Abstract
Purpose
Pancreatic cancer is a lethal form of cancer that can be triggered by prolonged or acute inflammation of the pancreas. Inflammation have been shown to be regulated by a group of key protein molecules known as the inflammasomes. The NLRP3 inflammasome is the most studied inflammasome and have been strongly implicated to regulate cancer cell proliferation. Therefore, this study aimed to examine the regulation of NLRP3 inflammasome under LPS-induced inflammation and its role in modulating cell proliferation in a panel of pancreatic cancer cells.
Methods
The effects of LPS-induced NLRP3 activation in the presence or absence of MCC950, NLRP3-specific inhibitor, was tested on a panel of three pancreatic cancer cell lines (SW1990, PANC1 and Panc10.05). Western blotting, cell viability kits and ELISA kits were used to examine the effects of LPS-induced NLRP3 activation and inhibition by MCC950 on NLRP3 expression, cell viability, caspase-1 activity and cytokine IL-1β, respectively.
Results
LPS-induced inflammation in the presence of ATP activates NLRP3 that subsequently increases pancreatic cancer cell proliferation by increasing caspase-1 activity leading to overall production of IL-1β. The inhibition of the NLRP3 inflammasome activation via the specific NLRP3 antagonist MCC950 was able to reduce the cell viability of pancreatic cancer cells. However, the efficacy of MCC950 varies between cell types which is most probably due to the difference in ASC expressions which have a different role in inflammasome activation.
Conclusion
There is a dynamic interaction between inflammasome that regulates inflammasome-mediated inflammation in pancreatic adenocarcinoma cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inflammation has long been identified as a potential risk factor for the development of cancer. Chronic inflammation caused by prolonged exposure to chemicals causes tissue stress and subsequently tissue damage. This accumulation of damage and stress leads to the onset of cancer (Ahn et al. 2018). Moreover, following the transformation of a cell to malignant state, inflammatory mediators further support tumour growth by providing signalling molecules to the tumour environment. The tumour cells itself also promote inflammation to maintain the inflammatory microenvironment (Chauhan and Trivedi 2020). A study on inflammatory bowel disease (IBD) and its association to the onset of colon cancer as well as a study showing high correlations of gastric ulcers and its relationship to gastric cancer (Ernst and Gold 2000; Marusawa and Jenkins 2014) further indicate that inflammation is related to cancer formation. However, although a strong relationship has been documented between the onset of cancer and chronic inflammation, the mechanisms underlying this relationship are still unclear.
Pancreatic cancer is fatal due to poor prognosis (Sanabria Mateos and Conlon 2016; Greer and Whitcomb 2009; Farrow and Evers 2002). Several studies have shown that cytokines (i.e. interleukins, interferons and tumour necrosis factors) measured in serum, plasma, tissue and cell culture supernatant were correlated with cancer risk, stage and prognosis (Singh et al. 2019; Lippitz and Harris 2016). Recently, studies have also demonstrated the association of pancreatitis to the onset of pancreatic cancer (McKay et al. 2008; Whitcomb 2004). The pathogenesis of pancreatitis involves damage of the acinar cells, which then sets the acinar cells on a destructive path starting with the release of a wide range of inflammatory mediators. These mediators then recruit neutrophils, monocytes, lymphocytes and macrophages to the pancreas which causes the production of more inflammatory cytokines to be released by the recruiting cells. This inadvertently causes a ‘cytokine storm’ and subsequent amplification of pancreatic injury and cellular malfunction. This pathway is believed to be the link between inflammation, pancreatitis and the onset of pancreatic cancer (Gukovsky et al. 2013). However, due to the lack of specificity and short half-life of these inflammatory mediators (i.e. cytokines and interleukins), their routine use as cancer biomarkers were limited (Chauhan and Trivedi 2020).
