Abstract
Introduction
During laparoscopic cholecystectomy (LC), common bile duct (CBD) visualization either directly or with cholangiography (IOC) is less routine. Cholangiography can be used to identify and possibly prevent bile duct injury (BDI), which is a dreaded complication of cholecystectomy. The purpose of our study was to evaluate the trend of IOC/CBD exploration and BDI during LC for benign disease.
Methods
A state-wide database (SPARCS) was used to identify all LC for benign biliary non-obstructive and obstructive disease between 2000 and 2014 in the state of New York. ICD-9 and CPT codes were used to identify IOC/CBD exploration and BDI. Multivariable logistic regression models were used in examining the linear trend in the risk of complication, 30-day readmission, 30-day ED visits, and BDI among all cholangiogram patients after controlling for possible confounding factors.
Results
During 2000–2014, 391,945 patients underwent laparoscopic cholecystectomy. The trend of IOC/CBD exploration performed significantly decreased for LC overall (12.37–10.44%, relative risk = 0.98, p <.0001) and particularly, in the outpatient setting (10.77–7.52%, relative risk = 0.96, p value <.0001). Among patients with IOC, overall complication rate, 30-day readmission rate, and 30-day ED visit rates increased. When looking at overall complication rate, there was an increase by about 4% per year (relative risk = 1.04, p value <.0001). After controlling for confounding factors, the complication risk and 30-day ED visit risk increased through years, while the 30-day readmission risk did not have significant change. Risk of BDI also increased significantly (p = 0.03).
Conclusion
In an era of laparoscopy, the rate of IOC/CBD exploration during LC has significantly decreased, while BDI significantly increased.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Since it advent in the 1980s, laparoscopic cholecystectomy has gained popularity, as it accounts for approximately 1.2 million cases/year in the United States in 2014 [1]. This procedure has been widely accepted both in the surgery community as well as the general public due to its advantages of reduced cost, diseased hospital length of stay (HLOS), and increased patient satisfaction [2,3,4]. Although it is considered a safe procedure, major morbidity occurs in approximately 5% of the patients [5].
Bile duct injury (BDI) remains a dreaded complication following laparoscopic cholecystectomy. Although its incidence has improved since laparoscopy was first introduced, studies have described an incidence of 0.08% and up to 0.5% [6, 7]. In addition, this complication has been associated with significant morbidity and mortality [8, 9]. Thus, prevention of this complication is of high importance and strategies for minimizing bile duct injuries (BDIs) have become a top priority for general surgeons. Although intraoperative cholangiogram (IOC) is used to identify stones in the common bile duct (CBD), using routine IOC for prevention of BDI is controversial [10]. Some claim that this relatively simple procedure can provide valuable information about the anatomy of the biliary tract, thus improving the safety of LC [11]. In one study, the authors state that the adoption of routine IOC at a university medical center has led to a remarkable reduction in major BDIs, as BDI was 1.9% in the selective IOC group and 0% in the routine IOC group, p = 0.004 [12]. Others claim that although it may not lower the rate of BDIs, it can minimize the extent of the injury, thus making it easier to repair [10]. Opponents claim increased cost and operative time as major drawbacks [13]. In addition, IOC requires certain operative skills in order to be performed laparoscopically. Thus, more inexperienced surgeons may not feel comfortable performing this procedure.
The purpose of our study was to assess the trend of IOC/CBD exploration in an era of laparoscopy. In addition, trend of complication rates, including BDI, are examined and compared with those trends among all LC. The importance of this information can help elucidate the role of IOC in LC.
Methods
A retrospective cohort analysis was performed to identify all LC for benign biliary non-obstructive and obstructive disease between 2000 and 2014 using the Statewide Planning and Research Cooperative System (SPARCS). SPARCS is an all-payer, administrative database that collects patient level data on every inpatient and outpatient procedure and Emergency Department (ED) visit in the state of New York. Patients in SPARCS are assigned a unique identifier that permits longitudinal follow-up across many institutions in NYS. IOC/CBD exploration and BDI were defined using the International Classification of Disease, 9th Revision, Clinical Modification procedure codes for inpatient procedures and Current Procedural Terminology codes for outpatient procedures. Patients with age <18 years, incomplete or duplicate records were excluded from the analysis. Variables included incidence of IOC/CBD exploration; patient demographics, such as age, gender, race, insurance; co-morbidities; complications; 30-day readmissions; and 30-day complications.
