Abstract
New approaches to the clinical treatment of traumatic nerve injuries may one day utilize stem cells to enhance nerve regeneration. Adipose-derived stem cells (ASC) are found in abundant quantities and can be harvested by minimally invasive procedures that should facilitate their use in such regenerative applications. We have analyzed the properties of human ASC isolated from the deep and superficial layers of abdominal fat tissue obtained during abdominoplasty procedures. Cells from the superficial layer proliferate significantly faster than those from the deep layer. In both the deep and superficial layers, ASC express the pluripotent stem cell markers oct4 and nanog and also the stro-1 cell surface antigen. Superficial layer ASC induce the significantly enhanced outgrowth of neurite-like processes from neuronal cell lines when compared with that of deep layer cells. However, analysis by reverse transcription with the polymerase chain reaction and by enzyme-linked immunosorbent assay has revealed that ASC isolated from both layers express similar levels of the following neurotrophic factors: nerve growth factor, brain-derived neurotrophic factor and glial-derived neurotrophic factor. Thus, human ASC show promising potential for the treatment of traumatic nerve injuries. In particular, superficial layer ASC warrant further analysis of their neurotrophic molecules.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A nerve injury is a relatively common clinical problem often affecting young patients (mean age 30) and in spite of advanced treatment involving microsurgical procedures, almost all patients are left with lifelong disabilities involving the loss of sensation and motor control in the affected limbs (Lundborg 2000). The development of novel tissue-engineered approaches might facilitate the process of nerve repair and regeneration (Pfister et al. 2007; Terenghi et al. 2009; Walsh and Midha 2009). Mesenchymal stem cells (MSC) isolated from adult tissues such as bone marrow, skin and fat are an attractive cell source for the regeneration of nervous tissue, since they are self-renewing and have the ability to differentiate across multiple cell lineages. Adipose-derived stem cells (ASC) are, in addition, found in abundant quantities and can be harvested by minimally invasive procedures, which should facilitate their use in regenerative medicine applications (Sterodimas et al. 2009; Bunnell et al. 2008; Gimble et al. 2007).
Experimentally, native MSC have been shown to reduce neuronal damage and stimulate re-myelination in various nerve injury models (Dezawa et al. 2001; Enzmann et al. 2006). We have shown that rat ASC can be differentiated into cells resembling Schwann cells, which promote neurite outgrowth in vitro (Kingham et al. 2007) and enhance peripheral nerve regeneration in vivo (di Summa et al. 2009). Although some trans-differentiation of transplanted MSC might occur in vivo, the exact mechanisms behind the neuroprotective and growth-promoting effects of adult stem cells are largely unknown. However, some of the benefits elicited by transplanted cells probably occur as a direct result of their production of neurotrophic factors.
An optimal source of human ASC for the treatment of nerve injuries has yet to be found. Human abdominal adipose tissue consists in superficial and deep layers, which are separated by a fibrous connective tissue fascia. A previous study has shown that ASC isolated from the superficial layer are relatively more resistant to apoptosis than those from the deep layer (Schipper et al. 2008). Furthermore, studies by the same group have revealed that the osteogenic differentiation of superficial layer ASC is faster and more efficient when compared with the deep layer cells (Aksu et al. 2008). In this study, we have investigated whether ASC taken from the two different layers might also exhibit differences in neurotrophic activity and give an indication of their usefulness for nerve regeneration therapies.
Materials and methods
Harvest and culture of ASC
All studies were approved by the University of Lausanne ethics committee. Adipose tissue (1 g) was harvested from the two abdominal layers (deep and superficial) of eight patients undergoing elective abdominoplasty. The superficial part was taken to be the region between the skin and the superficial fibrous connective tissue fascia. The deep layer adipose tissue was defined as the layer below this fascia and above the deep muscular fascia. The majority of patients were women (75%) and patient ages ranged from 36–64 years (mean 45.5 ± 3.1 years) with a body mass index from 24.0 to 40.7 (mean 29.2 ± 2.0). Adipose tissue was carefully dissected, minced by using a sterile razor blade and placed for 2 h at 37°C in a phosphate-buffered saline (PBS) solution containing 0.15% (w/v) collagenase type I (Invitrogen, UK) for enzymatic digestion. Next, the solution was passed through a 70-μm filter to remove any remaining undissociated tissue and the enzyme was neutralized by the addition of Modified Eagle’s Medium (α-MEM; Invitrogen, UK) containing 10% (v/v) fetal bovine serum (FBS). The samples were centrifuged at 800g for 5 min and the resultant stromal cell pellet was resuspended in growth medium, viz., α-MEM containing 10% (v/v) FBS and 1% (v/v) penicillin/streptomycin solution and plated in a 75 cm2 tissue-culture flask. Cells were incubated at 37°C with 5% CO2 and were maintained at sub-confluent levels with passage by trypsin/EDTA (Invitrogen, UK) when required.