The inflammasomes are characterised as intracellular multiprotein complexes and have been shown to play a key role in controlling the inflammatory response of tissues and cells. A wide range of stimuli could trigger the activation of these inflammasomes, for example, microbes, environmental factors and in some cases endogenous molecules (Martinon et al. 2009). The NOD-like receptor family pyrin domain-containing 3 (NLRP3) inflammasome is one of the most extensive studied inflammasomes (McKay et al. 2008). It is shown to interact with pro-caspase-1 along with the apoptosis-associated speck-like protein (ASC) which function as the adaptor molecule to activate the NLRP3 inflammasome (Mariathasan and Monack 2007). Once activated, the NLRP3 inflammasome catalyses the proteolytic process of modifying pro-caspase-1 into caspase-1, which is the active form. This then triggers downstream cleavage of pro-interleukin (IL)-1β and pro-IL-18 into their active forms of IL-1β and IL-18 (Huang et al. 2017). These interleukins have been extensively shown to play crucial roles in driving inflammation. Furthermore, recent evidences have demonstrated that chronic overexpression of NLRP3 inflammasome is linked to the increase in activity of colon cancer, lung cancer and even in skin cancer cell models (Ernst and Gold 2000; Marusawa and Jenkins 2014; Huang et al. 2017; Zaalberg et al. 2019; Demb et al. 2018). It was found that the NLRP3 inflammasome is highly expressed in colon cancer cells and, importantly, knockdown of NLRP3 reverses the mesenchymal characteristics of these cells and reduces their invasion and migration capabilities (Wang et al. 2016). Another study on liver cancer revealed that the NLRP3 inflammasome was severely downregulated in liver cancer cells (Wei et al. , 2013). Subsequently, introduction of treatment (oestrogen) that upregulated NLRP3 expression reduces tumour progression and malignancy (Wei et al. 2015). These studies suggested that the regulation of NLRP3 is ostensibly linked to the onset of tumourigenesis. However, the regulation of NLRP3 in inflammation-induced pancreatic cancer cells remains unknown.
Therefore, this study aims to (i) determine the effect of lipopolysaccharide (LPS)-induced NLRP3 inflammasome activation on pancreatic cancer cell proliferation in the presence or absence of an NLRP3-specific inhibitor (MCC950) and (ii) to examine the expression levels of NLRP3 inflammasome and its associated proteins, such as the apoptosis-associated speck-like protein containing a carboxy-terminal CARD (ASC), caspase-1 and IL-1β in a panel of human pancreatic cancer cell lines upon LPS-induced inflammation in the presence or absence of MCC950. MCC950’s high specificity to NLRP3 is due to the fact that this molecule binds to the TP1 region of the NACHT domain of NLRP3, which is responsible for the hydrolysis of ATP (Tapia-Abellán et al. 2019; Vande Walle et al. 2019). Once bound to NLRP3, the MCC950 molecule prevents ATP hydrolysis needed for the NLRP3 to assume its active shape, thus preventing ASC recruitment and oligomerization (Tapia-Abellán et al. 2019; Vande Walle et al. 2019). Hence, in this study, MCC950 was used to specifically inhibit NLRP3 activation in order to examine the effect of LPS-induced NLRP3 inflammasome activation in a panel of pancreatic cancer cells.
Results
Cell viability of pancreatic cancer cells under LPS and/or ATP stimulation in the presence or absence of MCC950 inhibition
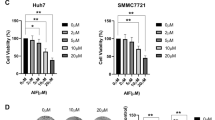
As shown in Fig. 1, different pancreatic cancer (PC) cells Panc10.05, SW1990 and PANC1 responded differently to the stimulation by LPS and/or ATP, in the presence or absence of the specific NLRP3 inhibitor, MCC950. LPS treatment did not induce significant cell viability difference in SW1900, Panc10.05 and PANC1 cells, compared to untreated cells. The addition of ATP with or without LPS significantly (p < 0.05) increases the viability of these PC cells. In the presence of MCC950, there was also no significant change in cell viability when treated with LPS in all three PC cells when compared to the control (MCC950 alone). However, in the presence of MCC950, in cells treated with LPS and/or ATP, there was a significant decrease (p < 0.05) in cell viability relative to that without MCC950. The reduction in percent cell viability for both Panc10.05 and PANC1 cells were more than that observed for SW1990 cells. In SW1900 cells, upon the addition of MCC950, the reduction in percent cell viability was higher compared to that of the control (MCC950 alone), while in Panc10.05 and PANC1 cell lines, the percent cell viability is significantly reduced (p < 0.05; lesser than the control without MCC950) in the presence of LPS or ATP.
The viability of a panel of three pancreatic cancer cells, Panc10.05, SW1990 and PANC1, was examined using CellTiter-Glo® luminescent cell viability assay kit. The cells were stimulated using 1 µg/mL of LPS (24 h), primed with 5 µM of ATP (4 h) or/and inhibited with 10 µM MCC950 (24 h). Data shown are representative of three independent experiments and presented as mean ± SEM. Means with the same letter are not significantly different from each other (p > 0.05).
Expression of ASC and NLRP3 in pancreatic cancer cells under LPS and/or ATP stimulation in the presence or absence of MCC950 inhibition
As shown in Fig. 2a, ASC was found in the SW1990 cell line but not in PANC1 and Panc10.05 PC cell lines. LPS stimulation does not affect the expression of ASC in SW1990 PC cells. In Fig. 2b, the expression of NLRP3 in all three PC cell lines shows an increase in NLRP3 protein expression when subjected to LPS and/or ATP stimulation (p < 0.05). However, upon the addition of MCC950, the NLRP3 protein expressions reduced relative to the groups without exposure to MCC950.
