Abstract
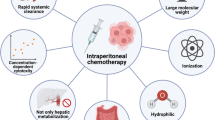
Intraperitoneal (IP) chemotherapy for peritoneal carcinomatosis (PC) from gastrointestinal cancer has been investigated and applied clinically for several decades. Cytoreductive surgery plus hyperthermic intraperitoneal chemotherapy have been considered to be the optimal treatment options for selected patients with colorectal and gastric cancers with PC. Accumulating evidence suggests that the administration of IP paclitaxel for patients with PC from gastric cancer may improve the patient survival. The pharmacokinetics of such treatment should be considered to optimize IP chemotherapy. In addition, newly emerging molecular-targeted therapies and research into new drug delivery systems, such as nanomedicine or controlled absorption/release methods, are essential to improve the effects of IP chemotherapy. This review summarizes the current status and future prospects of IP chemotherapy for the treatment of gastrointestinal cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Peritoneal carcinomatosis (PC) is the most serious metastatic pattern in gastrointestinal cancer, and is associated with an extremely poor prognosis [1, 2]. PC has long been considered to be a consequence of the systemic spread of cancer; therefore, systemic chemotherapy has usually been given as standard therapy. In spite of the consistent improvement in systemic chemotherapy regimens, the effects on PC are still limited, possibly because of the peritoneum-plasma barrier, which prevents effective drug delivery from the systemic circulation into the peritoneal cavity [3]. In contrast, intraperitoneal (IP) chemotherapy combined with cytoreductive surgery (CRS) as regional therapy for PC has demonstrated notable efficacy for the treatment of PC in various malignancies [4–7].
In 1978, Dedrick et al. [8] published the theoretical rationale that the IP administration of drugs would result in a higher drug concentration and longer half-life in the peritoneal cavity compared with intravenous (IV) administration. Since then, a number of basic studies on the pharmacokinetic and antitumor effects of IP administration and a number of clinical trials have proven the validity of IP chemotherapy. Three multicenter, randomized, phase III clinical trials have shown that IP chemotherapy is superior to standard IV systemic chemotherapy as the first-line chemotherapy against small volume, residual, advanced epithelial ovarian cancer [9–11]. Based on these results, the National Comprehensive Cancer Network guidelines now recommend IP chemotherapy for patients with stage III epithelial ovarian cancer after optimal debulking surgery [12]. Although evidence of the efficacy of CRS plus hyperthermic IP chemotherapy (HIPEC) has been established for gastrointestinal cancer, there is still controversy concerning whether IP chemotherapy, including HIPEC, is a standard treatment option or an experimental approach [13].
The peritoneum is not a simple membrane, but is a complicated organ. The route of peritoneal absorption and pharmacokinetics following IP administration vary a great deal between drugs. In addition, the formulation, solvent, concentration, administration rate and other factors critically affect the pharmacokinetics [14]. Ideally, the agents used for IP chemotherapy should slowly exit the peritoneal cavity to allow for optimal surface penetration of the tumors [14]. For some drugs, use under hyperthermic conditions can increase the cytotoxicity in the peritoneal cavity without an increase in systemic toxicity [15]. Investigations into drug delivery systems (DDS) are ongoing to develop new strategies that can be used in addition to IP administration of drugs to achieve better clinical results [16, 17]. Molecular-targeted therapy should be taken into account as one such option, and the development of drugs or solvents specific for IP chemotherapy may be a future issue that needs to be resolved in this field.
In this review, we summarize the current status of IP chemotherapy for PC from gastric cancer (GC) and colorectal cancer (CRC) and ongoing basic research on the DDS in IP chemotherapy.
Pharmacokinetics of IP chemotherapy
The aim of IP chemotherapy is to increase the dose and exposure time of anticancer drugs to the intraabdominal cancer cells, while inducing minimal systemic toxic effects. The pharmacokinetics after IP administration are affected by a variety of biophysical parameters, including the molecular weight and electric charge of the agent, as well as the temperature, pH and other conditions of the solution. Prolonged retention in the peritoneal cavity and clearance from systemic circulation are believed to be the key attributes for ideal drug candidates designed for IP chemotherapy [8, 14, 18]. Intraperitoneally administered materials are mainly absorbed by two anatomical routes. After IP administration, hydrophilic low-weight molecular materials, such as cisplatin (CDDP) or mitomycin C(MMC), are rapidly absorbed into the subperitoneal capillary vessels through the peritoneal mesothelial layer. In contrast, hydrophobic high-weight molecular materials, such as taxanes, are gradually drained, mainly from stomata or milky spots that are the direct openings of lymphatic vessels [19, 20]. Thus, the time–concentration curves of drugs in the peritoneum and plasma vary widely according to the drug type. The area under the curve (AUC) ratio of the peritoneal cavity to the plasma (AUC peritoneum/plasma) is approximately 1000 for paclitaxel (PTX) and approximately 10–21 for CDDP (Table 1) [14, 21–24]. In IP chemotherapy, the pharmacokinetic profile of each drug is as important as its cytotoxic activity.
Currently used IP chemotherapy agents
HIPEC and agents with heat synergy
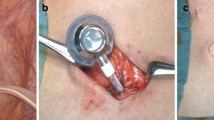
The aim of HIPEC is to achieve a high local concentration of chemotherapeutic agents in the peritoneal cavity and to promote good absorption of these agents from the surface of peritoneal tumors with minimal systemic toxic effects. Practically, multiple drainage tubes are placed in different areas of the abdomen after CRS. A roller pump with a heat exchanger is used, and the temperature is maintained at 42–43 °C throughout the perfusion duration of 30–120 min [25]. Heat has a synergistic effect with MMC, CDDP, oxaliplatin, and docetaxel (Table 1). MMC, CDDP, and oxaliplatin are generally used for HIPEC for CRC and GC. The previously reported clinical results of IP chemotherapy for CRC [26–40] and GC [39, 41–53] are shown in Tables 2 and 3, respectively. In these tables, most studies included only patients who underwent complete CRS, except for a few references [39, 46, 47, 49, 51–53].
A few studies have compared HIPEC with early postoperative intraperitoneal chemotherapy (EPIC) or non-hyperthermic sequential postoperative intraperitoneal chemotherapy (SPIC). Elias et al. [54] reported that HIPEC with oxaliplatin was better tolerated than EPIC with MMC, and that 5-fluorouracil (5-FU) was twice as efficient at curing residual PC from CRC with minimal residual disease after surgery. Cashin et al. [40, 55] reported that HIPEC was associated with an improved overall survival (OS) and disease-free survival compared with SPIC, with similar morbidity and mortality in patients with PC from CRC. They concluded that CRS and HIPEC might be the optimal treatment for patients with PC from CRC with minimal residual disease. However, in the SPIC and EPIC studies, the IP drug combination was MMC and 5-FU, whereas IP oxaliplatin was used in HIPEC studies, suggesting that further studies using oxaliplatin may be required in future EPIC and SPIC studies for a more reasonable comparison.
As for GC, Yonemura et al. [56] suggested that a combination of neoadjuvant IP/systemic chemotherapy (NIPS), such as CRS plus HIPEC, and EPIC/SPIC might be the best treatment strategy.
Mitomycin C
MMC is the most extensively used clinical IP chemotherapy agent that demonstrates favorable outcomes [28]. It is usually the first agent to be selected for HIPEC for CRC, and is used in combination with other drugs for GC. MMC can be co-administered with other agents such as oxaliplatin, CDDP and 5-FU due to its favorable compatibility profile. HIPEC achieves high peritoneal concentrations of MMC with limited systemic absorption [57].
