Abstract
Proton pump inhibitors (PPIs) are potent blockers of gastric acid secretion, used by millions of patients suffering from gastric acid-related complaints. Although PPIs have an excellent safety profile, an increasing number of case reports describe patients with severe hypomagnesemia due to long-term PPI use. As there is no evidence of a renal Mg2+ leak, PPI-induced hypomagnesemia is hypothesized to result from intestinal malabsorption of Mg2+. The aim of this study was to investigate the effect of PPIs on Mg2+ homeostasis in an in vivo mouse model. To this end, C57BL/6J mice were treated with omeprazole, under normal and low dietary Mg2+ availability. Omeprazole did not induce changes in serum Mg2+ levels (1.48 ± 0.05 and 1.54 ± 0.05 mmol/L in omeprazole-treated and control mice, respectively), urinary Mg2+ excretion (35 ± 3 μmol/24 h and 30 ± 4 μmol/24 h in omeprazole-treated and control mice, respectively), or fecal Mg2+ excretion (84 ± 4 μmol/24 h and 76 ± 4 μmol/24 h in omeprazole-treated and control mice, respectively) under any of the tested experimental conditions. However, omeprazole treatment did increase the mRNA expression level of the transient receptor potential melastatin 6 (TRPM6), the predominant intestinal Mg2+ channel, in the colon (167 ± 15 and 100 ± 7 % in omeprazole-treated and control mice, respectively, P < 0.05). In addition, the expression of the colonic H+,K+-ATPase (cHK-α), a homolog of the gastric H+,K+-ATPase that is the primary target of omeprazole, was also significantly increased (354 ± 43 and 100 ± 24 % in omeprazole-treated and control mice, respectively, P < 0.05). The expression levels of other magnesiotropic genes remained unchanged. Based on these findings, we hypothesize that omeprazole inhibits cHK-α activity, resulting in reduced extrusion of protons into the large intestine. Since TRPM6-mediated Mg2+ absorption is stimulated by extracellular protons, this would diminish the rate of intestinal Mg2+ absorption. The increase of TRPM6 expression in the colon may compensate for the reduced TRPM6 currents, thereby normalizing intestinal Mg2+ absorption during omeprazole treatment in C57BL/6J mice, explaining unchanged serum, urine, and fecal Mg2+ levels.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Proton pump inhibitors (PPIs) are indicated for gastric acid-related diseases like gastroesophageal reflux disease, Zollinger–Ellison syndrome, Barrett's esophagus, duodenal peptic ulcers, and gastritis [22]. All PPIs have a similar chemical structure and an identical mode of action. They are administered in the form of lipophilic, membrane-permeable, inactive pro-drugs [25]. PPIs are absorbed from the small intestine into the blood, after which they accumulate in the highly acidic canaliculi of the parietal cells of the stomach. Here, PPIs are protonated, which induces covalent binding between the PPI and specific cysteine residues of the gastric H+,K+-ATPase (gHK-α), resulting in potent inhibition of acid secretion [25]. Although PPIs are generally considered to have an excellent safety profile, over 65 cases of PPI-induced hypomagnesemia (PPIH) have been reported since 2006 [3, 6, 7, 9–13, 16–18, 21, 29]. In addition to these case reports, reduced serum Mg2+ levels associated with the use of PPIs were reported in a cohort of hospitalized patients [14]. A recently published study, based on reports submitted to the Adverse Event Reporting System of the US Food and Drug Administration, suggests that PPIH might concern several hundreds of patients since 2004 [36].
PPIH typically manifests after years of chronic PPI use, and patients present with symptoms common to severe Mg2+ depletion such as tetany, seizures, convulsions, and cardiac arrhythmia, often coinciding with secondary hypocalcemia. The causal link between the use of PPIs and the development of hypomagnesemia was shown in PPIH patients by a classical challenge–dechallenge–rechallenge protocol, leading to fast recovery from hypomagnesemia during dechallenge and fast reappearance of hypomagnesemia after rechallenge [3, 10, 29]. Intravenous Mg2+ loading tests indicate that PPIH patients are severely Mg2+ depleted, and determination of fractional Mg2+ excretion shows appropriate renal retention of Mg2+ [3, 6, 18, 29]. These findings implicate that intestinal malabsorption of Mg2+ plays a central role in the etiology of PPIH. This sets PPIH apart from many other forms of drug-induced hypomagnesemia which most frequently result from renal Mg2+ losses [19]. However, the exact molecular mechanisms underlying PPIH remain unknown.
