Abstract
Cytomegalovirus (CMV) reactivation is a common complication in patients with inflammatory bowel diseases (IBD), particularly in those with steroid-resistant ulcerative colitis. It is usually diagnosed by histopathologic and immunohistochemical examination of the colon biopsy. The introduction of quantitative, real-time polymerase chain reaction (qPCR) has been recommended to improve the sensitivity, but there is little consensus on how to use it. We compared the two methods in samples from resected bowel of patients with IBD. Twelve patients with IBD who had undergone bowel resection were analysed for CMV, using qPCR and immunohistochemistry. In all cases, tissue samples from the base and the edge of ulcers and from uninvolved mucosa were obtained. The highest densities of CMV-positive cells were found in samples from the base of ulcers (immunohistochemistry 0–0.47 positive cells/mm2; qPCR 10–3809 viral copies/mg) or the edge of ulcers (immunohistochemistry 0.06–0.32 positive cells/mm2; qPCR 35–1049 viral copies/mg). In samples of uninvolved mucosa, immunohistochemistry was negative, whereas qPCR was either negative or showed very low values (0–3 viral copies/mg). We conclude that both immunohistochemistry and qPCR can be successfully used for diagnosing CMV reactivation in patients with IBD. The base and the edge of ulcers are the optimal sites for endoscopic biopsies. The density of CMV-positive cells was low and their distribution within the colon uneven. It therefore seems that the number of sampled biopsies and/or the number of investigated levels is more important that the choice of diagnostic method.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cytomegalovirus (CMV) is a member of the Herpesviridea family, causing common infection in humans, usually presenting as a mild, self-limited mononucleosis-like syndrome. After primary infection, the virus becomes latent and can be reactivated, particularly in a situation of immunosuppression, such as in patients with organ transplantation or in those receiving immunosuppressive treatment [1, 2]. It is important to distinguish between CMV infection and CMV disease. CMV infection is defined as isolation of CMV virus or detection of viral proteins or nucleic acids from body fluid or tissue, while CMV disease is defined as a combination of clinical symptoms, morphologic changes in the target organ(s) and demonstration of CMV in tissue by immunohistochemistry, in situ hybridisation or culture [3]. In patients with CMV reactivation, the colon is one of the most frequently involved organs [4]. Patients with inflammatory bowel disease (IBD) are a special risk group, particularly those with ulcerative colitis (UC) with a poor response to corticosteroid treatment [5–9]. It rarely occurs in patients with Crohn’s disease (CD) [8, 10, 11]. In patients with IBD, CMV reactivation is usually limited to the colon [5, 7, 12], systemic involvement is rare [13].
The clinical significance of CMV reactivation in patients with IBD remains controversial [14–16]. It seems that it is often a self-limited condition that does not require special treatment [10, 17–19]. However, there is evidence suggesting that it may be associated with a significant morbidity [7, 9, 20–22]. In these patients, antiviral therapy would probably be beneficial.
Diagnosing CMV reactivation in the colon is another unresolved issue. Several methods for CMV detection are available, with variable sensitivity and specificity, which can be performed on blood, peripheral leukocytes, body fluids etc. [1]. Most of them are of little value for diagnosing CMV colitis, particularly in patients with IBD, in whom CMV reactivation is usually limited to the colon and is not a part of systemic disease. Histopathologic examination of the colon biopsy with immunohistochemistry remains the gold standard for diagnosing CMV colitis [6, 12, 19, 23]. The introduction of quantitative, real-time polymerase chain reaction (qPCR) has been recommended in the diagnostic procedure of CMV colitis to improve the sensitivity, but there is little consensus on how to use it [9, 19, 24].
The aim of our study was to compare the two most important methods for detection of CMV, immunohistochemistry and qPCR, in samples from the resected colon of patients with IBD. We analyzed the density of CMV-positive cells in various sites of the resected colon to determine the optimal site for endoscopic biopsy, and we tested qPCR for CMV on formalin-fixed, paraffin-embedded tissue. The case selection was also important. The patients included in the study had CMV and IBD with various clinical significance, reflecting the complex nature of CMV reactivation in IBD.
Materials and methods
The study was approved by the Ethical Commission of the Republic of Slovenia.
