Abstract
Purpose
It has been shown in previous studies that nitrous oxide (N2O) suppresses the amplitude of motor evoked potentials (MEPs) in individual subjects. In the present study, we compared the absolute amplitude and latency of MEPs among groups of patients with various concentrations of N2O.
Methods
The subjects were 60 patients who were scheduled to undergo craniotomy with MEP monitoring. Anesthesia was induced and maintained with propofol and fentanyl. The patients were randomly assigned to one of three groups based on the concentration of N2O: 0% N2O (N0 group), 50% N2O (N50 group), and 66% N2O (N66 group). MEPs were elicited by transcranial electrical stimulation. The effect-site concentrations (ESCs) of anesthetics were calculated retrospectively. The effects of anesthetics on MEP were analyzed by analysis of covariance (ANCOVA) followed by Tukey’s method.
Results
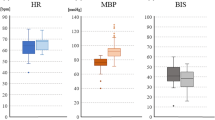
MEPs were elicited in all cases. The absolute amplitude of the MEP was significantly higher in the N0 group than in the N50 and N66 groups [4.16 ± 0.42 vs 1.00 ± 0.26 mV and 1.00 ± 0.27 mV, respectively (mean ± SD); P < 0.05]. In contrast, there was no significant difference in the latency of the MEP among the three groups of subjects (N0: 16.64 ± 0.72, N50: 16.78 ± 0.66, and N66: 16.82 ± 0.63 ms).
Conclusion
The results suggest that N2O can suppress the absolute amplitude of the MEP in patients under propofol and fentanyl anesthesia. Although monitoring of MEP as a trend is feasible even if N2O is used, the use of N2O may be better avoided.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Author information
Authors and Affiliations
Additional information
This paper was presented in part at the annual meeting of the American Society of Anesthesiologists, Orlando, Florida, USA, on October 12–16, 2002.
About this article
Cite this article
Kunisawa, T., Nagata, O., Nomura, M. et al. A comparison of the absolute amplitude of motor evoked potentials among groups of patients with various concentrations of nitrous oxide. J Anesth 18, 181–184 (2004). https://doi.org/10.1007/s00540-004-0245-5
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00540-004-0245-5