Cell proliferation
The proliferation of the ASC isolated from both tissue layers was assessed for 96 h by using the CellTiter 96 Aqueous non-radioactive cell proliferation assay (Promega, USA). At passage 2, the cells were plated in a 96-well plate by using 200 μl growth medium containing 2000 cells in each well. At regular intervals (24 h, 48 h, 72 h, 96 h), 20 μl Cell Titer 96 Aqueous Assay Reagents (Promega, USA) was added and incubated for 4 h at 37°C and 5% CO2. The absorbance was recorded at 490 nm by using a spectrophotometric plate reader and measurements were calculated by subtracting the average control absorbance (medium only) from the average cell absorbance.
For calculation of population-doubling times, cells were seeded at a density of 5 × 103 cells per cm2 in tissue-culture flasks and cultured for 1 week. The cells were then counted in a hemocytometer, reseeded at the same density and cultured for another week. This process was repeated through to passage 8.
Immunocytochemistry for stem cell markers
At passage 1, deep and superficial layer ASC were trypsinized and re-plated on Labtek 8-well chamber slides at a density of 5 × 103 cells. After 24 h, the cells were fixed with 4% (w/v) paraformaldehyde and immunolabeling was performed with a MSC characterization kit (Millipore, Sweden), in which antigens including CD54, integrin β1, collagen type I, fibronectin (all positive markers) and CD14 and CD45 (negative markers) were stained according to the manufacturer’s instruction. Staining specificity was tested by the omission of primary antibodies and the inclusion of mouse or rabbit IgG. The secondary detection antibodies used were Alexa-568 goat anti-mouse IgG (1:1000) and Alexa-488 goat anti-rabbit IgG (1:1000). Expression of the antigens were observed under a Leica Aristoplan microscope and images were captured with an attached Nikon DXM1200 digital camera at 1280 × 1024 pixels.
Reverse transcription with polymerase chain reaction
For reverse transcription with the polymerase chain reaction (RT-PCR), total RNA was isolated from human ASC (passages 2-4) by using an RNeasy kit (Qiagen, Sweden) and then 1 ng RNA was incorporated into the One-Step RT-PCR kit (Qiagen) per reaction mix. Primers were manufactured by Sigma, UK (Table 1). A thermocycler (Biometra, Göttingen, Germany) was used with the following parameters: a reverse transcription step (50°C, 30 min), a nucleic acid denaturation/reverse transcriptase inactivation step (95°C, 15 min) followed by 35 cycles of denaturation (95°C, 30 s), annealing (30 s, optimized per primer set as described in Table 1) and primer extension (72°C, 1 min) followed by final extension incubation (72°C, 5 min). PCR amplicons were electrophoresed (50 V, 90 min) through a 1.5% (w/v) agarose gel and the size of the PCR products was estimated by using Hyperladder IV (Bioline, UK). Samples were visualized under UV illumination following GelRed nucleic acid stain (BioNuclear, Sweden) incorporation into the agarose.
Western blotting
Lysates of deep and superficial layer ASC at passage 1 were prepared from one 75-cm2 flask of confluent cultures essentially as previously described (Kingham et al. 2007) by using a buffer containing 5 mM EGTA, 100 mM PIPES, 5 mM MgCl2, 20% (v/v) glycerol, 0.5% (v/v) Triton X-100 and a protease inhibitor cocktail (Sigma). The DC protein assay (Bio-Rad, Sweden) was performed to quantify sample protein levels. For each sample, 40 μg protein was denatured at 95°C and loaded onto a 10% SDS-polyacrylamide gel. The proteins were transferred to a nitrocellulose membrane, and then blots were blocked with 5% (w/v) non-fat milk in TRIS-buffered saline with Tween and incubated with anti-oct3/4 (1:100; Santa Cruz Biotechnology sc-25401) or anti-nanog (1:100; Santa Cruz Biotechnology sc-33759) overnight at 4°C. After incubation with the corresponding horseradish-peroxidase-conjugated secondary antibodies and then enhanced chemiluminescence substrate, the membranes were exposed to Kodak XPS films. The blots were also re-probed with anti-actin (1:20000; Millipore MAB-1501R) as a loading control. A postive control lysate of human embryonic stem cells (MEL-1; Abcam, UK) was also used at 10 μg.
