Abstract
Objectives
To evaluate the prognostic significance of the Choi criteria for assessing the responses of a renal mass and inferior vena cava (IVC) tumor thrombus in patients with renal cell carcinoma (RCC) receiving targeted therapy.
Materials and methods
We reviewed the medical records of 22 patients diagnosed with RCC and IVC thrombus between 2005 and 2012. The efficacy of targeted therapy in renal mass and IVC tumor thrombus was evaluated using response evaluation criteria in solid tumors (RECIST) and Choi criteria, respectively. Overall survival was estimated, and the prognostic significance of each variable was estimated using Cox proportional-hazards regression modeling.
Results
There were no significant differences in overall survival between patients with partial response (PR) and nonresponse according to RECIST criteria (19.3 vs 43 months; p = 0.212) or Choi criteria (9.0 vs 23.3 months; p = 0.109) in primary tumor. Regarding the response of IVC tumor thrombi, according to Choi criteria, nine patients (40.9 %) demonstrated PR and longer survival than patients with stable disease (7.2 vs 23.3 months; p = 0.014). In multivariable analysis, response to IVC thrombus according to Choi criteria was the only significant predictive factor. Patients with IVC thrombus who demonstrate the PR according to Choi criteria were at 0.35-fold greater overall risk of death compared with patients who did not demonstrate this response (p = 0.043).
Conclusions
A response according to Choi criteria in IVC tumor thrombus was an independent prognostic predictor in patients with RCC and IVC thrombus who receive targeted therapy.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Despite advancements in the imaging and detection of renal cell carcinoma (RCC) following stage migration (Pantuck et al. 2001), approximately 10 % of patients develop a tumor thrombus in the inferior vena cava IVC, Pouliot et al. (2010). Up to 60 % of these patients also develop concurrent subclinical metastases (Klatte et al. 2007). The clinical prognosis of patients with RCC and IVC thrombus has traditionally been poor (median 1–2-year survival rate = 10–20 %) due to the lack of effective chemotherapy agents and the limited usefulness of radiation therapy (Motzer et al. 1999; Reese et al. 2013). Currently, surgery is the only potential cure. However, the resection of RCC and IVC thrombus is technically demanding and historically associated with high rates of perioperative morbidity and mortality (Martinez-Salamanca et al. 2011; Zastrow et al. 2011). The emergence of new therapies that target the angiogenesis pathway has improved the clinical prognosis of patients with advanced RCC. Targeted therapy can now be integrated with surgery, thereby optimizing clinical outcomes in patients with advanced RCC (Motzer 2011). However, review of a large series of patients treated with targeted therapy with in situ RCC tumor thrombi revealed minimal clinical effect on the tumor thrombus level (Cost et al. 2011).
On the other hand, clinically meaningful responses may be underestimated by only assessing changes in tumor size, as targeted therapies can result in tumor necrosis without a marked decrease in size (Flaherty 2007; van der Veldt et al. 2008). Treatment-induced necrosis is not included in the response evaluation criteria in solid tumors (RECIST) and may mimic progressive disease (PD). Choi et al. developed new response criteria for evaluating imatinib treatment in patients with gastrointestinal stromal cell tumor. These criteria include changes in tumor attenuation on computed tomography (CT), which reflects tumor density (Choi et al. 2007). Several studies indicate that sunitinib can induce necrosis in metastatic RCC. During sunitinib treatment, responsive RCC lesions demonstrate a dramatic decrease in attenuation but little change in size (Baccala et al. 2007; van der Veldt et al. 2008). van der Veldt et al. (2010) reported that the Choi criteria could be used to define early metastatic RCC patients who could benefit from sunitinib. Choi criteria in metastatic RCC and lesions have also been explored (Hittinger et al. 2012; van der Veldt et al. 2010), demonstrating that the impact on IVC tumor thrombus is minimal. Therefore, here we evaluate the prognostic significance of the Choi criteria for assessing the responses of renal mass and IVC tumor thrombus in patients with RCC who received targeted therapy.
Materials and methods
We reviewed the medical records of all patients who presented at the Department of Urology or Oncology of the Asan Medical Center (Seoul, Korea) for evaluation or treatment of RCC and IVC thrombus between April 2005 and December 2012. The study was performed with the approval and oversight of the institutional review board, which waived the requirement for informed consent because of its retrospective design.