Some authors speculate that PPIH might result from genetic variants in the epithelial Mg2+ channel transient receptor potential melastatin 6 (TRPM6) [3, 6, 18]. The vital role of TRPM6 in the maintenance of Mg2+ homeostasis has been well established [31]. The Mg2+ channel is expressed at the apical membrane of epithelial cells in the distal convoluted tubules of the kidney and at the luminal side of the gastrointestinal epithelium [1]. Recently, several magnesiotropic hormones including epidermal growth factor, estrogen, and insulin have been described to influence Mg2+ absorption via TRPM6 [15, 23, 38]. In addition to the hormonal regulation, it is known that the presence of extracellular protons enhances inward currents via TRPM6, meaning that Mg2+ influx via this channel is strongly dependent on the extracellular pH [20].
The primary target of omeprazole, gHK-α, has a homologue named the colonic H+,K+-ATPase (cHK-α), which extrudes protons into the lumen of the intestine in exchange for potassium ions [5]. In vitro studies using guinea pig colonic crypts or colon tissue in Ussing chambers indicate that PPIs do not only reduce the activity of the gastric H+,K+-ATPase (gHK-α), but also that of the colonic H+,K+-ATPase (cHK-α) [28, 39]. Based on these observations, we hypothesize that omeprazole inhibits cHK-α activity, resulting in a lower amount of protons being extruded into the large intestine, subsequently leading to a reduced rate of intestinal Mg2+ absorption via TRPM6.
The aim of our study was, therefore, to create a mouse model of PPIH to test our hypothesis that omeprazole reduces TRPM6-mediated colonic Mg2+ absorption. To this end, we investigated the effect of omeprazole treatment on Mg2+ homeostasis in vivo by means of serum, urine, and fecal Mg2+ measurements and by determination of mRNA expression patterns of TRPM6 and cHK-α in the intestine and kidney.
Methods
Animal studies
C57BL/6J mice (8 weeks old) were purchased from Charles River, the Netherlands. Animals were housed in a temperature- and light-controlled room with pelleted chow (SSNIFF Spezialdiäten GmbH, Germany) and drinking water available ad libitum. Omeprazole (Fagron, the Netherlands) was dispersed in a solution containing 0.5 % (w/v) methylcellulose and 0.2 % (w/v) NaHCO3 (pH 9.0). Mice received a daily dose of 20 mg omeprazole per kilogram body weight, which was administered via oral gavage. For urine and feces collection, animals were individually housed in metabolic cages for 24 h. Blood was sampled from the submandibular facial vein at the end of the stay in the metabolic cages, and sera were collected for Mg2+ measurements. All experiments were performed in compliance with the animal ethics board of Radboud University Nijmegen.
For the first experiment, animals were randomly divided into an omeprazole group (n = 10) and a control group (n = 10), receiving vehicle only. They were fed a standard chow with normal Mg2+ content (0.2 % w/w Mg2+, SSNIFF Spezialdiäten GmbH, Germany) during 28 days. A second experiment was performed, in which both groups of mice were fed a Mg2+-deficient diet (0.02 % w/w Mg2+, SSNIFF Spezialdiäten GmbH, Germany) for 22 days followed by a recovery period of 2 days in which the mice were reintroduced to a diet with normal Mg2+ content.
Tissue collection and pH measurements
At the end of each experiment, blood was collected and animals were sacrificed via cervical dislocation under isoflurane anesthesia. Kidneys, duodenum, and colon segments were extracted, cleaned, and snap frozen in liquid nitrogen. In addition, stomach pH was analyzed using diagnostic test strips (Merck, Germany).
Analytical procedures
Before analysis, fecal samples were homogenized and digested in 65 % nitric acid (Sigma-Aldrich, USA) for 2 h at 70 °C, followed by an overnight incubation at room temperature. Serum, urinary, and fecal Mg2+ concentrations were determined by a colorimetric xylidyl-II blue method (Cobas Roche Diagnostics, UK) on a Nanodrop 2000c spectrophotometer (Thermo Fisher Scientific, USA) at 600 nm wavelength and were verified using a commercial serum standard (Precinorm U, Roche, Switzerland).
