Abstract
Background
Endoscopic management of hepaticojejunostomy anastomotic strictures is technically demanding due to surgically altered anatomy. The promise of double-balloon endoscope-assisted endoscopic retrograde cholangiopancreatography (DB-ERCP) has been reported in this setting. No large study has examined long-term outcomes of this new treatment modality and predictive factors for the stricture resolution.
Methods
We included 102 patients who received DB-ERCP for a hepaticojejunostomy anastomotic stricture between 2008 and 2018. Balloon dilation was performed as a first-line treatment, and plastic stent(s) were placed for refractory cases. Potential predictive factors for the stricture resolution were examined using multivariable logistic regression analyses.
Results
DB-ERCP was technically successful in 91 patients (89.2%). Overall, stricture resolution was achieved in 70 patients (76.9%) with a median follow-up period of 30.9 months (range 1–118.5 months). Among 64 patients (71.9%) who underwent successful re-canalization via balloon dilation, anastomotic stricture recurred in 22 patients (34.4%). In cases with refractory or recurrent stricture after balloon dilation, 20 patients (52.6%) underwent stricture resolution via plastic stent placement, and the recurrence was observed in two patients (10%). Post-operative time to DB-ERCP of > 12 months and the scar-like appearance around the anastomosis were associated with a higher rate of stricture resolution (odds ratios, 5.59 [95% CI 1.69–18.5] and 5.22 [95% CI 1.29–21.1], respectively).
Conclusions
Treatment of hepaticojejunostomy anastomotic strictures via DB-ERCP was technically feasible, providing a reasonably high rate of stricture resolution. Alternative treatment should be explored for refractory cases.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Hepaticojejunostomy is conducted as a means of bilioenteric anastomosis for patients who receive surgical procedures involving the extrahepatic bile duct (e.g., pancreaticoduodenectomy, extended hepatectomy). An anastomotic stricture has been a clinically relevant adverse event of hepaticojejunostomy, which has been reported to occur in 3–13% of patients and associated with significant morbidities and a high mortality rate [1,2,3,4,5]. Surgically altered anatomy (e.g., Roux-en-Y and Billroth-II reconstructions) associated with hepaticojejunostomy has compromised endoscopic approach to the biliary system [6]. Therefore, hepaticojejunostomy anastomotic strictures were conventionally managed via percutaneous transhepatic biliary drainage (PTBD) or surgical re-anastomosis [7,8,9,10,11,12,13].
The double-balloon endoscope (DBE) was initially developed for investigations of the small intestine [14], and a short-type DBE has opened new opportunities to perform non-surgical pancreatobiliary interventions with a high technical success rate [15,16,17]. In the setting of hepaticojejunostomy anastomotic strictures, several clinical studies suggested the feasibility of balloon dilation and placement of multiple plastic stents via DBE-assisted ERCP (DB-ERCP) and a high rate of the short-time stricture resolution ranging 70–100% [18,19,20]; however, there is the paucity of large cohort studies on the topic. In addition, few studies have reported long-term outcomes of DB-ERCP for hepaticojejunostomy anastomotic strictures, and predictive factors for successful endoscopic management remain unclear.
In this retrospective study at a high-volume center, we aimed to evaluate clinical outcomes of DB-ERCP for hepaticojejunostomy anastomotic strictures and identify predictive factors for long-term treatment success.
Materials and methods
Study design
We conducted a single-center retrospective observational study to examine long-term treatment outcomes of DB-ERCP for a hepaticojejunostomy anastomotic stricture and predictive factors for stricture resolution. We included patients who were diagnosed with a hepaticojejunostomy anastomotic stricture and received DB-ERCP between May 2008 and February 2018. As endoscopic treatment procedures, we evaluated balloon dilation and plastic stent placement. The primary study outcome was the resolution of the anastomotic stricture. Technical success, recurrence of an anastomotic stricture, adverse events, and predictive factors for the resolution of the stricture were examined as secondary outcomes.
