Preface
This is the third special issue focused on “Transglutaminases” that is now available on this journal and dedicated to one of the pioneers of these enzymes, John Edward Folk, who died December 2010 [see in this issue Beninati et al. 2012a]. The first edition, “Polyamines and Transglutaminases” was published in Amino Acids, vol 26, no. 4, 2004, with the contribution of two prestigious Guest Editors as Alberto Abbruzzese and Mauro Piacentini. This editorial initiative was followed by the second special issue published in occasion of the 50th years of the discovery of transglutaminase. Indeed, “Transglutaminase 2: 50th Anniversary of the Discovery” Amino Acids, vol 36, no. 4, 2009, was published with the valuable collaboration of Carlo Maria Bergamini and Mauro Piacentini (Beninati et al. 2009). To continue with this editorial tradition, on this occasion, an outstanding board of Guest Editors composed by Francesco Facchiano and Mauro Piacentini has also been invited to promote this initiative and recruit a selected panel of Authors, many of who participated in the first and second edition of the Gordon Conference on Transglutaminases: “Transglutaminases in Human Diseases Processes” chaired by Rickard L Eckert and Kapil Mehta on July 18–23, 2010, and by Kapil Mehta and Mauro Piacentini on July 15–20, 2012, held at Davidson College, NC, USA. In this Amino Acids special issue, the manuscripts were selected to reflect the progress and the future perspectives of transglutaminases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Editorial
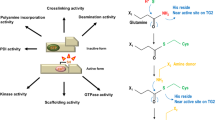
Transglutaminase (TG) was identified as a liver enzyme incorporating amines into proteins by Heinrich Waelsch (Sarkar et al. 1957). The presence of an acyl-enzyme thioester intermediate between an active site cysteine and a polypeptide-bound glutamine and the further reaction of the thioester intermediate with a suitable nucleophile is the base of the enzymatic mechanism (Folk and Cole 1966). In vertebrates, nine evolutionary-related genes encoding FXIIIa, TG1–7 and epb42, a structural protein, which lacks catalytic activity, have evolved by successive duplications. A remarkable degree of sequence similarity is revealed by the alignment of the gene products. A similar gene organization is shown by all family members, with conservation of intron distribution and intron splice types (Grenard et al. 2001). Of the eight catalytic TGs, TG2 has been the most comprehensively studied due to its ubiquitous expression in multiple cell types, engaged in various biochemical functions. TG2 is responsible for different related protein post-translational modifications such as incorporation of di- and polyamines into proteins (Folk et al. 1980), protein–protein cross-linking and when one substrate is a water molecule instead of an amine a site-specific deamidation (Lorand and Graham 2003). The enzyme can be exposed on the external layer of the plasma membrane or released outside the cells, where it has been shown to mediate the interaction between integrins and fibronectin and the extracellular matrix (ECM), without the involvement of its transamidating activity. The absence of catalytic activity of intracellular and extracellular TG2 is not surprising, given the allosteric effects of Ca+2 and GTP/GDP, and the demonstrated role of TG2 as a G-protein inside the cell (Lorand and Graham 2003). Integrins have been found to play an important part in mediating cell-signaling events by regulating the binding of growth factors or cytokines to growth factor receptors, including a large number of tyrosine kinase receptors (RTKs) (Legate et al. 2009). Receptors from this family are of key interest in the investigation of stem cell growth and differentiation (Arai et al. 2004) and drug resistance and metastasis of cancers (Hollier et al. 2008; Kashyap et al. 2011).
The first evidence of a direct TG-mediated interaction between an RTK and an integrin came from the observation that factor XIIIa activates the VEGFR2 in a growth factor-independent fashion by cross-linking the receptor to the αvβ3 integrin and enhancing vascular endothelial cell migration, proliferation and survival (Dardik et al. 2005). Expanding interest toward discovery of the relationship between RTKs and TGs will enable us to improve our knowledge of the pattern of TG-mediated interactions under various disease states. Increasing evidence directed to how TGs and RTKs work together raises possibilities of how this could act as a fundamental mediator of the eukaryotic signaling and trafficking system (Sivaramakrishnan et al. 2011).
Several evidence have been found on additional physiological or pathological functions that TG2 may affect. These include irreversible membrane stiffening of erythrocytes (Siefring et al. 1978), opacification of eye lens (Lentini et al. 2011), modulation of neurotransmitter release (Facchiano et al. 2010), receptor-mediated endocytosis (Abe et al. 2000), regulation of cell growth and differentiation (Nurminskaya and Belkin 2012), metastasis, cardiovascular and neurodegenerative diseases (Tabolacci et al. 2012), programmed cell death, autophagy (Fimia and Piacentini 2010) and celiac disease (Sollid and Jabri 2011). Moreover, a significant role of TGs and their numerous substrates in human diseases has also been reviewed (Facchiano and Facchiano 2009) as well as thoroughly discussed at the Gordon Research Conference entitled “Transglutaminases in Human Disease Processes” (July 18–23, 2010, Davidson College Davidson, NC) Chaired by Richard L. Eckert and Kapil Mehta. This volume contains a selection of original contributions presented as reviews and original papers, illustrating the present challenges in this area of research.
