Abstract
Purpose
Previous studies have demonstrated vertebral coplanar alignment (VCA) as an effective surgical option for adolescent idiopathic scoliosis (AIS). The purpose of this study is to analyze the outcome of VCA for the surgical correction of adult idiopathic scoliosis (AdIS).
Methods
35 AdIS patients (mean age: 24.2 years) undergoing VCA-instrumentation were reviewed. The main thoracic curve and thoracic kyphosis (TK, T5-T12) were evaluated preoperatively, immediate postoperatively, and at the final follow-up (>1 year). All patients were stratified by the TK modifier before surgery: “+” (TK, >40°), “−” (TK, <10°), and “N” (TK, 10°–40°) for normal. The apical vertebral body-to-rib ratio (AVB-R), rib hump (RH), and rotational angle to sacrum (RAsac) were measured to assess the correction of rotational deformity. Quality of life was evaluated with SRS-20 questionnaires.
Results
The main thoracic curve (59.1° vs. 19.3°, P < 0.001) and rotational deformity (AVB-R: 2.4 vs. 1.7 %, P < 0.001, RH: 34.9 vs. 19.1 mm, P < 0.001, RAsac: 19.6° vs. 11.9°, P < 0.001) were significantly reduced with surgery. Sagittal deformity improved significantly in group “+” (51.4° vs. 31.6°, P < 0.001) and group “−” (6.2° vs. 20.1°, P < 0.001), while no significant postoperative change in TK was observed in group “N” (23.5° vs. 26.3°, P = 0.270). Patients were followed for an average of 18.7 months with no significant loss of correction. SRS scores improved greatly from 57.7 preoperatively to 71.6 at the final follow-up.
Conclusions
VCA can be effectively used for the correction of the coronal and rotational deformity, with better sagittal profile restoration in adult thoracic idiopathic scoliosis with sagittal malalignment.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Adult idiopathic scoliosis (AdIS) is defined as patients presenting with scoliosis during childhood or adolescence that may progress or become symptomatic when reach adulthood [1–3]. Aside from the esthetic considerations, it is also well known that untreated scoliosis in adults could eventually develop into progressive deformity, or coronal and sagittal plane imbalance with chronic muscle fatigue [4–6]. Thus, surgical correction for the treatment of AdIS is usually recommended, especially for patients with a large curve [5].
The deformity of idiopathic scoliosis is 3-D. Treatment of scoliosis should preferably be aimed at addressing reduction of the abnormal curvature in each of the three spatial planes. Pedicle screws were universally accepted in treating various spinal deformities for a long-time period. Traditional techniques of spinal instrumentation with pedicle screws corrected scoliosis by applying distraction, derotation, and translation on the concave side or their contribution [7, 8]. Although satisfactory correction of coronal deformity achieved by these traditional techniques has been reported, several studies also stressed that corrections starting from the concave side in treating thoracic curves may decrease the thoracic kyphosis [9, 10] and may increase the neurologic complications when screw malposition occurred on the concave side.
The vertebral coplanar alignment (VCA) technique was initially introduced by Vallespir et al. [11] to correct rotation and translation deformity and to restore the normal sagittal profile in thoracic scoliosis. Contrary to the previously described techniques, VCA occupied the following advancements: better ability to derotation; better ability to restore thoracic kyphosis, which is significantly smaller in AIS patients; reducing the risk of screw misplacement-related neurological complication since the screw insertion started at the concave side of the curve where the spinal cord is not touched and pedicles of the concave side have larger diameters that allow for an easier insertion and greater derotation force than those at the concave side. [11–13] Excellent outcomes from VCA in correcting the coronal and transverse planes with normalization of thoracic kyphosis in Lenke type 1 adolescent idiopathic scoliosis (AIS) have been reported [8, 11, 14]. Adult idiopathic scoliosis is not as flexible as adolescent idiopathic scoliosis, and patients with thoracic curvature are often combined with sagittal malalignment, such as flatback or hyperkyphosis [1, 15, 16]. The purpose of this study was to investigate the preliminary results of VCA for the correction of AdIS with respect to curve correction, vertebra derotation, sagittal profile realignment, operation time, intra-operative blood loss, and health-related quality of life (HRQoL) as measured by Scoliosis Research Society (SRS)-20 scores.
