of imipramine and venlafaxine involves suppression of nitric oxide synthesis. Behav Brain Res 218:57–63
Krystal JH, Sanacora G, Duman RS (2013) Rapid-acting glutamatergic antidepressants: the path to ketamine and beyond. Biol Psychiatry 73:1133–1141
Laursen SE, Belknap JK (1986) Intracerebroventricular injections in mice. Some methodological refinements. J Pharmacol Methods 16:355–357
Lei SZ, Pan ZH, Aggarwal SK, Chen HS, Hartman J, Sucher NJ et al (1992) Effect of nitric oxide production on the redox modulatory site of the NMDA receptor-channel complex. Neuron 8:1087–1099
Li N, Liu RJ, Dwyer JM, Banasr M, Lee B, Son H et al (2011) Glutamate N-methyl-D-aspartate receptor antagonists rapidly reverse behavioral and synaptic deficits caused by chronic stress exposure. Biol Psychiatry 69:754–761
Lipton SA, Rayudu PV, Choi YB, Sucher NJ, Chen HS (1998) Redox modulation of the NMDA receptor by NO-related species. Prog Brain Res 118:73–82
Lonart G, Wang J, Johnson KM (1992) Nitric oxide induces neurotransmitter release from hippocampal slices. Eur J Pharmacol 220:271–272
Lorrain DS, Hull EM (1993) Nitric oxide increases dopamine and serotonin release in the medial preoptic area. Neuro Rep 5:87–89
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Ludka FK, Zomkowski AD, Cunha MP, Dal-Cim T, Zeni AL, Rodrigues AL et al (2013) Acute atorvastatin treatment exerts antidepressant-like effect in mice via the l-arginine-nitric oxide-cyclic guanosine monophosphate pathway and increases BDNF levels. Eur Neuropsychopharmacol 23:400–412
Lugenbiel P, Sartorius A, Vollmayr B, Schloss P (2010) Creatine transporter expression after antidepressant therapy in rats bred for learned helplessness. World J Biol Psychiatry 11:329–333
Lyoo IK, Yoon S, Kim TS, Hwang J, Kim JE, Won W et al (2012) A randomized, double-blind placebo-controlled trial of oral creatine monohydrate augmentation for enhanced response to a selective serotonin reuptake inhibitor in women with major depressive disorder. Am J Psychiatry 169:937–945
Machado DG, Cunha MP, Neis VB, Balen GO, Colla A, Grando J, Brocardo PS, Bettio LE, Capra JC, Rodrigues AL (2012) Fluoxetine reverses depressive-like behaviors and increases hippocampal acetylcholinesterase activity induced by olfactory bulbectomy. Pharmacol Biochem Behav 103:220–229
Mantovani M, Pértile R, Calixto JB, Santos AR, Rodrigues AL (2003) Melatonin exerts antidepressant-like effect in the tail suspension test in mice: evidence for involvement of N-methyl-D-aspartate receptors and the l-arginine-nitric oxide pathway. Neurosci Lett 343:1–4
Manzoni O, Prezeau L, Marin P, Deshager S, Bockaert J, Fagni L (1992) Nitric oxide-induced blockade of NMDA receptors. Neuron 8:653–662
Moghaddam B, Adams B, Verma A, Daly D (1997) Activation of glutamatergic neurotransmission by ketamine: a novel step in the pathway from NMDA receptor blockade to dopaminergic and cognitive disruptions associated with the prefrontal cortex. J Neurosci 17:2921–2927
Molz S, Decker H, Dal-Cim T, Cremonez C, Cordova FM, Leal RB et al (2008) Glutamate-induced toxicity in hippocampal slices involves apoptotic features and p38 MAPK signaling. Neurochem Res 33:27–36
Moretti M, Freitas AE, Budni J, Fernandes SC, Balen Gde O, Rodrigues AL (2011) Involvement of nitric oxide-cGMP pathway in the antidepressant-like effect of ascorbic acid in the tail suspension test. Behav Brain Res 225:328–333
Moretti M, Budni J, Ribeiro CM, Rodrigues AL (2012) Involvement of different types of potassium channels in the antidepressant-like effect of ascorbic acid in the mouse tail suspension test. Eur J Pharmacol 687:21–27
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65:55–63
Nikonenko I, Boda B, Steen S, Knott G, Welker E, Muller D (2008) PSD-95 promotes synaptogenesis and multiinnervated spine formation through nitric oxide signaling. J Cell Biol 183:1115–1127