Written informed consent was obtained from each patient before the procedure. The study was conducted in accordance with the Declaration of Helsinki and was approved by the ethics committee at the hospital.
Endoscopic procedures and patient follow-up
DB-ERCP procedures were carried, as previously described [15,16,17]. A short DBE (EC-450BI5/EI-530B with a 2.8-mm-wide working channel; or EI-580BT, developed recently with a 3.2-mm-wide working channel; Fujifilm, Tokyo, Japan) was inserted. Biliary cannulation through the stricture was attempted via a contrast-assisted or wire-guided method using a straight cannula and a 0.035- or 0.025-inch hydrophilic guidewire. In cases with severe stricture, a tapered-metal-tip cannula (PR-132Q; Olympus, Tokyo, Japan) and a 0.018-inch hydrophilic guidewire were used. When biliary cannulation was achieved, the guidewire was replaced with a 0.025-inch stiff guidewire. The stricture was dilated using a balloon catheter (Hurricane RX, Boston Scientific Japan, Tokyo, Japan; REN, Kaneka Medix Corp., Osaka, Japan; or ZARA, Century Medical, Tokyo, Japan) at 6–8 atmospheres for 1 min (Fig. 1). In cases where the stricture was not resolved, 5-F or 7-F plastic stent(s) were deployed across the stricture (Fig. 2). Biliary stones, if present, were removed using a basket or balloon catheter.
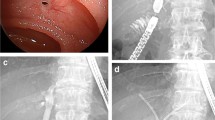
Balloon dilation of a hepaticojejunostomy anastomotic stricture using a double-balloon endoscope. A Cholangiogram delineating a hepaticojejunostomy anastomotic stricture and intrahepatic stones in the left hepatic duct. B Balloon dilation of the hepaticojejunostomy anastomotic stricture. C Balloon-occluded cholangiogram suggesting resolution of the anastomotic stricture. D Endoscopic image of the hepaticojejunostomy anastomotic stricture with scar-like appearance around the anastomosis site. E Endoscopic image after balloon dilation showing fully dilated hepaticojejunostomy anastomosis. F Endoscopic image of extraction of intrahepatic stones by a basket catheter
Plastic stent placement for a hepaticojejunostomy anastomotic stricture using a double-balloon endoscope. A Cholangiogram delineating a hepaticojejunostomy anastomotic stricture. B Two plastic stents placed across the anastomotic stricture after balloon dilation. C Endoscopic image showing the hepaticojejunostomy anastomotic stricture with biliary sludge. D Endoscopic image of two plastic stents placed across the hepaticojejunostomy anastomosis. E Endoscopic image showing fully dilated hepaticojejunostomy anastomosis after plastic stent placement for 3 months
Patients visited our outpatient clinic every month, and underwent a physical examination and a blood test including hepatobiliary enzymes. If there were signs suggesting cholangitis or cholestasis, abdominal ultrasonography and computed tomography were performed along with/without magnetic resonance cholangiopancreatography (MRCP). Plastic stents were exchanged endoscopically every 3–4 months. In each DB-ERCP procedure, the anastomotic stricture was evaluated on endoscopic and fluoroscopic views, and stent placement was not performed when the stricture was considered resolved.
Definitions of outcome variables
Resolution of an anastomotic stricture was defined when (1) the anastomosis was considered sufficiently dilated on endoscopic and fluoroscopic views, (2) an inflated extraction balloon catheter passed the anastomosis smoothly without resistance, (3) contrast in the bile duct readily flowed into the jejunum, and (4) no additional intervention was required during the index hospitalization. Recurrence of the anastomotic stricture was defined as elevated liver enzymes or cholangitis with images showing the bile duct dilatation which required an endoscopic, percutaneous, or surgical re-intervention. Technical success was defined as achievement of balloon dilation or plastic stent placement across the stricture via DB-ERCP. Small opening of the hepaticojejunostomy anastomosis was defined when a 1.6-mm-wide ERCP cannula could not pass the stricture. The length of the anastomotic stricture was measured from the distal end of the bile duct delineated fluoroscopically to the jejunum. The scar-like appearance was defined when an endoscopic view showed whitish cicatricial mucosal change around the anastomosis (Fig. 3). Adverse events were diagnosed according to the lexicon [21].
