Abstract
Apelin receptor (APJ) deficiency has been reported to be preventive against atherosclerosis. However, the mechanism of this effect remains unknown. In this study, quantitative real-time RT-PCR, Western blotting and ELISA analyses revealed a significant increase in the expression of intercellular adhesion molecule-1(ICAM-1), vascular cell adhesion molecule-1 (VCAM-1) and monocyte chemoattractant protein-1 (MCP-1) in human umbilical vein endothelial cells (HUVECs) treated with apelin. Inhibitors of cellular signal transduction molecules were used to demonstrate involvement of nuclear factor kappa-B (NF-κB) and c-Jun N-terminal kinase (JNK) pathways in apelin–APJ-induced activation of adhesion molecules and chemokines. Inhibition of APJ expression by RNA interference abrogated apelin-induced expression of adhesion molecules and chemokines and apelin-stimulated cellular signal transduction in HUVECs. The apelin–APJ system in endothelial cells is involved in the expression of adhesion molecules and chemokines, which are important for the initiation of endothelial inflammation-related atherosclerosis. Therefore, apelin–APJ and the cell signaling pathways activated by this system in endothelial cells may represent targets for therapy of atherosclerosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Growing evidence supports the role of the apelin–APJ system as a modulator of cardiovascular functions such as vasomotion, myocardial contractility and artery calcification (Karmazyn et al. 2008; Shan et al. 2011). Apelin and its receptor APJ are ubiquitously expressed at the mRNA level in many rat and human tissues (Zeng et al. 2007; Barnes et al. 2010). Both apelin and APJ are expressed in the heart, large and small conduit vessels and endothelial cells (Dray et al. 2008; Eyries et al. 2008). Recently, it has been shown that high plasma apelin concentrations are associated with obesity in humans and hyperinsulinemic obese mice (Boucher et al. 2005), suggesting a link between apelin and feeding. Furthermore, a marked reduction in the number of atherosclerotic lesions were detected in APJ and apolipoprotein E (ApoE) double-knockout (APJ−/− ApoE−/−) mice that were fed a high-cholesterol diet compared with APJ+/+ ApoE−/− mice (Hashimoto et al. 2007), thus suggesting that APJ deficiency could reduce atherogenesis.
The contribution of the apelin–APJ system to atherogenesis is generally accepted. However, the mechanisms underlying this effect remain to be elucidated. It has been proposed that oxidative stress in smooth muscle cells mediated by the apelin–APJ system is an important factor in atherogenesis (Hashimoto et al. 2007). Inflammation of the vascular endothelia, which may initiate the atherogenic process (Libby 2002), may be importantly linked to activation of monocytes and macrophages via APJ (Seehaus et al. 2009).
This study aimed to identify the effects of apelin–APJ system on the expression and regulation of adhesion molecules and chemokines, in order to explore a potential association between this system and endothelial inflammation. Vascular cell adhesion molecule-1(VCAM-1) and intercellular adhesion molecule-1 (ICAM-1) participate in firm adhesion of leukocytes to endothelial cells (Blankenberg et al. 2003) and monocyte chemoattractant protein-1 (MCP-1) is involved in leukocyte rolling and cross-endothelium migration (Gu et al. 1998). The results of this study indicate that the apelin–APJ system stimulates ICAM-1, VCAM-1 and MCP-1 expression and secretion in human umbilical vein endothelial cells (HUVECs). Moreover, these data demonstrate a link between the apelin–APJ system and nuclear factor kappa-B (NF-κB)/c-Jun N-terminal kinase (JNK) signal transduction in HUVECs.
Materials and methods
Reagents
Synthetic apelin-13 peptide was purchased from the American Peptide Company Inc. (Sunnyvale, CA, USA). The amino acid sequence of apelin-13 is Gln-Arg-Pro-Arg-Leu-Ser-His-Lys-Gly-Pro-Met-Pro-Phe. Pertussis toxin (PTX) was purchased from Sigma (St. Louis, MO, USA). Anti-human ICAM-1, VCAM-1, MCP-1, JNK, phosphorylated JNK (pJNK), IkBα, NF-κB-p65, β-actin and proliferating cell nuclear antigen (PCNA) antibodies and also anti-mouse and rabbit IgG peroxidase conjugated antibodies were purchased from Santa Cruz Biotechnology Inc. (Santa Cruz, CA, USA). Anti-human apelin receptor (APJ) antibody was purchased from Abcam Inc. (Cambridge, MA, USA). SP600125 and SN50 were purchased from Calbiochem-Novabiochem Corp. (San Diego, CA, USA). Short hairpin RNA vectors were synthesized by Genesil Biotechnology Co. (Wuhan, China). Anti-human ICAM-1, VCAM-1 and MCP-1 ELISA kits were purchased from Boster Biological Engineering Co. (Wuhan, China).
Cell culture
HUVECs were isolated by 0.1 % collagenase digestion of freshly obtained human umbilical cords (human umbilical cords were obtained from donors after receipt of informed consent and upon approval by the local research ethics committee) as described previously (Jaffe et al. 1973) and cultured in Dulbecco’s modified Eagle’s medium (DMEM, Sigma) containing 10 % fetal bovine serum (FBS, Gibco), 50 μg/ml endothelial cell growth supplement, 50 μg/ml heparin, 100 IU/ml penicillin and 100 μg/ml streptomycin at 37 °C in an atmosphere containing 5 % CO2. Cells were used for experiments at passages two to four.
Quantitative real-time reverse transcription (RT) PCR
Total RNA was isolated from cells with Trizol (Gibco) according to the instructions provided by the manufacturer. cDNA synthesis was performed using 2 μg total RNA and the Reverse Transcription System (Promega). Quantitative real-time PCR was performed using a LightCycler (Roche Diagnostics) with gene-specific primers and SYBR Premix Ex Taq™ II(Takara) containing SYBR Green I. The following primers were used to amplify cDNA fragments:
-
human ICAM-1, (forward) 5′-CTC CAA TGT GCC AGG CTT G-3′ and (reverse) 5′-CAG TGG GAA AGT GCC ATC CT-3′;
-
human VCAM-1, (forward) 5′-TTC CCT AGA GAT CCA GAA ATC GAG-3′ and (reverse) 5′-CTT GCA GCT TAC AGT GAC AGA GC -3′;
-
human MCP-1, (forward) 5′-CAT TGT GGC CAA GGA GAT CTG-3′ and (reverse) 5′-CTT CGG AGT TTG GGT TTG CTT-3′;
-
human β-actin, (forward), 5′-CTC TTC CAG CCT TCC TTC CT-3′ and (reverse) 5′-AGC ACT GTG TTG GCG TAC AG-3′.
