Abstract
Purpose
To conduct a retrospective multicenter study to investigate the accuracy of pedicle screw (PS) placement in the cervical spine by freehand technique and the related complications in various pathological conditions including trauma, rheumatoid arthritis, degenerative conditions and others.
Methods
283 patients with 1,065 PSs in the cervical spine who were treated at eight spine centers and finished postoperative CT scan were enrolled. The numbers of placed PSs were 608 for trauma, 180 for rheumatoid arthritis (RA), 199 for spondylosis, and 78 for others. Malposition grades on CT image in the axial plane were defined as grade 0 (G-0) correct placement, grade 1 (G-1): malposition by less than half screw diameter, grade 2 (G-2): malposition by more than half screw diameter. The direction of malposition was classified into four categories: medial, lateral, superior and inferior.
Results
Overall malposition rate was 14.8 % (9.6 % in G-1 and 5.3 % in G-2). The highest malposition rate was 26.7 % for RA, followed by 16.6 % for spondylosis, and 11.2 % for trauma. The malposition rate for RA was significantly higher than those for other pathologies. 79.7 % of the malpositioned screws were placed laterally. Though intraoperative vertebral artery injury was observed in two patients with RA, there were no serious complications during a minimal 2-year follow-up.
Conclusions
Malposition rate of PS placement in the cervical spine by freehand technique was high in rheumatoid patients even when being performed by experienced spine surgeons. Any guidance tools including navigation systems are recommended for placement of cervical PSs in patients with RA.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
There have been increasing reports of posterior instrumentation surgery with cervical pedicle screws (PSs) for reconstruction of the cervical spine with various pathologies [1–5]. Despite the biomechanical superiority of cervical PSs [6], placement of cervical PSs inherits considerable risks of injuries either to nerves or to vertebral artery. Abumi et al. [7] reported that 45 out of 669 inserted screws (6.7 %) were misplaced in his early series. Since then, numerous reports have been published regarding the malposition rates of cervical PSs. Neo et al. [8] reported that his malposition rate was 29 % in patients with degenerative conditions. Onishi et al. [9] reported a patient who had cerebral infarction due to brain embolism after placement of cervical PSs. In order to avoid such serious complications, there have been several attempts to improve the accuracy of cervical PS insertion using innovative techniques such as navigation systems [10, 11]. Since such high-tech navigation systems are expensive, there are limited numbers of hospitals using high-tech navigation systems, and freehand placement of CPSs under fluorography is still a popular technique for placing PSs in the cervical spine.
Previous reports regarding cervical PSs were from a single institute with a limited sample size and pathological condition [12, 13]. There is a significant need of a multicenter study with a large sample size and different pathological conditions to discern unbiased malposition rates of cervical PSs, and differences in risks of malposition and related complications among various pathological conditions in the cervical spine. The purpose of this study was to conduct a retrospective multicenter study to investigate the accuracy of cervical PS placement by freehand insertion technique and its related complications in various pathological conditions such as trauma, rheumatoid arthritis, degenerative conditions and others.
Materials and methods
Between April 2001 and April 2006, 1200 cervical PSs were inserted in 322 patients with freehand technique under lateral fluoroscopic guidance in eight spine centers in Hokkaido, Japan. These hospitals were referral spine centers in Hokkaido and eight experienced spine surgeons participated in this study. All surgeons involved in this study were board-certified spine surgeons of the Japanese Society for Spine Surgery and Related Research (JSSR) and their experience levels of PS fixation in the cervical spine were more than 100 patients in 2 surgeons, 50–99 patients in 3, and 20–49 patients in 3.
