Abstract
Purpose
To evaluate the feasibility of cortical bone trajectory (CBT) screws fixation via pedicle or pedicle rib unit in the cadaveric thoracic spine (T9–T12).
Methods
Computed tomography (CT) images of 100 patients are analyzed by multiplanar reconstruction. Ten cadaveric thoracic spines are used to insert 4.5 × 35.0 mm CBT screws at all levels from T9 to T12.
Results
Maximal screw length obtained by CT has a tendency to gradually increase from T9 (29.64 mm) to T12 (32.84 mm), and the difference reaches significant level at all levels except T9 versus T10 (P < 0.01). Maximal screw diameter increases from T9 (4.92 mm) to T12 (7.47 mm) and the difference reaches significant level among all levels (P < 0.01). Lateral angle increases from T9 (7.37°) to T12 (10.47°), and the difference reaches significant level among all levels except T11 versus T12. Cephalad angle from T9 to T12 are 19.03°, 22.10°, 25.62° and 27.50° (P < 0.01), respectively. The percentage of the inner and outer pedicle breakage are 2.5 and 22.5 %, respectively. The violation of lateral pedicle wall occurs at T9 and T10, especially for women at T9.
Conclusions
Both radiographic and cadaveric studies establish the feasibility of CBT screws placement via pedicle or pedicle rib unit in the lower thoracic spine (T9–T12). Furthermore, our measurements are also useful for application of this technique.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Santoni et al. [1] are the first to introduce lumbar cortical bone trajectory (CBT) technique and demonstrates a 30 % increase in uniaxial yield pullout load relative to the traditional pedicle screws. The trajectory of traditional pedicle screw uses a transpedicular path through the anatomic axis of the pedicle, however, the new cortical trajectory follows a caudocephalad path sagittally and a laterally directed path in the transverse plane, engaging with cortical bone maximally from the pedicle to the vertebral body. At the same time, a new screw design that is shorter and smaller than the traditional pedicle screw, which may maximize the thread contact with this higher density bone surface. Moreover, single level minimally invasive posterior lumbar fusion with CBT screws demonstrates significantly lower rate of screw loosening, less loss of correction, and is less invasive compared to that with percutaneous pedicle screws fixation [2]. In addition, a new fusion technique that combined O-arm guided navigation and lumbar CBT screws to treat patients with symptomatic adjacent-segment lumbar disease, eliminating the need to expose, remove, or connect to preexisting hardware, with the benefits of reduced operative time, blood loss, and dissection [3]. Although other morphometric and biochemical studies have supported the use of lumbar CBT screws [4, 5], long term follow-up studies still should be performed to fully understand the clinical outcome of this method [6].
Since then, Matsukawa et al. [7] investigated thoracic CBT technique (T9–T12), which was angulating cranially toward the posterior one-third of the superior endplate in the sagittal plane, and directed straight forward in the transverse plane, however, their CBT technique also has some drawbacks. First of all, the percentage of pedicle width 4.5 mm and lesser is extremely high in women (34.75 % at T9 and 13.56 % at T10) as compared with men (7.46 % at T9 and 2.99 % at T10) [8]. Thus, Matsukawa et al. inserted 5.5-mm-diameter thoracic CBT screws only via pedicle, which is not suitable for some patients at T9 and T10, especially women. Besides, the starting point of their technique is around the lateral part of the pars edge, increasing high possibility of lateral pars fracture, especially T12, since the lamina width is smaller than that of upper levels. Eventually, the original lumbar CBT screws follow a laterally directed path in the transverse plane, whereas Matsukawa’s technique is without a lateral angle in the transverse plane, indicating that it reduces the advantage to avoid spinal cord injury when compared with the original lumbar CBT screws.
According to that, we investigate CBT screws fixation via pedicle or pedicle rib unit in the lower thoracic spine, following caudad part of the pedicle with a caudocephalad path toward the superior endplate sagittally, and a laterally directed path in the transverse plane (Figs. 1, 2a, b). In the present study, we conduct morphometric measurement using computed tomography (CT) and also insert screws in cadaveric specimens to assess the feasibility of our technique.
