Abstract
Purpose
To compare outcomes between transdiscal and conventional pedicle fixation for high-grade L5-S1 spondylolisthesis.
Methods
This was a retrospective case–control study with patients prospectively followed. Twenty-five consecutive patients with mean age of 36.7 years underwent transdiscal fixation, and 31 other with mean age of 42.0 years to pedicle fixation were clinically and radiographically compared. Clinical assessments were performed using Oswestry Disability Index (ODI), Core Outcomes Measures Index (COMI), Short-Form 12 (SF-12), and pain visual analog scale (VAS). Radiographic spinopelvic parameters were also evaluated. The mean follow-up was 2.7 years (range 2.0–5.3).
Results
Preoperative data were comparable between groups. Surgery time, blood loss, and hospital stay were similar between groups. At last follow-up, clinical and radiographic outcomes were significantly improved in both groups. Postoperatively, both lumbar and leg pain VAS were similar between groups, but ODI (20.2 vs. 31.6, p = 0.010), COMI (1.6 vs. 2.8, p = 0.012), and SF-12 physical (84.3 vs. 61.5, p = 0.004) and mental (81.5 vs. 69.4, p = 0.021) scores were significantly better in the transdiscal group. The neurologic complication rate was similar in both groups. There were 4 pseudoarthroses in the pedicle group, and none in the transdiscal group.
Conclusion
L5-S1 transdiscal screw fixation provided better functional and radiographic outcomes at medium-term than conventional pedicle fixation for high-grade spondylolisthesis, although transdiscal sacral screws are difficult to place in correct position.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
High-grade spondylolisthesis can be a debilitating condition for the patient and present a significant challenge for the surgeon [1]. Today, surgical stabilization of high-grade spondylolisthesis remains controversial. Several surgical techniques have been advocated to deal with symptomatic L5-S1 isthmic spondylolisthesis. Posterolateral fusion with pedicle screw fixation has become increasingly popular over the past years for treatment of spondylolisthesis [2], but it has been also associated with a relatively high rate of pseudoarthrosis and progressive slippage [1].
On the basis of pseudoarthrosis rate and biomechanical considerations [3], alternative L5-S1 transdiscal screwing has been considered. This technique [4] uses the concept of three-column fixation by means of a posterior approach, and the triangular construct potentially provides stability to the anterior column. Many case-series studies of lumbosacral fusion for spondylolisthesis have been reported, but only a few have focused on L5-S1 fixation with transdiscal screws [5–7], and only 2 of these had more than 20 patients [8, 9]. In addition, other studies had used transdiscal screwing associated with some other technique of fusion [10–13]. We have not found any study comparing the results between transdiscal and pedicle fixation.
According to the literature [7–9], in this study transdiscal fixation was defined as screw placement in the S1 pedicles, across the L5-S1 disc space, and penetrating into the L5 vertebral body. We hypothesized that the transdiscal fixation was mechanically stronger to resist L5-S1 slipping compared with pedicle fixation, regardless of the fixation level proximal to L5.
The objective of this study was to compare functional and radiographic outcomes between transdiscal and pedicle fixation in patients younger than 60 years with high-grade L5-S1 isthmic spondylolisthesis.
Materials and methods
Patient selection
A retrospective case–control study with patients prospectively followed was conducted to compare the outcomes between L5-S1 transdiscal fixation and conventional pedicle fixation for high-grade L5-S1 spondylolisthesis. The study was approved by our institutional ethical committee, and informed consent was required. All consecutive patients who underwent surgery for spondylolisthesis at our center between January 2007 and December 2012 were eligible for the study. Indications for surgery were chronic low back pain and/or radiating pain of the lower extremity, severity slippage and radiological findings of spondylolisthesis including sagittal balance. In that time, fusion for spondylolisthesis was always instrumented at our department by either using a conventional posterolateral fusion with pedicle screws fixation or stabilization with transdiscal screwing. According to their preferences, each of the two surgical teams at our department used only one of these techniques in that time. The inclusion criteria for this study were high-grade slippage (grade III or higher) [14], level of L5-S1, and age of 60 years or less. A minimum postoperative follow-up of 2 years was required for analysis of results in this study. The exclusion criteria were evidence of spinal stenosis or previous spine surgery. Patients were assigned to one of two study groups according the surgical technique performed, with the understanding that each technique was performed by just one of the teams.