Cisplatin
CDDP is one of the most widely used drugs for various cancers, including GC [58]. It is used for IP chemotherapy with or without hyperthermia. The AUC for the peritoneum/plasma is approximately 12–20 [14], which is not as high as that of many other drugs. However, significant antitumor activity during systemic chemotherapy has led physicians to evaluate IP CDDP, which led to improved survival compared with IV administration in patients with ovarian cancer [9]. Heat synergy of CDDP has been reported [59]. To prolong the retention of CDDP in the peritoneal cavity, continuous IP infusion was attempted with tolerable toxicity [60].
Oxaliplatin
Oxaliplatin is the main agent used during systemic chemotherapy for CRC. Elias et al. [35, 61–64] reported on the pharmacokinetics and significant efficacy of IP oxaliplatin for patients with PC from CRC. They demonstrated the effectiveness of bidirectional chemotherapy, that is, a combination of HIPEC with oxaliplatin and intraoperative IV chemotherapy [61, 62]. Then, they retrospectively compared patients with resectable PC treated with complete CRS and HIPEC (n = 48) to those treated with standard systemic chemotherapy (n = 48). The median OS was 63 months in the HIPEC group versus 24 months in the systemic chemotherapy group [35].
Agents without heat synergy
Paclitaxel and docetaxel
PTX is water insoluble, and for clinical use, it is conventionally solubilized in a polyoxyethylated castor oil called Cremophor EL and ethanol (i.e., Taxol®) [65, 66]. Taxol® is considered to be suitable for IP chemotherapy due to its large particle size (10–12 nm in diameter), which can result in prolonged retention of the drug in the peritoneal cavity [14, 67, 68], although Cremophor EL can cause severe hypersensitivity reactions, which occur in 2–4 % of patients [65, 66].
In patients with GC, IP PTX was demonstrated to be clinically safe and effective in phase I and II trials [51, 69–72]. The bidirectional administration of IV and IP PTX maintained effective concentrations of PTX in the peritoneal cavity for over 72 h [70] (Fig. 1). In a phase II trial of combination chemotherapy with oral S-1 and IV and IP PTX for patients with PC from GC, the one-year OS rate was 78 % and the overall response rate (ORR) was 22 %, even though most of the patients had highly advanced PC [51]. The advantage of this regimen was the administration of IP chemotherapy both before and after CRS, whereas in the previous studies, IP therapy was limited to a short postoperative period. A randomized, multicenter, phase III trial (PHOENIX-GC trial, UMIN Trial ID: UMIN000005930) comparing S-1 in combination with IV and IP PTX versus S-1 with IV CDDP, as a standard regimen for Japanese patients with advanced or recurrent GC [58], began in November 2011 (Fig. 2).
The concentration-versus-time curves of intraperitoneal and serum PTX. After the administration of PTX (50 mg/m2 intravenously, 20 mg/m2 intraperitoneally), serum and intraperitoneal fluid was periodically collected. The PTX concentrations were measured by a reverse-phase high-performance liquid chromatography assay. PTX paclitaxel (adapted from Ref. [70])
IP docetaxel for patients with PC from GC was also evaluated; the one-year OS rate was 70 % and the ORR was 22 % [53, 73].
Taxanes are not commonly used for systemic chemotherapy for patients with CRC since phase II trials yielded negative results [74–76]. However, clinical evaluation of IP PTX could also be considered for patients with PC from CRC, because the pharmacokinetics of PTX after IP administration are very different from those after IV administration, and preclinical investigations of IP PTX for CRC showed desirable efficacy [77, 78].
Irinotecan
Irinotecan is one of the key drugs used for the treatment of CRC and GC. It is a pro-drug that exerts its anticancer activity after transformation into SN-38 by carboxylesterases in the liver. SN-38 is 100- to 1000-fold more cytotoxic than irinotecan. Carboxylesterases are reported to be minimally present in the peritoneum [79], and Elias et al. [80] performed an IP administration of irinotecan and reported that SN-38 was detected in the peritoneal cavity just after the IP administration of irinotecan. However, their clinical trial comparing CRS plus HIPEC using oxaliplatin with or without irinotecan showed that the addition of irinotecan did not confer a survival benefit, and instead increased morbidity [81]. These results were unexpected, but might be explained by the local inefficiency of irinotecan from the viewpoint of its metabolism. In addition, it was speculated that the efficiency of HIPEC might be less dependent on the drug used, unlike the case for systemic chemotherapy.
5-Fluorouracil
5-FU is a widely used IP agent for the treatment of patients with gastrointestinal cancer. Because it has no heat synergy, 5-FU is currently used in EPIC and SPIC for CRC and GC. Since IP administration of 5-FU results in absorption from the peritoneum and direct first-pass metabolism in the liver, IP administration requires a 1.5-fold higher dose than that used for systemic administration [82]. Cashin et al. [40] reported a retrospective cohort study of SPIC treatment consisting of IP 5-FU at 500–600 mg/m2 and IV leucovorin at 60 mg/m2 once a day for 6 days. Eight cycles of SPIC with at 4- to 6-week intervals over a six-month period were planned as an adjuvant chemotherapy regimen. The OS of 57 patients who underwent CRS and received SPIC was 25 months, with a five-year survival rate of 18 %. Glehen et al. [28] reported that the OS of 235 patients with CRC who received EPIC with 5-FU and/or MMC was 19.2 months.
Molecular-targeted therapy in patients with malignant ascites
Catumaxomab
Epithelial cell adhesion molecule (EpCAM, CD326) is a surface antigen present on various kinds of epithelial cancer and normal epithelial cells [83]. Catumaxomab is a trifunctional monoclonal antibody with two different antigen-binding sites and a functional Fc domain [84]. It binds to human EpCAM-positive cancer cells and redirects CD3-positive T lymphocytes and Fcγ-receptor-positive accessory cells to the cancer cells, thereby activating a complex antitumor immune reaction through various effector functions, such as antibody-dependent cellular cytotoxicity, phagocytosis and T cell-mediated cytotoxicity [85–89] (Fig. 3).
The mechanism(s) of action of catumaxomab. ADCC antibody-dependent cellular cytotoxicity, DC dendritic cell, DC-CK1 dendritic cell cytokine 1, EpCAM epithelial cell adhesion molecule (adapted from Ref. [89])
A randomized phase II/III trial of catumaxomab in patients with malignant ascites due to epithelial cancer, including ovarian, gastric, breast, pancreatic, colorectal and endometrial cancers was conducted. Patients with malignant ascites (n = 258) were randomized to receive paracentesis plus catumaxomab or paracentesis alone and stratified by cancer type. The puncture-free survival was significantly longer in the catumaxomab group than in the control group (46 vs. 11 days, hazard ratio = 0.254, P < 0.0001) as was the median time to the next paracentesis (77 vs. 13 days, P < 0.0001). The OS showed a positive trend in the catumaxomab group and was significantly prolonged in patients with GC (71 vs. 44 days, P = 0.0313) [90]. Moreover, treatment with catumaxomab significantly delayed the deterioration of the patient quality of life (QoL) in the same trial [91].
Bevacizumab
Vascular endothelial growth factor A (VEGF-A) is a key mediator of angiogenesis [92, 93]. The activities of VEGF-A are mediated by two tyrosine kinase receptors, vascular endothelial growth factor receptors 1 and 2. In patients with CRC, bevacizumab, a humanized variant of an antiVEGF antibody, has shown significant efficacy in combination with chemotherapy, and is now widely used in the clinical setting [94]. Although, the primary endpoint of OS was not reached in the AVAGAST trial, the addition of bevacizumab to chemotherapy was associated with significant increases in progression-free survival and the ORR in the first-line treatment of patients with advanced GC [95].