Reconstructed three-dimensional image demonstrates CBT screws placed in lower thoracic spine (T9–T12). Bone widow is made transparent to enable visualization of screws. a AP view, CBT screws with a laterally directed path in the transverse plane. b Lateral view, CBT screws follow caudad part of the pedicle with a caudocephalad path toward the superior endplate in the sagittal plane. c Posterior view, screw heads of CBT technique are line-up in the sagittal plane
Materials and methods
Clinical materials
The research was approved by the institutional review board of the hospital. We carried out the study on patients who came to the Second Affiliated Hospital of Wenzhou Medical University for lung diseases and underwent chest CT scans from January 2011 to October 2015. Standard CT images (5 mm thickness) were obtained by Philips Brilliance 256 iCT scan machine (Philips Medical Systems, Eindhoven, and The Netherlands). Reformatted images with a thickness ≤1 mm were obtained from these images. Scan parameters included: 120 kV, 180 MA, 512 × 512 matrix, layer thickness of 0.9 mm, collimation of 128 × 0.625 mm, pitch of 0.6 mm, Dose Right of Z-DOM and 250 mAs/Slice. Then, original data were entered into the EBW work station (a post-processing work station of the Philips Medical System) and 2-dimensional image reconstruction performed by multiplanar reconstruction. CT scans of thoracic vertebrae (50 men and 50 women, mean age 49.60 ± 9.50 years, range 30–68 years) were randomly selected for this study, and the exclusion criteria for evaluation consisted of thoracic spine with any deformities, trauma, tumor, or infection.
Measurement methods
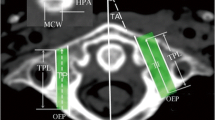
All measurements in our study were performed by one spine surgeon who was familiar with the anatomy and the screw insertion technique in lower thoracic spine (T9–T12). Every parameter was measured three times in one patient by the spine surgeon. The mean was obtained to be the ultimate value. We used the method to minimize the deviation and make our research more reliable. Firstly, we increased layer thickness of the coronary plane to exhibit the pedicle projection, therefore, we can move horizontal and sagittal axis to the lower and medial border of pedicle projection, respectively. Then, we drew an angle of 45° to make the angle’s extension line to overlap pedicle projection, and we can find there was a point of intersection between the extended line and the pedicle projection, which was the starting point (Fig. 3). Thirdly, we enhanced the layer thickness of the sagittal plane, and adjusted the horizontal axis to make it overlap the anatomic axis of the pedicle projection to obtain a new axial plane (Figs. 3, 4). Finally, we measured the following parameters: (1) maximal screw length, (2) maximal screw diameter, (3) lateral angle, (4) cephalad angle (Figs. 3, 5).
CBT screws placement via pedicle or pedicle rib unit in cadaveric specimens
Ten cadaveric thoracic spines (6 men and 4 women, mean age 56.10 ± 9.26 years, range 42–71 years) were provided by the Department of Anatomy, Wenzhou Medical University. Lateral and anteroposterior (AP) X-rays were taken to exclude obvious neoplastic, traumatic, congenital conditions, earlier surgery, or facet arthropathy. Three of cadaveric spines (2 men and 1 woman) were separated at each level from T9 to T12 (Group S) and seven thoracic specimens (4 men and 3 women) were not separated (Group NS). Similar to the lumbar CBT technique [9], the screw was inserted approximately at the 5 (7) o’clock orientation and aimed in the 11–12 (12–1) o’clock direction of the pedicle (Fig. 6a), and also followed caudad part of the pedicle with a caudocephalad path toward the superior endplate sagittally (Figs. 1b, 6b). The screw insertion point was the intersection of the center of the superior articular process and the middle of the transverse process for T9, T10, T11, and inferior 1/3 of the transverse process for T12 (Fig. 7). All vertebrae were placed with 4.5 × 35.0 mm CBT screws in both sides. The position of the screw was identified by lateral and AP views in Group NS and axial view was also obtained in Group S through Kubtec® Radiography System. Finally, we checked inner or outer cortex breakage of 80 CBT screws via splitting vertebrae in Group NS or axial view of X-Ray image in Group S, respectively.
