Abstract
Introduction
Hepatocellular carcinoma (HCC) is a tumor of increasing incidence and high mortality worldwide. Diagnosis of HCC is often difficult, especially at early stages of disease. Additionally, current treatment options are limited. HCC usually develops in an environment of chronic liver disease. The immune system has an important role in shaping this environment, especially in chronic viral hepatitis, the leading cause of HCC. However, the immune system also plays a role in natural immunity against HCC although this is apparently not sufficient to control the majority of tumors. This failure in tumor control is due to multiple immunomodulatory mechanisms employed by HCC to subvert the immune system.
Summary
In this review, we will summarize the current knowledge about the role of the immune system in hepatocarcinogenesis. Additionally, we will describe the mechanisms used by the immune system to control established lesions and the reasons why these immune responses apparently fail so often. Finally, possible implications for the design of novel immunotherapeutic strategies will be discussed.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hepatocellular carcinoma (HCC) is a malignant neoplasm of hepatocytes. It is a frequently occurring tumor, ranking fifth in worldwide prevalence and third in mortality [1, 2]. HCC is a worldwide health problem, but it is especially prevalent in South-East Asia and sub-Saharan Africa. Globally, the incidence of HCC is increasing. This is especially due to a rise in the incidence of infections with the hepatitis C virus (HCV) [3]. Chronic infections with HCV and the hepatitis B virus (HBV) induce a chronic inflammation which can lead to liver fibrosis and subsequently cirrhosis, i.e., a replacement of liver tissue by connective tissue and regenerative nodules. Of note, chronic hepatic inflammation and liver cirrhosis can also be caused by several other factors such as alcohol abuse or hereditary liver diseases [4]. This inflamed and cirrhotic environment can ultimately give rise to HCC lesions.
The diagnosis of HCC is particularly difficult since it usually remains clinically asymptomatic until late stages of disease. However, even at early stages, therapeutic options for HCC are limited [5, 6]. Treatment options include liver transplantation, partial liver resection, or less invasive procedures such as radio-frequency thermal ablation (RFTA) and trans-arterial chemo-embolization [6]. Several new molecularly targeted therapies are currently under investigation. So far, sorafenib, a multi-kinase inhibitor, has been approved for treatment of patients with advanced HCC but has only shown modest clinical benefits [7]. Thus, there is an urgent need for new therapeutic options for HCC to treat end-stage patients or to limit the rate of recurrence of HCC after liver transplantation or liver resection.
Immunotherapy is a relatively new approach to tumor therapy. The aim of immunotherapy is to boost the immune system in order to destroy pathogens or malignantly transformed cells [8, 9]. For the development of such a complex therapeutic regimen, a detailed understanding of the natural role of the immune system in the development and control of HCC lesions is required.
The role of the immune system in hepatocarcinogenesis
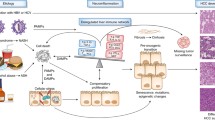
Tumors develop from single cells that accumulate mutations over time. These mutations alter the expression and function of genes responsible for cellular proliferation among others. This process ultimately leads to cells with uncontrolled proliferative and metastatic potential [10]. The exact molecular nature of these changes in HCC has been reviewed elsewhere and is not in the scope of this review [11, 12]. In brief, it could be demonstrated that HCC lesions accumulated diverse genomic alterations over time, whose number correlated with the pathological appearance of the lesions [13]. Especially signaling pathways such as Hedgehog and Wnt/β-catenin pathways were altered during hepatocarcinogenesis [14, 15]. Some of these changes can also be induced by chronic viral hepatitis, the leading cause for HCC [16]. For example, chronic HCV infection induces changes at the level of lipid metabolism and gene expression in the liver, whereas the HB antigen derived from HBV is believed to be capable of altering the transcription of several cellular genes which might also contribute to HCC development [17, 18]. Apart from these direct changes, chronic viral hepatitis also induces a chronic inflammation of the liver. Indeed, in the HBV transgenic mouse model, it could be shown that this chronic inflammation alone, i.e., in the absence of a productive viral infection, was sufficient to induce hepatocarcinogenesis [19]. Inflammation is associated with an abundance of different cytokines and growth factors in order to repair the tissue by cellular proliferation. However, in chronic inflammation, this can lead to permanently increased cellular turnover and finally the development of various malignancies [20]. This finding also elucidates why different causes of chronic hepatitis ultimately give rise to HCC. In HCC, especially cytokines of the lymphotoxin (LT) family have been associated with tumor development [21]. LTs are produced by a variety of lymphocytes such as T cells or natural killer (NK) cells, thereby demonstrating that the adaptive as well as the innate immune response are involved in the development of HCC. Interestingly, a recent study was able to demonstrate that the rate of DNA double strand breaks is increased in a mouse model of chronic hepatitis [22]. This directly contributes to mutagenesis and thus carcinogenesis. In addition, Toll-like receptors (TLRs) have been suggested to play a role in the development of HCC [23]. TLRs are pattern-recognition receptors that normally recognize conserved danger signals found on pathogens or also on necrotic cells, so called pathogen-associated molecular patterns. They are capable of inducing inflammatory processes, again supporting a role for chronic inflammation in hepatocarcinogenesis [24]. Indeed, the activation of TLR9 by unmethylated CpG DNA induced the proliferation as well as the expression of several anti-apoptotic proteins in hepatoma cells [25].
