Abstract
We present an extremely rare case of a benign cystic ovarian teratoma with structures of male accessory sexual glands. The patient was a 30-year-old woman. A unilocular cystic tumor, measuring 5cm in the largest diameter, was found in her right ovary and was removed. The teratoma contained epidermis, skin appendages, respiratory and intestinal epithelia, cartilage, muscle, and nervous and connective tissue. In addition to these histologically mature tissues, there were nodules with prostatic acini, prostate duct-like structures strongly positive for prostate-specific antigen and acid prostatic phosphatase, structures resembling Cowper’s glands, and seminal vesicles surrounded by fibromuscular stroma. To our knowledge, this is the first case in the English literature describing seminal vesicles associated with prostatic tissue and bulbo-urethral glands in a mature ovarian teratoma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mature cystic teratomas of the ovary containing structures from all three germ layers are common neoplasms in this localization. Epidermis, cutaneous appendages, respiratory and intestinal epithelia, cartilage, muscle, and nervous and connective tissue are almost always detected in the tumors. Other tissues including pancreas, kidney, brain, and thymus are rarely found. Foci of urothelial epithelium in association with prostatic tissue have been described in teratomas of the ovary in a small number of reports [1, 2, 3, 6, 8, 9, 12].
The present case revealed male accessory sexual glands, such as prostatic and Cowper’s glands, and seminal vesicles occurring in a benign ovarian teratoma. To our knowledge, such a combination of male accessory sexual glands in an ovarian teratoma has not been previously reported.
Clinical history
A 30-year-old woman, nulligravida, nullipara, who had been treated for Hashimoto thyreoiditis, presented with a 1-week history of pain in the lower abdomen. Ultrasound investigation disclosed a cyst of the right ovary approximately 4cm in diameter. An ovarectomy was performed by a laparoscopy, and the cystic lesion was removed. The post-operative course was uneventful.
Material and methods
The tumorous tissue was fixed in 4% formalin, routinely processed and stained with hematoxylin and eosin. Immunohistochemical studies were performed on formalin-fixed, paraffin-embedded sections using prostate-specific antigen (PSA; polyclonal; Glostrup) and prostatic alkaline phosphatase (polyclonal; Dakocytomation, Glostrup).
Results
On gross examination, the lesion measured 5 × 3.5 × 1.5cm, was multilocular, and contained oily material found in some cysts.
Histologically, the neoplasm contained the usual tissues of a mature cystic adult teratoma, including epidermis, skin appendages, respiratory and intestinal epithelia, cartilage, muscle, and nervous and connective tissue. In addition, one area in the fibromuscular wall of the teratoma revealed structures identical to prostatic glands, Cowper glands, and seminal vesicles (Fig. 1a,b). The prostatic glands were composed of simple ducts and acini lined by luminal cuboidal cells supported by a layer of basal cells and surrounded by a fibromuscular stroma (Fig. 1c). The Cowper glands were lined by cuboidal epithelial cells with very pale cytoplasm and basally located nuclei; these glands had the appearance of mucinous minor salivary glands embedded within a skeletal muscle (Fig. 1d). The seminal vesicles with highly complex mucosal folds were lined by the epithelium made up of columnar and basal cells, with occasional brown pigment in the cytoplasm of the columnar cells.
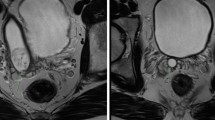
a Part of the teratoma with a structures identical to prostatic glands, Cowper glands, and seminal vesicles embedded in a fibromuscular tissue. b Complex folded seminal vesicles can be seen. The cyst in the lower portion was lined by intestinal epithelium. c Close-up view of the prostatic glands: Note simple ducts and acini lined by luminal cuboidal cells supported by a layer of basal cells and surrounded by a fibromuscular stroma. d Close-up view of the Cowper glands: glands lined by cuboidal epithelial cells with very pale cytoplasm and basally located nuclei. Note the resemblance to mucinous minor salivary glands embedded within a skeletal muscle. e The prostatic glands showed positivity for PSA
Immunohistochemically, the prostatic glands showed positivity for PSA and acid prostatic phosphatase (Fig. 1e). In contrast, the cells of the Cowper’s glands and seminal vesicles were negative for these markers.