Out of the 322 patients, 283 patients with 1,065 cervical PSs who underwent postoperative CT scan were enrolled in this study. In this series, pedicle screw was the only anchor for fixation. Other anchoring methods such as lateral mass screws and laminar screws were not used in all the patients. The patients were classified into four groups according to the pathologic conditions; trauma, spondylosis, rheumatoid arthritis (RA) and others. All the patients had unstable conditions or deformities in the cervical spine, which were treated by surgical correction or fixation using pedicle screw instrumentation. There were 161 patients (608 PSs) with trauma, 63 (180 PSs) with RA, 39 (199 PSs) with cervical spondylotic myelopathy and/or radiculopathy and 20 with miscellaneous pathological conditions (78 PSs) (Table 1). The number of PSs placed at each spinal level was 148 in C2, 75 in C3, 135 in C4, 222 in C5, 284 in C6, and 201 in C7 (Tables 2, 3, 4, 5). Detailed information regarding the number of PSs placed in the cervical spinal levels and four different pathologic conditions is also listed in Tables 2, 3, 4, 5. Follow-up periods ranged from 24 to 100 months, with an average of 50. This study was approved by the Internal Review Board of Hokkaido University Hospital (No. 009-0230).
Pedicle screw insertion was done by freehand technique under the guidance of lateral fluoroscopy. With true lateral images of fluoroscopy of a patient placed prone with a Mayfield device, the leading surgeon stood at the top of the patient’s head and a starting hole for a PS was created with an automated diamond burr with a 2-mm head. When the cancellous channel of the pedicle was seen at the bottom of the hole, a probe specially designed for cervical pedicle screw placement was used to dig into the vertebral body through the pedicle. The depth of the probe tip was monitored by a true lateral view of fluoroscopy. A pedicle sounder with a small ball tip was used to check whether there was no breach into either the spinal canal or the vertebral foramen. After tapping was done, the created hole was checked again by a pedicle sounder and then a PS with a proper length and width was inserted. All the used implants were the CERVICAL pedicle screw system (Robert-Reid Inc., Tokyo, Japan). The sizes of the screws were 3.5 or 4.0 mm in diameter and 20–24 mm in length.
Postoperative CT images (2-mm slices in the axial plane) were taken in the patients within 2 weeks. CT images were evaluated by an independent spine surgeon who was a board-certified spine surgeon of JSSR and had not been involved in surgical treatment. Placement accuracy of CPS was evaluated in the axial CT images and classified into three grades; grade 0 (G-0): correct placement, grade 1 (G-1): malposition by less than half screw diameter, grade 2 (G-2): malposition by more than half screw diameter. Screw malposition at each spinal level was also classified into four categories according to the direction of malposition; medial, lateral, superior and inferior. Malposition rates of PSs were evaluated from C2 to C7 in different pathological conditions including trauma, rheumatoid arthritis, spondylosis and miscellaneous. Intraoperative and postoperative complications either related or unrelated to PS placement were also evaluated retrospectively.
Malposition rates both per screw and per patient were statistically analyzed between pathological conditions or spinal levels using the Tukey–Kramer test. Complication rates were also statistically analyzed between pathological conditions in the same way. P values less than 0.05 were regarded as statistically significant.
Results (Tables 2–6)
Overall accuracy of PS placement by freehand technique under lateral fluoroscopic guidance was 85.2 % (907/1,065 PSs) (Fig. 1). Overall malposition rate was 14.8 % (158/1,065 PSs); 9.6 % (102 PSs) in G-1 and 5.3 % (56 PSs) with G-2.
As to pathological conditions, the highest malposition rate was 26.7 % (48/180 PSs) in patients with RA; 12.8 % with G-1 (23/180 PSs), 13.9 % (25/180 PSs). The second highest malposition rate was 16.6 % (33/199 PSs) in those with spondylotic conditions; 10.6 % with G-1 (21/199 PSs), 6.0 % with G-2 (12/199 PSs). The lowest malposition rate was 11.2 % in those with trauma (68/608 PSs); 8.7 % with G-1 (53/608 PSs), 2.5 % with G-2 (15/608 PSs). Malposition rate in patients with RA was significantly higher than those of trauma (P < 0.05) and spondylosis (P < 0.05).
