Abstract
Purpose
Surgical adolescent idiopathic scoliosis (AIS) management can be associated with loss of thoracic kyphosis and a secondary loss of lumbar lordosis leading to iatrogenic flatback. Such conditions are associated with poorer clinical outcomes during adulthood. The aim of this study was to evaluate sagittal plane reciprocal changes after posterior spinal fusion in the setting of AIS.
Methods
Thirty consecutive adolescents (mean age 14.6 years) with AIS Lenke 1, 2 or 3 were included in this retrospective study with 2 year follow-up. Full-spine standing coronal and lateral radiographs were obtained preoperatively, at 3 and 24 months postoperatively. Coronal Cobb angle, thoracic kyphosis (TK) and lumbar lordosis (LL) were measured. Surgical procedure was similar in all the cases, with use of pedicular screws between T11 and the lowest instrumented vertebra (≥L2), sublaminar hooks applied in compression at the upper thoracic level and sub-laminar bands and clamps in the concavity of the deformity. Statistical analysis was done using t test and Pearson correlation coefficient.
Results
Between preoperative and last follow-up evaluations a significant reduction of Cobb angle was observed (53.6° vs. 17.2°, p < 0.001). A significant improvement of the instrumented thoracic kyphosis, TK (19.7° vs. 26.2°, p < 0.005) was noted, without difference between 3 and 24 months postoperatively. An improvement in lumbar lordosis, LL (43.9° vs. 47.3°, p = 0.009) was also noted but occurred after the third postoperative month. A significant correlation was found between TK correction and improvement of LL (R = 0.382, p = 0.037), without correlation between these reciprocal changes and the amount of coronal correction.
Conclusion
Results from this study reveal that sagittal reciprocal changes occur after posterior fusion when TK is restored. These changes are visible after 3 months postoperatively, corresponding to a progressive adaptation of patient posture to the surgically induced alignment. These changes are not correlated with coronal plane correction of the deformity. In the setting of AIS, TK restoration is a critical goal and permits favorable postural adaptation. Further studies will include pelvic parameters and clinical scores in order to evaluate the impact of the noted reciprocal changes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Surgical management of Adolescent Idiopathic scoliosis (AIS) remains controversial, particularly regarding optimal posterior fusion strategy [1, 2]. However, consensus appears to exist in the necessity to restore a global spinal alignment in the sagittal plane while correcting the thoracic hypokyphosis [3–7].
The recent development of deformity correction techniques via instrumented posterior fusion using only pedicular screws has been reported to provide excellent results in terms of axial correction and coronal plane restoration [8]. However, all-screw constructs have also been reported to create loss of thoracic kyphosis [9], and according to reciprocal interactions occurring in unfused segments, this loss of kyphosis can be related to a secondary loss of lumbar lordosis potentially leading to iatrogenic flatback [10].
Conversely, hybrid instrumentation strategies which do not employ pedicular screws in the thoracic region may have potential advantages such as reduction of the neurological risk due to screws misplacement [11]. Furthermore, these hybrid constructs may be more efficient for the restoration of thoracic kyphosis with little disadvantage in terms of coronal correction of the deformity compared to pedicular screws [5, 12].
According to these reported findings, we have formulated the hypothesis that a correction of the thoracic hypokyphosis would be associated to a compensatory increase of lumbar lordosis in unfused segments below instrumentation ending in the upper lumbar spine. The aim of this study was therefore to evaluate the reciprocal sagittal alignment changes between thoracic kyphosis and lumbar lordosis after posterior instrumented hybrid fusion with sublaminar bands and to determining if correlation exists between these reciprocal changes and the amount of correction in the coronal plane in AIS patients.
Methods
Study design and inclusion criteria
Thirty adolescent consecutive patients diagnosed with AIS were included in this retrospective single center and single operator study.
