Abstract
Background
Pediatric esophageal stenosis can be challenging to manage due to post-dilation tissue response involving fibroblast activity resulting in scar reformation. The functional lumen imaging probe (FLIP) uses high-resolution impedance planimetry to measure key luminal parameters during a volume-controlled distension. We sought to evaluate the safety as well as possible settings of EndoFLIP and EsoFLIP in the pediatric population.
Method
We performed a retrospective chart review of all patients that had EndoFLIP (with and without balloon dilation) or EsoFLIP done between July 2017 and May 2018.
Results
Eighteen patients were identified and 19 FLIP procedures were performed during esophagogastroduodenoscopy (10 EndoFLIP, 6 EndoFLIP + traditional balloon dilation, 3 EsoFLIP). Median age for the population was 13.7 years. Dysphagia was the most common chief complaint prior to endoscopic intervention. EndoFLIP measurements were most commonly taken at 20 ml and/or 30 ml of infusion. Diameter, compliance, cross-sectional area, and distensibility index were similar between infusion volumes. Median procedure time of the EndoFLIP + traditional balloon dilation group was longer (60.5 min) than the median procedure time of the EsoFLIP group (35 min, p = 0.12). Median fluoroscopy time of the EndoFLIP + traditional balloon dilation group was 0.6 min and the median fluoroscopy time of the EsoFLIP group was 0.5 min (p = 0.79). EndoFLIP + traditional balloon dilation was associated with a smaller diameter increase compared to EsoFLIP (2.2 mm vs. 4 mm; p = 0.09). There were no complications.
Conclusion
Functional lumen imaging probe (FLIP) can safely provide important luminal measurements in pediatric patients with esophageal stenosis, and may guide therapy. Esophageal dilation using EsoFLIP may yield a larger diameter change and may potentially reduce procedure time when compared to traditional balloon dilation. Pediatric patients with epidermolysis bullosa and esophageal stenosis responded well to EsoFLIP dilation.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Pediatric esophageal stenosis is the consequence of many conditions and can be associated with substantial morbidity. Causes include repaired congenital conditions (i.e.,: esophageal atresia and tracheoesophageal fistula) as well as acquired conditions such as eosinophilic esophagitis, caustic injury, genetic disorders, and peptic disease [1,2,3,4,5,6]. Most conditions are associated with fibrosis formation, which leads to luminal narrowing and symptoms such as difficulty in swallowing, chest pain, sore throat, and cough. After dilation procedures, there is increased fibroblast activity, which may result in scar reformation and luminal narrowing. Various endoscopic techniques and medical adjuncts have been used to manage esophageal stenosis, but the current mainstays are balloon dilation and mechanical dilation performed during esophagogastroduodenoscopy (EGD). Newer tools include esophageal stenting as well as electrocautery incisional therapy [7, 8].
Although these tools yield a therapeutic effect, none accurately provide details regarding the actual effect of the intervention on the diameter, cross-sectional area, compliance, pressure, or distensibility of the GI lumen. Present tools require that the endoscopist rely on a combination of endoscopic landmarks, fluoroscopy, and the comparative relationship between the area of narrowing and the endoscopic tool employed to estimate the pre- and post-intervention luminal parameters and to guide treatment. For example, the physician may subjectively use the size of the gastroscope and whether or not there is appreciable resistance as the gastroscope transverses through a narrowed segment to gauge the dimensions of the esophageal narrowing. When balloon dilation is performed, it is typically done with fluoroscopy to guide placement of the balloon device and to confirm that the narrowed region, or “waist,” has been eliminated. Although visually helpful, this form of endoscopic assessment is imprecise and potentially misleading. Moreover, there are other important luminal characteristics (such as the distensibility and compliance) that we cannot infer with our naked eyes yet these parameters may help determine not only if therapy is needed but also how much. Having these additional parameters clarifies the degree of stiffness at the area of narrowing before and after therapeutic intervention which better characterizes the therapeutic response.
Functional lumen imaging probe (FLIP) is an endoscopic tool that measures pressure–geometry relationships of GI luminal space [9]. It is a cylinder-shaped balloon with a 16-sensor catheter inside that measures electrical voltage between neighboring sensors [10]. It provides a number of luminal parameters including diameter, compliance, cross-sectional area (CSA), pressure, and distensibility index (a calculated value which equals the smallest CSA divided by the median pressure required to maintain the smallest CSA) [10]. The data are generated dynamically and displayed pictorially on a dedicated screen with the numerical measurements. Diseases where FLIP has been employed include esophageal stenosis, reflux esophagitis, eosinophilic esophagitis, gastroparesis, anal sphincter disease, achalasia, and it has also been used in peroral endoscopic myotomy [11,12,13,14,15].
