Abstract
Objective
We prospectively compared posterior lumbar interbody fusion (PLIF) and transforaminal lumbar interbody fusion (TLIF) used in adult isthmic spondylolisthesis (IS) after surgical reduction with pedicle screws.
Methods
Between January 2009 and December 2010, 66 adult patients with single-level IS were randomly assigned to two groups treated using the PLIF technique (PLIF group, n = 34) and the TLIF technique (TLIF group, n = 32). Both groups were followed up for an average of 30.5 months (range 24–48 months). Clinical outcomes were assessed using the visual analog scale (VAS), Oswestry disability index (ODI) and Japanese orthopedic association (JOA) scores. Radiographic outcomes included percentage of vertebral slippage, focal lordosis and disk height. Clinical and radiographic outcomes were compared between the two groups.
Results
The average operative time and blood loss during surgery were significantly more in PLIF group than in TLIF group. Spondylolisthesis, disk height and focal lordosis were significantly improved postoperatively in both groups. There was no obvious difference in clinical outcomes, as assessed using the VAS, ODI and JOA scores, and radiographic outcomes. In PLIF group, there were two cases of neuropathic pain after surgery.
Conclusions
After instrumented reduction of adult IS, either PLIF or TLIF can provide good clinical and radiological outcomes. With a single cage, TLIF was superior to PLIF in terms of surgical time and blood loss, but these differences may not be clinically relevant.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
There has been an ongoing debate on whether it is necessary to reduce the slipped vertebra in an adult with isthmic spondylolisthesis (IS). Opponents of reduction techniques cite the increased risk of neurological complications with reduction procedures and do not believe that the benefit to the patient outweighs this potential risk [1, 2]. Advocates for instrumented reduction of spondylolisthesis cite normalization of spine biomechanics, improvements in posture and self-image, enhanced fusion rates, and the restoration of sagittal balance at the involved segment, which is especially prevalent [3, 4]. In numerous previous studies, the number of neurological complications associated with reduction procedures was very low and there was no significant difference from the in situ fusion [3–6]. As a result, using modern surgical techniques and instrumentation, surgical reduction of the slipped vertebra has been recommended by many authors for IS [3, 7, 8].
However, there is still controversy over the choice of fusion technique for IS. Both posterolateral fusion (PLF) and posterior lumbar interbody fusion (PLIF) are widely used in the treatment of IS. In Ekman’s series, they found that the use of PLIF versus PLF as surgical treatment for adult IS had no effect on the patients’ 2-year outcomes [9]. In a recent meta-analysis, Luo et al. stated that there was no significant difference in the global assessment of clinical outcomes between the two fusion procedures [10]. Conversely, the study also suggested that PLF shows a significantly lower fusion rate compared to PLIF [10]. In another study, Feng et al. found that from the point of the sagittal spinopelvic balance, the PLIF may be better than the PLF for patients with IS [11]. In a long-term prospective cohort comparison study, PLIF was found to provide better short-term and long-term results than PLF, and when analyzing only single-level fusions the difference in treatments is more pronounced [12]. Due to its benefits, PLIF, which can maintain the load-bearing capacity of the anterior column and enhance both the opportunity for arthrodesis and restoration of sagittal balance, has been extensively adopted to treat IS [3, 4, 13].
As another modality of interbody fusion from posterior approach, transforaminal lumbar interbody fusion (TLIF) is an alternative option to treat IS [2]. To our knowledge there is little literature comparing PLIF and TLIF after instrumented reduction in adult IS. Therefore, the purpose of this study was to compare these two techniques in a prospective and randomized manner with a focus on surgical invasiveness, clinical and radiographic outcomes, and complications.
Materials and methods
Between January 2009 and December 2010, 73 consecutive adult patients with IS were enrolled in this study. The inclusion criterion was that the patient had single-level IS without degenerative disease in adjacent level. The exclusion criteria included multilevel IS and previous lumbar spine surgery. The study was carried out with the approval of the ethics committee of our hospital.
Every patient was given a serial number according to the consecutive sequence of hospitalization, and randomly assigned to the PLIF group or the TLIF group, according to the serial number. Written informed consent to participate in this study was obtained from all the patients. Seven patients were lost to follow-up within 6 months after the operation. Of the remaining 66 patients (90.4 %), there were 34 patients in PLIF group, and 32 patients in TLIF group. There were 27 men and 39 women, aged from 21 to 62 years (mean 43.4 years) at the time of the surgery. The levels of spondylolisthesis were diagnosed at L4 in 28 cases and L5 in 38 cases. The patients’ age, gender distribution and surgery level were similar in the two groups (Table 1).