Neurite outgrowth assay
ASC (passages 2-4) isolated from the deep or superficial layers were seeded at 5 × 103 per cm2 on Lab-Tek Chamber slides (Nunc-Fischer Scientific, UK) for 24 h. Then, 1 × 103 NG108-15 cells (a neuroblastoma/glioma hybrid cell line used to model motor neurons; Choi et al. 1997) were added onto the confluent monolayer of ASC and incubated for 48 h before fixation with 4% (w/v) paraformaldehyde for 20 min at room temperature. Immunocytochemistry (essentially as above) was used to identify the NG108-15 cells and the neurite outgrowth. Monoclonal β-III tubulin (1:500; Sigma, UK) was added overnight at 4°C. The following day, after PBS washes, the slides were incubated for 1 h in the dark with the Alexa-488 Fluor goat anti-mouse secondary antibody (1:100; Invitrogen, USA). The slides were mounted in Vectashield with 4,6-diamidino-2-phenylindole (DAPI; Vector Labs, UK) and examined under a Zeiss fluorescence microscope (25× magnification). Images were captured by using Image ProPlus software (MediaCybernetics, Marlow, UK). The trace function was used to assess the following parameters: the percentage of NG108-15 cells expressing neurite-like processes, the average length of the processes (μm), and the average length of the longest process (μm). A minimum of 100 NG108-15 cell bodies were analyzed for each condition in each experiment. To confirm the origin of the neurite process outgrowth, NG108-15 cells in some experiments were pre-labeled with Cell Tracker Green CMFDA dye (30 min at 37°C and then washed twice by centrifugation in PBS) and then co-cultured with the ASC for 48 h. The neurite outgrowth assay protocol was also repeated by using the human SH-SY5Y neuronal cell line.
Enzyme-linked immunosorbant assay
ASC were seeded onto Lab-Tek Chamber slides under identical conditions to those used for neurite outgrowth assays and maintained for 72 h. The supernatant was then collected and analyzed by enzyme-linked immunosorbant assay (ELISA) with the ChemiKine BDNF (brain-derived neurotrophic factor) sandwich ELISA kit (Millipore, UK) or NGF(nerve growth factor) and GDNF (glial-derived neurotrophic factor) sandwich ELISA kits (RayBiotech, USA) according to the manufacturers' protocol. All samples were analyzed in triplicate and the absorbance was measured at 450 nm on a SpectraMax 190 microplate reader (Molecular Devices, USA). The quantity of neurotrophic factors (pg/ml) was calculated against standard curves produced by using recombinant proteins provided in the kits.
Statistical analysis
Data are presented as means±SEM from five to eight individual patient samples. The t-test or one-way analysis of variance with the Bonferonni post-hoc test for multiple comparisons was used where appropriate to determine any statistically significant differences between groups. The following convention was used in the figures: *P < 0.05; **P < 0.01.
Results
Harvest and characterization of ASC cultures
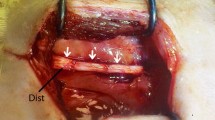
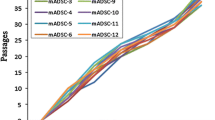
A 1-g adipose tissue biopsy was harvested from the two abdominal fat layers (deep and superficial, Fig. 1a) during the abdominoplasty procedure on patients. After enzymatic digestion and centrifugation, the stromal cell fraction was isolated from mature adipocytes and plated in a 75-cm2 flask. Following 3 weeks in culture and upon reaching confluence, cells were trypsinized and counted. At passage 1, the number of cells from the superficial layer was significantly (P < 0.05) higher than the number of cells from the deep layer (Fig. 1b). We compared the proliferation of the ASC cells (passage 2) isolated from both deep and superficial layers over a 96-h period. The cells from the superficial layer showed a trend of greater proliferation after 96 h in comparison with the deep layer and a significant difference for proliferation between 24 and 96 h in culture (Fig. 1c). We also calculated population doubling (PD) times by counting the number of cells expanded 1 week after plating at an initial density of 5 × 103 cells per cm2 (Fig. 1d). At passage 2, PD was significantly (P < 0.05) lower for superficial layer cells versus deep layer cells (98.2 ± 12 h and 167.0 ± 27.7 h, respectively). PD times remained higher for deep layer cells through to passage 8. The cultures were analyzed for phenotypic markers of MSC (Fig. 2). ASC isolated from both the deep and superficial layers were positive for CD54, stro-1 and β1 integrin proteins (general stem cell markers) produced characteristic stem cell extracellular matrix molecules (fibronectin and collagen type I) and were negative for hematopoietic cell markers (CD45 and CD14). No observable differences in phenotypic expression and morphology were seen between ASC from each layer. RT-PCR analysis showed that cultures of both deep and superficial layer cells expressed the pluripotent stem cell markers oct4 and nanog (Fig. 2q). Western blot analysis confirmed that ASC expressed these molecules at the protein level; however, the expression levels were markedly lower than those found in human embryonic stem cells (Fig. 2r).