There are two versions of the FLIP tool, EndoFLIP and EsoFLIP (Medtronic, Minneapolis, MN). EndoFLIP is a soft balloon tool that is used solely for geometric measurements and, for example, it can be used before and after intervention to confirm effective treatment. EsoFLIP uses a stiffer balloon analogous to a controlled radial expansion (CRE) dilation balloon. Although EsoFLIP can only measure the diameter and cross-sectional area of the narrowing, it can also dilate the narrowing itself while informing the user of the exact diameter and cross-sectional area changes in real time.
Little is known about the potential utility of FLIP in the pediatric population and there is currently no standardized protocol for its use in children. There was one published pediatric manuscript that looked at the utility of EndoFLIP in children with eosinophilic esophagitis [13]. Taylor et al. described the use of EsoFLIP to dilate a tracheoesophageal fistula-related stricture in a child [11]. There may be other GI conditions where FLIP may be useful either during the diagnostic work-up or to provide treatment. We sought to review of our single-center experience with both EndoFLIP and EsoFLIP in order to assess its safety, and to assess possible clinical settings for the pediatric population.
Materials and methods
Study design
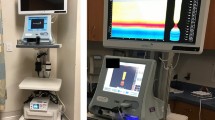
We performed a retrospective chart review of all patients under the age of 19 years who had EndoFLIP (with and without balloon dilation) or EsoFLIP between July 2017 and May 2018 at our institution (Fig. 1). EGD with either EndoFLIP or EsoFLIP was performed by a single provider (KN) at our institution. The Johns Hopkins University Internal Review Board approved this study. Medical records of the eligible patients were reviewed and information including demographics, chief complaints, procedure type, procedure length, fluoroscopy time, complication, imaging, biopsy results, and FLIP data (i.e., diameter, cross-sectional area, compliance, and distensibility index) were collected.
EndoFLIP procedure
Patients who received EndoFLIP were performed in the endoscopy unit at Johns Hopkins Children’s Center (Baltimore, MD). These patients were sedated via general anesthesia by a pediatric anesthesiologist. Propofol was typically used and no paralytic agents were utilized. Pre-study catheter calibration was performed via the FLIP computer by the endoscopy nurse per manufacturer’s guidelines. The EndoFLIP catheter was positioned under direct visualization using an Olympus (Tokyo, Japan) gastroscope at the area of interest. The FLIP computer was first programmed to infuse 15 ml of sodium chloride (0.30%) solution, provided by the manufacturer, into the balloon and the catheter was subsequently adjusted to center the balloon at the area of interest. Measurements were taken at 20 ml, 30 ml, and/or 40 ml infusion at the discretion of the endoscopist. Balloon inflation was stopped if balloon pressure exceeded 60 mmHg per manufacturer’s guidelines. If this occurred, measurements taken at the previous inflation settings were used. Luminal parameters including diameter, compliance, cross-sectional area (CSA), pressure, and distensibility index were recorded. Once all necessary measurements were recorded, the EndoFLIP balloon was then fully deflated and removed. If the area of interest appeared narrowed (i.e.,: the gastroscope was unable to pass through), balloon dilation was then performed using a CRE balloon. Once dilation was completed, the EndoFLIP balloon was reintroduced into the area of narrowing and measurements taken again following the same steps during the pre-dilation phase. Upon completion, the balloon was deflated and removed. Biopsies were taken at the discretion of the endoscopist.
EsoFLIP procedure
Those patients who received EsoFLIP were sedated via general anesthesia by a pediatric anesthesiologist similar to patients who had EndoFLIP done. Pre-study catheter calibration was performed via the FLIP computer by the endoscopy nurse per manufacturer’s guidelines. The EsoFLIP catheter was placed under direct visualization using an Olympus gastroscope at the esophageal stenotic area. The catheter was infused with 15 ml of sodium chloride (0.30%) solution and the catheter was repositioned to center the balloon at the area of interest. The balloon was inflated to 20 ml and the diameter of the stenotic area was recorded. Additional volumes were infused in 2 ml increments and the volume was held for 15–20 s increments until either effacement of the stenotic segment was achieved or there has been approximately 3 mm of change in the diameter of the stenotic area. The balloon was then deflated to 20 ml and the final measurements were taken again before the balloon was fully deflated and removed.
