Abstract
Background
Studies dealing with laparoscopic colectomy for cancer have reached conflicting results in regards to various inflammatory cytokines. Most of them have not examined potential differences with the open procedures at later postoperative days, when the immunologic advantage of laparoscopic surgery would be more demanding to demonstrate (for earlier administration of adjuvant treatment). The aim of this work is to detect differences of proinflammatory cytokines between conventional and laparoscopic colectomy for cancer.
Patients and methods
30 patients who underwent laparoscopic colectomy were age, sex, and preoperative stage-matched with 30 patients treated by open surgery. C-reactive protein (CRP), interleukin (IL)-1, -6, and -8, and interferon (IFN)-γ serum levels were measured preoperatively, at 24 h, and at the 7th postoperative day (POD).
Results
CRP and IL-6 postoperative values (24 h and 7th POD) were significantly higher than baseline for both groups (p = 0.001), but the respective values at the 7th POD were less than at 24 h (p = 0.001). IL-1 and -8 levels did not show any differences between assessment timepoints. A higher IFN-γ measurement was demonstrated at 24 h compared with baseline for the laparoscopic group only (p = 0.03). This difference was not maintained at the 7th POD. IFN-γ levels at 24 h and the 7th POD were significantly less for the open compared with the laparoscopic group of patients (p = 0.001). No correlation was revealed between measured serum values and age, sex, tumor location, or stage.
Conclusions
This matched case–control study verifies the already reported lack of differences regarding IL-1. Controversy still exists on likely IL-6 differences. The inadequately studied IL-8 does not seem to play an important role in immunologic differences. The immunologically beneficial IFN-γ, produced by the principal effectors of cell-mediated immunity Th1 cells, seems to have a more active presence following laparoscopic colectomy, potentially contributing to an immunologic “advantage” by counteracting “harmful” cytokines, such as IL-1.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Following two decades of evolution, the laparoscopic approach has been well established in the surgical armamentarium. Shorter hospital stay, less postoperative pain, decreased wound infection rate, and faster recovery have been revealed as advantages of laparoscopic surgery [1]. Those benefits are also encountered after laparoscopic colectomy (LC), and despite the initial skepticism, the ambiguous viewpoints regarding port-site tumor recurrence, and the slow expansion of the method, oncologic equivalency with its open counterpart has been well proven in randomized trials [2–5].
Although various aspects of the laparoscopic approach in surgical treatment of benign and laparoscopic colorectal diseases have been extensively studied, sufficient and firm data regarding relative differences in immunologic response between conventional, open colectomy (OC) and LC are still not sufficient to draw definite, useful, and clinically applicable conclusions [6]. Existing studies, though, tend to support better preservation of immunologic function after LC [7]. However, assessment of the systemic inflammatory response and comparison of various inflammatory cytokines between the two approaches in colon cancer surgery by different research groups have been dominated by conflicting results [8]. What is also underexamined is the presence of potential differences with the open procedures at later postoperative days, when the immunologic advantage of laparoscopic surgery would be more demanding to demonstrate, in order for earlier administration of adjuvant treatment to be better justified.
Based on the imperative need to clarify the potential immunologic advantage of LC, especially at later postoperative days, this study attempts to compare the inflammatory response of patients who underwent OC and LC for colorectal cancer up to the end of the first postoperative week. Interleukin 1 (IL-1), interleukin 6 (IL-6), interleukin 8 (IL-8), interferon γ (IFN-γ), and C-reactive protein (CRP) are proinflammatory cytokines with central systemic role and are detected and analyzed in the present comparative study.