Malignant ascites caused by PC not only leads to the deterioration of the patients’ QoL, but also results in a poor prognosis [96, 97]. VEGF is markedly elevated in malignant ascites, where it worsens the condition by increasing the endothelial cell permeability [98]. VEGF inhibition in the peritoneal cavity is therefore considered to be beneficial not only as an inhibitor of tumorigenesis, but also as an inhibitor of the formation of malignant ascites [99]. In surgically resected specimen from patients with GC, the VEGF expression was indicated to be an independent predictor of peritoneal recurrence [100].
With regard to the route of administration, bevacizumab should be administered systemically, because it is rapidly absorbed from the peritoneum and enters the systemic circulation when administered by IP injection [101, 102].
There have been so far no clinical trials addressing the use of bevacizumab with IP chemotherapy, although the effects of bevacizumab on murine PC models of GC were promising [103, 104].
Utilization of new DDS in IP chemotherapy
Nanodrugs
Nanodrugs are a new type of drug formulation, comprising particles of 20–100 nm in molecular diameter, smaller than conventional drugs. Since the discovery of selective accumulation by passive targeting, known as the enhanced permeability and retention (EPR) effect [105], various kinds of nanodrugs have been developed for cancer treatment (Table 4) [106–108]. One of the barriers to systemic chemotherapy is the high interstitial pressure of solid tumors, which prevents drugs from leaking from vessels and penetrating into tumor tissue [109–112]. Nanodrugs accumulate in tumor tissue by the EPR effect, which results in enhanced antitumor effects and less toxicity in normal tissues. The EPR effect is based on the special characteristics of solid tumor tissues, such as incomplete vascular architecture, hyperpermeability of tumor vessel walls and immature lymphatic drainage [105] (Fig. 4). Nanodrugs of the polymeric micellar type are retained for a long period in the systemic blood stream [113, 114], where they are easily extravasated from tumor vessels into the interstitium of tumor tissue, resulting in greater intratumoral exposure compared with conventional small-molecule agents [105, 115].
The enhanced permeability and retention (EPR) effect. a Small molecules easily leak from normal capillary vessels and are drained via lymphatic vessels in normal tissue, whereas nanoparticle macromolecules do not pass through the normal vessel walls. Nanoparticles do not harm the normal tissue. b In contrast, nanoparticles leak from vessels and persist for a long time in the tumor tissue, where the vascular permeability is elevated and the lymphatic system is immature. As a result, nanoparticles accumulate in the tumor tissue
Various types of Cremophor-free, nanoparticulate PTX have recently been investigated to reduce the risk of allergic reactions and to take advantage of the EPR effect [116–120]. Abraxane®, an albumin-bound PTX, is currently in clinical use for breast, lung and gastric cancers [121, 122]. NK105 is a PTX-incorporating “core–shell-type” polymeric micellar nanoparticle formulation [123, 124] (Fig. 5). A phase II trial of NK105 as second-line chemotherapy in patients with advanced GC reported an ORR of 25 % and a median OS of 14.4 months [125]. A phase III trial to verify the non-inferiority of NK105 to Taxol® in terms of the progression-free survival in patients with metastatic or recurrent breast cancer is ongoing (NCT01644890).
The IV administration of NK012, an SN-38-releasing polymeric nanomicellar agent, showed a significantly enhanced antitumor effect against PC in a mouse GC xenograft model compared with irinotecan [126]. However, the IP administration of nanoparticulate anticancer agents for PC has received little attention despite the existence of data indicating the potency of this type of treatment [127].
PMB-30W is a water-soluble, amphiphilic polymer composed of 2-methacryloxyethyl phosphorylcholine and n-butyl methacrylate. As is the case for NK105, this co-polymer is biocompatible, forms micelles when dissolved in aqueous media, and provides hydrophobic domains in such media. As a solvent, PMB-30W is 1000-fold better than water, and enables the construction of PTX-containing nanoparticles approximately 50 nm in diameter [119]. The IP administration of nanoparticulate PTX resulted in deeper penetration into peritoneal nodules and exhibited enhanced antitumor effects compared to conventional Cremophor-conjugated PTX (Fig. 6) [128, 129], although the reason why nanomicellar particles can penetrate deeply into peritoneal nodules is unclear.
The spatial distribution of Cremophor-conjugated paclitaxel (PTX) or nanomicellar PTX (PTX-30W) in disseminated tumors after IP injection. Peritoneal xenografts in nude mice were excised 24 h after IP injection of Cremophor-conjugated PTX (a) or PTX-30W (b). PTX was labeled by Oregon green fluorescence. The infiltration of PTX into nodules was significantly deeper following PTX-30W (b) compared with Cremophor-conjugated PTX (a) treatment. Scale bars indicate 1 mm (adapted from Ref. [128])
Higher and longer retention in the systemic circulation after IP administration of NK105 was also shown in a mouse model [130]. IP NK105 showed significantly enhanced antitumor effects against both subcutaneous and peritoneal xenografts of human GC compared with IP Taxol®. IP chemotherapy with nanoparticulate agents could be a promising strategy for the treatment of PC.
Controlled absorption and drug release
Water-soluble low molecular weight agents such as CDDP are rapidly absorbed via the capillary blood vessels of the peritoneum after IP administration [14]. Therefore, the ratio of the AUC for the peritoneum to that for plasma of these agents is low [15, 18, 131]. To keep this ratio high, frequent or continuous IP administration of these agents has been attempted, which sometimes caused stress for patients because of catheter-related complications [4, 17]. The IP administration of CDDP in a hypotonic solution resulted in a high AUC in the plasma, a high intratumoral uptake and prolonged survival in animal models; however, the AUC in the IP fluid was low, and this strategy caused an increase in the renal toxicity [132, 133].
However, IP administration of water-soluble agents is still widely performed without any special artifice in DDS in clinical practice, but further research is needed to prolong the retention of drugs in the peritoneal cavity [14, 17, 134].
Hydrogels are formed by cross-linking hydrophilic macromolecules. They have been reported to prolong drug retention in the peritoneal cavity and to enhance the antitumor effects for PC [135–138]. The hyaluronic acid (HA)-based hydrogel is a biocompatible material that prevents peritoneal adhesion after surgical processes [139–141]. Hydrogels that are sensitive to stimuli such as temperature [136, 137, 142, 143] or pH [144] have considerable potential in biomedical and pharmaceutical applications, especially in site-specific and controlled DDS [145].
The IP administration of CDDP via a HA-based hydrogel resulted in the sustained release of CDDP in the peritoneal cavity and enhanced antitumor activity against PC in a mouse model [146], revealing a novel DDS for the treatment of PC. A combination of controlled release and target-specific delivery by HA-based hydrogel through interactions between CD44 and HA also seems promising [147–149].
Conclusion
This review has attempted to highlight the current status and future prospects of IP chemotherapy for patients with PC from GC and CRC, with a focus mainly on the pharmacokinetics. Since the infusion of anticancer agents into the abdominal cavity enables direct exposure of a high concentration of drugs to each tumor cell, it seems to be a reasonable drug delivery method. The results suggest that multimodal treatment including IP chemotherapy may be the best approach for PC, with the potential to improve the survival of the patients with this dismal disease.
References
Sadeghi B, Arvieux C, Glehen O, Beaujard AC, Rivoire M, Baulieux J, et al. Peritoneal carcinomatosis from non-gynecologic malignancies: results of the EVOCAPE 1 multicentric prospective study. Cancer. 2000;88(2):358–63.
Shinohara S, Korenaga D, Edagawa A, Koushi K, Itoh S, Kawanaka H, et al. Significant prognostic factors in patients with Stage IV gastric cancer with special reference to the curability of surgery. Surg Today. 2013;43(1):40–7.