A direct role in HCC progression has also been shown for other cells of the immune system. For example, the detection of intratumoral neutrophils has been shown to predict a reduced recurrence-free survival time of HCC patients after liver resection [26, 27]. Of note, neutrophils the tumor edge induced angiogenesis and thus directly enhanced tumor growth [28]. This observation becomes especially intriguing in light of the finding that neutrophils can be recruited by interleukin-17 (IL-17) [29]. IL-17 is produced by T cells, termed TC17 or TH17, in the CD8+ or CD4+ T cell compartment, respectively. Indeed, IL-17 producing cells have been found to be enriched in HCC lesions and to correlate negatively with overall survival of HCC patients after liver resection [30]. Furthermore, TC17 and TH17 cells were also found to be enriched in the peritumoral stroma, where their numbers correlated with those of tumor-associated monocytes (TAMs) that have been shown to readily induce expansion of IL-17 producing cells [31, 32].
This data supports a model in which the immune system is creating an environment of increased cellular turnover which prone to mutagenesis and thus ultimately the development of neoplastic lesions. These data also support the concept that tumors of a certain size gain the ability to manipulate immune cells for their own benefit.
Immune responses against HCC
In HCC, the immune system certainly can induce hepatocarcinogenesis. However, several lines of evidence also suggest a protective role, e.g., by controlling tumor growth. Indeed, this assumption is based on several findings. First, HCC patients with an intratumoral accumulation of lymphocytes had a superior 5-year survival rate and a prolonged recurrence-free survival after liver resection [33, 34]. A certain level of protection was especially conferred by cytotoxic CD8+ T cells [35]. Of note, these tumor infiltrating lymphocytes (TILs) were associated with an inflammatory microenvironment that was a predictor of overall patient survival, indicating a protective role of TILs in HCC [36, 37]. Furthermore, a strong CD8+ T cell response against several tumor-associated antigens (TAAs) was found to coincide with improved recurrence-free survival after liver resection [38]. The important role of CD8+ T cells in HCC control is further supported by a study in mice. Here, interferon γ (IFNγ) produced by CD8+ TILs could be shown to be one effector mechanism for apoptosis of hepatoma cells [39].
Of note, the antigen specificities of TILs in HCC patients are currently still under investigation. To date, several TAAs of HCC have been identified. This has been reviewed recently by Breous and Thimme [8]. Briefly, several shared tumor-specific antigens could also be identified as antigens targeted by CD8+ T cells in HCC, e.g., human telomerase-reverse transcriptase (hTERT) or NY-ESO-1. Expression of these antigens has been reported for other malignancies as well. They comprise genes required for sustained proliferation such as hTERT. Other antigens are expressed specifically in HCC and are also recognized by cells of the immune system, e.g., α-fetoprotein (AFP) or Glypican-3. The latter two antigens belong to the family of oncofetal antigens. Oncofetal antigens are expressed during ontogenesis but not in the adult. However, re-expression of such antigens is frequently observed in tumors. The exact reasons for the specific reexpression of these antigens in HCC are still not completely clear. Further research is also required to determine the frequency, immunodominance and strength of the immune responses induced against different TAAs.
Next to HCC-specific cytotoxic T cells, other cell types have also been implicated in a successful immune response against HCC. For example, NK cells play an important role in anti-tumor immune responses, e.g., by direct lysis of malignant cells [40]. Indeed, in HCC patients an increased preoperative NK cell activity correlated with prolonged recurrence-free survival [41]. Furthermore, a decreased functionality of NK cells was shown to predict the occurrence of HCC [42]. Other studies also showed that the stimulation of natural killer T cells (NKT cells) leads to an activation of NK cells and clearance of hepatoma cells in mice [43].