Patients and methods
Amongst the 36 patients who were treated by laparoscopic colectomy with therapeutic intent between December 2007 and June 2009 at the 1st Propaedeutic Surgical Department of Athens University, 30 patients elected to enter the study, and were age, sex, stage, American Society of Anesthesiologists (ASA) score, and colectomy type-matched with 30 colorectal cancer patients derived from a cohort of 120 patients who had undergone open colectomy during the same time period and had blood drawn at the defined assessment timepoints of the study. To perform this matched case–control study, we used a matching algorithm based on the type of surgery performed according to tumor location (right colectomy, sigmoidectomy, low anterior resection). Patients were classified and arranged according to colectomy type. An independent reviewer, who was blinded to all clinical data except the matching criteria, matched the patients manually one by one on the basis of the remaining criteria [tumor–node–metastasis (TNM) stage, age, sex, and ASA score] (Table 1).
All patients included had adenocarcinoma of the colon or the rectum confirmed by pathology. Exclusion criteria were age older than 80 years or younger than 18 years, presence of severe comorbidities (ASA score >3), presence of immune compromise, hepatic or renal insufficiency, history of inflammatory bowel disease or inherited colorectal polyposis syndrome, malnutrition, presence of metastatic disease, neoadjuvant treatment, emergency surgery, surgery for complicated cancer (i.e., large bowel obstruction), complications during postoperative course, and conversion at laparoscopic colectomy. Patients in both groups had generally uneventful recovery.
Institutional review board (IRB) approval has been obtained, and informed consent was given by the patients. Preoperative data, such as demographics and medical history, were recorded. All patients received mechanical bowel preparation, and intravenous chemoprophylaxis was also administered. None of the patients received blood transfusion.
Blood from peripheral venipuncture was taken from the patients preoperatively, 24 h after completion of the operation, and at the 7th postoperative day (POD). The blood sample was centrifuged, and part of the collected serum was stored at −20°C whereas the rest was used to measure CRP by immunonephelometry. The stored specimens were assayed by enzyme-linked immunosorbent assay (ELISA) for IL-1a, IL-6, IL-8, and IFN-γ. The concentrations in serum were measured with a commercially available enzyme-linked immunosorbent assay kit (human ELISA kits, Mergenix EASIA®; Immunotech Marseille, France and DSX system Dynex; Magellan Biosciences).
The patients underwent typical segmental colorectal resections, either open or laparoscopic, by surgeons experienced in both techniques. All patients received general anesthesia with standardized anesthetic techniques. A urinary catheter and a nasogastric tube were routinely used. During the conventional procedures, an abdominal midline incision was undertaken and either a stapled or a handsewn anastomosis was created depending on surgeon preference. During the laparoscopic operations, CO2 pneumoperitoneum was created via Hasson technique and maintained intraoperatively at pressure of 12–14 mmHg. Standardized equipment was used in all the laparoscopic operations, including a 30º laparoscope; at the end, small (<10 cm length), transverse or vertical, peri- or infraumbilical incisions were used for specimen extraction and anastomosis (right colectomies). Sites and number of trocars were generally standardized to the corresponding large bowel section removed each time. Oncologic principles were ascertained and preserved in both operational procedures.
All data were collected and statistical analysis was undertaken with SPSS statistical package version 16.0. Nonparametric tests were used for statistical analysis. Changes of examined measured values of inflammatory markers with time were analyzed with Wilcoxon’s signed-rank test comparing follow-up values with baseline, as well as timepoint values in between (i.e., 24 h versus 7 days). Differences between examined subgroups of patients (open versus laparoscopic) were analyzed by Mann–Whitney U tests. Statistical significance was set at p < 0.05.
Results
No significant differences existed between groups in terms of basic demographic and pathologic data (Table 1). Except for length of operation time, which was greater for LC (p < 0.05), body mass index, concurrent illness, number of retrieved lymph nodes, tumor size, etc. did not differ significantly between the two groups.
Examined cytokines and CRP values at the three assessment timepoints (preoperatively, at 24 h, and at the 7th POD) are presented in Table 2. CRP and IL-6 postoperative values at 24 h and at the 7th POD were significantly higher than baseline for both groups (p = 0.001), but the respective values at the 7th POD were less than at 24 h (p = 0.001) (Table 2). Changes in IL-1 and IL-8 levels were not statistically significant between assessment timepoints or between groups of patients (Table 2). Postoperative IFN-γ measurements were significantly higher compared with baseline for the LC group only (p = 0.03).