Isolation and culture of ASC. a Fat isolated from abdominoplasty surgery shows two clearly defined regions, the superficial and deep layers separated by a connective tissue fascia. b Cell counts at passage 1 show significantly (**P < 0.01) more cells expanded in cultures taken from the superficial layer of fat. c A proliferation assay of cells seeded at passage 2 shows a significant (*P < 0.05) increase between 24 h and 96 h for ASC isolated from the superficial layer but not the deep layer. d Population doubling times were significantly (*P < 0.05) lower for the superficial layer ASC (sf) versus the deep layer ASC (dp) at passage 2. Data are means±SEM from eight individual patients
Stem cell markers in ASC cultures. Cultures of deep and superficial layer ASC were positive for general mesenchymal stem cell (MSC) markers CD54 (a, b), β1-integrin (c, d) and stro-1 (e, f), positive for extracellular matrix molecules type I collagen (g, h) and fibronectin (k, l) and negative for hematopoietic cell markers CD45 (i, j) and CD14 (m, n). Specificity of staining was confirmed by using mouse IgG (o) or rabbit IgG (p) with corresponding secondary antibodies only (red, green, respectively). Nuclei are stained blue by 4,6-diamidino-2-phenylindole (DAPI). q Reverse transcription with polymerase chain reaction (RT-PCR) shows expression of transcripts for the pluripotent cell markers oct4 and nanog in cells isolated from both deep (dp) and superficial (sf) layers (GAPDH D-glyceraldehyde-3-phosphate dehydrogenase). Size of amplicon is shown in base pairs (bp). r Western blot analysis indicates expression of oct4 and nanog proteins in both deep (dp) and superficial (sf) layer cultures. Note that human embryonic stem cell (hESC pos) lysates (10 μg) show much stronger expression compared with the ASC (40 μg)
ASC and neurotrophic activity
To compare the ability of the cells from both deep and superficial layers to promote neurite-like process outgrowth, a co-culture of the ASC and the NG108-15 cell line was performed. A comparison was made with control cultures of NG108-15 cells grown alone in the same medium used for the co-cultures. Computerized image analysis (Fig. 3a–c) of co-cultures after 48 h was used and the following quantitative parameters were analyzed: percentage of NG108-15 cells expressing neurite-like processes, average length of processes (μm), average length of the longest process (μm). The interaction between the cells isolated from the superficial layer and the NG108-15 cells showed significantly (P < 0.05) higher values for all the parameters in comparison with co-cultures with the cells from the deep layer (Fig. 3e–g). The number of NG108-15 cells expressing neurite-like processes increased in the presence of cells from the superficial layer (69.96%) in comparison with the co-cultures with the cells from the deep layer (13.22%). The average process length (for superficial: 77.59 μm; for deep: 45.3 μm) and the average length of the longest process (for superficial: 348.76 μm; for deep: 84.07 μm) of the NG108-15 cells was significantly higher for the co-cultures with the cells from the superficial layer. Pre-labeling of NG108-15 cells with Cell Tracker Green CMFDA fluorescent dye confirmed that the NG108-15 cells had extended processes indicating that any possibility for the trans-differentiation of ASC into neurons was unlikely to contribute significantly to our results (Fig. 3d). Further, to confirm that the strong neurotrophic effect of the superficial layer ASC was not specific to NG108-15 cells, we also generated co-cultures with the SH-SY5Y human neuronal cell line. Although deep layer ASC stimulated SH-SY5Y neurite outgrowth, superficial layer cells still evoked significantly longer process lengths (Fig. 3h). The presence of various nerve growth factor gene transcripts was assessed by using semi-quantitative RT-PCR methodology (Fig. 4a). Transcripts for NGF, BDNF, GDNF and neurotrophin-3 (NT3) were detected in both deep and superficial layers. The RT-PCR amplification efficacy of the mRNA was confirmed by the amplification of the D-glyceraldehyde-3-phosphate dehydrogenase housekeeping gene. ELISA analysis of cell culture supernatants showed that ASC released NGF, GDNF and BDNF (Fig. 4b). No significant differences were observed in the quantities produced by deep versus superficial layer ASC but the amounts were higher than those produced by human Schwann cells. Despite the detection of NT-3 gene transcripts, we were unable to detect significant levels of NT-3 protein in the supernatants (Fig.4b).