The linear trends of cholangiogram surgery volume, the complication rate, readmission rate or ED visit rate for cholangiogram patients, and BDI among cholangiogram patients over different years were examined using log-linear Poisson regression models with year as an explanatory variable. The trend analysis for surgery volume was on record level (537 patients had multiple times of laparoscopic cholecystectomy and only initial cholecystectomy was used), while for complication, 30-day readmission, 30-day ED visit, length of stay and BDI, the analysis was on patient level and patients’ first surgery outcome were analyzed. Over-dispersion and under-dispersion were checked and corrected using Quasi-Poisson regression if there were such issues. Furthermore, multivariable logistic regression models were also used in examining the linear trend in the complication risk, readmission risk, ED visit risk, BDI risk among all cholangiogram patients, and admitted ED visit risk among cholangiogram patients having ED visits after controlling for possible confounding factors that were significantly associated with these outcomes based on χ2 tests, respectively. In these multivariable regression models, any comorbidity/complication was used instead of specific ones because of limited number of events [14]. Welch’s test was utilized to compare length of stay across different groups. The linear trend of length of stay for inpatients having cholangiogram was examined using simple linear regression with year as an explanatory variable first and further using a multiple linear regression model after controlling for possible confounding factors that were significantly associated with length of stay based on Welch’s test at a significance level of 0.1. Log-transformation was applied to HLOS to make the normality assumption met. Statistical analysis was performed using SAS 9.3 (SAS Institute, Inc., Cary, NC) and significance level was set at 0.05. This study was approved by the institutional review board of Stony Brook Medical Center and New York Department of Health data protection review board.
Results
In total, 392, 485 cholecystectomy records (391,945 patients) were used for analysis between 2000 and 2014: 195,423 (49.8%) inpatient procedures and 197,062 (50.2%) outpatient procedures. Among all LC procedures, the proportion of patients having cholangiogram decreased from 2000 to 2014 overall (12.37–10.44%, RR = 0.98, p value <.0001) and among outpatients only (10.77–7.52%, RR = 0.96, p value <.0001, Table 1).
Univariate analysis showed that for patients undergoing LC with IOC, their overall complication rate, 30-day readmission rate, and 30-day ED visit rates increased (all RRs >1 with p values <0.01, Tables 2, 3, and 4). Patients undergoing LC also had an increase in complications by about 2% (RR = 1.02, p value <.0001, Table 2) and an increase in ED visits by about 4% (RR = 1.04, p value <0.0001, Table 4). After taking other confounding factors such as age, gender, race, region, insurance, inpatient or not, and comorbidity into consideration, the odds of complication risk for patients with IOC increased by about 3% per year (Adjusted OR 1.03, 95% CI 1.02–1.04, p value <.0001); and the odds of complication risk for LC patients increased by 2% each year (adjusted OR 1.02, 95% CI 1.02–1.04, p value <.0001). After controlling for confounding factors, such as age, gender, race, region, insurance, any comorbidity, and any complication, LC as well as IOC had increased 30-day ED visit risk through 2004–2014 (IOC: adjusted OR 1.04, 95% CI 1.02–1.05, p value <.0001; LC: adjusted OR 1.14, 95% CI 1.14–1.14, p value <.0001), while the 30-day readmission risk did not have significant linear change between 2000 and 2014 (IOC: adjusted OR 1, 95% CI 0.99–1.01, p value = 0.9976; LC: adjusted OR 1, 95% CI 0.99–1, p value = 0.3761).
Marginally, hospital length of stay (HLOS) did not have a significant change between 2000 and 2014 among IOC patients (p value = 0.2446, Table 5); while it showed a decreasing trend among LC (p value = 0.0065, Table 5). However, HLOS dropped 0.25% per year among both IOC and LC after adjusting for age, gender, race, insurance, health region, and any comorbidity, any complication (IOC: 95% CI 0.07–0.43%, p value = 0.0075; LC: 95% CI 0.21–0.29%, p value <.0001).
When examining rate of BDI among all LC patients, there is a rate of approximately 0.09% (25/29,312) in 2000 (Table 6). This rate had a significant increasing trend by around 3% per year. Similarly, there was a rate of 0.17% (6/3479) rate of BDI among cholangiogram patients in 2000, which increased significantly by around 6% from 2000 to 2013 (Table 6). This type of linear increasing trend also existed among LC after adjusting for patents’ age, insurance, race, inpatient or not, IOC patient or not, any comorbidity and overall complication (adjusted OR 1.03 with 95% CI 1.00–1.06, p value = 0.0189); while among IOC there was no significant linear trend for CBD risk (adjusted OR 1.03 with 95% CI 0.98–1.08, p value = 0.2064). Marginally, BDI was more common in patients >65 years of age (p <0.0001), Asian and African American, those with inpatient procedures, those with certain co-morbidities (congestive heart failure, hypertension, diabetes, renal failure, liver disease, obesity, coagulopathy, and fluid, and electrolyte disorders). After considering these variables in one multivariable regression model, only patients with inpatient procedures were more likely to have CBD injury (p value <0.0001, Table 7).