Depending on the cell type and its localization within the cell, TG2 can act as an anti-apoptotic or a pro-apoptotic protein. In general, the presence of high levels of Ca2+ induces its transamidating activity, which promotes inter- and intramolecular cross-linking of proteins resulting in cell death. In contrast, low levels of Ca2+ and a high concentration of GTP promotes TG2-mediated cell survival signaling (Chhabra et al. 2009). TG2 exerts its anti-apoptotic effects through different mechanisms involving both its transamidation and GTP-binding activities. For instance, TG2-induced protein cross-linking protects cells from caspase cleavage and promotes NFκB-dependent cell survival (Verma and Mehta 2007; Jang et al. 2010). Moreover, TG2-mediated transamidation of tumor suppressor protein p110 Rb in the nucleus protects this oncogenic protein from degradation, thereby promoting survival (Boehm et al. 2002). Furthermore, the association of TG2 with some members of the integrins family promotes the anchoring of cells to the ECM and activates cell survival pathways (Akimov et al. 2000; Mangala et al. 2007). These often contradictory cellular functions attributed to TG2 are puzzling, and they raise questions regarding how its transamidation activity might account for such opposing biological outcomes, as cell survival versus apoptosis. More surprising, however, is the observation that extracellular TG2 is catalytically inactive under ordinary physiological conditions (Griffin et al. 2002), and its role is independent on the catalytic activity in cell adhesion, spreading, migration or differentiation (Zemskov et al. 2006). Recent reports may clarify these divergent functions (Pinkas et al. 2007; Lentini et al. 2012). Intracellular and extracellular TG2 are predominantly in a closed conformation in a normal stress-free environment. The enzymes are maintained in the closed conformation as a result of guanine nucleotide and/or integrin binding, despite relatively high extracellular Ca+2 concentrations. Physical or certain forms of chemical injury trigger rapid activation of TG2 into its catalytically active, open conformation (Pinkas et al. 2007). These observations provide structural support for the kinetic analysis of both guinea pig liver TG2 and human factor XIIIa performed by Folk (1983) who presupposed the transient formation of a tunnel in the active site during acylation. Another possibility that could explain some of the discrepancies involves alternative processing of the TG transcript. In fact, several groups have reported the identification of a novel TG2 RNA transcript whose expression can be induced in cells by cytokines and is detected in the brains of Alzheimer’s patients (Citron et al. 2001), which does not contain the long 3′-untranslated region and encodes for a novel TG2 enzyme whose C terminus lacks a site that affects the enzyme’s interaction with GTP. Expression of two clones revealed that the long form (TG-L) is inhibited non-competitively by GTP, but the short form (TG-S) significantly less so. The different affinities for GTP may account for the difference in physiological function between these two enzymes. Furthermore, TG-S exerts diametrically opposite effects on cell viability compared with its full-length counterpart, because the latter protein confers a strong survival advantage to cells, whereas TG-S is apoptotic (Antonyak et al. 2006). The binding of GTP or Ca2+ inhibits, respectively, the transamidation and GTPase functions of TG2, which are mutually exclusive enzymatic activities in vivo (Monsonego et al. 1997). Although a significant correlation in expression of canonical and alternative TG2 isoforms in normal human tissue was observed, in cancer cell line, the alternative splicing of TG2 is a more active process (Phatak et al. 2011). TG2 expression has been found increased in several tumors, where it was considered a potential negative prognostic marker, and it is often associated with advanced stages of the disease, metastatic spread and drug resistance. TG2 expression and activity display a different role in primary or in metastatic cells. TG2 expression is low in the primary mass, but augmented when cell acquire a metastatic phenotype, suggesting that this enzyme is a key regulator of cancer metastasis (Lentini et al. 2012). Differentiation therapy is an important and rapidly evolving aspect in cancer research. It is based on the concept that drugs and natural substances can inhibit carcinogenesis and development of tumors through the induction of cellular terminal differentiation (Thiele et al. 2000), avoiding the typical cytotoxicity of currently used chemotherapeutic agents. Cell differentiation correlated with a remarkable increase in the activity of the transamidating form of TG2, with a significative enhancement of cell adhesion and aggregation (Lentini et al. 2008).
Androgen-independent human prostate PC-3 cell line as a target and α- and γ-tocopherol as potential inducers of differentiation were investigated (Torricelli et al. 2011). A decreased progression into the S-phase was observed for α- and γ-tocopherol-treated prostate carcinoma PC3 cells. This effect, particularly evident for γ-tocopherol, was associated with an up-regulation and increased expression and activity of TG2, a reduced DNA synthesis and a remarkable decreased levels of cyclin D1 and cyclin E.
To seize the meaning of TG2 role in cancer, an in vivo study with a more direct approach is presented by Facchiano et al. (2012). TG2 was in vivo overexpressed in a murine model of melanoma, by means of a plasmid carrying the TG2 cDNA. The evaluation of the frequency and size of the metastases indicated that the number of melanoma lung foci was more markedly reduced by TG2 overexpression than the metastatic size. Furthermore, TG2 overexpressing mice showed a prolonged survival with respect to control mice. These findings suggest a protective role of TG2 enzymatic activity in melanoma progression in vivo.
TG2 has emerged as a putative gene involved in cells drug résistance and evasion of apoptosis. Acquired résistance to anticancer treatments is a substantial barrier to reducing the morbidity and mortality that is attributable to malignant tumors. TG2 mediates cell drug résistance through the activation of survival pathways and the inhibition of apoptosis, but also by regulating ECM formation, the epithelial to mesenchymal transition (EMT) or autophagy (Budillon et al. 2011). Although inhibition of TG2 expression may reverse drug resistance and induce apoptosis in cancer cells (Budillon et al. 2011), many other factors should be considered. TG2 has recently been shown to activate nuclear factor-jB (NF-jB) in a non-canonical way, through the depletion of the inhibitory subunit of NF-jB (I-jBa) via protein cross-linking, which extends the period of NF-jB activity during inflammation (Park et al. 2006). Therefore, increased expression of TG2 contributes to inflammatory disease pathogenesis via constitutive NF-jB activation. Conversely, TG2 inhibition often reverses inflammation in animal models. Kim et al. (2011) report that TG2 was found cross-linked with cathepsin D (CTD). Binding of TG2 to CTD resulted in the depletion of this aspartic protease via cross-linking in vitro as well as in mouse embryonic fibroblasts, leading to decreased levels of apoptosis. Authors conclude that TG2 may regulate the balance between cell survival and cell death through the modulation of CTD levels. Kumar and Mehta (2011) recently found that aberrant tissue TG2 expression induces the EMT and stem cell characteristics in epithelial cells. This finding, in conjunction with the observation that inflammatory signals (e.g., TGFβ, TNFα and NF-κB) which induce EMT, also induce TG2 expression, suggests a possible link between TG2, inflammation and cancer progression. In this context, we have to take into account that components of tissue microenvironments are recognized to profoundly influence cellular phenotypes, including susceptibilities to toxic insults. It was recently reported that the effects of cytotoxic chemotherapy in vivo was reduced by the expression of WNT16B in the prostate microenvironment, promoting cell survival and disease progression (Sun et al. 2012).
