Abstract
Aim of the present study was to investigate the neuroprotective effect of dental pulp cells (DPCs) in in vitro models of Alzheimer and Parkinson disease. Primary cultures of hippocampal and ventral mesencephalic neurons were treated for 24 h with amyloid beta (Aβ1–42) peptide 1–42 and 6-OHDA, respectively. DPCs isolated from adult rat incisors were previously cultured in tissue culture inserts and added to the neuron cultures 2 days prior to neurotoxin treatment. Cell viability was assessed by the MTT assay. The co-culture with DPCs significantly attenuated 6-OHDA and Aβ1–42-induced toxicity in primary cultures of mesencephalic and hippocampal neurons, and lead to an increase in neuronal viability in untreated cultures, suggesting a neurotrophic effect in both models. Furthermore, human dental pulp cells expressed a neuronal phenotype and produced the neurotrophic factors NGF, GDNF, BDNF, and BMP2 shown by microarray screening and antibody staining for the representative proteins. DPCs protected primary neurons in in vitro models of Alzheimer’s and Parkinson’s disease and can be viewed as possible candidates for studies on cell-based therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s (AD) and Parkinson’s disease (PD) are the first and second commonest age-related neurodegenerative disorders of unknown aetiology. Especially AD is referred to as the pandemic of the twentyfirst century, with a strong influence on the national economy of the industrialized countries. So far both AD and PD are predominantly treated symptomatically.
High hopes have been pinned on the prospects of using stem and progenitor cell-based therapy in the central nervous system. Clinical studies involving intrastriatal transplantation of embryonic mesencephalic tissue in patients with PD have provided proof-of-principle for the cell replacement strategy in this disorder.
The dental pulp contains a population of multipotent stem cells with the capacity to differentiate into several different cells lineages in vitro and in vivo, including glial and nerve cells (Gronthos et al. 2002; Miura et al. 2003). Dental pulp cells (DPCs) originate from the cranial neural crest and share neuronal characteristics, including the production of neurotrophic factors like nerve growth factor (NGF), brain-derived neurotrophic factor (BDNF) and glial cell-line derived neurotrophic factor (GDNF) (Nosrat et al. 2001). The neuroprotective effects of these factors are well-established (Heese et al. 2006; Lin et al. 1993). The release of neurotrophic factors by genetically modified cells has proven to be successful (Arenas and Persson 1994; Arenas et al. 1995). Other cells and tissue can also produce neurotrophic factors and have been grafted into the brain, leading to functional recovery in animal models of PD (Sanberg et al. 1997; Espejo et al. 1998; Granholm et al. 1998; Choi-Lundberg and Rosenthal 1999).
Both in vitro and in vivo, NGF, BDNF, and GDNF produced by DPCs from neonatal rats have been found to promote the survival of sensory and dopaminergic neurons, and to favour the rescue of motorneurons in an animal model of spinal cord injury (Nosrat et al. 2001, 2004). Here, we describe for the first time the neuroprotective effect of DPCs derived from adult rodents in in vitro models of AD and PD. The present evidence suggests that DPCs maybe viewed as a potential source of adult multipotent cells, with promising implications for the development of cell-based therapy models in neurodegenerative disorders.
Materials and methods
The animal experiments were approved by the animal care ethics committee of the University of São Paulo, Brazil and all national guidelines were taken into consideration.
Primary cultures of hippocampal neurons
Pregnant Wistar rats were killed by cervical dislocation at gestational day 18 (E18), and the respective embryos obtained by laparotomy. Whole embryonic brains were isolated and kept immersed on Hank’s balanced salt solution (HBSS, Gibco) through micro-dissection, yielding multiple samples of hippocampal tissue. Single cell suspensions were obtained by trypsinisation followed by mechanical dissociation with fire-polished Pasteur pipettes. Cells were counted and re-suspended in Neurobasal medium containing B-27 supplement (both Gibco), 2 mM glutamine, penicillin (100 IU), streptomycin (100 μg/ml), and 5% foetal calf serum (LGC Biotechnologia, Cotia, Brazil). Cells were plated onto poly-d-lysine coated 24-well plates at a density of 5 × 104 cells per culture well. Culture medium was replaced by serum-free media after 24 h of incubation and half-changed every 48 h. Cultures were incubated for 7 days at 37°C/5% CO2. Experiments were performed on day 7 in culture, at which time pyramidal neurons are fully differentiated.