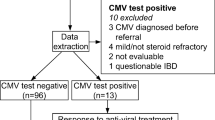
The files of the Institute of Pathology, Faculty of Medicine, University of Ljubljana, were searched for the last 3 years for bowel resections from patients with IBD with positive immunohistochemistry for CMV. The control group consisted of bowel resections from matched patients with IBD with negative immunohistochemistry for CMV. Finally, bowel resections were also included from patients with IBD in whom biopsy prior to surgery exhibited positive immunohistochemistry for CMV but was negative on resection specimens. The diagnosis of IBD was made on the basis of clinical, endoscopic, radiologic and histological findings. For the purpose of this study, the most important demographic (age, gender) and clinical data (IBD type and duration, therapy, indication for bowel resection) were collected.
The resection specimens had been handled according to the published international guidelines [25]. Samples had been taken from inflamed mucosa, ulcers and erosions, as well as from resection margins and macroscopically normal mucosa, if present. All samples had been embedded in paraffin and cut at 4 μm, stained with haematoxylin and eosin (HE) and analyzed according to standard procedures. Immunohistochemistry had been performed on the basis of microscopic features or on the basis of clinical suspicion. PCR had not been performed as part of routine procedure.
For the purpose of this study, all HE slides were reviewed, and in each case, 3 samples with corresponding paraffin blocks were chosen for additional analyses (immunohistochemistry and qPCR): one from the base of erosions/ulcers with abundant granulation tissue, one from the edge of the erosions/ulcers, and one from the normal/uninvolved mucosa. If this was not present, the sample with the least involved mucosa was chosen; it may have contained inflammation, but not erosions or ulcers.
For immunohistochemistry, 3 step sections at 50 μm intervals were obtained from the selected paraffin blocks. Commercially available antibodies against CMV (Dako, CCH2 + DDG9, dilution 1:20) were used. Antigen retrieval and staining with antibodies was performed in an automatic immunostainer Benchmarck™ XT (Ventana Medical System, Tucson, AZ, USA). Sections were treated with biotinylated secondary antibody, followed by incubation with peroxidase conjugated streptavidin (iVIEW™ DAB Detection Kit, Ventana Medical System, Tucson, AZ, USA). Visualisation of the immunoreaction was carried out with 3.3′ diaminobenzidine. Finally, sections were counterstained with haematoxylin. The density of positive cells was determined using NIS Elements microscope imaging software for microscopy (Nikon, Tokyo, Japan) and expressed as the number of positive cells per square millimeter. Positive controls and negative controls omitting the primary antibodies were also included.
The extraction of nucleic acids from paraffin-embedded tissue was performed manually, using QIAamp DNA Mini Kit (Qiagen GmbH, Hilden, Germany) according to the manufacturer’s instructions. Extracted nucleic acids were eluted in 100 μl of elution buffer. Quantitative real-time PCR was performed using R-gene CMV HHV6,7,8 diagnostic reagents (Argene, BioMerieux, France), with 10 μl of DNA in 25 μl reaction volume, using Roche LightCycler 480 II system (Roche Applied Science, Mannheim, Germany). The positive results were expressed as genome copies of CMV per milligram of paraffin-embedded tissue.
For statistical analysis, the results of immunohistochemistry and PCR had been attributed a value of 0 for a negative result and a value of 1 for a positive result. Results have been compared using two-tailed Fisher’s exact test.
Results
The most important demographic and clinical data and the results of immunohistochemistry and qPCR are presented in Table 1.
Group 1 (patients 1–5 in Table 1) consisted of 5 patients with IBD with CMV reactivation (4 patients with UC and 1 with CD). There were 3 females and 2 males, aged 24–67 years (mean 51.4 ± 18.3). Patients had suffered from IBD for 1 to 8 years (mean 3.2 ± 2.95). In 1 patient, the indication for surgery was perforation of the colon, and in the remaining patients, indication for surgery was severe colitis, unresponsive to treatment.
Group 2 (patients 6–10 in Table 1) consisted of 5 patients with IBD with no immunohistochemical evidence of CMV reactivation (4 patients with UC and 1 with CD). There were 3 females and 2 males, aged 27–65 years (mean 49.6 ± 15.27). Patients had suffered from IBD for 1 to 14 years (mean 4.8 ± 5.40). In 1 patient, the indication for surgery was perforation of the colon, and in the remaining patients, the indication for surgery was severe colitis, unresponsive to treatment.