Tumor angiogenic activity is the capability of tumor cells to stimulate neoangiogenesis (Giatromanolaki et al. 2004). During angiogenic process, endothelial cells, in response to key growth factors, such as vascular endothelial growth factor and fibroblast growth factor, form tubular structures, which grow toward and colonize the growing tumors. Although originally thought that the vasculogenesis of tumors could only occur via the growth of surrounding blood vessels into the tumor, it has recently been shown that the vascular structures of some tumor has a neoplastic origin (Ricci-Vitiani et al. 2010) and share comparable genomic features with the neoplastic cells themselves. These tumor-derived vascular structures, referred to as vasculogenic mimicry (Bissell 1999), are able to join up with the normal endothelial-derived surrounding blood vessels to provide a highly vascularized tumor. One protein shown to be linked to endothelial cell–derived angiogenesis is TG2 (Griffin et al. 2002). The roles of TG2 in tube formation are directed toward the outside of the cell and are dependent on its transamidating ability in both matrix deposition and cell migration. Inhibition of TG2 activity may therefore offer itself as an alternative therapeutic target in blocking aggressive tumor growth and progression where vasculogenic mimicry is found (Jones et al. 2012).
A new aspect of TG2 in cancer research is the potential oncogenic and prognostic significance of the eukaryotic translation initiation factor 5A (eIF-5A), the only cell protein that contains the unusual basic amino acid hypusine [N ε-(4-amino-2-hydroxybutyl) lysine]. eIF-5A from human erythrocytes was found to be a substrate for both plasma Factor XIIIa and guinea pig liver TG2 (Beninati et al. 1995). TG2 affects hypusine metabolism, thus regulating the eIF-5A activity and cell proliferation (Beninati et al. 1998). These data strongly suggested that the post-translational modifications of eIF-5A could be a suitable target for anticancer agents (Caraglia et al. 1999). In this issue, Caraglia et al. (2011) focused their review on the role of hypusine formation in the eIF-5A protein isoforms in the regulation of cell proliferation and apoptosis in cancer.
Although several investigations suggest a role for TG in the pathogenesis of neurodegenerative diseases, conclusive experimental findings have not yet been obtained. A potential role for polyamines and TGs in memory mechanisms has been proposed (Tiboldi et al. 2012). These studies are in progress and knowledge on interaction between polyamines and TG report for the first time that γ-glutamyl-spermine and transamidating activity of TG that may form the basis for future neurochemical and pharmacological studies. The role of TG2-catalyzed reactions in the physiopathology of neurodegeneration disorders is extensively discussed in the review by Martin et al. (2011). They re-examine the possible molecular mechanism by which transamidating TG could be involved in the pathogenesis of neurodegenerative diseases, such as Alzheimer, Parkinson, supranuclear palsy and Huntington. Badarau et al. (2011) suggest the use of selective inhibitors for TG2 both cell penetrating and non-cell penetrating as a novel therapeutic tools for the treatment of neurological diseases. Jeitner and coworkers (2008, 2009) presupposed that TG-derived γ-glutamylamines may play a more significant role in neurodegeneration. Indeed, aggregation of particular proteins in the brain is thought to be a contributing factor in a number of important neurodegenerative disorders. This assumption suggests a reciprocal association between amounts of cerebral polyamines and insoluble aggregates as the brain ages. Polyamine levels in the brain decreases with age, increasing the amount of γ-glutamyl-ε-lysine linkages in CNS proteins (Liu et al. 2008). The ratio of bis- γ-glutamylpolyamines to γ-glutamyl-ε-lysine linkages in polymerized protein affects the solubility of these aggregates. The same proteins can be polymerized into insoluble agglomerate cross-linked by bis- γ-glutamylpolyamine bonds or larger precipitates held together by a combination of hydrophobic interactions and γ-glutamyl-ε-lysine bonds (Jeitner et al. 2012). More evidence on the role of γ-glutamylamine cyclotransferase (gGACT) an enzyme able to catalyze γ-glutamylamines should improve our understanding on the role of these TG derivatives in neurodegenerative diseases. The article of Bowser and Trawick (2011) give a good contribution to this subject. gGACT catalyzes the intramolecular cyclization of a variety of l-γ-glutamylamines producing 5-oxo-l-proline and free amines (Fink and Folk 1981). In order to elucidate the mechanism by which gGACT distinguishes between l-γ-glutamylamine and amino acid substrates, Authors probed, through the kinetic analysis of a series of l-γ-glutamylamines, the specificity of the rabbit kidney enzyme for the amide region of substrates.
The NMDA (N-methyl-d-aspartate) receptor (NMDAR), a glutamate receptor, is the predominant molecular device for controlling synaptic plasticity and memory function (Li and Tsien 2009). NMDA is the name of a selective agonist that binds to NMDAR but not to other glutamate receptors. Data presented by Caccamo et al. (2011) suggest that TG2 might be protective against NMDA-evoked excitotoxic insult in neuronal-like SH-SY5Y cells, in a way independent from transamidation. Abundant expression of at least two TG isozymes, TG1 and TG3, in the CNS has been previously reported (Kim et al. 1999). In this special issue, Thomas and coworkers (2011) show an enhanced expression of TG6 in CNS of mouse. Analysis of its temporal and spatial pattern of induction, in mouse development, indicates an association with neurogenesis. Authors concluded that given that TG6 similar to TG2 is a protein that can be detected in the cell cytosol, as well as at the cell surface, it may have independent intra- and extracellular functions that may employ the enzymes ability to bind GTP or act as a Ca2+-dependent cross-linking enzyme, respectively.
In order to investigate the in vivo function of TG2, two mouse knockout models were developed by different groups ( De Laurenzi and Melino 2001; Nanda et al. 2001). Despite the observed in vitro role for TG2 in several biological processes, no obvious developmental defects were observed in either of these mouse models. These phenotypes suggested the common biological phenomenon of backup compensation, which occurs when functionally overlapping proteins compensate for the loss of each other. The original article presented by Deasey et al. (2011) shows evidence on a tissue-specific mechanism of compensation for the loss of TG2, including transcriptional compensation in heart and liver versus functional compensation in aorta. On the contrary, no compensation has been shown in skeletal muscle, suggesting a limited role for the TG2-mediated transamidation in normal development of this tissue.
Understanding the role of TG2 in sepsis is crucial due to the development of TG2 inhibitors for use in treating chronic inflammatory diseases or cancer. TNF-α, a pro-inflammatory cytokine, induces systemic inflammation, which is characterized by hemodynamic shock and liver toxicity. Acute liver failure commonly occurs due to increased production of chemokines and TNF-α by macrophages (Muto et al. 1988). Yoo et al. (2012) report that the outcomes of different septic shock models were totally opposite in TG2 knockout mice. Indeed, the effects of septic shock observed in TG2−/− mice are dependent on the source of the septic shock, and hepatocytes and macrophages are affected. They conclude that great care must be taken when selecting therapeutic agents that inhibit TG2, particularly with regard to their potential to cause liver damage.