Statistical analysis
The Fisher’s exact test and Student’s t test or Wilcoxon rank-sum test were used to compare categorical and continuous variables between the groups, respectively. Logistic regression analyses were performed to compute odds ratios (ORs) for the resolution of the anastomotic stricture and corresponding 95% confidence intervals (CIs). We entered potential predictive factors for the anastomotic stricture resolution with a P value of < 0.15 in a univariable analysis into a multivariable model. Time to biliary stricture recurrence was estimated by the Kaplan–Meier product-limit method. In Kaplan–Meier analyses, patients who lost to follow-up were dealt as censored cases.
All P values were two-sided, and P values of < 0.05 were considered statistically significant. All statistical analyses were performed using the EZR software (Saitama Medical Center, Jichi Medical University, Saitama, Japan), which is a graphical user interface for the R software (The R Foundation for Statistical Computing, Vienna, Austria, version 3.2.2) [22].
Results
We included 102 patients who underwent DB-ERCP as treatment of a hepaticojejunostomy anastomotic stricture during 9.8-year study period (Fig. 4 and Supplementary Fig. 1). Table 1 and Supplementary Table 1 summarize clinical characteristics of the study population, overall and by the presence of biliary stricture resolution, respectively. The median time between hepaticojejunostomy and DB-ERCP was 2.2 years (range 0.2–46.4 years; interquartile range 0.6–7.7 years). The procedures of DB-ERCP for the hepaticojejunostomy anastomotic stricture are summarized in Table 2.
The treatment via DB-ERCP was technically successful in 91 patients (technical success rate, 89.2%). For two patients, the endoscopic ultrasound-guided or percutaneous transhepatic rendezvous technique was utilized for biliary access. Overall, the resolution of an anastomotic stricture was achieved in 70 patients (76.9%) with the median follow-up period of 2.7 years (range 0.1–9.7 years). Among 89 patients treated by balloon dilation, the anastomotic stricture was successfully resolved in 64 patients (71.9%). Plastic stent(s) were placed for a total of 38 patients including 27 patients who received plastic stent placement at the initial session and 11 patients who underwent stricture recurrence after successful balloon dilation. The numbers of plastic stents placed were 1, 2, and 3 in 5 (13.2%), 32 (84.2%), and 1 (2.6%) patients, respectively. The resolution of a hepaticojejunostomy anastomotic stricture via plastic stent placement was achieved in 18 (47.4%) patients with the median duration of stent placement of 5.6 months (range 1–29.6 months) and the median number of DB-ERCP sessions of 2 (range 1–10). After failed re-canalization via plastic stent placement, PTBD and surgical re-anastomosis were performed to manage cholangitis in four and one patients, respectively. Procedure-related adverse events were observed in 18 patients (17.6%): cholangitis in 10 patients (9.8%), intra-abdominal and/or retroperitoneal air in 6 (5.9%), bile leakage in 1 (1%), and bleeding in 1 (1%). No severe adverse events were observed. All cases with adverse events were managed conservatively.
Figure 5 illustrates the cumulative recurrence rate of the hepaticojejunostomy anastomotic stricture after successful balloon dilation. Among 53 patients who underwent initial successful balloon dilation and were followed up for more than 12 months, a stricture recurrence was observed in 22 patients (41.5%) with the median time to recurrence of 3.4 months (range 1–36.2 months). The cumulative recurrence rate at 12 months was 35.8%. The recurrent stricture was noted within 1 year of balloon dilation in a vast majority of the cases. Among patients treated with plastic stent placement, two patients (10%) experienced a stricture recurrence at 8.0 and 12.3 months of stent removal.