Inclusion criteria were defined as follows: AIS classified Lenke 1, 2 or 3 with coronal Cobb angle superior to 45°, surgical treatment by posterior instrumented fusion with sublaminar bands and a lower instrumented vertebra above or at L2, an absence of preoperative systemic disorder or neurologic deficit and a normal preoperative spinal axis MRI. Exclusion criteria included: lumbar major curve, the necessity to perform an anterior discectomy, congenital or neuromuscular scoliosis, an abnormal MRI or the impossibility to obtain preoperative neuro-monitoring.
Data collection and radiographic analysis
For each patient, full-spine postero-anterior and lateral radiographs were obtained in standing position preoperatively, at 3 months and 2 years postoperatively. On every radiograph the coronal Cobb angle, the T4–T12 thoracic kyphosis (TK) and the L1–L5 lumbar lordosis (LL) were measured by an independent observer.
Surgical procedure
During the preoperative evaluation, selection of the lower instrumented vertebra was done using lateral bending radiographs. The surgical procedure was conducted under general anesthesia in prone position using a Jackson table and under neuro-monitoring surveillance (SSEP and MEP). Posterior instrumented fusion was performed according to a protocol previously described [13] and summarized hereafter. After posterior exposure of the spine, an hybrid construct was systematically applied including: pedicular screws in the caudal area between T11 and the lower instrumented vertebra (superior or equal to L2); sub-laminar hooks in compression in the cranial area, two 5.5 mm titanium rods, and sublaminar bands (Universal Clamp, Zimmer, Bordeaux) on 3–6 levels on the concavity of the deformity and 1 or 2 on the convexity for stabilization purpose.
Reduction of the deformity was accomplished in a progressive and multi-level manner by applying a tensioning force on the sublaminar bands affixed to two pre-bent rods. Using the reduction tool, it was therefore possible to apply a postero-lateral translation force on the vertebrae, leading to a posterior traction effect of the spine toward the pre-bent rods (Figs. 1, 2).
A postero-lateral bone graft was then performed using autologous bone material from the spinous processes augmented with synthetic bone substitute (Biosorb, SBM, Lourdes).
Statistical analysis
Changes in radiographic parameters (coronal Cobb angle, TK and LL) between preoperative and postoperative evaluations were analyzed using a paired Student t test. Reciprocal changes between TK and LL, as well as the relationship between sagittal reciprocal changes and the amount of coronal correction were assessed by a Pearson correlation coefficient. A subgroup comparison analysis was then conducted on patients with a preoperative TK <20° or ≥20° using an impaired (>) t test. For all statistical analysis, the level of significance (alpha risk) was set as 5 % (i.e., p < 0.05) (Fig. 3).
Results
Demographic data and surgical parameters
Thirty consecutive AIS patients (28 females and 2 males, mean age 14.7 years, with closed triradiate cartilage) diagnosed with Lenke type 1, 2 or 3 curves were analyzed in this retrospective study. Full-spine coronal and lateral radiographs were available for preoperative, 3 months and 2 years postoperative follow-up for all patients (Fig. 4).
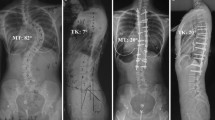
Sagittal radiographs (same patient): preoperative evaluation (left) showed a thoracic hypokyphosis. Surgical restoration of the TK is visible on the 3 months postoperative X-ray (middle) and reciprocal improvement of the lumbar lordosis appeared after the third postoperative month (2 year follow-up on the right)
An average of six sub-laminar bands and clamps (range 4–8) were used in order to reduce the deformity during surgery. No intraoperative changes in neuromonitoring recordings were noted, however, one patient exhibited delayed motor activity of the lower extremities with full-recovery 1 h later.
Global results of radiographic measurements (Table 1)
Preoperative analysis across the study group demonstrated a mean coronal Cobb angle of 53.6° (SD = 7), a thoracic kyphosis of 19.7° (SD = 8) and a lumbar lordosis of 43.9˚ (SD = 11). According to Lenke’s Thoracic Sagittal modifier, 6 patients showed a preoperative thoracic hypokyphosis (TK <10°), 21 were normal (10 < TK < 40°) and 3 patients were hyperkyphotic (TK >40°).