Over the years, osteoblasts and chondrocytes have been shown to express both TG2 and FXIII (Nurminskaya and Kaartinen 2006). Investigations have been performed to elucidate the significance of TGs in bone formation (Kaartinen et al. 2002; Forsprecher et al. 2009). Increased TG2 expression is observed in human and experimental osteoarthritis. Tarantino and coworkers (2011) suggest that the level of TG2 expression may represent an additional marker to monitor tissue remodeling occurring in osteoarthritic joint tissue.
MC3T3-E1, a mouse calvaria-derived cell line, is a useful in vitro model system for studying the process of osteoblastic differentiation, because this cell line displays a temporal sequence of development similar to in vivo bone formation (Quarles et al. 1992). FXIII and TG2 have been expressed in differentiating MC3T3-E1 cells, where FXIII is induced depending on differentiation and TG2 is constitutively expressed (Al-Jallad et al. 2006). The intracellular substrates for TGs cross-linking activity are still under investigation. Watanabe et al. (2011) attempted to identify possible distinct substrates for FXIII and TG2 in differentiating MC3T3-E1 cells. They established a system in which two isozymes co-existed for the identification of isozyme-specific substrate proteins in cells. Several intracellular and extracellular substrate proteins were identified from the differentiating osteoblastic cell lines. Further investigation into the cross-linking pattern of these proteins and their contribution to cell functions and matrix formation and mineralization are ongoing and might be further improved by applying the internet resources (http://bioinformatica.isa.cnr.it/TRANSIT/) specifically developed to make easier the study of TGs substrates (Facchiano et al. 2003).
Analysis of the available genomic databases clearly shows that the protein coding sequence of human TG2 has very low polymorphism in the population, and it has the lowest variability when compared to other members of the human TGs family. Király et al. (2011) collected data on and produced some of the rare genetic variants of TGM2 by site directed mutagenesis and found that some were less stable than the most abundant (wild-type) enzyme variant, and the majority had deficient transamidating activity.
Since troponins are clinically relevant markers of muscular and cardiac cell dysfunction (Panteghini 2009), the observation that this protein is post-translational modified by TG2, in subunit T of the native rabbit skeletal muscle troponin complex (Bergamini et al. 1995) is of clinical interest. However, McDonough et al. (1999) reported that also TnI is cross-linked by TG2 to the C-terminal (190–275) proteolytic fragment of TnT, and the derived aggregates are released in heart perfusates following infarction/reperfusion injury. In order to clarify these discrepancies, Squerzanti et al. (2011) investigated the role of Glutamine 13 residue and found that this is the precise site of labeling occurring only at subunit T of troponin.
The existence of retinoid (Nagy et al. 1996) and TGF-β response elements in the TG2 gene promoter has been known for a long time (Ritter and Davies 1998). Macrophages engulfing apoptotic cells release TGF-β (Fadok et al. 1998), and it was observed that neutralization of TGF-β in vivo attenuates the expression of TG2 following apoptosis initiation in the thymus (Szondy et al. 2003) indicating that TGF-β might contribute to the induction of TG2 in dying thymocytes. However, neutralizing of TGF-β could not fully block the in vivo induction of TG2 expression, suggesting that in addition to TGF-β, other signals must contribute to the thymic apoptosis-coupled TG2 expression. Since TG2 is a retinoid target gene (Nagy et al. 1996) and retinoids are also actively produced in the thymus (Kiss et al. 2008), Garabuczi et al. (2011) centered their contribution on an investigation with the aim of testing, whether retinoids produced in the thymus could also contribute to the appearance of TG2 in the apoptotic thymocytes. Here, they report that in vitro retinoic acids, or TGF-β and retinoic acids together can significantly enhance the TG2 mRNA expression in dying thymocytes, and the apoptotic signal contributes to the TG2 induction.
Finally, this issue is concluded by original articles focused on various aspect of TGs: identification of human salivary TGs and their potential impact in celiac disease (CD) Pérez-Alea et al. (2011); the importance of intracellular TG activation as central in the context of CD pathogenesis (Caputo et al. 2011); food allergy in children by ovomucoid and its inactivation by a microbial TG (Porta et al. 2011); progression of cardiovascular diseases (Jandu et al. 2011); and partial identification of some novel plant TGs (Beninati et al. 2012b).
Identification of human salivary TGs was performed by Pérez-Alea et al. (2011). Specific antibodies showed the co-existence of TG1, TG2, TG3 and TG4. TG2 and TG3 were found in native and multiple proteolytic forms. Since the early contact of gluten-containing food with salivary TG1 and/or TG2 takes place in the oral cavity, the potential impact of the salivary TGs in CD represents a new subject of study. Indeed, anti-TG2 antibodies are specifically produced in the small intestinal mucosa of CD patients. It is now recognized that these antibodies, acting on cell surface TG2, may play an active role in CD pathogenesis triggering an intracellular response via the activation of different signal transduction pathways. Anti-TG2 antibodies induce a rapid Ca2+ mobilization from intracellular stores in Caco-2 cells. The increased Ca2+ level in the cells was sufficient to activate TG2, which is normally present as a latent protein due to the low Ca2+ and to the inhibitory effect of GTP/GDP (Caputo et al. 2011).
Hen’s egg is one of the most common offending foods that cause food allergy in children (Bock and Atkins 1990). The hypersensitivity reactions are triggered not only by ingestion of egg products but also by direct contact with the skin. Approximately 75 % of patients with contact urticaria caused by hen’s egg also develop some allergic symptoms with oral ingestion (Yamada et al. 2000). In contrast, the remainder of patients shows dermal reactions on contact with egg products in spite of the absence of symptoms on ingestion. The mechanisms underlying this discrepancy may be related to the different routes of entry of food antigens. Proteolytic enzymes in the alimentary tract degrade food antigens into fragments with small molecules. However, food antigens causing contact urticaria penetrate through the epidermis and react with IgE molecules attached to mast-cell membranes without breakdown by digestive enzymes. Ovomucoid, the dominant allergen in hen’s egg, is a highly glycosylated protein comprising 186 amino acids arranged in three tandem domains. It has a more important role in the pathogenesis of allergic reactions to eggs than other proteins in egg white. Ovomucoid acts as an effective acyl donor substrate for a microbial isoform (mTG) of TG2, and this modification reduces its capability in inhibiting the proteolytic activity of trypsin and affects also the protein antigenicity (Porta et al. 2011). These data encourage further studies on the possibility to apply mTG as a biotechnological tool for decrease ovomucoid allergenic responses and to prevent white egg hypersensitivity.