Amplifications were performed (including calibration curves) and then run in parallel in triplicates. Six replicates were included for each amplification. The experiments were carried out at least twice. The mRNA expression levels were quantified according to the ΔΔCT method (Livak and Schmittgen 2001), then normalized against β-actin expression and presented relative to control levels.
RNA interference
Two short hairpin RNA vectors were constructed encoding sequences targeting human APJ mRNA (siAPJ-1:5′-AACTACTATGGGGCAGACAAC-3′ and siAPJ-2:5′-AAGGTGCAGTGC TACATGGAC-3′). A scrambled RNAi plasmid (SiHK) was used as a negative control. Transfection was performed using Lipofectamine 2000 (Invitrogen) in accordance with the instructions provided by the manufacturer. HUVECs were plated in serum and antibiotic-free DMEM medium with a mixture of Lipofectamine 2000 and shRNA vectors previously equilibrated to room temperature for 20 min. After 24 h, the culture medium was changed to DMEM complete medium with antibiotics and G418 (400 μg/ml, Invitrogen) for selection of integrated clones. During 10 days of selection, green fluorescence was monitored under blue excitation light by fluorescence microscopy and resistant clones were picked at random. Clones identified as endothelial cells by VIII factor-related antigen immunocytochemical staining were amplified for further experiments using standard HUVEC culture conditions.
Preparation of cytoplasmic and nuclear extracts
Cytoplasmic and nuclear extracts were prepared by a modification of the Dignam method (Carmody et al. 2007). Cell monolayers (3 × 106–5 × 106 cells) were washed in ice-cold phosphate-buffered saline (PBS) before incubation in ice-cold buffer A (10 mM HEPES–NaOH, pH 7.9, 10 mM KCl, 1.5 mM MgCl2, 1 % Nonidet P-40, 1 mM DTT and supplemented with a protease inhibitor mixture and two phosphatase inhibitors, Na3VO4 and NaF) for 10 min on ice. Cells were then harvested by scraping and vortexed vigorously for 15 s. After centrifugation for 10 min at 12,000×g, the resulting supernatant containing the cytoplasmic extract was collected. The nuclear pellet was rinsed once in buffer A, resuspended in ice-cold buffer B (25 % glycerol, 20 mM HEPES–NaOH, pH 7.9, 1.5 mM MgCl2, 420 mM NaCl, 0.1 mM EGTA, 1 mM DTT and supplemented with a protease inhibitor mixture) and incubated for 20 min on ice. Nuclei were sonicated for 10 s and clarified by centrifugation at 15,000×g at 4 °C for 2 min. Cellular debris was removed and the supernatant containing the nuclear extract was collected. Aliquots of cytoplasmic and nuclear extracts were stored at −70 °C. Protein concentrations were determined by the Bradford protein assay.
Western blot analysis
Western blotting was performed as previously described (Cui et al. 2010; Yuan et al. 2010). Cell extracts (20 μg) from each fraction were subjected to 10 % SDS-PAGE. Proteins were transferred to PVDF membrane (Amersham Pharmacia Biotech). After blocking with 5 % milk in PBS, membranes were incubated with specific antibodies at 1:500 dilution factor (anti-ICAM-1, VCAM-1, MCP-1, APJ, JNK, pJNK and IkBα for cytoplasmic proteins, anti-NF-κB-p65 for nuclear proteins) overnight at 4 °C followed by incubation with horseradish peroxidase-conjugated anti-rabbit or anti-mouse IgG at 1:5,000 dilution factor and room temperature for 1 h. Antibody binding was quantitated using an enhanced chemiluminescence (ECL) detection system (GE Biosciences) following the instructions provided by the manufacturer and visualized by fluorography with Hyperfilm.
ELISA
A sandwich ELISA was performed using matched anti-human ICAM-1, VCAM-1 and MCP-1 antibodies according to the instructions provided by the manufacturer. Conditioned media were diluted (between 1:30 and 1:70) and lysates (standardized according to protein concentration) were diluted 1:100 prior to the assay.
Statistical analysis
Differences among groups were tested for significance by one-way ANOVA followed by Bonferroni’s test and the Newman–Keuls test for pairwise comparisons. Statistical significance was considered to occur at a value of P < 0.01. Data are expressed as the mean ± SD of three independent experiments.
Results
Apelin induces the expression of adhesion molecules and chemokines in HUVECs in a concentration- and time-dependent manner
Elevated levels of ICAM-1, VCAM-1 and MCP-1 mRNA expression (Fig. 1a) and protein secretion (Fig. 1b–d) were detected in HUVECs treated with apelin by quantitative real-time RT-PCR and ELISA techniques, respectively. Levels of ICAM-1, VCAM-1 and MCP-1 expression were found to be elevated following treatment with apelin (10−10–10−7 M). Levels of ICAM-1, VCAM-1 and MCP-1 produced by 10−8 M apelin-treated cells were significantly greater than those produced by controls (P < 0.01). The effect of apelin reached a plateau between 10−8 and 10−7 M (Fig. 1a), which is entirely in agreement with the expected affinity of apelin for APJ. No difference was observed in the effects of 10−9 and 10−8 M apelin. Therefore, 10−8 M apelin was selected as the standard concentration for use in further studies. Stimulation at this concentration resulted in robust increases in ICAM-1, VCAM-1 and MCP-1 expression. Treatment with 10−8 M apelin at different time points stimulated increased expression of ICAM-1, VCAM-1 and MCP-1 mRNA (Fig. 2a) in cytoplasmic extracts (Fig. 2b) and conditioned media (Fig. 2c) of HUVECs. The induction of ICAM-1, VCAM-1 and MCP-1 expression by apelin was maximal after 4, 12 and 24 h, respectively.