Data were collected prospectively by independent observers, using standardized data collection forms.
Surgical technique
All the operations were performed by two senior surgeons (XF and JG), and each surgeon performed both procedures.
A full posterior decompression, including laminectomy and total facetectomy was performed. Pedicle screw instrumentation (Click’X, Synthes, Switzerland) was used to reduce the slipped vertebra with a drawing-back technique [4]. Then the pedicle screws were distracted to increase the interbody disk height for interbody fusion. In PLIF group, the procedure was performed in the standard fashion with two rectangular cages (CO, Scient’x Company, France) packed with autogenous bone graft (Fig. 1). In TLIF group, the procedure was performed in the standard fashion with one kidney-shape cage (CC, Scient’x Company, France) packed with autogenous bone graft (Fig. 2). In both PLIF and TLIF, before cage insertion, the morselized bone graft from facetectomy and laminectomy was grafted into the prepared disc space. Finally, the pedicle screws were compressed to restore the lumbar lordosis.
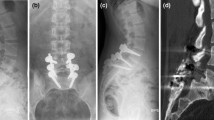
The PLIF procedure with slippage reduction for a 59-year-old woman with IS. The severe disk space collapse and grade II spondylolisthesis was shown on the preoperative lateral X-ray (a). Postoperative X-ray showed that slippage reduction and disk space restoration was obtained (b). Postoperative CT scan showed that two cages were inserted in the intervertebral space with the PLIF procedure (c)
The TLIF procedure with surgical reduction was performed for a 60-year-old woman with IS. Preoperative lateral X-ray showed the severe disk space collapse and grade II spondylolisthesis (a). Postoperative X-ray showed that slippage was almost completely reduced and disk height improved (b). Postoperative CT scan showed that a single cage was inserted in the intervertebral space with the TLIF procedure (c)
Clinical assessment
Clinical outcome was assessed using visual analog scale (VAS), Oswestry Disability Index (ODI) and Japanese Orthopedic Association (JOA) scores preoperatively and at 3 days, 3, 6 months, 1 and 2 years postoperatively. Functional improvement was expressed by the rate of recovery of the JOA score [14].
All surgical complications were recorded.
Radiological assessment
Radiographs were taken in neutral laterally 1 day postoperatively and additional extension-flexion positions at 3, 6, 12, 24 months and final follow-up to evaluate the bony fusion and the sagittal alignment of lumbar spine after surgery. The amount of vertebral slip was measured from the standing lateral radiographs and calculated according to the Taillard technique [15] and Meyerding grade [16]. Focal lordosis was measured with the Cobb technique [17]. Disk space height was normalized as the percentage of the superior endplate over the rostral vertebral body [18].
Radiograph fusion criteria included the presence of bony trabeculation bridging the fusion area and the absence of bony lucency at the area [19]. If it was difficult to decide whether bony fusion was obtained from radiograph, an additional two-dimensional CT scan was taken. The fusion criteria of two-dimensional CT were the ingrowth of bone into the cage and bony graft emanating from the vertebrae (Fig. 3). The radiograph and two-dimensional CT studies were independently evaluated by two spine surgeons and one radiologist.
Statistical analysis
A sample size was calculated according to previous studies and deemed efficient enough to detect a possible relevant clinical difference in surgical outcome [20, 21]. We calculated that a sample population with 29 participants per group would be required to obtain 80 % power to detect differences in the pain score as depicted with VAS, with a standard deviation of 2.0 (α = 0.05 and β = 0.20).
All follow-up data were collected by an independent observer and expressed as mean ± SD. The SPSS statistical program (version 17.0) was used for the statistical analysis. Classic t tests and Chi square tests were used to compare the groups. P values <0.05 were considered statistically significant.
Results
All 66 patients were followed up for 24–48 months (mean 30.5 months). The average operative time was 125 min in PLIF group and 113 min in TLIF group; the difference between the two groups was significant (P = 0.008). The average blood loss during surgery was 521 ml in PLIF group and 433 ml in TLIF group, with a significant difference (P = 0.043, see Table 1).