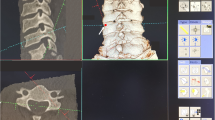
A 61-year-old male with cervical myelopathy and cervical kyphosis caused by spondylosis underwent simultaneous posterior decompression and correction with CPSs at C2-6. a Preoperative lateral X-ray film shows cervical kyphosis with 35 degrees. Postoperative AP (b) and lateral (c) X-ray films show correction of kyphosis after C2-6 posterior fusion. Axial images at C4 (d) and C5 (e) of postoperative CT images show that CPSs were placed appropriately in the cervical pedicles
As to the relationship between pedicle levels and malposition rates, malposition rates were 23.0 % (34/148 PSs) in C2, 17.3 % (13/75 PSs) in C3, 16.3 % (22/135 PSs) in C4, 15.8 % (35/222 PSs) in C5, 11.3 % (32/284 PSs) in C6 and 10.9 % (22/201 PSs) in C7. Statistically significant difference was observed between C2 and C6 (P < 0.05) and between C2 and C7 (P < 0.05). Overall malposition rate at C3-6 was 14.2 % (102/716PSs), which did not show statistically significant difference from C2 to C7.
As to the malposition rate per patient, the probability of malposition in each patient was 46 % in RA, 41 % in spondylosis, 15 % in miscellaneous and 13 % in trauma. Statistically significant difference was observed between RA and trauma, spondylosis and trauma, and miscellaneous and RA (P < 0.05).
As to the direction of screw malposition, 79.7 % (126/158 PSs) of the malpositioned screws were laterally placed, 19.0 % (30/158 PSs) medially placed, 1.3 % (2/158 PSs) superiorly placed. There was no screw placed inferiorly.
Surgery-related complications were seen in 30 patients (10.6 %); intraoperative vertebral artery injury in two patients with RA [arterial bleeding from a tapping hole was treated by bone wax and a PS was not inserted in one patient; the other was treated by bone wax and a PS was placed in the end (Fig. 2)], loosening of PSs in 8 patients (RA in 5 patients, spondylosis in 1, trauma in 1, metastasis in 1), nerve root irritation by PS in 3 which was recovered by removal of screws, postoperative infection in 5, postoperative C5 nerve root palsy in 3 without any relation to PSs, CSF leak in 4, adjacent segment disease needing additional fusion in 3 with RA, and hematoma needing surgical removal in 2 with trauma. Two patients out of three with postoperative C5 tardy palsy required additional foraminotomy within 2 weeks after surgery. As to the complication rates according to pathological conditions, the highest complication rate was 19.0 % (12/63 patients) in RA, 12.8 % (5/39 patients) in those with spondylosis and 3.1 % (5/161 patients) in those with trauma. The complication rate of RA was significantly higher than trauma (P < 0.05). One rheumatoid patient who had intraoperative VA injury showed mild dizziness after surgery for several days, but her dizziness disappeared during follow-up (Fig. 2). There were no surgery-related deaths, major complications related to VA injury, or cerebral infraction caused by malpositioned PSs during follow-up periods.