Concentration dependence of apelin-induced ICAM-1, VCAM-1 and MCP-1 mRNA expression and protein secretion in cultured HUVECs. a The dose response of apelin on ICAM-1, VCAM-1 and MCP-1 mRNA expression. HUVECs were incubated with the vehicle control (apelin, 0 M) or apelin (10−10–10−7 M) for 12 h. Total RNA from the cells was extracted and expression of ICAM-1, VCAM-1 and MCP-1 mRNA was analyzed by quantitative real-time RT-PCR. b–d The dose response of apelin on ICAM-1, VCAM-1 and MCP-1 protein secretion, respectively. The concentration of ICAM-1, VCAM-1 and MCP-1 in the supernatants of cultured HUVECs was analyzed by ELISA. The data shown represent the mean ± SD of three independent experiments, *P < 0.01 versus control cells
Time dependence of apelin-induced ICAM-1, VCAM-1 and MCP-1 expression in cultured HUVECs. a Apelin-induced ICAM-1, VCAM-1 and MCP-1 mRNA expression in cultured HUVECs in a time-dependent manner. HUVECs were incubated with the vehicle control (apelin, 0 h) or apelin (10−8 M) for the indicated time periods. Total RNA was extracted from the cells and expression of ICAM-1, VCAM-1 and MCP-1 mRNA was analyzed by quantitative real-time RT-PCR. b1, b2, b3 Time dependence of apelin-induced ICAM-1, VCAM-1 and MCP-1 protein expression in cultured HUVECs. Total protein was extracted from the cells and expression of ICAM-1, VCAM-1 and MCP-1 protein was analyzed by Western blotting. b4 The OD of Western blot autoradiographic signals was quantified and calculated as the ratio of target protein to β-actin. c1, c2, c3 Apelin-induced ICAM-1, VCAM-1 and MCP-1 protein secretion into the supernatants of cultured HUVECs in a time-dependent manner. The concentration of ICAM-1, VCAM-1 and MCP-1 in the supernatants of cultured HUVECs was analyzed by ELISA. The data represent the mean ± SD of three independent experiments and values are expressed relative to those observed for the control cells. *P < 0.01 versus control cells
Intracellular signaling pathways involved in apelin–APJ-induced expression of adhesion molecules and chemokines
To identify the signal transduction mechanism that mediates apelin-induced ICAM-1, VCAM-1 and MCP-1 expression in HUVECs, the ability of apelin to stimulate JNK phosphorylation, nuclear NF-κB-p65 expression and cytoplasmic IkBα degradation was determined. Serum-starved HUVECs were treated with apelin for various lengths of time and the activation status of JNK was assessed using phospho-specific antibodies. Increased levels of pJNK were evident at 60 min following apelin treatment and increased subsequently in a time-dependent manner (Fig. 3a). Apelin significantly stimulated IkBα degradation in the cytoplasm of HUVECs in a dose-dependent manner (Fig. 3b1). Furthermore, it was confirmed that apelin induced a significant increase in nuclear NF-κB-p65 expression in HUVECs (Fig. 3b2) at 30 min. β-actin and PCNA were used as internal controls. In addition, the involvement of JNK phosphorylation, nuclear NF-κB-p65 expression and cytoplasmic IkBα degradation in apelin-induced ICAM-1, VCAM-1 and MCP-1 expression was investigated. Decreased levels of ICAM-1, VCAM-1 and MCP-1 were detected in HUVECs following pre-treatment with the JNK inhibitor SP600125 or the NF-κB inhibitor SN50 (Fig. 3c).
Involvement of JNK/NF-κB in apelin-stimulated cellular signal transduction. a, b HUVECs were incubated without or with apelin (10−8 M) for the indicated time periods. Cytoplasmic and nuclear protein was extracted from the cells. Expression of phospho-JNK protein was analyzed by Western blotting using anti-phospho-JNK antibody (total JNK as control). NF-κB-p65 (nuclear protein, PCNA as endogenous control) and IκBα (cytoplasmic protein, β-actin as endogenous control) expression was also examined by immunoblotting. a Apelin activated JNK phosphorylation in cultured HUVECs in a time-dependent manner. b Apelin promoted NF-κB-p65 activation and IκBα degradation in cultured HUVECs in a time-dependent manner. a1, b1, b2 Western blot autoradiograph representative of three independent experiments. a2, b3 The OD of Western blot autoradiographic signals was quantified and calculated as the ratio of the target protein to endogenous control protein. c HUVECs were untreated (control), treated with 10−8 M apelin (4 h for ICAM-1 detection, 12 h for VCAM-1 and 24 h for MCP-1) or pre-incubated with the JNK inhibitor SP600125 (10 μM) or the NFκB-p65 inhibitor SN50 (100 μg/ml) for 2 h and then treated with apelin. Total RNA was extracted from the cells and expression of ICAM-1, VCAM-1 and MCP-1 mRNA was examined by quantitative real-time PCR. The data shown represent the mean ± SD of three independent experiments, and values are expressed relative to those observed for the control cells. *P < 0.01 versus control cells, **P < 0.05 versus cells treated with 10−8 M apelin
APJ is required for apelin-induced expression of adhesion molecules and chemokines and apelin-stimulated cellular signal transduction in HUVECs
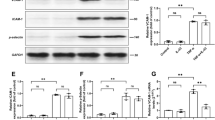
Silencing vectors were constructed to express either shRNA targeting human APJ (siAPJ-1 and siAPJ-2) or scrambled shRNA (SiHK). Quantitative RT-PCR and Western blot analysis indicated that siAPJ-2 reduced APJ mRNA and protein expression in HUVECs to approximately 26 % (Fig. 4a) and 25 % (Fig. 4b, c), respectively, of the level observed in the presence of SiHK. In contrast, siAPJ-1 did not alter APJ expression in HUVECs. The mRNA and protein levels of ICAM-1, VCAM-1 and MCP-1 were measured in HUVECs treated with siAPJ-2 or SiHK vectors and untransfected cells. The mean apelin-induced elevations of ICAM-1, VCAM-1 and MCP-1 mRNA expression in siAPJ-2-treated HUVECs were approximately 5, 28 and 37 %, respectively, of those in SiHK-treated HUVECs and approximately 5, 26 and 36 %, respectively, of those in untransfected HUVECs (Fig. 5a). The mean apelin-induced elevations of ICAM-1, VCAM-1 and MCP-1 protein expression in siAPJ-2-treated HUVECs were approximately 6, 27 and 27 %, respectively, of those in SiHK-treated HUVECs and approximately 6, 26 and 36 %, respectively, of those in untransfected HUVECs (Fig. 5b4). Investigation of apelin-treated HUVECs transfected with the siAPJ-2 vector, the SiHK vector or untransfected cells at the indicated time revealed that JNK was not phosphorylated in HUVECs transfected with the siAPJ-2 vector. Furthermore, pJNK signaling was evident in cells transfected with SiHK vector and untransfected cells (Fig. 6a). Clear expression of NF-κB-p65 protein in nuclear extracts of HUVECs transfected with SiHK vector or untransfected cells was detected, although there was very little expression in the nucleus of HUVECs treated with the siAPJ-2 vector (Fig. 6a). Moreover, IκBα degradation in cytoplasmic extracts of APJ gene-silenced HUVECs was not detected as it was in those of HUVECs expressing the APJ gene (Fig. 6a).