The transdiscal group consisted of 25 patients, 7 male and 18 female with a mean age of 36.7 years (range 14–60). Before surgery, 15 of these patients had severe low back pain, and 8 had radiating leg pain. Eleven patients had muscular weakness, 1 motor deficit, 3 sensory deficit, and 2 sphincter incontinence. The pedicle group consisted of 31 patients, 15 male and 16 female with a mean age of 42.0 years (range 10–60). Before surgery, 18 of these patients had severe low back pain, and 11 had radiating leg pain. Nine patients had muscular weakness, 1 motor deficit, 4 sensory deficit, and 1 sphincter incontinence. Preoperative data were comparable between groups (Table 1). In the transdiscal group, there were 52 % of patients with grade IV-V preoperatively and 64 % in the pedicular group (p = 0.417).
Surgical procedure
A routine posterior midline approach was used in both groups. Partial reduction was only performed in those patients who had severe spinopelvic sagittal imbalance. Standard titanium screw systems were used in all patients, all similar but from several manufacturers (Transpine, Laffit, Spain; USS, Synthes, Zwitzerland; Colorado, Medtronic, France). The ratios of these systems were similar in both groups.
The technique of transdiscal lumbosacral fixation has previously been described [4, 6]. The sacral screws were placed in the S1 pedicle, through the endplate of S1, cross the disc space, and through the inferior endplate of L5 to terminate in the L5 body. The instrumented level was L4-S1 in 22 patients (88 %) and L5-S1 in 3 (12 %). In situ fusion was performed in 23 patients (92 %) and partial listhesis reduction via manipulation of the L5 body through implanted screws in 2 (8 %).
In the pedicle group, a standard pedicle screw fixation was performed. The instrumented level was L4-S1 in 23 patients (71 %) and L5-S1 in 8 (29 %). In situ fusion was performed in 25 patients (81 %) and partial reduction in 6 (19 %). Interbody fusion (L5-S1 cages) was used in 3 patients.
In both groups, decompression was performed and standard posterolateral fusion using the bone fragments removed during the surgical approach. In addition, autologous iliac crest bone graft and/or bone substitute (Actifuse, Baxter, USA) was used in 5 patients in transdiscal group and in 6 patients en pedicular group. Comparing both groups, level instrumentation rate (L4-5-S1 vs. L5-S1, p = 0.311) or reduction rate (partial vs. in situ, p = 0.276).were not significantly different.
Multimodal neuromonitoring techniques of sensory evoked potential, transcraneal electrical motor-evoked potentials and electromyography were used for all surgeries. Postoperative protocol was similar in both groups. All patients in both groups were braced with a lumbosacral orthosis for a three-month period after surgery.
Evaluations
At our institution, standardized prospective assessment was made pre- and postoperatively at 3, 6, 12, and at least 24 months after surgery. Additionally for this study, patients were also invited to perform new clinical and radiographic evaluations, and none refused. At last follow-up, all the patients were clinically assessed by two specially trained independent fellows who were not involved in the surgeries and did not know which type of lumbar fusion had been used.
Primary outcome measure in this study was the Oswestry Disability Index (ODI) score [15] from 0 to 100 points, with lower scores indicating less severe symptoms. Clinical assessment was also performed in each visit by the Core Outcomes Measures Index (COMI) [16], and Short-Form 12 (SF-12) [17]. COMI was ranged from 0 to 10 points, with lower scores indicating better outcome. SF-12 questionnaire included physical and mental components which were transformed to a 0–100 scale with higher scores indicating a better quality of life. Pain at the lower back and the leg were each measured separately with a visual analog scale (VAS) [18] from 0 (no pain) to 10 (maximal pain). Postoperative major complications were those that needed revision surgery or resulted in permanent neurological deficit.
Standard radiographic evaluation including standing anteroposterior, lateral, and oblique view was made preoperatively and in each follow-up. Computed tomography scan (CT) was made preoperatively and postoperatively at 6, 12 and 24 months. Magnetic resonance imaging was used when there was presence of neurological deficit. All radiographs and CT were assessed by independent observers not involved in the surgical procedure. Grading of slippage was assessed by the classification of Meyerding [14]. The slip angle (SA) was defined according to Dubousset (lumbosacral angle) [19]. Lumbar lordosis was assessed by Cobb’s method [20]. Spinopelvic parameters were obtained according to Duval-Beaupère criteria [21] including pelvic incidence angle (PI), pelvic tilt (PT), and sacral slope (SS). Both fusion and implant position were assessed by radiographs and CT scan. Successful radiographic outcome was defined as evidence of bone bridging with absence of radiolucent lines around the screws, or nonprogressive slippage.