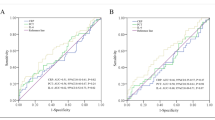
Comparing the relative differences of cytokine concentrations (i.e., the difference of INF-γ values between baseline and 24 h versus the difference of IL-1 values between baseline and 24 h), it was found that the IFN-γ increment noted in the laparoscopic group was more accentuated than the respective IL-1 value changes at 24 h and at the 7th POD (p = 0.09 and p = 0.02, respectively). Similarly, IFN-γ levels at 24 h and at the 7th POD were significantly less for the OC group compared with the LC group of patients (p = 0.001) (Table 2; Fig. 1). No correlation was revealed between measured serum values and other parameters such as age, sex, tumor location, or stage of disease.
Discussion
Operative procedures have major impact on patient homeostasis, expressed mainly by an immune response compromise [9]. The unavoidable inflammatory response involves regional and systemic release of cytokines, hormones, acute-phase proteins, eicosanoids, and other substances by surgical manipulation-activated immune cells. This stress response is responsible for the attenuated cell-mediated immune response and the probable immune compromise which may contribute to postoperative morbidity [9–12]. The impaired immune response has been well appreciated in cancer patients [12–15]. In this sensitive group of patients, fast and uneventful recovery is a prerequisite for timely administration of adjuvant treatment.
Measuring the levels of circulating cytokines at several postoperative timepoints is indicative of the degree of inflammatory response in both conventional and laparoscopic techniques. Initially, better preservation of patient immune status was proved with the conduction of common operations, such as cholecystectomy, by laparoscopic means [16–23]. That was attributed to the CO2 pneumoperitoneum, the less and gentler tissue manipulations, and the smaller surgical wounds [16–23]. While the immunological benefits may be expected to be pronounced in procedures where the access incision constitutes a proportionally large burden of injury, such as in laparoscopic cholecystectomy, in other procedures, where the intra-abdominal insult is more major, such as laparoscopic colectomy, the evidence remains, in many aspects, unclear. This is due to the fact that, although the humoral response after open and laparoscopic colectomies has been the subject of intense investigation, heterogeneity in surgical indications, humoral factors measured, measurement timing, and method of sample analysis do not permit firm conclusions. As a consequence, results are conflicting and opinions remain divided [24–36, 39–44] (Table 3). Applying the methodology of a matched case–control study, we managed to diminish the influence of some potentially immunologically implicated factors and to elucidate whether there are any real differences between some of the known involved cytokines easily measured in patients’ serum.
In accordance with our results, the measured CRP was not significantly different between the two approaches in several studies [24–30]. To the contrary, according to other groups, lower CRP values were demonstrated during the early postoperative days after laparoscopic colectomy [31–34].
In the few studies dealing with IL-1, no appreciable differences have been noticed, as in the current study [35, 36]. Nevertheless, IL-1b exhibited significantly higher peak serum levels at 2 h after open surgery compared with laparoscopic surgery for rectosigmoid carcinoma in one study [36]. Without any significant findings in our study, IL-8 remains the least studied interleukin in this setting [28]. IL-8 is a potent chemoattractant for neutrophils and lymphocytes, as well as an angiogenic growth factor that promotes wound healing [37]. Wu et al. [28] are the only other researchers to have comparatively assessed IL-8, in the serum of patients at 2 and 24 h and 4 days postoperatively; only at 2 h was a significant difference ascertained, with lower levels after laparoscopic procedures. Based on the much higher local IL-8 expression than the systematically measured levels, the same group accentuated the idea of compartmentalization of cytokines, pointing out that what is measured systemically represents only a small fragment of what is generated locally [28]. Such observation may render real inflammatory response comparisons even more difficult.
