Abstract
Thunbergia laurifolia Linn (Rang Chuet) possesses antioxidant and anti-inflammatory properties as well as anticancer activities. The aim of the present study was to evaluate the efficacy of T. laurifolia in reducing inflammation from pathological changes in Syrian hamsters infected with the human liver fluke Opisthorchis viverrini. Hamster groups were also administered N-nitrosodimethylamine (NDMA) and treated with T. laurifolia. Light microscopic observation of histopathological changes, liver function tests for alanine transaminase (ALT) and alkaline phosphatase (ALP) and kidney function tests for blood urea nitrogen (BUN) and creatinine were performed. Antioxidant effects of both fresh and dried Rang Chuet solutions were observed. Analysis of the histopathological changes showed anti-inflammatory properties, both in the case of O. viverrini infection or with NDMA administration, by reducing the aggregation of inflammatory cells surrounding the hepatic bile ducts as indicated by normal serum ALT, ALP, BUN and creatinine levels in treated Syrian hamsters. The present study found that fresh and dried Rang Chuet solutions clearly reduced the inflammatory cells in both O. viverrini-infected and NDMA-administered groups and was correlated with the total antioxidant capacity. These findings suggest that T. laurifolia possesses antioxidant and anti-inflammatory properties and that its application may be useful for prevention of the inflammatory process, one of the risk factors of O. viverrini-associated cholangiocarcinoma (CCA).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Thunbergia laurifolia Linn, commonly known as laurel clock vine or blue trumpet vine, is native to India (Starr et al. 1999), and in the Indomalaya ecozone, the species occurs from Indochina to Malaysia (Schonenberger 1999). It is locally known as “kar tuau” in Malaysia and “Rang Chuet” in Thailand (Chan and Lim 2006). In Malaysia, juice from crushed leaves of T. laurifolia are taken for menorrhagia, placed into the ear for deafness and applied as a poultice for cuts and boils (Burkill 1966). In Thailand, leaves are used as an antipyretic and for their detoxifying effects, e.g., as an antidote for poisons (Ussanawarong et al. 2000; Ussanawarong and Thesiri 2001; Kanchanapoom et al. 2002). Several Thai herbal companies have started producing and exporting Rang Chuet tea (Chan and Lim 2006). The tea has been claimed to counteract the harmful effects of drugs, alcohol and cigarettes.
Opisthorchis viverrini, a human liver fluke, is the primary risk factor for cholangiocarcinoma (CCA), a rare but highly fatal disease most prevalent in Southeast Asia including Thailand (IARC 1994). Humans are infected by ingestion of raw cyprinid fish, which are contaminated by the infective stage known as metacercariae. After O. viverrini metacercariae ingestion, the excysted juveniles migrate to the bile canal at the duodenum and grow to adulthood at the common bile duct or gallbladder, an area which is suitable for their survival. At the early stages of infection, liver changes are due to the inflammatory response (eosinophils, monocytes and neutrophils) around the juvenile flukes in the intrahepatic bile ducts. The severity of inflammation gradually increases and reaches a maximum at about 3 to 4 weeks post-infection, as evidenced by the accumulation of mononuclear cells and eosinophils which infiltrate the intrahepatic bile ducts. The virulence of the disease also depends on the number of parasites and the duration of infection, which involves the host's immune response such as cytokine expression and free radicals (Pinlaor et al. 2004). Chronic infection with O. viverrini for many years is associated with hepatobiliary diseases (Sripa 2003) including the development of hepatobiliary cancer and CCA. Reducing the behavior of eating raw fish has proven to be difficult, so the infection rate of this parasite remains high. Therefore, reducing the pathogenesis from an O. viverrini infection may be one of the preferred options to reduce the risk of CCA development.