When we focused on 80 patients with Roux-en-Y reconstruction (Supplementary Tables 2 and 3), the procedure time was significantly longer in patients with Roux-en-Y reconstruction than in those with Billroth-II reconstruction (median 72 min [range 15–240 min] vs. 52 min [range 19–90 min], respectively; P = 0.001). In 28 patients with Roux-en-Y reconstruction and available data on previous surgical procedures, the length of an afferent loop was 40 cm (range 30–50 cm). Biliary cannulation and technical success were achieved in 91.3% and 87.5% patients, respectively. Overall, the resolution of an anastomotic stricture was achieved in 56 patients (70%) with the median follow-up period of 2.7 years (range 0.1–9.7 years). The resolution of an anastomotic stricture was achieved by balloon dilation alone in 42 patients (52.5%) and by plastic stent placement following balloon dilation in 14 patients (17.5%). Supplementary Fig. 2 illustrates the cumulative recurrence rate of the hepaticojejunostomy anastomotic stricture after successful balloon dilation among patients with Roux-en-Y reconstruction.
We examined predictive factors for anastomotic stricture resolution via endoscopic treatment (balloon dilation with/without plastic stent placement) using logistic regression analyses (Table 3). In the multivariable analysis, time to DB-ERCP of > 12 months (OR 5.59; 95% CI 1.69–18.5), and the scar-like appearance (OR 5.22; 95% CI 1.29–21.1) were positively associated with the resolution. When we entered the time to DB-ERCP as a continuous variable in a multivariable model considering the potential effect of an arbitrary cut-off value, an increase in the time was associated with a high likelihood of the stricture resolution (P = 0.039). When examining associations of biliary stricture resolution with balloon dilation and plastic stent placement separately, time to DB-ERCP of > 12 months was associated with the resolution via balloon dilation (Supplementary Table 4). Male sex and the scar-like appearance were associated with the resolution via plastic stents (Supplementary Table 5). However, the statistical power was limited in these subgroup analyses.
Discussion
In this retrospective study involving the largest sample of patients in this field, the technical success of DB-ERCP for a hepaticojejunostomy anastomotic stricture was achieved in a majority of patients. Using balloon dilation and plastic stents, the stricture resolution was observed in up to 75% of the study population. In our risk-factor analysis, longer post-operative period and the scar-like appearance on the endoscopic view were preferably associated with the stricture resolution.
The emerging DB-ERCP has enabled endoscopic pancreatobiliary interventions that were traditionally performed using a duodenoscope for patients with normal upper gastrointestinal anatomy. For patients with a hepaticojejunostomy anastomotic stricture, the feasibility of balloon dilation followed by plastic stent placement has been documented in several retrospective studies [18,19,20] (Table 4). The dilation of the anastomotic stricture using a balloon catheter has been generally performed as a first-choice treatment option and associated with a high rate of short-term stricture resolution of 78–100% [18, 20]. However, the stricture recurrence rate during the follow-up period was reported to be as high as 50–71%. Placing plastic stent(s) might provide additional effects on prolongation of the anastomosis patency; however, there are only limited data on this treatment strategy [19]. In line with the prior studies, our study supports the technical feasibility of balloon dilation for a hepaticojejunostomy anastomotic stricture, and more than one-third patients experienced recurrent strictures, half of which were resolved by prolonged placement of plastic stents.