IL-6 is considered to be a major mediator of the acute-phase protein response following injury, and in comparison with other cytokines, the concentration of IL-6 is most consistently increased in the circulation of injured patients [38]. Rationally, this is the most studied serum interleukin after laparoscopic and open colectomies [24, 25, 27–29, 31–36, 39–42]. Although discrepancy still characterizes the results on IL-6, most studies agree on the ameliorated inflammatory response after laparoscopic colectomy in the first few postoperative hours, as far as it concerns lower IL-6 levels. In our study that focused on the end of the first postoperative day, such a difference was not apparent. Even though certain studies support significantly higher IL-6 levels extending to 24 h after open versus laparoscopic colectomy [25, 32, 33, 42, 45], others are in keeping with the results derived from our study [27–29, 34, 39–41, 44]. At later postoperative days no difference between the two procedures has ever been revealed [27, 29, 34].
Excluding a small portion of the studies and our study, the rest have not examined any potential inflammatory differences at the end or after the first week [27, 31, 34]. From that time on, following assurance of well-healed anastomosis and surgical trauma, administration of postoperative chemotherapy could be considered; taking into consideration that oncological outcomes may be improved by laparoscopic techniques as a result of diminished inflammatory response [45], restoration of deranged inflammatory cytokines and of required immunologic adequacy at such potential chemotherapy-induction timeframes may be of paramount importance.
Our principal novel finding, not previously studied, is the significantly higher levels of INF-γ after laparoscopic colectomy, a difference that was also maintained at the 7th postoperative day. IFN-γ is a stimulator of human leukocyte antigen (HLA)-DR expression on the surface of antigen-presenting cells, monocytes, and macrophages, contributing to better presentation of peptide segments of the antigen to T helper lymphocytes so that the processing of the antigens in the cognitive phase of the immune response is adequately preserved [46–48]. In response to antigenic stimulation, naive T cells differentiate into either Th1 or Th2 subsets with relatively restricted profiles of cytokine production. Th1 cells produce IL-2 and INF-γ, which activates macrophages, and they are the principal effectors of cell-mediated immunity and of the delayed-type hypersensitivity reaction [7]. Th2 cells produce IL-4, IL-5, and IL-10, which activate antibody production by B cells and suppress cell-mediated immunity [7]. So, IFN-γ indicates better preserved cell-mediated immune function [7, 30, 46–49]. A study by Fujii et al. [50] showed increased production of INF-γ representing Th1 function and decreased production of IL-4 representing Th2 cell function after laparoscopic distal gastrectomy in gastric cancer patients. The authors concluded that laparoscopic distal gastrectomy contributes to preservation of postsurgical Th1 cell-mediated immune function [50]. The sustained increment of this immunologically beneficial agent in the context of laparoscopic colectomy, as well as its more striking increment in relation to IL-1 value changes in the laparoscopic group, should be taken into serious consideration and merit further exploration, as such effects may provide a theoretically basis for earlier administration of chemotherapy.
In conclusion, this study adds to the accumulating literature data on inflammatory response after laparoscopic and open colectomies, revealing the previously inadequately measured INF-γ as a potentially important indicator, which seems to have a more active presence following laparoscopic colectomy, potentially contributing to an immunologic “advantage” by counteracting “harmful” cytokines such as IL-1. Further work is necessary to further establish an immunologic advantage of laparoscopic colectomy in cancer patients.