Materials and methods
This study was approved by the ethics committee of the hospital. Patients who were diagnosed with AdIS and received posterior pedicle screw instrumentation and VCA between November 2008 and January 2012 were retrospectively reviewed. SRS-20 scores were collected preoperatively and at final follow-up. The inclusion criteria were as follows: (1) patients over the age of 20 with an established diagnosis of AdIS. (2) Main thoracic curve with Cobb angle between 50° and 115°. (3) Treated with VCA and Follow-up more than 1 year. Patients with previous spinal surgery were excluded.
Radiographic analysis
Correction of coronal and sagittal plane deformities was evaluated on the long-cassette standing coronal and lateral radiographs of the whole spine. Preoperative curve flexibility was determined on the supine-side bending films. The thoracic kyphosis (the Cobb angle from the T5 upper endplate to the T12 lower endplate on the lateral radiographs, TK) as well as lumbar lordosis (the Cobb angle from the L1 upper endplate to the S1 upper endplate on the lateral radiographs, LL) was measured to assess the correction of sagittal deformity. Parameters used to assess the correction of apical rotation include (1) rotational angle to sacrum (the angle between the middle line of the apical body and the sagittal line on CT scanning, RAsac), (2) rib hump (the distance between the left and right posterior rib humps on the lateral radiographs at the level of the apical vertebrae, RH), (3) apical vertebral body-to-rib ratio (the ratio of linear measurements from lateral borders of the apical vertebrae to chest wall in the anteroposterior radiograph, AVB-R). All radiographic parameters were evaluated on the preoperative, postoperative, and last follow-up radiographs. All measurements were made using the Surgimap Spine software (Version: 1.1.2.293, Nemaris Inc, New York, USA).
Patients were divided into three subgroups according to TK [17]: group “−” with TK <10° was regarded as flatback deformity; group “+” with TK >40° was defined as hyperkyphosis; group “N” with TK between 10° and 40° was indicative of normal thoracic sagittal alignment.
Surgical procedure
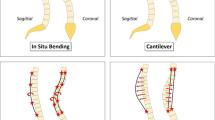
The basic principle and procedure of the VCA described by Vallespir et al. [11] was followed. Pedicle screws were inserted at each index level with more screws on the convex side. A slotted tube was screwed in line with a screw axis to each pedicle screw on the convex side of the main thoracic curve. Once all the tubes were anchored, their tips were spread in accordance to the spinal deformity caused by the vertebral rotation and translation. Two rigid bars were sequentially inserted through the uppermost part of the slotted tube starting from the most cephalad screw. The lower bar was progressively driven down towards the bottom of the tubes. As the lower bar descended and the upper bar was kept in its place, the pedicle screw axis converged into the same plane, correcting the pathological translation and rotation of the spine. The magnitude of the curve was measured in both the coronal and sagittal (T5–T12) planes using Cobb’s method in standing AP and lateral radiographs of the whole spine taken in the immediate preoperative. According to the preoperative TK, a normal thoracic kyphosis was reconstructed by inserted polyethylene spacers with various lengths (20, 25, and 30 cm) between the tops of each tube. The ends of the tubes have to be spread to achieve the physiologic posterior divergence in kyphotic area. To avoid flattening, the previously achieved thoracic kyphosis by the descent of the second bar, a polyethylene block is inserted into the slots of the tubes at both ends of the instrumented kyphosis. These blocks will act as stoppers, allowing for a relative sinking of the ends of the thoracic area relative to the apex. Stoppers are used at the limits of the kyphotic area to avoid flattening of the spine. A precontoured rod (only sagittal kyphosis) was inserted and secured to each screw on the concave side with minor derotation and distraction force because the majority of the correction force has been transmitted by the VCA system. The slotted tubes and two bars were then removed from the convex side and the convex rod was placed. The convex rod was under-contoured to achieve further compression and correction of the deformity. Two cross-links were used between the two rods as closely as possible at the ends of the instrumentation. Posterolateral bone grafting was then performed. Intra-operative neurological monitoring (somatosensory evoked potential, SEP/ motor evoked potential, MEP) was used over the whole course of the intervention.
Statistical analysis
The statistical differences were analyzed using SPSS18.0. Paired sample t tests were performed to determine whether there was a significant change in any of the clinical measurements after surgery. A value of P < 0.05 was considered statistically significant.
