Abstract
Purpose
To find out whether the most popular pathogenesis hypothesis of the bisphosphonate (BP) related osteonecrosis of the jaw (BRONJ) is comprehensible: (1) is there a higher bone remodeling in the jaw compared with other skeletal sites? (2) Is the bone turnover (BT) of the jaw overly altered after BP intake? (3) Are there gender- or entity-specific differences in BT before and after BP intake?
Methods
Bone scintigraphies of 42 patients with prostate cancer were retrospectively analyzed (n = 21 with BP intake; n = 21 no BP). All patients received bone scintigraphy prior to the therapy and in the course of the treatment (after 12 and 24 months). Data were quantitatively analyzed using six predetermined regions of interest and compared with a breast cancer cohort.
Results
The mandible revealed a similar BT as the femur and a significant lower BT compared with the maxilla. All investigated bone regions showed no significant changes under BP administration. Inter-gender differences revealed significantly lower BT values for the prostate cancer compared with the female breast cancer cohort, changes over the course of time could not be found.
Conclusions
The finding that the mandible revealed a significant lower BT than the maxilla and the fact that 2/3 of the BRONJ cases occur in the mandible are inconsistent with the investigated hypothesis. Furthermore, the BT in the jawbone is not overly suppressed by BP. Thus, it seems implausible that a high BT and its over-suppression play the key role in the pathomechanism of BRONJ.
Similar content being viewed by others

Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Prostate cancer is one of the most frequent malignancies in men (Heidenreich et al. 2008). Bone metastases play a crucial role in this cancer entity and are an important cause of morbidity and disability mostly due to bone pain, spinal cord compression and/or pathologic fractures (Lein et al. 2007). Bisphosphonates (BP) are drugs that reduce bone resorption and bone remodeling. Due to their antiresorptive effects, BP have emerged as an integral tool to reduce and possibly obviate skeletal complications caused by bone metastasis (Aghaloo et al. 2010; Walter et al. 2008).
Although generally well tolerated, in 2003, a new and divesting side effect of a long-term BP administration has been reported: the BP related osteonecrosis of the jaw (BRONJ) (Marx 2003). BRONJ meanwhile has become a major clinical problem of rising importance (Walter et al. 2008). The exact pathomechanism how BP cause BRONJ is unclear. Different theories are discussed including (1) over-suppression of bone turnover (BT) (Huja et al. 2006; Bauss et al. 2008; Walter et al. 2010); (2) altered immune response to infection (Wolf et al. 2006); (3) inhibition of angiogenesis (Scavelli et al. 2007); (4) direct soft tissue toxicity (Otto et al. 2009; Reid et al. 2007); and (5) BP accumulation due to local acidification of the jawbone (Otto et al. 2010). Furthermore, several risk factors have been discussed as promoting the onset of BRONJ (Hoff et al. 2008).
Indeed, the most popular and most cited pathogenesis theory claims that the jawbone exhibits increased BT compared with that of other skeletal sites. Thus, the suppression of bone remodeling with BP would result in the over-suppression of bone areas with high turnover. The clinical consequence of this over-suppression would be osteonecrosis (Garetto and Tricker 1998; Walter et al. 2010). There are several inconsistencies in this theory that is mainly based on few animal studies supporting the limited human data (Garetto and Tricker 1998; Huja et al. 2006; Han et al. 1997). For example, because BRONJ only exceptionally manifests in other bone sites, the BT in the jaw would have to be higher than that of any other bone in the body. Furthermore, the inhibition of BT resulting from BP intake in the jaw would have to be greater than that of the rest of the skeleton. There are other conditions associated with chronically reduced BT (e.g., hyperparathyroidism or antiestrogenic therapy) in which BRONJ-like lesions occur less frequently (Reid 2009). Indeed, the reported prevalence of BRONJ of female patients suffering from breast cancer is significant lower compared with male patients suffering from prostate cancer (2.9 % (Bamias et al. 2005) to 9 %, (Aguiar Bujanda et al. 2007) versus 4.9 % (Bamias et al. 2005) to 18.6 % (Walter et al. 2008), respectively). Thus, it is of utmost interest whether there is a hormone or gender dependency in the pathogenesis of BRONJ.