References
Barlehner E, Benhidjeb T, Anders S, Schicke B (2004) Laparoscopic surgery for colon and rectal cancer. Surg Technol Int 13:93–99
Colon Cancer Laparoscopic or Open Resection Study Group, Buunen M, Veldkamp R, Hop WC, Kuhry E, Jeekel J, Haglind E, Pahlman L, Cuesta MA, Msika S, Morino M, Lacy A, Bonjer HJ (2009) Survival after laparoscopic surgery versus open surgery for colon cancer: long term outcome of a randomized clinical trial. Lancet Oncol 10(1):44–52
Lujan HJ, Plasencia G, Jacobs M, Viamonte M 3rd, Hartmann RF (2002) Long term survival after laparoscopic colon resection for cancer: complete five-year follow up. Dis Colon Rectum 45(4):491–501
Jacob BP, Salky B (2005) Laparoscopic colectomy for colon adenocarcinoma: an 11-year retrospective review with 5-year survival rates. Surg Endosc 19(5):643–649
Barlehner E, Benhidjeb T, Anders S, Schicke B (2005) Laparoscopic resection for rectal cancer: outcomes in 194 patients and review of the literature. Surg Endosc 19(6):757–766
Gupta A, Watson DI (2001) Effect of laparoscopy on immune function. Br J Surg 88(10):1296–1306
Lee SW, Whelan RL (2006) Immunologic and oncologic implications of laparoscopic surgery: what is the latest? Clin Colon Rect Surg 19(1):5–12
Tsamis D, Theodoropoulos G, Michalopoulos NV, Delistathi T, Nikiteas N, Tsigris C, Leandros E (2010) Inflammatory response after laparoscopic versus open colonic resection: Review of the literature. Int J Medic Med Sci 2(4):106–110
Koerner P, Westerholt A, Kessler W, Traeger T, Maier S, Heidecke CD (2008) Surgical trauma and postoperative immunosuppression. Chirurg 79(4):290–294
Sammour T, Kahokehr A, Chan S, Booth RJ, Hill AG (2010) The humoral response after laparoscopic versus open colorectal surgery: a meta-analysis. J Surg Res 164(1):28–37
Brivio F, Perego M, Mauri E, Gramazio F, Brivio O, Gariboldi G, Urso G, Nespoli A (1998) Variations in interleukin-2 and interleukin-6 due to surgical trauma in cancer patients. G Chir 19(10):377–380
Buunen M, Gholghesaei M, Veldkamp R, Meijer DW, Bonjer HJ, Bouvy ND (2004) Stress response to laparoscopic surgery: a review. Surg Endosc 18(7):1022–1028
Hartley JE, Mehigan BJ, Monson JR (2001) Alterations in the immune system and tumor growth in laparoscopy. Surg Endosc 15(3):305–313
Carter JJ, Whelan RL (2001) The immunologic consequences of laparoscopy in oncology. Surg Oncol Clin North Am 10(3):655–677
Ishikawa M, Nishioka M, Hanaki N, Miyauchi T, Kashiwagi Y, Ioki H, Kagawa A, Nakamura Y (2009) Perioperative immune responses in cancer patients undergoing digestive surgeries. W J Surg Oncol 7:7–16
Kuntz C, Wunsch A, Bay F, Windeler J, Glaser F, Herfarth C (1998) Prospective randomized study of stress and immune response after laparoscopic vs conventional colonic resection. Surg Endosc 12(7):963–967
Grande M, Tucci GF, Adorisio O, Barini A, Rulli F, Neri A, Franchi F, Farinon AM (2002) Systemic acute-phase response after laparoscopic and open cholecystectomy. Surg Endosc 16:313–316
Redmond HP, Watson RW, Houghton T, Condron C, Watson RG, Bouchier-Hayes D (1994) Immune function in patients undergoing open vs laparoscopic cholecystectomy. Arch Surg 129:1240–1246
Holub Z (2002) Impact of laparoscopic surgery on immune function. Clin Exp Obstet Gynec 29:77–81
Malik E, Buchweitz O, Muller-Steinhardt M, Kressin P, Meyhofer-Malik A, Diedrich K (2001) Prospective evaluation of the systemic immune response following abdominal, vaginal and laparoscopically assisted vaginal hysterectomy. Surg Endosc 15:463–466
