Abstract
Purpose
Cell therapy would be favorably performed immediately after nucleotomy, to restore intervertebral disc functionality and to slow down disc degeneration. Promising results were reported from small animal models but remaining problems, especially in larger animals, include loss of vital cells due to annular damage at the injection site and detrimental intradiscal conditions. The aim of the present study was to optimize cell-based disc therapy using a new albumin–hyaluronan hydrogel together with bone marrow-derived mesenchymal stem cells in a large porcine disc model.
Methods
Luciferase cell labeling was evaluated to follow-up stem cells metabolically up to 7 days in 3D cell cultures mimicking the harsh disc environment with low oxygen and glucose concentrations. As a pilot in vivo study, the implant was injected into porcine discs after removal of ~10 % of nucleus volume and animals were killed immediately after surgery (n = 6) and 3 days later (n = 6). 24 discs were analyzed. Implant persistence and cell activity (luciferase + WST assay) were observed simultaneously.
Results
In vitro cell culture with reduction of glucose (20, 5, 0.5, 0 mM) and oxygen (21, 5, 2 %) significantly decreased metabolic cell activity and luciferase activity after 3 days, with no recovery and a further decrease after 7 days, establishing luciferase activity as a metabolic sensor. During 3 days of 3D culture with disc-like conditions, luciferase activity decreased to 8 %. In vivo, initial implant volume shrank to 61 % at day 3 with evidence for hydrogel compression. Luciferase activity in vivo at day 3 was 2 % without referencing but 23 % after referencing to in vitro cell adaptation, and 38 % after additional consideration of detected implant volume loss.
Conclusion
In vitro analysis up to 7 days established for the first time luciferase activity as a metabolic sensor for mesenchymal stem cells used in regenerative disc therapy. Under the present protocol, short-term in vivo analysis after 3 days suggests improved implant retainment inside the disc and persistence of metabolically active cells; however, further studies will have to prove long-term in vivo outcome.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Disc degeneration is considered a major cause for disc prolapse incidents and of low back pain, the latter summarized as degenerative disc disease (DDD). Detailed biochemical, anatomical, radiological, and biomechanical changes associated with DDD are described but the complex pathophysiological pattern, especially with regard to what causes low back pain is still poorly understood [1–16]. Several reasons for the development of DDD are discussed including disc loading, disc injury, post-nucleotomy syndrome, and genetic predisposition [17–20].
Lumbar discectomy or nucleotomy are frequently performed procedures to treat nucleus pulposus herniations with neurological symptoms due to compression of neural structures [19]. However, these procedures often cause additional annular damage and can result in exacerbation of DDD [19–24]. Consequently, it would be desirable to apply cell therapy to the disc immediately during nucleotomy procedures to avoid progressive DDD in intervertebral discs (IVD) with beginning or moderate disc degeneration but preserved disc integrity. However, such early approaches to humans are not yet routinely used, due to remaining concerns about safety and biological potency.
Biological treatment options have been proposed to revitalize IVDs for decades. Cell therapy approaches to the disc include transplantation of autologous bone marrow derived or adipose stem cells on the one hand and the use of culture-expanded, autologous, disc-derived cells with first clinical results [25] on the other. Promising results were reported from smaller animal models with rather small discs offering a higher regenerative potential due to better disc nutrition caused by shorter diffusion distances as well as lower biomechanical forces due to lower body weights [26–32]. Outcome in larger animal models with biomechanical properties closer to human beings is more heterogeneous in the literature with evidence for considerable remaining problems [33–35]. Recently, a new method to follow-up implanted bone marrow-derived porcine mesenchymal stem cells (pMSCs) was introduced in a large porcine nucleotomy model with biomechanical properties close to human beings [34]. Al2O3 particles were added to a cell-seeded fibrin hydrogel and hence implant persistence could be visualized and quantitatively measured by µCT analysis. Cell retention was measured simultaneously using pre-labeled cells which carried a luciferase transgene, but quantification of luciferase enzyme activity was technically limited due to high implant loss caused by annular damage at the nucleotomy and cell insertion site with more than 90 % implant loss within 3 days after cell transfer.
Therefore, the aim of the present study was to establish luciferase cell labeling in vitro up to 7 days for quantification of metabolic cell activity and to re-evaluate stem cell-based regenerative disc therapy in partially nucleotomized discs in the large porcine nucleotomy model. In vivo analysis was done in a pilot study with 3-day follow-up after optimization of the implantation technique and use of a new albumin-based, hyaluronan-enriched hydrogel matrix, which was developed for better retention inside the disc through a cross-linking reaction [36–38]. To judge whether luciferase activity is a valid quantitative measure for follow-up of genetically pre-labeled cells under IVD-like conditions, the value of luciferase labeling was further investigated. Therefore, retrovirally transduced luciferase expressing pMSCs were analyzed under 3D culture conditions with gradually decreasing glucose and oxygen supply, thus mimicking the harsh intervertebral disc environment with low oxygen and glucose concentrations.
Materials and methods
Cell isolation, cultivation, and retroviral gene transfer
Autologous pMSCs were isolated from fresh bone marrow samples, from the proximal tibiae [34]. Briefly, cells were washed with PBS, seeded in culture flasks and maintained at 37 °C in a humidified atmosphere and 6 % CO2 in expansion medium (DMEM high glucose w/o l-glutamine, 12.5 % fetal calf serum, 2 mM l-glutamine, 1 % nonessential amino acids, 0.1 % beta-mercaptoethanol (all from Gibco, Life technologies, Darmstadt, Germany), 100 units/mL penicillin, and 100 mg/mL streptomycin, supplemented with 4 ng/mL basic fibroblast growth factor (Active Bioscience, Hamburg, Germany). Beta-mercaptoethanol was used to reduce the oxidative pressure by increased glutathione synthesis. It is part of an expansion medium composition, which has been adopted from common embryonic stem cell culture protocols and was found to be most effective to support proliferation and differentiation of pMSC. After 24–48 h, cultures were washed with phosphate-buffered saline (PBS) to remove non-adherent material. During expansion, medium was replaced twice a week. Cells were used after 2–6 passages.