In this present study, we used bone scans as method of choice to determine (1) whether the BT occurs at a higher rate in the jaw (maxilla/mandible) and (2) whether BT change in bone after BP intake altered to a greater extend in the jaw than in other skeletal sites in men with metastatic prostate cancer. (3) Furthermore, we compared these results to the existing BT results of a female breast cancer collective in order to find out whether there are any gender- or entity-specific differences in BT before and after BP intake.
Materials and methods
Patients
We conducted a retrospective review of all log books, picture database (PACS, version R 11.4.1, Philips Medical Systems, Nederland B.V.), and health plan database (SAP, Release 6.0, Walldorf, Germany) to identify all available patients that received routine staging bone scintigraphy at the Department of Nuclear Medicine, Technische Universität München, Germany, with the diagnosis of prostate cancer between 2009 and 2012 (n = 246). Of this cohort, we identified and included all patients diagnosed with bone metastasis receiving intravenous zoledronic acid (BP group, n = 21) and controls with neither bone metastasis nor BP administration (no-BP group n = 21) with prostate cancer as primary malignancy and existent in-house follow-up bone scintigraphies, with at least one acquisition before BP intake (for the BP group) and follow-up after 12 and 24 months for further analysis (mean age 70.48; standard deviation ±7.25; range 51–86). Patients in the BP group received 4 mg zoledronic acid intravenously every 4 weeks. Furthermore, in order to perform a gender contrasting analysis, data of already published breast cancer patients diagnosed with bone metastasis receiving intravenous zoledronic acid and existent in-house follow-up bone scintigraphies were included for further analysis (n = 45) (Ristow et al. 2013). Patients who had received radiation to the maxilla or mandible, subjects with metastatic or other bone diseases in the jaw as well as diffusely increased skeletal tracer uptake were excluded from the study. Due to the retrospective nature of this study, it was granted an exemption in writing by the University of Munich IRB.
Nuclear medicine imaging
For imaging during routine staging, follow-up, and/or therapy control with respect to a bone involvement, in all patients, a late static whole-body bone scintigraphy 2–4 h after intravenous injection of Technetium-99 m—labeled Diphosphonates (700 MBq) in planar technique was performed. Recordings of the anterior and posterior projections with a table feed of 10 cm/min (>1,500 kCts) using a double-head gamma camera with a high-resolution low-energy parallel hole collimator and a large field of view (Symbia T6 or e.cam, Siemens, Germany) in a 256 × 1,024 matrix were created with a 10 % energy window over the 140-keV photopeak of 99 TC M. Following the acquisition of whole-body imaging additional shots of the left and right lateral cranium centered in maxillary and mandibular regions about 5 min in a 256 × 256 matrix were carried out.
Imaging analysis
For evaluation of images, the available raw data were used. All imaging analysis was performed by the same investigators using OsiriX® Imaging Software (version 5.6., aycan digital systems, Germany) for Mac® OSX 10.7.5 (Apple inc., Cupertino, California, US). For the study group (BP group), all images evaluated were acquired at the same specific investigation points (T): before BP intake (T0 = baseline), 12 (T1) and 24 months (T2) after BP intake. Images of the control group (no-BP group) were routine staging acquisitions acquired at the same specific investigation points (T): at T0 (baseline), 12 (T1) and 24 months (T2) after T0.