Clinical outcomes
The patients were encouraged to sit up and to walk with assistance, for two or three postoperative days, to the lavatory to urinate after the drainage tube was removed. Within 1 week after surgery, all patients in both groups could sit up and walk independently.
Before surgery, VAS, ODI and JOA scores were similar between two groups. Both groups showed a significant decrease of VAS scores. Both groups showed a significant improvement in the mean ODI score. The mean JOA scores of both groups also improved significantly (see Table 2). For each data collection time, the differences of VAS, ODI and JOA scores between two groups were not significant (see Table 2). At the final check the postoperative recovery rate of JOA score was 65.6 % in PLIF group and 60.7 % in TLIF group, without significant difference (P = 0.213).
Radiological outcomes
Before surgery, the average of slippage, focal lordosis and disk height was 28.4 %, 12.1°, 13.9 % in PLIF group and 27.1 %, 11.7°, 13.3 % in TLIF group (Table 3). Three months postoperatively, they improved significantly to 5.1 %, 19.7°, 27.3 % in PLIF group and 5.8 %, 18.6°, 26.1 % in TLIF group, respectively (Table 3). Neither group showed substantial further change at final follow-up. At every time point, the average slippage, focal lordosis and disk height were similar in the two groups (Table 3).
All 66 patients achieved spinal fusion with no cases of cage extrusion in the final follow-up.
Surgical complications
Four instances of complications were recorded in PLIF group: neuropathic pain in two patients, cerebrospinal fluid leakage in one patient and wound infection in one patient. Three instances of complications were recorded in TLIF group: two cases of cerebrospinal fluid leakage and one case of wound infection. Both postoperative infections were treated by thorough debridement and continuous irrigation and drainage [22]. Complications in the other five patients resolved with conservative treatment within 3 months postoperatively.
Discussion
The optimal surgical approach to the treatment of adult IS has not been determined yet. As a surgical procedure with low technical demands and surgical risks [23], PLF has been used extensively and effectively to treat IS. However, without providing sufficient anterior column support and ineffectiveness of segmental control, PLF alone may be correlated with a higher incidence of nonunion and an increase in implant-related complications [10]. A biomechanical study has shown that PLIF is superior to PLF in regard to improving anterior column support, restoration of lordosis, and indirect decompression of the foramen [24]. From these results, it is concluded from the point of restoration of sagittal balance at involved segments that PLIF showed superior results to PLF [11]. Recently, in a system review with meta-analysis, the authors indicated that PLIF could improve the clinical satisfaction and increase the fusion rate compared to PLF in spodylolisthesis [25].
The goals of surgical treatment of IS are fusing as few motion segments as possible, restoring the sagittal balance of the lumbar spine, and fusing the disk space if it is not competent. Because fusion in situ is usually performed to extend one or two levels above the slipped vertebrae, fusing normal motion segments [19, 26], many authors advocate reducing the slipped vertebrae to restore sagittal balance of lumbar spine for IS [3, 5, 27, 28]. In a long-term prospective study, Cunningham et al. find that improved sagittal alignment or fusion rate may result in better outcomes [12]. Also, slip reduction and sagittal balance restoration may be important in the long run by preventing premature disk degeneration at the adjacent level [5, 29].
With the development of surgical techniques and instrumentation, many reduction procedures have been developed to reduce spondylolisthetic deformity and restore spinal balance. To fuse as few motion segments as possible in IS without degenerative disease at the adjacent level, monosegmental surgical treatment is advocated [4, 30]. According to previous studies [3, 4], using PLIF technique when the slipped vertebra was reduced with pedicle screws, the sagittal balance can be restored successfully. However, besides PLIF, TLIF is also an alternative method of interbody fusion, with comparable biomechanical stability and segmental flexibility [31]. In a previous study, Recnik et al. demonstrated that reduction of slippage and restoration of disc height were readily achieved with single level TLIF for IS [32]. Therefore, in this prospective randomized study, we compare PLIF and TLIF after instrumented reduction in adult IS.
Both the PLIF and TLIF techniques are more biomechanically stable because with each technique the bone graft is placed along the weight-bearing axis of the spine. The graft is therefore under maximal compression with both the anterior and posterior columns under tension, thus enhancing the opportunity for arthrodesis. In our series, with posterior instrumentation, all the patients in both groups achieved spinal fusion.