Primary cultures of mesencephalic neurons
Mesencephalic cells were isolated from embryonic brains obtained from female Wistar rats, at gestational days 14–15 (E14–15). The ventral mesencephalon (VM) was dissected using a lateral approach described by Dunnet and Björklund (1999). After treatment with trypsin and mechanical dissection with fire-polished Pasteur pipettes, the cells were resuspended in Neurobasal Medium with 2 mM l-glutamine, supplemented with B-27 Supplement (both Gibco), containing streptomycin (100 μg/ml), penicillin (100 IU), and 5% foetal calf serum (LGC Biotechnologia, Cotia, Brazil). The cell suspension was plated on 24-well plates coated with poly-l-lysine (100 μg/ml), at a density of 5 × 104 cells/well. Cultures were maintained at 37°C under a 5% CO2 atmosphere. Culture medium was replaced by serum-free media after 24 h of incubation and half-changed every 48 h.
Isolation and cultivation of dental pulp cells
The same pregnant rats killed by cervical dislocation to obtain the embryos for neuronal cultures were used to provide DPCs. Both maxillary and mandibular incisors were dissected, and the surfaces of the teeth were cleaned with 70% alcohol. Apical areas were then removed to decrease the influence from periodontal and periapical tissue, and dental pulps were removed. The pulp tissue was digested in a solution of 3 mg/ml collagenase type I and 4 mg/ml dispase (both Sigma, Steinheim, Germany) for 1 h at 37°C. Single-cell suspensions were obtained by passing the cells through a 70-μm strainer (BD, Heidelberg, Germany). Then, the dental pulp cells were seeded in culture flasks containing an α-modification of Eagle’s medium supplemented with 10% FCS (both LGC Biotechnologia, Cotia, Brazil), streptomycin (100 μg/ml), and penicillin (100 IU) and incubated at 37°C in 5% CO2.
The third passage of isolated cells was harvested and suspended in culture medium containing 10% (v/v) dimethyl sulfoxide (DMSO) and stored at −80°C. For the experiment, the cryopreserved rat dental pulp cells were thawed and expanded in the medium as described above. After reaching a confluent stage, the cells were removed with TrypleLE Express (Invitrogen) and cultured on cell culture inserts to enable a co-culture with the neurons. Cells from the fourth up to the seventh passage were used for the experiments.
Human dental pulp cells were used for basic characterization. To this end normal human impacted third molars were collected. Tooth surfaces were cleaned and cut around the cementum–enamel junction by using sterilized dental burs to reveal the pulp chamber. The pulp tissue was separated from the crown and roots and digested in a solution of 3 mg/ml collagenase type I and 4 mg/ml dispase (both from Sigma, Steinheim, Germany) for 1 h at 37°C. Single-cell suspensions were obtained by passing the cells through a 70-μm strainer (BD, Heidelberg, Germany). Then, the DPCs were seeded in culture flasks containing an α-modification of Eagle’s medium (Gibco, Karlsruhe, Germany) supplemented with 20% foetal calf serum (FCS; PAA, Cölbe, Germany), 100 mM l-ascorbic-acid-2-phosphate (Sigma, Steinheim, Germany), and 50 mg/ml Gentamycine (Gibco, Karlsruhe, Germany). The procedure was approved by the local University committee on Ethics in Medicine.
Co-culture and neurotoxin treatment
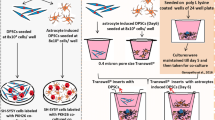
To prevent direct contact between DPCs and neurons, tissue culture inserts with a pore size of 1 μm (BD, Franklin Lakes, USA) were used. The DPCs were seeded at a density of 5 × 104 cells per insert and cultured until confluency. On day 5 of the neuron cultures the inserts with the DPCs were added to the neurons. After 2 days of co-culture (day 7 of the neuron culture) the neurotoxins were added.