Quantitative real-time PCR
Total RNA was extracted from tissues using TRIzol® reagent (Invitrogen, UK) according to the manufacturer's protocol. The obtained RNA was subjected to DNase treatment (Promega, USA) to prevent genomic DNA contamination. Subsequently, RNA was reverse transcribed with murine leukemia virus reverse transcriptase. The obtained cDNA was used to determine mRNA expression levels of various magnesiotropic genes and H+,K+-ATPases, as well as mRNA levels of glyceraldehyde 3-phosphate dehydrogenase (GAPDH) as an endogenous control. The mRNA expression levels were quantified by real-time PCR on a CFX69 real-time detection system (BioRad, USA) using SYBR Green (BioRad, USA). Primers (Biolegio, the Netherlands) were designed with Primer 3 software (Whitehead Institute for Biomedical Research, USA) and are listed in Table 1.
Statistics
Values are expressed as means ± SEM. Differences between single groups of omeprazole-treated mice and controls were tested using a two-tailed, unpaired Student's t test. Comparison of multiple groups was performed by a one-way ANOVA with a Bonferroni correction. Differences between groups were considered to be statistically significant when P < 0.05. Analysis of the datasets was performed using GraphPad Prism (Macintosh version, 4.51).
Results
Effect of omeprazole on serum Mg2+ levels as well as 24-h urinary and fecal Mg2+ excretion under normal and low dietary Mg2+ availability
To study the effect of omeprazole on serum Mg2+ levels as well as 24-h urinary and fecal excretion of Mg2+, mice were treated with 20 mg/kg body weight omeprazole (or vehicle) via oral gavage once a day. Serum Mg2+ levels, 24-h urinary Mg2+ excretion as well as 24-h fecal Mg2+ excretion were determined at the start of the experiment and after 28 days of treatment. There were no significant differences in body weight, food and water intake, diuresis, and fecal weight between the omeprazole-treated mice and vehicle-treated controls (P > 0.2 for all parameters) during their stay in the metabolic cages (Table 2). Serum Mg2+ levels (Fig. 1a) were unaltered in omeprazole-treated mice compared to the vehicle-treated controls (1.48 ± 0.05 and 1.54 ± 0.05 mmol/L in omeprazole-treated versus vehicle-treated mice, respectively, P > 0.2). The urinary excretion of Mg2+ (Fig. 1b) did not significantly differ between the omeprazole group and the control group (35 ± 3 μmol/24 h and 30 ± 4 μmol/24 h for omeprazole-treated and vehicle-treated mice, respectively, P > 0.2). In addition, fecal Mg2+ excretion (Fig. 1c) was not significantly different in omeprazole-treated mice compared to the vehicle-treated controls (76 ± 4 μmol/24 h and 84 ± 4 μmol/24 h in omeprazole-treated and control mice, respectively, P > 0.2)
To determine whether the effect of omeprazole on Mg2+ homeostasis is influenced by dietary Mg2+ availability, a subsequent experiment was performed in which mice were fed a Mg2+-deficient diet in addition to the treatment with omeprazole or vehicle. This diet induced a significant decline in serum Mg2+ values; however, no differences were observed between omeprazole- and vehicle-treated mice after 8 or 20 days of treatment (Fig. 2). After 22 days on the Mg2+-deficient diet, the animals were reintroduced to a diet with normal Mg2+ content, to investigate the recovery rate between the two groups of mice. Within 2 days, serum Mg2+ levels normalized to baseline values with no differences between omeprazole-treated animals and controls (1.42 ± 0.02 and 1.44 ± 0.02 mmol/L for omeprazole-treated and vehicle-treated controls, respectively, P > 0.2).
Effects of dietary Mg2+ restriction and omeprazole on serum Mg2+ in CB57BL/6J mice. Vehicle-treated controls (white bars) and omeprazole-treated mice (black bars) were fed a Mg2+-deficient diet (0.02 % w/w Mg2+) for 22 days and then switched to a normal diet (0.2 % w/w Mg2+) to monitor recovery. * # P < 0.05 compared to the corresponding group on day 0
Effect of omeprazole treatment on gastric pH
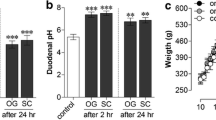
To confirm the effect of omeprazole treatment on gastric acid secretion in our mouse model, we measured the pH in the gastric lumen using pH indicator strips (Fig. 3). Four hours after administration of omeprazole, the intragastric pH was pH 6.7 ± 0.2 indicating that gastric acid production was effectively inhibited by omeprazole. Twenty-eight hours after the last dose of omeprazole was administered, the stomach pH remained significantly elevated with a pH 4.4 ± 0.4 in omeprazole-treated mice compared to a pH of 2.6 ± 0.3 in vehicle-treated mice (P < 0.05). These findings indicate that the omeprazole treatment ensured a continuous suppression of gastric acid secretion throughout the experiment.