Jacquet P, Sugarbaker PH. Peritoneal-plasma barrier. Cancer Treat Res. 1996;82:53–63.
Markman M, Walker JL. Intraperitoneal chemotherapy of ovarian cancer: a review, with a focus on practical aspects of treatment. J Clin Oncol. 2006;24(6):988–94.
Chua TC, Moran BJ, Sugarbaker PH, Levine EA, Glehen O, Gilly FN, et al. Early- and long-term outcome data of patients with pseudomyxoma peritonei from appendiceal origin treated by a strategy of cytoreductive surgery and hyperthermic intraperitoneal chemotherapy. J Clin Oncol. 2012;30(20):2449–56.
Chua TC, Chong CH, Morris DL. Peritoneal mesothelioma: current status and future directions. Surg Oncol Clin North Am. 2012;21(4):635–43.
Piso P, Arnold D. Multimodal treatment approaches for peritoneal carcinosis in colorectal cancer. Dtsch Arztebl Int. 2011;108(47):802–8.
Dedrick RL, Myers CE, Bungay PM, DeVita VT Jr. Pharmacokinetic rationale for peritoneal drug administration in the treatment of ovarian cancer. Cancer Treat Rep. 1978;62(1):1–11.
Alberts DS, Liu PY, Hannigan EV, O’Toole R, Williams SD, Young JA, et al. Intraperitoneal cisplatin plus intravenous cyclophosphamide versus intravenous cisplatin plus intravenous cyclophosphamide for stage III ovarian cancer. N Engl J Med. 1996;335(26):1950–5.
Markman M, Bundy BN, Alberts DS, Fowler JM, Clark-Pearson DL, Carson LF, et al. Phase III trial of standard-dose intravenous cisplatin plus paclitaxel versus moderately high-dose carboplatin followed by intravenous paclitaxel and intraperitoneal cisplatin in small-volume stage III ovarian carcinoma: an intergroup study of the Gynecologic Oncology Group, Southwestern Oncology Group, and Eastern Cooperative Oncology Group. J Clin Oncol. 2001;19(4):1001–7.
Armstrong DK, Bundy B, Wenzel L, Huang HQ, Baergen R, Lele S, et al. Intraperitoneal cisplatin and paclitaxel in ovarian cancer. N Engl J Med. 2006;354(1):34–43.
Morgan RJ Jr, Alvarez RD, Armstrong DK, Boston B, Burger RA, Chen LM, et al. Epithelial ovarian cancer. J Natl Compr Cancer Netw. 2011;9(1):82–113.
Sugarbaker PH, Ryan DP. Cytoreductive surgery plus hyperthermic perioperative chemotherapy to treat peritoneal metastases from colorectal cancer: standard of care or an experimental approach? Lancet Oncol. 2012;13(8):e362–9.
Markman M. Intraperitoneal antineoplastic drug delivery: rationale and results. Lancet Oncol. 2003;4(5):277–83.
Sugarbaker PH, Mora JT, Carmignani P, Stuart OA, Yoo D. Update on chemotherapeutic agents utilized for perioperative intraperitoneal chemotherapy. Oncologist. 2005;10(2):112–22.
Yamada J, Kitayama J, Tsuno NH, Yamashita H, Miyato H, Soma D, et al. Intra-peritoneal administration of paclitaxel with non-animal stabilized hyaluronic acid as a vehicle—a new strategy against peritoneal dissemination of gastric cancer. Cancer Lett. 2008;272(2):307–15.
Bajaj G, Yeo Y. Drug delivery systems for intraperitoneal therapy. Pharm Res. 2010;27(5):735–8.
Dedrick RL, Flessner MF. Pharmacokinetic problems in peritoneal drug administration: tissue penetration and surface exposure. J Natl Cancer Inst. 1997;89(7):480–7.
Flessner MF, Fenstermacher JD, Blasberg RG, Dedrick RL. Peritoneal absorption of macromolecules studied by quantitative autoradiography. Am J Physiol. 1985;248(1 Pt 2):H26–32.
Wang ZB, Li M, Li JC. Recent advances in the research of lymphatic stomata. Anat Rec (Hoboken). 2010;293(5):754–61.
Ceelen WP, Flessner MF. Intraperitoneal therapy for peritoneal tumors: biophysics and clinical evidence. Nat Rev Clin Oncol. 2010;7(2):108–15.
Yan TD, Cao CQ, Munkholm-Larsen S. A pharmacological review on intraperitoneal chemotherapy for peritoneal malignancy. World J Gastrointest Oncol. 2010;2(2):109–16.
Fushida S, Kinoshita J, Yagi Y, Funaki H, Kinami S, Ninomiya I, et al. Dual anti-cancer effects of weekly intraperitoneal docetaxel in treatment of advanced gastric cancer patients with peritoneal carcinomatosis: a feasibility and pharmacokinetic study. Oncol Rep. 2008;19(5):1305–10.
Yonemura Y, Elnemr A, Endou Y, Hirano M, Mizumoto A, Takao N, et al. Multidisciplinary therapy for treatment of patients with peritoneal carcinomatosis from gastric cancer. World J Gastrointest Oncol. 2010;2(2):85–97.
Glehen O, Cotte E, Kusamura S, Deraco M, Baratti D, Passot G, et al. Hyperthermic intraperitoneal chemotherapy: nomenclature and modalities of perfusion. J Surg Oncol. 2008;98(4):242–6.
Verwaal VJ, van Ruth S, de Bree E, van Sloothen GW, van Tinteren H, Boot H, et al. Randomized trial of cytoreduction and hyperthermic intraperitoneal chemotherapy versus systemic chemotherapy and palliative surgery in patients with peritoneal carcinomatosis of colorectal cancer. J Clin Oncol. 2003;21(20):3737–43.
Mahteme H, Hansson J, Berglund A, Pahlman L, Glimelius B, Nygren P, et al. Improved survival in patients with peritoneal metastases from colorectal cancer: a preliminary study. Br J Cancer. 2004;90(2):403–7.
Glehen O, Kwiatkowski F, Sugarbaker PH, Elias D, Levine EA, De Simone M, et al. Cytoreductive surgery combined with perioperative intraperitoneal chemotherapy for the management of peritoneal carcinomatosis from colorectal cancer: a multi-institutional study. J Clin Oncol. 2004;22(16):3284–92.
Elias D, Delperro JR, Sideris L, Benhamou E, Pocard M, Baton O, et al. Treatment of peritoneal carcinomatosis from colorectal cancer: impact of complete cytoreductive surgery and difficulties in conducting randomized trials. Ann Surg Oncol. 2004;11(5):518–21.
Verwaal VJ, van Ruth S, Witkamp A, Boot H, van Slooten G, Zoetmulder FA. Long-term survival of peritoneal carcinomatosis of colorectal origin. Ann Surg Oncol. 2005;12(1):65–71.
Kianmanesh R, Scaringi S, Sabate JM, Castel B, Pons-Kerjean N, Coffin B, et al. Iterative cytoreductive surgery associated with hyperthermic intraperitoneal chemotherapy for treatment of peritoneal carcinomatosis of colorectal origin with or without liver metastases. Ann Surg. 2007;245(4):597–603.
Verwaal VJ, Bruin S, Boot H, van Slooten G, van Tinteren H. 8-year follow-up of randomized trial: cytoreduction and hyperthermic intraperitoneal chemotherapy versus systemic chemotherapy in patients with peritoneal carcinomatosis of colorectal cancer. Ann Surg Oncol. 2008;15(9):2426–32.