Discussion
Currently, the use of IOC during LC has decreased over time. In our study, this number is between 10 and 12% in the state of New York. Since its introduction in the 1930s [15], its benefits have been considerably debated. Many advocate routine use of IOC [12, 16, 17], although selective use has been advised as well [18]. IOC is used to show the presence of stones or provide information about aberrant anatomy, in addition to identification of BDI [19], thus it can be used to prevent or decrease the severity of injuries [12]. Opponents consider IOC as a time consuming, cumbersome, and unnecessary procedure.
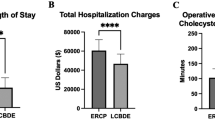
In the current study, we examined the use of IOC during LC for benign non-obstructive and obstructive biliary disease. The rate of performing IOC during LC has significantly decreased from 2000 to 2014, which shows that surgeons are performing this procedure less. In addition, the rate of complications, including BDI, and 30-day readmissions have significantly increased for patients undergoing LC with IOC (Fig. 1), despite these patients having less co-morbidities over time. This may reflect more surgeon’s inexperience with the procedures, or that fact that cholangiography is now only performed in cases of difficult anatomy or feared complication, potentially even after that complication has occurred. The proportion of all patients with cholangiogram decreased by about 2% per year and the rate of BDI increased by around 6% per year. This rate of injury increased in both the LC overall (p = 0.049) and the LC with IOC groups (Table 6). Thus, the increase is independent of the presence of a cholangiogram.
Since the introduction of LC in 1990s, the rate of BDI was found to be higher compared to open cholecystectomy [12, 20]. Fletcher et al. showed that compared to open procedures, LC carries a twofold risk of BDI. Fletcher advocated for operative cholangiography and suggested a reduced rate for all injuries and leaks with IOC (OR 0.5, 95% CI 0.35–0.7) [20]. The increase in BDI was attributed to the learning curve of LC, as this study was examining procedures being performed between 1988 and 1994 [20]. Due to concern for these injuries, the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) has made it a high priority to promote the adoption of a universal culture of safety during laparoscopic cholecystectomy. The Safe Cholecystectomy Task Force was initiated in order to reduce BDI. The group endorses liberal use of IOC especially in difficult cases or unclear anatomy [21].
Similar to our study, Buddingh recently advocated for use of IOC for reduction of BDI. The group described their experience in the Netherlands with adoption of routine IOC during LC and reported BDI prior and following adoption of this policy. In this study, 421 patients underwent cholecystectomy with selective IOC versus 435 patients with routine IOC. The rate of major BDI was 1.9% in the selective IOC group compared to 0% in the routine IOC group (p = 0.004) [12]. Alvarez et al. performed a retrospective analysis of patients with routine IOC between 1991 and 2012, which comprised of 11,423 patients. Twenty patients (0.17%) sustained a BDI with 18 of these patients being diagnosed at the time of IOC. The authors also concluded that routine use of IOC a high-volume center was associated with low incidence of BDI and helped in early detection [22]. Others have examined the use of cholangiography (groups with and without IOC) and did not find that routine use of IOC reduces BDI or the number of injuries missed during surgery (both 0.3%, p = 0.755) [23].
Our study has several limitations, including the limitations that are inherent to the use of retrospective data in a prospectively maintained database. Although we show an increase in BDI in groups with and without IOC, we suspect some of the IOCs are performed following BDI. We also do not know the experience of physicians with laparoscopic cholecystectomy or IOC, which may play a significant role in outcomes. Finally, we may undercapture the true rate of BDI as any outpatient facility with purely outpatient ERCP for bile duct injury may not have been reported. This should only magnify the trends identified.
Despite these limitations, the main advantage of our study is the use of a longitudinal data across many institutions in the state of New York. Through the use of a unique identifier we were able to track patients across institutions and throughout time, which is a main disadvantage of other databases, which may only capture 30-day outcomes. We are able to describe the trends over time of both LC, IOC, and determine complications, in addition to readmission and ED visits across institutions.
Conclusion
Our study shows a concerning increase in CBD injury in patients with and without IOC between 2000 and 2014 in the state of New York. At the same time, the rate of IOC/CBD exploration during LC has significantly decreased. In addition, the rate of complications and 30-day ED visits increased, although HLOS showed a decreasing trend. Routine IOC at time of LC may help early identification and potentially decrease the rate of BDI.