When the PLIF procedure is being performed, the thecal sac and nerve root should be mobilized and retracted to the midline, to obtain unobstructed access to the disk. This manipulation can lead to nerve root injury, neuropathic pain and dura tear [33–35]. In our series, two patients in PLIF group complained of neuropathic pain, which may have resulted from nerve root retraction when PLIF was performed. In contrast, because TLIF accesses the intervertebral space via a unilateral posterolateral transforaminal route that avoids retraction of the dura, potential complications that can arise from PLIF, such as postoperative radiculitis, are reduced [36, 37]. In TLIF group of our series, the complication of nerve root injury did not occur with the TLIF procedure. There were three cases of cerebrospinal fluid leakage; one in PLIF group and two in TLIF group, whose dura tearing happened in decompression but not in the interbody fusion procedure. So in our series, with either PLIF or TLIF, the dura will not be torn during the interbody fusion procedure.
Because the dura sac and nerve root obstruct the approach to the disk space when PLIF is performed bilaterally, the spine surgeon must perform the discectomy and cage insertion in a bilateral fashion, increasing the operative time and blood loss. In contrast, TLIF is performed in a unilateral approach to the disk space with a single cage, thus reducing operative time and blood loss. In the present study, the average operative time was 125 min in PLIF group and 113 min in TLIF group (P = 0.008). The average blood loss was 521 ml in PLIF group and 433 ml in TLIF group (P = 0.043). However, in clinical practice, a 12-min time difference and 88 mL difference in blood loss are not significant disparities between the two groups.
With the help by pedicle screws [3, 4], the slipped vertebra could be reduced successfully for adult IS. Combining this technique with PLIF, lumbar sagittal balance could be restored. In our series, after reduction by the pedicle screws, with TLIF the average slippage, focal lordosis and disk height were improved significantly postoperatively. And compared with PLIF, there was no difference in these parameters. For clinical outcomes measured by VAS, ODI and JOA, both groups showed a similar improvement at the same time point. We can conclude that after instrumented reduction of adult IS, both PLIF and TLIF can provide good clinical and radiological outcomes, without clinically significant differences regarding surgical time and blood loss.
The main weakness of this study is the unsatisfactory randomization procedure and small sample population. Instead of setting a maximum required sample population, the study was performed over a two-year period. It is essential to conduct a multicenter prospective randomized trial with more patients in the further study. Another limitation of our study is its relatively short-term follow-up. The measurements of global sagittal alignment and pelvic incidence were not included in this study because gross spinal imbalance is rare in low-grade IS. This is also a significant weakness of the study, as it will not allow an understanding of the relationship of overall sagittal balance and outcomes.
References
Bartolozzi P, Sandri A, Cassini M, Ricci M (2003) One-stage posterior decompression-stabilization and trans-sacral interbody fusion after partial reduction for severe L5–S1 spondylolisthesis. Spine 28:1135–1141. doi:10.1097/01.BRS.0000067274.38273.5C
Goyal N, Wimberley DW, Hyatt A, Zeiller S, Vaccaro AR, Hilibrand AS, Albert TJ (2009) Radiographic and clinical outcomes after instrumented reduction and transforaminal lumbar interbody fusion of mid and high-grade isthmic spondylolisthesis. J Spinal Disord Tech 22:321–327. doi:10.1097/BSD.0b013e318182cdab
Sears W (2005) Posterior lumbar interbody fusion for lytic spondylolisthesis: restoration of sagittal balance using insert-and-rotate interbody spacers. Spine J 5:161–169. doi:10.1016/j.spinee.2004.05.256