Shen P, Thai K, Stewart JH, Howerton R, Loggie BW, Russell GB, et al. Peritoneal surface disease from colorectal cancer: comparison with the hepatic metastases surgical paradigm in optimally resected patients. Ann Surg Oncol. 2008;15(12):3422–32.
Bijelic L, Yan TD, Sugarbaker PH. Treatment failure following complete cytoreductive surgery and perioperative intraperitoneal chemotherapy for peritoneal dissemination from colorectal or appendiceal mucinous neoplasms. J Surg Oncol. 2008;98(4):295–9.
Elias D, Lefevre JH, Chevalier J, Brouquet A, Marchal F, Classe JM, et al. Complete cytoreductive surgery plus intraperitoneal chemohyperthermia with oxaliplatin for peritoneal carcinomatosis of colorectal origin. J Clin Oncol. 2009;27(5):681–5.
Franko J, Ibrahim Z, Gusani NJ, Holtzman MP, Bartlett DL, Zeh HJ 3rd. Cytoreductive surgery and hyperthermic intraperitoneal chemoperfusion versus systemic chemotherapy alone for colorectal peritoneal carcinomatosis. Cancer. 2010;116(16):3756–62.
Elias D, Gilly F, Boutitie F, Quenet F, Bereder JM, Mansvelt B, et al. Peritoneal colorectal carcinomatosis treated with surgery and perioperative intraperitoneal chemotherapy: retrospective analysis of 523 patients from a multicentric French study. J Clin Oncol. 2010;28(1):63–8.
Elias D, Glehen O, Pocard M, Quenet F, Goere D, Arvieux C, et al. A comparative study of complete cytoreductive surgery plus intraperitoneal chemotherapy to treat peritoneal dissemination from colon, rectum, small bowel, and nonpseudomyxoma appendix. Ann Surg. 2010;251(5):896–901.
Glehen O, Gilly FN, Boutitie F, Bereder JM, Quenet F, Sideris L, et al. Toward curative treatment of peritoneal carcinomatosis from nonovarian origin by cytoreductive surgery combined with perioperative intraperitoneal chemotherapy: a multi-institutional study of 1,290 patients. Cancer. 2010;116(24):5608–18.
Cashin PH, Graf W, Nygren P, Mahteme H. Cytoreductive surgery and intraperitoneal chemotherapy for colorectal peritoneal carcinomatosis: prognosis and treatment of recurrences in a cohort study. Eur J Surg Oncol. 2012;38(6):509–15.
Fujimoto S, Takahashi M, Mutou T, Kobayashi K, Toyosawa T, Isawa E, et al. Improved mortality rate of gastric carcinoma patients with peritoneal carcinomatosis treated with intraperitoneal hyperthermic chemoperfusion combined with surgery. Cancer. 1997;79(5):884–91.
Beaujard AC, Glehen O, Caillot JL, Francois Y, Bienvenu J, Panteix G, et al. Intraperitoneal chemohyperthermia with mitomycin C for digestive tract cancer patients with peritoneal carcinomatosis. Cancer. 2000;88(11):2512–9.
Hall JJ, Loggie BW, Shen P, Beamer S, Douglas Case L, McQuellon R, et al. Cytoreductive surgery with intraperitoneal hyperthermic chemotherapy for advanced gastric cancer. J Gastrointest Surg. 2004;8(4):454–63.
Glehen O, Schreiber V, Cotte E, Sayag-Beaujard AC, Osinsky D, Freyer G, et al. Cytoreductive surgery and intraperitoneal chemohyperthermia for peritoneal carcinomatosis arising from gastric cancer. Arch Surg. 2004;139(1):20–6.
Yonemura Y, Kawamura T, Bandou E, Takahashi S, Sawa T, Matsuki N. Treatment of peritoneal dissemination from gastric cancer by peritonectomy and chemohyperthermic peritoneal perfusion. Br J Surg. 2005;92(3):370–5.
Yonemura Y, Bandou E, Sawa T, Yoshimitsu Y, Endou Y, Sasaki T, et al. Neoadjuvant treatment of gastric cancer with peritoneal dissemination. Eur J Surg Oncol. 2006;32(6):661–5.
Cheong JH, Shen JY, Song CS, Hyung WJ, Shen JG, Choi SH, et al. Early postoperative intraperitoneal chemotherapy following cytoreductive surgery in patients with very advanced gastric cancer. Ann Surg Oncol. 2007;14(1):61–8.
Yonemura Y, Endou Y, Shinbo M, Sasaki T, Hirano M, Mizumoto A, et al. Safety and efficacy of bidirectional chemotherapy for treatment of patients with peritoneal dissemination from gastric cancer: selection for cytoreductive surgery. J Surg Oncol. 2009;100(4):311–6.
Yang XJ, Li Y, Yonemura Y. Cytoreductive surgery plus hyperthermic intraperitoneal chemotherapy to treat gastric cancer with ascites and/or peritoneal carcinomatosis: results from a Chinese center. J Surg Oncol. 2010;101(6):457–64.
Glehen O, Gilly FN, Arvieux C, Cotte E, Boutitie F, Mansvelt B, et al. Peritoneal carcinomatosis from gastric cancer: a multi-institutional study of 159 patients treated by cytoreductive surgery combined with perioperative intraperitoneal chemotherapy. Ann Surg Oncol. 2010;17(9):2370–7.
Ishigami H, Kitayama J, Kaisaki S, Hidemura A, Kato M, Otani K, et al. Phase II study of weekly intravenous and intraperitoneal paclitaxel combined with S-1 for advanced gastric cancer with peritoneal metastasis. Ann Oncol. 2010;21(1):67–70.
Yang XJ, Huang CQ, Suo T, Mei LJ, Yang GL, Cheng FL, et al. Cytoreductive surgery and hyperthermic intraperitoneal chemotherapy improves survival of patients with peritoneal carcinomatosis from gastric cancer: final results of a phase III randomized clinical trial. Ann Surg Oncol. 2011;18(6):1575–81.
Fushida S, Kinoshita J, Kaji M, Hirono Y, Goda F, Yagi Y, et al. Phase I/II study of intraperitoneal docetaxel plus S-1 for the gastric cancer patients with peritoneal carcinomatosis. Cancer Chemother Pharmacol. 2013;71(5):1265–72.
Elias D, Benizri E, Di Pietrantonio D, Menegon P, Malka D, Raynard B. Comparison of two kinds of intraperitoneal chemotherapy following complete cytoreductive surgery of colorectal peritoneal carcinomatosis. Ann Surg Oncol. 2007;14(2):509–14.
Cashin PH, Graf W, Nygren P, Mahteme H. Intraoperative hyperthermic versus postoperative normothermic intraperitoneal chemotherapy for colonic peritoneal carcinomatosis: a case-control study. Ann Oncol. 2012;23(3):647–52.
Yonemura Y, Endou Y, Sasaki T, Hirano M, Mizumoto A, Matsuda T, et al. Surgical treatment for peritoneal carcinomatosis from gastric cancer. Eur J Surg Oncol. 2010;36(12):1131–8.
Jacquet P, Averbach A, Stephens AD, Stuart OA, Chang D, Sugarbaker PH. Heated intraoperative intraperitoneal mitomycin C and early postoperative intraperitoneal 5-fluorouracil: pharmacokinetic studies. Oncology. 1998;55(2):130–8.
Koizumi W, Narahara H, Hara T, Takagane A, Akiya T, Takagi M, et al. S-1 plus cisplatin versus S-1 alone for first-line treatment of advanced gastric cancer (SPIRITS trial): a phase III trial. Lancet Oncol. 2008;9(3):215–21.
Urano M, Kuroda M, Nishimura Y. For the clinical application of thermochemotherapy given at mild temperatures. Int J Hyperthermia. 1999;15(2):79–107.