Co-expression of TRPM6 and colonic H+,K+-ATPase in the colon
To confirm the co-localization of TRPM6 and cHK-α, their mRNA expression levels were determined in a murine gastrointestinal tissue panel (Fig. 4). TRPM6 mRNA expression was found predominantly in the cecum and throughout the colon, while expression levels in the duodenum were negligible. cHK-α mRNA expression was low in the duodenum and cecum whereas in the colon, expression increased from the proximal towards the distal end.
Gastrointestinal expression pattern of TRPM6 and cHK-α mRNA. mRNA expression levels of TRPM6 (black bars) and cHK-α (white bars) in the different segments of the gastrointestinal tract of CB57BL/6J mice as determined by real-time PCR. Expression levels are shown as a percentage of total gastrointestinal expression and were corrected for GAPDH expression. Data are presented as means ± SEM
Omeprazole treatment specifically enhances mRNA expression of TRPM6 and cHK-α in the colon
Next, we investigated whether omeprazole affected TRPM6 and cHK-α mRNA expression levels in the colon (Fig. 5a and b). Since the mRNA expression of both genes overlaps in the proximal as well as the distal colon, TRPM6 and cHK-α mRNA expression levels were analyzed in both colonic segments, to determine if they are affected by omeprazole treatment. The expression of TRPM6 in the proximal segment of the colon was not significantly increased (127 ± 17 and 100 ± 4 % in omeprazole-treated and control mice, respectively, P > 0.2). There was, however, a significant upregulation of cHK-α in omeprazole-treated mice compared to vehicle-treated controls (257 ± 55 and 100 ± 7 % in omeprazole-treated and control mice, respectively, P < 0.05).
Effects of omeprazole treatment on mRNA expression levels of various magnesiotropic genes and H+-K+-ATPases in the colon and kidney. Relative mRNA expression levels (corrected for GAPDH) of TRPM6 and cHK-α in vehicle-treated controls (white bars) and omeprazole-treated mice (black bars) in the proximal (a) and distal (b) colon, as well as in the kidney (c). Expression levels of various magnesiotropic genes and the gHK-α in the distal colon of vehicle-treated controls and omeprazole-treated mice (d). Data are presented as means ± SEM, *P < 0.05 compared to vehicle-treated controls
In the distal colon, the expression level of TRPM6 mRNA was increased ∼1.5 times in omeprazole-treated mice compared to the vehicle-treated controls (167 ± 15 and 100 ± 7 % for omeprazole-treated and vehicle-treated mice, respectively, P < 0.05). Similar to our findings in the proximal colon, cHK-α mRNA expression levels in the distal colon were ∼3.5 times higher in omeprazole-treated mice compared to controls (354 ± 43 and 100 ± 24 % for omeprazole-treated and vehicle-treated mice, respectively, P < 0.05).
In the kidney (Fig. 5c), TRPM6 mRNA expression was significantly lower in omeprazole-treated mice compared to the controls (89 ± 4 and 100 ± 1 % for omeprazole-treated and vehicle-treated mice, respectively, P < 0.05). The levels of cHK-α mRNA were unaltered by the omeprazole treatment (112 ± 22 and 100 ± 3 % for omeprazole-treated and vehicle-treated mice, respectively, P > 0.2).
The mRNA expression levels of magnesiotropic genes other than TRPM6 could function as important negative controls as they could demonstrate the specificity of the upregulation of TRPM6 and cHK-α in the colon in reaction to omeprazole treatment. Therefore, we determined the expression levels of the following well-known magnesiotropic genes in the distal colon of omeprazole- and vehicle-treated mice: TRPM7, epidermal growth factor (EGF), EGF receptor (EGFR), potassium voltage-gated channel subfamily A member 1 (Kv1.1), Cyclin M2 (CNNM2), and hepatocyte nuclear factor 1 homeobox B (HNF1B).
The mRNA expression level of TRPM7, the closest homologue of TRPM6 and therefore the most important negative control, was unaltered in the distal colon of omeprazole-treated mice compared to the expression in vehicle-treated controls (104 ± 7 and 100 ± 3 % for omeprazole-treated and vehicle-treated mice, respectively, P > 0.2). The expression levels of the other tested magnesiotropic genes were also not significantly altered by omeprazole treatment.