Three PC cell lines (SW1990, PANC1, and Panc10.05) in the presence or absence of LPS stimulation were incubated for 24 h. Western blotting was then performed using the cell lysate to analyse the ASC protein expression levels. β-actin expression serves as the control.
Three PC cell lines, Panc10.05, SW1990 and PANC1, were stimulated using 1 µg/mL of LPS (24 h), primed with 5 µM of ATP (4 h) or/and inhibited with 10 µM MCC950 (24 h). Western blotting was then performed using the cell lysate to analyse the NLRP3 protein expression levels. Densitometric analysis of Western blots was performed using Image Lab 4.0 software. The expression levels were normalised to β-actin (endogenous control) levels. Data shown are representative of three independent experiments and presented as mean ± SEM. Means with the same letter are not significantly different from each other (p > 0.05).
Gene expressions of various inflammasomes including NLRP3 data obtained from the gene expression omnibus (GEO) database for pancreatic cancer versus normal tissue
According to the gene expression omnibus (GEO) public datasets, the mRNA levels of NLRP1, NLRP3, NLRP6 and NLRP12 were significantly lower in pancreatic ductal adenocarcinoma compared to normal tissue samples (p < 0.01), while NLRC4 and AIM2 were higher.
Analysis of the gene expressions of various inflammasomes, including NLRP3 inflammasome, obtained from the GEO database for pancreatic cancer versus normal tissue was generated using unpaired, non-parametric, Mann–Whitney test.
Expression of caspase-1 activation and IL-1β secretion in pancreatic cancer cells under LPS/ATP stimulation in the presence or absence of MCC950 inhibition
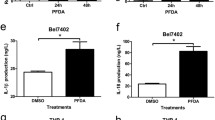
LPS and/or ATP stimulated the activation of caspase-1 and IL-1β secretion (p < 0.05; Fig. 3) in all three pancreatic cancer cells: (i) Panc10.05, (ii) SW1990 and (iii) PANC1. When NLRP3-specific inhibitor, MCC 950, was added, the levels of caspase-1 and IL-1β secretion upon LPS and/or ATP stimulation gets increased in Panc10.05 and PANC1 (p < 0.05) but the level was close to the control (non-stimulated and without MCC950) in SW1990 (Figs. 3).
Three PC cell lines, Panc10.05, SW1990 and PANC1, were stimulated using 1 µg/mL of LPS (24 h), primed with 5 µM of ATP (4 h) or/and inhibited with 10 µM MCC950 (24 h). The caspase-1 expression level in cell lysate was determined using caspase-1 colorimetric assay. Data shown are representative of three independent experiments and presented as mean ± SEM. Means with the same letter are not significantly different from each other (p > 0.05).
Three PC cell lines, Panc10.05, SW1990 and PANC1, were stimulated using 1 µg/mL of LPS (24 h), primed with 5 µM of ATP (4 h) or/and inhibited with 10 µM MCC950 (24 h). The IL-1β levels in the cell supernatant was determined using enzyme-linked immunosorbent assay. Data shown are representative of three independent experiments and presented as mean ± SEM. Means with the same letter are not significantly different from each other (p > 0.05).
Discussion
Pancreatic cancer, like many other forms of cancer, have been shown to have a strong link with inflammation, whereby the prolonged onset of inflammation can trigger either cell death or proliferation in different types of cancer (Kantono and Guo 2017; Kolb et al. 2014; Xue et al. 2019; Moossavi et al. 2018). Recent studies have further shown that inflammasomes are responsible for mediating the complex biological mechanisms of inflammation especially within cancer cells (Kantono and Guo 2017; Kolb et al. 2014; Xue et al. 2019). However, there are few studies that clearly outline the precise roles of inflammasomes in pancreatic cancer.
In this study, all three PC cell lines (SW1990, PANC1 and Panc10.05) show a significant (p < 0.05) increase in cell viability under LPS and ATP stimulated inflammation (Fig. 1). In the presence of the NLRP3 antagonist MCC950, SW1990 shows a significant decrease (p < 0.05) in cell viability relative to its counterpart (treatment groups without MCC950) (Fig. 1). On the other hand, although the other two PC cell lines, PANC1 and Panc10.05, also exhibit a significant decrease in cell viability relative to its counterparts without MCC950, the decrease in cell viability with or without LPS and/or ATP stimulation was lower than control (treatment groups without MCC950). The observation in the PC cells’ viability clearly demonstrated that LPS and ATP were able to induce cell proliferation, while the specific inhibition of NLRP3 by MCC950 inhibited PC cells’ proliferation regardless of LPS and/or ATP stimulation. The differences observed for the cell viability of the three different PC cells could be due to the types of PC cancer cells whereby SW1990 cells are metastatic cancer cells, while PANC1 and PANC10.05 cells are primary adenocarcinoma cells (Cui et al. 2012; Kong et al. 2020). These metastatic and primary adenocarcinoma cells could have different response to LPS- and/or ATP-induced stimulation and MCC950 inhibition.