Three months after the surgical procedure, the mean coronal Cobb angle was significantly (p < 0.001) reduced by 68 % on average, without significant modifications between 3 months and 24 months postoperatively (p = 0.314).
Between the preoperative evaluation and 3 months postoperatively, the mean thoracic kyphosis on the study population was significantly increased (average 6.5˚, SD = 5; p = 0.005) without further significant modification between 3 and 24 months postoperatively (p = 0.275). At final follow-up, none of the patients showed a hypokyphosis, 28 had a normal TK and 2 had a TK >40° according to Lenke’s thoracic sagittal modifier.
The lumbar lordosis across the study population was increased (average 3.4°, SD = 6; p = 0.009) between preoperative evaluation and last follow-up, without significant change during the three first postoperative months (p = 0.845).
Results on the whole population are summarized in Table 1.
Subgroup analysis by preoperative thoracic kyphosis (Table 2)
Results from the subgroup based on preoperative TK showed a significantly (p < 0.05) improved coronal Cobb angle in both groups (preoperative TK <20° or ≥20°), but different postoperative radiographic sagittal measurements.
At final follow-up, patients with a preoperative hypokyphosis (TK <20°), exhibited on average a significant increase of the instrumented TK of 10.3° (p < 0.001), with a reciprocal LL increase of 5.5° (p = 0.005). On the other hand, for patients with a normal preoperative kyphosis (TK ≥20°), the instrumentation maintained a normal TK and secondary a normal LL.
Results of the subgroup analysis are summarized in Table 2.
Correlation between radiographic parameters (Table 3)
Based on initial and latest follow-up, across the study population, a significant correlation was found between restoration of thoracic kyphosis and increase in lumbar lordosis (p = 0.037, r = 0.382). However, no significant correlation was found between sagittal reciprocal changes and amount of correction of the Cobb angle in the coronal plane (p = 0.442 and p = 0.691 for kyphosis and lordosis, respectively).
These results were also found in the group of patients with a preoperative TK <20°, for whom the improvement of TK was also associated with an increased LL (p = 0.05, r = 0.423), without significant correlation to correction of the Cobb angle (p = 0.232).
Discussion
Objectives and technical considerations in the surgical management of AIS bear several differences when compared to adult spinal deformity treatment.
Westrick and Ward [14] summarized the five main objectives in the surgical treatment of AIS: arrest deformity progression through a solid fusion, obtain a permanent correction of the deformity, improve appearance of the patient, improve functional outcomes and decrease the risk of degenerative disorders during adulthood.
According to these objectives, AIS treatment strategy will be mainly based on the radiographic characteristic of the deformity while pain and disability are the major parameters of the treatment strategy in adult deformity [15]. Of note, sagittal malalignment (loss of lumbar lordosis, anterior malalignment and pelvic retroversion) have been reported as the main drivers of disability in adults with spinal deformities [16, 17].
Restoration of a satisfactory postoperative sagittal alignment therefore appears a crucial goal, in the management of AIS, whatever the surgical strategy or implant system applied to obtain a solid arthrodesis.
The aim of this study was to analyze the sagittal reciprocal interactions between surgical correction of thoracic kyphosis and improvement of lumbar lordosis, and to search for a correlation between these reciprocal changes and the amount of correction of the coronal Cobb angle.
Hybrid constructs and kyphosis correction
Lehman et al. [9] reported in 2008, on a series of 114 patients, with an average loss of thoracic kyphosis of 9.9° when performing reduction by all-screw constructs but without using rod-derotation maneuvers. When applied, the rod-derotation maneuvers can lead to an improvement of the thoracic kyphosis with an average gain reported to be 5° by Suk et al. [8], but this can also lead to coronal hypercorrection of the deformity with trunk inclination and shoulder asymmetry [18, 19]. Results from this study confirm the ability of hybrid constructs using sub-laminar bands and clamps to maintain TK for normokyphotic patients, and to restore a satisfactory TK for hypokyphotic patients, by applying a posterior traction force on the spine toward pre-bent rods, with an average gain of 6.5° at last follow-up. Furthermore, this technique can limit the risk of hypercorrection due to the absence of rod-derotation maneuvers. A crucial point is the necessity to choose the appropriate lower instrumented vertebra. In this study, we used supine side-bending radiographs in order to take into account curve flexibility but recent reports revealed that the use of fulcrum-bending radiographs was more likely to approximate the coronal postoperative outcomes [20].