Results
A total of 35 cases undergoing VCA-instrumentation were included in this study with an average follow-up of 18.7 months (range 12–46 months). There were 26 females and 9 males with a mean age of 24.2 years (range 20–35 years). According to the above-mentioned modifier of TK, there were 12 patients who had “−” type with an average kyphosis angle of 6.2°, 15 “N” type with an average kyphosis angle of 23.5°, and 8 “+” type with an average kyphosis angle of 51.4°. The range for levels fused, implant density, and other surgical information are shown in Table 1.
Preoperative average main thoracic curves of 59.1° (SD 16.5°) with a mean flexibility of 43.0 % were corrected to 19.3° (SD 9.8°) (67.3 % correction) postoperatively (P < 0.001). Preoperative and postoperative RAsac, RH, and AVB-R were significantly different as provided in Table 2. The correction rate of RAsac, RH, and AVB-R were 39.3, 45.3, and 29.2 %, respectively. The hyperkyphosis and flatback deformity in group “+” (51.4° VS. 31.6°, P < 0.001) and group “−” (6.2° VS. 20.1°, P < 0.001) were both corrected after surgery, whereas no difference in postoperative thoracic kyphosis was noted in group “N” (23.5° VS. 26.3°, P = 0.270). All the parameters remained stable at the final follow-up (Table 2). SRS scores improved greatly from 57.7 preoperatively to 71.6 at final follow-up. The mean SRS-20 questionnaire scores for function, pain, general self-image, and mental health were 14.4, 12.2, 15.8, and 14.6, preoperatively and improved significantly to 16.7, 15.6, 19.9, and 16.8, at the final follow-up (Table 3).
Complications
The VCA correction technique was performed for all patients successfully without major complications. There was one case of hemothorax which resolved during 3 months follow-up without chest tube drainage. There were five patients with nine pedicle screw malposition on the concave side but none of the perforated screws were in positions that posed medical risk to the patient (breaching out more than 4 mm of pedicle perforation or touching aorta) [18]. At last follow-up, no neurologic complications, delayed deep wound infection, pseudoarthrosis were noticed.
Discussion
Surgery for rigid spinal deformity in adults remains a challenge in spinal surgery [19]. From a biomechanical point of view, ideal correction of larger and stiffer curves will require applying higher corrective torques and forces to counteract the large elastic springback due to the rigid and three-dimensional deformity in AdIS [20]. Over the last decade, the cantilever, translational, and vertebral derotation techniques with pedicle screws have been commonly used for the treatment of adults with scoliosis.
The correction of main coronal curves achieved with pedicle screws in AdIS were reported ranges from 37 to 69 % [20–24]. Mermer et al. [21], in 2006, evaluated the radiographic outcomes of 97 adult patients treated with third-generation instrumentation included cantilever and translational techniques, the results showed that the main coronal curves was corrected from 53° preoperatively to 32° postoperatively (39.6 % correction). Silvestre et al. [25] found that the direct vertebral derotation procedure showed a significantly better final correction of main thoracic curve (61.3 %). Raed et al. [24] reviewed the results of surgical treatment for adult scoliosis using third-generation segmental instrumentation techniques, the results showing a coronal correction of 64 %. Suk et al. [26] presented that the thoracic curvature was reduced from 51° to 16° (69 % correction). In the present series, using VCA, the percentages of correction obtained are in consonance with previously published literature, with a 67.3 % correction in main thoracic curve.
There were few studies reported the correction of rotational deformity in AdIS. Previous studies have confirmed that rotation at the apex vertebra can be directly measured by the rotational angle to sacrum (RAsac), using preoperative and postoperative CT-scans [27, 28], and apical vertebral body-rib ratio (AVB-R) and rib hump (RH) were also calculated as indirect measurements of the vertebral thoracic rotation [29]. The average RAsac correction rate using rod rotational and translational techniques was approximately 10 % [30]. Steib et al. [31] analyzed the surgical correction of scoliosis by means of in situ contouring technique and found that the correction rate of the axial rotation was about 60 %. Lee et al. [32] measured rotational correction obtained by the direct vertebral rotation technique using the RAsac and reported a correction of 42.5 %. Other studies have shown that the correction rate of RH ranged from 51 to 65 %, and the correction rate of AVB-R ranged from 29 to 54 % [10, 11]. Mattila et al. [33] performed vertebral column derotation for 48 children and adolescents, the correction of thoracic RH was 51 %. A literature review [34] showed that VCA has been assessed with radiographic measures of RH achieving 50–65 % correction in adolescent idiopathic scoliosis; however, no comparisons of rib hump by VCA vs. traditional techniques have been made. In our study, the correction rate of RAsac (39.3 %) was higher than that of rod rotational and translational techniques, and similar with the correction rate of direct vertebral rotation by Lee. The correction rate of RH (45.3 %) and AVB-R (29.2 %) in our study was lower to those of adolescent idiopathic scoliosis in previous reports. [10, 11] This may due to the spinal curvature of AdIS is not as flexible as that of adolescent idiopathic scoliosis, and the rib cage is more rigid in adult patients.