In addition to different cell types, the differences in proliferation of SW1990 cells in comparison to both PANC1 and Panc10.05 could be due to the expression of the ASC protein since it is found that ASC is only expressed in SW1990 cells (Fig. 2a). The ASC adaptor molecule is essential for the proper function of NLRP3 whereby NLRP3 recruits ASC which in turn recruits caspase-1 molecules. However, in the activation of inflammasome, transcriptional modulation of ASC is not required (Sutterwala et al. 2014). A study has shown that ASC expressions were different in seven different PC cell lines (PK-1, KP-4, PK-8, PK-9, PK-59, Miapaka and KLM-1) (Ohtsuka et al. 2008). The ASC protein expression was absent in KP-4 and Miapaka, whereas in this study, ASC was absent in Panc10.05 and PANC1 cells. In the presence of ASC, cancer cell proliferation, migration and even invasion capabilities can either be promoted or inhibited depending on various factors, such as type of cancer associated with its microenvironment (Protti and Monte 2020). In human melanoma cells, the presence of ASC in primary melanoma cells decreases cancer tumourigenesis and cell viability. However, the opposite is true in metastatic human melanoma cells (Coll et al. 2015; Broz et al. 2010). These observations were in accordance to these findings as the SW1990 cell line is metastatic pancreatic ductal cancer cells, while PANC1 and Panc10.05 are primary pancreatic epithelial cancer cells. Thus, the effects of ASC on cell proliferation were observed only in metastatic PC cells (SW1990).
The trend of NLRP3 expressions upon LPS and/or ATP stimulation in the presence or absence of MCC950 inhibition was very similar across the three PC cell lines. Upon LPS and or ATP stimulation, the expression of NLRP3 increases significantly (p < 0.05). Conversely, upon the addition of MCC950, there was a significant reduction (p < 0.05) in the expression of NLRP3 (Fig. 2b). These observations are in accordance to the activating mechanism of NLRP3, whereby PAMPs, such as LPS, stimulate TLR signalling which primes the intracellular transcription of NLRP3, following which a second factor, such as ATP (from either endogenous or artificial sources), activates the NLRP3 inflammasome (Swanson et al. 2019; Yang et al. 2019; Kelley et al. 2019). MCC950, which functioned as a selective inhibitor to NLRP3, prevented NLRP3 from activating or sustaining its activated state, although it does not directly interfere with NLRP3 priming (Tapia-Abellán et al. 2019; Vande Walle et al. 2019; Wu et al. 2019; Coll et al. 2019). However, a research showed that MCC950 could indirectly affect the priming step of NLRP3 through interaction and subsequent repression of the NF-κB/p65 molecule (Ismael et al. 2018). Since NF-κB/p65 is a crucial intermediary signal upstream of NLRP3 inflammasome transcription, repression of NF-κB/p65 would influence NLRP3 expression level (Ismael et al. 2018). This could explain the significant decrease (p < 0.05) in NLRP3 protein expression observed in all three PC cell lines (Fig. 2b). Interestingly, based on the GEO public datasets, the mRNA levels of NLRC4 and AIM2 inflammasomes, which do not required ASC for activation, were higher in pancreatic ductal adenocarcinoma compared to normal tissue samples, while the other inflammasomes have a significantly lower mRNA expression (Fig. 2c). This further suggests that ASC did in fact play an important role in pancreatic ductal adenocarcinoma.
In addition, the regulation of NLRP3 expression could also affect the cell viability of PC cells. In this study, it was observed that inhibition of NLRP3 expression (Fig. 2b) had a lower percentage in cell viability as shown in Fig. 1. This finding is consistent with a study by Daley et al. (2017), which demonstrated that pharmacological inhibition of NLRP3 attenuates PC cell proliferation and even triggers reprogramming of the innate and adaptive immunity within the tumour microenvironment (Daley et al. 2017). Furthermore, knocking down the NLRP3 affects PC cell growth and development (Hu et al. 2018). In this study, NLRP3 activation were indirectly shown to promote proliferation of PC cells. However, a previous study noted that NLRP3 activation promotes normal colorectal cancer tumour growth but suppresses metastatic colon cancer cells that have migrated to the liver (He et al. 2018). This contrasting effect on cell proliferation highlights a context-dependent duality in the roles of NLRP3 in cancers.