Amyloid-β peptide (1–42) was purchased from Bachem (H-1368; Torrance, USA), solved in sterilized Milli-Q water at a concentration of 500 μM, and aged for 6 days at 37°C (Perini et al. 2002). Thereafter, a freeze thaw cycle was included. Aβ1–42 was added to the hippocampal neuron cultures at day 7 in final concentrations of 5 and 10 μM.
6-OHDA (Tocris Bioscience, Ellisville, USA) was solved in sterilized Milli-Q water containing 0.1% ascorbic acid. At day 7, 6-OHDA was added to the ventral mesencephalic neuron cultures in final concentrations of 5 and 40 μM. All neurotoxins lasted 24 h at the neuronal cell cultures. Thereafter, the cell culture inserts with the DPCs and the medium were removed and 500 μl fresh medium was added. The viability of the neurons was assessed by MTT assay; 50 μl MTT (5 mg/ml PBS) was added to the cell culture and incubated for 3 h. For the solubilization of the formazan precipitates 500 μl of 10% SDS in 0.01 N HCl was added and incubated overnight. The absorbance was measured with a microplate reader at 570 nm using 690 nm as reference. The inhibition of MTT reduction indicates the degree of neurotoxin-induced toxicity. All experiments were performed in triplicates and repeated three times in different days using fresh neuronal cultures and pulp cell lines.
Microarray analysis
Microarray analysis was used as a primary explorative screen to identify a set of genes that were expressed by human dental pulp cells. Total RNA was isolated using the Qiagen RNeasy kit. RNA quality was assessed using the RNA 6000 Nano Assay (Agilent Bioanalyser) and RNA quantity was assessed using the NanoDrop 1000. All further processing of the total RNA (1.2 μg, RNA integrity number of 10) was performed according the GeneChip® Whole Transcript (WT) Sense Target Labeling Assay Manual (Affymetrix). The fragmented labelled sample was hybridized to an Affymetrix GeneChip Human Exon 1.0 ST Array (1.4 million probe sets covering >1 million exon clusters). The microarray analysis was performed using Bioconductor (Gentleman et al. 2004) packages under R 2 (Team 2006). For this study, we used expression data of the 20,011 core annotated genes that are supported by putative full-length mRNA from, e.g. the RefSeq database (Geo dataset accession number GSE9385).
Only genes with signal intensity higher than the mean of all negative controls (n = 2,904) plus three times the SD or rather, signal intensity higher than five times the mean of all negative controls were considered as truly expressed. The values in the graph are given in log2 of fold over the mean of the negative controls.
Immunocytochemistry
Human dental pulp cells were grown on glass chamber slides (Lab-Tek Chamber Slide, Nunc, Germany) and fixed with 4% paraformaldehyde in PBS for 20 min at room temperature. The cells were then permeabilized in PBS with 0.15% Triton X-100 including 10% donkey serum (Sigma, Steinheim, Germany) and incubated with the following primary antibodies: mouse monoclonal anti-beta 3 tubulin (clone Tuj-1, 1:2000, overnight, Promega), rabbit polyclonal anti- microtuble associated protein (MAP2, 1:100, overnight, Chemicon), rabbit polyclonal anti-brain derived neurotrophic factor (BDNF, 1:50, overnight, Santa Cruz Biotechnology), mouse monoclonal anti-human neuron specific enolase (NSE, 1:20, 45 min, Dako), mouse monoclonal anti-human glial fibrillary acidic protein (GFAP, 1:10, 45 min, Dako), goat polyclonal anti-bone morphogenic protein 2 (BMP2, 1:50, 45 min, Santa Cruz Biotechnology), mouse monoclonal anti-human nestin (1:100, overnight, R&D Systems), goat polyclonal anti-glial cell derived neurotrophic facor (GDNF, 1:100, overnight, R&D Systems), goat polyclonal anti-human beta nerve growth factor (NGF, 1:100, overnight, R&D Systems). Secondary antibodies were donkey anti-mouse IgG-NL493, anti-goat IgG-NL557 (both R&D Systems) and donkey anti-rabbit IgG-FITC (Santa Cruz Biotechnology). Nuclei were counterstained with DAPI. Negative controls were processed in the same way, except that the first antibody was replaced with an isotype-matched negative control antibody.