Lian XF, Hou TS, Xu JG, Zeng BF, Zhao J, Liu XK, Yang EZ, Zhao C (2014) Single segment of posterior lumbar interbody fusion for adult isthmic spondylolisthesis: reduction or fusion in situ. Eur Spine J 23:172–179. doi:10.1007/s00586-013-2858-6
Floman Y, Millgram MA, Ashkenazi E, Smorgick Y, Rand N (2008) Instrumented slip reduction and fusion for painful unstable isthmic spondylolisthesis in adults. J Spinal Disord Tech 21:477–483. doi:10.1097/BSD.0b013e31815b1abf
Audat ZM, Darwish FT, Al Barbarawi MM, Obaidat MM, Haddad WH, Bashaireh KM, Al-Aboosy IA (2011) Surgical management of low grade isthmic spondylolisthesis; a randomized controlled study of the surgical fixation with and without reduction. Scoliosis 6:14. doi:10.1186/1748-7161-6-14
Mehdian SM, Arun R, Jones A, Cole AA (2005) Reduction of severe adolescent isthmic spondylolisthesis: a new technique. Spine 30:E579–E584
Ruf M, Koch H, Melcher RP, Harms J (2006) Anatomic reduction and monosegmental fusion in high-grade developmental spondylolisthesis. Spine 31:269–274. doi:10.1097/01.brs.0000197204.91891.eb
Ekman P, Moller H, Tullberg T, Neumann P, Hedlund R (2007) Posterior lumbar interbody fusion versus posterolateral fusion in adult isthmic spondylolisthesis. Spine 32:2178–2183. doi:10.1097/BRS.0b013e31814b1bd8
Luo J, Cao K, Yu T, Li L, Huang S, Gong M, Cao C, Zou X (2015) Comparison of posterior lumbar interbody fusion versus posterolateral fusion for the treatment of isthmic spondylolithesis. J Spinal Disord Tech. doi:10.1097/BSD.0000000000000297
Feng Y, Chen L, Gu Y, Zhang ZM, Yang HL, Tang TS (2015) Restoration of the spinopelvic sagittal balance in isthmic spondylolisthesis: posterior lumbar interbody fusion may be better than posterolateral fusion. Spine J 15:1527–1535. doi:10.1016/j.spinee.2015.02.036
Cunningham JE, Elling EM, Milton AH, Robertson PA (2013) What is the optimum fusion technique for adult isthmic spondylolisthesis—PLIF or PLF? A long-term prospective cohort comparison study. J Spinal Disord Tech 26:260–267. doi:10.1097/BSD.0b013e3182417103
Suh KT, Park WW, Kim SJ, Cho HM, Lee JS, Lee JS (2008) Posterior lumbar interbody fusion for adult isthmic spondylolisthesis: a comparison of fusion with one or two cages. J Bone Jt Surg Br 90:1352–1356. doi:10.1302/0301-620X.90B10.21078
Okuda S, Miyauchi A, Oda T, Haku T, Yamamoto T, Iwasaki M (2006) Surgical complications of posterior lumbar interbody fusion with total facetectomy in 251 patients. J Neurosurg Spine 4:304–309. doi:10.3171/spi.2006.4.4.304
Taillard W (1954) Spondylolisthesis in children and adolescents. Acta Orthop Scand 24:115–144
HW M (1932) Spondylolisthesis. Can Med Assoc J 26:16–18
Cobb J (1948) The detection of beta-radiation by photographic film. Rev Sci Instrum 19:441–447
Kwon BK, Berta S, Daffner SD, Vaccaro AR, Hilibrand AS, Grauer JN, Beiner J, Albert TJ (2003) Radiographic analysis of transforaminal lumbar interbody fusion for the treatment of adult isthmic spondylolisthesis. J Spinal Disord Tech 16:469–476
Poussa M, Remes V, Lamberg T, Tervahartiala P, Schlenzka D, Yrjonen T, Osterman K, Seitsalo S, Helenius I (2006) Treatment of severe spondylolisthesis in adolescence with reduction or fusion in situ: long-term clinical, radiologic, and functional outcome. Spine 31:583–590. doi:10.1097/01.brs.0000201401.17944.f7 (discussion 591–582)
Cook JA, Hislop J, Altman DG, Fayers P, Briggs AH, Ramsay CR, Norrie JD, Harvey IM, Buckley B, Fergusson D, Ford I, Vale LD, group D (2015) Specifying the target difference in the primary outcome for a randomised controlled trial: guidance for researchers. Trials 16:12. doi:10.1186/s13063-014-0526-8
Ekman P, Moller H, Hedlund R (2005) The long-term effect of posterolateral fusion in adult isthmic spondylolisthesis: a randomized controlled study. Spine J 5:36–44. doi:10.1016/j.spinee.2004.05.249
Lian XF, Xu JG, Zeng BF, Liu XK, Li H, Qiu ML, Yang EZ (2014) Continuous irrigation and drainage for early postoperative deep wound infection after posterior instrumented spinal fusion. J Spinal Disord Tech 27:E315–E317. doi:10.1097/BSD.0000000000000122