ASC and neurite outgrowth. The NG108-15 neuron cell line was cultured alone (a) or on confluent monolayers of ASC isolated from the deep (b) and superficial (c) layers of fat. Neurons were labeled with βIII tubulin antibody (green) and DAPI staining (blue) highlighted the nuclei of the ASC monolayers. In some experiments, Cell Tracker Green CMFDA-labeled NG108-15 cells were co-cultured with the ASC (d). As revealed by computerized image analysis, cocultures with superficial layer ASC show significantly (*P < 0.05) increased numbers of neurons with processes (e), average length of process (f) and length of longest process (g) when compared with coculture in the presence of deep layer ASC. h Data for coculture with SH-SY5Y cells. Data are means±SEM from five individual patient samples
RT-PCR analysis of neurotrophic factors. a ASC isolated from both deep and superficial layers of fat express nerve growth factor (NGF), brain-derived neurotrophic factor (BDNF), glial-derived neurotrophic factor (GDNF) and neurotrophin-3 (NT3) transcripts. The housekeeping gene D-glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was also analyzed. Amplicon size is indicated in base pairs (bp). b Enzyme-linked immunosorbant assay was used to determine NGF, GDNF and BDNF protein levels in cell culture supernatants from deep and superficial layer ASC and compared with expression levels in human Schwann cell cultures. Data are means±SEM from five individual patients
Discussion
Advances in regenerative medicine therapy rely on identifying the ideal cells to be used for any particular application. Stem and progenitor cells can be harvested from many adult tissues including bone marrow, skin, muscle and fat (Barrilleaux et al. 2006). In particular, human subcutaneous adipose tissue is an abundant and accessible source of multi-potent adult stem cells (Gimble et al. 2007). Adipose tissue is mainly obtained during liposuction or abdominoplasty and with the increased incidence of obesity in our society, these operations are becoming more common, resulting in the increased availability of adipose tissue. In this study, we have isolated ASC from the two subcutaneous abdominal fat layers (deep and superficial) during abdominoplasty procedures and have subsequently assessed the capacity of the cells to proliferate and their respective neurotrophic profiles. We have found that cells cultured from the superficial layer might be a better source of ASC to use in nerve repair and other regenerative therapies.
We have found it easy to identify the two layers in the adipose tissue separated by the fascia. This allows either precise excision of the tissue or controlled liposuction to obtain the desired cell population to be used in the clinic. The superficial layer of fat yields the greatest number of cells and they proliferate significantly faster than ASC isolated from the deep layer. A recent study has shown that significant differences exist in the amount of cells that can be isolated from the various body regions and that the lower abdominal region is the best source (Padoin et al. 2008). In contrast, another study has demonstrated no difference in the viable cell number isolated from the abdomen versus hip or mamma regions but has revealed that liposuction-extracted cells proliferate at a slower rate than those obtained by resection (Oedayrajsingh-Varma et al. 2006). The ability of cells to differentiate into multiple lineages is determined by their expression of various “stemness”-related transcription factors. We have found that both deep and superficial layer cells express oct4 and nanog, consistent with previous studies of human ASC (Baglioni et al. 2009; Riekstina et al. 2009). Although the functional role for these molecules in adult stem cells is controversial, studies of embryonic stem cells have shown that these factors act together to maintain pluripotency (Rodda et al. 2005). Furthermore, recent studies of ASC indicate that the addition of exogenous oct4 improves cell proliferation and differentiation potency through the epigenetic reprogramming of endogenous Oct4 and nanog genes (Kim et al. 2009). Our cell cultures also express the stro-1 surface protein. Stro-1 expression identifies perivascular cells in adipose tissue and cells fractionated by using stro-1 antibody exhibit enhanced clonogenic fibroblastic colony counts (Zannettino et al. 2008). We have detected no phenotypic differences for general MSC markers (CD54, β1-inetgrin, collagen type I and fibronectin) expression between the deep and superficial layer cells. A search of the literature indicates that ASC cultures consist in a highly heterogeneous population of cells that varies from laboratory to laboratory and might be influenced by the harvesting site, donor patient age and body mass index and by the subsequent isolation protocols and the media and supplements used to expand the cells in culture. In this study, we have examined the crude populations of cells taken from the deep and superficial layers. However, it would be interesting to determine whether differences occur in the percentage of cells expressing a pericyte phenotype (CD146+/CD34−) or endothelial progenitor (CD31+/CD34+) or mature endothelial cell phenotype (CD31+/CD34−), all of which have been proposed to mediate the beneficial effects of adipose tissue cultures (Zimmerlin et al. 2010). CD271-selected populations have also been shown to exhibit greater differentiation potential than crude cultures (Quirici et al. 2009). In our preliminary studies with immuno-magnetic cell sorting, we have found that both deep and superficial layer cultures contain 5%-10% of cells that express the CD271 protein (data not shown).