Group 3 (patients 11–12 in Table 1) consisted of 2 patients (a female and a male, aged 34 and 69 years) with UC who had immunohistochemically proven CMV reactivation on biopsy, but not on subsequently performed resection of the colon. Patients had suffered from IBD for 1 and 2 years, respectively (mean 1.5 years).
Immunohistochemistry for CMV was positive in all patients from Group 1 (patients 1–5 in Table 1 and Fig. 1). The density of positive cells in samples from the base of ulcers ranged from 0 to 0.47 cells/mm2 (mean 0.25 ± 0.20) and in the samples from the edge of ulcers, it ranged from 0.06 to 0.32 cells/mm2 (mean 0.17 ± 0.11). In 4 patients, the highest density was found in samples from the base of the ulcer, and in one patient, in samples from the edge of the ulcer.
No positive cells were found in the samples of uninvolved/the least involved mucosa. In these samples, mucosa was normal in 2 cases and inflamed in 3 cases, but there were no erosions or ulcers.
Immunohistochemistry was negative in all samples from Groups 2 and 3 (patients 6–12 in Table 1). In samples of uninvolved/the least involved mucosa, mucosa was normal in 4 cases and inflamed in 3 cases, but there were no erosions or ulcers.
qPCR for CMV was positive in all patients from Group 1 (patients 1–5 in Table 1). The number of viral copies/mg of paraffin-embedded tissue in samples from the base of ulcers ranged from 0 to 3809 (mean 1578.60 ± 1669.49), in samples from the edge of ulcers from 35 to 1049 (mean 437.20 ± 456.91), and in samples from uninvolved mucosa, it ranged from 0 to 3 (mean 0.8 ± 1.3). In 3 patients, the highest values were observed in samples from the base of ulcers, and in 2 patients, in samples from the edge of ulcers. qPCR for CMV was negative in all patients from Groups 2 and 3 (patients 6–12 in Table 1).
Cytomegalovirus reactivation in ulcerative colitis. a Macroscopic features of the resected colon: diffuse erythema of the mucosa, with ulcerations and pseudopolyps. b Base of an ulcer with abundant proliferation of granulation tissue, without clearly visible viral inclusions. c A small, atypical inclusion in an endothelial cell (arrow). d Positive immunohistochemical reaction in two capillary endothelial cells
Positive or negative immunohistochemical result corresponded to a positive or negative qPCR, respectively (p = 0.002 for base of ulcer and p = 0.0013 for edge of ulcer, Fisher’s exact test).
Discussion
Our results indicate that CMV colitis can be successfully diagnosed by immunohistochemistry and qPCR. The highest values of CMV by both methods were detected in samples from the base of the ulcer in some patients, and in samples from the edge of the ulcer in the others. These findings suggest that, at endoscopy, biopsy samples should be obtained from the base and edge of ulcers. Our study also shows that qPCR can be successfully performed on formalin-fixed, paraffin-embedded tissue.
Immunohistochemistry is generally accepted as the gold standard for diagnosing CMV colitis. Our results fully support this view. In contrast to other organs, CMV infection in the colon, particularly in association with IBD, does not always produce the diagnostic large cells with viral inclusions with owl’s eyes appearance. Rather, the infected cells are frequently smaller, up to twice as big as their normal counterparts, and have small basophilic inclusions, often with no characteristic clear halo. They have been called “atypical inclusions” [5]. A diagnosis of CMV colitis cannot therefore be made on the basis of morphology alone. Immunohistochemistry must be performed in all cases with suspicious enlarged cells and/or clinical indication. Positive cells usually show nuclear and occasionally cytoplasmic inclusions, mostly located in endothelial cells. In our study, the density of positive cells was highest in samples from the base of ulcers, but they were also found in samples from the edge of ulcers. The density of positive cells was low, from 0.06 to 0.47 per mm2. Importantly, positive cells were not detected in uninvolved mucosa.