The impact of vertebral derotation on sagittal alignment and rib hump is also an important parameter. In our experience, no direct vertebral derotation forces were applied to vertebrae. However, the postero-medial translation forces applied on the concavity of the curve can decrease vertebral rotation [21], but this parameter was not measured in our series. It has been recently reported that direct vertebral body derotation was associated with a significant decrease of rib hump [22], even if for large rib prominences better inclinometer readings were achieved with thoracoplasty alone [23].
Furthermore, impact of direct vertebral derotation (DVD) on sagittal alignment is still controversial. According to Kadoury et al. [24] there is a 74 % axial rotation correction and a better 3D correction achieved with DVD compared to Harrington–Luque, and Cotrel–Dubousset instrumentation but all of these techniques were associated to a loss of lumbar lordosis and loss of correction has been described at 2-year follow-up especially in skeletally immature patients [25]. More recently, Hwang et al. [26] showed on 323 patients that DVD did not worsen the sagittal profile compared to rod-derotation technique but both groups showed a postoperative decrease of thoracic kyphosis, highlighting the importance of appropriate rod contouring. Similar findings were also reported in another study based on 30 patients [27] where the authors concluded that DVD was responsible for a loss of thoracic kyphosis and lumbar lordosis. The same authors therefore recommended pulling posteriorly the concave side of the spine in order to preserve sagittal alignment, which is the equivalent of the technique we used in this study with sublaminar bands and clamps.
Another concern with hybrid construct is the possible occurrence of postoperative crankshaft phenomenon as described by Dubousset et al. [28] as a consequence of a continued anterior spinal growth in the presence of a posterior fusion. Tao et al. [29] have suggested that hybrid construct were not likely to prevent crankshaft phenomenon when compared to pedicle screws construct. This complication is essentially encountered with skeletally immature patients, and was not seen in our series as all patients showed a closed triradiate cartilage at the time of surgery.
Reciprocal sagittal interactions and correlations
Results from this study confirm the initial research hypothesis on the presence of sagittal reciprocal interactions in the unfused segments of the spine. Conversely to surgical constructs where the loss of thoracic kyphosis is followed by a secondary loss of lumbar lordosis [10], our results demonstrate a significant correlation between correction of thoracic kyphosis and improvement of lumbar lordosis for hypokyphotic patients, corresponding to a positive reciprocal change. These reciprocal changes have also been reported in adult deformity patients in the unfused spinal segments, potentially leading, according to the type of compensation, to favorable or unfavorable radiographic outcomes [30, 31].
Such interactions have also been described in AIS patients but in the coronal plane with a spontaneous correction of the lumbar curve [32]. Considering the sagittal plane, Hilibrand et al. [33] have reported presence of such reciprocal interactions on the upper spine, with a significant correlation between hypokyphosis and loss of cervical lordosis.
Interestingly, the results from this study showed that improvement of lumbar lordosis secondary to thoracic kyphosis correction occurred after the third postoperative month, reflecting, in our opinion, the necessary adaptation of posture to the new imposed alignment.
Notably, no correlation was found between sagittal reciprocal interactions and the amount of coronal correction. This finding leads to questioning the need to obtain maximal coronal plane correction of scoliotic deformities in the setting of AIS. Hybrid constructs with sub-laminar bands may not offer the same amount of coronal correction than all-screw constructs, however, this difference will not lead to inferior sagittal reciprocal changes. This consideration supports other reports questioning the necessity to obtain a perfect coronal correction to the detriment of sagittal alignment [10, 19].