Statistical analysis
All statistical analyses were performed with the Statistical Package for the Social Sciences (SPSS (version 23.0, Armonk, NY). Categorical data were evaluated by the Chi-square test. Independent continuous variables were compared using the Mann–Whitney U test. Paired continuous variables were compared using the Wilcoxon Signed-Rank Test. Two-sided p values less than 0.05 were statistically significant.
Results
Patient characteristics
Our review identified 18 patients and a total of 19 FLIP cases (10 EndoFLIP, 6 EndoFLIP + traditional balloon dilation, 3 EsoFLIP) (Table 1). Median age of the entire cohort was 13.7 years. One patient was 10 months old and two patients were 11 months old at the time of the procedure. Most patients were Caucasian males. Dysphagia was the most common chief complaint. The most common diagnoses of the patients in this study were eosinophilic esophagitis, GERD, and radiographic esophageal narrowing of unclear etiology (all conditions with n = 3). All 3 dystrophic epidermolysis bullosa (EB) patients had EsoFLIP and a history of dysphagia due to proximal esophageal stenosis. Two of the three patients had prior esophageal dilations. Twelve of the 18 patients had prior EGD and 8 had prior esophageal dilations. EndoFLIP measurements were most commonly taken at 20 ml (n = 14) and 30 ml of infusion (n = 12).
Safety of FLIP
There were 16 outpatient and 3 inpatient cases. There were no complications in any of the 19 procedures. Intraoperative esophagram were done after all dilation cases and there was no contrast extravasation to suggest perforation. All families had follow-up phone calls from the hospital to confirm that there were no complications after discharge.
EndoFLIP cohort parameter comparison
Ten of the 18 patients had lower esophageal sphincter measurements using EndoFLIP without requiring dilation. Seven patients had no prior lower esophageal sphincter (LES) reconstructive surgery (“native LES”) and 3 patients had prior LES surgery (“reconstructed LES”) who had either a Heller myotomy or surgical repair of a tracheoesophageal fistula or esophageal atresia. Median age of the native LES group was 13.3 years old and the median age of the reconstructed LES group was 16.4 years old (p = 0.08).
Median procedure time between the two groups was similar between the native LES group and the reconstructed LES group (30 min vs. 28 min, p = 0.73). Six patients had measurements taken at both 20 ml and 30 ml infusions; diameter, compliance, cross-sectional area, and distensibility index were similar between groups suggesting that measurements taken at different infusions were comparable (Table 2).
Dilation cohort analysis
Two subgroups required dilation (Table 3). Six patients had EndoFLIP with traditional (CRE) balloon dilation; three EB patients had EsoFLIP dilation. Median age of the EndoFLIP + traditional balloon dilation group was 13.4 years and the median age of the EsoFLIP group was 5.4 years (p = 0.46).
The median procedure time of the EndoFLIP + traditional balloon dilation group was longer than the median procedure time of the EsoFLIP group (60.5 min vs. 35 min, p = 0.12). Median diameter change in the EndoFLIP + traditional balloon dilation group was less than the median diameter change in the EsoFLIP group (2.2 vs. 4 mm, p = 0.09). Fluoroscopy was used during all CRE balloon dilations and at the end of all dilation cases (CRE and EsoFLIP) to ensure there was no obvious perforation. Median fluoroscopy time of the EndoFLIP + traditional balloon dilation group was similar to the EsoFLIP group (p = 0.79).
Further analysis compared the EsoFLIP dilation of EB patients to their prior esophageal dilations done with either mechanical dilation or with CRE balloon dilation (traditional dilation vs. EsoFLIP). The median procedure time of the traditional dilation group (n = 4) appears longer than the EsoFLIP group (n = 3) (49 vs. 22 min, p = 0.23). The median fluoroscopy time in the traditional dilation group (n = 4) seems longer than the EsoFLIP group (n = 3, 1.17 vs. 0.5 min, p = 0.23). Fluoroscopy was not required for the EsoFLIP dilations but the endoscopist (KN) elected to use it to confirm that there was no perforation. Two of the three EB patients did not require any additional dilation after their EsoFLIP dilation and remained asymptomatic as of this report (1 year after their procedure). The third patient had 3 prior dilations over 3 months before his EsoFLIP dilation, and after the 1st EsoFLIP dilation did not require another EsoFLIP dilation for 9 months.