Nowak G, Ordway GA, Paul IA (1995) Alterations in the N-methyl-D-aspartate (NMDA) receptor complex in the frontal cortex of suicide victims. Brain Res 675:157–164
Oliveira MS, Furian AF, Fighera MR, Fiorenza NG, Ferreira J, Rubin MA et al (2008) The involvement of the polyamines binding sites at the NMDA receptor in creatine-induced spatial learning enhancement. Behav Brain Res 187:200–204
Papouin T, Ladepeche L, Ruel J, Sacchi S, Labasque M, Hanini M et al (2012) Synaptic and extrasynaptic NMDA receptors are gated by different endogenous coagonists. Cell 150:633–646
Parodi M, Rebaudo R, Perasso L, Gandolfo C, Cupello A, Balestrino M (2003) Effects of exogenous creatine on population spike amplitude and on postanoxic hyperexcitability in brain slices. Brain Res 963:197–202
Poleszak E, Szewczyk B, Wlaz A, Fidecka S, Wlaz P, Pilc A et al (2008) D-serine, a selective glycine/N-methyl-D-aspartate receptor agonist, antagonizes the antidepressant-like effects of magnesium and zinc in mice. Pharmacolog Rep 60:996–1000
Raley KM, Lipton P (1990) NMDA receptor activation accelerates ischemic energy depletion in the hippocampal slice and the demonstration of a threshold for ischemic damage to protein synthesis. Neurosci Lett 110:118–123
Reus GZ, Stringari RB, Rezin GT, Fraga DB, Daufenbach JF, Scaini G et al (2012) Administration of memantine and imipramine alters mitochondrial respiratory chain and creatine kinase activities in rat brain. J Neural Transm 119:481–491
Rieger DK, Costa AP, Budni J, Moretti M, Barbosa SG, Nascimento KS, Teixeira EH, Cavada BS, Rodrigues AL, Leal RB (2014) Antidepressant-like effect of Canavalia brasiliensis (ConBr) lectin in mice: evidence for the involvement of the glutamatergic system. Pharmacol Biochem Behav 122:53–60
Rodrigues AL, Rosa JM, Gadotti VM, Goulart EC, Santos MM, Silva AV, Sehnem B, Rosa LS, Gonçalves RM, Corrêa R, Santos AR (2005) Antidepressant-like and antinociceptive-like actions of 4-(4′-chlorophenyl)-6-(4′’-methylphenyl)-2-hydrazinepyrimidine Mannich base in mice. Pharmacol Biochem Behav 82:156–162
Romero TR, Galdino GS, Silva GC, Resende LC, Perez AC, Cortes SF et al (2011) Ketamine activates the l-arginine/Nitric oxide/cyclic guanosine monophosphate pathway to induce peripheral antinociception in rats. Anesth Analg 113:1254–1259
Rosa AO, Lin J, Calixto JB, Santos AR, Rodrigues AL (2003) Involvement of NMDA receptors and l-arginine-nitric oxide pathway in the antidepressant-like effects of zinc in mice. Behavioral Brain Res 144:87–93
Royes LF, Fighera MR, Furian AF, Oliveira MS, Fiorenza NG, Ferreira J et al (2008) Neuromodulatory effect of creatine on extracellular action potentials in rat hippocampus: role of NMDA receptors. Neurochem Int 53:33–37
Sanacora G, Zarate CA, Krystal JH, Manji HK (2008) Targeting the glutamatergic system to develop novel, improved therapeutics for mood disorders. Nat Rev Drug Discov 7:426–437
Satoh S, Murayama T, Nomura Y (1996) Sodium nitroprusside stimulates noradrenaline release from rat hippocampal slices in the presence of dithiothreitol. Brain Res 733:167–174
Segieth J, Pearce B, Fowler L, Whitton PS (2001) Regulatory role of nitric oxide over hippocampal 5-HT release in vivo. Naunyn-Schmiedeberg’s Arch Pharmacol 363:302–306
Sharp JW, Petersen DL, Langford MT (1995) DNQX inhibits phencyclidine (PCP) and ketamine induction of the hsp70 heat shock gene in the rat cingulate and retrosplenial cortex. Brain Res 687:114–124
Skolnick P (1999) Antidepressants for the new millennium. Eur J Pharmacol 375:31–40
Somjen GG, Aitken PG, Balestrino M, Schiff SJ (1987) Uses and abuses of in vitro systems in the study of the pathophysiology of the central nervous system. In: Schurr A, Teyler TJ, Tseng MT (eds) Brain slices in the study of brain damage. Karger, Basel, pp 89–104
Spandou E, Karkavelas G, Soubasi V, Avgovstides-Savvopoulou P, Loizidis T, Guiba-Tziampiri O (1999) Effect of ketamine on hypoxic-ischemic brain damage in newborn rats. Brain Res 819:1–7