All images were evaluated using a previously described semiquantitative analysis performed with the OsiriX® regions of interest (ROI) tool (Van den Wyngaert et al. 2010). In order to measure density and signal intensity, six ROI were predetermined (Area: 1.001 cm2, w: 10.0 mm, h: 10.0 mm) and set over right/left lateral views of the cranium scans (0: background, 1: posterior maxilla, 2: anterior maxilla, 3: anterior mandible, 4: posterior mandible, 5: frontobasal) (Fig. 1a) and anterior/posterior views of the whole-body images (6: femur) (Fig. 1b). The pixel density and the gray value within the region of interest correlate with the bone mineralization and the bone activity, respectively: Increased/decreased tracer activity indicates increased/decreased osteoblastic activity. The ROI on the radionuclide bone scan was defined and the minimal, maximal, and mean count per pixel were determined.
a To quantify bone turnover six regions of interest (ROI) were set over right and left lateral views of the cranium scans: (0) background, (1) posterior maxilla, (2) anterior maxilla, (3) anterior mandible, (4) posterior mandible, (5) frontobasal. Mean BT was measured: Area: 1.001 cm2, w: 10.0 mm, h: 10.0 mm. b Displayed is region of interest (ROI) at (6) femur bone set over anterior/posterior views of the whole-body images. Mean BT was measured: Area: 1.001 cm2, w: 10.0 mm, h: 10.0 mm
Statistical analysis
Further, measurements of the mean count per pixel for all patients were processed in order to derive the variables to be analyzed. First, ROI (0) was subtracted from all ROIs to cancel out background activity. Mean BT of the maxilla and mandible were calculated as follows: Mean BT maxilla: \( {{\left( {\frac{{{\text{ROI}}1_{\text{right }} + {\text{ROI}}2_{\text{right}} }}{2} + \frac{{{\text{ROI}}1_{\text{left }} + {\text{ROI}}2_{\text{left}} }}{2}} \right)} \mathord{\left/ {\vphantom {{\left( {\frac{{{\text{ROI}}1_{\text{right }} + {\text{ROI}}2_{\text{right}} }}{2} + \frac{{{\text{ROI}}1_{\text{left }} + {\text{ROI}}2_{\text{left}} }}{2}} \right)} 2}} \right. \kern-0pt} 2} \); mean BT mandible: \( {{\left( {\frac{{{\text{ROI}}3_{\text{right }} + {\text{ROI}}4_{\text{right}} }}{2} + \frac{{{\text{ROI}}3_{\text{left}} + {\text{ROI}}4_{\text{left}} }}{2}} \right)} \mathord{\left/ {\vphantom {{\left( {\frac{{{\text{ROI}}3_{\text{right }} + {\text{ROI}}4_{\text{right}} }}{2} + \frac{{{\text{ROI}}3_{\text{left}} + {\text{ROI}}4_{\text{left}} }}{2}} \right)} 2}} \right. \kern-0pt} 2} \). For the frontobasal ROI, mean BT was calculated using right/left scans measurements \( \left( {\frac{{{\text{ROI}}5_{\text{right }} + {\text{ROI}}5_{\text{left}} }}{2}} \right) \). Respectively, mean BT of the femur ROI was calculated using the anterior/posterior scans \( \left( {\frac{{{\text{ROI}}6_{\text{ant}} + {\text{ROI}}6_{\text{post}} }}{2}} \right) \). The outcomes represent the analysis variables (adjusted mean BT) and served as basis for further statistical analysis. All statistical analysis was performed using IBM SPSS Statistics software (version 21.0). In addition to the descriptive statistics, the differences between ROIs and the development across time were compared with each other respectively using the two-sided paired samples t test for differences in means. The significance level was set at 5 %.
For the analysis of a potential gender dependency, the results of the present study were correlated to a female cohort, who received zoledronate due to bone metastasis of breast cancer recently published (Ristow et al. 2013). Data of the differences between ROIs and the development across time were respectively compared to the results of the prostate cancer cohort with BP intake using the two-sided paired samples t test for differences in means.