Recombinant retrovirus encoding the firefly luciferase gene (Rv-Luc) was used as described before [34] to follow-up pMSCs after injection into IVDs. Briefly, cells were seeded and were incubated on the following day with 30 µL/cm2 medium containing the Rv-Luc at 5 multiplicity of infection (MOI) and 8 µg/mL polybrene for 2 h at 37 °C. Fresh medium was supplemented afterward. Five days after primary infection, the process was repeated to enhance transduction efficiency. Cells were grown to confluence. During expansion of pMSC-Luc, medium was replaced twice a week. After harvest, pMSC-Luc was stored in the gas phase above liquid nitrogen. After thawing, cells were cultured for one additional passage prior to use.
In vitro analysis under low oxygen and low glucose conditions
3D pellets consisting of 5 × 105 expanded Rv-Luc transduced cells were formed by centrifugation in 1.5 mL tubes and mixing with 25 µL of fibrinogen/PBS solution (35–55 mg/mL, Tissucol Duo S, Baxter, Unterschleissheim, Germany) and 25 µL thrombin/PBS solution (10 IU Thrombin/mL, Tissucol Duo S, Baxter, Unterschleissheim, Germany). 3D pellets were cultured in chondrogenic medium (DMEM w/o glucose with 0.1 µM dexamethasone, 0.17 mM ascorbic acid-2-phosphate, 5 µg/mL insulin, 5 µg/mL transferrin, 5 ng/mL selenous acid, 1 mM sodium pyruvate, 0.35 mM proline, 1.25 mg/mL BSA, 100 units/mL penicillin, 100 µg/mL streptomycin and 10 ng/mL TGF-β1 (Peprotech, Hamburg, Germany) and 10 ng/mL BMP-6 (R&D Systems, USA). For modulation of glucose concentrations, chondrogenic medium was supplemented with 20, 5, 0.5 mM, or no glucose for up to 7 days. For cultivating cells under low oxygen tension, chondrogenic medium supplemented with 20 mM glucose was used and 2, 5, or 21 % oxygen was supplied for up to 7 days in a special incubator.
WST assay
To get further information about pMSC activity and metabolism, a WST assay was performed measuring mitochondrial activity of viable cells. Therefore, 2.5 × 105 cells per well were directly plated in 6-well plates (monolayer culture) or were incorporated into 3D pellets as described above. Monolayer cultures received expansion medium and 3D pellets were incubated in chondrogenic medium supplemented either with 20 or 0.5 mM glucose. Those pellets receiving chondrogenic medium with low glucose concentration were additionally incubated at low oxygen tension with oxygen <2 %. For the assay, medium was replaced by 1.8 mL medium plus 0.2 mL Cell Proliferation Reagent (WST-1) (Roche Diagnostics, Mannheim, Germany). After 30 min, 0.2 mL of each culture supernatant was collected and the absorbance was determined at 450 nm. For measurement at day 0, cells of the monolayer culture group were allowed to adhere for 2 h after initial plating prior to assay start. Corresponding luciferase activity was determined as described below from parallel cultivated wells or pellets, respectively.
Luciferase assay
Luciferase activity was measured as described before [34]. In summary, in vitro 3D pellets were rinsed in PBS and lysed with 100 µL 1× lysis buffer per 500,000 cells. Nuclei pulposi from the in vivo study and corresponding in vitro hydrogel reference pellets (see below) were pulverized in a freezer mill and homogenized in 1 mL lysis buffer. Lysates were stirred at 800 rpm in a thermomixer for 30 min at 21 °C and centrifuged at 12,000 rpm for 30 s to pellet debris. Ten microliters of lysate was mixed with 50 µL luciferase assay reagent (Luciferin, Mg2+, ATP and coenzyme A), and the light emitted within 5 s at 25 °C was detected with an ELISA reader (Wallac Victor2 1420 Multilabel Counter, Wallac, Finland).
Preparation of injectable cell hydrogel
3.3 × 106 cells were suspended in 50 µL DMEM supplemented with 0.5 mM glucose, 100 units/mL penicillin, and 100 µg/mL streptomycin. Then, 100 mg of Al2O3 powder consisting of 10 µm sized particles (Degussit, Friatec, Mannheim, Germany) and 1 mL of hyaluronan-enhanced albumin hydrogel (TETEC AG, Reutlingen, Germany) [36–38] were added. Rheological measurements of the visco-elastic properties of the hydrogel had been performed earlier with a Kinexus Pro rheometer (Malvern Instruments GmbH, Herrenberg, Germany). Here, the gelation phase (~150 s) and the following curing phase was analyzed up to 1,200 s for shear modulus (Pa) and the visco-elastic properties remained constant (shear modulus of 300 Pa) after gelation was completed [36]. In pre-experiments, Al2O3 particles were tested on MSC 3D cultures (n = 6) containing 5 × 105 cells and 50 mg Al2O3 by measuring the luciferase activity after 0 and 4 days. The Al2O3-supplemented samples reached 92 % of the control luciferase activity (constructs without Al2O3), revealing no pronounced toxicity of the particles.
The cell–hydrogel suspension was injected in the larger part of a double channel syringe. The smaller part of the syringe was filled up with the appropriate amount of cross-linking agent [36]. For the in vivo segments, 1 mL of the cell-seeded albumin–hyaluronan hydrogel was injected immediately after partial nucleotomy of the disc (see below) and, as an in vitro reference pellet, the same amount of cell-seeded albumin–hyaluronan hydrogel was injected in a 1.5 mL tube and kept for 3 days in an incubator at 37 °C and <2 % oxygen in DMEM containing 0.5 mM glucose.
Surgical procedure, animal groups
Twelve domestic pigs (~6 months of age, weight 25–50 kg) were approved for use by the Institutional Review Board of the Animal Experimentation Committee at the Regierungspraesidium Karlsruhe, Germany. As previously described [8, 34], an antero-lateral retroperitoneal approach to the spine was used. The L2/3 and L3/4 lumbar IVDs were surgically exposed and underwent partial nucleotomy using a special biopsy device (Bard Angiomed, Karlsruhe, Germany) consisting of a 16G cannula with an interior needle, pierced through the annulus fibrosus and inserted into the nucleus pulposus. For partial nucleotomy, 0.06–0.14 g of gel-like nucleus (~10 % of total nucleus volume) was sucked inside the cannula by high intrinsic nucleus pulposus pressure and repeated syringe aspirations. Then, the syringe was removed for injection of the implant. Contrary to a prior study [34], the biopsy cannula was not removed for implant injection and, hence, the double channel syringe with the implant material was attached to the remaining biopsy cannula. For implant injection, multiple cannula insertions with additional annular damage were thus avoided. Implant material consisted of 1 mL total volume of the albumin–hyaluronan hydrogel supplemented with Al2O3 particles and pMSC-Luc. After injection, the syringe was not moved for 60 s to allow polymerization of the hydrogel. Treated IVDs were marked by fixation of non-resorbable suture material at the transversal processus. Musculature and skin were closed by suture. Six animals were killed immediately after surgery and injection and served as day 0 controls. The other six animals were assigned to a postoperative survival time of 3 days and were allowed free unrestricted weight bearing and activity in cages.