Our previous report (Boonjaraspinyo et al. 2009) showed that a traditional medicine, a mixture of turmeric and fingerroot, reduced the inflammatory cells surrounding the hepatic bile duct but could not be used for prevention of cholangiocarcinogenesis. Thus, the present study was performed to evaluate the efficacy of another Thai medicinal plant, T. laurifolia or Rang Chuet in Thai. T. laurifolia is widely used for detoxification from lead poisoning or other toxins (Ussanawarong et al. 2000; Ussanawarong and Thesiri 2001; Chattaviriya et al. 2010; Tangpong and Satarug 2010; Palipoch et al. 2011). Recently, several papers have reported that apigenin, one of the flavonoid compounds in Rang Chuet (Oonsivilai et al. 2007), has antioxidant (Chan and Lim 2006; Oonsivilai et al. 2008) and anticancer properties (Ujiki et al. 2006; Ruela-de-Sousa et al. 2010).
The anti-inflammatory and antioxidant effects of Rang Chuet were studied in a Syrian hamster opisthorchiasis model and in hamsters with N-nitrosodimethylamine administration (NDMA). Histopathological changes were observed. Liver function tests for alanine transaminase (ALT) and alkaline phosphatase (ALP) and kidney function tests for blood urea nitrogen (BUN) and creatinine were performed. Total antioxidant capacity was measured by FRAP assay.
Materials and methods
Parasite preparation
Parasites were prepared following the method in a previous report (Wonkchalee et al. 2011a). In brief, O. viverrini metacercariae were obtained from naturally infected cyprinid fish in an endemic area of Khon Kaen, northeast Thailand. Fresh fish were digested in 1% pepsin/HCl and incubated at 37°C for 1 h and then filtered and precipitated with normal saline in a sedimentation jar. Afterwards the metacercariae—oval-shaped, with large, black excretory bladders—were identified under a dissecting microscope.
Rang Chuet preparation
Rang Chuet was acquired from a farm in Khon Kaen province, Thailand. Fresh and dried leaves were used; fresh leaves were minced in distilled water and dried leaves were ground into a powder and then kept until used. Rang Chuet powder was diluted with distilled water, then boiled for 30 min and 0.5 ml (or 100 mg/kg/day) of the solution was used for oral treatment of the assigned groups.
FRAP assay
The ferric-reducing antioxidant power (FRAP) of extracts was determined following the previous method of Chan and Lim (2006), with modifications. Samples had to be diluted because precipitation occurred upon color development. Dilutions of extracts (1 ml) were added to 2.5 ml phosphate buffer (0.2 M, pH 6.6) and 2.5 ml of potassium ferricyanide (1% w/v). Each mixture was incubated at 50°C for 20 min. A total of 2.5 ml trichloroacetic acid solution (10% w/v) was added to the mixture to stop the reaction. The mixture was then separated into aliquots of 2.5 ml and diluted with 2.5 ml water. A total of 500 μl ferric chloride solution (0.1% w/v) was added, and the resulting solution was allowed to stand for 30 min until the color was fully developed. Absorbance measured at 700 nm in triplicate was used to normalized with the Fe2+ standard curve. Results of the FRAP assay were expressed as millimoles per Fe2+ per gram.
Infection with O. viverrini
Fifteen Syrian hamsters were each administered 50 O. viverrini metacercariae by oral intragastric intubation, as in a previous protocol (Wonkchalee et al. 2011b) and then fed with the assigned herb.
Animal groups
Thirty Syrian hamsters were divided into six groups: 1) infected with O. viverrini alone (OV), 2) infected with O. viverrini and administered with fresh Rang Chuet solutions (OVFRC), 3) infected with O. viverrini and administered with dried Rang Chuet solutions (OVDRC), 4) administered with NDMA alone (NDMA), 5) administered with NDMA and fresh Rang Chuet solutions (NDMAFRC) and 6) administered with NDMA and dried Rang Chuet solutions (NDMADRC). Hamsters were sacrificed on day 30; whole liver tissues were collected for observation of histopathological changes, and sera were tested for liver and kidney function. The protocol was approved by the Animal Ethics Committee of the Faculty of Medicine, Khon Kaen University, Thailand (Ethical Clearance No. AEKKU23/2554).