A 63-year-old female patient with atlanto-axial subluxation (AAS) due to rheumatoid arthritis underwent occiput-C2 posterior fusion. Vertebral artery was damaged during tapping at C2 on the right side. The surgeon put bone wax into the screw hole and inserted a PS afterward. a Preoperative lateral X-ray film shows AAS. Preoperative CT angiography in the axial plane (b) at C3 and the coronal plane show (c) that the both VAs are intact with dominancy of the right VA. d Postoperative lateral X-ray film shows reduction of AAS after occiput-C2 fusion. Postoperative CT angiogram and the axial plane (e) show that the right pedicle screw was misplaced laterally to the transverse foramen at C2 and obstructed VA. The right VA at C3 was not observed, and the left one became bigger than before surgery (f). g Postoperative CT angiogram in the coronal plane shows that blood flow above the C2 was seen on the both sides (white arrows)
Discussion
Due to the biomechanical superiority of the PS system in spinal reconstruction surgery, it has been used for patients with cervical deformities or unstable pathological conditions such as acute traumatic lesions, subaxial lesions of RA, destructive spondyloarthropathy due to long-term hemodialysis and tumor metastasis to the cervical spine [1–5]. Recent clinical applications of the PS system include correction of kyphotic deformity in the cervical spine and occipitocervical reconstruction to correct malalignment in the craniocervical junction caused by various pathological conditions [14]. Despite its increasing popularity for cervical reconstruction surgery, malposition of PSs has a potential risk of injuries to both vertebral artery and nerves, which is a significant clinical concern and has been intensively discussed among experts for years. Reported malposition rates of PSs under freehand technique varied from 6.9 to 29 % [7, 8]. There has been little information, however, regarding the differences in malposition rates of PSs between different pathological conditions operated on by experienced spine surgeons who are familiar with placement of PSs in the cervical spine [12, 13].
Eight surgeons involved in this study had experienced placing PSs in the cervical spine for more than 20 patients. The most senior surgeon had trained the other seven surgeons. Therefore, as to the accuracy of freehand technique under lateral fluoroscopy guidance, the present study shows the most reliable data regarding the real placement accuracy of PSs in the cervical spine by experienced spine surgeons with the same surgical technique. Although the overall misplacement rate of PS in the present study was 14.8 %, there were large variations in rates of screw malposition among different pathologies and pedicle levels. The highest screw misplacement rate was observed in those with RA and the lowest in those with trauma. The highest misplacement rate in RA may derive from the difficulty in finding the entry points of screws due to destructive changes in the posterior elements of the cervical spine and severe bone fragility [15]. Although C2 and C7 were reported to be safe and easy for pedicle screw placement, the malposition rate at C2 in RA was 28.3 % in our series. This result suggests that the use of any guiding tools is recommended while placing PSs, especially in patients with RA even at C2 level. In cases with spondylosis, sclerotic changes around the pedicles may lead surgeons to misplace PSs. The main reason for the lowest malposition rate in trauma patients may be that PSs were inserted into the intact normal pedicles without fractures away from the levels of injury. In addition, precise preoperative planning based on multiplanar CT images is indispensable in each patient for safe placement of cervical pedicle screws by assessing the three-dimensional anatomy of each cervical pedicle and abnormal running of the vertebral artery.
In terms of the learning curve for placement of PS in the cervical spine, Yoshimoto et al. [16] reported that significant improvement in accuracy of placement PSs was observed in the later period after placing 192 PSs. Gonzalvo et al. [17] reported that the accuracy of placement showed significant improvement after placing 80 PSs. They concluded that inexperienced surgeons should perform PS fixation independently only after placement of 80 screws (25 patients) with the assistance of an experienced senior surgeon to avoid serious complications. In the present study, most surgeons had experienced placement of PS more than 25 patients. Despite their surgical experience, some pathologies and spinal levels showed high malposition rates exceeding 20 %. This result implies that even experienced spine surgeons need more meticulous preoperative planning or any available guidance tools such as navigation systems for accurate placement of CPSs in some difficult pathologies including RA.
There have been many attempts to improve accuracy of PS placement in the cervical spine. Yukawa et al. [18, 19] reported the use of multiplanar fluoroscopy tilted to pedicle axis to find out the ideal entry point of and orientation of a pedicle screw. Once fluoroscopy depicted the approximate circle of pedicle cortex wall, the center of a cortical circle in the image intensifier indicates the screw insertion point and X-ray trajectory indicates the orientation of the pedicle screw. After creating the entry hole by an awl, a blunt-tipped pedicle probe is inserted into the pedicle cavity and placement of a guide wire follows under fluoroscopic visualization in lateral and pedicle axis views. The incidence of screw malposition by this method was reportedly 4.0 %. Another attempt was reported by Ryken et al. [20] to use image-based templates. Templates were created by preoperative volumetric CT scans and computer software. Up to the present, other types of templates for placement of PSs have also been introduced.