Patients
During the study period, 76 patients presented with RCC and IVC thrombus. Of these, 54 patients were excluded because of surgical resection of thrombi. Only 22 patients who received only targeted therapy were included. These 22 patients received biopsy confirmation of RCC histology before the initiation of targeted therapy. The medical records of these 22 patients were reviewed, and information on potential prognostic factors was obtained including age, sex, targeted agent, presentation (Patard et al. 2004), time from diagnosis to treatment, histology, Fuhrman grade (Fuhrman et al. 1982), regional lymph node involvement, metastasis, and number of risk factors according to the criteria proposed by the Memorial Sloan-Kettering Cancer Center (Motzer et al. 2002).
Treatment and evaluation
Staging workup at the time of diagnosis included chest X-ray, abdominopelvic CT, and a bone scan. Selected patients also underwent CT scans of the chest and/or brain. Extent of tumor thrombus was determined using either CT or magnetic resonance imaging (MRI) and graded according to the Nevus classification: level I (tumor thrombus extending ≤2 cm above the ostium of the renal vein into the IVC); level II (thrombus extending ≥2 cm above the ostium of the renal vein and infrahepatic vein); level III (thrombus extending into the intrahepatic portion of the vena cava but below the diaphragm); or level IV thrombus extending into the right atrium, Neves and Zincke (1987).
Patients received oral sunitinib (n = 18) or sorafenib (n = 4) according to standard scheduling: once-daily 50 mg sunitinib for 4 weeks, followed by 2 weeks without treatment, or twice-daily 400 mg sorafenib. Dose reduction was allowed to manage toxicity reduction to 37.5 mg and then once-daily 25 mg sunitinib, or reduction to once-daily 400 mg and then 400 mg sorafenib every other day, Escudier et al. (2007); Motzer et al. (2007).
Objective responses to systemic therapy were assessed by thoroughly reviewing the baseline and follow-up CT images obtained 12 weeks later. Treatment was continued until disease progression, unacceptable toxicity, or death.
Imaging techniques and interpretation
CT was performed using a 16-channel Sensation 16 MDCT scanner (Siemens Medical System, Erlangen, Germany). The scanning parameters for unenhanced scanning included the following: 16-detector array at 24-mm collimation; table speed, 24–36 mm per rotation (48 mm/s); pitch, 1.0–1.5; 5-mm reconstruction interval; 120 kV tube voltage; and 170–250 mA tube current (determined using the automatic dose modulation technique).
The diameter of the primary tumor was measured across the longest cross-sectional dimension on the axial image, and the diameter of the thrombus was measured on the coronal image. The responses of the primary tumors and thrombi were independently evaluated by two readers (T. Kwon and J. K. Kim) according to RECIST 1.1 (Eisenhauer et al. 2009). In the case of interobserver discrepancies, agreement was reached by discussion.
Choi criteria were used to assess the portal venous phase on the contrast-enhanced CT. Axial images of the enhanced lesions (which we assumed included the primary tumor and thrombus) were used to measure the CT number included in the picture-archiving communication system. The CT number was expressed in Hounsfield units (HU). Image J (version 1.38×/Java 1.6.0_02) was downloaded from the National Institutes of Health (http://rsb.info.nih.gov/ij) and used to analyze all images. The region of interest (ROI) that coincided with the outline of the primary tumor and thrombus was drawn, and mean HU value of each ROI was determined by two independent readers T. Kwon and J. K. Kim, Fig. 1. Mean HU values were used in the statistical analysis, and interobserver variability was negligible (Spearman correlation coefficient = 0.978; p < 0.001). The Choi criteria define partial response (PR) as ≥10 % decrease in one-dimensional tumor size or ≥ 15 % decrease in tumor attenuation on CT, whereas PD is defined as ≥10 % increase in size without meeting the PR criteria for change in attenuation (Table 1). Patients were divided into two groups according to the Choi criteria for thrombus: response group (PR according to Choi criteria) and nonresponse group [stable disease (SD) or PD according to Choi criteria].