In contrast to immunohistochemistry, the use of qPCR in the diagnosis of CMV reactivation in IBD is more controversial. Recent guidelines of the European Crohn’s and Colitis Organisation (ECCO) recommend the use of qPCR to diagnose CMV colitis [19]. However, there is little consensus on how to use it, and the use of qPCR on colon tissue alone is not widely considered to provide definitive proof of CMV colitis [3, 26]. The most important concern is related to the specificity of PCR [12, 27–29]. CMV typically produces latent infection residing in leukocytes. The concern has been raised that positive PCR might therefore not necessarily reflect active disease in the colon but only latent infection. However, in our study, we observed good correlation amongst the density of positive cells by immunohistochemistry, the morphology and the number of viral copies by qPCR. Furthermore, good correlation was also found in uninvolved mucosa: there were no positive cells by immunohistochemistry and qPCR was either negative or gave very low values of viral copies. The usefulness of both immunohistochemistry and qPCR for detecting CMV reactivation is further supported by our observation of negative qPCR and immunohistochemistry in the resected colon of two patients with IBD who had had biopsy-proven episodes of CMV reactivation prior to resection. These results suggest that past episodes of CMV reactivation in the colon do not result in positive PCR.
Another problematic issue is fresh versus paraffin-embedded tissue. Previous investigations have mostly been performed on fresh tissue, which can be difficult to obtain in routine practice, while formalin-fixed, paraffin-embedded tissue samples are widely available. Introduction of qPCR on formalin-fixed, paraffin-embedded tissue would enable prior routine histopathology evaluation and immunohistochemistry and the selection of the most appropriate block for qPCR, when necessary. Recent studies by Mills et al. [30] and MyCoy et al. [31] and our own results clearly show that PCR can be successfully performed on formalin-fixed, paraffin-embedded tissue samples. It must be kept in mind, however, that the number of viral copies per mg of paraffin-embedded tissue will be lower than in the same amount of fresh tissue.
Our findings are in accordance with recent studies comparing immunohistochemistry and qPCR for CMV on endoscopic biopsy samples of gastrointestinal mucosa [30, 31]. In these studies, qPCR also proved to be a sensitive and specific method for detection of CMV disease. For qPCR, a specificity of 98.7 % was found using traditional histology as a true negative definition. For traditional histology, a 97 % specificity was detected using qPCR as a true negative definition [31]. There is, however, an important difference in relation to the three studies: in the present study, only patients with IBD were included, whereas other patients with CMV disease of the gastrointestinal tract were also included in the other two [30, 31], for example those with HIV and after organ transplantation. This different patient selection is important because, in our experience, CMV reactivation in IBD patients is even more difficult to diagnose than in other patients, because the characteristic viral inclusions tend to be scarce.
Our selection criteria resulted in a small number of patients, because surgical therapy in such patients is quite rare. This is the main limitation of our study. However, this approach enabled to perform analyses which would not be possible in small endoscopic colon samples, usually available in routine work. In resection specimens of the colon, enough tissue was available for comparison of the two methods. Furthermore, we were able to choose samples from various sites: from the base and edge of the ulcers and erosions, and from uninvolved mucosa to analyse the density and distribution of CMV-positive cells within the colon.
Finally, our study unfortunately does not provide an answer to the most important question—that of the clinical significance of CMV reactivation in patients with IBD. In fact, the patients included in our study reflect the complex nature of CMV reactivation in the colon. It appears that in rare patients, CMV reactivation is associated with severe complications (for example, perforation of the colon), and they would probably benefit from antiviral treatment, whereas in the others, CMV reactivation is a self-limiting disease that does not require treatment. Episodes of CMV reactivation also occur in patients with severe colitis that responds poorly to treatment and eventually requires surgical treatment, regardless of CMV reactivation. It remains to be determined which patients with CMV colitis would benefit from treatment with antiviral agents.
In conclusion, both immunohistochemistry and qPCR can be successfully used for diagnosing CMV reactivation in patients with IBD. The base and the edge of ulcers are the optimal sites for endoscopic biopsies. We agree with Mills et al. [30] suggesting that qPCR should be used as an adjunct to immunohistochemistry in biopsies in which immunohistochemistry is negative or equivocal but a strong clinical suspicion of CMV reactivation exists. The density of CMV-positive cells was low and their distribution within the colon was uneven. It therefore seems that the amount of tissue evaluated, as illustrated by the number of sampled biopsies and/or the number of investigated levels, is more important that the choice of diagnostic method. Future studies, which specifically address this issue, are warranted.