Ishigami H, Kitayama J, Kaisaki S, Yamaguchi H, Yamashita H, Emoto S, et al. Phase I study of biweekly intravenous paclitaxel plus intraperitoneal cisplatin and paclitaxel for gastric cancer with peritoneal metastasis. Oncology. 2010;79(3–4):269–72.
Elias D, Bonnay M, Puizillou JM, Antoun S, Demirdjian S, El OA, et al. Heated intra-operative intraperitoneal oxaliplatin after complete resection of peritoneal carcinomatosis: pharmacokinetics and tissue distribution. Ann Oncol. 2002;13(2):267–72.
Elias DM, Sideris L. Pharmacokinetics of heated intraoperative intraperitoneal oxaliplatin after complete resection of peritoneal carcinomatosis. Surg Oncol Clin North Am. 2003;12(3):755–769, xiv.
Elias D, Sideris L, Pocard M, Ede C, Ben Hassouna D, Ducreux M, et al. Efficacy of intraperitoneal chemohyperthermia with oxaliplatin in colorectal peritoneal carcinomatosis. Preliminary results in 24 patients. Ann Oncol. 2004;15(5):781–5.
Elias D, Goere D, Blot F, Billard V, Pocard M, Kohneh-Shahri N, et al. Optimization of hyperthermic intraperitoneal chemotherapy with oxaliplatin plus irinotecan at 43 degrees C after compete cytoreductive surgery: mortality and morbidity in 106 consecutive patients. Ann Surg Oncol. 2007;14(6):1818–24.
Rowinsky EK, Donehower RC. Paclitaxel (taxol). N Engl J Med. 1995;332(15):1004–14.
Singla AK, Garg A, Aggarwal D. Paclitaxel and its formulations. Int J Pharm. 2002;235(1–2):179–92.
Markman M, Rowinsky E, Hakes T, Reichman B, Jones W, Lewis JL Jr, et al. Phase I trial of intraperitoneal taxol: a Gynecoloic Oncology Group study. J Clin Oncol. 1992;10(9):1485–91.
Soma D, Kitayama J, Ishigami H, Kaisaki S, Nagawa H. Different tissue distribution of paclitaxel with intravenous and intraperitoneal administration. J Surg Res. 2009;155(1):142–6.
Kodera Y, Ito Y, Ito S, Ohashi N, Mochizuki Y, Yamamura Y, et al. Intraperitoneal paclitaxel: a possible impact of regional delivery for prevention of peritoneal carcinomatosis in patients with gastric carcinoma. Hepatogastroenterology. 2007;54(75):960–3.
Ishigami H, Kitayama J, Otani K, Kamei T, Soma D, Miyato H, et al. Phase I pharmacokinetic study of weekly intravenous and intraperitoneal paclitaxel combined with S-1 for advanced gastric cancer. Oncology. 2009;76(5):311–4.
Imano M, Imamoto H, Itoh T, Satou T, Peng YF, Yasuda A, et al. Safety of intraperitoneal administration of paclitaxel after gastrectomy with en-bloc D2 Lymph node dissection. J Surg Oncol. 2012;105:43–7.
Yamaguchi H, Kitayama J, Ishigami H, Emoto S, Yamashita H, Watanabe T. A phase 2 trial of intravenous and intraperitoneal paclitaxel combined with S-1 for treatment of gastric cancer with macroscopic peritoneal metastasis. Cancer. 2013;119:3354–8.
Fujiwara Y, Takiguchi S, Nakajima K, Miyata H, Yamasaki M, Kurokawa Y, et al. Neoadjuvant intraperitoneal and systemic chemotherapy for gastric cancer patients with peritoneal dissemination. Ann Surg Oncol. 2011;18(13):3726–31.
Pazdur R, Lassere Y, Soh LT, Ajani JA, Bready B, Soo E, et al. Phase II trial of docetaxel (Taxotere) in metastatic colorectal carcinoma. Ann Oncol. 1994;5(5):468–70.
Sternberg CN, ten Bokkel Huinink WW, Smyth JF, Bruntsch V, Dirix LY, Pavlidis NA, et al. Docetaxel (Taxotere), a novel taxoid, in the treatment of advanced colorectal carcinoma: an EORTC Early Clinical Trials Group Study. Br J Cancer. 1994;70(2):376–9.
Einzig AI, Neuberg D, Wiernik PH, Grochow LB, Ramirez G, O’Dwyer PJ, et al. Phase II trial of paclitaxel in patients with advanced colon cancer previously untreated with cytotoxic chemotherapy: an Eastern Cooperative Oncology Group Trial (PA286). Am J Ther. 1996;3(11):750–4.
Hribaschek A, Ridwelski K, Pross M, Meyer F, Kuhn R, Halangk W, et al. Intraperitoneal treatment using taxol is effective for experimental peritoneal carcinomatosis in a rat model. Oncol Rep. 2003;10(6):1793–8.
Hribaschek A, Meyer F, Schneider-Stock R, Pross M, Ridwelski K, Lippert H. Comparison of intraperitoneal with intravenous administration of taxol in experimental peritoneal carcinomatosis. Chemotherapy. 2007;53(6):410–7.
Matsui A, Okuda M, Tsujitsuka K, Enomoto K, Maruyama K. Pharmacology of intraperitoneal CPT-11. Surg Oncol Clin North Am. 2003;12(3):795–811, xv.
Elias D, Matsuhisa T, Sideris L, Liberale G, Drouard-Troalen L, Raynard B, et al. Heated intra-operative intraperitoneal oxaliplatin plus irinotecan after complete resection of peritoneal carcinomatosis: pharmacokinetics, tissue distribution and tolerance. Ann Oncol. 2004;15(10):1558–65.
Quenet F, Goere D, Mehta SS, Roca L, Dumont F, Hessissen M, et al. Results of two bi-institutional prospective studies using intraperitoneal oxaliplatin with or without irinotecan during HIPEC after cytoreductive surgery for colorectal carcinomatosis. Ann Surg. 2011;254(2):294–301.
Sugarbaker PH, Gianola FJ, Speyer JC, Wesley R, Barofsky I, Meyers CE. Prospective, randomized trial of intravenous versus intraperitoneal 5-fluorouracil in patients with advanced primary colon or rectal cancer. Surgery. 1985;98(3):414–22.
Patriarca C, Macchi RM, Marschner AK, Mellstedt H. Epithelial cell adhesion molecule expression (CD326) in cancer: a short review. Cancer Treat Rev. 2012;38(1):68–75.
Bokemeyer C. Catumaxomab—trifunctional anti-EpCAM antibody used to treat malignant ascites. Expert Opin Biol Ther. 2010;10(8):1259–69.
Riesenberg R, Buchner A, Pohla H, Lindhofer H. Lysis of prostate carcinoma cells by trifunctional bispecific antibodies (alpha EpCAM x alpha CD3). J Histochem Cytochem. 2001;49(7):911–7.
Ruf P, Lindhofer H. Induction of a long-lasting antitumor immunity by a trifunctional bispecific antibody. Blood. 2001;98(8):2526–34.
Schmitt M, Schmitt A, Reinhardt P, Thess B, Manfras B, Lindhofer H, et al. Opsonization with a trifunctional bispecific (alphaCD3 x alphaEpCAM) antibody results in efficient lysis in vitro and in vivo of EpCAM positive tumor cells by cytotoxic T lymphocytes. Int J Oncol. 2004;25(4):841–8.
Ruf P, Gires O, Jager M, Fellinger K, Atz J, Lindhofer H. Characterisation of the new EpCAM-specific antibody HO-3: implications for trifunctional antibody immunotherapy of cancer. Br J Cancer. 2007;97(3):315–21.