Discussion
This report showed that both EndoFLIP and EsoFLIP can be safely used in pediatric patients as young as infants. EndoFLIP can be utilized in native esophagus or surgically corrected esophagus, and procedure lengths are similar regardless of surgical history. Luminal measurements taken at 20 ml and 30 ml infusions appear to be comparable. Our study suggested that esophageal dilation with EsoFLIP may yield a larger diameter increase as well as shorter procedure time compared to traditional CRE balloon dilation. Our data also suggested that procedure time and fluoroscopy time were shorter in the EsoFLIP cases when compared to other traditional dilation methods in EB patients. Most importantly, two of the three EB patients have not required a repeat dilation for at least 12 month and our third EB patient with multiple previous CRE balloon dilations was symptom free for 9 months. These data suggest that there is utility of EsoFLIP in the pediatric population.
Esophageal stenosis in the pediatric population can be challenging to manage and may require multiple rounds of treatment due to scar tissue formation. We postulate that knowledge of crucial luminal parameters (such as compliance and distensibility) can better guide endoscopic interventions by helping the endoscopist decide how much dilation is needed and how much dilation has been done. This in turn may reduce scar tissue formation post intervention. FLIP provides key GI luminal values and therefore can play an important role in esophageal stenosis treatment. EsoFLIP is unique since it can provide real-time measurements (diameter and cross-sectional area) of the stenotic area before, during, and at the end of the dilation without radiation. If compliance, pressure, and/or distensibility index measurements are needed, the endoscopist needs to measure the stenotic area with EndoFLIP before and after the EsoFLIP dilation.
There is limited pediatric data on the use of FLIP and there is no standardized protocol for FLIP in children. We took measurements most commonly at 20 ml and 30 ml which correlated in terms of diameter, cross-sectional area, compliance, and distensibility index. Measurements taken at these settings were well tolerated without any complications. Since the measurements were expected to be similar with incremental volume increase, we elected to not take measurements at higher settings (i.e.,: 50 ml, 60 ml, 70 ml) to avoid extending the length of the cases. We used fluoroscopy after all dilations to confirm that there was no perforation. However, neither EsoFLIP nor EndoFLIP require fluoroscopy, which is important especially when considering their use in children.
There were limitations in this study. This was a retrospective single-center study that captures our experience with a small cohort. In our analysis, we did not measure how much time was added onto the EGD for EndoFLIP measurements in the non-dilation cases. Interestingly, the median procedure time of the first five EndoFLIP (non-dilation) cases was 32 min and the last five EndoFLIP (non-dilation) cases were 25 min, which likely reflects the learning curve using the new equipment. Our initial protocol was derived from the adult experience and higher volume measurements were taken in the earlier cases; in hindsight this approach may not have been necessary as it added to the procedural time. There is currently no published study comparing EsoFLIP against traditional dilation tools. Future directions should include a multi-center prospective study to compare the traditional dilation methods versus EsoFLIP for better generalizability. Nonetheless, this study offers new insight about new devices that enhance our understanding of GI luminal characteristics as well as a new dilation technique for pediatric patients.
Conclusion
Functional lumen imaging probe (FLIP) can safely provide important luminal measurements in pediatric patients with esophageal stenosis and in turn may help guide therapy. More studies are needed but our limited data showed that esophageal dilation using EsoFLIP may yield a larger diameter change and may potentially reduce procedure time when compared to traditional balloon dilation. EsoFLIP appears to be a reasonable alternative to traditional balloon dilation devices in pediatric patients with epidermolysis bullosa and esophageal stenosis.
Change history
25 June 2019
This article has been corrected to include the middle initial of senior author Mouen A. Khashab.