Light microscopic observation
Hamster livers were fixed in 10% buffered formalin. After fixation, liver tissue was soaked with phosphate-buffered saline and then dehydrated through a series of various concentrations of ethyl alcohol. The tissue was then embedded in paraffin wax. Sections of 5 μm thickness were cut using a microtome and then stained with hematoxylin–eosin and observed under a light microscope, as in previous studies (Boonmars et al. 2009; Boonjaraspinyo et al. 2011). Photographs of each slide were taken at 10× and 40× magnification. The histological feature of liver biopsy and grading criteria levels are shown in Table 1.
Biochemical estimation
Measurement of serum liver enzymes and kidney function
Syrian hamster sera were obtained to determine liver and kidney damage; ALT, ALP, BUN and creatinine analysis was performed at the Chemistry Room, Community Laboratory, Faculty of Associated Medical Sciences, Khon Kaen University.
Statistical analysis
The data on histopathological changes and serum levels of ALT, ALP, BUN and creatinine were presented as means ± SD. Statistics were analyzed using one-way ANOVA (SPSS version 13.0, USA). Values were considered statistically significant when p < 0.05.
Results
Total antioxidant capacity
The effect of the temperature of diluents on total antioxidant capacity was evaluated. Fresh and dried Rang Chuet solutions using room temperature water resulted in 10.36 and 95.12 mmol Fe2+/g sample, respectively, while fresh and dried Rang Chuet solutions using boiling water showed 15.72 and 156.29 mmol Fe2+/g sample, respectively. Therefore, boiled dried Rang Chuet solutions were used to treat animal models.
Inhibitory effects of Rang Chuet on inflammation
Observation of the gross pathology of the livers revealed few differences between groups with O. viverrini infection (OV) and those treated with Rang Chuet (OVFRC and OVDRC). Liver surfaces were smooth and shiny, with slightly opaque common bile ducts and straw-colored bile fluid. However, a reduction in thickening of the wall of the common bile duct was evident in both OVFRC and OVDRC groups (Fig. 1b, c).
Gross and histopathological changes in the group of O. viverrini infection (OV; a, d), O. viverrini infection with fresh Rang Chuet solutions (OVFRC; b, e), O. viverrini infection with dried Rang Chuet solutions (OVDRC; c, f) and the group of administration NDMA (NDMA; g, j), administration NDMA with fresh Rang Chuet solutions (NDMAFRC; h, k), administration NDMA with dried Rang Chuet solutions (OVDRC;i, l). GB gall bladder, CBC common bile duct, P parasite. Asterisk indicates inflammation. Magnification × 10
Analysis of histopathological changes focused on the aggregation of inflammatory cells surrounding the hepatic bile ducts and liver tissue, and hepatic bile duct proliferation. Histopathological changes in the O. viverrini-infected groups (Fig. 1a–f) were similar to those observed in the NDMA groups (Fig. 1g–l). Aggregation of inflammatory cells surrounding the hepatic bile ducts was observed both in O. viverrini-infected groups (Fig. 1a, d) and in those receiving NDMA administration (Fig. 1g, j). A reduction of inflammatory cells surrounding the intrahepatic bile ducts was observed in the OVFRC, OVDRC, NDMAFRC and NDMADRC groups (Fig. 1e, f, k, l). The degree of inflammatory aggregation is shown in Table 1.
Effects of Rang Chuet on liver enzyme and kidney function
Table 2 shows the activities of serum ALT, ALP, BUN and creatinine, which correlate with histopathological changes (Fig. 1). The liver and kidney serum markers (ALT, ALP, BUN and creatinine) in the Rang Chuet group remained within normal levels. Serum ALT levels increased about 3- to 10-fold after Syrian hamsters were administered with NDMA or infected with O. viverrini. There was a significant decrease in serum ALT in the groups of OVFRC (p = 0.012), OVDRC (p = 0.001) and NDMAFRC (p = 0.000) at 1 month. Serum BUN, ALP and creatinine levels in the OV, OVFRC, OVDRC, NDMA, NDMAFRC and NDMADRC groups remained within normal levels.