Our findings of predictive factors for the resolution of a hepaticojejunostomy anastomotic stricture via DB-ERCP may have clinical relevance. In the current study, patients with shorter post-operative time or those without the scar-like appearance were more likely to be refractory to endoscopic treatment. The scar-like appearance may implicate that the intestinal mucosa surrounding the anastomosis does not have active inflammatory changes due to the surgery or host factors, and thus, be susceptible to the mechanical dilation. Similarly, patients with prolonged post-operative time may be amenable to the endoscopic therapy. Therefore, alternative strategies should be established for this subset of patients with a hepaticojejunostomy anastomotic stricture. Clinical studies suggest the effectiveness of a covered self-expandable metal stent (SEMS) for benign biliary strictures including strictures after liver transplantation or those due to chronic pancreatitis [23,24,25,26,27]. Although the SEMS would reportedly decrease the number of ERCP sessions as well as the length of endoscopic treatment, the use of SEMS might also increase cost effectiveness. The usefulness and cost effectiveness should be further evaluated in those with benign biliary strictures in patients with surgically altered anatomy. An electrocautery dilation catheter or local steroid injection might be considered as an additional option to improve clinical outcomes of DB-ERCP for a hepaticojejunostomy anastomotic stricture [28,29,30].
We acknowledge limitations in the current study. A retrospective observational study design in a single center is a limitation, i.e., there might be a treatment selection bias. Similarly, the criteria for placement and removal of plastic stents were not strictly pre-defined. Nonetheless, using our prospectively maintained endoscopy database, we included consecutive patients who received DB-ERCP for a hepaticojejunostomy anastomotic stricture. Furthermore, our relatively large sample size and long follow-up duration allowed us to evaluate predictive factors for the stricture resolution (or recurrence).
In conclusion, endoscopic treatment utilizing balloon dilatation combined with plastic stent placement appeared to be a safe and effective treatment strategy for hepaticojejunostomy anastomotic strictures. Given a prolonged period of stent placement and a large number of DB-ERCP procedures, investigations of alternative modalities should be designed targeting the population who are likely to be refractory to balloon dilation and/or plastic stent placement.
References
House MG, Cameron JL, Schulick RD, Campbell KA, Sauter PK, Coleman J, Lillemoe KD, Yeo CJ (2006) Incidence and outcome of biliary strictures after pancreaticoduodenectomy. Ann Surg 243:571–576 (discussion 576-578)
Reid-Lombardo KM, Ramos-De la Medina A, Thomsen K, Harmsen WS, Farnell MB (2007) Long-term anastomotic complications after pancreaticoduodenectomy for benign diseases. J Gastrointest Surg 11:1704–1711
Dimou FM, Adhikari D, Mehta HB, Olino K, Riall TS, Brown KM (2016) Incidence of hepaticojejunostomy stricture after hepaticojejunostomy. Surgery 160:691–698
Asano T, Natsume S, Senda Y, Sano T, Matsuo K, Kodera Y, Hara K, Ito S, Yamao K, Shimizu Y (2016) Incidence and risk factors for anastomotic stenosis of continuous hepaticojejunostomy after pancreaticoduodenectomy. J Hepatobiliary Pancreat Sci 23:628–635
Booij KAC, Coelen RJ, de Reuver PR, Besselink MG, van Delden OM, Rauws EA, Busch OR, van Gulik TM, Gouma DJ (2018) Long-term follow-up and risk factors for strictures after hepaticojejunostomy for bile duct injury: an analysis of surgical and percutaneous treatment in a tertiary center. Surgery 163:1121–1127