Recently there has been an increasing number of studies using computer-assisted placement of PSs in the cervical spine. Kim et al. [21] and Ludwig et al. [22] conducted a comparative study of computer-assisted placement of cervical PSs and original fluoroscopy-assisted placement in laboratory settings almost 10 years ago. Their reported malposition rates were around 10 % at the early stage of development of computer-assisted spinal surgery. By virtue of technical development, Richter et al. [23] and Rath et al. [24] used VectorVison® (Brain Lab AG, Heimstetten, Germany) for the placement of cervical PSs at C3-6 and reported that this system led to a significantly reduced misplacement rates. Ito et al. [11] reported their experience using a 3D fluoroscopy navigation system (Siremobil Iso-C3D, Siemens Medical Solutions USA, Inc.) and computer navigation by the Stealth Station (Medtronic Surgical Navigation Technologies). Their results showed that 97.2 % of the inserted pedicle screws out of 176 screws were placed correctly, and only 2.8 % were classified as grade 2 (screw perforation of the cortex by up to 2 mm). By the use of high-tech navigation systems, the accuracy of placement of cervical PSs has been dramatically improved. Despite its advantages, the cost of navigation systems is extremely high and image quality of these high-tech devices is sometimes suboptimal, especially in obese or osteoporotic patients.
In the present study, almost 80 % of malpositioned screws were placed laterally to penetrate into the transverse foramens. The main factors for laterally misplaced screws are: (1) the lateral wall of the pedicle is mechanically weaker than the medial wall of it [25], (2) the trajectories of cervical PSs are around 40° oblique, which is often disturbed by the surrounding paravertebral muscles and the distal screw heads tend to go medially with screw tips going laterally. Oblique trajectory of CPS through posterior midline approach can be hindered by the cervical paravertebral muscles so that percutaneous placement of CPS would be a choice to avoid such an effect from the paravertebral muscles [23]. Surgeons should be aware of these facts before placing PSs in the cervical spine.
Regarding surgery-related complications, Kast et al. [26] found that 9 % of placed cervical PSs had a critical breach and 3 % caused temporary paresis or a sensory loss. Another serious complication is cerebral infarction due to an embolism related to malpositioned PSs [9]. Onishi et al. reported that the left C4 PS was proven to breach the transverse foramen, and an angiogram showed a thrombus cranial to the C4 PS. After anticoagulation therapy for 2 weeks, the thrombus disappeared and subsequent screw removal was conducted. At the final follow-up, the patient showed significant neural deficits such as a grade 4/5 hemiparesis, facial nerve palsy, and hearing loss in his left ear. In the present case series, it was fortunate not to experience such serious complications related to VA injury or occlusion by PSs even though two rheumatoid patients had intraoperative VA injury. Longer follow-up is needed to assess future complications related to malpositioned screws.
The limitations of this study were as follows: (1) there are wide variations in the number of patients in different pathological conditions and spinal levels where PSs were inserted; (2) there are variations among hospitals or surgeons in terms of the number of patients in specific pathologic condition treated; (3) there was no consensus among the surgeons when to put PS or not to put PS according to the size and shape of each pedicle. In some patients with RA, PSs were placed in the pedicles whose diameter was much smaller than that of a screw (the right pedicle of C2 in Fig. 2); (4) due to the nature of a retrospective multicenter clinical study, the use of preoperative assessment of pedicle size and location of vertebral artery using CT axial images were not consistent among eight spine centers at the time of survey; (5) the present study did not conduct any further imaging studies as to the relationship between the malpositioned screws and blood flow of the VA distal to the malpositioned screws.