Statistical analysis
Statistical analyses were conducted with IBM-SPSS 19.0 software (IBM-SPSS, Armonk, NY, USA).
The Chi-square test or nonparametric Mantel–Haenszel test was used to compare categorical data between groups. For continuous data, unpaired t test or Mann–Whitney U test was used. For comparison between pre- and postoperative data, the paired t test or Wilcoxon signed-rank test were used. Correlation was made by Pearson coefficient. A p value less than 0.05 was considered significant. Potential predictors in univariate analyses were used in a regression logistic analysis to determine their effects on the functional outcomes. The results were presented as Odds ratio (OR) with 95 % confidence interval (95 % CI).
A posteriori Cohen’s statistical power analysis was performed in relation to the postoperative ODI scores. Considering a clinically relevant difference [15] between groups of 10, standard deviation of 14, and a minimum sample size of 25 in each group, for an alpha error of 0.05 the study power was 81 %.
Results
The mean postoperative follow-up was 2.6 years (range 2.0–4.9) in the transdiscal group, and 2.9 years (range 2.0–5.3) in the pedicle group. The mean operating time, perioperative blood loss, and hospitalization stay were similar in both groups (Table 2). There were no significant differences between groups regarding the severity of spondylolisthesis (p = 0.417), instrumentation level (p = 0.311) or reduction rate (p = 0.276).
Clinical outcomes
Mean functional outcomes related to ODI, COMI, SF12, and VAS-pain improved significantly in both groups at last follow-up (p = 0.001). However, all the functional outcomes were significantly better in the transdiscal group than in pedicle group, except for VAS scores (Table 3).
In the transdiscal group, all patients had an ODI score of 44 or less at last follow-up. Fourteen patients (56 %) were able to return to their previous occupation, 2 (8 %) had some limitation, and 9 (36 %) were forced to change job. Two of the 6 patients who practiced a sport before the intervention were able to continue practicing. Previous leg weakness was recovered in all patients except 2, and the sensorial deficit was also recovered in all patients except in 2 other patients. Two other patients developed transitory L5 root irritation after surgery. One other patient with previous urinary incontinence, from which she recovered, postoperatively developed L4 partial neurologic deficit. In this patient, a broken rod was also observed but solid fusion was achieved at 1 year after surgery, resulting in moderate disability (ODI = 32).
In the pedicle group, 8 patients (25.8 %) had an ODI score of 50 or greater at last follow-up. Fifteen patients (48.3 %) were able to return to their previous occupation, 8 (25.8 %) had some limitation, 5 (16.1 %) changed their occupation, and 3 (9.6 %) could not return to work. Among the 10 patients who practiced a sport before the intervention, 5 were able to continue practicing. Previous leg weakness or sensory deficit was recovered in all patients except 2. Three other patients developed L5 partial neurologic deficit after surgery.
Analyzing only those patients with L4-S1 instrumentation level, there were significant differences between groups regarding to the functional outcomes such as ODI (p = 0.032), COMI (p = 0.019), SF12-physical (p = 0.007) and SF12-mental (p = 0.018). Logistic regression analysis showed that the level of instrumentation was not an independent predictor of functional outcomes in either transdiscal (OR = 0.31, 95 % CI 0.19–1.14, p = 0.542) and pedicular (OR = 0.43, 95 % CI 0.22–1.33, p = 0.628) group.
Radiographic results
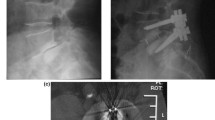
In the transdiscal group, all of patients had a radiographic fusion or nonprogressive slippage at last follow-up (Fig. 1), whereas in the pedicle group 4 patients (12.9 %) developed pseudoarthrosis (p = 0.123). Preoperatively (Table 4), there were no significant differences related to radiographic parameters between groups. Postoperatively (Table 4), in the pedicle group there were no significant changes in the PI or SS, but SA increased significantly (p = 0.001) and the PT decreased significantly (p = 0.008) at last follow-up. In the transdiscal group, all radiographic parameters were unchanged significant from preoperative to last follow-up.