In addition to the magnesiotropic genes, we have also analyzed the expression levels of the gHK-α. There was a small but significant increase in the expression of gHK-α in omeprazole-treated mice versus vehicle-treated controls (148 ± 15 and 100 ± 2 % in omeprazole-treated and control mice, respectively, P < 0.05).
Discussion
This study demonstrates for the first time that omeprazole treatment enhances the colonic expression levels of both TRPM6 and cHK-α mRNA suggesting that omeprazole indeed influences intestinal Mg2+ absorption. However, prolonged exposure to omeprazole had no effect on either serum Mg2+ levels, urinary Mg2+ excretion, or fecal Mg2+ excretion in C57BL/6J mice under normal or low dietary Mg2+ conditions. Moreover, omeprazole did not affect the development of hypomagnesemia under dietary Mg2+ restriction, nor the recovery from hypomagnesemia under normal dietary Mg2+ conditions.
Under conditions of normal dietary Mg2+ availability, the majority of intestinal Mg2+ absorption takes place in the small intestine via a passive, paracellular pathway. When dietary Mg2+ concentrations are low, or when bodily needs are high, active transcellular transport via TRPM6 becomes more important [27]. By performing our experiments both under normal and low dietary Mg2+ availability, we aimed to distinguish between the effect of omeprazole on the paracellular and transcellular absorption pathways. Although there was no effect of omeprazole treatment on serum Mg2+ levels nor on urinary and fecal Mg2+ excretion, there was a significant increase in both TRPM6 and cHK-α mRNA levels in the distal colon of omeprazole-treated mice. The difference in the effect of omeprazole on TRPM6 mRNA expression in the proximal and distal colon is most likely the result of the lower baseline cHK-α expression in the proximal segment (as shown in Fig. 4); the net increase in cHK-α expression is therefore much lower in the proximal colon, consequently resulting in a less robust effect on TRPM6.
The mRNA expression levels of several other known magnesiotropic genes, including the TRPM6 homologue TRPM7, were not affected, indicating that the effect of omeprazole treatment on TRPM6 expression in the colon is highly specific.
In addition to the effect in the colon, omeprazole treatment also slightly decreased TRPM6 mRNA expression in the kidney; however, the renal expression of cHK-α remained unchanged. Importantly, the unaltered urinary Mg2+ excretion of the mice indicates that the final renal Mg2+ balance was not compromised by the slight decrease of renal TRPM6 expression.
The increased expression of cHK-α mRNA in the colon upon treatment with omeprazole was very distinct. We also found a small, but statistically significant, increase in gHK-α mRNA expression in the distal colon of omeprazole-treated mice compared to the vehicle-treated controls. The expression levels of gHK-α in the colon are, however, very low, so the functional relevance of this small increase is disputable. Previous studies have described an increase in mRNA expression level of the gHK-α in the stomach induced by omeprazole treatment [37]. Most likely, the increased mRNA levels of the H+,K+-ATPases in the colon represent an adaptation mechanism to restore acid secretion. There is clear evidence from in vivo models that omeprazole can indeed accumulate in the colonic epithelium, although this accumulation is not as strong as in the stomach [24, 26]. As described before, omeprazole is a lipophilic pro-drug which easily passes the plasma membrane. In the presence of protons, the pro-drug is converted into an active form, trapping it into the cell. The conversion of the PPI, which causes its accumulation in the cell, also enables the binding of the PPI to intracellular cystein residues of the gHK-α, thereby inhibiting the extrusion of protons [30]. The fact that omeprazole accumulates in the colon indicates that the colonic cells have a sufficiently low pH to allow for omeprazole activation, potentially leading to inhibition of cHK-α. The function and pharmacological sensitivity of the various HK-αs depends on the species, tissues, and systems in which they are studied [33, 35]. The inhibitory effect of omeprazole on cHK-α was shown in fractionized membranes of guinea pig distal colon, in which omeprazole was found to reduce cHK-α activity by 30 % [39]. Furthermore, studies in Ussing chambers indicated that omeprazole inhibits cHK-α activity in the colon [28]. Inhibition of cHK-α by omeprazole would lead to a reduction of proton secretion into the lumen of the colon. Importantly, it has been shown that extracellular protons enhance inward currents via TRPM6, indicating that Mg2+ influx via TRPM6 is strongly dependent on the extracellular pH [20]. We therefore hypothesized that the effect of omeprazole on intestinal Mg2+ absorption is the result of an indirect effect of omeprazole on TRPM6, elicited via a reduction of cHK-α-mediated proton secretion. This hypothesis is in line with findings from previous studies which show that fermentable substrates, such as carbohydrates, stimulate intestinal Mg2+ absorption [4]. The fermentation of these substrates by bacteria leads to an acidification of the cecum and colon, without influencing systemic acid/base homeostasis. Interestingly, increasing the amount of fermentable substrate in the food results in increased intestinal Mg2+ absorption, whereas the absorption of other minerals such as calcium, iron, and zinc remains unchanged. Several human studies have confirmed the enhancing effect of fermentable oligo- or polysaccharides on Mg2+ absorption [4]. These findings are in line with our hypothesis that changes in pH can influence Mg2+ absorption in the colon.