Results
All results are shown for the BP group as mean BT of all patients for each evaluated bone region at three specific investigation points (before BP intake (T0 = baseline), 12 (T1) and 24 months (T2) after BP intake) (Fig. 2a). For the BP group, results for the comparison of different bone regions at three different investigation points showed a significantly (p < 0.01) higher BT within the maxilla (T0: 39.6 ± 9.2; T1: 39.3 ± 10.5; T2: 37.9 ± 11.2) and frontal bone region (T0: 38.6 ± 8.2; T1: 41.0 ± 11.6; T2: 38.3 ± 10.5) compared with the mandible (T0: 27.7 ± 6.5; T1: 28.1 ± 7.3; T2: 28.8 ± 10.3) and the femur bone region (T0: 25.6 ± 8.8; T1: 29.7 ± 7.9; T2: 30.9 ± 11.1) for all three points in time. However, there is no significant difference between the mandible and the femur as well as the maxilla and the frontal bone region of interest (p > 0.05). Respectively for the no-BP group, the results for the comparison of different bone regions at the three specific investigation points showed similar significances as the results of the BP group (p > 0.05). Comparing the results of the BP group and the no-BP group for all respective bone regions at the three specific investigation points, no significant differences could be shown (p > 0.05) (Table 1).
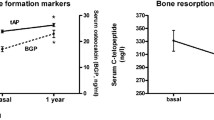
a Shown are mean BT of all patients for each evaluated bone region at three specific investigation points (T0 = before BP administration; T1 = 12 months, T2 = 24 months after BP administration). b Shown are mean BT values as mean of all evaluated bone regions (maxilla, mandible, frontal, femur) comparing the BP-prostate cancer with the BP-breast cancer cohort at three specific investigation points (T0 = before BP administration; T1 = 12 months, T2 = 24 months after BP administration). Note, that inter-gender differences revealed significantly lower BT values for the prostate cancer than the breast cancer group (p < 0.05). However, no significant differences in BT changes over time could be found (p > 0.05)
Changes in BT over time after BP intake for all evaluated bone regions separately were calculated as difference of BT between the three investigation points (T0–T1; T0–T2; T1–T2). For all respective bone regions over the course of time, no significant changes in BT could be found after BP intake (p > 0.05) as well as for the no-BP group (p > 0.05) (Table 2).
For all ROIs at all investigation points, inter-gender differences revealed significantly lower BT values for the prostate cancer than the breast cancer group (p < 0.05) (Fig. 2b). However, comparing the prostate and the breast cancer group, no significant difference in BT changes over the course of time could be found after BP intake for all respective bone regions (p > 0.05).
Discussion
The vast majority of advanced prostate cancer patients suffer from skeletal metastases (Bubendorf et al. 2000). Zoledronic acid is one of the most potent BP with proven efficacy to reduce skeletal complications in patients with metastatic prostate cancer (Aghaloo et al. 2010). One severe adverse effect associated with the use of intravenous BP the osteonecrosis of the jaw. Recent studies have found that the clinical prevalence of BRONJ with oral BP is up to 1 % (Hansen et al. 2012) and up to 20 % in certain patient cohorts receiving intravenous administration (Then et al. 2012). Several reasons might be responsible for the development: an increasing prescription rate of antiresorptive drugs, an advanced detection rate of BRONJ due to higher awareness for this side effect, and a prolonged administration duration of BP. Although this side effect has been known for 10 years, the key questions that surround the manifestation of BRONJ remain to be elucidated: Why is the jawbone almost exclusively affected? What are the pathomechanisms of BRONJ? Several pathogenesis theories exist (Allen and Burr 2009; Otto et al. 2010) while the over-suppression of BT in the jaw is the most popular and the most cited one.
In order to further elucidate the BRONJ pathogenesis, the present study was designed to investigate whether the commonly accepted over-suppression of the jawbone turnover is a crucial event. In animal studies, it could be shown that BP do neither overly accumulate in the jawbone nor suppress the BT in the jaw more than in other sites (Bauss et al. 2008). However, studies on human BT lack.
Bone scans are simple tools for quantitative bone metabolism and blood flow evaluation. In contrast with other techniques, this method does not provide an absolute measure of whole-body skeletal uptake or plasma clearance (Van den Wyngaert et al. 2010). However, it is straightforward to perform and does not require the acquisition of images immediately following tracer administration. Moreover, it allows the quantification of BT of a specified region relative to another skeletal site.