Increased tissue TG2 cross-linking activity contributes to age-related increases in vascular stiffness (Santhanam et al. 2010). TG2 is highly expressed in all cellular components of the vasculature including endothelial, smooth muscle cells, fibroblasts and monocytes/macrophages (Sane et al. 2007, Bakker et al. 2008). TG2 is externalized to the cell surface and exported to the ECM through an undefined mechanism. It was recently shown that nitric oxide (NO) facilitate TG2 externalization in endothelial and fibroblast cells (Santhanam et al. 2010). The potential role of NO in regulating protein trafficking in the cardiovascular system is discussed by Jandu et al. (2011). This is of particular interest in understanding vascular aging, where reduced NO bioavailability is well established.
TGs are widespread in all plant organs, and cell compartments studied until now. The physiological role of plant TG appears related to photosynthesis, fertilization, response to abiotic and biotic stresses, senescence and programmed cell death. In chloroplasts, plant TG appears to stabilize the photosynthetic complexes and ribulose bisphosphate carboxylase/oxygenase, being regulated by light and other factors, possibly exerting a positive effect on photosynthesis and photo-protection. Similarly to animal, TG plant enzymes are Ca2+ -dependent and able to produce γ-glutamylpolyamine derivatives (Serafini-Fracassini et al. 1995). Three TGs expressed and enzymatically active were identified in immature cells of Helianthus tuberosus sprout apices. These proteins appear similar to those found in differentiate cells of other plant systems and show an amino acids composition comparable with two mammalian TGs. Authors suggest that these TGs are constitutive enzyme phylogenetically very conserved (Beninati et al. 2012b).
We hope that the articles published in this special issue will continue to generate an interest in such unique family of enzymes and will further improve our understanding of the biological role of TGs.
References
Abe S, Yamashita K, Kohno H, Ohkubo Y (2000) Involvement of transglutaminase in the receptor-mediated endocytosis of mouse peritoneal macrophages. Biol Pharm Bull 23:1511–1513
Akimov SS, Krylov D, Fleischman LF, Belkin AM (2000) Tissue transglutaminase is an integrin-binding adhesion co-receptor for fibronectin. J Cell Biol 148:825–838
Al-Jallad HF, Nakano Y, Chen JL, McMillan E, Lefebvre C, Kaartinen MT (2006) Transglutaminase activity regulates osteoblast differentiation and matrix mineralization in MC3T3-E1 osteoblast cultures. Matrix Biol 25:135–148
Antonyak MA, Jansen JM, Miller AM, Ly TK, Endo M, Cerione RA (2006) Two isoforms of tissue transglutaminase mediate opposing cellular fates. Proc Natl Acad Sci USA 103:18609–18614
Arai F, Hirao A, Ohmura M, Sato H, Matsuoka S, Takubo K, Ito K, Koh GY, Suda T (2004) Tie2/angiopoietin-1 signaling regulates hematopoietic stem cell quiescence in the bone marrow niche. Cell 118:149–161
Badarau E, Collighan RJ, Griffin M (2011) Recent advances in the development of tissue transglutaminase (TG2) inhibitors. Amino Acids. doi:10.1007/s00726-011-1188-4
Bakker EN, Pistea A, VanBavel E (2008) Transglutaminases in vascular biology: relevance for vascular remodeling and atherosclerosis J Vasc Res. 45:271–278
Beninati S, Nicolini L, Jakus J, Passeggio A, Abbruzzese A (1995) Identification of a substrate site for transglutaminases on the human protein synthesis initiation factor 5A. Biochem J 305:725–728
Beninati S, Gentile V, Caraglia M, Lentini A, Tagliaferri P, Abbruzzese A (1998) Tissue transglutaminase expression affects hypusine metabolism in BALB/c 3T3 cells. FEBS Lett 437:34–38
Beninati S, Bergamini CM, Piacentini M (2009) An overview of the first 50 years of transglutaminase research. Amino Acids 36:591–598
Beninati S, Park MH, Wolff E, Fésüs L, Abbruzzese A, Chung SI, Carmassi F, Cocuzzi E, Trawick ML, Piacentini M (2012a) In memoriam: John E. Folk (1925–2010). Amino Acids Doi:10.1007/s00726-012-1367-y
Beninati S, Iorio RA, Tasco G, Serafini-Fracassini D, Casadio R, Del Duca S (2012b) Expression of different forms of transglutaminases by immature cells of Helianthus tuberosus sprout apices. Amino Acids. doi:10.1007/s00726-012-1411-y
Bergamini CM, Signorini M, Barbato R, Menabò R, Di Lisa F, Gorza L, Beninati S (1995) Transglutaminase-catalyzed polymerization of troponin in vitro. Biochem Biophys Res Commun 206:201–206
Bissell MJ (1999) Tumor plasticity allows vasculogenic mimicry, a novel form of angiogenic switch. A rose by any other name? Am J Pathol 155:675–679
Bock SA, Atkins FM (1990) Patterns of food hypersensitivity during sixteen years of double-blind, placebo-controlled food challenges. J Pediatr 117:561–567
Boehm JE, Singh U, Combs C, Antonyak MA, Cerione RA (2002) Tissue transglutaminase protects against apoptosis by modifying the tumor suppressor protein p110 Rb. J Biol Chem 277:20127–20130
Bowser TE, Trawick ML (2011) Probing the specificity of gamma-glutamylamine cyclotransferase: an enzyme involved in the metabolism of transglutaminase-catalyzed protein crosslinks. Amino Acids. doi:10.1007/s00726-011-1153-2
Budillon A, Carbone C, Di Gennaro E (2011) Tissue transglutaminase: a new target to reverse cancer drug resistance. Amino Acids. doi:10.1007/s00726-011-1167-9
Caccamo D, Condello S, Ferlazzo N, Currò M, Griffin M, Ientile R (2011) Transglutaminase 2 interaction with small heat shock proteins mediate cell survival upon excitotoxic stress. Amino Acids. doi:10.1007/s00726-011-1083-z