Effects of RNA interference on APJ gene silencing in cultured HUVECs. Total RNA and protein from transfected cells (siHK, siAPJ-1 and siAPJ-2) and untransfected cells (control) was extracted and APJ mRNA and protein expression was analyzed by quantitative real-time RT-PCR and Western blotting, respectively. a RNA expression was quantified and calculated as the ratio of APJ to β-actin. b Western blot autoradiograph representative of three independent experiments from the same transfection. c The OD of Western blot autoradiographic signals was quantified and calculated as the ratio of APJ to β-actin. The data shown represent the mean ± SD of three independent experiments and values are expressed relative to those observed for the control cells. *P < 0.01 versus control cells
Inhibition of apelin-induced ICAM-1, VCAM-1 and MCP-1 expression by APJ silencing in HUVECs. Transfected HUVECs (siHK and siAPJ-2) and untransfected cells (control) were incubated with 10−8 M apelin (4 h for ICAM-1 detection, 12 h for VCAM-1 and 24 h for MCP-1). Total RNA was extracted from the cells and ICAM-1, VCAM-1 and MCP-1 mRNA were analyzed by quantitative real-time RT-PCR. Total protein was extracted from the cells and expression of ICAM-1, VCAM-1 and MCP-1 protein was analyzed by Western blotting. a APJ silencing inhibited apelin-induced ICAM-1, VCAM-1 and MCP-1 mRNA expression in HUVECs. The mRNA expression was quantified and calculated as the ratio of target mRNA to β-actin. b APJ silencing inhibited apelin-induced ICAM-1, VCAM-1 and MCP-1 protein expression in HUVECs. To normalize the amount and quality of total protein, protein expression levels were determined on the basis of the amount of the target protein relative to the endogenous control gene, β-actin. b1, b2, b3 Western blot autoradiograph representative of three independent experiments from the same transfection. b4 The OD of Western blot autoradiographic signals was quantified and calculated as the ratio of target protein to β-actin. The data shown represent the mean ± SD of three independent experiments from the same transfection and values are expressed relative to those observed for the control cells. *P < 0.01 versus control cells
Blockade of apelin-induced cellular signal transduction by APJ silencing and PTX. a Transfected HUVECs (siHK and siAPJ-2) and untransfected cells (control) were incubated with 10−8 M apelin (60 min for pJNK detection, 30 min for NF-κB-p65 and 30 min for IκBα). Cytoplasmic and nuclear protein was extracted from the cells and pJNK (JNK as endogenous control), NF-κB-p65 (PCNA as endogenous control) and IκBα (β-actin as endogenous control) expression was analyzed by Western blotting. b HUVECs were incubated with 10−8 M apelin (60 min for pJNK detection, 30 min for NF-κB-p65 and 30 min for IκBα). Cytoplasmic and nuclear protein was extracted from the cells and pJNK (JNK as endogenous control), NF-κB-p65 (PCNA as endogenous control) and IκBα (β-actin as endogenous control) expression was examined by Western blot. Activity of pJNK, NF-κB-p65 and IκBα in HUVECs stimulated with 10−8 M apelin for 60 min was determined by immunoblotting of pJNK, NF-κB-p65 and IκBα proteins (JNK, PCNA and β-actin as endogenous control) and compared with those obtained after pre-treatment with PTX (25 ng/ml, 16 h)
Apelin–APJ activates NF-κB/JNK signal pathway via a PTX-sensitive G-Protein
The apelin–APJ system is thought to function directly via G-protein heterotrimers, and through Gi alpha subunits in particular (Masri et al. 2002). To identify the G-protein coupled with apelin–APJ for activation of NF-κB/JNK signaling, HUVECs were pretreated with PTX, which uncouples Gi/Go proteins from their receptor. PTX completely abrogated the activation of NF-κB/JNK signaling induced by apelin–APJ (Fig. 6b).
Discussion
Cell adhesion molecules secreted by endothelial cells activated by proinflammatory factors are thought to play a central role in the development of vascular inflammation (Miller et al. 2003; Yamawaki et al. 2005; Pate et al. 2010; Rautou et al. 2011), which leads to the development of cardiovascular complications. Furthermore, the cytokine-activated endothelial cells secrete monocyte-specific chemoattractant molecules, which recruit monocytes to sites of vascular injury and inflammation (Zhan et al. 2005; Feng et al. 2005).
This study clearly demonstrated that apelin–APJ significantly stimulated time- and concentration-dependent expression of ICAM-1, VCAM-1 and MCP-1 in cultured endothelial cells. JNK and NF-κB signaling were shown to be involved in the cellular signal transduction mechanism during these regulatory procedures. These adhesion molecules and chemokines are major regulators of monocyte recruitment and play primary roles in the development of many vascular inflammatory states.