Having determined that cells isolated from the deep and superficial layers of fat exhibit a stem cell phenotype, we next sought to identify their respective neurotrophic potentials. Using our previously published co-culture model with the NG108-15 cell line (Kingham et al. 2007), we found that ASC isolated from the superficial layer of fat significantly enhanced neurite outgrowth compared with deep layer cells. As far as we are aware, this is the first study to show that human ASC can directly promote neurite outgrowth. We and other groups have shown that rat ASC enhance neurite outgrowth but only after treatment with various stimulating factors (Jiang et al. 2008; Kingham et al. 2007; Xu et al. 2008). Untreated rat ASC can however protect against neuronal apoptosis, an effect in part mediated by their expression of soluble growth proteins, such as insulin-like growth factor (Wei et al. 2008). Therefore, we decided to examine the expression of neurotrophic factors in cells taken from the various layers. Analysis of RNA transcripts and ELISA studies showed similar levels of NGF, BDNF and GDNF in both deep and superficial layer ASC. The quantity of protein released by the cells was greater than that from Schwann cell cultures suggesting that the cells significantly influenced neural regeneration mechanisms. Although our results did not identify a factor to account for the differences in neurite outgrowth of NG108-15 cells, the observation that human abdominal ASC express multiple growth factors that could be of benefit during neural repair is of importance.
In our direct co-culture model, the deep and superficial layer cells might express different surface molecules known to regulate neurite outgrowth. For example, cell adhesion molecules such as the cadherins, L1 and neural cell adhesion molecule are expressed in various stem cell systems but also play a role in neurite outgrowth. Extracellular matrix (ECM) molecules such as laminin can also potentiate nerve regeneration (Chen et al. 2007; Chernousov and Carey 2000) and a recent study has shown that ASC express laminin, which can facilitate axon sorting, myelination and functional recovery in mice deficient for Schwann-cell-derived laminin (Carlson et al. 2010). Remodeling of the ECM and neurite outgrowth involves interactions with other molecules such as the matrix metalloproteinases, which are also produced by ASC (Kim et al. 2007). Angiogenic molecules such as vascular endothelial growth factor (VEGF) can also promote neurite outgrowth (Sondell et al. 2000). VEGF is expressed at high levels by ASC (Rehman et al. 2004) and deep and superficial layer ASC might express different levels of this factor given the variation in vascularity across the adipose tissue layers.
To date, most studies have focused on differentiating human ASC toward a neural phenotype for transplantation into injured patients (Anghileri et al. 2008; Franco Lambert et al. 2009; Safford et al. 2002). These studies have shown that treatment with a variety of induction protocols can lead to the expression of neural and glial markers but they have not examined the neurotrophic potential of undifferentiated cells. Our study is the first to examine the neurotrophic factor profile of human ASC. Human ASC have recently been transplanted into athymic rats subjected to sciatic nerve transection (Santiago et al. 2009). Treatment with ASC enhances nerve regeneration and reduces muscle atrophy but no evidence has been seen for an in vivo trans-differentiation of the cells toward a Schwann cell phenotype (Santiago et al. 2009). Some of the benefits afforded by the cells are thus probably a result of their production of neurotrophic factors and other molecules involved in the ECM.
In conclusion, our study has shown that human ASC express a range of neurotrophic factors and cells isolated from the superficial abdominal fat layer promote neurite process outgrowth in vitro. Together with their favorable proliferation kinetics, future in vivo nerve regeneration studies with human superficial layer ASC are warranted.