As concerns about sagittal profile restoration arised, Roussouly et al. [35], in 2013, assessed the changes of sagittal alignment in 52 adult idiopathic scoliosis after using translation technique. They noticed that no changes could be found in thoracic kyphosis in the entire group. However, when sub-classified according to thoracic hypokyphosis vs. normal-kyphosis (≥20°) preoperatively, there was a significant improved of TK in the hypokyphotic group, while TK were decreased in the normokyphotic group (36°–30°). Mermer et al. [21] found that the thoracic kyphosis increased at follow-up (36° preoperatively, 39° postoperatively, and then 46° at follow-up). Rod rotation techniques correct in the sagittal plane by simply translating the coronal curvature of the rod to posterior, improving hypokyphosis [30]. While the improvement of TK was mostly reported in adolescent idiopathic scoliosis [9, 12, 32, 35], and few studies analyze the change of sagittal profile of AdIS in subgroups.
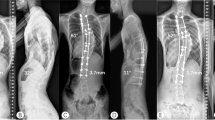
Traditionally, the curvature of the rod determines the degree of deformity correction. Operators usually bend the rod to the estimated value of TK by “hand feeling” intraoperatively. The principle of VCA is based on both returning the normally coplanar axes (x and z) into a single plane and returning the x-axis to its normal posterior divergence in the sagittal plane [11]. The normal TK was obtained by spacers. According to the preoperative TK, a normal thoracic kyphosis was reconstructed by inserted polyethylene spacers with various length (20, 25, and 30 cm) between the tops of each tube. Results from the present study showed a significant improvement of TK in hypokyphosis group (6.2°–20.1°) (Fig. 1) and in hyperkyphosis group (51.4°–31.6°) (Fig. 2), and there were no change in normokyphotic group postoperatively. The sagittal profile remained stable at the final follow-up. These outcomes might be achieved through the technique of VCA, which has the ability to correct sagittal plane deformities in every segments.
A 28-year-old female with main thoracic curve and hyperkyphosis deformity was operated on with the vertebral coplanar alignment technique. a, b radiographs of pre-operative; c, d radiographs of 1 year and 3 months follow-up. The hyperkyphosis was corrected to normal sagittal profile after surgery. MT main thoracic Cobb angle, TK thoracic kyphosis angle
Thus, VCA has demonstrated an ability to obtain good correction of the coronal curve and apical derotation, with better sagittal profile restoration and with lower complication rate in the correction of AdIS. We utilized the SRS-20 scores, which has been used in previous literature as an effective tool in quantifying the improvements of HRQoL in AdIS [19], and the mean questionnaire scores for function, pain, general self-image, mental health of the patients in this study were greatly improved at last follow-up.
Several limitations exist in the current study, such as the lack of control groups, small number of patients, and relative short follow-up period. Also, there are potentially differences in surgeons’ familiarity with the technique and variability in its execution. Thus, a long-term follow-up and controlled study is necessary, which is a project the present authors propose to carry out in the future.
In summary, the vertebral coplanar alignment (VCA) technique demonstrated its effectiveness as well as its advantage in improving the correction of main thoracic scoliosis and rotational deformities, particularly in young adult idiopathic scoliosis with thoracic hyperkyphosis or hypokyphosis.