APJ, a G-protein-coupled receptor (GPCR) originally identified by O’Dowd et al. (O’Dowd et al. 1993), has a similarity with the angiotensin II type 1(AT1) receptor, but does not bind angiotensin II. Apelin, the natural ligand of APJ, was originally isolated from bovine stomach tissue (Tatemoto et al. 1998). Apelin mRNA encodes a 77-amino acid (aa) pre-proprotein that is proteolytically cleaved to yield bioactive peptides of 36, 17 and 13 aa. Each of these peptides contains the C-terminal 13 residues of the precursor protein and most bioactivity is thought to reside in this segment (Kawamata et al. 2001). The sequence of the apelin 13-peptide is the same in most vertebrates, suggesting evolutionary conservation of a critical function (Kälin et al. 2007). In our preliminary experiments, the shorter C-terminal peptide, apelin-13, with a median effective concentration (EC50) value of 0.37 nM, exhibited significantly higher activity than apelin-36 or apelin-17. Consequently, apelin-13 was used at concentrations from 10−10 to 10−7 M in our experiments. We detected expression of APJ mRNA and protein in primary HUVECs cultures, which is consistent with several previous reports (Devic et al. 1996, 1999; Katugampola et al. 2001). In contrast, Kasai et al. (2004) did not detect an APJ mRNA signal in an unidentified HUVEC-derived cell line. This could relate to the effects of cell immortalization.
In vitro exposure of HUVECs to apelin resulted in upregulation of the rate of transcription and protein secretion of several proinflammatory genes, such as ICAM-1, VCAM-1 and MCP-1. Real-time PCR studies showed that apelin caused a concentration-dependent induction of mRNA of these proinflammatory genes, with maximal expression at 10−8 apelin. This concentration-dependent effect of apelin on adhesion molecule and chemokine expressions in HUVECs is in accordance with that observed on the promotion of the acidification rate in the cells expressing the APJ receptor (Tatemoto et al. 1998). Furthermore, diverse time-dependent stimulation of ICAM-1, VCAM-1 and MCP-1 gene transcription, translation and protein secretion was observed. It can be speculated that these regulatory effects are associated with the complex features of APJ signaling. In contrast with other GPCR that are desensitized by receptor internalization following attachment of an agonist, APJ receptor signaling and receptor endocytosis are dissociated functionally (El Messari et al. 2004) via mechanism(s) that remain to be elucidated.
This study demonstrated that JNK phosphorylation, NF-κB nucleus translocation and IκB degradation are involved in apelin–APJ-induced expression of adhesion molecules and chemokines in HUVECs. The JNK protein serine/threonine kinases play a critical regulatory role in the expression of various transcription factors, such as activator protein-1 (AP-1, c-Jun/c-Fos) (Dérijard et al. 1994), and activate expression of the genes encoding ICAM-1, VCAM-1 and MCP-1 (Wang et al. 1999; Kacimi et al. 1998). NF-κB belongs to a family of transcription factors that function as dimers. This factor is a prototypic example of the family, forming a heterodimer with relA (p65) or p50 (Hayden and Ghosh 2004). In resting endothelial cells, NF-κB dimers are sequestered in an inactive form in the cytoplasm through interaction with inhibitory IκB proteins. Apelin–APJ signaling pathways leading to the activation of NF-κB function at the level of the IκB kinase (IKK) complex (Hayden and Ghosh 2004). The active form of this complex phosphorylates IκB and targets it for proteasomal degradation. This may augment the release of NF-kB and lead to its shuttling to the nucleus, and enhanced expression of ICAM-1, VCAM-1 and MCP-1 (Iademarco et al. 1992; van de Stolpe et al. 1994).
To verify the receptor-specific effect of apelin on the expression of ICAM-1, VCAM-1 and MCP-1 and on the cellular signaling in HUVECs, APJ gene expression was silenced by RNA interference. Expression cassettes encoding shRNA targeting human APJ, using cDNA 25th (siAPJ-1) and 532nd (siAPJ-2) as initiation sites, were generated and transfected into cultured HUVECs. Real-time PCR and Western blot analysis showed that siAPJ-2 blocked APJ expression. It is hypothesized that the siAPJ-1 targeting initiation site of the gene coding sequence is relatively close to the 5′-end and therefore could be shielded by regulatory proteins, thus preventing correct mRNA targeting and APJ silencing. Our results indicate that receptor-specific combination of apelin and APJ is required for apelin-induced expression of ICAM-1, VCAM-1 and MCP-1 and apelin-stimulated JNK phosphorylation, NF-κB nucleus translocation and cytoplasmic IκBα degradation in HUVECs.
Atherosclerosis is a chronic inflammatory disease of the arterial wall, characterized by the formation of lipid-laden lesions (Ross 1999). Adhesion molecules such as ICAM-1 and VCAM-1 are particularly implicated in vascular inflammation in atherogenic processes (Butcher and Picker 1996). It has been observed that these adhesion molecules mediate leukocyte capture through binding to lymphocyte integrins (Diamond et al. 1991; Barreiro et al. 2002). Leukocyte trans-endothelial migration (TEM) is a vital physiological process that occurs during further inflammatory processes. Specific chemokines (such as MCP-1 secreted by endothelial cells) attract leukocytes to migrate toward the site of the lesion (Piga et al. 2007). Apelin–APJ participates in vascular inflammation through induction of ICAM-1, VCAM-1 and MCP-1 expression in HUVECs. Apelin–APJ stimulate vascular inflammation-related atherosclerosis. It has been suggested that lowering apelin levels, silencing APJ (Hashimoto et al. 2007; Fukushima et al. 2010), or blocking the cellular JNK/NF-κB signaling (Zakkar et al. 2008) may prevent the onset of atherosclerosis. The observations made in this study provide firm proof of the role of apelin–APJ as connected to JNK pathways in generation of atherogenic linker proteins, and may provide the basis for development of drugs for the clinical treatment of human atherosclerosis.