Strohlein MA, Heiss MM. The trifunctional antibody catumaxomab in treatment of malignant ascites and peritoneal carcinomatosis. Future Oncol. 2010;6(9):1387–94.
Heiss MM, Murawa P, Koralewski P, Kutarska E, Kolesnik OO, Ivanchenko VV, et al. The trifunctional antibody catumaxomab for the treatment of malignant ascites due to epithelial cancer: results of a prospective randomized phase II/III trial. Int J Cancer. 2010;127(9):2209–21.
Wimberger P, Gilet H, Gonschior AK, Heiss MM, Moehler M, Oskay-Oezcelik G, et al. Deterioration in quality of life (QoL) in patients with malignant ascites: results from a phase II/III study comparing paracentesis plus catumaxomab with paracentesis alone. Ann Oncol. 2012;23(8):1979–85.
Ferrara N, Gerber HP, LeCouter J. The biology of VEGF and its receptors. Nat Med. 2003;9(6):669–76.
Ferrara N, Hillan KJ, Gerber HP, Novotny W. Discovery and development of bevacizumab, an anti-VEGF antibody for treating cancer. Nat Rev Drug Discov. 2004;3(5):391–400.
Hurwitz H, Fehrenbacher L, Novotny W, Cartwright T, Hainsworth J, Heim W, et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med. 2004;350(23):2335–42.
Ohtsu A, Shah MA, Van Cutsem E, Rha SY, Sawaki A, Park SR, et al. Bevacizumab in combination with chemotherapy as first-line therapy in advanced gastric cancer: a randomized, double-blind, placebo-controlled phase III study. J Clin Oncol. 2011;29(30):3968–76.
Parsons SL, Watson SA, Steele RJ. Malignant ascites. Br J Surg. 1996;83(1):6–14.
Ayantunde AA, Parsons SL. Pattern and prognostic factors in patients with malignant ascites: a retrospective study. Ann Oncol. 2007;18(5):945–9.
Zebrowski BK, Liu W, Ramirez K, Akagi Y, Mills GB, Ellis LM. Markedly elevated levels of vascular endothelial growth factor in malignant ascites. Ann Surg Oncol. 1999;6(4):373–8.
Kobold S, Hegewisch-Becker S, Oechsle K, Jordan K, Bokemeyer C, Atanackovic D. Intraperitoneal VEGF inhibition using bevacizumab: a potential approach for the symptomatic treatment of malignant ascites? Oncologist. 2009;14(12):1242–51.
Aoyagi K, Kouhuji K, Yano S, Miyagi M, Imaizumi T, Takeda J, et al. VEGF significance in peritoneal recurrence from gastric cancer. Gastric Cancer. 2005;8(3):155–63.
Yagi Y, Fushida S, Harada S, Tsukada T, Kinoshita J, Oyama K, et al. Biodistribution of humanized anti-VEGF monoclonal antibody/bevacizumab on peritoneal metastatic models with subcutaneous xenograft of gastric cancer in mice. Cancer Chemother Pharmacol. 2010;66(4):745–53.
Shah DK, Veith J, Bernacki RJ, Balthasar JP. Evaluation of combined bevacizumab and intraperitoneal carboplatin or paclitaxel therapy in a mouse model of ovarian cancer. Cancer Chemother Pharmacol. 2011;68(4):951–8.
Ninomiya S, Inomata M, Tajima M, Ali AT, Ueda Y, Shiraishi N, et al. Effect of bevacizumab, a humanized monoclonal antibody to vascular endothelial growth factor, on peritoneal metastasis of MNK-45P human gastric cancer in mice. J Surg Res. 2009;154(2):196–202.
Imaizumi T, Aoyagi K, Miyagi M, Shirouzu K. Suppressive effect of bevacizumab on peritoneal dissemination from gastric cancer in a peritoneal metastasis model. Surg Today. 2010;40(9):851–7.
Matsumura Y, Maeda H. A new concept for macromolecular therapeutics in cancer chemotherapy: mechanism of tumoritropic accumulation of proteins and the antitumor agent smancs. Cancer Res. 1986;46(12 Pt 1):6387–92.
Peer D, Karp JM, Hong S, Farokhzad OC, Margalit R, Langer R. Nanocarriers as an emerging platform for cancer therapy. Nat Nanotechnol. 2007;2(12):751–60.
Davis ME, Chen ZG, Shin DM. Nanoparticle therapeutics: an emerging treatment modality for cancer. Nat Rev Drug Discov. 2008;7(9):771–82.
Matsumura Y, Kataoka K. Preclinical and clinical studies of anticancer agent-incorporating polymer micelles. Cancer Sci. 2009;100(4):572–9.
Boucher Y, Baxter LT, Jain RK. Interstitial pressure gradients in tissue-isolated and subcutaneous tumors: implications for therapy. Cancer Res. 1990;50(15):4478–84.
Kyle AH, Huxham LA, Yeoman DM, Minchinton AI. Limited tissue penetration of taxanes: a mechanism for resistance in solid tumors. Clin Cancer Res. 2007;13(9):2804–10.
Minchinton AI, Tannock IF. Drug penetration in solid tumours. Nat Rev Cancer. 2006;6(8):583–92.
Jain RK, Stylianopoulos T. Delivering nanomedicine to solid tumors. Nat Rev Clin Oncol. 2010;7(11):653–64.
Vicent MJ, Duncan R. Polymer conjugates: nanosized medicines for treating cancer. Trends Biotechnol. 2006;24(1):39–47.
Duncan R. Polymer conjugates as anticancer nanomedicines. Nat Rev Cancer. 2006;6(9):688–701.
Maeda H, Wu J, Sawa T, Matsumura Y, Hori K. Tumor vascular permeability and the EPR effect in macromolecular therapeutics: a review. J Control Release. 2000;65(1–2):271–84.
Xiao K, Luo J, Fowler WL, Li Y, Lee JS, Xing L, et al. A self-assembling nanoparticle for paclitaxel delivery in ovarian cancer. Biomaterials. 2009;30(30):6006–16.
Colson YL, Liu R, Southard EB, Schulz MD, Wade JE, Griset AP, et al. The performance of expansile nanoparticles in a murine model of peritoneal carcinomatosis. Biomaterials. 2011;32(3):832–40.
Liu Y, Pan J, Feng SS. Nanoparticles of lipid monolayer shell and biodegradable polymer core for controlled release of paclitaxel: effects of surfactants on particles size, characteristics and in vitro performance. Int J Pharm. 2010;395(1–2):243–50.
Konno T, Watanabe J, Ishihara K. Enhanced solubility of paclitaxel using water-soluble and biocompatible 2-methacryloyloxyethyl phosphorylcholine polymers. J Biomed Mater Res A. 2003;65(2):209–14.
Desai N, Trieu V, Yao Z, Louie L, Ci S, Yang A, et al. Increased antitumor activity, intratumor paclitaxel concentrations, and endothelial cell transport of cremophor-free, albumin-bound paclitaxel, ABI-007, compared with cremophor-based paclitaxel. Clin Cancer Res. 2006;12(4):1317–24.
Gradishar WJ, Tjulandin S, Davidson N, Shaw H, Desai N, Bhar P, et al. Phase III trial of nanoparticle albumin-bound paclitaxel compared with polyethylated castor oil-based paclitaxel in women with breast cancer. J Clin Oncol. 2005;23(31):7794–803.
Petrelli F, Borgonovo K, Barni S. Targeted delivery for breast cancer therapy: the history of nanoparticle-albumin-bound paclitaxel. Expert Opin Pharmacother. 2010;11(8):1413–32.