µCT based analysis of implant persistence
The total lumbar spine was resected post mortem. IVDs with adjacent vertebral bodies were dissected using a bone-saw and used for µCT analysis. One hour after killing, segments were scanned using Skyscan 1076 in vivo µCT (Bruker microCT, Antwerp, Belgium) through a 0.5 aluminum prefilter with the following scanning parameters: resolution of 17.7 µm/pixel, voltage 48 kV, source current 200 µA, exposure time of 320 ms and a rotation step of 0.6 with an averaging of 3. Scans were reconstructed and analyzed using manufacturer’s software (NRecon and CTAn, Bruker microCT). Two-dimensional cross sections were used for gross observation of the hydrogel and Al2O3 distribution in the IVD. Despite the hydrogel clot is not radiopaque, it has a reduced X-ray opacity compared to IVD matrix and could be visualized as a negative shade. Al2O3 particles have a higher radio-opacity than IVD matrix. Hence, the total implant was detectable by a homogeneous distribution of Al2O3 particles in the hydrogel. For quantification, a region of interest (ROI) was designed which included the total IVD and excluded calcified vertebrae. A threshold ranging from lower gray level 65 to upper gray level 250 was used for volumetry. Applying the nomenclature published as guidelines for bone histomorphometry by ASBMR [39], three-dimensional analyses were accomplished at day 0 and 3 using the manufacturer’s software. Total implant volume was expressed as mm3 “dense” volume, total number of dense objects at maintained threshold was expressed as number of objects (N.ob.), and relative fraction of non-dense material based on binarization via thresholds within dense objects was expressed as % porosity (Po).
Statistical analysis
Mean ± standard deviations (SD) were calculated for all variables. The Student’s t test was applied to analyze differences between the two groups. For comparisons between multiple groups, anova analysis was performed with Bonferroni p value adjustment. Correlations were determined by calculating the Pearson’s coefficient. A two-tailed p value <0.05 was considered significant. Data analysis was performed with SPSS for Windows 11.0.1 (SPSS Inc., USA).
Results
Luciferase enzyme activity as a metabolic sensor
For monolayer culture conditions, a linear correlation between the number of transgene-labeled pMSC and the recorded luciferase activity was obtained, allowing a deduction of cell numbers from a standard curve under common cell culture conditions [34]. To allow a valid quantitative follow-up of the number of implanted luciferase-labeled cells also during in vivo disc cell therapy, it is mandatory to assess how altered environmental in vivo conditions in an IVD affect luciferase enzyme activity. When luciferase-labeled pMSCs were shifted from monolayer expansion conditions to 3D pellets under chondrogenic conditions for 3 days, the cell metabolism was considerably reduced according to a decline in mitochondrial activity measured by the WST assay (5.8-fold decline; p = 0.005) (Fig. 1a). 3D culture under low nutrient (0.5 mM glucose) and oxygen supply (<2 %) simulating an IVD environment did not further reduce cell metabolism according to the WST assay (Fig. 1a). Parallel to the decline in cell metabolism under 3D culture conditions simulating IVD conditions, luciferase enzyme activity showed a similar strong drop from initial levels to 6.7-fold lower values (p = 0.0003). Accordingly, calculation of the Pearson’s coefficient for all groups revealed a highly significant, strong correlation (r = 0.917, p < 0.01) between the progression of the WST and luciferase measurement values (Fig. 1b).
pMSC-Luc was cultured for 3 days in monolayer culture and incubated in expansion medium (filled circle), in 3D culture with chondrogenic medium (filled square) or in 3D culture with chondrogenic medium with reduced glucose (0.5 mM) and low oxygen (<2 %) (filled triangle). Metabolic activity and luciferase enzyme activity were determined via WST assay (a) and luciferase assay (b), respectively, on day 0, 1, 2 and 3. Monolayer day 0 was considered as day 0 for all other groups [*p < 0.05 versus day 0; sample size n = 4; data are presented as mean ± SD (capped lines)]
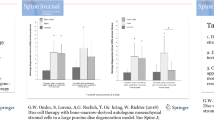
In contrast to the WST assay, however, monitoring of the luciferase activity allowed to distinguish between the different environmental conditions even in 3D, with a decline of luciferase activity by 81 % in 3D pellets and 95 % in 3D pellets with additional medium depletion (p < 0.01 compared to monolayer control on day 3). The drop in luciferase activity between the standard 3D chondrogenic conditions and the simulated IVD-like conditions was further analyzed in dose–response experiments regarding the glucose or oxygen supply, respectively (Fig. 2a, b). Here, luciferase enzyme activity was especially sensitive to a reduction of glucose supply. After 3 days of culture time, 5 mM glucose caused a 50 % decrease of luciferase enzyme activity (p < 0.001), reduction to 0.5 mM caused 75 % decrease (p = 0.001), and reduction to 0 mM caused 90 % decrease (p < 0.001) compared to standard conditions (20 mM glucose). There was a strong correlation (r = 0.979, p = 0.021) of the decrease in luciferase activity with the reduction of the glucose concentration (Fig. 2a). After 3 days of culture time, 5 % oxygen caused a 33 % decrease of luciferase enzyme activity compared to controls (p = 0.004), and 2 % oxygen caused a 52 % decrease of luciferase enzyme activity (p < 0.001) (Fig. 2b). Luciferase activity uniformly continued to decrease further significantly up to day 7, showing no recovery (Fig. 2a, b).