At the G-protein level, blockade of apelin-induced activation of NF-κB/JNK by PTX indicates that G-protein heterotrimers, and in particular Gi α subunits, transduce the extracellular stimulation by APJ into an intracellular signal. This transduction should be dependent on the primary coupling of APJ to Gi-containing heterotrimers (Banères and Parello 2003), which is likely to be reduced by PTX (Estes et al. 2011). Similar evidence has already been described for the blockade of apelin-induced ERK activation by PTX and the inhibition of adenylyl cyclase by apelin (Masri et al. 2002). The JAK/STAT, NF-κB and other coupled transduction/transcription systems can be activated via G-protein heterotrimers (Hunyady and Catt 2006; Wu and Wong 2005), which should be the primary partners of APJ. A common and important feature of some active human receptors including several chemokine receptors, the apelin–APJ receptor, the neuropeptide Y Y2 receptor and the herpes virus-8 receptor is the large fraction (up to 42 %) of residues with anionic side chains (Asp, Glu and benzene anions Tyr, Trp and Phe) in the N-terminal extracellular domain (Parker et al. 2005).These receptors all transduce predominantly via Gi subunits. Apelin may also interact significantly with some of these Gi-preferring receptors (e.g., via heterodimers, or even by direct binding), and its activity could be modified by acidic oligomers and polymers. Several chemokine and chemoattractant receptors are identified as contributors to atherosclerotic plaque formation (Gautier et al. 2009). The time course of induction that we observed is at least for MCP-1 typical of processes initiated by PTX-sensitive G-proteins. The more rapid effect on VCAM-1 could indicate a more direct association of APJ with non-G-protein transduction/transcription factors affecting the expression of this adhesion molecule.
Our experiments have demonstrated that the apelin–APJ system stimulates expression of the adhesion molecules ICAM-1 and VCAM-1 and the chemokine MCP-1 in HUVECs through JNK/NF-κB signaling. These stimulatory effects on vascular endothelial cells may be involved in atherosclerosis formation. Recent studies have focused on apelin activity in atherosclerosis. Apelin levels were found to be increased in atherosclerotic coronary arteries and this additional peptide localized to the plaque, co-localizing with markers for macrophages and smooth muscle cells (Pitkin et al. 2010). Increased apelin expression within the plaque may contribute to atherogenesis. Apelin stimulates both vascular smooth muscle cell proliferation (Li et al. 2008) and the division and migration of vascular smooth muscle cells into the neointima (Kojima et al. 2010), which indicates that the apelin/APJ system may have detrimental effects on atherosclerosis. However, apelin may limit atherosclerosis progression by inhibiting the effects of angiotensin II on the vasculature (Chun et al. 2008). This is in contrast to our findings. Other studies have identified decreased (Tasci et al. 2007; Sonmez et al. 2010) or unchanged (Rittig et al. 2011) levels of apelin in atherosclerosis-related diseases. Whether apelin/APJ activation is beneficial or detrimental in atherosclerosis requires further investigation using agonists and, in particular, apelin receptor-selective antagonists. However, our data indicate that the apelin–APJ system is involved in the initiation of atherosclerosis through endothelial inflammation-related pathways, providing further evidence in support of the apelin receptor as a target for therapeutic drug development in this condition.
References
Banères JL, Parello J (2003) Structure-based analysis of GPCR function: evidence for a novel pentameric assembly between the dimeric leukotriene B4 receptor BLT1 and the G-protein. J Mol Biol 329:815–829
Barnes G, Japp AG, Newby DE (2010) Translational promise of the apelin–APJ system. Heart 96:1011–1016
Barreiro O, Yanez-Mo M, Serrador JM, Montoya MC, Vicente-Manzanares M, Tejedor R, Furthmayr H, Sanchez-Madrid F (2002) Dynamic interaction of VCAM-1 and ICAM-1 with moesin and ezrin in a novel endothelial docking structure for adherent leukocytes. J Cell Biol 157:1233–1245
Blankenberg S, Barbaux S, Tiret L (2003) Adhesion molecules and atherosclerosis. Atherosclerosis 170:191–203
Boucher J, Masri B, Daviaud D, Gesta S, Guigné C, Mazzucotelli A, Castan-Laurell I, Tack I, Knibiehler B, Carpéné C, Audigier Y, Saulnier-Blache JS, Valet P (2005) Apelin, a newly identified adipokine up-regulated by insulin and obesity. Endocrinology 146:1764–1771
Butcher EC, Picker LJ (1996) Lymphocyte homing and homeostasis. Science 272:60–66
Carmody RJ, Ruan Q, Palmer S, Hilliard B, Chen YH (2007) Negative regulation of toll-like receptor signaling by NF-kappaB p50 ubiquitination blockade. Science 317:675–678
Chun HJ, Ali ZA, Kojima Y, Kundu RK, Sheikh AY, Agrawal R, Zheng L, Leeper NJ, Pearl NE, Patterson AJ, Anderson JP, Tsao PS, Lenardo MJ, Ashley EA, Quertermous T (2008) Apelin signaling antagonizes Ang II effects in mouse models of atherosclerosis. J Clin Invest 118:3343–3354
Cui RR, Mao DA, Yi L, Wang C, Zhang XX, Xie H, Wu XP, Liao XB, Zhou H, Meng JC, Yuan LQ, Liao EY (2010) Apelin suppresses apoptosis of human vascular smooth muscle cells via APJ/PI3-K/Akt signaling pathways. Amino Acids 39:1193–1200
Dérijard B, Hibi M, Wu IH, Barrett T, Su B, Deng T, Karin M, Davis RJ (1994) JNK1: a protein kinase stimulated by UV light and Ha-Ras that binds and phosphorylates the c-Jun activation domain. Cell 76:1025–1037