The results of this study show that the BT of the mandible was similar to the femur and significantly lower compared with the maxilla (and the frontal bone region) for all three investigation time points. Another interesting result of the present study is that all investigated bone regions (including mandible and maxilla) showed no significant BT changes over the course of time and after 24 months of BP administrations. These results are also reflected in the findings of the gender-specific comparison with the existing breast cancer data (Ristow et al. 2013). Although there is an overall significant higher BT in females, no significant BT changes over the course of time could be declared in this cohort as well. On the one hand, a possible over-suppression particularly of the jawbone appears thus unlikely to be a crucial factor in the pathogenesis of BRONJ. On the other hand, a significant and measurable difference between male and female jawbone turnover was found. The finding that the female cohort reveals a significant higher BT but a significant lower BRONJ prevalence is in line with the finding that the maxilla exhibits a significant higher BT but a significant lower BRONJ manifestations compared with the mandible (approximately 2/3 of the published BRONJ cases occur in the mandible (Abu-Id et al. 2008; Otto et al. 2012)). Therefore, it seems implausible that a high BT is a predictive value or a crucial risk factor for a BRONJ manifestation.
A small number of studies have been performed showing the potential of bone scintigraphy using 99mTc-labeled BP in studies examining the pathophysiology of BRONJ. However, none of these studies was performed in a longitudinal manner evaluating BT changes prior to the initiation of BP and subsequently compared with measurements during the BP therapy (Van den Wyngaert et al. 2010; Morris et al. 2010). Both investigators (Morris et al. 2010; Van den Wyngaert et al. 2010) applied a technique previously described using a ratio to calculate the different BT. In the present study, we concentrated on observing BT development over time. Since a ratio change over time does not allow any conclusions on changes of numerator or denominator, we decided not to use the same approach. Instead, we investigated the trends of the different ROIs separately.
A limitation of this study is the semiquantitative nature of the applied technique. It is not possible to make an ultimate statement on the measured magnitude of skeletal sites BT since this method is influenced by differences in bone mass, differences of trabecular and cortical bone as well as local soft tissue attenuation (Ackerman and Shirazi 1997; Boyle et al. 2003).
Conclusion
The present study showed that the BT in the mandible is comparable to other bone sites (femur) and significantly lower than maxilla. It was further demonstrated that the BT in the jawbone (both mandible and maxilla) was not overly suppressed after BP administration. Although there was an overall higher BT in female patients (suffering from breast cancer compared to the male cohort suffering from prostate cancer), the gender-specific comparison showed no significant difference in BT after BP administration over the course of time and after 24 months.
References
Abu-Id MH, Warnke PH, Gottschalk J, Springer I, Wiltfang J, Acil Y, Russo PA, Kreusch T (2008) “Bis-phossy jaws”—high and low risk factors for bisphosphonate-induced osteonecrosis of the jaw. J Craniomaxillofac Surg 36(2):95–103. doi:10.1016/j.jcms.2007.06.008
Ackerman L, Shirazi P (1997) Abnormal skull uptake on bone scan. Semin Nucl Med 27(2):190–193