3D cell culture results under modulation of glucose (a) and oxygen (b) concentrations: Luciferase enzyme activity significantly decreased from day 0 to day 7. Reduction of glucose or oxygen concentrations caused further activity decrease [*p < 0.05 versus day 0; sample size n = 4; data are presented as mean ± SD (capped lines)]
In vivo study
All animals completed the study to the follow-up endpoint. No adverse events of the injection were seen. µCT analysis was primary outcome measure for implant integrity and volume after necropsy.
In harvested segments, the nucleotomy and implant insertion site was macroscopically still visible after 3 days. However, annular damage was less pronounced compared to prior results [34], due to avoidance of multiple cannula insertions. The use of a modified double channel syringe attached to the nucleotomy cannula which remained in one position throughout the injection process allowed for only one cannula insertion during the whole procedure. At harvest, implant material was not macroscopically visible outside the disc or around the annular lesion.
In vivo follow-up of injected hydrogel with µCT
Segments from day 0 and day 3 animals (n = 6 each) were analyzed for retained volume and distribution of Al2O3 particles in the hydrogel by µCT. The hydrogel was located in the nucleus and inner annulus region of the IVD in all treated segments. No remaining injection canal or extruded implant material outside the disc was detectable. Some dilution effects in the surrounding scar tissue and loss at tissue preparation cannot, however, be excluded.
Quantitative µCT analysis showed a significant decrease of the total volume of Al2O3 particle and cell supplemented hydrogel within 3 days. The initial implant volume (86.82 ± 46.81 mm3, mean ± SD) detected in day 0 animals was reduced to an average of 61 % (53.02 ± 58.3 mm3, mean ± SD; p = 0.0079) at day 3 (Fig. 3).
µCT analysis of implant material consisting of Al2O3 particles and stem cell augmented hydrogel. Box plot with volumes (mm3) measured after transplantation at day 0 (n = 6) and day 3 (n = 6) (*p < 0.05). Boxes indicate the 25/75 % data intervals, medians (solid line) and standard deviations (capped lines)
Between day 0 and day 3, the amount of single measurable objects (clustered Al2O3 particles) decreased from 643.16 ± 614.98 N.ob. (mean ± SD) to 38.6 ± 62.39 N.ob. (mean ± SD). Within dense objects, porosity of the transferred material decreased significantly from 89.20 ± 3.84 % (mean ± SD) to 70.14 ± 12.86 % (mean ± SD; p = 0.0159) (Fig. 4). This was in line with a concentration of heterogeneously dispersed implant material inside the whole nucleus and inner annulus (day 0 segments) to form a more centrally localized implant material with higher signal intensity in the disc nucleus (day 3 segments), possibly as a consequence of implant compression during movements and load bearing of the animals. Representative slice images from µCT analysis with depiction of the implant material are shown in Fig. 5.
Box plot with porosity results: µCT analysis of the transplanted hydrogel demonstrates changes in the Al2O3 particle containing hydrogel distribution between day 0 (n = 6) and day 3 (n = 6). During in vivo loading, the implant material was compressed and became denser which is expressed by a decrease of the µCT parameter “porosity”. Boxes indicate the 25/75 % data intervals, medians (solid line) and standard deviations (capped lines)
µCT images of the Al2O3 supplemented hydrogel inside the disc at day 0 (a–d) and day 3 (e–h): Upper row (a, c, e, g): µCT overview slide through the disc [1] which is surrounded by a red dashed line: Inside the disc, the implant is marked by a red line [2]; adjacent bone of the vertebrae is marked as [3]. The implant was detectable by a homogeneous distribution of Al2O3 particles in the hydrogel. Lower row (b, d, f, h): Enlargements of the implant from the corresponding picture above. Higher signal intensity in F and H compared to b and d was in line with compression of the hydrogel and changes in Al2O3 particle distribution
Follow-up of luciferase enzyme activity
Two additional pellets of non-implanted cell-albumin–hyaluronan hydrogel material from each animal experiment were immediately subjected to in vitro 3D cell culture under simulated IVD conditions (0.5 mM glucose and <2 % oxygen) to serve as day 0 and day 3 references. Culture was terminated after 3 days parallel to the end of the animal experiment. A significant decrease (p < 0.0001) of relative luciferase enzyme activity to 8 % (64,911 ± 4,809, mean ± SD) of the initial activity at day 0 (808,355 ± 86,361, mean ± SD) was found. This in vitro occurring drop to 8 % luciferase activity was used as a reference to calculate the expected reduction of activities from day 0 animals to day 3 animals in the in vivo trial (78,250 ± 35,078, mean ± SD). Hence, a calculated expected activity of 6,260 was obtained and set as 100 % for the in vivo trial considering the effects related to cell adaptation to the 3D environment together with low glucose and oxygen conditions (Fig. 6). According to µCT analysis, retention of 61 % of implant material was expected to generate about 61 % of this control signal given exact simulation of IVD conditions in the in vitro controls. Disc lysates from day 3 animals (n = 6) retained a luciferase enzyme activity of 1,446 ± 1,405, mean ± SD (p = 0.0031) corresponding to 23 % of the referenced control activity and 38 % if implant loss was additionally considered. Unreferenced in vivo activity, however, dropped to 2 % at day 3 (Fig. 6).
Luciferase activity of hydrogel-embedded, labeled pMSC in vitro and in vivo: 3.3 × 106 pMSCs were suspended in 1 mL albumin–hyaluronan hydrogel and were injected either in a reaction tube and maintained under low glucose (0.5 mM) and low oxygen (<2 %) in an incubator (in vitro reference) or into a partially nucleotomized lumbar porcine in vivo disc [*p < 0.05; data are presented as mean ± SD (capped lines)]. a In vitro reference pellets and in vivo discs were harvested immediately after surgery/polymerization of the hydrogel at day 0 and day 3 to determine luciferase activity of the labeled pMSC (n = 6 per group and day). Measurement values of day 0 were set to 100 %. b In vivo luciferase activity at day 3 (dark gray bar) was calculated in reference to the respective in vitro controls on day 3 (white bar; 100 %). The light gray bar shows luciferase activity loss expected from implant volume loss assessed by µCT analysis
Discussion
To avoid progressive disc degeneration caused by annular damage and progression of degenerative cascades after discectomy or nucleotomy procedures, disc cell therapy has been proposed even in moderately degenerated discs immediately during the nucleotomy procedure [32]. This, however, implies that discs with mainly intact nuclei without relevant nuclear tissue loss might be treated by disc cell therapy, as well, since further removal of intact nuclear material or the complete nucleus seems unfavorable and avoidable. Under such circumstances, only limited amounts of the implant material such as hydrogels with embedded stem cells will be injected into the disc. Whether such small implants can be beneficial against the development of DDD is unknown [32] and it is, therefore, desirable to analyze this strategy in large animal models with biomechanical properties close to humans.