As expected, LPS and/or ATP stimulation increases the production and secretion of both caspase-1 and IL-1β. However, upon the addition of the NLRP3 inhibitor MCC950, caspase-1 and IL-1β expression levels in SW1990 cells dropped to almost the control level (non-stimulated PC cells without MCC950), whereas the expression levels of caspase-1 and IL-1β in both Panc10.05 and PANC1 do not differ significantly from the other treatment groups without MCC950 (Fig. 3). Although the NLRP3 expression level decreases in all three PC cells upon the addition of MCC950 (Fig. 2b), it does not translate in a decrease in caspase-1 and IL-1β in Panc10.05 and PANC1 cells (Fig. 3). These findings correspond to the differences in the expression of ASC protein, whereby only SW1990 cells with ASC proteins shown a significant decrease in expression of caspase-1 and IL-1β (p < 0.05). As for Panc10.05 and PANC1, the increase in productions of caspase-1 and IL-1β could be due to the activation of other inflammasome that does not require ASC to form inflammasome complexes like NLRC4. The NLRC4 inflammasomes uses its oligomerised CARD to nucleate caspase-1 filaments and cause caspase-1 to be activated, thus eliminating the requirement of ASC (Fusco and Duncan 2018). The activated caspase-1 subsequently activates IL-1β (Fusco and Duncan 2018). Furthermore, a recent study had demonstrated that NLRP3 is able to interact with NLRC4, which also can be activated through LPS and ATP stimulation (Qu et al. 2016). A study by Coll et al. (2015) also showed that NLRC4-stimulated IL-1β secretion was not inhibited by MCC950. As such, NLRC4 could initiate ASC-independent caspase-1 activation in Panc10.05 and PANC1 cells, leading to an increase in cell pyroptosis and subsequent decrease in cell viability as shown in Fig. 1. The putative interaction between NLRP3 with other inflammasomes, however, requires further examination. A better understanding of the dynamic in inflammasome signalling would help in identifying more effective biomarkers and the potential targets for better drug development for pancreatic cancer.
Methods
Cell culture
A panel of pancreatic cancer cells (PANC1, Panc10.05 and SW1990) were obtained from American type culture collection (ATCC, USA). PANC1 cells were cultured in Dulbecco’s modified Eagle’s medium (DMEM) with additional sodium pyruvate (DMEM; Gibco, USA), while Panc10.05 and SW1990 cells were cultured in Roswell Park Memorial Institute Medium (RPMI; Gibco, USA). Both media were supplemented with 10% heat-inactivated foetal bovine serum (FBS; ATCC, USA) and 1% penicillin–streptomycin (Lonza, USA). All cells were cultured at 37 °C in a humidified cell incubator under 95%/5% (v/v) mixture of air and carbon dioxide.
Preparation of lipopolysaccharide (LPS), adenosine triphosphate (ATP) and NLRP3-specific inhibitors (MCC950)
Lipopolysaccharide (LPS; Escherichia coli serotype 0111:B4; Sigma, USA) and adenosine triphosphate (ATP; Sigma, USA) were dissolved with sterile filtered phosphate-buffered saline (PBS) and diluted to working concentrations of 10 μg/mL and 50 μM with the appropriate serum-free media to give a final effective concentration of 1 μg/mL and 5 μM, respectively. MCC950 (Sigma, USA) was dissolved in dimethyl sulfoxide (DMSO; Calbiochem, USA) followed by further dilution with sterile filtered PBS and diluted to working concentrations of 100 μM with the appropriate serum-free media to give a final effective concentration of 10 μM (Coll et al. 2015; Xu et al. 2015; Marijon et al. 2013).
Treatment
Throughout this study, the treatment regimens were conducted in eight groups: (1) control (cells exposed to only serum-free media); (2) LPS (cell exposed to 1 μg/mL LPS); (3) ATP (cells exposed to 5 μM ATP); (4) LPS + ATP (cells exposed to 1 μg/mL LPS and 5 μM ATP); (5) MCC950 (cells exposed to 10 μM MCC950); (6) MCC950 + LPS (cells exposed to 10 μM MCC950 and 1 μg/mL LPS); (7) MCC950 + ATP (cells exposed to 10 μM MCC950 and 5 μM ATP) and (8) MCC950 + LPS + ATP (cells exposed to 10 μM MCC950, 1 μg/mL LPS and 10 μM MCC950). Cells were treated with LPS (24 h), ATP (4 h) and/or MCC950 (24 h).
Cell viability assay
Cell viability of PANC1, Panc10.05 and SW1990 cells were measured using a CellTiter-Glo® luminescent cell viability assay kit (Promega, USA). The panel of pancreatic cancer cells (PANC1, Panc10.05 and SW1990 cells) were seeded at a density of 8000 cells per well in white opaque 96-well plates and incubated overnight at 37 °C in a CO2 incubator. The serum-free media, MT cell viability substrate and NanoLuc® enzyme (components of the assay kit) were pre-warmed to 37 °C in water bath before a 2 × concentration of the enzyme–substrate mixture was prepared and pipetted in the samples, mixing with the treatments to give a final 1 × concentration. The cells were then exposed to the respective treatments in serum-free media and the luminescence signal was measured with SpectraMAX M3 microplate reader at 24 h. The assay was performed with eight replicates per sample.