A tissue panel of the mouse intestinal tract shows abundant TRPM6 mRNA expression in the cecum as well as the colon, which is in line with earlier observations from our group [15]. cHK-α mRNA expression was predominantly found in the colon, where its expression increases towards the distal end, that is in accordance with the fact that active potassium absorption predominantly takes place in the distal part of the colon [34]. The co-expression of TRPM6 and cHK-α along the entire colon supports our hypothesis. The concurring upregulation of TRPM6 and cHK-α mRNA expression could represent a compensatory mechanism aiming to maintain sufficient Mg2+ absorption by counteracting the inhibitory effects of omeprazole on cHK-α-mediated proton secretion and TRPM6-mediated Mg2+ absorption. This would explain the lack of an effect of omeprazole on serum Mg2+ levels as well as urinary and fecal Mg2+ excretion in our mouse model.
Recently, a mathematical model simulating intestinal Mg2+ absorption has been described, aiming to explain PPIH. According to this model, PPI treatment reduces Mg2+ absorption, leading to a 5 % decrease of serum Mg2+ [2]. In a study with healthy volunteers, administration of omeprazole (40 mg) once a day for 7 days reduced Mg2+ absorption by 1 % [32]. Bai et al. showed that a 1 % reduction of Mg2+ absorption could lead to an 80 % depletion of Mg2+ stores over the course of 1 year. The minute changes described might go undetected in clinical practice or experimental conditions but could, over longer periods, result in PPIH. This is in line with the fact that most PPIH patients described so far are indeed long-term (>1 year) PPI users [7].
Several questions concerning the development of PPIH in human patients remain unanswered. The incidence of PPIH is still unknown, although there are indications that the case reports only represent the tip of the iceberg [36]. A simple explanation may be found in the dietary intake of Mg2+; as the changes in Mg2+ absorption due to omeprazole treatment are small, they are easily corrected by a higher intake of Mg2+, which could explain why certain patients develop PPIH whereas others do not [2]. The low incidence could, however, also indicate that patients will only develop PPIH if they are in some way predisposed. For example, a recent study shows a strong correlation between PPIH and the combined use of PPIs and diuretics [8]. Another possibility, outlined in case reports, is that the presence of mutations or single-nucleotide polymorphisms (SNPs) in magnesiotropic genes such as TRPM6 contributes to the development PPIH. In a single case of PPIH, TRPM6 was sequenced, but no abnormalities were found in exonic regions of TRPM6 [12]. Another study excluded the presence of mutations in SLC12A3, which is one of the genes involved in Gitelman syndrome [18]. However, these individual cases do not exclude the involvement of SNPs in magnesiotropic genes, and larger studies are needed in order to confirm or exclude the involvement of predisposing factors in the development of PPIH.
In conclusion, this study provides new insights in the effect of omeprazole on Mg2+ homeostasis in an in vivo setting, which could potentially shed light on the molecular aspects of the etiology of PPIH. A significant and specific effect of omeprazole treatment on TRPM6 and cHK-α mRNA expression levels in the distal colon was found, while the serum Mg2+ levels, 24-h urinary Mg2+ excretion as well as 24-h fecal Mg2+ excretion were not affected. The stimulation of mRNA levels was distinct in the colon, whereas in the kidney, little or no changes occurred. This is in line with the clinical findings indicating that PPIH results from reduced intestinal Mg2+ absorption and not from renal Mg2+ wasting. Further research, both on a clinical as well as a fundamental level, is needed to fully understand and prevent PPIH in the near future.