Aghaloo TL, Felsenfeld AL, Tetradis S (2010) Osteonecrosis of the jaw in a patient on Denosumab. J Oral Maxillofac Surg 68(5):959–963. doi:10.1016/j.joms.2009.10.010
Aguiar Bujanda D, Bohn Sarmiento U, Cabrera Suarez MA, Aguiar Morales J (2007) Assessment of renal toxicity and osteonecrosis of the jaws in patients receiving zoledronic acid for bone metastasis. Ann Oncol 18(3):556–560. doi:10.1093/annonc/mdl408
Allen MR, Burr DB (2009) The pathogenesis of bisphosphonate-related osteonecrosis of the jaw: so many hypotheses, so few data. J Oral Maxillofac Surg 67(5 Suppl):61–70. doi:10.1016/j.joms.2009.01.007
Bamias A, Kastritis E, Bamia C, Moulopoulos LA, Melakopoulos I, Bozas G, Koutsoukou V, Gika D, Anagnostopoulos A, Papadimitriou C, Terpos E, Dimopoulos MA (2005) Osteonecrosis of the jaw in cancer after treatment with bisphosphonates: incidence and risk factors. J Clin Oncol 23(34):8580–8587. doi:10.1200/JCO.2005.02.8670
Bauss F, Pfister T, Papapoulos S (2008) Ibandronate uptake in the jaw is similar to long bones and vertebrae in the rat. J Bone Miner Metab 26(4):406–408. doi:10.1007/s00774-007-0837-x
Boyle WJ, Simonet WS, Lacey DL (2003) Osteoclast differentiation and activation. Nature 423(6937):337–342. doi:10.1038/nature01658
Bubendorf L, Schopfer A, Wagner U, Sauter G, Moch H, Willi N, Gasser TC, Mihatsch MJ (2000) Metastatic patterns of prostate cancer: an autopsy study of 1,589 patients. Hum Pathol 31(5):578–583
Garetto LP, Tricker ND (1998) Remodeling of bone surrounding the implant interface. In: Garetto LP, Turner CH, Duncan RL, Burr DB (eds) Bridging the gap between dental and orthopaedic implants. Indianapolis, IN
Han ZH, Palnitkar S, Rao DS, Nelson D, Parfitt AM (1997) Effects of ethnicity and age or menopause on the remodeling and turnover of iliac bone: implications for mechanisms of bone loss. J Bone Min Res 12(4):498–508. doi:10.1359/jbmr.1997.12.4.498
Hansen PJ, Knitschke M, Draenert FG, Irle S, Neff A (2012) Incidence of bisphosphonate-related osteonecrosis of the jaws (BRONJ) in patients taking bisphosphonates for osteoporosis treatment-a grossly underestimated risk? Clin Oral Invest. doi:10.1007/s00784-012-0873-3
Heidenreich A, Aus G, Bolla M, Joniau S, Matveev VB, Schmid HP, Zattoni F (2008) EAU guidelines on prostate cancer. Eur Urol 53(1):68–80. doi:10.1016/j.eururo.2007.09.002
Hoff AO, Toth BB, Altundag K, Johnson MM, Warneke CL, Hu M, Nooka A, Sayegh G, Guarneri V, Desrouleaux K, Cui J, Adamus A, Gagel RF, Hortobagyi GN (2008) Frequency and risk factors associated with osteonecrosis of the jaw in cancer patients treated with intravenous bisphosphonates. J Bone Mineral Res 23(6):826–836. doi:10.1359/jbmr.080205
Huja SS, Fernandez SA, Hill KJ, Li Y (2006) Remodeling dynamics in the alveolar process in skeletally mature dogs. Anat Rec A Discov Mol Cell Evol Biol 288(12):1243–1249. doi:10.1002/ar.a.20396
Lein M, Wirth M, Miller K, Eickenberg HU, Weissbach L, Schmidt K, Haus U, Stephan C, Meissner S, Loening SA, Jung K (2007) Serial markers of bone turnover in men with metastatic prostate cancer treated with zoledronic Acid for detection of bone metastases progression. Eur Urol 52(5):1381–1387. doi:10.1016/j.eururo.2007.02.033
Marx RE (2003) Pamidronate (Aredia) and zoledronate (Zometa) induced avascular necrosis of the jaws: a growing epidemic. J Oral Maxillofac Surg 61(9):1115–1117
Morris PG, Poznak CV, Modi S, Mak AF, Patil S, Larson S, Hudis CA, Divgi C, Grewal RK (2010) Intravenous bisphosphonate therapy does not acutely alter nuclear bone scan results. Clin Breast Cancer 10(1):33–39. doi:10.3816/CBC.2010.n.004