One important point is to know, how much of the implant is retained inside the disc (application safety and efficiency) and a second issue is whether the cells remain vital and maintain an active metabolism in vivo (potency). In the present study, we optimized the implantation technique and applied a new albumin-based hydrogel allowing us to retain 61 % of the initial implant volume over 3 days compared to 10 % in a former study [34]. This may be attributed to the lower annular damage resulting from a less invasive injection procedure and better retention of a new albumin–hyaluronan hydrogel implant solidifying through a cross-linking reaction [36–38] versus previously used fibrin hydrogel. As an important limitation, however, the short 3-day in vivo follow-up time has to be taken into account and hence, long-term results are needed for final evaluation.
µCT data documented a decrease in implant porosity from 80 to 74 % over 3 days and a reduction of detectable single objects inside the disc suggesting a compression of the hydrogel implant material caused by high intradiscal pressure. Whether these found changes in implant characteristics are a disadvantage of the used hydrogel cannot be answered in the present short-term study. The hydrogel was initially not designed to increase the compressive properties inside the nucleus as a rigid biomechanically stable implant but more intended to fill irregularly shaped defects inside the disc and provide a scaffold for implanted cells. Further biomechanical tests and long-term evaluation of the hydrogel will give further information in future studies. Compression of the hydrogel may have also contributed to some degree of implant volume reduction. Although extruded implant material was not macroscopically or radiologically found outside the disc, residual leakage due to annular damage and high intradiscal pressures during immediate postoperative load bearing of the animals cannot be excluded, since extruded material outside the disc would have probably been lost during segment preparation at harvest. Loss of implant volume may, however, be acceptable as long as sufficient amounts of viable cells are retained inside the disc.
In the used animal model, nucleotomy with annular damage significantly increased annular inflammation being still detectable 24 weeks after nucleotomy [24]. Therefore, the use of a hydrogel with anti-inflammatory properties might be beneficial to slow down annular inflammation and positively influence pain associated with DDD. The documented anti-inflammatory activity of stem cells [40, 41] may add value to achieve such an effect. The used albumin-based hydrogel was also designed to have an anti-inflammatory effect via the hyaluronan component [42, 43] and pMSCs were applied in the implant. A quantitative evaluation of such anti-inflammatory in vivo effects, however, awaits further investigation in a follow-up study using later time points.
Apart from inflammation caused by annular damage and exposition of the nucleus pulposus to the surrounding tissues with increased disc degeneration [14, 23, 44, 45], damage of the annulus fibrosus can also cause biomechanical instability of the ring structure with subsequent implant loss [23, 35, 46, 47]. In the present animal model, however, annular damage is only localized to the small needle insertion site and will not significantly influence biomechanical properties, which may be concluded from spine tester analyses in a former study after applying the same nucleotomy procedure, where changes were not as pronounced, resulting in measurable biomechanical changes [8].
Remarkably, a modulation of luciferase enzyme activity of genetically labeled cells dependent on the cellular microenvironment became apparent in this study. Although it is established that ATP is required as a co-substrate to display the luciferase enzyme activity, no attention was so far paid to this fact in the literature, possibly because the luciferase assay was so far not applied in transition from 2D to 3D culture systems. We clearly demonstrated that a close correlation exists between mitochondrial cell activity and luciferase activity of labeled pMSC both declining considerably when cells get shifted to chondrogenic 3D conditions which come with serum withdrawal and high cell density. Whereas the decline in cell metabolism in the WST assay was already so strong with the shift to 3D conditions that there were no considerable changes seen in cell metabolism with longer incubation periods (day 2 and 3) or additional medium depletion, monitoring of luciferase activity allowed to distinguish between the different environmental conditions also in 3D culture. Luciferase is a protein with a short half-life; therefore, the decreased luciferase activity might be related to a reduced anabolic activity of the cells including a down-regulated protein synthesis, which seems to be stronger affected than the energy-related metabolism of the cells which is assessed by the WST assay and which was rapidly stabilized within 24 h.
Luciferase activity reacted strongly to the reduction of glucose or oxygen concentrations with a continuous decrease over 7 days, indicating an adverse effect on cell anabolism. This seems contradictory to other studies, which reported beneficial effects of low glucose concentrations [48] on cell number and aggrecan production or of hypoxia on MSC chondrogenesis [49]. But in these studies, analyses were conducted at later time points and the negative effects on luciferase activity shown here may be part of a transient adaptation process which comes with the altered environmental conditions as there are several studies which also state an initial crisis in luciferase activity after transplantation followed by a recovery or stabilization after several weeks [50, 51].
Thus, surprisingly, the irreversible labeling of cells with a luciferase transgene for the purpose of cell quantification turned into a valuable possibility to follow the cell metabolism under environmental conditions of an IVD in vivo. This observation allows the option that luciferase enzyme activity may serve as a metabolic sensor. As such, the luciferase assay provides very valuable tools for regenerative medicine to fathom a deprived microenvironment like in IVDs. One important consequence of our findings, however, is that luciferase activity cannot, thus, serve as a direct measure of cell persistence under conditions in which the microenvironment is expected to change. Thus, a 3D low glucose, low oxygen control culture was included in this study as a reference point to subtract metabolic effects.
In vitro results showed that the environmental influences (especially the shift from monolayer to 3D conditions) on luciferase activity were so strong, that these results could not be ignored and accordingly a parallel in vitro 3D pellet control was established as a reference, in order not to underestimate the number of vital remaining cells. Even if the chosen reference conditions do not exactly simulate the situation in vivo, they give an approximation, mainly based on the literature [52–54]. The authors´ decided not to adopt the pH, because this parameter had no influence on disc cell viability when glucose was reduced to 0.5 mM glucose under hypoxic conditions [54]. In contrast, Wuertz et al. [48] found a significant influence of the pH on MSC viability, but this was analyzed under normoxic conditions.