Abbreviations
- CRE:
-
Controlled radial expansion
- CSA:
-
Cross-sectional area
- EB:
-
Epidermolysis bullosa
- EGD:
-
Esophagogastroduodenoscopy
- FLIP:
-
Functional lumen imaging probe
- LES:
-
Lower esophageal sphincter
References
Menard-Katcher C, Furuta GT, Kramer RE (2017) Dilation of pediatric eosinophilic esophagitis: adverse events and short-term outcomes. J Pediatr Gastroenterol Nutr 64(5):701–706. https://doi.org/10.1097/MPG.0000000000001336
Landisch RM, Foster S, Gregg D et al (2017) Utilizing stricture indices to predict dilation of strictures after esophageal atresia repair. J Surg Res 216:172–178. https://doi.org/10.1016/j.jss.2017.04.024
Lamoria S, De A, Agarwal S, Lamba BMS, Sharma V (2016) Peptic esophageal stricture in an adolescent with Barrett’s esophagus. Int J Adolesc Med Health. https://doi.org/10.1515/ijamh-2015-0106
Gollu G, Ergun E, Ates U, Can OS, Dindar H (2017) Balloon dilatation in esophageal strictures in epidermolysis bullosa and the role of anesthesia. Dis Esophagus 30(3):1–6. https://doi.org/10.1111/dote.12503
Abreu M, Nunes I, Corujeira S, Tavares M, Trindade E, Dias JA (2016) Caustic esophageal stenosis: a case report of endoscopic dilation with a dynamic stent. GE Port J Gastroenterol 23(4):218–223. https://doi.org/10.1016/j.jpge.2015.12.006
Manfredi MA (2016) Endoscopic management of anastomotic esophageal strictures secondary to esophageal atresia. Gastrointest Endosc Clin 26(1):201–219. https://doi.org/10.1016/j.giec.2015.09.002
Manfredi MA, Jennings RW, Anjum MW, Hamilton TE, Smithers CJ, Lightdale JR (2014) Externally removable stents in the treatment of benign recalcitrant strictures and esophageal perforations in pediatric patients with esophageal atresia. Gastrointest Endosc 80(2):246–252. https://doi.org/10.1016/j.gie.2014.01.033
Manfredi MA, Clark SJ, Medford S et al (2018) Endoscopic electrocautery incisional therapy as a treatment for refractory benign pediatric esophageal strictures. J Pediatr Gastroenterol Nutr. https://doi.org/10.1097/mpg.0000000000002008
Hirano I, Pandolfino JE, Boeckxstaens GE (2017) Functional lumen imaging probe for the management of esophageal disorders: expert review from the clinical practice updates committee of the AGA institute. Clin Gastroenterol Hepatol 15(3):325–334. https://doi.org/10.1016/j.cgh.2016.10.022
Ahuja NK, Agnihotri A, Lynch KL et al (2017) Esophageal distensibility measurement: impact on clinical management and procedure length. Dis Esophagus 30(8):1–8. https://doi.org/10.1093/dote/dox038
Taylor JS, Danzer E, Berquist WE, Wall JK (2018) Dilation of esophageal stricture in a pediatric patient using functional lumen imaging probe technology without the use of fluoroscopy. J Pediatr Gastroenterol Nutr. https://doi.org/10.1097/mpg.0000000000001936
Hanna AN, Datta J, Ginzberg S, Dasher K, Ginsberg GG, Dempsey DT (2018) Laparoscopic heller myotomy versus per oral endoscopic myotomy: patient-reported outcomes at a single institution. J Am Coll Surg. https://doi.org/10.1016/j.jamcollsurg.2017.12.050
Menard-Katcher C, Benitez AJ, Pan Z et al (2017) Influence of age and eosinophilic esophagitis on esophageal distensibility in a pediatric cohort. Am J Gastroenterol 2(suppl):61. https://doi.org/10.1038/ajg.2017.131
Leroi AM, Melchior C, Charpentier C et al (2018) The diagnostic value of the functional lumen imaging probe versus high-resolution anorectal manometry in patients with fecal incontinence. Neurogastroenterol Motil 30(6):e13291. https://doi.org/10.1111/nmo.13291
Ata-Lawenko RM, Lee YY (2017) Emerging roles of the endolumenal functional lumen imaging probe in gastrointestinal motility disorders. J Neurogastroenterol Motil 23(2):164–170. https://doi.org/10.5056/jnm16171
Author information
Authors and Affiliations
Contributions
KN was the primary author of the manuscript including creation of the tables and figure. DM helped edit the manuscript, figure, and tables, providing valuable feedback to help shape the work. JH helped edit the manuscript, figure, and tables, providing valuable feedback. MK oversaw the project and also helped edit the manuscript, figure, and tables.
Corresponding author
Ethics declarations
Disclosures
Dr. Kenneth Ng is a consultant for Medtronic. Dr. Mouen A. Khashab is a consultant for Olympus, Boston Scientific, and Medtronic. Drs. Douglas Mogul and John Hollier have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article has been corrected to include the middle initial of senior author Mouen A. Khashab.
Rights and permissions
About this article
Cite this article
Ng, K., Mogul, D., Hollier, J. et al. Utility of functional lumen imaging probe in esophageal measurements and dilations: a single pediatric center experience. Surg Endosc 34, 1294–1299 (2020). https://doi.org/10.1007/s00464-019-06898-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-06898-5