Decreased attenuation due to targeted therapy. The ROI (yellow solid line) was drawn to coincide with the lesions and HU histogram. a At baseline, primary renal mass attenuation was 159.717 HU. b After 12 weeks of targeted therapy, primary renal mass attenuation was 127.496 HU (–20 %). c At baseline, IVC thrombus attenuation was 135.048 HU. d After 12 weeks of targeted therapy, IVC thrombus attenuation was 112.502 HU (–17 %)
Statistical analysis
The clinicopathological factors were compared between groups using the Pearson’s chi-square test for categorical variables or Student’s t test for continuous variables. Quantitative data are expressed as mean values with standard deviations or median values with ranges. The efficacy of the targeted therapy was evaluated according to RECIST and Choi criteria. Overall survival (OS) was calculated from the time of diagnosis to death from any cause. Survivors were censored at the date of last contact. We used Cox proportional-hazards modeling to estimate the prognostic significance of each variable, including the prognostic factors proposed by the Memorial Sloan-Kettering Cancer Center (Motzer et al. 2002). Significant variables (p < 0.2) according to the univariate analysis were included in the multivariable analysis. Correlations between clinical outcomes and the assessed variables are expressed as hazard ratios (HR) and 95 % CIs. All statistical tests were two sided, and p < 0.05 is considered statistically significant. Data were analyzed using the Statistical Package for Social Science (version 18.0; SPSS Inc., Chicago, IL, USA).
Results
Baseline characteristics
Table 2 shows the clinicopathological characteristics of the patients at diagnosis. There were no significant differences between groups except changes in thrombotic density and survival duration. Patients in the response group demonstrated greater changes in thrombotic density (−25.8 vs −4.2 % in the response and nonresponse groups, respectively; p = 0.001) and longer survival (30.5 vs 13.1 months, respectively; p = 0.018). Overall mean age was 64.2 years (59.9 and 67.2 years, respectively; p = 0.108), overall mean tumor size was 8.9 cm (9.8 and 8.7 cm, respectively; p = 0.238), and overall mean time from diagnosis to treatment was 1.2 months (0.8 and 1.5 months, respectively; p = 0.121).
Efficacy of targeted therapy in terms of response criteria and OS
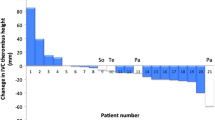
According to the RECIST criteria, only one patient (4.6 %) demonstrated PR, 20 patients (90.8 %) demonstrated SD, and one patient (4.6 %) demonstrated PD in their primary tumors within 12 weeks after the start of therapy. According to the Choi criteria, nine patients (40.9 %) demonstrated PR and 13 patients (59.1 %) demonstrated SD in their primary tumors. There were no significant differences in OS between PR and nonresponsive patients according to RECIST (19.3 vs 43 months, respectively; p = 0.212) or Choi criteria (9.0 vs 23.3 months, respectively; p = 0.109). Regarding response in IVC tumor thrombi, two patients (9.1 %) demonstrated PR according to RECIST but no differences in survival were found (9.1 vs 44.6 months; p = 0.188). According to the Choi criteria, nine patients (40.9 %) demonstrated PR and longer survival than SD patients 7.2 vs 23.3 months, respectively; p = 0.014; Table 3. There was no pulmonary embolism caused by spontaneous migration of tumor thrombus during targeted therapy.
Predictive factors of OS
According to the univariate Cox proportional-hazards model used to predict the probability of overall mortality, Karnofsky performance status and Choi response in thrombi are significant predictors of mortality. According to the multivariable analysis, the Choi response in IVC tumor thrombi is the only significant predictive factor. Patients demonstrating response according to Choi criteria in thrombi were at 0.35-fold greater overall risk of death (95 % CI 0.13–0.96; p = 0.043) compared with nonresponsive patients. RECIST and Choi response in the primary tumor did not predict the probability of overall mortality according to the univariate or multivariate analyses (Table 4).
Discussion
We retrospectively evaluated the prognostic significance of the Choi criteria for assessing renal mass and IVC tumor thrombus in patients who received targeted therapy. Patients who demonstrated response according to Choi criteria in IVC thrombus had longer median survival than nonresponsive patients (23.3 vs 7.2 months, respectively; p = 0.014). Although patients who demonstrated response according to Choi or RECIST criteria in primary mass also demonstrated longer median survival than nonresponsive patients, this finding was not statistically significant.