Otto S, Hafner S, Grotz KA (2009) The role of inferior alveolar nerve involvement in bisphosphonate-related osteonecrosis of the jaw. J Oral Maxillofac Surg 67(3):589–592. doi:10.1016/j.joms.2008.09.028
Otto S, Hafner S, Mast G, Tischer T, Volkmer E, Schieker M, Sturzenbaum SR, von Tresckow E, Kolk A, Ehrenfeld M, Pautke C (2010) Bisphosphonate-related osteonecrosis of the jaw: is pH the missing part in the pathogenesis puzzle? J Oral Maxillofac Surg 68(5):1158–1161. doi:10.1016/j.joms.2009.07.079
Otto S, Schreyer C, Hafner S, Mast G, Ehrenfeld M, Sturzenbaum S, Pautke C (2012) Bisphosphonate-related osteonecrosis of the jaws—characteristics, risk factors, clinical features, localization and impact on oncological treatment. J Craniomaxillofac Surg 40(4):303–309. doi:10.1016/j.jcms.2011.05.003
Reid IR (2009) Osteonecrosis of the jaw: who gets it, and why? Bone 44(1):4–10. doi:10.1016/j.bone.2008.09.012
Reid IR, Bolland MJ, Grey AB (2007) Is bisphosphonate-associated osteonecrosis of the jaw caused by soft tissue toxicity? Bone 41(3):318–320. doi:10.1016/j.bone.2007.04.196
Ristow O, Gerngroß C, Schwaiger M, Hohlweg-Majert B, Kehl V, Jansen H, Hahnefeld L, Otto S, Pautke C (2013) Is the bone turnover of the jawbone and its possible oversuppression by bisphosphonates of etiological importance for the pathogenesis of the bisphosphonate-related osteonecrosis? J Oral Maxillofac Surg. doi:10.1016/j.joms.2013.11.005
Scavelli C, Di Pietro G, Cirulli T, Coluccia M, Boccarelli A, Giannini T, Mangialardi G, Bertieri R, Coluccia AM, Ribatti D, Dammacco F, Vacca A (2007) Zoledronic acid affects over-angiogenic phenotype of endothelial cells in patients with multiple myeloma. Mol Cancer Ther 6(12 Pt 1):3256–3262. doi:10.1158/1535-7163.MCT-07-0311
Then C, Horauf N, Otto S, Pautke C, von Tresckow E, Rohnisch T, Baumann P, Schmidmaier R, Bumeder I, Oduncu FS (2012) Incidence and risk factors of bisphosphonate-related osteonecrosis of the jaw in multiple myeloma patients having undergone autologous stem cell transplantation. Onkologie 35(11):658–664. doi:10.1159/000343950
Van den Wyngaert T, Huizing MT, Fossion E, Vermorken JB (2010) Scintigraphic evaluation of mandibular bone turnover in patients with solid tumors receiving zoledronic acid. Oral Oncol 46(3):214–218. doi:10.1016/j.oraloncology.2010.01.001
Walter C, Al-Nawas B, Grotz KA, Thomas C, Thuroff JW, Zinser V, Gamm H, Beck J, Wagner W (2008) Prevalence and risk factors of bisphosphonate-associated osteonecrosis of the jaw in prostate cancer patients with advanced disease treated with zoledronate. Eur Urol 54(5):1066–1072. doi:10.1016/j.eururo.2008.06.070
Walter C, Klein MO, Pabst A, Al-Nawas B, Duschner H, Ziebart T (2010) Influence of bisphosphonates on endothelial cells, fibroblasts, and osteogenic cells. Clin Oral Invest 14(1):35–41. doi:10.1007/s00784-009-0266-4
Wolf AM, Rumpold H, Tilg H, Gastl G, Gunsilius E, Wolf D (2006) The effect of zoledronic acid on the function and differentiation of myeloid cells. Haematologica 91(9):1165–1171
Acknowledgments
This research project is part of the doctoral thesis of Roswitha Schuster.
Conflicts of interest
We declare that we have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ristow, O., Gerngroß, C., Schwaiger, M. et al. Does regular zoledronic acid change the bone turnover of the jaw in men with metastatic prostate cancer: A possible clue to the pathogenesis of bisphosphonate related osteonecrosis of the jaw?. J Cancer Res Clin Oncol 140, 487–493 (2014). https://doi.org/10.1007/s00432-014-1588-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-014-1588-4