Under these conditions and using the in vitro control culture which was taken simultaneously during the in vivo experiment as a reference, luciferase activity dropped to 23 % 3 days after in vivo disc cell therapy (instead of an unreferenced 2 % luciferase activity). Considering, however, an implant loss of 39 % detected by μCT analysis, a higher value of 38 % remaining luciferase activity could be calculated, but this higher value remains speculative, since the amount of implant leakage could not be proven and implant compression might be responsible for the implant loss detected by μCT analysis, as well.
Despite a strong decline of luciferase activity, results demonstrate for the first time that metabolically active cells remain in the IVD for at least 3 days. The observed decline of luciferase activity may be explained by several reasons. Beyond the implant loss which was detected by μCT analysis, the harsh disc environment with high intradiscal pressures, low pH, and the potential accumulation of metabolic waste products would have further contributed to the decrease of luciferase activity after in vivo disc cell therapy [48].
Important limitations of the study have to be taken into account. Most important, the short 3 days in vivo follow-up time does not allow conclusions about mid- or long-term results. Another limitation is the used porcine animal model with important differences to human beings (persistence of notochordal cells, intradiscal pressure, anatomy). As a further limitation, detrimental effects of the Al2O3 particles cannot be completely ruled out, although no macroscopic signs of increased scarring, inflammation or degeneration were found after 3 days, but these surely were time spans too short for the evaluation of possible detrimental effects. However, for the short time span analyzed in this study, cellular toxicity should be considered more relevant than the influence on the tissue itself, and in vitro no pronounced toxicity of the particles was found. Moreover micron-sized Al2O3 particles, as used in this study, are substantially less toxic than their nano-scaled counterparts [55, 56].
Accepting the suitability of luciferase enzyme activity as a metabolic sensor of pMSC activity in both our in vivo and in vitro studies suggests that further efforts should be made to search for methods supporting the anabolic activity of transplanted cells. Receptor-mediated opening of vascular endplate channels [10] or even direct endplate manipulation to reduce endplate sclerosis and increase disc nutrition might be a future option. Whether pMSCs are the optimal cell source or whether other cells including extracted and externally cultivated nucleus cells or even notochordal disc cells might be better remains unsolved. Nonetheless, our data and the data from others indicate that pMSCs are quite capable to adjust to adverse conditions [57–59] and that, vice versa, conditions in an injured disc may not forbid cell therapy.
Our current data imply that––in a scenario with only small amounts of injected implant material used for small defect areas inside an otherwise intact nucleus pulposus, pMSC administered in a hydrogel will first adapt to the harsh intradiscal environment including low oxygen and glucose concentrations by reducing their cell metabolism. Interestingly, it was recently demonstrated that human MSCs re-enter the cell-cycle and re-enhance their metabolism 10–21 days after shift to 3D culture under chondrogenic conditions [60]. This could mean that MSCs have the versatility and capacity to initiate an anabolic response after a lag phase necessary for adaptation and hence future investigations should follow up implanted cells during the first weeks.
In conclusion, this study established for the first time luciferase enzyme activity as a metabolic sensor of pMSC activity in both in vitro and in vivo analyses. Procedural improvements with less annular damage resulted in sufficient albumin–hyaluronan hydrogel implant retainment and persistence of metabolically active pMSC after 3 days in vivo. Based on the limitation of only a short 3 days in vivo follow-up time, long-term outcome remains unclear. Whether the in situ remaining pMSC will further degenerate under the harsh intradiscal properties, or whether they survive and may have the capacity to even resume higher cell activity after adaptation as seen in an in vitro model [60] and suggested by other disc studies on smaller animals [27, 29, 30, 61], awaits to be determined by further studies with long-term follow-up.
References
Lyons G, Eisenstein SM, Sweet MB (1981) Biochemical changes in intervertebral disc degeneration. Biochim Biophys Acta 673:443–453
Benneker LM, Heini PF, Alini M, Anderson SE, Ito K (2005) 2004 Young investigator award winner: vertebral endplate marrow contact channel occlusions and intervertebral disc degeneration. Spine 30:167–173
Chanchairujira K, Chung CB, Kim JY, Papakonstantinou O, Lee MH, Clopton P, Resnick D (2004) Intervertebral disk calcification of the spine in an elderly population: radiographic prevalence, location, and distribution and correlation with spinal degeneration. Radiology 230:499–503
Freemont AJ, Watkins A, Le Maitre C, Jeziorska M, Hoyland JA (2002) Current understanding of cellular and molecular events in intervertebral disc degeneration: implications for therapy. J Pathol 196:374–379
Grunhagen T, Wilde G, Soukane DM, Shirazi-Adl SA, Urban JP (2006) Nutrient supply and intervertebral disc metabolism. J Bone Jt Surg Am 88(2):30–35
Guiot BH, Fessler RG (2000) Molecular biology of degenerative disc disease. Neurosurgery 47:1034–1040
Omlor GW, Lorenz H, Engelleiter K, Richter W, Carstens C, Kroeber MW, Guehring T (2006) Changes in gene expression and protein distribution at different stages of mechanically induced disc degeneration—an in vivo study on the New Zealand white rabbit. J Orthop Res 24:385–392