References
Truven Health Analytics (Thomson/Solucient), USA Procedure Volumes 2014
Calland JF, Tanaka K, Foley E et al (2001) Outpatient laparoscopic cholecystectomy: patient outcomes after implementation of a clinical pathway. Ann Surg 233(5):704–715
Shea JA, Berlin JA, Bachwich DR et al (1998) Indications for and outcomes of cholecystectomy: a comparison of the pre and postlaparoscopic eras. Ann Surg 227(3):343–350
Lillemoe KD, Lin JW, Talamini MA, Yeo CJ, Snyder DS, Parker SD (1999) Laparoscopic cholecystectomy as a “true” outpatient procedure: initial experience in 130 consecutive patients. J Gastrointest Surg 3(1):44–49
Giger UF, Michel JM, Opitz I et al (2006) Risk factors for perioperative complications in patients undergoing laparoscopic cholecystectomy: analysis of 22,953 consecutive cases from the Swiss Association of Laparoscopic and Thoracoscopic Surgery database. J Am Coll Surg 203(5):723–728
Halbert C, Pagkratis S, Yang J et al (2016) Beyond the learning curve: incidence of bile duct injuries following laparoscopic cholecystectomy normalize to open in the modern era. Surg Endosc 30(6):2239–2243
Archer SB, Brown DW, Smith CD, Branum GD, Hunter JG (2001) Bile duct injury during laparoscopic cholecystectomy: results of a national survey. Ann Surg 234(4):549–558
Halbert C, Altieri MS, Yang J et al (2016) Long-term outcomes of patients with common bile duct injury following laparoscopic cholecystectomy. Surg Endosc 30(10):4294–4299
Kern KA (1997) Malpractice litigation involving laparoscopic cholecystectomy. Cost, cause, and consequences. Arch Surg 132(4):392–397
Vezakis A, Davides D, Ammori BJ, Martin IG, Larvin M, McMahon MJ (2000) Intraoperative cholangiography during laparoscopic cholecystectomy. Surg Endosc 14(12):1118–1122
Kullman Borch K, Lindstrom E, Svanvik J, Anderberg B (1996) Value of routine intraoperative cholangiography in detecting aberrant bile ducts and bile duct injuries during laparoscopic cholecystectomy. Br J Surg 83(2):171–175
Buddingh KT, Weersma RK, Savenije RA, van Dam GM, Nieuwenhuijs VB (2011) Lower rate of major bile duct injury and increased intraoperative management of common bile duct stones after implementation of routine intraoperative cholangiography. J Am Coll Surg 213(2):267–274
Massarweh NN, Flum DR (2007) Role of intraoperative cholangiography in avoiding bile duct injury. J Am Coll Surg 204(4):656–664
Peduzzi P, Concato J, Kemper E, Holford TR, Feinstein AR (1996) A simulation study of the number of events per variable in logistic regression analysis. J Clin Epidemiol 49(12):1373–1379
Mirizzi PL (1937) Operative cholangiography. Surg Gynecol Oncol 65:702–710
Soper NJ, Brunt LM (1994) The case for routine operative cholangiography during laparoscopic cholecystectomy. Surg Clin North Am 74(4):953–959
Flum DR, Dellinger EP, Cheadle A, Chan L, Koepsell T (2003) Intraoperative cholangiography and risk of common bile duct injury during cholecystectomy. JAMA 289(13):1639–1644
Ladocsi LT, Benitez LD, Filippone DR, Nance FC (1997) Intraoperative cholangiography in laparoscopic cholecystectomy: a review of 734 consecutive cases. Am Surg 63(2):150–156
Woods MS, Traverso LW, Kozarek RA et al (1995) Biliary tract complications of laparoscopic cholecystectomy are detected more frequently with routine intraoperative cholangiography. Surg Endosc 9(10):1076–1080
Fletcher DR, Hobbs MS, Tan P et al (1999) Complications of cholecystectomy: risks of the laparoscopic approach and protective effects of operative cholangiography: a population-based study. Ann Surg 229(4):449–457
Pucher PH, Brunt LM, Fanelli RD, Asbun HJ, Aggarwal R (2015) SAGES expert Delphi consensus: critical factors for safe surgical practice in laparoscopic cholecystectomy. Surg Endosc 29(11):3074–3085
Alvarez FA, de Santibanes M, Palavecino M et al (2014) Impact of routine intraoperative cholangiography during laparoscopic cholecystectomy on bile duct injury. Br J Surg 101(6):677–684
Giger U, Ouaissi M, Schmitz SF, Krähenbühl S, Krähenbühl L (2011) Bile duct injury and use of cholangiography during laparoscopic cholecystectomy. Br J Surg 98(3):391–396
Acknowledgement
We acknowledge the biostatistical consultation and support from the Biostatistical Consulting Core at the School of Medicine, Stony Brook University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
No industry or other external funding was used for this research. Dr. Pryor receives honoraria for speaking for Ethicon, Medtronic, Stryker, and Gore; is a consultant for Medicines Company, Merck, and Intuitive, and has ownership interest in Transenterix.
Rights and permissions
About this article
Cite this article
Altieri, M.S., Yang, J., Obeid, N. et al. Increasing bile duct injury and decreasing utilization of intraoperative cholangiogram and common bile duct exploration over 14 years: an analysis of outcomes in New York State. Surg Endosc 32, 667–674 (2018). https://doi.org/10.1007/s00464-017-5719-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5719-2