Devic E, Paquereau L, Vernier P, Knibiehler B, Audigier Y (1996) Expression of a new G protein-coupled receptor X-msr is associated with an endothelial lineage in Xenopus laevis. Mech Dev 59:129–140
Devic E, Rizzoti K, Bodin S, Knibiehler B, Audigier Y (1999) Amino acid sequence and embryonic expression of msr/apj, the mouse homolog of Xenopus X-msr and human APJ. Mech Dev 84:199–203
Diamond MS, Staunton DE, Marlin SD, Springer TA (1991) Binding of the integrin Mac-1 (CD11b/CD18) to the third immunoglobulin-like domain of ICAM-1 (CD54) and its regulation by glycosylation. Cell 65:961–971
Dray C, Knauf C, Daviaud D, Waget A, Boucher J, Buléon M, Cani PD, Attané C, Guigné C, Carpéné C, Burcelin R, Castan-Laurell I, Valet P (2008) Apelin stimulates glucose utilization in normal and obese insulin-resistant mice. Cell Metab 8:437–445
El Messari S, Iturrioz X, Fassot C, De Mota N, Roesch D, Llorens-Cortes C (2004) Functional dissociation of apelin receptor signaling and endocytosis: implications for the effects of apelin on arterial blood pressure. J Neurochem 90:1290–1301
Estes AM, McAllen K, Parker MS, Sah R, Sweatman T, Park EA, Balasubramaniam A, Sallee FR, Walker MW, Parker SL (2011) Maintenance of Y receptor dimers in epithelial cells depends on interaction with G-protein heterotrimers. Amino Acids 40:371–380
Eyries M, Siegfried G, Ciumas M, Montagne K, Agrapart M, Lebrin F, Soubrier F (2008) Hypoxia-induced apelin expression regulates endothelial cell proliferation and regenerative angiogenesis. Circ Res 103:432–440
Feng L, Matsumoto C, Schwartz A, Schmidt AM, Stern DM, Pile-Spellman J (2005) Chronic vascular inflammation in patients with type 2 diabetes: endothelial biopsy and RT-PCR analysis. Diabetes Care 28:379–384
Fukushima H, Kobayashi N, Takeshima H, Koguchi W, Ishimitsu T (2010) Effects of olmesartan on Apelin/APJ and Akt/endothelial nitric oxide synthase pathway in Dahl rats with end-stage heart failure. J Cardiovasc Pharmacol 55:83–88
Gautier EL, Jakubzick C, Randolph GJ (2009) Regulation of the migration and survival of monocyte subsets by chemokine receptors and its relevance to atherosclerosis. Arterioscler Thromb Vasc Biol 29:1412–1418
Gu L, Okada Y, Clinton SK, Gerard C, Sukhova GK, Libby P, Rollins BJ (1998) Absence of monocyte chemoattractant protein-1 reduces atherosclerosis in low density lipoprotein receptor-deficient mice. Mol Cell 2:275–281
Hashimoto T, Kihara M, Imai N, Yoshida S, Shimoyamada H, Yasuzaki H, Ishida J, Toya Y, Kiuchi Y, Hirawa N, Tamura K, Yazawa T, Kitamura H, Fukamizu A, Umemura S (2007) Requirement of apelin–apelin receptor system for oxidative stress-linked atherosclerosis. Am J Pathol 171:1705–1712
Hayden MS, Ghosh S (2004) Signaling to NF-kappaB. Genes Dev 18:2195–2224
Hunyady L, Catt KJ (2006) Pleiotropic AT1 receptor signaling pathways mediating physiological and pathogenic actions of angiotensin II. Mol Endocrinol 20:953–970
Iademarco MF, McQuillan JJ, Rosen GD, Dean DC (1992) Characterization of the promoter for vascular cell adhesion molecule-1 (VCAM-1). J Biol Chem 267:16323–16329
Jaffe EA, Nachman RL, Becker CG, Minick CR (1973) Culture of human endothelial cells derived from umbilical veins. Identification by morphologic and immunologic criteria. J Clin Invest 52:2745–2756
Kacimi R, Karliner JS, Koudssi F, Long CS (1998) Expression and regulation of adhesion molecules in cardiac cells by cytokines: response to acute hypoxia. Circ Res 82:576–586
Kälin RE, Kretz MP, Meyer AM, Kispert A, Heppner FL, Brändli AW (2007) Paracrine and autocrine mechanisms of apelin signaling govern embryonic and tumor angiogenesis. Dev Biol 305:599–614
Karmazyn M, Purdham DM, Rajapurohitam V, Zeidan A (2008) Signalling mechanisms underlying the metabolic and other effects of adipokines on the heart. Cardiovasc Res 79:279–286
Kasai A, Shintani N, Oda M, Kakuda M, Hashimoto H, Matsuda T, Hinuma S, Baba A (2004) Apelin is a novel angiogenic factor in retinal endothelial cells. Biochem Biophys Res Commun 325:395–400
Katugampola SD, Maguire JJ, Matthewson SR, Davenport AP (2001) ((125)I)-(Pyr(1)) Apelin-13 is a novel radioligand for localizing the APJ orphan receptor in human and rat tissues with evidence for a vasoconstrictor role in man. Br J Pharmacol 132:1255–1260
Kawamata Y, Habata Y, Fukusumi S, Hosoya M, Fujii R, Hinuma S, Nishizawa N, Kitada C, Onda H, Nishimura O, Fujino M (2001) Molecular properties of apelin: tissue distribution and receptor binding. Biochim Biophys Acta 1538:162–171
Kojima Y, Kundu RK, Cox CM, Leeper NJ, Anderson JA, Chun HJ, Ali ZA, Ashley EA, Krieg PA, Quertermous T (2010) Upregulation of the apelin–APJ pathway promotes neointima formation in the carotid ligation model in mouse. Cardiovasc Res 87:156–165
Li F, Li L, Qin X, Pan W, Feng F, Chen F, Zhu B, Liao D, Tanowitz H, Albanese C, Chen L (2008) Apelin-induced vascular smooth muscle cell proliferation: the regulation of cyclin D1. Front Biosci 13:3786–3792
Libby P (2002) Inflammation in atherosclerosis. Nature 420:868–874
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)). Methods 25:402–408
Masri B, Lahlou H, Mazarguil H, Knibiehler B, Audigier Y (2002) Apelin (65-77) activates extracellular signal-regulated kinases via a PTX-sensitive G protein. Biochem Biophys Res Commun 290:539–545
Miller AP, Chen YF, Xing D, Feng W, Oparil S (2003) Hormone replacement therapy and inflammation: interactions in cardiovascular disease. Hypertension 42:657–663