Omlor GW, Nerlich AG, Wilke HJ, Pfeiffer M, Helga Lorenz, Schaaf-Keim M, Bertram H et al (2009) A new porcine in vivo animal model of disc degeneration—response of annulus fibrosus cells, chondrocyte-like nucleus pulposus cells and notochordal nucleus pulposus cells to partial nucleotomy. Spine 34(25):2730–2739
Pfirrmann CW, Metzdorf A, Elfering A, Hodler J, Boos N (2006) Effect of aging and degeneration on disc volume and shape: a quantitative study in asymptomatic volunteers. J Orthop Res 24:1086–1094
Rajasekaran S, Venkatadass K, Naresh Babu J, Ganesh K, Shetty AP (2008) Pharmacological enhancement of disc diffusion and differentiation of healthy, ageing and degenerated discs. Results from in vivo serial post-contrast MRI studies in 365 human lumbar discs. Eur Spine J 17:626–643
Setton LA, Chen J (2006) Mechanobiology of the intervertebral disc and relevance to disc degeneration. J Bone Jt Surg Am 88(Suppl 2):52–57
Moore RJ (2006) The vertebral endplate: disc degeneration, disc regeneration. Eur Spine J 15(Suppl 3):333–337
Boos N, Weissbach S, Rohrbach H, Weiler C, Spratt KF, Nerlich AG (2002) Classification of age related changes in lumbar intervertebral discs: 2002 Volvo award in basic science. Spine 27:2631–2644
Le Maitre CL, Freemont AJ, Hoyland JA (2007) Catabolic cytokine expression in degenerate and herniated human intervertebral discs: IL-1b and TNFα expression profile. Arthr Res Ther 9:77
Burke JG, Watson RW, McCormack D, Dowling FE, Walsh MG, Fitzpatrick JM (2002) Intervertebral discs which cause low back pain secrete high levels of proinflammatory mediators. J Bone Jt Surg Br 84:196–201
Shamji MF, Setton LA, Jarvis W, So S, Chen J, Jing L, Bullock R, Isaacs RE, Brown C, Richardson WJ (2010) Proinflammatory cytokine expression profile in degenerated and herniated human intervertebral disc tissues. Arthr Rheum 62:1974–1982
Battié MC, Videman T, Kaprio J, Gibbons LE, Gill K, Manninen H, Saarela J, Peltonen L (2009) The twin spine study: contributions to a changing view of disc degeneration. Spine J 9:47–59
Livshits G, Popham M, Malkin I, Sambrook PN, Macgregor AJ, Spector T, Williams FM (2011) Lumbar disc degeneration and genetic factors are the main risk factors for low back pain in women: the UK twin spine study. Ann Rheum Dis 70:1740–1745
Atlas SJ, Keller RB, Wu YA, Deyo RA, Singer DE (2005) Long-term outcomes of surgical and nonsurgical management of sciatica secondary to a lumbar disc herniation: 10 year results from the Maine lumbar spine study. Spine 30:927–935
Choy DS (2000) Familial incidence of intervertebral disc herniation: an hypothesis suggesting that laminectomy and discectomy may be counterproductive. J Clin Laser Med Surg 18:29–32
Carragee EJ, Han MY, Suen PW, Kim D (2003) Clinical outcomes after lumbar discectomy for sciatica: the effects of fragment type and anular competence. J Bone Jt Surg Am 85-A:102–108
Hegewald AA, Ringe J, Sittinger M, Thome C (2008) Regenerative treatment strategies in spinal surgery. Front Biosci 13:1507–1525
Bron JL, Helder MN, Meisel HJ, Van Royen BJ, Smit TH (2009) Repair, regenerative and supportive therapies of the annulus fibrosus: achievements and challenges. Eur Spine J 18:301–313
Omlor GW, Nerlich AG, Lorenz H, Bruckner T, Richter W, Pfeiffer M, Gühring T (2012) Injection of a polymerized hyaluronic acid/collagen hydrogel matrix in an in vivo porcine disc degeneration model. Eur Spine J 21:1700–1708
Meisel HJ, Ganey T, Hutton WC, Libera J, Minkus Y, Alasevic O (2006) Clinical experience in cell based therapeutics: intervention and outcome. Eur Spine J 15(3):397–405
Gruber HE, Johnson TL, Leslie K, Ingram JA, Martin D, Hoelscher G, Banks D et al (2002) Autologous intervertebral disc cell implantation: a model using Psammomys obesus, the sand rat. Spine 27:1626–1633
Sato M, Asazuma T, Ishihara M, Ishihara M, Kikuchi T, Kikuchi M, Fujikawa K (2003) An experimental study of the regeneration of the intervertebral disc with an allograft of cultured annulus fibrosus cells using a tissue-engineering method. Spine 28:548–553
Wei A, Tao H, Chung SA, Brisby H, Ma DD, Diwan AD (2009) The fate of transplanted xenogeneic bone marrowderived stem cells in rat intervertebral discs. J Orthop Res 27:374–379
Sakai D, Mochida J, Iwashina T, Watanabe T, Nakai T, Ando K, Hotta T (2005) Differentiation of mesenchymal stem cells transplanted to a rabbit degenerative disc model: potential and limitations for stem cell therapy in disc regeneration. Spine 30:2379–2387
Sakai D, Mochida J, Iwashina T, Hiyama A, Omi H, Imai M, Nakai T et al (2006) Regenerative effects of transplanting mesenchymal stem cells embedded in atelocollagen to the degenerated intervertebral disc. Biomaterials 27:335–345
Zhang YG, Guo X, Xu P, Kang LL, Li J (2005) Bone mesenchymal stem cells transplanted into rabbit intervertebral discs can increase proteoglycans. Clin Orthop Relat Res 430:219–226
Paesold G, Nerlich AG, Boos N (2007) Biological treatment strategies for disc degeneration: potentials and shortcomings. Eur Spine J 16:447–468
Henriksson HB, Svanvik T, Jonsson M, Hagman M, Horn M, Lindahl A, Brisby H (2009) Transplantation of human mesenchymal stems cells into intervertebral discs in a xenogeneic porcine model. Spine 34:141–148
Omlor GW, Bertram H, Kleinschmidt K, Fischer J, Brohm K, Guehring T, Anton M, Richter W (2010) Methods to monitor distribution and metabolic activity of mesenchymal stem cells following in vivo injection into nucleotomized porcine intervertebral discs. Eur Spine J 19:601–612
Reitmaier S, Kreja L, Gruchenberg K, Kanter B, Silva-Correia J, Oliveira JM, Reis RL et al (2013) In vivo biofunctional evaluation of hydrogels for disc regeneration. Eur Spine J [Epub ahead of print]
Benz K, Stippich C, Osswald C, Gaissmaier C, Lembert N, Badke A, Steck E et al (2012) Rheological and biological properties of a hydrogel support for cells intended for intervertebral disc repair. BMC Musculoskelet Disord 13:54