References
Aebi M (2005) The adult scoliosis. Eur Spine J 14:925–948
Schwab FJ, Smith VA, Biserni M, Gamez L, Farcy J-PC, Pagala M (2002) Adult scoliosis: a quantitative radiographic and clinical analysis. Spine 27:387–392
Whyte Ferguson L (2014) Adult Idiopathic scoliosis: the tethered spine. J Bodywork Move Ther 18:99–111
Ascani E, Bartolozzi P, Logroscino C, Marchetti P, Ponte A, Savini R, Travaglini F, Binazzi R, Di Silvestre M (1986) Natural history of untreated idiopathic scoliosis after skeletal maturity. Spine 11:784–789
Weinstein S, Ponseti I (1983) Curve progression in idiopathic scoliosis. J Bone Joint Surg 65:447–455
Bradford DS, Tay BK, Hu SS (1999) Adult scoliosis: surgical indications, operative management, complications, and outcomes. Spine 24:2617
Liljenqvist UR, Halm HF, Link TM (1997) Pedicle screw instrumentation of the thoracic spine in idiopathic scoliosis. Spine 22:2239–2245
Qiu Y, Zhu F, Wang B, Yu Y, Zhu Z, Qian B, Sun X, Ma W (2011) Comparison of surgical outcomes of lenke type 1 idiopathic scoliosis: vertebral coplanar alignment versus derotation technique. J Spinal Disorders Tech 24:492–499
Rhee JM, Bridwell KH, Won DS, Lenke LG, Chotigavanichaya C, Hanson DS (2002) Sagittal plane analysis of adolescent idiopathic scoliosis: the effect of anterior versus posterior instrumentation. Spine 27:2350–2356. doi:10.1097/01.BRS.0000030301.48250.3D
Potter BK, Kuklo TR, Lenke LG (2005) Radiographic outcomes of anterior spinal fusion versus posterior spinal fusion with thoracic pedicle screws for treatment of Lenke Type I adolescent idiopathic scoliosis curves. Spine 30:1859–1866
Vallespir GP, Flores JB, Trigueros IS, Sierra EH, Fernández PD, Olaverri JCR, Alonso MG, Galea RR, Francisco AP, de Paz BR (2008) Vertebral coplanar alignment: a standardized technique for three dimensional correction in scoliosis surgery: technical description and preliminary results in Lenke type 1 curves. Spine 33:1588–1597
Liljenqvist UR, Allkemper T, Hackenberg L, Link TM, Steinbeck J, Halm HF (2002) Analysis of vertebral morphology in idiopathic scoliosis with use of magnetic resonance imaging and multiplanar reconstruction. The Journal of bone and joint surgery American 84:359–368
Liljenqvist UR, Link TM, Halm HF (2000) Morphometric analysis of thoracic and lumbar vertebrae in idiopathic scoliosis. Spine 25:1247–1253
Sun L, Song Y, Liu L, An Y, Zhou C, Zhou Z (2013) Bilateral apical vertebral derotation technique by vertebral column manipulation compared with vertebral coplanar alignment technique in the correction of lenke type 1 idiopathic scoliosis. BMC Musculoskeletal Disorders 14:175
Luk KD, Vidyadhara S, Lu DS, Wong YW, Cheung WY, Cheung KM (2010) Coupling between sagittal and frontal plane deformity correction in idiopathic thoracic scoliosis and its relationship with postoperative sagittal alignment. Spine 35:1158–1164. doi:10.1097/BRS.0b013e3181bb49f3
Lowe T, Berven SH, Schwab FJ, Bridwell KH (2006) The SRS classification for Adult Spinal Deformity - Building on the King/Moe and Lenke Classification Systems. Spine 31:S119–S125. doi:10.1097/01.brs.0000232709.48446.be
Lenke LG, Edwards CC, Bridwell KH (2003) The Lenke classification of adolescent idiopathic scoliosis: how it organizes curve patterns as a template to perform selective fusions of the spine. Spine 28:S199–S207
Belmont PJ Jr, Klemme WR, Robinson M, Polly DW Jr (2002) Accuracy of thoracic pedicle screws in patients with and without coronal plane spinal deformities. Spine 27:1558–1566
Cunningham ME (2012) Adult spinal deformity surgery. Curr Orthopaedic Pract 23:177–180
Martino J, Aubin CE, Labelle H, Wang X, Parent S (2013) Biomechanical analysis of vertebral derotation techniques for the surgical correction of thoracic scoliosis. A numerical study through case simulations and a sensitivity analysis. Spine 38:E73–E83. doi:10.1097/BRS.0b013e31827a641e