The long-term impacts of the radiographic results noted in this study are difficult to evaluate. While the presence of a thoracic hyperkyphosis has been correlated with a decrease of clinical outcomes (SRS-score) [34], no modifications of clinical outcomes has been reported at 2-year follow-up in AIS patients with a postoperative hypokyphosis [4]. However, the lack of differences at short-term follow-up does not indicate the long-term prognosis for these patients. Further studies will be necessary in order to evaluate the clinical impact of sagittal reciprocal changes, including aspects of cervical spinal alignment and pelvic parameters (spino-pelvic chain of correlation).
Conclusion
Despite limitations due to the retrospective design of this study, and a limited follow-up, sagittal reciprocal changes between improvement of thoracic kyphosis and improvement of lumbar lordosis was determined. These results underline the necessity to restore optimal thoracic kyphosis, whatever the surgical strategy used, in order to offer adolescents suffering from AIS optimal sagittal alignment as they mature into adulthood.
References
Bess S, Boachie-Adjei O, Burton D, Cunningham M, Shaffrey C, Shelokov A, Hostin R, Schwab F, Wood K, Akbarnia B (2009) Pain and disability determine treatment modality for older patients with adult scoliosis, while deformity guides treatment for younger patients. Spine (Phila Pa 1976) 34:2186–2190. doi:10.1097/BRS.0b013e3181b05146
Cheng I, Kim Y, Gupta MC, Bridwell KH, Hurford RK, Lee SS, Theerajunyaporn T, Lenke LG (2005) Apical sublaminar wires versus pedicle screws–which provides better results for surgical correction of adolescent idiopathic scoliosis? Spine (Phila Pa 1976) 30:2104–2112
Clement JL, Chau E, Kimkpe C, Vallade MJ (2008) Restoration of thoracic kyphosis by posterior instrumentation in adolescent idiopathic scoliosis: comparative radiographic analysis of two methods of reduction. Spine (Phila Pa 1976) 33:1579–1587. doi:10.1097/BRS.0b013e31817886be
Cui G, Watanabe K, Nishiwaki Y, Hosogane N, Tsuji T, Ishii K, Nakamura M, Toyama Y, Chiba K, Matsumoto M (2012) Loss of apical vertebral derotation in adolescent idiopathic scoliosis: 2-year follow-up using multi-planar reconstruction computed tomography. Eur Spine J. doi:10.1007/s00586-012-2274-3
Daffner SD, Beimesch CF, Wang JC (2010) Geographic and demographic variability of cost and surgical treatment of idiopathic scoliosis. Spine (Phila Pa 1976) 35:1165–1169. doi:10.1097/BRS.0b013e3181d88e78
de Jonge T, Dubousset JF, Illes T (2002) Sagittal plane correction in idiopathic scoliosis. Spine (Phila Pa 1976) 27:754–760
Dubousset J, Herring JA, Shufflebarger H (1989) The crankshaft phenomenon. J Pediatr Orthop 9:541–550
Fletcher ND, Hopkins J, McClung A, Browne R, Sucato DJ (2011) Residual thoracic hypokyphosis following posterior spinal fusion and instrumentation in adolescent idiopathic scoliosis: risk factors and clinical ramifications. Spine (Phila Pa 1976). doi:10.1097/BRS.0b013e318216106c
Hilibrand AS, Tannenbaum DA, Graziano GP, Loder RT, Hensinger RN (1995) The sagittal alignment of the cervical spine in adolescent idiopathic scoliosis. J Pediatr Orthop 15:627–632
Hwang SW, Samdani AF, Cahill PJ (2011) The impact of segmental and en bloc derotation maneuvers on scoliosis correction and rib prominence in adolescent idiopathic scoliosis. J Neurosurg Spine 16:345–350. doi:10.3171/2011.11.SPINE11277