Caputo I, Lepretti M, Secondo A, Martucciello S, Paolella G, Sblattero D, Barone MV, Esposito C (2011) Anti-tissue transglutaminase antibodies activate intracellular tissue transglutaminase by modulating cytosolic Ca(2+) homeostasis. Amino Acids. doi:10.1007/s00726-011-1120-y
Caraglia M, Tagliaferri P, Budillon A, Abbruzzese A (1999) Post-translational modifications of eukaryotic initiation factor-5A (eIF-5A) as a new target for anti-cancer therapy. Adv Exp Med Biol 472:187–198
Caraglia M, Park MH, Wolff EC, Marra M, Abbruzzese A (2011) eIF5A isoforms and cancer: two brothers for two functions? Amino Acids. doi:10.1007/s00726-011-1182-x
Chhabra A, Verma A, Mehta K (2009) Tissue transglutaminase promotes or suppresses tumors depending on cell context. Anticancer Res 29:1909–1919
Citron BA, SantaCruz KS, Davies PJ, Festoff BW (2001) Intron–exon swapping of transglutaminase mRNA and neuronal Tau aggregation in Alzheimer’s disease. J Biol Chem 276:3295–3301
Dardik R, Loscalzo J, Eskaraev R, Inbal A (2005) Molecular mechanisms underlying the proangiogenic effect of factor XIII. Arterioscler Thromb Vasc Biol 25:526–532
De Laurenzi V, Melino G (2001) Gene disruption of tissue transglutaminase. Mol Cell Biol 21:148–155
Deasey S, Shanmugasundaram S, Nurminskaya M (2011) Tissue-specific responses to loss of transglutaminase 2. Amino Acids. doi:10.1007/s00726-011-1183-9
Facchiano A, Facchiano F (2009) Transglutaminases and their substrates in biology and human diseases: 50 years of growing. Amino Acids 36:599–614
Facchiano AM, Facchiano A, Facchiano F (2003) Active sequences collection (ASC) database: a new tool to assign functions to protein sequences. Nucleic Acids Res 31:379–382
Facchiano F, Deloye F, Doussau F, Innamorati G, Ashton AC, Dolly JO, Beninati S, Facchiano A, Luini A, Poulain B, Benfenati F (2010) Transglutaminase participates in the blockade of neurotransmitter release by tetanus toxin: evidence for a novel biological function. Amino Acids 39:257–269
Facchiano F, D’Arcangelo D, Lentini A, Rossi S, Senatore C, Pannellini T, Tabolacci C, Facchiano AM, Facchiano A, Beninati S (2012) Tissue transglutaminase activity protects from cutaneous melanoma metastatic dissemination: an in vivo study. Amino Acids. doi:10.1007/s00726-012-1351-6
Fadok VA, Bratton DL, Konowal A, Freed PW, Westcott JY, Henson PM (1998) Macrophages that have ingested apoptotic cells in vitro inhibit proinflammatory cytokine production through autocrine/paracrine mechanisms involving TGF-beta, PGE2, and PAF. J Clin Invest 101:890–898
Fimia GM, Piacentini M (2010) Regulation of autophagy in mammals and its interplay with apoptosis. Cell Mol Life Sci 67(10):1581–1588
Fink ML, Folk JE (1981) γ-Glutamylamine cyclotransferase. An enzyme involved in the catabolism of epsilon-(gamma-glutamyl) lysine and other gamma-glutamylamines. Mol Cell Biochem 38:59–67
Folk JE (1983) Mechanism and basis for specificity of transglutaminase catalyzed epsilon-(gamma-glutamyl) lysine bond formation. Adv Enzymol Relat Areas Mol Biol 54:1–56
Folk JE, Cole PW (1966) Mechanism of action of guinea pig liver transglutaminase. I. Purification and properties of the enzyme: identification of a functional cysteine essential for activity. J Biol Chem 241:5518–5525
Folk JE, Park MH, Chung SI, Schrode J, Lester EP, Cooper HL (1980) Polyamines as physiological substrates for transglutaminases. J Biol Chem 255:3695–3700
Forsprecher J, Wang Z, Nelea V, Kaartinen MT (2009) Enhanced osteoblast adhesion on transglutaminase 2-crosslinked fibronectin. Amino Acids 36:747–753
Garabuczi E, Kiss B, Felszeghy S, Tsay GJ, Fésüs L, Szondy Z (2011) Retinoids produced by macrophages engulfing apoptotic cells contribute to the appearance of transglutaminase 2 in apoptotic thymocytes. Amino Acids. doi:10.1007/s00726-011-1119-4
Giatromanolaki A, Sivridis E, Koukourakis MI (2004) Tumour angiogenesis: vascular growth and survival. APMIS 112:431–440
Grenard P, Bates MK, Aeschlimann D (2001) Evolution of transglutaminase genes: identification of a transglutaminase gene cluster on human chromosome 15q15. Structure of the gene encoding transglutaminase X and a novel gene family member, transglutaminase Z. J Biol Chem 276:33066–33078
Griffin M, Casadio R, Bergamini CM (2002) Transglutaminases: nature’s biological glues. Biochem J 368:377–396
Hollier BG, Kricker JA, Van Lonkhuyzen DR, Leavesley DI, Upton Z (2008) Substrate-bound insulin-like growth factor (IGF)-I-IGF binding protein-vitronectin-stimulated breast cell migration is enhanced by coactivation of the phosphatidylinositide 3-kinase/AKT pathway by (alpha)v-integrins and the IGF-I receptor. Endocrinology 149:1075–1090
Jandu SK, Webb AK, Pak A, Sevinc B, Nyhan D, Belkin AM, Flavahan NA, Berkowitz DE, Santhanam L (2011) Nitric oxide regulates tissue transglutaminase localization and function in the vasculature. Amino Acids. doi:10.1007/s00726-011-1090-0
Jang GY, Jeon JH, Cho SY, Shin DM, Kim CW, Jeong EM, Bae HC, Kim TW, Lee SH, Choi Y, Lee DS, Park SC, Kim IG (2010) Transglutaminase 2 suppresses apoptosis by modulating caspase 3 and NF-kappaB activity in hypoxic tumor cells. Oncogene 29:356–367
Jeitner TM, Matson WR, Folk JE, Blass JP, Cooper AJL (2008) Increased levels of γ-Glutamyl amines in Huntington disease CSF. J Neurochem 106:37–44
Jeitner TM, Pinto JT, Krasnikov BF, Horswill M, Cooper AJL (2009) Transglutaminases and neurodegeneration. J Neurochem 109:160–166
Jeitner TM, Battaile K, Cooper AJ (2012) γ-Glutamylamines and neurodegenerative diseases. Amino Acids. doi:10.1007/s00726-011-1209-3