References
Landolfo S, Gariglio M, Gribaudo G, Lembo D (2003) The human cytomegalovirus. Pharmacol Ther 98:269–297
Crough K, Khanna R (2009) Immunobiology of cytomegalovirus: from bench to bedside. Clin Microbiol Rev 22:76–98
Ljungman P, Griffiths P, Paya C (2002) Definitions of cytomegalovirus infection and disease in transplant recipients. Clin Infect Dis 34:1094–1097
You DM, Johnson MD (2012) Cytomegalovirus infection and the gastrointestinal tract. Curr Gastroenterol Rep 14:334–342
Kambham N, Vij R, Cartwright CA, Longacre T (2004) Cytomegalovirus infection in steroid-refractory ulcerative colitis: a case-control study. Am J Surg Pathol 28:365–373
Kandiel A, Lashner B (2006) Cytomegalovirus colitis complicating inflammatory bowel disease. Am J Gastroenterol 101:2857–2865
Domènech E, Vega R, Ojanguren I, Hernández A, Garcia-Planella E, Bernal I, Rosinach M, Boix J, Cabré E, Gassull MA (2008) Cytomegalovirus infection in ulcerative colitis: a prospective, comparative study on prevalence and diagnostic strategy. Inflamm Bowel Dis 14:1373–1379
Roblin X, Pillet S, Oussalah A, Berthelot P, Del Tedesco E, Phelip JM, Chambonnière ML, Garraud O, Peyrin-Biroulet L, Pozzetto B (2011) Cytomegalovirus load in inflamed intestinal tissue is predictive of resistance to immunosuppressive therapy in ulcerative colitis. Am J Gastroenterol 106:2001–2008
Maher MM, Nassar MI (2009) Acute cytomegalovirus infection is a risk factor in refractory and complicated inflammatory bowel disease. Dig Dis Sci 54:245662
Kim JJ, Simpson N, Klipfel N, Debose R, Barr N, Laine L (2010) Cytomegalovirus infection in patients with active inflammatory bowel disease. Dig Dis Sci 55:1059–1065
Nakase H, Yoshino T, Honzawa Y, Chiba T (2010) Low prevalence of CMV infection in patients with Crohn’s disease in comparison with ulcerative colitis: effect of different immune response on prevalence of CMV infection. Dig Dis Sci 55:1498–1499
Lawlor G, Moss AC (2010) Cytomegalovirus in inflammatory bowel disease: pathogen or innocent bystander? Inflamm Bowel Dis 16:1620–1627
Hamlin PJ, Shah MN, Scott N, Wyatt JI, Howdle PD (2004) Systemic cytomegalovirus infection complicating ulcerative colitis: a case report and review of the literature. Postgrad Med J 80:233–235
Hommes DW, Sterringa G, van Deventer SJ, Tytgat GN, Weel J (2004) The pathogenicity of cytomegalovirus in inflammatory bowel disease: a systematic review and evidence-based recommendations for future research. Inflamm Bowel Dis 10:245–250
Pillet S, Pozzetto B, Jarlot C, Paul S, Roblin X (2012) Management of cytomegalovirus infection in inflammatory bowel diseases. Dig Liver Dis 44:541–548
Garrido E, Carrera E, Manzano R, Lopez-Sanroman A (2013) Clinical significance of cytomegalovirus infection in patients with inflammatory bowel disease. World J Gastroenterol 19:17–25
Matsuoka K, Iwao Y, Mori T, Sakuraba A, Yajima T, Hisamatsu T, Okamoto S, Morohoshi Y, Izumiya M, Ichikawa H, Sato T, Inoue N, Ogata H, Hibi T (2007) Cytomegalovirus is frequently reactivated and disappears without antiviral agents in ulcerative colitis patients. Am J Gastroenterol 102:331–337
Delvincourt M, Lopez A, Pillet S, Bourrier A, Seksik P, Cosnes J, Carrat F, Gozlan J, Beaugerie L, Roblin X, Peyrin-Biroulet L, Sokol H (2014) The impact of cytomegalovirus reactivation and its treatment on the course of inflammatory bowel disease. Aliment Pharmacol Ther 39:712–720
Rahier JF, Magro F, Abreu C, Armuzzi A, Ben-Horin S, Chowers Y, Cottone M, de Ridder L, Doherty G, Ehehalt R, Esteve M, Katsanos K, Lees CW, Macmahon E, Moreels T, Reinisch W, Tilg H, Tremblay L, Veereman-Wauters G, Viget N, Yazdanpanah Y, Eliakim R, Colombel JF, European Crohn’s Colitis Organisation (ECCO) (2014) Second European evidence-based consensus on the prevention, diagnosis and management of opportunistic infections in inflammatory bowel disease. J Crohns Colitis 8:443–468