Western blot analysis
PANC1, Panc10.05 and SW1990 cells were lysed using extraction buffer, and protein concentration was determined using the Bradford assay. Samples with an equal amount of protein were separated on 10% sodium dodecyl sulfate polyacrylamide gels and transferred onto a polyvinylidene difluoride membrane. Transferred membranes were blocked with Blocking One (Nacalai Tesque, Kyoto, Japan) for 1 h and incubated overnight at 4 °C with specific primary antibodies: rabbit monoclonal anti-NLRP3 (1:1000; Cat. #15101S) and rabbit monoclonal anti-ASC (1:1000; Cat. #67824S) from Cell Signaling Technology in 1:1000 ratio. Individual membranes were then incubated with a horseradish peroxidase-conjugated secondary antibody anti-rabbit IgG (Cat. #7074P2; Cell Signaling Technology) in 1:2000 ratio dilution for 1 h at room temperature. The blots were developed using Chemi-Lumi One Super enhanced chemiluminescence reagent (Nacalai Tesque, Kyoto, Japan). Blot visualisation and densitometric analyses were performed using Bio-Rad Image Lab 6.0.1 software. All Western blots were performed in triplicate. Beta-actin was used as a loading control.
Caspase-1 colorimetric assay
The activity of caspase-1 was assayed with Caspase-1 colorimetric assay kit (Calbiochem; Merck Milipore, Germany) according to the manufacturer’s instruction. In brief, 50 µL of cell lysate (200 µg protein) were was incubated for 2 h at 37 °C with 50 µL of reaction buffer containing 10 mM dithiothreitol (DTT) and 5 µL of 200 µM YVAD-p-nitroanilide (pNA) substrate. The absorbance was determined at 400 nm using a microplate reader (Tecan, Switzerland).
Enzyme-linked immunosorbent assay (ELISA)
The levels of IL-1β in the supernatants of PANC1, Panc10.05 and SW1990 cells were determined using IL-1β-ELISA kit (Cat. #336111; Qiagen, Germany) according to the manufacturer’s instructions. Data are expressed as percentages of the mean value from the concurrently assayed controls.
Gene omnibus analysis
The mRNA gene expressions of various inflammasomes in pancreatic cancer and normal tissue were obtained from the gene expression database (GEO). The differences in mRNA gene expressions between pancreatic cancer and normal tissue were analysed using unpaired, non-parametric, Mann–Whitney test with values expressed as mean ± the standard error of the mean (SEM).
Statistical analysis
All statistical analyses were performed using the GraphPad prism software version 7. Data were analysed using one-way analysis of variance (ANOVA), followed by Tukey’s post hoc test. The differences were considered statistically significant when p < 0.05. Data are presented as mean ± standard error of mean (SEM).
References
Ahn KS, Hwang JY, Han H-S, Kim ST, Hwang I, Chun Y-O (2018) The impact of acute inflammation on progression and metastasis in pancreatic cancer animal model. Surg Oncol 27:61–69
Broz P, von Moltke J, Jones JW, Vance RE, Monack DM (2010) Differential requirement for caspase-1 autoproteolysis in pathogen-induced cell death and cytokine processing. Cell Host Microbe 8:471–483
Chauhan R, Trivedi V (2020) Inflammatory markers in cancer: potential resources. Front Biosci Sch 12:1–24
Coll RC, Robertson AAB, Chae JJ, Higgins SC, Muñoz-Planillo R, Inserra MC, Vetter I, Dungan LS, Monks BG, Stutz A et al (2015) A small-molecule inhibitor of the NLRP3 inflammasome for the treatment of inflammatory diseases. Nat Med 21:248
Coll RC, Hill JR, Day CJ, Zamoshnikova A, Boucher D, Massey NL, Chitty JL, Fraser JA, Jennings MP, Robertson AAB et al (2019) MCC950 directly targets the NLRP3 ATP-hydrolysis motif for inflammasome inhibition. Nat Chem Biol 15:556–559
Cui Y, Brosnan JA, Blackford AL, Sur S, Hruban RH, Kinzler KW, Vogelstein B, Maitra A, Diaz LA, Iacobuzio-Donahue CA et al (2012) Genetically defined subsets of human pancreatic cancer show unique in vitro chemosensitivity. Clin Cancer Res 18:6519–6530