Results
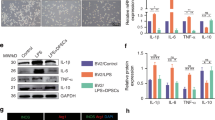
Exposure to 6-OHDA for 24 h resulted in a concentration-dependent decrease in the viability of VM cell cultures, as measured by the MTT assay [14.2% (SD ±1.6%) at a concentration of 5 μM, and 53.6% (SD ±1.8%) at 40 μM of 6-OHDA] compared to the viability of untreated controls (100%). Interestingly, we observed an increment of 16.0% (SD ±1.0%) in the viability of untreated neurons in co-culture with DPCs (a positive control of the DPC model), which suggests a neurotrophic effect. In addition, the co-culture with DPCs prevented or attenuated the 6-OHDA-induced loss of viability of primary cultures of VM neurons. At lower concentrations of 6-OHDA (5 μM), the final viability of VM neurons in co-culture with DPCs was 94.1% (SD ±4.2%) and significantly higher compared to the group without DPCs in co-culture [85.8% (SD ±1.6%), P = 0.0058); at higher, neurotoxic concentrations (40 μM), the co-culture with DPCs increased the survival rate of VM neurons by 16.5%. This difference was also statistically significant (P < 0.0001) (Fig. 1).
Primary cultures of ventral mesencephalic neurons treated with 6-OHDA (5 and 40 µM) for 24 h with and without DPCs in co-culture, and respective controls. Cell viability was evaluated by MTT assay. The data are reported as means ± SD from three distinct experiments measured in triplets, considering controls = 100% for each distinct experiment. ANOVA and Tuckey post hoc tests at α = 5% display statistical significant differences between the means (P < 0.0001). Columns with different letters display a statistical significant difference (P < 0.05)
Similar findings were observed in the Aβ-induced neurotoxicity model, although with some more variability across different experiments, as compared to the 6-OHDA model. Treatment with Aβ1–42 for 24 h significantly reduced the viability of primary cultures of hippocampal neurons. As compared to controls, the mean reduction of viability in cultures treated with 5 and 10 μM of Aβ1–42 was of 16.3% (SD ±6.2%) and 31.8% (SD ±7.2%), respectively. In all experiments the co-culture with DPCs partially prevented the loss of viability induced by treatment with Aβ1–42 (Figs. 2, 3). This neuroprotective effect was in a range of 10% in both 5 and 10 μM Aβ1–42, respectively. At lower concentrations of Aβ1–42 (5 μM), the final viability of hippocampal neurons in co-culture with DPCs was not significantly different from that of the controls (P = 0.9498). Equally to the PD model, the DPCs lead to an increased number of viable cells in the positive control, as shown by a 10.1% (SD ±1.3%) increase in the output of the MTT assay (Figs. 2, 3).
Primary cultures of hippocampal neurons treated with Aβ1–42 (5 and 10 µM) for 24 h with and without DPCs in co-culture, and respective controls. Cell viability was evaluated by MTT assay. The data are reported as means ± SD from three distinct experiments measured in triplets, considering controls = 100% for each distinct experiment. ANOVA and Tuckey post hoc tests at α = 5% display statistical significant differences between the means (P < 0.0001). Columns with different letters display a statistical significant difference (P < 0.05)
The data obtained from microarray analysis revealed that human DPCs express many genes related to cells with neural phenotype (Fig. 4). All neurotrophins, except neurotrophin 4/5, and also GDNF were expressed by the DPCs above a stringent threshold. Additionally, the growth factors BMP2 and bFGF are also present at a higher level.
Expression profile of selected mRNAs related to a neural phenotype in human dental pulp cells. Given is the log2 value of the fold factor over the baseline. The baseline represents the mean of all (2,904) negative controls (NC) on the array. Threshold 1 (dashed line) marks the log2 value of the NC plus three times the SD. Threshold 2 (continuous line) indicates the log2 value of five times the NC
Interestingly, DPCs express neuron specific markers like NSE, and beta-tubulin 3 on the genomic level, but also nestin and GFAP. MAP2 was just expressed below the threshold, but could be also detected with immunofluorescent staining.
Immunocytochemical staining with some selected antibodies supported the findings received from microarray analysis on the protein level. DPCs clearly produce the growth factors NGF, BDNF, GDNF and BMP2. Furthermore, human DPCs are immunopositive for the neuron markers NSE, beta-tubulin III and MAP2. Nestin, a marker for neuronal stem cells, is also present in DPCs (Fig. 5).