References
Aksu AE, Rubin JP, Dudas JR, Marra KG (2008) Role of gender and anatomical region on induction of osteogenic differentiation of human adipose-derived stem cells. Ann Plast Surg 60:306–322
Anghileri E, Marconi S, Pignatelli A, Cifelli P, Galie M, Sbarbati A, Krampera M, Belluzzi O, Bonetti B (2008) Neuronal differentiation potential of human adipose-derived mesenchymal stem cells. Stem Cells Dev 17:909–916
Baglioni S, Francalanci M, Squecco R, Lombardi A, Cantini G, Angeli R, Gelmini S, Guasti D, Benvenuti S, Annunziato F, Bani D, Liotta F, Francini F, Perigli G, Serio M, Luconi M (2009) Characterization of human adult stem-cell populations isolated from visceral and subcutaneous adipose tissue. FASEB J 23:3494–3505
Barrilleaux B, Phinney DG, Prockop DJ, O'Connor KC (2006) Review: ex vivo engineering of living tissues with adult stem cells. Tissue Eng 12:3007–3019
Bunnell BA, Flaat M, Gagliardi C, Patel B, Ripoll C (2008) Adipose-derived stem cells: isolation, expansion and differentiation. Methods 45:115–120
Carlson KB, Singh P, Feaster MM, Ramnarain A, Pavlides C, Chen ZL, Yu WM, Feltri ML, Strickland S (2010) Mesenchymal stem cells facilitate axon sorting, myelination, and functional recovery in paralyzed mice deficient in Schwann cell-derived laminin. Glia 59:267–277
Chen ZL, Yu WM, Strickland S (2007) Peripheral regeneration. Annu Rev Neurosci 30:209–233
Chernousov MA, Carey DJ (2000) Schwann cell extracellular matrix molecules and their receptors. Histol Histopathol 15:593–601
Choi RC, Pun S, Dong TT, Wan DC, Tsim KW (1997) NG108-15 cells induce the expression of muscular acetylcholinesterase when co-cultured with myotubes. Neurosci Lett 236:167–170
Dezawa M, Takahashi I, Esaki M, Takano M, Sawada H (2001) Sciatic nerve regeneration in rats induced by transplantation of in vitro differentiated bone-marrow stromal cells. Eur J Neurosci 14:1771–1776
Enzmann GU, Benton RL, Talbott JF, Cao Q, Whittemore SR (2006) Functional considerations of stem cell transplantation therapy for spinal cord repair. J Neurotrauma 23:479–495
Franco Lambert AP, Fraga Zandonai A, Bonatto D, Cantarelli Machado D, Pêgas Henriques JA (2009) Differentiation of human adipose-derived adult stem cells into neuronal tissue: does it work? Differentiation 77:221–228
Gimble JM, Katz AJ, Bunnell BA (2007) Adipose-derived stem cells for regenerative medicine. Circ Res 100:1249–1260
Jiang L, Zhu JK, Liu XL, Xiang P, Hu J, Yu WH (2008) Differentiation of rat adipose tissue-derived stem cells into Schwann-like cells in vitro. NeuroReport 19:1015–1019
Kim JH, Jee MK, Lee SY, Han TH, Kim BS, Kang KS, Kang SK (2009) Regulation of adipose tissue stromal cells behaviors by endogenic Oct4 expression control. PLoS ONE 4:e7166
Kim Y, Kim H, Cho H, Bae Y, Suh K, Jung J (2007) Direct comparison of human mesenchymal stem cells derived from adipose tissues and bone marrow in mediating neovascularization in response to vascular ischemia. Cell Physiol Biochem 20:867–876
Kingham PJ, Kalbermatten DF, Mahay D, Armstrong SJ, Wiberg M, Terenghi G (2007) Adipose-derived stem cells differentiate into a Schwann cell phenotype and promote neurite outgrowth in vitro. Exp Neurol 207:267–274
Lundborg G (2000) A 25-year perspective of peripheral nerve surgery: evolving neuroscientific concepts and clinical significance. J Hand Surg Am 25:391–414
Oedayrajsingh-Varma MJ, Ham SM van, Knippenberg M, Helder MN, Klein-Nulend J, Schouten TE, Ritt MJ, Milligen FJ van (2006) Adipose tissue-derived mesenchymal stem cell yield and growth characteristics are affected by the tissue-harvesting procedure. Cytotherapy 8:166–177
Padoin AV, Braga-Silva J, Martins P, Rezende K, Rezende AR, Grechi B, Gehlen D, Machado DC (2008) Sources of processed lipoaspirate cells: influence of donor site on cell concentration. Plast Reconstr Surg 122:614–618
Pfister LA, Papaloizos M, Merkle HP, Gander B (2007) Nerve conduits and growth factor delivery in peripheral nerve repair. J Peripher Nerv Syst 12:65–82