Daley D, Mani VR, Mohan N, Akkad N, Pandian GSDB, Savadkar S, Lee KB, Torres-Hernandez A, Aykut B, Diskin B et al (2017) NLRP3 signaling drives macrophage-induced adaptive immune suppression in pancreatic carcinoma. J Exp Med 214:1711–1724
Demb J, Wei EK, Izano M, Kritchevsky S, Swede H, Newman AB, Shlipak M, Akinyemiju T, Gregorich S, Braithwaite D (2018) Chronic inflammation and risk of lung cancer in older adults in the health, aging and body composition cohort study. J Geriatr Oncol 10:265–271
Ernst PB, Gold BD (2000) The disease spectrum of Helicobacter Pylori: the immunopathogenesis of gastroduodenal ulcer and gastric cancer. Annu Rev Microbiol 54:615–640
Farrow B, Evers BM (2002) Inflammation and the development of pancreatic cancer. Surg Oncol 10:153–169
Fusco WG, Duncan JA (2018) Novel aspects of the assembly and activation of inflammasomes with focus on the NLRC4 inflammasome. Int Immunol 30:183–193
Greer JB, Whitcomb DC (2009) Inflammation and pancreatic cancer: an evidence-based review. Curr Opin Pharmacol 9:411–418
Gukovsky I, Li N, Todoric J, Gukovskaya A, Karin M (2013) Inflammation, autophagy, and obesity: common features in the pathogenesis of pancreatitis and pancreatic cancer. Gastroenterology 144(1199–1209):e4
He Q, Fu Y, Tian D, Yan W (2018) The contrasting roles of inflammasomes in cancer. Am J Cancer Res 8:566–583
Hu H, Wang Y, Ding X, He Y, Lu Z, Wu P, Tian L, Yuan H, Liu D, Shi G et al (2018) Long non-coding RNA XLOC_000647 suppresses progression of pancreatic cancer and decreases epithelial-mesenchymal transition-induced cell invasion by down-regulating NLRP3. Mol Cancer 17:18
Huang C-F, Chen L, Li Y-C, Wu L, Yu G-T, Zhang W-F, Sun Z-J (2017) NLRP3 inflammasome activation promotes inflammation-induced carcinogenesis in head and neck squamous cell carcinoma. J Exp Clin Cancer Res 36:116
Ismael S, Nasoohi S, Ishrat T (2018) MCC950, the selective inhibitor of nucleotide oligomerization domain-like receptor protein-3 inflammasome, protects mice against traumatic brain injury. J Neurotrauma 35:1294–1303
Kantono M, Guo B (2017) Inflammasomes and cancer: the dynamic role of the inflammasome in tumor development. Front Immunol 8:1132
Kelley N, Jeltema D, Duan Y, He Y (2019) The NLRP3 inflammasome: an overview of mechanisms of activation and regulation. Int J Mol Sci 20:3328
Kolb R, Liu G-H, Janowski AM, Sutterwala FS, Zhang W (2014) Inflammasomes in cancer: a double-edged sword. Protein Cell 5:12–20
Kong K, Guo M, Liu Y, Zheng J (2020) Progress in animal models of pancreatic ductal adenocarcinoma. J Cancer 11:1555–1567
Lippitz BE, Harris RA (2016) Cytokine patterns in cancer patients: a review of the correlation between interleukin 6 and prognosis. Oncoimmunology 5:e1093722–e1093722
Liu W, Luo Y, Dunn JH, Norris DA, Dinarello CA, Fujita M (2013) Dual role of apoptosis-associated speck-like protein containing a CARD (ASC) in tumorigenesis of human melanoma. J Invest Dermatol 133:518–527
Mariathasan S, Monack DM (2007) Inflammasome adaptors and sensors: intracellular regulators of infection and inflammation. Nat Rev Immunol 7:31
Marijon E, Le Heuzey J-Y, Connolly S, Yang S, Pogue J, Brueckmann M, Eikelboom J, Themeles E, Ezekowitz M, Wallentin L et al (2013) Causes of death and influencing factors in patients with atrial fibrillation. Circulation 128:2192–2201
Martinon F, Mayor A, Tschopp J (2009) The inflammasomes: guardians of the body. Annu Rev Immunol 27:229–265
Marusawa H, Jenkins BJ (2014) Inflammation and gastrointestinal cancer: an overview. Cancer Lett 345:153–156
McKay CJ, Glen P, McMillan DC (2008) Chronic inflammation and pancreatic cancer. Best Pract Res Clin Gastroenterol 22:65–73
Moossavi M, Parsamanesh N, Bahrami A, Atkin SL, Sahebkar A (2018) Role of the NLRP3 inflammasome in cancer. Mol Cancer 17:158
Ohtsuka T, Mitsuno M, Kitajima Y, Ide T, Lee SW, Miyazaki K (2008) Role of ASC in hypoxia-mediated cell death in pancreatic cancer. Mol Med Rep 1:827–831