Immunofluorescent staining of the neuronal markers beta tubulin 3, microtubule associated protein 2 (MAP2), neuron specific enolase (NSE), the growth factors glial cell derived neurotrophic factor (GDNF), nerve growth factor (NGF), brain derived neurotrophic factor (BDNF), and bone morphogenetic protein 2 (BMP2), as well as for the intermediate filaments glial fibrillary acidic protein (GFAP) and nestin. Scale bar 50 µm
Discussion
Because the available therapies for AD and PD remain up to now symptomatic, and are unlikely to prevent further neurodegeneration, cell-replacement strategies are of interest to be developed. The ability to both avoid neuronal death and to repair and regenerate the diseased nervous system is currently the investigational horizon for regenerative medicine. For this, neural stem cells that can be derived either from the CNS itself or from pluripotent embryonic stem cells (ESCs), are promising candidates. Their ability to ameliorate symptoms and to improve functional recovery has been demonstrated in various animal models. Furthermore, allografted tissue from fetal ventral mesencephalon has proven the principle of cell replacement therapy in clinical trails of PD (Lindvall and Hagell 2001). However, due to controversial results and the fact that research involving ESCs has received significant opposition over the years because of the obvious ethical concerns, and due to the limited availability of fetal tissue, alternative strategies should be developed. Over the past years, evidence has accumulated indicating that adult stem cells might have pluripotent properties similar to ESC. Especially bone marrow stromal mesenchymal stem cells (BMSC) have received most attention (Hellmann et al. 2006). However, at this stage it is not foreseeable whether adult stem cells are useful in the CNS and the search for a “perfect cell” is ongoing.
Given the properties of DPCs to differentiate into neurons and glial cells, in addition to their potential to secrete several neurotrophic factors (Nosrat et al. 2001; Gronthos et al. 2002; Miura et al. 2003), the current study shed some additional insight to the recent publications that support the potential use of DPCs in cell-replacement therapy. We provide evidence that DPCs derived from adult rodents may protect neurons in in vitro models of Alzheimer’s and Parkinson’s disease. Furthermore, we also show a neurotrophic effect of DPCs when co-cultivated with neurons.
Direct induced toxicity of amyloid beta peptide (1–42) in hippocampal neurons and 6-OHDA-induced death in ventral mesencephalic neurons are widely used in vitro models to study protective effects in AD and PD regimes. The direct, toxic properties of Aβ-related fragments (Aβ 1–40, Aβ 1–42, Aβ 25–35) in cultured rat and human neurons and in in vivo models are well established (Busciglio et al. 1993; Loo et al. 1993; Maurice et al. 1996). The noradrenergic analog 6-OHDA has been introduced as catecholaminergic neurotoxin over 30 years ago and has remained extensively used for both in vitro and in vivo investigations. The formation of reactive oxygen species (ROS) by the autooxidation of 6-OHDA is considered as the main molecular mechanism underlying the neurotoxicity of 6-OHDA (Dauer and Przedborski 2003).
The treatment of the VM cultures with 6-OHDA in the present experiments caused a reproducible and dose-dependent loss in cell viability. This toxic effect could be prevented or attenuated by the co-culture with rodent DPCs. The toxic effect of the Aβ1–42 was more fluctuating compared to the effect of the 6-OHDA. This observation is maybe related to fact that different batches of Aβ1–42 were used. The solubilization of the peptide and the formation of the toxic fibrils are crucial steps during preparation. However, in all experiments a neuroprotective effect of the DPCs could be observed. This effect was less intense in the AD than in the in the PD model. The observation of the neuroprotection in both, the AD and PD model suggests that the underlying effect is mediated by the same factors. Because in our experimental setup the direct contact of the neurons with the DPCs is prevented, we assume that secreted factors seem to be responsible for the observed neuroprotection. Neurotrophins produced by the DPCs are possibly favourable candidates.