Discussion
The present study clearly shows that Rang Chuet has anti-inflammatory and antioxidant properties which improve liver function in hamsters with liver fluke infection or after administration of NDMA. Pathological changes, as evidenced by a reduction of the inflammatory cells surrounding the hepatic bile ducts, were correlated with the results of the liver function tests (especially ALT) showing decreased liver cell damage. Higher antioxidant activity, as shown by FRAP analysis, was due to the reduction of inflammatory cells surrounding the hepatic bile duct and to the reduction of ALT levels.
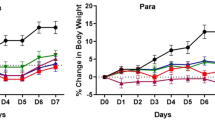
Examination of pathological changes in the livers revealed the anti-inflammatory property of Rang Chuet in Syrian hamsters with inflammatory cells induced by O. viverrini infection or NDMA administration. This was in agreement with a previous report in which Rang Chuet, administered at 5 g/kg to mice with induced paw edema, demonstrated anti-inflammatory activity at 3 h (p > 0.01) and 6 h (p > 0.001) (Pongphasuk et al. 2005). Histopathological results, supported by liver function tests, showed that Rang Chuet has no toxic side effects; this was in line with previous reports where Rang Chuet demonstrated no toxic effects in a mouse model at 8 g/kg/days for 30 days (Pongphasuk et al. 2005) and in a rat model at up to 2 g/kg/days for 6 months (Chivapat et al. 2009). The administration of NDMA was directly toxic to liver tissue and induced the infiltration of inflammatory cells surrounding the biliary tree and hepatic tissue by day 30, similar to the findings of Boonmars et al. (2009). Moreover, NDMA administration in rats induced chronic inflammation and led to liver tumors (Peto et al. 1991), bile duct proliferation and liver fibrosis (George et al. 2001). The anti-inflammatory property of Rang Chuet was clearly demonstrated by the reduction of inflammatory cells in hepatic tissue, leading to decreased serum ALT (Table 1) in all groups treated with a Rang Chuet solution. This result agrees with a previous study in which the extract compounds from Rang Chuet showed anti-inflammatory effects as well as antioxidant effects as determined by FRAP assay (Oonsivilai et al. 2007). In addition, phenolic profiling of Rang Chuet water extract revealed the presence of apigenin and apigenin glucosides as well as phenolic acids such as caffeic acid, gallic acid and protocatechuic acid (Oonsivilai et al. 2007); these compounds are involved in its anti-inflammatory and anticancer properties. About eight steroid substances have also reportedly been found by thin-layer chromatographic study of the extracts.
The histopathology of Syrian hamsters infected with O. viverrini was similar to previous reports (Boonmars et al. 2007; 2008; 2009). At 30 days post-infection, a peak of inflammatory cells (mononuclear cells and eosinophils) was observed surrounding the hepatic bile ducts as well as epithelial hyperplasia, goblet cell metaplasia, adenomatous metaplasia and thickened periductal fibrosis (Fig. 1), findings which correspond with increased serum ALT level. A slight decrease in inflammatory cells was observed, both in the case of O. viverrini infection and NDMA administration, when a Rang Chuet diet was administered. Although the results were similar for all Rang Chuet-treated groups, different inflammatory inducers may trigger different host immune response mechanisms. The metabolized product from NDMA is directly toxic to the liver and subsequently generates an inflammatory cell response, whereas O. viverrini induces a host immune response, as evidenced by inflammatory cells surrounding the hepatic bile duct. Moreover, the present study shows that the antioxidant property was in agreement with previous reports, which found that Rang Chuet powder diluted with boiling water had a high antioxidant capacity with low toxicity (Wong et al. 2006; Oonsivilai et al. 2008).
The present study demonstrates the advantages of Rang Chuet as an antioxidant and anti-inflammatory agent in Syrian hamsters that were administered NDMA as well as in those infected with O. viverrini, leading to a reduction in liver pathology and an improvement in liver function.