Screw insertion point for CBT screws. a CBT screws are inserted in the cadaveric specimen. b The blue line, the middle of transverse process, the red line, inferior 1/3 of transverse process, the black line, the center of the superior facet. The white circle, starting point for T9–T11, the green circle, screw entry point for T12
Statistical analysis
Statistical analysis was performed using SPSS statistical software program 22.0 (SPSS Inc.). Mean values and corresponding standard deviations were calculated and independent sample t-test was used for the test of differences between male and female. One-way analysis of variance and the Tukey analysis were performed for statistical comparison among each thoracic segment. A P value of less than 0.05 was selected to represent statistical significance.
Results
Maximal screw length (MSL) and Maximal screw diameter (MSD)
MSL had a tendency to gradually increase from T9 to T12, and the difference reached significant level at all levels except T9 versus T10 (P < 0.01). There were significant differences between male and female for T9, T11, and T12 (P < 0.01) (Table 1). MSD gradually increased from T9 (4.92 mm) to T12 (7.47 mm). The difference reached significant level among all levels (P < 0.01). There were significant differences between male and female among all levels (P < 0.01) (Table 1).
Lateral angle (LA) and cephalad angle (CA)
LA increased from T9 (7.37°) to T12 (10.47°), and the difference reached significant level among all levels except T11 versus T12. There were no significant differences between male and female (P > 0.05) (Table 1). CA from T9 to T12 were 19.03°, 22.10°, 25.62°, and 27.50°, respectively. There were significant differences among all levels (P < 0.01) and no significant differences between male and female (P > 0.05) (Table 1).
Inner or outer pedicle cortex breakage
There was no pedicle cortex breakage of CBT screws in Group S. In Group N–S, two inner pedicle cortices and eighteen outer pedicle cortices were violated. Percentage of outer pedicle cortex breakage at T9 and T10 was higher than that of other levels, especially women (Table 2).
Discussion
CBT screws fixation has evolved as a method of spinal instrumentation that may avoid some limitations of traditional pedicle screw fixation [10]. Wray et al. [11] have demonstrated that cortical trajectory could provide denser bone that allows for utilization of smaller screws to obtain mechanical purchase that is equivalent to long pedicle screws placed in traditional pedicle screw trajectories for both normal and low quality bone. As an alternative method to conventional pedicle screw fixation, we investigated thoracic CBT screws placement via pedicle or pedicle rib unit (Figs. 8, 9). Several studies reported that a significantly larger screw can be placed within the pedicle rib unit, which enlarged transverse width of the area of insertion [12–14]. CBT screws fixation via pedicle rib unit can result in costovertebral joint violation, however, the frequently used “in–out-in” technique, which also penetrated the lateral pedicle wall and passed out into the costovertebral articulation to avoid penetration of the medial pedicle wall. It was commonly performed in cases in which the pedicle width was clearly lesser than the intended screw diameter [8, 15].
According to our measurements, maximal screw diameter from T9 to T12 were 4.92, 5.83, 6.88, 7.47 mm, and maximal screw diameter 4.5 mm and lesser accounted for 27.03 % at T9 in women and 14 % at T9 in men. Zhuang et al. [8] studied pedicle width of the isthmus and showed its width ranged from 5.85 mm at T9 to 8.99 mm at T12 in men and 4.89 mm at T9 to 7.56 mm at T12 in women. What’s more, they also found the percentage of pedicle width ≤4.5 mm was extremely high in women (34.75 % at T9) as compared with men (7.46 % at T9). Therefore, some patients may not be placed with ≥4.5 mm CBT screws only via pedicle at T9, especially women. Maximal screw length increased from T9 (29.64 mm) to T12 (32.84 mm), which indicated 30-35 mm length CBT screws could be used in the spinal surgery.