Comparing both groups, the PI and SS did not differ significantly at last follow-up, but SA and PT tilt were significantly different (Table 4). In both groups, significant correlation between postoperative ODI and postoperative radiographic parameters (p > 0.302) was not found.
Complications and revisions
Complications are shown in Table 5. In the transdiscal group, 2 patients developed a deep wound infection treated with debridement and final moderate functional outcome (ODI = 32 and 44, respectively). Three patients had a poor orientation of the sacral screws without fusion consequences and good functional results (ODI = 10 and 16, respectively) in two of these (Fig. 2). The third patient was severely symptomatic due to a sacral screw misplacement that produced L5 radiculopathy, and this screw was subsequently removed, with moderate final result (ODI = 42). Breakage of a sacral screw was observed in a fourth patient at 3 postoperative years, although solid fusion was achieved and revision was not required (ODI = 17).
In the pedicle group, one patient had a dural tear which was repaired intraoperatively without residual sequelae (ODI = 20). Two patients developed superficial wound infections (ODI = 8 and 32, respectively). Another patient had breakage of both sacral and lumbar screws due to pseudoarthrosis, with poor functional outcome (ODI = 60). Three other patients had a pseudarthrosis. These 4 pseudoarthroses required surgical revision to transdiscal fixation with successful final outcomes.
Discussion
To our knowledge, this is the first clinical study to compare the outcomes of transdiscal and conventional pedicle fixation for patients younger than 60 years with high-grade L5-S1 isthmic spondylolisthesis. Management of this spondylolisthesis is variable. Posterolateral fusion with pedicle screw instrumentation has become increasingly popular over the past years. Successful results have been reported with this technique [2], but relatively high rates of pseudoarthrosis, neurologic dysfunction, and progressive slippage have also been observed [1]. In our study, there was a clinically relevant pseudoarthrosis rate in the pedicle group.
Transdiscal L5-S1 screw fixation [4] uses the concept of three-column fixation achieved from a single posterior approach. The direction of the sacral screws provides a triangular construct of screw-to-screw and screw-to L5 plate which potentially provides greater fixation strength [5]. All of this potentially improves the resistance against the shear forces across the disc space while posterolateral fusion is occurring [5, 6]. In a biomechanical analysis of cadaver models with spondylolisthesis [3], the authors found that the transdiscal L5–S1 screw fixation produced constructs that were 1.6–1.8 times stiffer than traditional pedicle screw fixation. In another study [8], the stiffness of the transdiscal fixation was found to be equivalent to fixation with a combined interbody fusion and pedicle screw fixation. On the other hand, transdiscal L5-S1 fixation could be considered difficult regarding positioning of the sacral screws. In our study, sacral screw misplacement was observed in 4 patients (16 %). Although they all had solid fusion, one patient had poor clinical result due to L5 radiculopathy.
Landi et al. [22] believed that the choice of treatment or to extend the fusion at L4-L5 for high-grade spondylolisthesis was related to a correct clinical and diagnostic planning, in particular the severity index and the standard measurements described in the literature. Reduction of the slipped vertebrae is still debatable, mainly due to the potential risk of L5 nerve injury [23, 24]. Several authors suggested that in situ fusion was better than reduction and fusion in high-grade spondylolisthesis with respect to long-term clinical outcome [24–26]. In our series, reduction was not performed in most patients, and partial reduction was carried out in patients who had severe spinopelvic sagittal imbalance. Other authors have obtained successful results using in situ fusion with transdiscal fixation [10–12]. Francois et al. [6] treated 4 patients according to the transdiscal technique with good clinical and fusion was noted in all patients. Boachie-Adjei et al. [5] used a technique of partial reduction and transdiscal fixation in 6 patients with high-grade spondylolisthesis followed a minimum of 2 years. They reported fusion in all patients which were able to resume their previous occupation. Rodriguez-Olaverri et al. [8] compared the outcomes of unilateral transforaminal lumbar interbody fusion (TLIF) with those of transdiscal screw fixation in high-grade spondylolisthesis. They found no significant differences in radiographic or clinical outcome in either group. Among 20 patients who were treated by transdiscal fixation, there was 1 pseudarthrosis and 1 implant failure, whereas in the TLIF group there was an increased risk of intraoperative complications. Logroscino et al. [7] compared 15 patients underwent L5-S1 pedicle instrumentation associated with transdiscal screw fixation, and 15 other underwent L5-S1 pedicle instrumentation associated with a posterolateral interbody fusion (PLIF). They observed that those patients treated with transdiscal had a faster resolution of the symptoms and a more rapid return to daily activities. In group transdiscal, one misplaced sacral screw was observed in a patients showing radicular leg pain which required revision surgery. Zagra et al. [9] treated 62 patients by posterolateral fusion with autologous bone graft and additional transdiscal screws followed 5 years. They reported successful clinical outcomes and fusion in all patients.