References
Boonjaraspinyo S, Boonmars T, Aromdee C, Srisawangwong T, Kaewsamut B, Pinlaor S, Yongvanit P, Puapairoj A (2009) Turmeric reduces inflammatory cells in hamster opisthorchiasis. Parasitol Res 105:1459–1463
Boonjaraspinyo S, Boonmars T, Aromdee C, Puapairoj A, Wu Z (2011) Indirect effect of a turmeric diet: enhanced bile duct proliferation in Syrian hamsters with a combination of partial obstruction by Opisthorchis viverrini infection and inflammation by N-nitrosodimethylamine administration. Parasitol Res 108(1):7–14
Boonmars T, Boonjaraspinyo S, Kaewsamut B (2009) Animal models for Opisthorchis viverrini infection. Parasitol Res 104:701–703
Boonmars T, Srirach P, Kaewsamut B, Srisawangwong T, Pinlaor S, Pinlaor P, Yongvanit P, Sithithaworn P (2008) Apoptosis-related gene expression in hamster opisthorchiasis post praziquantel treatment. Parasitol Res 102:447–455
Boonmars T, Srisawangwong T, Srirach P, Kaewsamut B, Pinlaor S, Sithithaworn P (2007) Apoptosis-related gene expressions in hamsters re-infected with Opisthorchis viverrini and re-treated with praziquantel. Parasitol Res 102:57–62
Burkill I.H (1966) A dictionary of the economic products of the Malay Peninsula. Volume II (I–Z). Ministry of Agriculture and Cooperatives, Kuala Lumpur.
Chan EWC, Lim YY (2006) Antioxidant activity of Thunbergia laurifolia tea. Journal of Tropical Forest Science 18(2):130–136
Chattaviriya P, Morkmek N, Lertprasertsuke N, Ruangyuttikarn W (2010) Drinking Thunbergia laurifolia Lindl. leaf extract helps prevent renal toxicity induced by cadmium in rats. Thai J Toxicology 25(2):124–132
Chivapat S, Chavalittumrong P, Attawish A, Bansiddhi J, Padungpat S (2009) Chronic toxicity of Thunbergia laurifolia Lindl. extract. Journal of Thai Traditional and Alternative Medicine 7(1):18–25
George J, Rao KR, Stern R, Chandrakasan G (2001) Dimethylnitrosamine-induced liver injury in rats: the early deposition of collagen. Toxicology 156:129–138
IARC (1994) Infection with liver flukes (Opisthorchis viverrini, Opisthorchis felineus and Clonorchis sinensis). IARC monographs on the evaluation of carcinogenic risks to humans 61:121–175
Kanchanapoom T, Kasai R, Yamasaki K (2002) Iridoid glucosides from Thunbergia laurifolia. Phytochemistry 60(8):769–771
Oonsivilai R, Cheng C, Bomser J, Ferruzzi MG, Ningsanond S (2007) Phytochemical profiling and phase II enzyme-inducing properties of Thunbergia laurifolia Lindl. (RC) extracts. J Ethnopharmacol 114(3):300–306
Oonsivilai R, Ferruzzi MG, Ningsanond S (2008) Antioxidant activity and cytotoxicity of Rang Chuet (Thunbergia laurifolia Lindl.) extracts. As J Food Ag-Ind 1(02):116–128
Palipoch S, Jiraungkoorskul W, Tansatit T, Preyavichyapugdee N, Jaikua W, Kosai P (2011) Protective efficiency of Thunbergia laurifolia leaf extract against lead (II) nitrate-induced toxicity in Oreochromis niloticus. Journal of Medicinal Plants Research 5(5):719–728
Pongphasuk N, Khunkitti W, Chitcharoenthum M (2005) Traditional medicine and nutraceuticals. WOCMAP Congress on Medicinal and Aromatic Plants—Volume 6, Palaniswamy UR, Gardner ZE. Craker LE eds. ISHS, Acta Horticulturae, p 680