O’Dowd BF, Heiber M, Chan A, Heng HH, Tsui LC, Kennedy JL, Shi X, Petronis A, George SR, Nguyen T (1993) A human gene that shows identity with the gene encoding the angiotensin receptor is located on chromosome 11. Gene 136:355–360
Parker SL, Parker MS, Sah R, Sallee F (2005) Angiogenesis and rhodopsin-like receptors: a role for N-terminal acidic residues? Biochem Biophys Res Commun 335:983–992
Pate M, Damarla V, Chi DS, Negi S, Krishnaswamy G (2010) Endothelial cell biology: role in the inflammatory response. Adv Clin Chem 52:109–130
Piga R, Naito Y, Kokura S, Handa O, Yoshikawa T (2007) Short-term high glucose exposure induces monocyte-endothelial cells adhesion and transmigration by increasing VCAM-1 and MCP-1 expression in human aortic endothelial cells. Atherosclerosis 193:328–334
Pitkin SL, Maguire JJ, Kuc RE, Davenport AP (2010) Modulation of the apelin/APJ system in heart failure and atherosclerosis in man. Br J Pharmacol 160:1785–1795
Rautou PE, Vion AC, Amabile N, Chironi G, Simon A, Tedgui A, Boulanger CM (2011) Microparticles, vascular function, and atherothrombosis. Circ Res 109:593–606
Rittig K, Hildebrandt U, Thamer C, Staiger H, Peter A, Stefan N, Fritsche A, Häring HU, Balletshofer BM, Siegel-Axel D (2011) Apelin serum levels are not associated with early atherosclerosis or fat distribution in young subjects with increased risk for type 2 diabetes. Exp Clin Endocrinol Diabetes 119:358–361
Ross R (1999) Atherosclerosis—an inflammatory disease. N Engl J Med 340:115–126
Seehaus S, Shahzad K, Kashif M, Vinnikov IA, Schiller M, Wang H, Madhusudhan T, Eckstein V, Bierhaus A, Bea F, Blessing E, Weiler H, Frommhold D, Nawroth PP, Isermann B (2009) Hypercoagulability inhibits monocyte transendothelial migration through protease-activated receptor-1-, phospholipase-Cbeta-, phosphoinositide 3-kinase-, and nitric oxide-dependent signaling in monocytes and promotes plaque stability. Circulation 120:774–784
Shan PF, Lu Y, Cui RR, Jiang Y, Yuan LQ, Liao EY (2011) Apelin attenuates the osteoblastic differentiation of vascular smooth muscle cells. PLoS ONE 6:e17938
Sonmez A, Celebi G, Erdem G, Tapan S, Genc H, Tasci I, Ercin CN, Dogru T, Kilic S, Uckaya G, Yilmaz MI, Erbil MK, Kutlu M (2010) Plasma apelin and ADMA levels in patients with essential hypertension. Clin Exp Hypertens 32:179–183
Tasci I, Dogru T, Naharci I, Erdem G, Yilmaz MI, Sonmez A, Bingol N, Kilic S, Bingol S, Erikci S (2007) Plasma apelin is lower in patients with elevated LDL-cholesterol. Exp Clin Endocrinol Diabetes 115:428–432
Tatemoto K, Hosoya M, Habata Y, Fujii R, Kakegawa T, Zou MX, Kawamata Y, Fukusumi S, Hinuma S, Kitada C, Kurokawa T, Onda H, Fujino M (1998) Isolation and characterization of a novel endogenous peptide ligand for the human APJ receptor. Biochem Biophys Res Commun 251:471–476
Van de Stolpe A, Caldenhoven E, Stade BG, Koenderman L, Raaijmakers JA, Johnson JP, van der Saag PT (1994) 12-O-tetradecanoylphorbol-13-acetate-and tumor necrosis factor alpha-mediated induction of intercellular adhesion molecule-1 is inhibited by dexamethasone. Functional analysis of the human intercellular adhesion molecular-1 promoter. J Biol Chem 269:6185–6192
Wang N, Verna L, Hardy S, Forsayeth J, Zhu Y, Stemerman MB (1999) Adenovirus-mediated overexpression of c-Jun and c-Fos induces intercellular adhesion molecule-1 and monocyte chemoattractant protein-1 in human endothelial cells. Arterioscler Thromb Vasc Biol 19:2078–2084
Wu EH, Wong YH (2005) Pertussis toxin-sensitive Gi/o proteins are involved in nerve growth factor-induced pro-survival Akt signaling cascade in PC12 cells. Cell Signal 17:881–890
Yamawaki H, Pan S, Lee RT, Berk BC (2005) Fluid shear stress inhibits vascular inflammation by decreasing thioredoxin-interacting protein in endothelial cells. J Clin Invest 115:733–738
Yuan LQ, Liu W, Cui RR, Wang D, Meng JC, Xie H, Wu XP, Zhou HD, Lu Y, Liao EY (2010) Taurine inhibits osteoclastogenesis through the taurine transporter. Amino Acids 39:89–99
Zakkar M, Chaudhury H, Sandvik G, Enesa K, le Luong A, Cuhlmann S, Mason JC, Krams R, Clark AR, Haskard DO, Evans PC (2008) Increased endothelial mitogen-activated protein kinase phosphatase-1 expression suppresses proinflammatory activation at sites that are resistant to atherosclerosis. Circ Res 103:726–732
Zeng XX, Wilm TP, Sepich DS, Solnica-Krezel L (2007) Apelin and its receptor control heart field formation during zebrafish gastrulation. Dev Cell 12:391–402
Zhan Y, Brown C, Maynard E, Anshelevich A, Ni W, Ho IC, Oettgen P (2005) Ets-1 is a critical regulator of Ang II-mediated vascular inflammation and remodeling. J Clin Invest 115:2508–2516
Acknowledgments
We thank the National Natural Science Foundation of China (No. 30801174, 81070246 and 30900622), China Postdoctoral Science Foundation (20100471240), the Ph.D. Programs Foundation of Ministry of Education of China (No.200805331017) and Clinic Medicine Special Research Fund-Endocrinology Disease Research Fund of Chinese Medical Association (10020040226).
Author information
Authors and Affiliations
Corresponding authors
Additional information
The authors Y. Lu and X. Zhu contributed equally to this work.
Rights and permissions
About this article
Cite this article
Lu, Y., Zhu, X., Liang, GX. et al. Apelin–APJ induces ICAM-1, VCAM-1 and MCP-1 expression via NF-κB/JNK signal pathway in human umbilical vein endothelial cells. Amino Acids 43, 2125–2136 (2012). https://doi.org/10.1007/s00726-012-1298-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-012-1298-7