Novel variations of L5-S1 transdiscal fixation has been recently developed for treatment of high-grade spondylolisthesis. Wu et al. [27], in an in vitro and cadaveric investigation, established that it was feasible to perform a percutaneous posterior transdiscal screw fixation associated with an especially designed model of interbody cage. Shedid et al. [28] used also a novel minimally invasive procedure for high-grade spondylolisthesis using a L5-S1 transdiscal rod screw in 3 patients, and successful clinical and radiological outcomes was obtained in all patients at latest follow-up (range 13–18 months). Jouve et al. [29] in 8 patients performed a original technique of circumferential L5-S1 fusion by posterior-only approach using a transdiscal custom-made screw and corticocancellous bone grafts, and they obtained a solid fusion at a mean 6 postoperative months. In specific cases, when a postoperative sagittal malalignment is predictable with the lumbosacral fusion, the construct is extended to L4 using a classical posterior instrumented fusion.
This study has several limitations. The design was retrospective, although patients were prospectively followed. As in other previous studies, there was a relatively small sample size which was due to the relatively low prevalence of the condition. However, the results included all consecutive patients with no loss to follow-up. No homogeneous fixation systems were used due to the availability in the hospital, but they were similar and the surgeries were performed by two teams of surgeons with extensive experience in the spine. There was no standardization of the surgical techniques but both were performed according to standard medical practice. Postoperative follow-up was short, so it is recommended that these results be confirmed by future investigations on a higher number of patients and longer follow-up.
Conclusions
Transdiscal fixation results in improved functional outcomes compared with posterolateral fusion and pedicle fixation. Based on our results, we recommend transdiscal fixation for patients with high-grade L5-S1 spondylolisthesis, but the difficulty of placing the sacral screws should be also informed.
References
Boxall D, Bradford DS, Winter RB, Moe JH (1979) Management of severe spondylolisthesis in children and adolescents. J Bone Joint Surg Am 61:479–495
Lee GW, Lee SM, Ahn MW, Kim HJ, Yeom JS (2014) Comparison of posterolateral lumbar fusion and posterior lumbar interbody fusion for patients younger than 60 years with isthmic spondylolisthesis. Spine 39:1475–1480
Minamide A, Akamaru T, Yoon ST, Tamaki T, Rhee JM, Hutton WC (2003) Transdiscal L5-S1 screws for the fixation of isthmic spondylolisthesis: a biomechanical evaluation. J Spinal Disord Tech 16:144–149
Abdu WA, Wilber RG, Emery SE (1994) Pedicular transvertebral screw fixation of the lumbosacral spine in spondylolisthesis: a new technique for stabilization. Spine 19:710–715
Boachie-Adjei O, Do T, Rawlins BA (2002) Partial lumbosacral kyphosis reduction, decompression, and posterior lumbosacral transfixation in high-grade isthmic spondylolisthesis: clinical and radiographic results in six patients. Spine 27:161–168
Francois J, Lauweryns P, Fabry G (2005) Treatment of high-grade spondylolisthesis by posterior lumbosacral transfixation with transdiscal screws: surgical technique and preliminary results in four cases. Acta Orthop Belg 71:334–341
Logroscino CA, Tamburrelli FC, Scaramuzzo L, Schiro GR, Sessa S, Proietti L (2012) Transdiscal L5-S1 screws for the treatment of adult spondylolisthesis. Eur Spine J 21(Suppl 1):128–133
Rodriguez-Olaverri JC, Zimick NC, Merola A, Vicente J, Rodriguez J, Tabuenca A et al (2008) Comparing the clinical and radiological outcomes of pedicular transvertebral screw fixation of the lumbosacral spine in spondylolisthesis versus unilateral transforaminal lumbar interbody fusion (TLIF) with posterior fixation using anterior cages. Spine 33:1977–1981