Although RECIST is the most widely used response evaluation criteria, assessment can evaluate changes in size, which is more suitable for conventional cytotoxic chemotherapy because this mainly induces tumor shrinkage (Eisenhauer et al. 2009). In contrast to cytotoxic chemotherapy, targeted agents [such as tyrosine-kinase inhibitors (TKIs)] are cytostatic drugs that stabilize disease by affecting cancer growth kinetics rather than size (Ratain and Eckhardt 2004). Most especially for RCC, which is often treated using antiangiogenic drugs such as sunitinib or sorafenib, treatment can result in perfusion changes and necrosis (Motzer et al. 2006). Primary lesions are not exclusively affected by perfusion changes (Cowey et al. 2010). Furthermore, primary RCC lesions are often difficult to evaluate because of very large size, irregular shape, internal necrosis, and hemorrhage. Therefore, the simple measurement of length according to RECIST can result in inaccurate or misleading responses. To overcome the limitations of RECIST, several response criteria have been used to evaluate metastatic RCC (Smith et al. 2010a, b; van der Veldt et al. 2010). Those criteria consider not only size but also attenuation, morphology, and/or structure and demonstrate some predictive value for prognosis.
Our results support the data in the literature, namely that targeted therapies demonstrate relatively limited efficacy in terms of tumor shrinkage (Escudier et al. 2007). After 12 weeks of targeted therapy, the mean change in primary tumor size was −1.0 %. RECIST defines SD according to a broad spectrum of tumor lesion sizes: ≥20 % increase in the sum of all lesions (or a new lesion) is required for PD, and ≥30 % decrease in the sum of all lesions is required for PR. The range between these two thresholds is defined as SD. Of 22 patients included in this study, only one patient demonstrated PR according to RECIST criteria in the primary tumor at the first follow-up examination performed 12 weeks after the start of therapy, while the remaining patients were nonresponsive at this time. Although one partial responder demonstrated favorable survival (43 months), the efficacy of the RECIST criteria is limited.
In recent studies, investigators report that metastatic RCC treated with TKIs exhibits decreased attenuation on contrast-enhanced CT (Baccala et al. 2007; Smith et al. 2010a). For example, markedly decreased attenuation with minimal changes in size has been observed on contrast-enhanced CT scans of patients with metastatic RCC following sunitinib therapy. Decreased attenuation is correlated with pathological evidence of necrosis upon resection (Baccala et al. 2007). RECIST does not account for changes in tumor attenuation or therapeutic failure-associated morphological enhancement patterns, which are commonly encountered in TKI-treated metastatic RCC (Therasse et al. 2000). Tumor angiogenesis is also directly associated with contrast-enhanced CT. Therefore, density is a biomarker of interest in patients receiving therapies that require an antiangiogenic profile (Miles 1999).
During targeted therapy, pronounced decreases in attenuation can be observed in responsive RCC lesions, but little change in size is generally noted. According to the Choi criteria, PR was observed 40.9 % of both primary tumors and thrombi. Although median OS in PR patients was consistent, only PR patients with IVC tumor thrombus demonstrated statistically longer OS than SD patients. The CT number is determined by assessing the physical density of the components of each object. A renal mass is composed of a few elements, including intracystic fluid, septa, solid nodules, and calcification. The CT number of a necrotic lesion is only 45 HU (Ayres et al. 2004), but the CT number of septa or nodules containing RCC can be >100 HU, and calcification can be >300 HU (Ayres et al. 2004). The mean HU of a renal mass is influenced by the relative distributions of these elements. Thus, the ambiguous CT number of a primary tumor could be attributed to the treatment response. In contrast, change in thrombotic density is a more accurate reflection of the treatment response because the IVC tumor thrombus itself is considered an RCC lesion.
We also evaluated whether the high rate of PR patients according to the Choi criteria could be used to identify targeted therapies and favorable clinical outcomes. In our limited study sample, the median survival of the PR patients with thrombus according to the Choi criteria demonstrated favorable outcomes. Van der Veldt reported that patients with metastatic RCC who receive sunitinib treatment and demonstrate the Choi criteria also demonstrate significantly better predictive values for progression-free survival and OS than PR patients who are evaluated according to RECIST (van der Veldt et al. 2010). In the future, the determination of prospective correlations between treatment response (according to Choi and RECIST criteria) and progression-free survival and OS in larger patient cohorts will help clarify the role of the Choi criteria for evaluating patients with advanced RCC who are receiving targeted treatment.
This study has several limitations. First, this is a small, retrospective study that contains potential biases. Because of this study’s insufficient power due to its small sample size, validation by a larger prospective cohort is warranted. Second, evaluation of treatment response at the first 12-week follow-up examination was insufficient because the survival period was short. Third, the attenuation of heterogeneous lesions may have been inaccurately assessed, as the mean value was only calculated in one slice in one ROI. Nonetheless, the present study is the first study to analyze the Choi criteria for assessing the response of renal mass and IVC tumor thrombus in patients with RCC receiving targeted therapy.