Peto R, Gray R, Brantom P, Grasso P (1991) Dose and time relationships for tumor induction in the liver and esophagus of 4080 inbred rats by chronic ingestion of N-nitrosodiethylamine or N-nitrosodimethylamine. Cancer Res 51:6452–6469
Pinlaor S, Hiraku Y, Ma N, Yongvanit P, Semba R, Oikawa S, Murata M, Sripa B, Sithithaworn P, Kawanishi S (2004) Mechanism of NO-mediated oxidative and nitrative DNA damage in hamsters infected with Opisthorchis viverrini: a model of inflammation-mediated carcinogenesis. Nitric Oxide 11:175–183
Ruela-de-Sousa RR, Fuhler GM, Blom N, Ferreira CV, Aoyama H, Peppelenbosch MP (2010) Cytotoxicity of apigenin on leukemia cell lines: implications for prevention and therapy. Cell Death Dis 1:19
Schonenberger J (1999) Floral structure, development and diversity in Thunbergia (Acanthaceae). Botanical Journal of the Linnean Society 130:1–36
Sripa B (2003) Pathobiology of opisthorchiasis: an update. Acta Tropica 88:209–220
Starr F, Martz K, Loope LL (1999) New plant records from East Maui for 1998. Bishop Mus Occ Pap 59(2):1–15
Tangpong J, Satarug S (2010) Alleviation of lead poisoning in the brain with aqueous leaf extract of the Thunbergia laurifolia (Linn.). Toxicol Lett 198(1):83–88
Ujiki MB, Ding XZ, Salabat MR, Bentrem DJ, Golkar L, Milam B, Talamonti MS, Bell RH, Iwamura T, Adrian TE (2006) Apigenin inhibits pancreatic cancer cell proliferation through G2/M cell cycle arrest. Mol Cancer 29:5–76
Ussanawarong S, Thesiri T, Mahakunakorn T, Parasupattana S (2000) Effect of Thunbergia laurifolia Linn on detoxification of paraquat. Khon Kaen University Research Journal 5.
Ussanawarong S, Thesiri T (2001) Effect of Thunbergia laurifolia Linn on detoxification of parathion in rat. Khon Kaen University Research Journal 6:3–13
Wong CC, Li H, Cheng K, Chen F (2006) A systemic survey of antioxidant activity of 30 Chinese medicinal plants using the ferric reducing antioxidant power assay. Food Chem 97:705–711
Wonkchalee O, Boonmars T, Kaewkes S, Chamgramol Y, Pairojkul C, Wu Z, Juasook A, Sudsarn P, Boonjaraspinyo S (2011a) Opisthorchis viverrini infection causes liver and biliary cirrhosis in gerbils. Parasitol Res 109(3):545–551
Wonkchalee O, Boonmars T, Kaewkes S, Chamgramol Y, Aromdee C, Wu Z, Juasook A, Sudsarn P, Boonjaraspinyo S, Pairojkul C (2011b) Comparative studies on animal models for Opisthorchis viverrini infection: host interaction through susceptibility and pathology. Parasitol Res Sep 1. [Epub ahead of print].
Acknowledgements
This work was supported by the Thailand research fund through RMU5480002, Khon Kaen University (KKU55) and the Royal Golden Jubilee-Ph.D. program (Grant No. PHD/0280/2552) to Miss. Orasa Wonkchalee and Associate Professor Thidarut Boonmars. We thank the Department of Parasitology, Liver Fluke and Cholangiocarcinoma Research Center, the Animal Experimental Unit, Faculty of Medicine, Khon Kaen University for their support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wonkchalee, O., Boonmars, T., Aromdee, C. et al. Anti-inflammatory, antioxidant and hepatoprotective effects of Thunbergia laurifolia Linn. on experimental opisthorchiasis. Parasitol Res 111, 353–359 (2012). https://doi.org/10.1007/s00436-012-2846-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00436-012-2846-5