Protti MP, De Monte L (2020) Dual role of inflammasome adaptor ASC in cancer. Front Cell Dev Biol 8:40
Qu Y, Misaghi S, Newton K, Maltzman A, Izrael-Tomasevic A, Arnott D, Dixit VM (2016) NLRP3 recruitment by NLRC4 during Salmonella infection. J Exp Med 213:877–885
Sanabria Mateos R, Conlon KC (2016) Pancreatic cancer. Surg 34:282–291
Singh J, Sohal SS, Lim A, Duncan H, Thachil T, De Ieso P (2019) Cytokines expression levels from tissue, plasma or serum as promising clinical biomarkers in adenocarcinoma of the prostate: a systematic review of recent findings. Ann Transl Med 7:245
Sutterwala FS, Haasken S, Cassel SL (2014) Mechanism of NLRP3 inflammasome activation. Ann NY Acad Sci 1319:82–95
Swanson KV, Deng M, Ting JP-Y (2019) The NLRP3 inflammasome: molecular activation and regulation to therapeutics. Nat Rev Immunol 19:477–489
Tapia-Abellán A, Angosto-Bazarra D, Martínez-Banaclocha H, de Torre-Minguela C, Cerón-Carrasco JP, Pérez-Sánchez H, Arostegui JI, Pelegrin P (2019) MCC950 closes the active conformation of NLRP3 to an inactive state. Nat Chem Biol 15:560–564
Vande Walle L, Stowe IB, Šácha P, Lee BL, Demon D, Fossoul A, Van Hauwermeiren F, Saavedra PHV, Šimon P, Šubrt V et al (2019) MCC950/CRID3 potently targets the NACHT domain of wild-type NLRP3 but not disease-associated mutants for inflammasome inhibition. PLOS Biol 17:e3000354
Wang H, Wang Y, Du Q, Lu P, Fan H, Lu J, Hu R (2016) Inflammasome-independent NLRP3 is required for epithelial-mesenchymal transition in colon cancer cells. Exp Cell Res 342:184–192
Wei Q, Mu K, Li T, Zhang Y, Yang Z, Jia X, Zhao W, Huai W, Guo P, Han L (2013) Deregulation of the NLRP3 inflammasome in hepatic parenchymal cells during liver cancer progression. Lab Invest 94:52–62
Wei Q, Guo P, Mu K, Zhang Y, Zhao W, Huai W, Qiu Y, Li T, Ma X, Liu Y et al (2015) Estrogen suppresses hepatocellular carcinoma cells through ERβ-mediated upregulation of the NLRP3 inflammasome. Lab Investig 95:804
Whitcomb DC (2004) Inflammation and cancer V. chronic pancreatitis and pancreatic cancer. Am J Physiol Liver Physiol 287:G315–G319
Wu D, Chen Y, Sun Y, Gao Q, Li H, Yang Z, Wang Y, Jiang X, Yu B (2019) Target of MCC950 in inhibition of NLRP3 inflammasome activation: a literature review. Inflammation 43:17–23
Xu Z-Y, Tang J-N, Xie H-X, Du Y-A, Huang L, Yu P-F, Cheng X-D (2015) 5-Fluorouracil chemotherapy of gastric cancer generates residual cells with properties of cancer stem cells. Int J Biol Sci 11:284–294
Xue Y, Du H-D, Tang D, Zhang D, Zhou J, Zhai C-W, Yuan C-C, Hsueh C-Y, Li S-J, Heng Y et al (2019) Correlation between the NLRP3 inflammasome and the prognosis of patients with LSCC. Front Oncol 9:588
Yang Y, Wang H, Kouadir M, Song H, Shi F (2019) Recent advances in the mechanisms of NLRP3 inflammasome activation and its inhibitors. Cell Death Dis 10:128
Zaalberg A, Moradi Tuchayi S, Ameri AH, Ngo KH, Cunningham TJ, Eliane J-P, Livneh M, Horn TD, Rosman IS, Musiek A et al (2019) Chronic inflammation promotes skin carcinogenesis in cancer-prone discoid lupus Erythematosus. J Invest Dermatol 139:62–70
Acknowledgements
This work was supported by International Medical University [project no.: MMM 1-2019(02)].
Author information
Authors and Affiliations
Contributions
EWLC and CWM are involved in conceptualisation; EWLC is involved in methodology development; ACKY and JKYY are involved in formal analysis; and EWLC, CWM, ACKY and JYKY are involved in writing review and editing. All the authors agreed to the final manuscript.
Corresponding author
Ethics declarations
Conflict of interests
There are no known conflicts of interest associated with this publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yaw, A.C.K., Chan, E.W.L., Yap, J.K.Y. et al. The effects of NLRP3 inflammasome inhibition by MCC950 on LPS-induced pancreatic adenocarcinoma inflammation. J Cancer Res Clin Oncol 146, 2219–2229 (2020). https://doi.org/10.1007/s00432-020-03274-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-020-03274-y