Hwang SW, Samdani AF, Gressot LV, Hubler K, Marks MC, Bastrom TP, Betz RR, Cahill PJ (2012) Effect of direct vertebral body derotation on the sagittal profile in adolescent idiopathic scoliosis. Eur Spine J 21:31–39. doi:10.1007/s00586-011-1991-3
Imrie M, Yaszay B, Bastrom TP, Wenger DR, Newton PO (2011) Adolescent idiopathic scoliosis: should 100 % correction be the goal? J Pediatr Orthop 31:S9–13. doi:10.1097/BPO.0b013e3181fd8a24
Jansen RC, van Rhijn LW, Duinkerke E, van Ooij A (2007) Predictability of the spontaneous lumbar curve correction after selective thoracic fusion in idiopathic scoliosis. Eur Spine J 16:1335–1342. doi:10.1007/s00586-007-0320-3
Jouve JL, de Gauzy JS, Blondel B, Launay F, Accadbled F, Bollini G (2009) Use of the Universal Clamp for deformity correction and as an adjunct to fusion: preliminary results in scoliosis. J Child Orthop. doi:10.1007/s11832-009-0221-6
Kadoury S, Cheriet F, Beausejour M, Stokes IA, Parent S, Labelle H (2009) A three-dimensional retrospective analysis of the evolution of spinal instrumentation for the correction of adolescent idiopathic scoliosis. Eur Spine J 18:23–37. doi:10.1007/s00586-008-0817-4
Lafage V, Schwab F, Patel A, Hawkinson N, Farcy JP (2009) Pelvic tilt and truncal inclination: two key radiographic parameters in the setting of adults with spinal deformity. Spine (Phila Pa 1976) 34:E599–E606. doi:10.1097/BRS.0b013e3181aad219
Lafage V, Schwab F, Boachie-Adjei O, Farcy JP, Shelokov A, Hostin R, Hart R, Akbarnia B, O’Brien M, Burton D, Shaffrey C, Group ISS (2009) The impact of reciprocal regional alignment changes distant from the site of spinal osteotomies affects post-operative spinal balance. Scoliosis Research Society, San Antonio
Lafage V, Klineberg E, Schwab F, Akbarnia B, Ames C, Boachie-Adjei O, Burton D, Hart R, Hostin R, Shaffrey C, Wood K, Bess RS, Group ISS (2010) Changes in thoracic kyphosis negatively impact sagittal alignment following lumbar pedicle subtraction osteotomy. Scoliosis Research Society, Kyoto
Lehman RA Jr, Lenke LG, Keeler KA, Kim YJ, Buchowski JM, Cheh G, Kuhns CA, Bridwell KH (2008) Operative treatment of adolescent idiopathic scoliosis with posterior pedicle screw-only constructs: minimum three-year follow-up of one hundred fourteen cases. Spine (Phila Pa 1976) 33:1598–1604. doi:10.1097/BRS.0b013e318178872a
Lenke LG, Betz RR, Harms J, Bridwell KH, Clements DH, Lowe TG, Blanke K (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am 83-A:1169–1181
Lenke LG, Edwards CC 2nd, Bridwell KH (2003) The Lenke classification of adolescent idiopathic scoliosis: how it organizes curve patterns as a template to perform selective fusions of the spine. Spine (Phila Pa 1976) 28:S199–S207. doi:10.1097/01.brs.0000092216.16155.33
Li J, Dumonski ML, Samartzis D, Hong J, He S, Zhu X, Wang C, Vaccaro AR, Albert TJ, Li M (2010) Coronal deformity correction in adolescent idiopathic scoliosis patients using the fulcrum-bending radiograph: a prospective comparative analysis of the proximal thoracic, main thoracic, and thoracolumbar/lumbar curves. Eur Spine J 20:105–111. doi:10.1007/s00586-010-1495-6
Lowenstein JE, Matsumoto H, Vitale MG, Weidenbaum M, Gomez JA, Lee FY, Hyman JE, Roye DP Jr (2007) Coronal and sagittal plane correction in adolescent idiopathic scoliosis: a comparison between all pedicle screw versus hybrid thoracic hook lumbar screw constructs. Spine (Phila Pa 1976) 32:448–452. doi:10.1097/01.brs.0000255030.78293.fd