Discussion
Prostatic gland, Cowper’s (bulbo-urethral) glands, and seminal vesicles are the main male accessory sexual glands. They form a functionally common group because they excrete liquid substances for slurring spermatozoons. Seminal vesicles in the male have no homologue in the female. Paraurethral (Skene’s) glands in the female are mesonephric derivates and represent the underdeveloped homologue of the prostatic glands. The Bartholin glands are the homologue of male bulbo-urethral glands (Cowper’s glands).
Prostatic tissue has rarely been described in the female genital tract [1–12]. Most reports documented the occurrence of prostatic tissue as a component of teratoma; however, ectopic prostatic tissue has also been found in the uterine cervix and vagina [5], including a patient with adrenogenital syndrome [4]. A unique case of benign prostatic tissue unassociated with a teratoma located at the ovarian hilum and merging with hyperplastic mesonephric remnants, which demonstrated various forms of epithelial metaplasia, is also on record [10].
Our review of the literature revealed about 19 cases of prostatic tissue being a component of an ovarian teratoma [9]. In addition, some of these reports described the presence of urothelium, Cowper’s excretory ducts and glands, and a vascularized area with sinusoids surrounded by a fibromuscular wall of the cavernous type [3, 6, 7, 8, 9]. A case of prostatic adenocarcinoma in a mature cystic teratoma of the ovary has also been reported [3]. Our case seems to be the first report describing seminal vesicles in association with the foresaid male urogenital sinus structures in an ovarian mature teratoma. Interestingly, we have not found a single case report that would describe the occurrence of prostatic glands in the testicular teratoma in the literature.
Male accessory sexual glands derive from mesonephric ducts and urogenital sinus; the common embryogenital origin of these structures in men and in women seems to be a logical explanation for the development of the prostate tissue, Cowper’s glands, and seminal vesicles in ovarian teratomas.
References
Bertrand GM (1986) Unique finding of prostatic tissue in a benign cystic ovarian teratoma. Arch Pathol Lab Med 110:683–684
Brumback RA, Brown BS, di Sant’Agnese PA (1985) Unique finding of prostatic tissue in a benign cystic ovarian teratoma. Arch Pathol Lab Med 109:675–677
Halabi M, Oliva E, Mazal PR, Breitenecker G, Young RH (2002) Prostatic tissue in mature cystic teratomas of the ovary: a report of four cases, including one with features of prostatic adenocarcinoma, and cytogenetic studies. Int J Gynecol Pathol 21:261–267
Kim KR, Park KH, Kim JW, Cho KJ, Ro JY (2004) Transitional cell metaplasia and ectopic prostatic tissue in the uterine cervix and vagina in a patient with adrenogenital syndrome: report of a case suggesting a possible role of androgen in the histogenesis. Int J Gynecol Pathol 23:182–187
McCluggage WG, Ganesan R, Hirschowitz L, Miller K, Rollason TP (2006) Ectopic prostatic tissue in the uterine cervix and vagina: report of a series with a detailed immunohistochemical analysis. Am J Surg Pathol 30:209–215
McLachlin CM, Srigley JR (1992) Prostatic tissue in mature cystic teratomas of the ovary. Am J Surg Pathol 16:780–784
Melniker LA, Slavutin LJ (1980) Prostatic tissue in a benign cystic teratoma of the ovary. Diagn Gynecol Obstet 2:139–145
Nogales FF, Vergara E, Medina MT (1995) Prostate in ovarian mature cystic teratoma. Histopathology 26:373–375
Resta L, Marzullo A, Pellegrino M, Rizzi E, Piscitelli D (2004) Male urogenital sinus structures in mature cystic teratomas of the ovary. Report of two cases. Histopathology 45:303–305
Smith CE, Toplis PJ, Nogales FF (1999) Ovarian prostatic tissue originating from hilar mesonephric rests. Am J Surg Pathol 23:232–236
Uzoaru I, Nadimpalli V (1993) Prostate in ovarian teratoma. Am J Surg Pathol 17:531
Vadmal M, Steven I (1996) Prostatic tissue in cystic ovarian teratomas. Hum Pathol 27:428–429
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shelekhova, K.V., Hejda, V., Kazakov, D.V. et al. Mature cystic teratoma of the ovary with male accessory sexual glands including seminal vesicles, prostatic tissue, and bulbo-urethral glands: a case report. Virchows Arch 452, 109–111 (2008). https://doi.org/10.1007/s00428-007-0546-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00428-007-0546-9