Yuen PM, Mak TW, Yim SF, Kee WD, Lam CW, Rogers MS, Chang AM (1998) Metabolic and inflammatory responses after laparoscopic and abdominal hysterectomy. Am J Obstet Gynecol 179:1–5
Perttila J, Salo M, Ovaska J, Gronroos J, Lavonius M, Katila A, Lahteenmaki M, Pullki K (1999) Immune response after laparoscopic and conventional Nissen fundoplication. Eur J Surg 165:21–28
Uzunkoy A, Coskum A, Akinci OF, Kocyigit A (2000) Systemic stress responses after laparoscopic or open hernia repair. Eur J Surg 166:467–471
Fukushima R, Kawamura YJ, Saito H, Saito Y, Hashiguchi Y, Sawada T, Muto T (1996) Interleukin-6 and stress hormone responses after uncomplicated gasless laparoscopic-assisted and open sigmoid colectomy. Dis Colon Rectum 39(10 Suppl):S29–S34
Mehigan BJ, Hartley JE, Drew PJ, Saleh A, Dore PC, Lee PW, Monson JR (2001) Changes in T cell subsets, interleukin-6 and C-reactive protein after laparoscopic and open colorectal resection for malignancy. Surg Endosc 15(11):1289–1293
Braga M, Vignali A, Zuliani W, Radaelli G, Gianotti L, Martani C, Toussoun G, Di Carlo V (2002) Metabolic and functional results after laparoscopic colorectal surgery: a randomized, controlled trial. Dis Colon Rectum 45(8):1070–1077
Dunker MS, Ten Hove T, Bemelman WA, Slors JF, Gouma DJ, Van Deventer SJ (2003) Interleukin-6, C-reactive protein and expression of human leukocyte antigen-DR on peripheral blood mononuclear cells in patients after laparoscopic vs. conventional bowel resection: a randomized study. Dis Colon Rectum 46(9):1238–1244
Wu FP, Sietses C, von Blomberg BM, van Leeuwen PA, Meijer S, Cuesta MA (2003) Systematic and peritoneal inflammatory response after laparoscopic or conventional colon resection in cancer patients: a prospective, randomized trial. Dis Colon Rectum 46(2):147–155
Ytting H, Christensen IJ, Basse L, Lykke J, Thiel S, Jensenius JC, Nielsen HJ (2006) Influence of major surgery on the mannan-binding lectin pathway of innate immunity. Clin Exp Immunol 144(2):239–246
Huang C, Huang R, Jiang T, Huang K, Cao J, Qiu Z (2010) Laparoscopic and open resection for colorectal cancer: an evaluation of cellular immunity. BMC Gastroenterol 28(10):127
Schwenk W, Jacobi C, Mansmann U, Bohm B, Muller JM (2000) Inflammatory response after laparoscopic and conventional colorectal resections-results of a prospective randomized trial. Langenbecks Arch Surg 385(1):2–9
Nishiguchi K, Okuda J, Toyoda M, Tanaka K, Tanigawa N (2001) Comparative evaluation of surgical stress of laparoscopic and open surgeries for colorectal carcinoma. Dis Colon Rectum 44(2):223–230
Delgado S, Lacy AM, Filella X, Castells A, Garcia-Valdecasas JC, Pique JM, Momblan D, Visa J (2001) Acute phase response in laparoscopic and open colectomy in colon cancer: randomized study. Dis Colon Rectum 44(5):638–646
Hasegawa H, Kabeshima Y, Watanabe M, Yamamoto S, Kitajima M (2003) Randomized controlled trial of laparoscopic versus open colectomy for advanced colorectal cancer. Surg Endosc 17(4):636–640
Harmon GD, Senagore AJ, Kilbride MJ, Warzynski MJ (1994) Interleukin-6 response to laparoscopic and open colectomy. Dis Colon Rectum 37(8):754–759
Leung KL, Lai PB, Ho RL, Meng WC, Yiu RY, Lee JF, Lau WY (2000) Systemic cytokine response after laparoscopic-assisted resection of rectosigmoid carcinoma: A prospective randomized trial. Ann Surg 231(4):506–511