Karataglis et al. [16] have shown that preservation of the dorsal vertebral cortex provided 26 % increase in peak pullout strength. Regions of higher density bone are found in the posterior-lateral portions of the vertebral body, and adjacent to the vertebral endplate [17–19]. Moreover, Lehman et al. [20] found caudad half of the pedicle was denser, and that withstood higher forces as compared with the cephalad aspect. Eventually, osteoporosis caused preferential bone loss in the center of the vertebral body, with the cortical shell relatively unaffected [21]. Thus, we proposed our CBT screws obtained six points purchase (Figs. 1b, 8, 9): dorsal cortex of lamina, medially or laterally oriented pedicle wall, lateral margin of the vertebral body, subendplate cortical bone and caudad part of the pedicle, even the medial wall of rib head, which have higher bone mineral density. In Group S, where all vertebrae were separated from thoracic spine, there was no inner or outer pedicle cortex breakage. On the contrary, in spinal columns where segments were not separated (Group N–S) reflecting a more clinical situation, using a free-hand technique based on our trajectory, showed eighteen outer cortex breakages and mainly occurred at T9 and T10, especially women at T9, which suggested we should insert CBT screws through pedicle rib unit at above levels in some patients. No screws broke outer pedicle cortex at T11 and T12, and maximal screw diameter was 6.88 mm at T11 and 7.47 mm at T12, which suggested the pedicle might accommodate 4.5–5.5 mm CBT screws at above levels.
There were six advantages of this CBT technique. Firstly, Ugur et al. [22] demonstrated pedicle–dural sac distance ranged from 0 to 0.7 mm so that improper screw insertion angle could cause neurologic damage. Trajectory of CBT screws was medial to lateral, which can decrease the incidence of spinal cord injury and contribute to reducing the surgeon’s stress in clinical practice. Secondly, screw insertion through a medial starting point enabled less tissue dissection and retraction for reduced muscle disruption. Thirdly, CBT technique can be utilized as a useful method to rescue failed screw because of the trajectory of CBT technique was different from that of traditional screw. Fourthly, the three dimensional position of the screw heads also can line-up in the sagittal plane without complicated rod bending compared with lumbar CBT screws when using it multilevel (Figs. 2c, 7a). Fifthly, we chose 5 o’clock orientation of the pedicle as the screw insertion point, more medial to the isthmus portion as compared with Matsukawa’s technique, decreasing the risk of isthmus fracture, especially T12. Finally, the aorta run anterolaterally (to the left) in the cephalad and middle aspects of the thorax, but changed to a vertebral midline position in the caudad part of the thorax. At the same time, CBT screws ended up in one-third or half of the superior endplate, indicating that the CBT technique had little possibility penetrating anterior vertebral cortex to cause aorta injury as compared with the traditional screw. Nevertheless, the above merits have to be proven in clinical trials.
In our study, there are some limitations deserved to be mentioned. First of all, previous studies have shown some differences between the thoracic pedicle size in Caucasian and Asian populations [23–25], but we performed our study in the Asian population. Therefore, further study should be carried out to analyze whether there is a difference among human races when using thoracic CBT screws. Considering, the CBT screw is shorter and smaller in length and diameter than the traditional pedicle screw to maximize the thread contact with higher density bone surface [1], we chose 4.5 mm diameter screw to carry out the thoracic CBT technique in cadavers, which may decrease the incidence of misplacement as compared with 5.5 mm diameter screw. Thus, further study is needed to compare the malposition rate between 4.5 and 5.5 mm diameter CBT screws. In addition, we will investigate the screw stability of 4.5–5.5 mm diameter thoracic CBT screws through biomechanical tests. Given the CBT screws should engage with cortical bone maximally, we measured the width of the outer margin of the cortex, however, further study still should be carried out to investigate how to accurately measure the acceptable screw diameter of the CBT technique. What’s more, assessing what is the optical pedicle diameter to accommodate 4.5–5.5 mm diameter thoracic CBT screw according to clinical experience is necessary to further study. Fourthly, we should perform the process of decompression before inserting CBT screws owing to the fact that the medial position of the screw head may lead to no space to perform decompression. Finally, it is important to prepare the screw path carefully to avoid cephalad facet joint violation.