Besides a biomechanical advantage of CPS, another benefit of PSs over other fixation techniques is that CPS can be used even for patients who do not have either the laminae after extensive laminectomy or medial part of the lateral masses in the fixation levels after severely comminuted fractures at the posterior element. Especially for those with severe cervical cord injury needing tracheotomy and a long-term use of ventilator, any procedures which can eliminate anterior reconstruction with instrumentation are beneficial to prevent post-surgical infection around a ventilation tube. Based on the present high malposition rates of CPS by a freehand technique, the authors do not recommend a freehand CPS placement as a routine technique for cervical spine reconstruction. However, by precise preoperative planning with multiplanar three-dimensional CT images and under any guidance tools such as navigation systems, which can enhance accuracy of CPS placement, CPS can be optional in particular destructive pathologies in the cervical spine.
Conclusion
Cervical PS placement by freehand technique under lateral fluoroscopic guidance had a high malposition rate in patients with RA (26.8 %): 12.8 % in grade 1 and 13.9 % in grade 2. Malposition rate in the spondylotic condition was less than rheumatoid patients (16.6 %): 10.6 % in grade 1 and 6.0 % in grade 2. Trauma cases showed the least malposition rate (11.2 %): 8.7 % in grade 1 and 2.5 % in grade 2. Even after surgeons became familiar with placement of cervical PSs, it is safer to use any guiding devices or systems for more accurate placement of cervical PSs, especially in those with RA or severe spondylotic changes.
References
Abumi K, Ito H, Taneichi H, Kaneda K (1994) Transpedicular screw fixation for traumatic lesions of the middle and lower cervical spine. Description of the techniques and preliminary report. J Spinal Disord 7:19–28
Abumi K, Takada T, Shono Y, Kaneda K, Fujiya M (1999) Posterior occipitocervical reconstruction using cervical pedicle screws and plate-rod systems. Spine 24:1425–1434
Sudo H, Ito M, Abumi K, Kotani Y, Takeuchi T, Yasui K, Minami A (2006) Long-term follow up of surgical outcomes in patients with cervical disorders undergoing hemodialysis. J Neurosurg Spine 5:313–319
Oda I, Abumi K, Ito M, Kotani Y, Oya T, Hasegawa K, Minami A (2006) Palliative spinal reconstruction using cervical pedicle screws for metastatic lesions of the spine: a retrospective analysis of 32 cases. Spine 31:1439–1444
Hasegawa K, Hirano T, Shimoda H, Homma T, Morita O (2008) Indications for cervical pedicle screw instrumentation in nontraumatic lesions. Spine 33:2284–2289
Kothe R, Rüther W, Schneider E, Linke B (2004) Biomechanical analysis of transpedicular screw fixation in the subaxial cervical spine. Spine 29:1869–1875
Abumi K, Shono Y, Ito M, Taneichi T, Kotani Y, Kaneda K (2000) Complication of pedicle screw fixation in reconstructive surgery of the cervical spine. Spine 25:962–969
Neo M, Sakamoto T, Fujibayashi S, Nakamura T (2005) The clinical risk of vertebral artery injury from cervical pedicle screws inserted in degenerative vertebrae. Spine 30:2800–2805
Onishi E, Sekimoto Y, Fukumitsu R, Yamagata S, Matsushita M (2010) Cerebral infraction due to an embolism after cervical pedicle screw fixation. Spine 35:E63–E66
Ishikawa Y, Kanemura T, Yoshida G, Matsumoto A, Ito Z, Tauchi R, Muramoto A, Ohno S, Nishimura Y (2011) Intraoperative, full-rotation, three-dimensional image (O-arm)-based navigation system for cervical pedicle screw insertion. J Neurosurg Spine 15:472–478
Ito Y, Sugimoto Y, Tomioka M, Hasegawa Y, Nakago K, Yagata Y (2008) Clinical accuracy of 3D fluoroscopy-assisted cervical pedicle screw insertion. J Neurosurg Spine 9:450–453