Quirici N, Scavullo C, Girolamo L de, Lopa S, Arrigoni E, Deliliers GL, Brini AT (2009) Anti-L-NGFR and -CD34 monoclonal antibodies identify multipotent mesenchymal stem cells in human adipose tissue. Stem Cells Dev 19:915–925
Rehman J, Traktuev D, Li J, Merfeld-Clauss S, Temm-Grove CJ, Bovenkerk JE, Pell CL, Johnstone BH, Considine RV, March KL (2004) Secretion of angiogenic and antiapoptotic factors by human adipose stromal cells. Circulation 109:1292–1298
Riekstina U, Cakstina I, Parfejevs V, Hoogduijn M, Jankovskis G, Muiznieks I, Muceniece R, Ancans J (2009) Embryonic stem cell marker expression pattern in human mesenchymal stem cells derived from bone marrow, adipose tissue, heart and dermis. Stem Cell Rev 5:378–386
Rodda DJ, Chew JL, Lim LH, Loh YH, Wang B, Ng HH, Robson P (2005) Transcriptional regulation of nanog by OCT4 and SOX2. J Biol Chem 280:24731–24737
Safford KM, Hicok KC, Safford SD, Halvorsen YD, Wilkison WO, Gimble JM, Rice HE (2002) Neurogenic differentiation of murine and human adipose-derived stromal cells. Biochem Biophys Res Commun 294:371–379
Santiago LY, Clavijo-Alvarez J, Brayfield C, Rubin JP, Marra KG (2009) Delivery of adipose-derived precursor cells for peripheral nerve repair. Cell Transplant 18:145–158
Schipper BM, Marra KG, Zhang W, Donnenberg AD, Rubin JP (2008) Regional anatomic and age effects on cell function of human adipose-derived stem cells. Ann Plast Surg 60:538–544
Sondell M, Sundler F, Kanje M (2000) Vascular endothelial growth factor is a neurotrophic factor which stimulates axonal outgrowth through the flk-1 receptor. Eur J Neurosci 12:4243–4254
Summa PG di, Kingham PJ, Raffoul W, Wiberg M, Terenghi G, Kalbermatten DF (2009) Adipose-derived stem cells enhance peripheral nerve regeneration. J Plast Reconstr Aesthet Surg 63:1544–1552
Sterodimas A, Faria J de, Nicaretta B, Pitanguy I (2009) Tissue engineering with adipose-derived stem cells (ADSCs): current and future applications. J Plast Reconstr Aesthet Surg 63:1886–1892
Terenghi G, Wiberg M, Kingham PJ (2009) Use of stem cells for improving nerve regeneration. Int Rev Neurobiol 87:393–403
Walsh S, Midha R (2009) Practical considerations concerning the use of stem cells for peripheral nerve repair. Neurosurg Focus 26:E2
Wei X, Du Z, Zhao L, Feng D, Wei G, He Y, Tan J, Lee WH, Hampel H, Dodel R, Johnstone BH, March KL, Farlow MR, Du Y (2008) IFATS series. The conditioned media of adipose stromal cells protect against hypoxia-ischemia-induced brain damage in neonatal rats. Stem Cells 27:478–488
Xu Y, Liu Z, Liu L, Zhao C, Xiong F, Zhou C, Li Y, Shan Y, Peng F, Zhang C (2008) Neurospheres from rat adipose-derived stem cells could be induced into functional Schwann cell-like cells in vitro. BMC Neurosci 9:21
Zannettino AC, Paton S, Arthur A, Khor F, Itescu S, Gimble JM, Gronthos S (2008) Multipotential human adipose-derived stromal stem cells exhibit a perivascular phenotype in vitro and in vivo. J Cell Physiol 214:413–421
Zimmerlin L, Donnenberg VS, Pfeifer ME, Meyer EM, Peault B, Rubin JP, Donnenberg AD (2010) Stromal vascular progenitors in adult human adipose tissue. Cytometry A 77:22–30
Author information
Authors and Affiliations
Corresponding author
Additional information
Grant support
This study was supported by the Swedish Medical Research Council, Umeå University, County of Västerbotten, Magn. Bergvalls Stiftelse, Clas Groschinskys Minnesfond, Åke Wibergs Stiftelse, the Gunvor and Josef Aner Foundation, SwissLife Foundation, the SUVA and the University of Lausanne FBM.
Rights and permissions
About this article
Cite this article
Kalbermatten, D.F., Schaakxs, D., Kingham, P.J. et al. Neurotrophic activity of human adipose stem cells isolated from deep and superficial layers of abdominal fat. Cell Tissue Res 344, 251–260 (2011). https://doi.org/10.1007/s00441-011-1142-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00441-011-1142-5