Conclusion
In conclusion, our cadaveric study demonstrates that patients can be placed with 4.5 mm CBT screws at T11 and T12 via pedicle. However, we may insert 4.5 mm CBT screws via pedicle rib unit at T9 and T10 in some patients, especially women at T9. Besides, findings of our study provide insights into screw size and insertion angle decision when performing thoracic CBT screws (T9–T12) in spinal surgery.
References
Santoni BG, Hynes RA, McGilvray KC, Rodriguez-Canessa G, Lyons AS, Henson MA, Womack WJ, Puttlitz CM (2009) Cortical bone trajectory for lumbar pedicle screws. Spine J 9(5):366–373. doi:10.1016/j.spinee.2008.07.008
Gonchar I, Kotani Y, Matsumoto Y (2014) Cortical bone trajectory versus percutaneous pedicle screw in minimally invasive posterior lumbar fusion. Spine J 14(11, Supplement):S114–S115. doi:10.1016/j.spinee.2014.08.286
Rodriguez A, Neal MT, Liu A, Somasundaram A, Hsu W, Branch CL Jr (2014) Novel placement of cortical bone trajectory screws in previously instrumented pedicles for adjacent-segment lumbar disease using CT image-guided navigation. Neurosurg Focus 36(3):E9. doi:10.3171/2014.1.focus13521
Matsukawa K, Yato Y, Imabayashi H, Hosogane N, Abe Y, Asazuma T, Chiba K (2016) Biomechanical evaluation of fixation strength among different sizes of pedicle screws using the cortical bone trajectory: what is the ideal screw size for optimal fixation? Acta Neurochir (Wien) 158(3):465–471. doi:10.1007/s00701-016-2705-8
Zhang H, Ajiboye RM, Shamie AN, Wu Q, Chen Q, Chen W (2016) Morphometric measurement of the lumbosacral spine for minimally invasive cortical bone trajectory implant using computed tomography. Eur Spine J 25(3):870–876. doi:10.1007/s00586-015-4224-3
Patel SS, Cheng WK, Danisa OA (2016) Early complications after instrumentation of the lumbar spine using cortical bone trajectory technique. J Clin Neurosci 24:63–67. doi:10.1016/j.jocn.2015.07.018
Matsukawa K, Yato Y, Hynes RA, Imabayashi H, Hosogane N, Asazuma T, Toshiyasu M, Kobayashi Y, Nemoto K (2014) Cortical bone trajectory for thoracic pedicle screws: a technical note. J Spinal Disord Tech. doi:10.1097/bsd.0000000000000130
Zhuang Z, Zhuang Z, Chen Y, Han H, Cai S, Wang X (2011) Thoracic pedicle morphometry in different body height population: a three-dimensional study using reformatted computed tomography. Spine (Phila Pa 1976) 36(24):E1547–E1554. doi:10.1097/BRS.0b013e318210f063
Matsukawa K, Yato Y, Nemoto O, Imabayashi H, Asazuma T, Nemoto K (2013) Morphometric measurement of cortical bone trajectory for lumbar pedicle screw insertion using computed tomography. J Spinal Disord Tech 26(6):E248–E253. doi:10.1097/BSD.0b013e318288ac39
Phan K, Hogan J, Maharaj M, Mobbs RJ (2015) Cortical bone trajectory for lumbar pedicle screw placement: a review of published reports. Orthop Surg 7(3):213–221. doi:10.1111/os.12185
Wray S, Mimran R, Vadapalli S, Shetye SS, McGilvray KC, Puttlitz CM (2015) Pedicle screw placement in the lumbar spine: effect of trajectory and screw design on acute biomechanical purchase. J Neurosurg Spine 22(5):503–510. doi:10.3171/2014.10.spine14205
Husted DS, Haims AH, Haims AH, Fairchild TA, Kershaw TS, Yue JJ, Yue JJ (2004) Morphometric comparison of the pedicle rib unit to pedicles in the thoracic spine. Spine (Phila Pa 1976) 29(2):139–146. doi:10.1097/01.brs.0000105537.49674.a3