Nakashima H, Yukawa Y, Imagama S, Kanemura T, Kamiya M, Yanase M, Ito K, Machino M, Yoshida G, Ishikawa Y, Matsuyama Y, Ishiguro N, Kato F (2012) Complications of cervical pedicle screw fixation for nontraumatic lesions: a multicenter study of 84 patients. J Neurosurg Spine 16:238–247
Kosmopoulous V, Schizas C (2007) Pedicle screw placement accuracy: a meta-analysis. Spine 32:E111–E120
Hojo Y, Ito M, Abumi K, Kotani Y, Sudo H, Takahata M, Minami A (2011) A late neurological complication following posterior correction surgery of severe cervical kyphosis. Eur Spine J 20:890–898
Miyata M, Neo M, Ito H, Yoshida M, Fujibashi S, Nakamura T (2008) Rheumatoid arthritis as a risk factor for a narrow C-2 pedicle: 3D analysis of the C2 pedicle screw trajectory. J Neurosurg Spine 9:17–21
Yoshimoto H, Sato S, Hyakumachi T, Yanagibashi Y, Kanno T, Masuda T (2009) Clinical accuracy of cervical pedicle screw insertion using lateral fluoroscopy: a radiographic analysis of the learning curve. Eur Spine J 18:1326–1334
Gonzalvo A, Fitt G, Liew S, de la Harpe D, Turner P, Ton L, Rogers MA, Wilde PH (2009) The learning curve of pedicle screw placement; how many screws are enough? Spine 34:E761–E765
Yukawa Y, Kato F, Yoshihara H, Yanase M, Ito K (2006) Cervical pedicle screw fixation in 100 cases of unstable cervical injuries: pedicle axis views obtained using fluoroscopy. J Neurosurg Spine 5:488–493
Yukawa Y, Kato F, Ito K, Horie Y, Hida T, Nakashima H, Machino M (2009) Placement and complications of cervical pedicle screws in 144 cervical trauma patients using pedicle axis view techniques by fluoroscope. Eur Spine J 18:1293–1299
Ryken TC, Owen BD, Christensen GE, Reinhardt JM (2009) Image-based drill templates for cervical pedicle screw placement. J Neurosurg Spine 10:21–26
Kim HS, Heller JG, Hudgins PA, Fountain JA (2003) The accuracy of computed tomography in assessing cervical pedicle screw placement. Spine 28:2441–2446
Ludwig SC, Kowalski JM, Edwards CC II, Heller JG (2000) Cervical pedicle screws: comparative accuracy of two insertion techniques. Spine 25:2675–2681
Richter M, Cakir B, Schmidt R (2005) Cervical pedicle screws: conventional versus computer-assisted placement of cannulated screws. Spine 30:2280–2287
Rath SA, Moszko S, Schäffner PM, Cantone G, Braun V, Richter HP, Antoniadis G (2008) Accuracy of pedicle screw insertion in the cervical spine for internal fixation using frameless stereotactic guidance. J Neurosurg Spine 8:234–245
Shin EK, Panjabi MM, Chen NC, Wang JL (2000) The anatomic variability of human cervical pedicles: consideration for transpedicular screw fixation in the middle and lower cervical spine. Eur Spine J 9:61–66
Kast E, Mohr K, Richter HP, Börm W (2006) Complications of transpedicular screw fixation in the cervical spine. Eur Spine J 15:327–334
Acknowledgement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000(5). Informed consent was obtained from all patients for being included in the study. The authors thank Hitoshi Haba, MD, Takashi Ishida, MD, Keigo Yasui, MD, and Tatsuto Takeuchi, MD, for their support in data collection. Also thanks to Mr. Mason Mark for his support in English language editing.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hojo, Y., Ito, M., Suda, K. et al. A multicenter study on accuracy and complications of freehand placement of cervical pedicle screws under lateral fluoroscopy in different pathological conditions: CT-based evaluation of more than 1,000 screws. Eur Spine J 23, 2166–2174 (2014). https://doi.org/10.1007/s00586-014-3470-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3470-0