Mermer MJ, Boachie-Adjei O, Rawlins BA, Peskin M, Bhatnagar R (2006) Comprehensive analysis of cantilever, translational, and modular corrective techniques in adults with scoliosis treated with surgery to the sacropelvis. J Spinal Disord Tech 19:513–522. doi:10.1097/01.bsd.0000211214.36189.27
Porter RW (2001) Can a short spinal cord produce scoliosis? Eur Spine J Off Publ Eur Spine Soc European Spinal Deform Soc Eur Sect Cervical Spine Res Soc 10:2–9
Dickson JH, Mirkovic S, Noble PC, Nalty T, Erwin WD (1995) Results of operative treatment of idiopathic scoliosis in adults. J Bone Joint Surg Am 77:513–523
Ali RM, Boachie-Adjei O, Rawlins BA (2003) Functional and radiographic outcomes after surgery for adult scoliosis using third-generation instrumentation techniques. Spine 28:1163–1169. doi:10.1097/01.BRS.0000067267.04011.91 (discussion 1169–1170)
Di Silvestre M, Lolli F, Bakaloudis G, Maredi E, Vommaro F, Pastorelli F (2013) Apical vertebral derotation in the posterior treatment of adolescent idiopathic scoliosis: myth or reality? Eur Spine J 22:313–323
S-l Suk, Lee S-M, Chung E-R, Kim J-H, Kim S-S (2005) Selective thoracic fusion with segmental pedicle screw fixation in the treatment of thoracic idiopathic scoliosis: more than 5-year follow-up. Spine 30:1602–1609
Krismer M, Sterzinger W, Haid C, Frischhut B, Bauer R (1996) Axial rotation measurement of scoliotic vertebrae by means of computed tomography scans. Spine 21:576–581. doi:10.1097/00007632-199603010-00009
Lee SM, Suk SI, Chung ER (2004) Direct vertebral rotation: a new technique of three-dimensional deformity correction with segmental pedicle screw fixation in adolescent idiopathic scoliosis. Spine 29:343–349. doi:10.1097/01.Brs.0000109991.88149.19
Kuklo TR, Potter BK, Lenke LG (2005) Vertebral rotation and thoracic torsion in adolescent idiopathic scoliosis: what is the best radiographic correlate? J Spinal Disord Tech 18:139–147
Krismer M, Bauer R, Sterzinger W (1992) Scoliosis correction by Cotrel-Dubousset instrumentation. The effect of derotation and three dimensional correction. Spine 17:S263–S269
Steib JP, Dumas R, Mitton D, Skalli W (2004) Surgical correction of scoliosis by in situ contouring: a detorsion analysis. Spine 29:193–199. doi:10.1097/01.BRS.0000107233.99835.A4
Lee SM, Suk SI, Chung ER (2004) Direct vertebral rotation: a new technique of three-dimensional deformity correction with segmental pedicle screw fixation in adolescent idiopathic scoliosis. Spine 29:343–349
Mattila M, Jalanko T, Helenius I (2013) En bloc vertebral column derotation provides spinal derotation but no additional effect on thoracic rib hump correction as compared with no derotation in adolescents undergoing surgery for idiopathic scoliosis with total pedicle screw instrumentation. Spine 38:1576–1583
Rushton PR, Grevitt MP (2014) Do vertebral derotation techniques offer better outcomes compared to traditional methods in the surgical treatment of adolescent idiopathic scoliosis? Eur Spine J Off Pub Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cervical Spine Res Soc 23:1166–1176. doi:10.1007/s00586-014-3242-x
Roussouly P, Labelle H, Rouissi J, Bodin A (2013) Pre- and post-operative sagittal balance in idiopathic scoliosis: a comparison over the ages of two cohorts of 132 adolescents and 52 adults. Eur Spine J Off Pub Eur Spine Soc Eur Spinal Deform Soc Eur Sect Cervical Spine Res Soc 22(Suppl 2):S203–S215. doi:10.1007/s00586-012-2571-x
Acknowledgments
National Public Health Benefit Research foundation, China (Grant No. 201002018), funds were received in support of this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We declare that we have no actual or potential conflict of interest in relation to this article. No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Rights and permissions
About this article
Cite this article
He, S., Bao, H., Zhu, Z. et al. Vertebral coplanar alignment technique: a surgical option for correction of adult thoracic idiopathic scoliosis. Eur Spine J 25, 417–423 (2016). https://doi.org/10.1007/s00586-015-4080-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-4080-1