Liljenqvist UR, Allkemper T, Hackenberg L, Link TM, Steinbeck J, Halm HF (2002) Analysis of vertebral morphology in idiopathic scoliosis with use of magnetic resonance imaging and multiplanar reconstruction. J Bone Joint Surg Am 84-a(3):359–368
O’Brien MF, Lenke LG, Mardjetko S, Lowe TG, Kong Y, Eck K, Smith D (2000) Pedicle morphology in thoracic adolescent idiopathic scoliosis: is pedicle fixation an anatomically viable technique? Spine (Phila Pa 1976) 25(18):2285–2293
McLain RF, Ferrara L, Kabins M (2002) Pedicle morphometry in the upper thoracic spine: limits to safe screw placement in older patients. Spine (Phila Pa 1976) 27(22):2467–2471. doi:10.1097/01.brs.0000031265.42972.15
Karataglis D, Kapetanos G, Lontos A, Christodoulou A, Christoforides J, Pournaras J (2006) The role of the dorsal vertebral cortex in the stability of transpedicular screws. A biomechanical study in human cadaveric vertebrae. J Bone Joint Surg Br 88(5):692–695. doi:10.1302/0301-620x.88b5.17422
Grant JP, Oxland TR, Dvorak MF (2001) Mapping the structural properties of the lumbosacral vertebral endplates. Spine (Phila Pa 1976) 26(8):889–896
Wu SS, Yuan HA (1998) Stiffness between different directions of transpedicular screws and vertebra. Clin Biomech (Bristol, Avon) 13(1 Suppl 1):S1–S8
Zhao FD, Pollintine P, Hole BD, Adams MA, Dolan P (2009) Vertebral fractures usually affect the cranial endplate because it is thinner and supported by less-dense trabecular bone. Bone 44(2):372–379. doi:10.1016/j.bone.2008.10.048
Lehman RA Jr, Helgeson MD, Dmitriev AE, Paik H, Bevevino AJ, Gaume R, Kang DG, Lenke LG (2012) What is the best way to optimize thoracic kyphosis correction? A micro-CT and biomechanical analysis of pedicle morphology and screw failure. Spine (Phila Pa 1976) 37(19):E1171–E1176. doi:10.1097/BRS.0b013e31825eb8fb
Antonacci MD, Hanson DS, Leblanc A, Heggeness MH (1997) Regional variation in vertebral bone density and trabecular architecture are influenced by osteoarthritic change and osteoporosis. Spine (Phila Pa 1976) 22(20):2393–2401 (discussion 2401–2392)
Ugur HC, Attar A, Uz A, Tekdemir I, Egemen N, Genc Y (2001) Thoracic pedicle: surgical anatomic evaluation and relations. J Spinal Disord 14(1):39–45
Datir SP, Mitra SR (2004) Morphometric study of the thoracic vertebral pedicle in an Indian population. Spine (Phila Pa 1976) 29(11):1174–1181
Kim NH, Lee HM, Chung IH, Kim HJ, Kim SJ (1994) Morphometric study of the pedicles of thoracic and lumbar vertebrae in Koreans. Spine (Phila Pa 1976) 19(12):1390–1394
Liau KM, Yusof MI, Abdullah MS, Abdullah S, Yusof AH (2006) Computed tomographic morphometry of thoracic pedicles: safety margin of transpedicular screw fixation in malaysian malay population. Spine (Phila Pa 1976) 31(16):E545–E550. doi:10.1097/01.brs.0000225978.97652.e0
Acknowledgments
This work was supported by the Grant from National Nature Foundation of China (Grant No: 81371988).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any potential conflict of interest.
Rights and permissions
About this article
Cite this article
Xuan, J., Zhang, D., Jin, HM. et al. Minimally invasive cortical bone trajectory screws placement via pedicle or pedicle rib unit in the lower thoracic spine: a cadaveric and radiographic study. Eur Spine J 25, 4199–4207 (2016). https://doi.org/10.1007/s00586-016-4730-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4730-y