Jones RA, Wang Z, Dookie S, Griffin M (2012) The role of TG2 in ECV304-related vasculogenic mimicry. Amino Acids. doi:10.1007/s00726-011-1214-6
Kaartinen MT, El-Maadawy S, Räsänen NH, McKee MD (2002) Tissue transglutaminase and its substrates in bone. J Bone Miner Res 17:2161–2173
Kashyap AS, Hollier BG, Manton KJ, Satyamoorthy K, Leavesley DI, Upton Z (2011) Insulin-like growth factor-I:vitronectin complex-induced changes in gene expression effect breast cell survival and migration. Endocrinology 152:1388–1401
Kim SY, Grant P, Lee JH, Pant HC, Steinert PM (1999) Differential expression of multiple transglutaminases in human brain. Increased expression and cross-linking by transglutaminases 1 and 2 in Alzheimer’s disease. J Biol Chem 274:30715–30721
Kim SJ, Kim KH, Ahn ER, Yoo BC, Kim SY (2011) Depletion of cathepsin D by transglutaminase 2 through protein cross-linking promotes cell survival. Amino Acids. doi:10.1007/s00726-011-1089-6
Király R, Barta E, Fésüs L (2011) Polymorphism of transglutaminase 2: unusually low frequency of genomic variants with deficient functions. Amino Acids. doi:10.1007/s00726-011-1194-6
Kiss I, Rühl R, Szegezdi E, Fritzsche B, Tóth B, Pongrácz J, Perlmann T, Fésüs L, Szondy Z (2008) Retinoid receptor-activating ligands are produced within the mouse thymus during postnatal development. Eur J Immunol 38:147–155
Kumar S, Mehta K (2011) Tissue transglutaminase, inflammation, and cancer: how intimate is the relationship? Amino Acids. doi:10.1007/s00726-011-1139-0
Legate KR, Wickstrom SA, Fassler R (2009) Genetic and cell biological analysis of integrin outside-in signaling. Genes Dev 23:397–418
Lentini A, Provenzano B, Caraglia M, Shevchenko A, Abbruzzese A, Beninati S (2008) Impairment of the metastatic activity of melanoma cells by transglutaminase-catalyzed incorporation of polyamines into laminin and matrigel. Amino Acids 34:251–256
Lentini A, Tabolacci C, Mattioli P, Provenzano B, Beninati S (2011) Spermidine delays eye lens opacification in vitro by suppressing transglutaminase-catalyzed crystallin cross-linking. Protein J 30:109–114
Lentini A, Abbruzzese A, Provenzano B, Tabolacci C, Beninati S (2012) Transglutaminases: key regulators of cancer metastasis. Amino Acids. doi:10.1007/s00726-012-1229-7
Li F, Tsien JZ (2009) Memory and the NMDA receptors. N Engl J Med 361:302–303
Liu P, Gupta N, Jing Y, Zhang H (2008) Age-related changes in polyamines in memory associated brain structures in rats. Neuroscience 155:789–796
Lorand L, Graham RM (2003) Transglutaminases: crosslinking enzymes with pleiotropic functions. Nat Rev Mol Cell Biol 4:140–156
Mangala LS, Fok JY, Zorrilla-Calancha IR, Verma A, Mehta K (2007) Tissue transglutaminase expression promotes cell attachment, invasion and survival in breast cancer cells. Oncogene 26:2459–2470
Martin A, Giuliano A, Collaro D, De Vivo G, Sedia C, Serretiello E, Gentile V (2011) Possible involvement of transglutaminase-catalyzed reactions in the physiopathology of neurodegenerative diseases. Amino Acids. doi:10.1007/s00726-011-1081-1
McDonough JL, Arrell DK, Van Eyk JE (1999) Troponin I degradation and covalent complex formation accompanies myocardial ischemia/reperfusion injury. Circ Res 84:9–20
Monsonego A, Shani Y, Friedmann I, Paas Y, Eizenberg O, Schwartz M (1997) Expression of GTP-dependent and GTP-independent tissue-type transglutaminase in cytokine-treated rat brain astrocytes. J Biol Chem 272:3724–3732
Muto Y, Nouri-Aria KT, Meager A, Alexander GJ, Eddleston AL, Williams R (1988) Enhanced tumour necrosis factor and interleukin-1 in fulminant hepatic failure. Lancet 2:72–74
Nagy L, Saydak M, Shipley N, Lu S, Basilion JP, Yan ZH, Syka P, Chandraratna RA, Stein JP, Heyman RA, Davies PJ (1996) Identification and characterization of a versatile retinoid response element (retinoic acid receptor response element-retinoid X receptor response element) in the mouse tissue transglutaminase gene promoter. J Biol Chem 271:4355–4365
Nanda N, Iismaa SE, Owens WA, Husain A, Mackay F, Graham RM (2001) Targeted inactivation of Gh/tissue transglutaminase II. J Biol Chem 276:20673–20678
Nurminskaya MV, Belkin AM (2012) Cellular functions of tissue transglutaminase. Int Rev Cell Mol Biol 294:1–97
Nurminskaya M, Kaartinen MT (2006) Transglutaminases in mineralized tissues. Front Biosci 11:1591–1606
Panteghini M (2009) Assay-related issues in the measurement of cardiac troponins. Clin Chim Acta 402:88–93
Park SS, Kim JM, Kim DS, Kim IH, Kim SY (2006) Transglutaminase 2 mediates polymer formation of I-kappaBalpha through C-terminal glutamine cluster. J Biol Chem 281:34965–34972
Perez Alea M, Thomas V, Martin G, El Alaoui S (2011) Identification of human salivary transglutaminases. Amino Acids. doi:10.1007/s00726-011-1142-5
Phatak VM, Croft SM, Rameshaiah Setty SG, Scarpellini A, Hughes DC, Rees R, McArdle S, Verderio EA (2011) Expression of transglutaminase-2 isoforms in normal human tissues and cancer cell lines: dysregulation of alternative slicing in cancer. Amino Acids. doi:10.1007/s00726-011-1127-4
Pinkas DM, Strop P, Brunger AT, Khosla C (2007) Transglutaminase 2 undergoes a large conformational change upon activation. PLoS Biol 25:2788–2796
Porta R, Giosafatto CV, di Pierro P, Sorrentino A, Mariniello L (2011) Transglutaminase-mediated modification of ovomucoid: effects on its trypsin inhibitory activity and antigenic properties. Amino Acids. doi:10.1007/s00726-011-1155-0