Feitoza AB, Baron TH (2002) Endoscopy and ERCP in the setting of previous upper GI tract surgery. Part II: postsurgical anatomy with alteration of the pancreaticobiliary tree. Gastrointest Endosc 55:75–79
Schumacher B, Othman T, Jansen M, Preiss C, Neuhaus H (2001) Long-term follow-up of percutaneous transhepatic therapy (PTT) in patients with definite benign anastomotic strictures after hepaticojejunostomy. Endoscopy 33:409–415
Kim JH, Lee SK, Kim MH, Song MH, Park DH, Kim SY, Lee SS, Seo DW, Bae JS, Kim HJ, Han J, Sung KB, Min YI (2003) Percutaneous transhepatic cholangioscopic treatment of patients with benign bilio-enteric anastomotic strictures. Gastrointest Endosc 58:733–738
Glas L, Courbiere M, Ficarelli S, Milot L, Mennesson N, Pilleul F (2008) Long-term outcome of percutaneous transhepatic therapy for benign bilioenteric anastomotic strictures. J Vasc Interv Radiol 19:1336–1343
Cantwell CP, Pena CS, Gervais DA, Hahn PF, Dawson SL, Mueller PR (2008) Thirty years’ experience with balloon dilation of benign postoperative biliary strictures: long-term outcomes. Radiology 249:1050–1057
Weber A, Rosca B, Neu B, Rosch T, Frimberger E, Born P, Schmid RM, Prinz C (2009) Long-term follow-up of percutaneous transhepatic biliary drainage (PTBD) in patients with benign bilioenterostomy stricture. Endoscopy 41:323–328
Saad WE, Wallace MJ, Wojak JC, Kundu S, Cardella JF (2010) Quality improvement guidelines for percutaneous transhepatic cholangiography, biliary drainage, and percutaneous cholecystostomy. J Vasc Interv Radiol 21:789–795
Bonnel DH, Fingerhut AL (2012) Percutaneous transhepatic balloon dilatation of benign bilioenteric strictures: long-term results in 110 patients. Am J Surg 203:675–683
Yamamoto H, Sekine Y, Sato Y, Higashizawa T, Miyata T, Iino S, Ido K, Sugano K (2001) Total enteroscopy with a nonsurgical steerable double-balloon method. Gastrointest Endosc 53:216–220
Tsujino T, Yamada A, Isayama H, Kogure H, Sasahira N, Hirano K, Tada M, Kawabe T, Omata M (2010) Experiences of biliary interventions using short double-balloon enteroscopy in patients with Roux-en-Y anastomosis or hepaticojejunostomy. Dig Endosc 22:211–216
Shimatani M, Hatanaka H, Kogure H, Tsutsumi K, Kawashima H, Hanada K, Matsuda T, Fujita T, Takaoka M, Yano T, Yamada A, Kato H, Okazaki K, Yamamoto H, Ishikawa H, Sugano K (2016) Diagnostic and therapeutic endoscopic retrograde cholangiography using a short-type double-balloon endoscope in patients with altered gastrointestinal anatomy: a multicenter prospective study in Japan. Am J Gastroenterol 111:1750–1758
Yamada A, Kogure H, Nakai Y, Takahara N, Mizuno S, Tada M, Koike K (2019) Performance of a new short-type double-balloon endoscope with advanced force transmission and adaptive bending for pancreaticobiliary intervention in patients with surgically altered anatomy: a propensity-matched analysis. Dig Endosc 31:86–93
Kamei H, Imai H, Onishi Y, Ishihara M, Nakamura M, Kawashima H, Ishigami M, Ito A, Ohmiya N, Hirooka Y, Goto H, Ogura Y (2015) Considerable risk of restenosis after endoscopic treatment for hepaticojejunostomy stricture after living-donor liver transplantation. Transplant Proc 47:2493–2498
Tomoda T, Tsutsumi K, Kato H, Mizukawa S, Yabe S, Akimoto Y, Seki H, Uchida D, Matsumoto K, Yamamoto N, Horiguchi S, Okada H (2016) Outcomes of management for biliary stricture after living donor liver transplantation with hepaticojejunostomy using short-type double-balloon enteroscopy. Surg Endosc 30:5338–5344