Conclusions
This study shows that response according to Choi criteria in IVC tumor thrombus is an independent prognostic predictor in RCC patients receiving targeted therapy. A prospective study on a large cohort will help clarify the role of the Choi criteria for assessing patients with advanced RCC who are receiving targeted therapy.
References
Ayres FJ, Zuffo MK, Rangayyan RM, Boag GS, Filho VO, Valente M (2004) Estimation of the tissue composition of the tumour mass in neuroblastoma using segmented CT images. Med Biol Eng Comput 42:366–377
Baccala A Jr, Hedgepeth R, Kaouk J, Magi-Galluzzi C, Gilligan T, Fergany A (2007) Pathological evidence of necrosis in recurrent renal mass following treatment with sunitinib. Int J Urol 14:1095–1097; discussion 1097
Choi H, Charnsangavej C, Faria SC, Macapinlac HA, Burgess MA, Patel SR, Chen LL, Podoloff DA, Benjamin RS (2007) Correlation of computed tomography and positron emission tomography in patients with metastatic gastrointestinal stromal tumor treated at a single institution with imatinib mesylate: proposal of new computed tomography response criteria. J Clin Oncol 25:1753–1759
Cost NG, Delacroix SE Jr, Sleeper JP, Smith PJ, Youssef RF, Chapin BF, Karam JA, Culp S, Abel EJ, Brugarolas J, Raj GV, Sagalowsky AI, Wood CG, Margulis V (2011) The impact of targeted molecular therapies on the level of renal cell carcinoma vena caval tumor thrombus. Eur Urol 59:912–918
Cowey CL, Fielding JR, Rathmell WK (2010) The loss of radiographic enhancement in primary renal cell carcinoma tumors following multitargeted receptor tyrosine kinase therapy is an additional indicator of response. Urology 75:1108–1113
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, Dancey J, Arbuck S, Gwyther S, Mooney M, Rubinstein L, Shankar L, Dodd L, Kaplan R, Lacombe D, Verweij J (2009) New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 45:228–247
Escudier B, Eisen T, Stadler WM, Szczylik C, Oudard S, Siebels M, Negrier S, Chevreau C, Solska E, Desai AA, Rolland F, Demkow T, Hutson TE, Gore M, Freeman S, Schwartz B, Shan M, Simantov R, Bukowski RM (2007) Sorafenib in advanced clear-cell renal-cell carcinoma. N Engl J Med 356:125–134
Flaherty KT (2007) Sorafenib in renal cell carcinoma. Clin Cancer Res 13:747s–752s
Fuhrman SA, Lasky LC, Limas C (1982) Prognostic significance of morphologic parameters in renal cell carcinoma. Am J Surg Pathol 6:655–663
Hittinger M, Staehler M, Schramm N, Ubleis C, Becker C, Reiser M, Berger F (2012) Course of size and density of metastatic renal cell carcinoma lesions in the early follow-up of molecular targeted therapy. Urol Oncol 30:695–703
Klatte T, Pantuck AJ, Riggs SB, Kleid MD, Shuch B, Zomorodian N, Kabbinavar FF, Belldegrun AS (2007) Prognostic factors for renal cell carcinoma with tumor thrombus extension. J Urol 178:1189–1195; discussion 1195
Martinez-Salamanca JI, Huang WC, Millan I, Bertini R, Bianco FJ, Carballido JA, Ciancio G, Hernandez C, Herranz F, Haferkamp A, Hohenfellner M, Hu B, Koppie T, Martinez-Ballesteros C, Montorsi F, Palou J, Pontes JE, Russo P, Terrone C, Villavicencio H, Volpe A, Libertino JA (2011) Prognostic impact of the 2009 UICC/AJCC TNM staging system for renal cell carcinoma with venous extension. Eur Urol 59:120–127
Miles KA (1999) Tumour angiogenesis and its relation to contrast enhancement on computed tomography: a review. Eur J Radiol 30:198–205
Motzer RJ (2011) New perspectives on the treatment of metastatic renal cell carcinoma: an introduction and historical overview. Oncologist 16(Suppl 2):1–3
Motzer RJ, Mazumdar M, Bacik J, Berg W, Amsterdam A, Ferrara J (1999) Survival and prognostic stratification of 670 patients with advanced renal cell carcinoma. J Clin Oncol 17:2530–2540