Zagra A, Giudici F, Minoia L, Corriero AS, Zagra L (2009) Long-term results of pediculo-body fixation and posterolateral fusion for lumbar spondylolisthesis. Eur Spine J 18(Suppl 1):151–155
Grob D, Humke T, Dvorak J (1996) Direct pediculo-body fixation in cases of spondylolisthesis with advanced intervertebral disc degeneration. Eur Spine J 5:281–285
Bartolozzi P, Sandri A, Cassini M, Ricci M (2003) One-stage posterior decompression-stabilization and trans-sacral interbody fusion after partial reduction for severe L5-S1 spondylolisthesis. Spine 28:1135–1141
Smith JA, Deviren V, Berven S, Kleinstueck F, Bradford DS (2001) Clinical outcome of trans-sacral interbody fusion after partial reduction for high-grade L5–S1 spondylolisthesis. Spine 26:2227–2234
Lakshmanan P, Ahuja S, Lewis M, Howes J, Davies PR (2009) Transsacral screw fixation for high-grade spondylolisthesis. Spine J 9:1024–1029
Meyerding H (1932) Spondylolisthesis. Surg Gynecol Obstet 54:371–377
Fairbank J, Pynsent PB (2000) The oswestry disability index. Spine J 25:2940–2953
Deyo RA, Battie M, Beurskens AJHM, Bombardier C, Croft P, Koes B et al (1998) Outcome measures for low back pain research: a proposal for standardized use. Spine 23:2003–2013
Ware JE Jr, Kosinski M, Keller SD (1996) A 12-item short-form health survey: construction of scales and preliminary tests of reliability and validity. Med Care 34:220–233
Guyatt GH, Townsend M, Berman LB, Keller JL (1987) A comparison of Likert and visual analogue scales for measuring change in function. J Chron Dis 40:1129–1133
Dubousset J (1997) Treatment of spondylolysis and spondylolisthesis in children and adolescents. Clin Orthop Relat Res 337:77–85
Li Y, Hresko MT (2012) Radiographic analysis of spondylolisthesis and sagittal spinopelvic deformity. J Am Acad Orthop Surg 20:194–205
Duval-Beaupère G, Schmidt C, Cosson PH (1992) A barycentremetric study of the sagittal shape of spine and pelvis: the conditions required for an economic standing position. Ann Biomed Eng 20(4):451–462
Landi A, Marotta N, Mancarella C, Tarantino R, Delfini R (2013) Trans-sacral screw fixation in the treatment of high dyplastic developmental spondylolisthesis. World J Clin Cases 1:116–120
DeWald RL, FautMM Taddonio RF, Neuwirth MG (1981) Severe lumbosacral spondylolisthesis in adolescents and children. J Bone Joint Surg Am 63:619–626
Poussa M, Remes V, Lamberg T, Tervahartiala P, Schlenzka D, Yrjönen T et al (2006) Treatment of severe spondylolisthesis in adolescence with reduction or fusion in situ: long-term clinical, radiologic, and functional outcome. Spine 31:583–590
Lamartina C (2010) Posterior instrumentation, reduction and fusion in spondyloptosis. Eur Spine J 19:1799–1800
Transfeldt EE, Mehbod AA (2007) Evidence-based medicine analysis of isthmic spondylolisthesis treatment including reduction versus fusion in situ for high-grade slips. Spine 32(Suppl 1):126–129
Wu AM, Ni WF, Shao ZX, Kong XJ, Tian NF, Huang YX et al (2015) Percutaneous posterior transdiscal oblique screw fixation with lateral interbody fusion: a radiological and cadaveric study. Eur Spine J 4:852–858
Shedid D, Weil AG, Lieberman I (2014) A novel minimally invasive technique for the treatment of high-grade isthmic spondylolisthesis using a posterior transsacral rod. J Spinal Disord Tech 27:41–48
Jouve JL, Blondel B, Fuentes S, Choufani E, Pesenti S, Bollini G (2014) Circumferential fusion using a custom-made screw in the management of high-grade spondylolisthesis. Eur Spine J 23(Suppl 4):457–462
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Collados-Maestre, I., Lizaur-Utrilla, A., Bas-Hermida, T. et al. Transdiscal screw versus pedicle screw fixation for high-grade L5-S1 isthmic spondylolisthesis in patients younger than 60 years: a case–control study. Eur Spine J 25, 1806–1812 (2016). https://doi.org/10.1007/s00586-016-4550-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-016-4550-0