de Loubresse CG, Bon T, Deburge A, Lassale B, Benoit M (1996) Posterolateral fusion for radicular pain in isthmic spondylolisthesis. Clin Orthop Relat Res 323:194–201
Sudo H, Oda I, Abumi K, Ito M, Kotani Y, Minami A (2006) Biomechanical study on the effect of five different lumbar reconstruction techniques on adjacent-level intradiscal pressure and lamina strain. J Neurosurg Spine 5:150–155. doi:10.3171/spi.2006.5.2.150
Liu X, Wang Y, Qiu G, Weng X, Yu B (2014) A systematic review with meta-analysis of posterior interbody fusion versus posterolateral fusion in lumbar spondylolisthesis. Eur spine J 23:43–56. doi:10.1007/s00586-013-2880-8
Grzegorzewski A, Kumar SJ (2000) In situ posterolateral spine arthrodesis for grades III, IV, and V spondylolisthesis in children and adolescents. J Pediatr Orthop 20:506–511
Spruit M, Pavlov PW, Leitao J, De Kleuver M, Anderson PG, Den Boer F (2002) Posterior reduction and anterior lumbar interbody fusion in symptomatic low-grade adult isthmic spondylolisthesis: short-term radiological and functional outcome. Eur Spine J 11:428–433. doi:10.1007/s00586-002-0400-3
Mehdian SH, Arun R (2011) A new three-stage spinal shortening procedure for reduction of severe adolescent isthmic spondylolisthesis: a case series with medium- to long-term follow-up. Spine 36:E705–E711. doi:10.1097/BRS.0b013e3182158c1f
Akamaru T, Kawahara N, Tim Yoon S, Minamide A, Su Kim K, Tomita K, Hutton WC (2003) Adjacent segment motion after a simulated lumbar fusion in different sagittal alignments: a biomechanical analysis. Spine 28:1560–1566
Shufflebarger HL, Geck MJ (2005) High-grade isthmic dysplastic spondylolisthesis: monosegmental surgical treatment. Spine 30:S42–S48
Harris BM, Hilibrand AS, Savas PE, Pellegrino A, Vaccaro AR, Siegler S, Albert TJ (2004) Transforaminal lumbar interbody fusion: the effect of various instrumentation techniques on the flexibility of the lumbar spine. Spine 29:E65–E70
Recnik G, Kosak R, Vengust R (2013) Influencing segmental balance in isthmic spondylolisthesis using transforaminal lumbar interbody fusion. J Spinal Disord Tech 26:246–251. doi:10.1097/BSD.0b013e3182416f5c
Chrastil J, Patel AA (2012) Complications associated with posterior and transforaminal lumbar interbody fusion. J Am Acad Orthop Surg 20:283–291. doi:10.5435/JAAOS-20-05-283
Cole CD, McCall TD, Schmidt MH, Dailey AT (2009) Comparison of low back fusion techniques: transforaminal lumbar interbody fusion (TLIF) or posterior lumbar interbody fusion (PLIF) approaches. Curr Rev Musculoskelet Med 2:118–126. doi:10.1007/s12178-009-9053-8
Liu J, Deng H, Long X, Chen X, Xu R, Liu Z (2015) A comparative study of perioperative complications between transforaminal versus posterior lumbar interbody fusion in degenerative lumbar spondylolisthesis. Eur Spine J. doi:10.1007/s00586-015-4086-8
Zhou J, Wang B, Dong J, Li X, Zhou X, Fang T, Lin H (2011) Instrumented transforaminal lumbar interbody fusion with single cage for the treatment of degenerative lumbar disease. Arch Orthop Trauma Surg 131:1239–1245. doi:10.1007/s00402-011-1292-7
Hackenberg L, Halm H, Bullmann V, Vieth V, Schneider M, Liljenqvist U (2005) Transforaminal lumbar interbody fusion: a safe technique with satisfactory three to five year results. Eur Spine Journal 14:551–558. doi:10.1007/s00586-004-0830-1
Acknowledgments
The authors thank Cameron Rawanduzy from Brain and Spine Center of Weill Cornell Medical College for his helpful discussion and contribution for this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No funds were received in support of this work. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Rights and permissions
About this article
Cite this article
Yang, EZ., Xu, JG., Liu, XK. et al. An RCT study comparing the clinical and radiological outcomes with the use of PLIF or TLIF after instrumented reduction in adult isthmic spondylolisthesis. Eur Spine J 25, 1587–1594 (2016). https://doi.org/10.1007/s00586-015-4341-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4341-z