Motzer RJ, Bacik J, Murphy BA, Russo P, Mazumdar M (2002) Interferon-alfa as a comparative treatment for clinical trials of new therapies against advanced renal cell carcinoma. J Clin Oncol 20:289–296
Motzer RJ, Michaelson MD, Redman BG, Hudes GR, Wilding G, Figlin RA, Ginsberg MS, Kim ST, Baum CM, DePrimo SE, Li JZ, Bello CL, Theuer CP, George DJ, Rini BI (2006) Activity of SU11248, a multitargeted inhibitor of vascular endothelial growth factor receptor and platelet-derived growth factor receptor, in patients with metastatic renal cell carcinoma. J Clin Oncol 24:16–24
Motzer RJ, Hutson TE, Tomczak P, Michaelson MD, Bukowski RM, Rixe O, Oudard S, Negrier S, Szczylik C, Kim ST, Chen I, Bycott PW, Baum CM, Figlin RA (2007) Sunitinib versus interferon alfa in metastatic renal-cell carcinoma. N Engl J Med 356:115–124
Neves RJ, Zincke H (1987) Surgical treatment of renal cancer with vena cava extension. Br J Urol 59:390–395
Pantuck AJ, Zisman A, Belldegrun AS (2001) The changing natural history of renal cell carcinoma. J Urol 166:1611–1623
Patard JJ, Leray E, Cindolo L, Ficarra V, Rodriguez A, De La Taille A, Tostain J, Artibani W, Abbou CC, Guille F, Chopin DK, Lobel B (2004) Multi-institutional validation of a symptom based classification for renal cell carcinoma. J Urol 172:858–862
Pouliot F, Shuch B, Larochelle JC, Pantuck A, Belldegrun AS (2010) Contemporary management of renal tumors with venous tumor thrombus. J Urol 184:833–841; quiz 1235
Ratain MJ, Eckhardt SG (2004) Phase II studies of modern drugs directed against new targets: if you are fazed, too, then resist RECIST. J Clin Oncol 22:4442–4445
Reese AC, Whitson JM, Meng MV (2013) Natural history of untreated renal cell carcinoma with venous tumor thrombus. Urol Oncol 31:1305–1309
Smith AD, Lieber ML, Shah SN (2010a) Assessing tumor response and detecting recurrence in metastatic renal cell carcinoma on targeted therapy: importance of size and attenuation on contrast-enhanced CT. AJR Am J Roentgenol 194:157–165
Smith AD, Shah SN, Rini BI, Lieber ML, Remer EM (2010b) Morphology, attenuation, size, and structure (MASS) criteria: assessing response and predicting clinical outcome in metastatic renal cell carcinoma on antiangiogenic targeted therapy. AJR Am J Roentgenol 194:1470–1478
Therasse P, Arbuck SG, Eisenhauer EA, Wanders J, Kaplan RS, Rubinstein L, Verweij J, Van Glabbeke M, van Oosterom AT, Christian MC, Gwyther SG (2000) New guidelines to evaluate the response to treatment in solid tumors. European Organization for Research and Treatment of Cancer, National Cancer Institute of the United States, National Cancer Institute of Canada. J Natl Cancer Inst 92:205–216
van der Veldt AA, Meijerink MR, van den Eertwegh AJ, Bex A, de Gast G, Haanen JB, Boven E (2008) Sunitinib for treatment of advanced renal cell cancer: primary tumor response. Clin Cancer Res 14:2431–2436
van der Veldt AA, Meijerink MR, van den Eertwegh AJ, Haanen JB, Boven E (2010) Choi response criteria for early prediction of clinical outcome in patients with metastatic renal cell cancer treated with sunitinib. Br J Cancer 102:803–809
Zastrow S, Leike S, Oehlschlager S, Grimm MO, Wirth M (2011) Surgery for renal cell cancer extending into the inferior vena cava - evaluation of survival and perioperative complications using a standardized classification system. BJU Int 108:1439–1443
Conflict of interest
The authors have no conflict of interest or financial disclosures.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kwon, T., Lee, JL., Kim, J.K. et al. The Choi response criteria for inferior vena cava tumor thrombus in renal cell carcinoma treated with targeted therapy. J Cancer Res Clin Oncol 140, 1751–1758 (2014). https://doi.org/10.1007/s00432-014-1703-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-014-1703-6