Mizukawa S, Tsutsumi K, Kato H, Muro S, Akimoto Y, Uchida D, Matsumoto K, Tomoda T, Horiguchi S, Okada H (2018) Endoscopic balloon dilatation for benign hepaticojejunostomy anastomotic stricture using short double-balloon enteroscopy in patients with a prior Whipple’s procedure: a retrospective study. BMC Gastroenterol 18:14
Cotton PB, Eisen GM, Aabakken L, Baron TH, Hutter MM, Jacobson BC, Mergener K, Nemcek A Jr, Petersen BT, Petrini JL, Pike IM, Rabeneck L, Romagnuolo J, Vargo JJ (2010) A lexicon for endoscopic adverse events: report of an ASGE workshop. Gastrointest Endosc 71:446–454
Kanda Y (2013) Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant 48:452–458
Kaffes A, Griffin S, Vaughan R, James M, Chua T, Tee H, Dinesen L, Corte C, Gill R (2014) A randomized trial of a fully covered self-expandable metallic stent versus plastic stents in anastomotic biliary strictures after liver transplantation. Therap Adv Gastroenterol 7:64–71
Haapamäki C, Kylänpää L, Udd M, Lindström O, Grönroos J, Saarela A, Mustonen H, Halttunen J (2015) Randomized multicenter study of multiple plastic stents vs. covered self-expandable metallic stent in the treatment of biliary stricture in chronic pancreatitis. Endoscopy 47:605–610
Coté GA, Slivka A, Tarnasky P, Mullady DK, Elmunzer BJ, Elta G, Fogel E, Lehman G, McHenry L, Romagnuolo J, Menon S, Siddiqui UD, Watkins J, Lynch S, Denski C, Xu H, Sherman S (2016) Effect of covered metallic stents compared with plastic stents on benign biliary stricture resolution: a randomized clinical trial. JAMA 315:1250–1257
Martins FP, De Paulo GA, Contini MLC, Ferrari AP (2018) Metal versus plastic stents for anastomotic biliary strictures after liver transplantation: a randomized controlled trial. Gastrointest Endosc 87:131.e131-131.e113
Tal AO, Finkelmeier F, Filmann N, Kylanpaa L, Udd M, Parzanese I, Cantu P, Dechene A, Penndorf V, Schnitzbauer A, Friedrich-Rust M, Zeuzem S, Albert JG (2017) Multiple plastic stents versus covered metal stent for treatment of anastomotic biliary strictures after liver transplantation: a prospective, randomized, multicenter trial. Gastrointest Endosc 86:1038–1045
Gao DJ, Hu B, Pan YM, Wang TT, Wu J, Lu R, Wang SP, Shi ZM, Huang H, Wang SZ (2013) Feasibility of using wire-guided needle-knife electrocautery for refractory biliary and pancreatic strictures. Gastrointest Endosc 77:752–758
Yang YL, Zhang C, Zhao G, Wu P, Ma YF, Zhang HW, Shi LJ, Li JY, Lin MJ, Yang SM, Lv Y (2015) Choledochoscopic high-frequency needle-knife electrotomy as an effective treatment for intrahepatic biliary strictures. J Gastroenterol Hepatol 30:1438–1443
Franzini T, Moura R, Rodela G, Andraus W, Herman P, D’Albuquerque L, de Moura E (2015) A novel approach in benign biliary stricture—balloon dilation combined with cholangioscopy-guided steroid injection. Endoscopy 47(Suppl 1):E571–E572
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Drs. Tatsuya Sato, Hirofumi Kogure, Yousuke Nakai, Kazunaga Ishigaki, Ryunosuke Hakuta, Kei Saito, Tomotaka Saito, Naminatsu Takahara, Tsuyoshi Hamada, Suguru Mizuno, Atsuo Yamada, Minoru Tada, Hiroyuki Isayama, and Kazuhiko Koike have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Sato, T., Kogure, H., Nakai, Y. et al. Double-balloon endoscopy-assisted treatment of hepaticojejunostomy anastomotic strictures and predictive factors for treatment success. Surg Endosc 34, 1612–1620 (2020). https://doi.org/10.1007/s00464-019-06924-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-06924-6