Despite the knowledge, that DNA-microarrays are generally used for comparative studies and in awareness of possible pitfalls, like variations deriving from heterogeneous cell populations, we have used this technology for a primary explorative screen to identify genes that were expressed by human dental pulp cells. Because the noise and background of microarray data can influence the interpretation of the results and because we did not include replications in our study, two internal thresholds were set. First, the log2 value of the onefold mean of all negative control probeset s (n = 2,904) plus three times the SD and second, the log2 value of five times the mean of all negative control probesets. Just above these values the representative genes were considered genes as truly expressed.
Because DNA microarray technology is limited to the study of gene expression at the mRNA level and do not necessarily correlate with protein levels, we included a verification of these explorative data by immunocytochemical staining for some selected representative proteins.
Combining the data obtained, there is clear evidence that DPCs express different markers related to cells with a neuronal phenotype. Among these, markers considered to be specific for neuronal cells, like MAP2, beta tubulin 3 and NSE. Furthermore, human DPCs express nestin, a marker for neuronal stem cells. Mesenchymal stem cells expressing nestin have been shown to be able to differentiate into functional neurons (Wislet-Gendebien et al. 2005).
The expression of neurotrophins by DPCs has been described previously (Nosrat et al. 2001). Especially NGF and GDNF have shown to support the survival of neurons in vitro and in vivo. Additionally, BMP2 and FGF2 are also known for their neurotrophic support (Jordan et al. 1997; Reuss and von Bohlen und Halbach 2003). All of these growth factors are expressed by DPCs and probably released in the cell culture medium.
In conclusion, the results of the present study support the use of dental pulp as an alternative source of multipotent cells, rendering DPCs promising candidates for cell based therapies for CNS disorders. The DPCs are easily available from adult subjects, and this procedure is devoid of any relevant ethical concerns. In addition, DPCs can be easily handled in laboratory, being expandable and robust in culture as well as cryopreservable. However, future studies should clarify whether the DPCs, beside the neurotrophic and neuroprotective effects, are also able to differentiate into fully functional neurons.
References
Arenas E, Persson H (1994) Neurotrophin-3 prevents the death of adult central noradrenergic neurons in vivo. Nature 367:368–371
Arenas E, Trupp M, Akerud P, Ibanez CF (1995) GDNF prevents degeneration and promotes the phenotype of brain noradrenergic neurons in vivo. Neuron 15:1465–1473
Busciglio J, Yeh J, Yankner BA (1993) Beta-amyloid neurotoxicity in human cortical culture is not mediated by excitotoxins. J Neurochem 61:1565–1568
Choi-Lundberg D, Rosenthal A (1999) Autotransplantation for Parkinson’s disease goes a step further. Neuron 22:635–636
Dauer W, Przedborski S (2003) Parkinson’s disease: mechanisms and models. Neuron 39:889–909
Dunnet SB, Björklund A (1999) Dissecting embryonic neural tissue for transplantation. In: Stephen B. Dunnett, Alan A. Boulton, Glen B. Baker (eds) Neural transplantation methods. 1st edn. Humana Press
Espejo EF, Montoro RJ, Armengol JA, Lopez-Barneo J (1998) Cellular and functional recovery of Parkinsonian rats after intrastriatal transplantation of carotid body cell aggregates. Neuron 20:197–206
Gentleman RC, Carey VJ, Bates DM, Bolstad B, Dettling M, Dudoit S, Ellis B, Gautier L, Ge Y, Gentry J, Hornik K, Hothorn T, Huber W, Iacus S, Irizarry R, Leisch F, Li C, Maechler M, Rossini AJ, Sawitzki G, Smith C, Smyth G, Tierney L, Yang JY, Zhang J (2004) Bioconductor: open software development for computational biology and bioinformatics. Genome Biol 5:R80
Granholm AC, Henry S, Herbert MA, Eken S, Gerhardt GA, van Horne C (1998) Kidney cografts enhance fiber outgrowth from ventral mesencephalic grafts to the 6-OHDA-lesioned striatum, and improve behavioral recovery. Cell Transplant 7:197–212