Spiacci A Jr, Kanamaru F, Guimaraes FS, Oliveira RM (2008) Nitric oxide-mediated anxiolytic-like and antidepressant-like effects in animal models of anxiety and depression. Pharmacol Biochem Behav 88:247–255
Steru L, Chermat R, Thierry B, Simon P (1985) The tail suspension test: a new method for screening antidepressants in mice. Psychopharmacology 85:367–370
Suzuki E, Yagi G, Nakaki T, Kanba S, Asai M (2001) Elevated plasma nitrate levels in depressive states. J Affect Disord 63:221–224
Volke V, Wegener G, Bourin M, Vasar E (2003) Antidepressant- and anxiolytic-like effects of selective neuronal NOS inhibitor 1-(2-trifluoromethylphenyl)-imidazole in mice. Behav Brain Res 140:141–147
Wlaź P, Kasperek R, Wlaź A, Szumiło M, Wróbel A, Nowak G, Poleszak E (2011) NMDA and AMPA receptors are involved in the antidepressant-like activity of tianeptine in the forced swim test in mice. Pharmacol Rep 63:1526–1532
Wu J, Kikuchi T, Wang Y, Sato K, Okumura F (2000) NOx concentrations in the rat hippocampus and striatum have no direct relationship to anaesthesia induced by ketamine. Br J Anaesth 84:183–189
Yamamoto M, Koshimura K, Sohmiya M, Murakami Y, Kato Y (2004) Effect of erythropoietin on nitric oxide production in the rat hippocampus using in vivo brain microdialysis. Neuroscience 128:163–168
Young LT (2002) Neuroprotective effects of antidepressant and mood stabilizing drugs. J Psychiatry Neurosci 27:8–9
Yuan TT, Qiao H, Dong SP, An SC (2011) Activation of hippocampal D1 dopamine receptor inhibits glutamate-mediated depression induced by chronic unpredictable mild stress in rats. Sheng Li Xue Bao (Acta Physiologica Sinica) 63:333–341
Zeni AL, Zomkowski AD, Dal-Cim T, Maraschin M, Rodrigues AL, Tasca CI (2011) Antidepressant-like and neuroprotective effects of Aloysia gratissima: investigation of involvement of l-arginine-nitric oxide-cyclic guanosine monophosphate pathway. J Ethnopharmacol 137:864–874
Zomkowski AD, Santos AR, Rodrigues AL (2006) Putrescine produces antidepressant-like effects in the forced swimming test and in the tail suspension test in mice. Prog Neuropsychopharmacol Biol Psychiatry 30:1419–1425
Zomkowski AD, Engel D, Gabilan NH, Rodrigues AL (2010) Involvement of NMDA receptors and l-arginine-nitric oxide-cyclic guanosine monophosphate pathway in the antidepressant-like effects of escitalopram in the forced swimming test. Eur Neuropsychopharmacol 20:793–801
Zomkowski AD, Engel D, Cunha MP, Gabilan NH, Rodrigues AL (2012) The role of the NMDA receptors and l-arginine-nitric oxide-cyclic guanosine monophosphate pathway in the antidepressant-like effect of duloxetine in the forced swimming test. Pharmacol Biochem Behav 103:408–417
Zhou W, Wang N, Yang C, Li XM, Zhou ZQ, Yang JJ (2014) Ketamine-induced antidepressant effects are associated with AMPA receptors-mediated upregulation of mTOR and BDNF in rat hippocampus and prefrontal cortex. Eur Psychiatry 29:419–423
Acknowledgments
This study was supported by grants from the Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Coordenação de Aperfeiçoamento de Pessoal de Ensino Superior (CAPES), Fundação de Apoio a Pesquisa Científica e Tecnológica do Estado de Santa Catarina (FAPESC), Rede Instituto Brasileiro de Neurociência (IBN-Net/CNPq), Núcleo de Excelência em Neurociências Aplicadas de Santa Catarina (NENASC) Project/PRONEX Program (CNPq/FAPESC).
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Handling Editor: V. Bolshakov.
Rights and permissions
About this article
Cite this article
Cunha, M.P., Pazini, F.L., Ludka, F.K. et al. The modulation of NMDA receptors and l-arginine/nitric oxide pathway is implicated in the anti-immobility effect of creatine in the tail suspension test. Amino Acids 47, 795–811 (2015). https://doi.org/10.1007/s00726-014-1910-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-014-1910-0