Papadakis KA, Tung JK, Binder SW, Kam LY, Abreu MT, Targan SR, Vasiliauskas EA (2001) Outcome of cytomegalovirus infections in patients with inflammatory bowel disease. Am J Gastroenterol 96:2137–2142
Maconi G, Colombo E, Zerbi P, Sampietro GM, Fociani P, Bosani M, Cassinotti A, Casini V, Russo A, Ardizzone S, Porta M, Bianchi Porro G (2005) Prevalence, detection rate and outcome of cytomegalovirus infection in ulcerative colitis patients requiring colonic resection. Dig Liver Dis 37:418–423
Al-Zafiri R, Gologan A, Galiatsatos P, Szilagyi A (2012) Cytomegalovirus complicating inflammatory bowel disease: a 10-year experience in a community-based, university-affiliated hospital. Gastroenterol Hepatol (N Y) 8:230–239
Muir SW, Murray J, Farquharson MA, Wheatley DJ, McPhaden AR (1998) Detection of cytomegalovirus in upper gastrointestinal biopsies from heart transplant recipients: comparison of light microscopy, immunocytochemistry, in situ hybridisation, and nested PCR. J Clin Pathol 51:807–811
Yoshino T, Nakase H, Ueno S, Uza N, Inoue S, Mikami S, Matsuura M, Ohmori K, Sakurai T, Nagayama S, Hasegawa S, Sakai Y, Chiba T (2007) Usefulness of quantitative real-time PCR assay for early detection of cytomegalovirus infection in patients with ulcerative colitis refractory to immunosuppressive therapies. Inflamm Bowel Dis 13:1516–1521
Magro F, Langner C, Driessen A, Ensari A, Geboes K, Mantzaris GJ, Villanacci V, Becheanu G, Borralho Nunes P, Cathomas G, Fries W, Jouret-Mourin A, Mescoli C, de Petris G, Rubio CA, Shepherd NA, Vieth M, Eliakim R, European Society of Pathology (ESP); European Crohn’s and Colitis Organisation (ECCO) (2013) European consensus on the histopathology of inflammatory bowel disease. J Crohns Colitis 7:827–851
Boeckh M (2011) Complications, diagnosis, management, and prevention of CMV infections: current and future. Hematol Am Soc Hematol Educ Program 2011:305–309
Ljungman P, de la Camara R, Cordonnier C, Einsele H, Engelhard D, Reusser P, Styczynski J, Ward K (2008) Management of CMV, HHV-6, HHV-7 and Kaposi-sarcoma herpesvirus (HHV-8) infections in patients with hematological malignancies and after SCT. Bone Marrow Transplant 42:227–240
Ganzenmueller T, Henke-Gendo C, Schlué J, Wedemeyer J, Huebner S, Heim A (2009) Quantification of cytomegalovirus DNA levels in intestinal biopsies as a diagnostic tool for CMV intestinal disease. J Clin Virol 46:254–258
Lemonovich TL, Watkins RR (2012) Update on cytomegalovirus infections of the gastrointestinal system in solid organ transplant recipients. Curr Infect Dis Rep 14:33–40
Mills AM, Guo FP, Copland AP, Pai RK, Pinsky BA (2013) A comparison of CMV detection in gastrointestinal mucosal biopsies using immunohistochemistry and PCR performed on formalin-fixed, paraffin-embedded tissue. Am J Surg Pathol 37:995–1000
McCoy MH, Post K, Sen JD, Chang HY, Zhao Z, Fan R, Chen S, Leland D, Cheng L, Lin J (2014) qPCR increases sensitivity to detect cytomegalovirus in formalin-fixed, paraffin-embedded tissue of gastrointestinal biopsies. Hum Pathol 45:48–53
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zidar, N., Ferkolj, I., Tepeš, K. et al. Diagnosing cytomegalovirus in patients with inflammatory bowel disease—by immunohistochemistry or polymerase chain reaction?. Virchows Arch 466, 533–539 (2015). https://doi.org/10.1007/s00428-015-1741-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00428-015-1741-8