Koch AE, Polverini PJ, Kunkel SL, Harlow LA, DiPietro LA, Elner VM, Elner SG, Strieter RM (1992) Interleukin-8 as a macrophage-derived mediator of angiogenesis. Science 11 258(5089):1798–1801
Baigrie R, Lamont P, Kwiatkowski D (1992) Systemic cytokine response after major surgery. Br J Surg 19:757
Hu JK, Zhou ZG, Chen ZX, Wang LL, Yu YY, Liu J, Zhang B, Li L, Shu Y, Chen JP (2003) Comparative evaluation of immune response after laparoscopical and open total mesorectal excisions with anal sphincter preservation in patients with rectal cancer. World J Gastroenterol 9(12):2690–2694
Hewitt PM, Ip SM, Kwok SP, Somers SS, Li K, Leung KL, Lau WY, Li AK (1998) Laparoscopic-assisted vs. open surgery for colorectal cancer: comparative study of immune effects. Dis Colon Rectum 41(7):901–909
Pascual M, Alonso S, Parés D, Courtier R, Gil MJ, Grande L, Pera M (2011) Randomized clinical trial comparing inflammatory and angiogenic response after open versus laparoscopic curative resection for colonic cancer. Br J Surg 98(1):50–59
Ordemann J, Jacobi CA, Schwenk W, Stosslein R, Muller JM (2001) Cellular and humoral inflammatory response after laparoscopic and conventional colorectal resections. Surg Endosc 15(6):600–608
Ozawa A, Konishi F, Nagai H, Okada M, Kanazawa K (2000) Cytokine and hormonal responses in laparoscopic-assisted colectomy and conventional open colectomy. Surg Today 30(2):107–111
Stage JG, Schulze S, Moller P, Overgaard H, Andersen M, Rebsdorf-Pedersen VB, Nielsen HJ (1997) Prospective randomized study of laparoscopic versus open colonic resection for adenocarcinoma. Br J Surg 84:391
Lacy AM, García-Valdecasas JC, Delgado S, Castells A, Taurá P, Piqué JM, Visa J (2002) Laparoscopy-assisted colectomy versus open colectomy for treatment of non-metastatic colon cancer: a randomised trial. Lancet 29 359(9325):2224–2229
Tang CL, Eu KW, Tai BC, Soh JG, MacHin D, Seow-Choen F (2001) Randomized clinical trial of the effect of open versus laparoscopically assisted colectomy on systemic immunity in patients with colorectal cancer. Br J Surg 88(6):801–807
Sietses C, Havenith CE, Eijsbouts QA, van Leeuwen PA, Meijer S, Beelen RH, Cuesta MA (2000) Laparoscopic surgery preserves monocyte-mediated tumor cell killing in contrast to the conventional approach. Surg Endosc 14(5):456–460
Bolla G, Tuzzato G (2003) Immunologic postoperative competence after laparoscopy versus laparotomy. Surg Endosc 17(8):1247–1250
Brune IB, Wilke W, Hensler T, Holzmann B, Siewert JR (1999) Downregulation of T helper type 1 immune response and altered pro-inflammatory and anti-inflammatory T cell cytokine balance following conventional but not laparoscopic surgery. AM J Surg 177:55–60
Fujii K, Sonoda K, Izumi K, Shiraishi N, Adachi Y, Kitano S (2003) T lymphocyte subsets and Th1/Th2 balance after laparoscopy-assisted distal gastrectomy. Surg Endosc 17:1440–1444
Disclosures
Authors Dimitrios Tsamis, George Theodoropoulos, Paraskevas Stamopoulos, Spyridon Siakavellas, Thalassini Delistathi, Nikolaos V. Michalopoulos, and George C. Zografos have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsamis, D., Theodoropoulos, G., Stamopoulos, P. et al. Systemic inflammatory response after laparoscopic and conventional colectomy for cancer: a matched case–control study. Surg Endosc 26, 1436–1443 (2012). https://doi.org/10.1007/s00464-011-2052-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-011-2052-z