Hamaguchi T, Matsumura Y, Suzuki M, Shimizu K, Goda R, Nakamura I, et al. NK105, a paclitaxel-incorporating micellar nanoparticle formulation, can extend in vivo antitumour activity and reduce the neurotoxicity of paclitaxel. Br J Cancer. 2005;92(7):1240–6.
Negishi T, Koizumi F, Uchino H, Kuroda J, Kawaguchi T, Naito S, et al. NK105, a paclitaxel-incorporating micellar nanoparticle, is a more potent radiosensitising agent compared to free paclitaxel. Br J Cancer. 2006;95(5):601–6.
Kato K, Chin K, Yoshikawa T, Yamaguchi K, Tsuji Y, Esaki T, et al. Phase II study of NK105, a paclitaxel-incorporating micellar nanoparticle, for previously treated advanced or recurrent gastric cancer. Invest New Drugs. 2012;30:1621–7.
Nakajima TE, Yanagihara K, Takigahira M, Yasunaga M, Kato K, Hamaguchi T, et al. Antitumor effect of SN-38-releasing polymeric micelles, NK012, on spontaneous peritoneal metastases from orthotopic gastric cancer in mice compared with irinotecan. Cancer Res. 2008;68(22):9318–22.
Reddy LH, Adhikari JS, Dwarakanath BS, Sharma RK, Murthy RR. Tumoricidal effects of etoposide incorporated into solid lipid nanoparticles after intraperitoneal administration in Dalton’s lymphoma bearing mice. AAPS J. 2006;8(2):E254–62.
Soma D, Kitayama J, Konno T, Ishihara K, Yamada J, Kamei T, et al. Intraperitoneal administration of paclitaxel solubilized with poly(2-methacryloxyethyl phosphorylcholine-co n-butyl methacrylate) for peritoneal dissemination of gastric cancer. Cancer Sci. 2009;100(10):1979–85.
Kamei T, Kitayama J, Yamaguchi H, Soma D, Emoto S, Konno T, et al. Spatial distribution of intraperitoneally administrated paclitaxel nanoparticles solubilized with poly (2-methacryloxyethyl phosphorylcholine-co n-butyl methacrylate) in peritoneal metastatic nodules. Cancer Sci. 2010;102(1):200–5.
Emoto S, Yamaguchi H, Kishikawa J, Yamashita H, Ishigami H, Kitayama J. Antitumor effect and pharmacokinetics of intraperitoneal NK105, a nanomicellar paclitaxel formulation for peritoneal dissemination. Cancer Sci. 2012;103(7):1304–10.
Echarri Gonzalez MJ, Green R, Muggia FM. Intraperitoneal drug delivery for ovarian cancer: why, how, who, what, and when? Oncology (Williston Park). 2011;25(2):156–165, 170.
Kondo A, Maeta M, Oka A, Tsujitani S, Ikeguchi M, Kaibara N. Hypotonic intraperitoneal cisplatin chemotherapy for peritoneal carcinomatosis in mice. Br J Cancer. 1996;73(10):1166–70.
Tsujitani S, Oka A, Kondo A, Katano K, Oka S, Saito H, et al. Administration in a hypotonic solution is preferable to dose escalation in intraperitoneal cisplatin chemotherapy for peritoneal carcinomatosis in rats. Oncology. 1999;57(1):77–82.
Howell SB. Pharmacologic principles of intraperitoneal chemotherapy for the treatment of ovarian cancer. Int J Gynecol Cancer. 2008;18(Suppl 1):20–5.
Luo Y, Kirker KR, Prestwich GD. Cross-linked hyaluronic acid hydrogel films: new biomaterials for drug delivery. J Control Release. 2000;69(1):169–84.
Wang Y, Gong C, Yang L, Wu Q, Shi S, Shi H, et al. 5-FU-hydrogel inhibits colorectal peritoneal carcinomatosis and tumor growth in mice. BMC Cancer. 2010;10:402.
Yu J, Lee HJ, Hur K, Kwak MK, Han TS, Kim WH, et al. The antitumor effect of a thermosensitive polymeric hydrogel containing paclitaxel in a peritoneal carcinomatosis model. Invest New Drugs. 2012;30(1):1–7.
Bajaj G, Kim MR, Mohammed SI, Yeo Y. Hyaluronic acid-based hydrogel for regional delivery of paclitaxel to intraperitoneal tumors. J Control Release. 2012;158(3):386–92.
Yeo Y, Highley CB, Bellas E, Ito T, Marini R, Langer R, et al. In situ cross-linkable hyaluronic acid hydrogels prevent post-operative abdominal adhesions in a rabbit model. Biomaterials. 2006;27(27):4698–705.
Ito T, Yeo Y, Highley CB, Bellas E, Benitez CA, Kohane DS. The prevention of peritoneal adhesions by in situ cross-linking hydrogels of hyaluronic acid and cellulose derivatives. Biomaterials. 2007;28(6):975–83.
Shimizu A, Suhara T, Ito T, Omichi K, Naruse K, Hasegawa K, et al. A new hepatectomy-induced postoperative adhesion model in rats, and evaluation of the efficacy of anti-adhesion materials. Surg Today. 2014;44:314–23.
Qiu Y, Park K. Environment-sensitive hydrogels for drug delivery. Adv Drug Deliv Rev. 2001;53(3):321–39.
Kwak MK, Hur K, Yu JE, Han TS, Yanagihara K, Kim WH, et al. Suppression of in vivo tumor growth by using a biodegradable thermosensitive hydrogel polymer containing chemotherapeutic agent. Invest New Drugs. 2010;28(3):284–90.
Wu W, Liu J, Cao S, Tan H, Li J, Xu F, et al. Drug release behaviors of a pH sensitive semi-interpenetrating polymer network hydrogel composed of poly(vinyl alcohol) and star poly[2-(dimethylamino)ethyl methacrylate]. Int J Pharm. 2011;416(1):104–9.
He C, Kim SW, Lee DS. In situ gelling stimuli-sensitive block copolymer hydrogels for drug delivery. J Control Release. 2008;127(3):189–207.
Emoto S, Yamaguchi H, Kamei T, Ishigami H, Suhara T, Suzuki Y et al: Intraperitoneal administration of cisplatin via an in situ cross-linkable hyaluronic acid-based hydrogel for peritoneal dissemination of gastric cancer. Surg Today. 2013.
Auzenne E, Ghosh SC, Khodadadian M, Rivera B, Farquhar D, Price RE, et al. Hyaluronic acid-paclitaxel: antitumor efficacy against CD44(+) human ovarian carcinoma xenografts. Neoplasia. 2007;9(6):479–86.
Luo Y, Ziebell MR, Prestwich GD. A hyaluronic acid-taxol antitumor bioconjugate targeted to cancer cells. Biomacromolecules. 2000;1(2):208–18.
Cai S, Xie Y, Bagby TR, Cohen MS, Forrest ML. Intralymphatic chemotherapy using a hyaluronan-cisplatin conjugate. J Surg Res. 2008;147(2):247–52.
Acknowledgments
This work was funded by the Ministry of Education, Culture, Sports, Science and Technology of Japan and the Ministry of Health, Labor and Welfare of Japan, and by a grant-in-aid from the Public Trust Surgery Research Fund, Tokyo, Japan.
Conflict of interest
Shigenobu Emoto received a grant from the Public Trust Surgery Research Fund.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Emoto, S., Sunami, E., Yamaguchi, H. et al. Drug development for intraperitoneal chemotherapy against peritoneal carcinomatosis from gastrointestinal cancer. Surg Today 44, 2209–2220 (2014). https://doi.org/10.1007/s00595-014-0848-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-014-0848-x