Mazda K, Ilharreborde B, Even J, Lefevre Y, Fitoussi F, Pennecot GF (2009) Efficacy and safety of posteromedial translation for correction of thoracic curves in adolescent idiopathic scoliosis using a new connection to the spine: the Universal Clamp. Eur Spine J 18:158–169. doi:10.1007/s00586-008-0839-y
Mladenov KV, Vaeterlein C, Stuecker R (2011) Selective posterior thoracic fusion by means of direct vertebral derotation in adolescent idiopathic scoliosis: effects on the sagittal alignment. Eur Spine J 20:1114–1117. doi:10.1007/s00586-011-1740-7
Newton PO, Yaszay B, Upasani VV, Pawelek JB, Bastrom TP, Lenke LG, Lowe T, Crawford A, Betz R, Lonner B (2010) Preservation of thoracic kyphosis is critical to maintain lumbar lordosis in the surgical treatment of adolescent idiopathic scoliosis. Spine (Phila Pa 1976) 35:1365–1370. doi:10.1097/BRS.0b013e3181dccd63
Petcharaporn M, Pawelek J, Bastrom T, Lonner B, Newton PO (1976) The relationship between thoracic hyperkyphosis and the Scoliosis Research Society outcomes instrument. Spine (Phila Pa 1976). doi:10.1097/BRS.0b013e31814b1bef
Samdani AF, Hwang SW, Miyanji F, Lonner B, Marks MC, Sponseller PD, Newton PO, Cahill PJ, Shufflebarger HL, Betz RR (2012) Direct vertebral body derotation, thoracoplasty or both: which is better with respect to inclinometer and SRS-22 scores? Spine (Phila Pa 1976). doi:10.1097/BRS.0b013e31824a4911
Schwab F, Patel A, Ungar B, Farcy JP, Lafage V (2010) Adult spinal deformity-postoperative standing imbalance: how much can you tolerate? An overview of key parameters in assessing alignment and planning corrective surgery. Spine (Phila Pa 1976) 35:2224–2231. doi:10.1097/BRS.0b013e3181ee6bd4
Senaran H, Shah SA, Gabos PG, Littleton AG, Neiss G, Guille JT (2008) Difficult thoracic pedicle screw placement in adolescent idiopathic scoliosis. J Spinal Disord Tech 21:187–191. doi:10.1097/BSD.0b013e318073cc1d
Suk SI, Lee SM, Chung ER, Kim JH, Kim SS (2005) Selective thoracic fusion with segmental pedicle screw fixation in the treatment of thoracic idiopathic scoliosis: more than 5-year follow-up. Spine (Phila Pa 1976) 30:1602–1609
Tao F, Zhao Y, Wu Y, Xie Y, Li M, Lu Y, Pan F, Guo F, Li F (2010) The effect of differing spinal fusion instrumentation on the occurrence of postoperative crankshaft phenomenon in adolescent idiopathic scoliosis. J Spinal Disord Tech 23:e75–e80. doi:10.1097/BSD.0b013e3181d38f63
Vora V, Crawford A, Babekhir N, Boachie-Adjei O, Lenke L, Peskin M, Charles G, Kim Y (2007) A pedicle screw construct gives an enhanced posterior correction of adolescent idiopathic scoliosis when compared with other constructs: myth or reality. Spine (Phila Pa 1976) 32:1869–1874. doi:10.1097/BRS.0b013e318108b912
Westrick ER, Ward WT (2011) Adolescent idiopathic scoliosis: 5-year to 20-year evidence-based surgical results. J Pediatr Orthop 31:S61–S68. doi:10.1097/BPO.0b013e3181fd87d5
Acknowledgments
Association pour le Développement des Recherches Biologiques et Médicales (A. DE.RE.M).
Conflict of interest
JL Jouve consultant Zimmer.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Blondel, B., Lafage, V., Schwab, F. et al. Reciprocal sagittal alignment changes after posterior fusion in the setting of adolescent idiopathic scoliosis. Eur Spine J 21, 1964–1971 (2012). https://doi.org/10.1007/s00586-012-2399-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-012-2399-4