Quarles LD, Yohay DA, Lever LW, Caton R, Wenstrup RJ (1992) Distinct proliferative and differentiated stages of murine MC-3T3-E1 culture; an in vitro model of osteoblast development. J Bone Miner Res 7:683–692
Ricci-Vitiani L, Pallini R, Biffoni M, Todaro M, Invernici G et al (2010) Tumour vascularization via endothelial differentiation of glioblastoma stem-like cells. Nature 468:824–828
Ritter SJ, Davies PJ (1998) Identification of a transforming growth factor-beta1/bone morphogenetic protein 4 (TGF-beta1/BMP4) response element within the mouse tissue transglutaminase gene promoter. J Biol Chem 273(21):12798–12806
Sane DC, Kontos JL, Greenberg CS (2007) Roles of transglutaminases in cardiac and vascular diseases. Front Biosci 12:2530–2545
Santhanam L, Tuday EC, Webb AK, Dowzicky P, Kim JH, Oh YJ, Sikka G, Kuo M, Halushka MK, Macgregor AM, Dunn J, Gutbrod S, Yin D, Shoukas A, Nyhan D, Flavahan NA, Belkin AM, Berkowitz DE (2010) Decreased S-nitrosylation of tissue transglutaminase contributes to age-related increases in vascular stiffness. Circ Res 107:117–125
Sarkar NK, Clarke DD, Waelsch H (1957) An enzymically catalyzed incorporation of amines into proteins. Biochim Biophys Acta 25:451–452
Serafini-Fracassini D, Del Duca S, Beninati S (1995) Plant transglutaminases. Phytochemistry 40:355–365
Siefring GE Jr, Apostol AB, Velasco PT, Lorand L (1978) Enzymatic basis for the Ca2+-induced cross-linking of membrane proteins in intact human erythrocytes. Biochemistry 17:2598–2604
Sivaramakrishnan M, Shooter GK, Upton Z, Croll TI (2011) Transglutaminases and receptor tyrosine kinases. Amino Acids. doi:10.1007/s00726-011-1113-x
Sollid LM, Jabri B (2011) Celiac disease and transglutaminase 2: a model for posttranslational modification of antigens and HLA association in the pathogenesis of autoimmune disorders. Curr Opin Immunol 23:732–738
Squerzanti M, Cervellati C, Ura B, Mischiati C, Pucci P, Annunziata S, Iannone C, Casadio R, Bergamini CM, Esposito C (2011) The side chain of glutamine 13 is the acyl-donor amino acid modified by type 2 transglutaminase in subunit T of the native rabbit skeletal muscle troponin complex. Amino Acids. doi:10.1007/s00726-011-1144-3
Sun Y, Campisi J, Higano C, Beer TM, Porter P, Coleman I, True L, Nelson PS (2012) Treatment-induced damage to the microenvironment promotes prostate cancer therapy resistance through WNT16B. Nat Med. doi:10.1038/nm.2890
Szondy Z, Sarang Z, Molnar P, Nemeth T, Piacentini M, Mastroberardino PG, Falasca L, Aeschlimann D, Kovacs J, Kiss I, Szegezdi E, Lakos G, Rajnavolgyi E, Birckbichler PJ, Melino G, Fesus L (2003) Transglutaminase 2−/− mice reveal a phagocytosis associated crosstalk between macrophages and apoptotic cells. Proc Natl Acad Sci USA 100:7812–7817
Tabolacci C, Lentini A, Provenzano B, Beninati S (2012) Evidences for a role of protein cross-links in transglutaminase-related disease. Amino Acids 42:975–986
Tarantino U, Ferlosio A, Arcuri G, Spagnoli LG, Orlandi A (2011) Transglutaminase 2 as a biomarker of osteoarthritis: an update. Amino Acids. doi:10.1007/s00726-011-1181-y
Thiele CJ, Gore S, Collins S, Waxman S, Miller W (2000) Differentiate or die: the view from Montreal. Cell Death Differ 7:1014–1017
Thomas H, Beck K, Adamczyk M, Aeschlimann P, Langley M, Oita RC, Thiebach L, Hils M, Aeschlimann D (2011) Transglutaminase 6: a protein associated with central nervous system development and motor function. Amino Acids. doi:10.1007/s00726-011-1091-z
Tiboldi A, Lentini A, Provenzano B, Tabolacci C, Höger H, Beninati S, Lubec G (2012) Hippocampal polyamine levels and transglutaminase activity are paralleling spatial memory retrieval in the C57BL/6 J mouse. Hippocampus 5:1068–1074
Torricelli P, Caraglia M, Abbruzzese A, Beninati S (2011) γ-Tocopherol inhibits human prostate cancer cell proliferation by up-regulation of transglutaminase 2 and down-regulation of cyclins. Amino Acids. doi:10.1007/s00726-012-1278-y
Verma A, Mehta K (2007) Tissue transglutaminase-mediated chemoresistance in cancer cells. Drug Resist Updat 10:144–151
Watanabe K, Tsunoda K, Itoh M, Fukui M, Mori H, Hitomi K (2011) Transglutaminase 2 and Factor XIII catalyze distinct substrates in differentiating osteoblastic cell line: utility of highly reactive substrate peptides. Amino Acids. doi:10.1007/s00726-011-1131-8
Yamada K, Urisu A, Kakami M, Koyama H, Tokuda R, Wada E, Kondo Y, Ando H, Morita Y, Torii S (2000) IgE-binding activity to enzyme-digested ovomucoid distinguishes between patients with contact urticaria to egg with and without overt symptoms on ingestion. Allergy 55:565–569
Yoo H, Ahn ER, Kim SJ, Lee SH, Oh SH, Kim SY (2012) Divergent results induced by different types of septic shock in transglutaminase 2 knockout mice. Amino Acids. doi:10.1007/s00726-012-1412-x
Zemskov EA, Janiak A, Hang J, Waghray A, Belkin AM (2006) The role of tissue transglutaminase in cell–matrix interactions. Front Biosci 11:1057–1076
Acknowledgments
The guest editors express their gratitude to Prof. Gert Lubec, Editor-in-Chief, for the opportunity to prepare this special issue of Amino Acids and all Authors for their commitment and contributions to this compilation and we trust that this will be the start of an expanding and long-standing partnership of Amino Acids with TGs research.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Beninati, S., Facchiano, F. & Piacentini, M. Transglutaminases: future perspectives. Amino Acids 44, 1–9 (2013). https://doi.org/10.1007/s00726-012-1431-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-012-1431-7