Gronthos S, Brahim J, Li W, Fisher LW, Cherman N, Boyde A, DenBesten P, Gehron Robey P, Shi S (2002) Stem cell properties of human dental pulp stem cells. J Dent Res 81:531–535
Heese K, Low JW, Inoue N (2006) Nerve growth factor, neural stem cells and Alzheimer’s disease. Neurosignals 15:1–12
Hellmann MA, Panet H, Barhum Y, Melamed E, Offen D (2006) Increased survival and migration of engrafted mesenchymal bone marrow stem cells in 6-hydroxydopamine-lesioned rodents. Neurosci Lett 395:124–128
Jordan J, Bottner M, Schluesener HJ, Unsicker K, Krieglstein K (1997) Bone morphogenetic proteins: neurotrophic roles for midbrain dopaminergic neurons and implications of astroglial cells. Eur J NeuroSci 9:1699–1710
Lin LF, Doherty DH, Lile JD, Bektesh S, Collins F (1993) GDNF: a glial cell line-derived neurotrophic factor for midbrain dopaminergic neurons. Science 21:1130–1132
Lindvall O, Hagell P (2001) Cell therapy and transplantation in Parkinson’s disease. Clin Chem Lab Med 39:356–361
Loo DT, Copani A, Pike CJ, Hittemore ER, Walencewicz AJ, Cotman CW (1993) Apoptosis is induced by beta-amyloid in cultured central nervous system neurons. Proc Natl Acad Sci USA 90:7951–7955
Maurice T, Lockhart BP, Privat A (1996) Amnesia induced in mice by centrally administered beta-amyloid peptides involves cholinergic dysfunction. Brain Res 706:181–193
Miura M, Grontos S, Zhao M, Lu B, Fisher LW, Gehron Robey P, Shi S (2003) SHED: stem cells from human exfoliated deciduous teeth. Proc Natl Acad Sci USA 100:5807–5812
Nosrat IV, Smith CA, Mullally P, Olson L, Nosrat CA (2004) Dental pulp cells provide neurotropic support for dopaminergic neurons and differentiate into neurons in vitro; implication for tissue engineering and repair in the nervous system. Eur J Neurosci 19:2388–2398
Nosrat IV, Widenfalk J, Olson L, Nosrat CA (2001) Dental pulp cells produce neurotrophic factors, interact with trigeminal neurons in vitro, and rescue motoneurons after spinal cord injury. Dev Biol 238:120–132
Perini G, Della-Bianca V, Politi V, Della Valle G, Dal-Pra I, Rossi F, Armato U (2002) Role of p75 neurotrophin receptor in the neurotoxicity by β-amyloid peptides and synergistic effect of inflammatory cytokines. J Exp Med 195:907–918
Reuss B, von Bohlen und Halbach O (2003) Fibroblast growth factors and their receptors in the central nervous system. Cell Tissue Res 313:139–157
Sanberg PR, Borlongan CV, Othberg AI, Saporta S, Freeman TB, Cameron DF (1997) Testis-derived sertoli cells have a trophic effect on dopamine neurons and alleviate hemiparkinsonism in rats. Nat Med 3:1129–1132
Team RDC (2006) R: a language and environment for statistical computing. Vienna, Austria, R Foundation for Statistical Computing
Wislet-Gendebien S, Hans G, Leprince P, Rigo JM, Moonen G, Rogister B (2005) Plasticity of cultured mesenchymal stem cells: switch from nestin-positive to excitable neuron-like phenotype. Stem Cells 23:392–402
Acknowledgments
This study was supported by grants from FAPESP (02/12633-7), the Interdisciplinary Centre for Clinical Research „BIOMAT.“ within the faculty of Medicine at the RWTH Aachen University (VV B110a), CAPES (PVE, 0098-11/2007), and the German Society of Dento-Maxillo-Facial Sciences (DGZMK). The Laboratory of Neuroscience receives financial support from the Associação Beneficente Alzira Denise Hertzog da Silva (ABADHS). We greatly acknowledge the experienced help of Patrica Buttler-Bücher concerning cell culture and immunocytochemistry.
Author information
Authors and Affiliations
Corresponding author
Additional information
C. Apel and O. V. Forlenza: both authors contributed equally to the work.
Rights and permissions
About this article
Cite this article
Apel, C., Forlenza, O.V., de Paula, V.J.R. et al. The neuroprotective effect of dental pulp cells in models of Alzheimer’s and Parkinson’s disease. J Neural Transm 116, 71–78 (2009). https://doi.org/10.1007/s00702-008-0135-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00702-008-0135-3