References
Alexander RT, Hoenderop JG, Bindels RJ (2008) Molecular determinants of magnesium homeostasis: insights from human disease. J Am Soc Nephrol 19:1451–1458
Bai JP, Hausman E, Lionberger R, Zhang X (2012) Modeling and simulation of the effect of proton pump inhibitors on magnesium homeostasis. 1. Oral absorption of magnesium. Mol Pharm 9:3495–3505
Broeren MA, Geerdink EA, Vader HL, van den Wall Bake AW (2009) Hypomagnesemia induced by several proton-pump inhibitors. Ann Intern Med 151:755–756
Coudray C, Demigne C, Rayssiguier Y (2003) Effects of dietary fibers on magnesium absorption in animals and humans. J Nutr 133:1–4
Cougnon M, Planelles G, Crowson MS, Shull GE, Rossier BC, Jaisser F (1996) The rat distal colon P-ATPase alpha subunit encodes a ouabain-sensitive H+, K+-ATPase. J Biol Chem 271:7277–7280
Cundy T, Dissanayake A (2008) Severe hypomagnesaemia in long-term users of proton-pump inhibitors. Clin Endocrinol 69:338–341
Cundy T, Mackay J (2011) Proton pump inhibitors and severe hypomagnesaemia. Curr Opin Gastroenterol 27:180–185
Danziger J, William JH, Scott DJ, Lee J, Lehman LW, Mark RG, Howell MD, Celi LA, Mukamal KJ (2013) Proton-pump inhibitor use is associated with low serum magnesium concentrations. Kidney Int 83:692–699
Doornebal J, Bijlsma R, Brouwer RM (2009) An unknown but potentially serious side effect of proton pump inhibitors: hypomagnesaemia. Ned Tijdschr Geneeskd 153:A711
Epstein M, McGrath S, Law F (2006) Proton-pump inhibitors and hypomagnesemic hypoparathyroidism. N Engl J Med 355:1834–1836
Fernandez-Fernandez FJ, Sesma P, Cainzos-Romero T, Ferreira-Gonzalez L (2010) Intermittent use of pantoprazole and famotidine in severe hypomagnesaemia due to omeprazole. Neth J Med 68:329–330
Fernandez-Fernandez FJ, Sesma P, Cainzos-Romero T, Ferreira L (2011) Hypomagnesemia related to the use of omeprazole with negative result for mutation in the TRPM6 gene. Med Clin (Barc) 137:188–189
Furlanetto TW, Faulhaber GA (2011) Hypomagnesemia and proton pump inhibitors: below the tip of the iceberg. Arch Intern Med 171:1391–1392
Gau JT, Yang YX, Chen R, Kao TC (2012) Uses of proton pump inhibitors and hypomagnesemia. Pharmacoepidemiol Drug Saf. doi:10.1002/pds.3224, Article first published online: 15 FEB 2012
Groenestege WM, Hoenderop JG, van den Heuvel L, Knoers N, Bindels RJ (2006) The epithelial Mg2+ channel transient receptor potential melastatin 6 is regulated by dietary Mg2+ content and estrogens. J Am Soc Nephrol 17:1035–1043
Hmu C, Moulik P, Macleod A (2009) Severe hypomagnesaemia due to lansoprazole. BMJ Case Rep (in press), published online 17 December 2009
Hoorn EJ, van der Hoek J, de Man RA, Kuipers EJ, Bolwerk C, Zietse R (2010) A case series of proton pump inhibitor-induced hypomagnesemia. Am J Kidney Dis 56:112–116
Kuipers MT, Thang HD, Arntzenius AB (2009) Hypomagnesaemia due to use of proton pump inhibitors—a review. Neth J Med 67:169–172
Lameris AL, Monnens LA, Bindels RJ, Hoenderop JG (2012) Drug-induced alterations in Mg2+ homoeostasis. Clin Sci (Lond) 123:1–14
Li M, Jiang J, Yue L (2006) Functional characterization of homo- and heteromeric channel kinases TRPM6 and TRPM7. J Gen Physiol 127:525–537
Mackay JD, Bladon PT (2010) Hypomagnesaemia due to proton-pump inhibitor therapy: a clinical case series. Qjm-an Int J Med 103:387–395
McKeage K, Blick SK, Croxtall JD, Lyseng-Williamson KA, Keating GM (2008) Esomeprazole: a review of its use in the management of gastric acid-related diseases in adults. Drugs 68:1571–1607
Nair AV, Hocher B, Verkaart S, van Zeeland F, Pfab T, Slowinski T, Chen YP, Schlingmann KP, Schaller A, Gallati S, Bindels RJ, Konrad M, Hoenderop JG (2012) Loss of insulin-induced activation of TRPM6 magnesium channels results in impaired glucose tolerance during pregnancy. Proc Natl Acad Sci U S A 109:11324–11329