Scholz B, Kinzelmann C, Benz K, Mollenhauer J, Wurst H, Schlosshauer B (2010) Suppression of adverse angiogenesis in an albumin-based hydrogel for articular cartilage and intervertebral disc regeneration. Eur Cell Mater 20:24–36
Benz K, Stippich C, Fischer L, Möhl K, Weber K, Lang J, Steffen F et al (2012) Intervertebral disc cell- and hydrogel-supported and spontaneous intervertebral disc repair in nucleotomized sheep. Eur Spine J 21:1758–1768
Parfitt AM, Drezner MK, Glorieux FH, Kanis JA, Malluche H, Meunier PJ, Ott SM et al (1987) Bone histomorphometry: standardization of nomenclature, symbols, and units. Report of the ASBMR histomorphometry nomenclature committee. J Bone Miner Res 2:595–610
Singer NG, Caplan AI (2011) Mesenchymal stem cells: mechanisms of inflammation. Annu Rev Pathol 6:457–478
Jiang XX, Zhang Y, Liu B, Zhang SX, Wu Y, Yu XD, Mao N (2005) Human mesenchymal stem cells inhibit differentiation and function of monocyte-derived dendritic cells. Blood 105:4120–4126
Hochberg MC (2000) Role of intra-articular hyaluronic acid preparations in medical management of osteoarthritis of the knee. Semin Arthr Rheum 30:2–10
Goa KL, Benfield P (1994) Hyaluronic acid. A review of its pharmacology and use as a surgical aid in ophthalmology and its therapeutic potential in joint disease and wound healing. Drugs 47:536–566
Key JA, Ford LT (1948) Experimental intervertebral-disc lesions. J Bone Jt Surg Am 30:621–630
Korecki CL, Costi JJ, Iatridis JC (2008) Needle puncture injury affects intervertebral disc mechanics and biology in an organ culture model. Spine 33:235–241
Wilke HJ, Heuer F, Neidlinger-Wilke C, Claes L (2006) Is a collagen scaffold for a tissue engineered nucleus replacement capable of restoring disc height and stability in an animal model? Eur Spine J 15(Suppl 3):433–438
Heuer F, Ulrich S, Claes L, Wilke HJ (2008) Biomechanical evaluation of conventional anulus fibrosus closure methods required for nucleus replacement. Laboratory investigation. J Neurosurg Spine 9:307–313
Wuertz K, Godburn K, Neidlinger-Wilke C, Urban J, Iatridis JC (2008) Behavior of mesenchymal stem cells in the chemical microenvironment of the intervertebral disc. Spine 33:1843–1849
Kanichai M, Ferguson D, Prendergast PJ, Campbell VA (2008) Hypoxia promotes chondrogenesis in rat mesenchymal stem cells: a role for AKT and hypoxia-inducible factor (HIF)-1α. J Cell Physiol 216:708–715
Bai X, Yan Y, Song YH, Seidensticker M, Rabinovich B, Metzele R, Bankson JA et al (2010) Both cultured and freshly isolated adipose tissue-derived stem cells enhance cardiac function after acute myocardial infarction. Eur Heart J 31:489–501
Dégano IR, Vilalta M, Bagó JR, Matthies AM, Hubbell JA, Dimitriou H, Bianco P et al (2008) Bioluminescence imaging of calvarial bone repair using bone marrow and adipose tissue-derived mesenchymal stem cells. Biomaterials 29:427–437
Holm S, Maroudas A, Urban JP, Selstam G, Nachemson A (1981) Nutrition of the intervertebral disc: solute transport and metabolism. Connect Tissue Res 8:101–119
Bartels EM, Fairbank JC, Winlove CP, Urban JP (1998) Oxygen and lactate concentrations measured in vivo in the intervertebral discs of patients with scoliosis and back pain. Spine 23:1–7
Bibby SR, Urban JP (2004) Effect of nutrient deprivation on the viability of intervertebral disc cells. Eur Spine J 13:695–701
Balasubramanyam A, Sailaja N, Mahboob M, Rahman MF, Hussain SM, Grover P (2009) In vivo genotoxicity assessment of aluminium oxide nanomaterials in rat peripheral blood cells using the comet assay and micronucleus test. Mutagenesis 24:245–251
Zhang Q, Xu L, Wang J, Sabbioni E, Piao L, Di Gioacchino M, Niu Q (2013) Lysosomes involved in the cellular toxicity of nano-alumina: combined effects of particle size and chemical composition. J Biol Regul Homeost Agents 27:365–375
Risbud MV, Albert TJ, Guttapalli A, Vresilovic EJ, Hillibrand AS, Vaccaro AR, Shapiro IM (2004) Differentiation of mesenchymal stem cells towards a nucleus pulposus-like phenotype in vitro: implications for cell-based transplantation therapy. Spine 29:2627–2632
Mylotte LA, Duffy AM, Murphy M, O’Brien T, Samali A, Barry F, Szegezdi E (2008) Metabolic flexibility permits mesenchymal stem cell survival in an ischemic environment. Stem Cells 26:1325–1336
Wuertz K, Godburn K, Iatridis JC (2009) MSC response to pH levels found in degenerating intervertebral discs. Biochem Biophys Res Commun 379:824–829
Dexheimer V, Frank S, Richter W (2012) Proliferation as a requirement for in vitro chondrogenesis of human mesenchymal stem cells. Stem Cells Dev 21:2160–2169
Sobajima S, Vadala G, Shimer A, Kim JS, Gilbertson LG, Kang JD (2008) Feasibility of a stem cell therapy for intervertebral disc degeneration. Spine J 8:888–896
Acknowledgments
We would like to thank S. Gantz for statistical support, J. Mollenhauer and K. Gaissmaier from TETEC AG for technical support, providing us with samples of the hydrogel implant and critically reading the manuscript, and V. Kraemer from Friatec AG for samples of Degussit. The study was funded by BioProfile Grant 0313755 and Grant 0315579 from the Ministry of Education and Research, Germany. Also parts of this work were financially supported by the Orthopaedic University hospital.
Conflict of interest
None of the authors has any potential conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
G. W. Omlor and J. Fischer share first authorship.
Rights and permissions
About this article
Cite this article
Omlor, G.W., Fischer, J., Kleinschmitt, K. et al. Short-term follow-up of disc cell therapy in a porcine nucleotomy model with an albumin–hyaluronan hydrogel: in vivo and in vitro results of metabolic disc cell activity and implant distribution. Eur Spine J 23, 1837–1847 (2014). https://doi.org/10.1007/s00586-014-3314-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3314-y