Nakamura M, Matsui H, Serizawa H, Tsuchimoto K (2007) Lansoprazole novel effector sites revealed by autoradiography: relation to Helicobacter pylori, colon, esophagus and others. J Clin Biochem Nutr 41:154–159
Olbe L, Carlsson E, Lindberg P (2003) A proton-pump inhibitor expedition: the case histories of omeprazole and esomeprazole. Nat Rev Drug Discov 2:132–139
Phillips DH, Hewer A, Osborne MR (1992) Interaction of omeprazole with DNA in rat tissues. Mutagenesis 7:277–283
Quamme GA (2008) Recent developments in intestinal magnesium absorption. Curr Opin Gastroenterol 24:230–235
Rechkemmer G, Frizzell RA, Halm DR (1996) Active potassium transport across guinea-pig distal colon: action of secretagogues. J Physiol-Lond 493:485–502
Regolisti G, Cabassi A, Parenti E, Maggiore U, Fiaccadori E (2010) Severe hypomagnesemia during long-term treatment with a proton pump inhibitor. Am J Kidney Dis 56:168–174
Sachs G, Shin JM, Vagin O, Lambrecht N, Yakubov I, Munson K (2007) The gastric H, K ATPase as a drug target: past, present, and future. J Clin Gastroenterol 41(Suppl 2):S226–S242
Schlingmann KP, Waldegger S, Konrad M, Chubanov V, Gudermann T (2007) TRPM6 and TRPM7—gatekeepers of human magnesium metabolism. Biochim Biophys Acta-Mol Basis of Dis 1772:813–821
Serfaty-Lacrosniere C, Wood RJ, Voytko D, Saltzman JR, Pedrosa M, Sepe TE, Russell RR (1995) Hypochlorhydria from short-term omeprazole treatment does not inhibit intestinal absorption of calcium, phosphorus, magnesium or zinc from food in humans. J Am Coll Nutr 14:364–368
Shao J, Gumz ML, Cain BD, Xia SL, Shull GE, van Driel IR, Wingo CS (2010) Pharmacological profiles of the murine gastric and colonic H, K-ATPases. Biochim Biophys Acta 1800:906–911
Sorensen MV, Matos JE, Praetorius HA, Leipziger J (2010) Colonic potassium handling. Pflugers Arch 459:645–656
Swarts HG, Koenderink JB, Willems PH, De Pont JJ (2007) The human non-gastric H, K-ATPase has a different cation specificity than the rat enzyme. Biochim Biophys Acta 1768:580–589
Tamura T, Sakaeda T, Kadoyama K, Okuno Y (2012) Omeprazole- and esomeprazole-associated hypomagnesaemia: data mining of the public version of the FDA Adverse Event Reporting System. Int J Med Sci 9:322–326
Tari A, Wu V, Sumii M, Sachs G, Walsh JH (1991) Regulation of rat gastric H+/K+-ATPase alpha-subunit messenger-RNA by omeprazole. Biochim Biophys Acta 1129:49–56
Thebault S, Alexander RT, Tiel Groenestege WM, Hoenderop JG, Bindels RJ (2009) EGF increases TRPM6 activity and surface expression. J Am Soc Nephrol 20:78–85
Watanabe T, Suzuki T, Suzuki Y (1990) Ouabain-sensitive K+-ATPase in epithelial-cells from guinea-pig distal colon. Am J Physiol 258:G506–G511
Acknowledgments
We kindly thank Henk Arnts and Jeroen Mooren for technical assistance and Dr. Joost Drenth for critical reading of the manuscript. This study was supported by the Netherlands Organization for Scientific Research [TOP ZonMw 91208026, NWO-ALW 818.02.001], a EURYI award from the European Science Foundation and the Dutch Kidney Foundation [C08.2252] and EURenOmics funding from the European Union seventh Framework Programme (FP7/2007-2013, agreement n° 305608). Mark Hess was supported by a grant of the Institute for Genetic and Metabolic Disease (IGMD) of the Radboud University Nijmegen Medical Centre.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lameris, A.L.L., Hess, M.W., van Kruijsbergen, I. et al. Omeprazole enhances the colonic expression of the Mg2+ transporter TRPM6. Pflugers Arch - Eur J Physiol 465, 1613–1620 (2013). https://doi.org/10.1007/s00424-013-1306-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00424-013-1306-0