The role of B cells in HCC control is unclear thus far. Auto-antibodies against several antigens have been described in mouse models of HCC as well as in HCC patients [44, 45]. Additional studies showed that monoclonal antibodies against Glypican-3 were able to induce antibody-dependent cellular cytotoxicity (ADCC) and thus lysis of human hepatoma cells in vitro and in mice [46]. However, the importance of ADCC and antibodies in general in the natural immune response against HCC has not been investigated so far.
Factors contributing to a successful immune response against HCC are summarized in Fig. 1.
Components of a successful immune response against HCC. Macrophages (M θ ), or other APCs such as DCs, take up material from necrotic tumor cells. Next, they become activated and present epitopes derived from TAAs on their respective MHC class I and class II molecules. Subsequently tumor-specific CD4+ helper T cells (T H ) are activated and support the activation of CD8+ cytotoxic T cells (T C ). Activated TC are able to lyse tumor cells that present the respective epitope on their MHC class I molecules. NK cells can lyse tumor cells directly or upon encounter of antibodies specific for antigens on the surface of tumor cells. The latter process is termed antibody-dependent cellular cytotoxicity (ADCC). Antibodies specific for TAAs are produced by B cells. Cytokines secreted by NKT cells and TH modulate the activity of TC and NK cells as well as the class switch of B cells
Mechanisms of failure of immune responses against HCC
In most patients, HCC-specific immune responses fail to control the tumor. This failure is partly due to the fact that HCC evades the immune response. The growing tumor is exposed to various effector mechanisms by which especially cytotoxic CD8+ T cells and NK cells lyse tumor cells [47, 48]. Thus, tumor cells that have acquired mutations allowing them to escape are selected by the pressure exerted by the immune system. This selection of tumor cells that are able to subvert the anti-tumor immune response is termed cancer immunoediting [49]. Indeed, HCC lesions were frequently found to have lost expression of Fas (CD95) and the IFNγ receptor. Both are important effector mechanisms usually engaged by cytotoxic cells of the immune system [50, 51].
On the other hand, a dysfunctionality of tumor-specific CD8+ T cells in HCC patients has also been reported. These cells were found to express inhibitory receptors such as programmed death-1 (PD-1). Additionally, they displayed downregulated costimulatory molecules such as CD28 or components of the T cell receptor complex, e.g., CD3ζ [52–54]. Accordingly, these cells were functionally impaired and prone to apoptosis. A recent study could also show that this impaired CD8+ T cell phenotype predicted an earlier recurrence of HCC after liver resection [55]. This supports the hypothesis that the failure of the immune response to HCC is mainly a failure of tumor-specific CD8+ T cells.
There are probably several reasons for this functional impairment. First, PD-1 on tumor-specific CD8+ T cells is engaged by its ligand programmed death-ligand 1 (PD-L1). PD-L1 is expressed on tumor cells and intratumoral Kupffer cells [56]. Second, DCs were described to have a distinct phenotype in HCC [57]. These cells were found to secrete less IL-12 than DCs from controls. IL-12 is required for proper activation and differentiation of T cells. Thus, this particular phenotype of DCs might lead to an improper activation of CD8+ T cells and thus help to explain their dysfunctional phenotype. Third, regulatory T cells (Treg) that are highly capable of suppressing CD8+ T cells were readily detectable in HCC. Indeed, the fraction of Treg among TILs correlated negatively with clinical outcome [35]. In addition, an increase in the number of Treg could be shown for HCC patients in the blood as well as in the liver [58, 59]. These immunosuppressive Treg were also found to directly infiltrate HCC lesions [60]. Indeed, a direct functional impairment of CD8+ T cell function by increased Treg numbers could be demonstrated for HCC patients [61]. Of note, an increase in Treg numbers was also shown to coincide with progressing hepatocarcinogenesis, i.e., the more malignant the tumor, the higher the Treg count observed [62]. Further studies revealed that Treg are induced by supernatants derived from HCC, specifically by factors secreted by TAMs [63, 64]. Thus, HCC actively recruits Treg in order to keep CD8+ T cell responses suppressed. Fourth, another immunosuppressive cell type termed myeloid-derived suppressor cells (MDSCs) has recently gained increasing interest in the field of tumor immunology. MDSCs are a mixture of diverse immature cell types of myeloid origin that are able to dampen immune responses. In HCC, MDSCs were found to infiltrate the tumor and to induce the Treg phenotype in naïve T cells [65].
As described, NK cells are also potent effectors against tumor cells. Interestingly, NK cell number and function were found to be generally reduced in HCC patients, which might point to sequestration or deletion of these cells [66, 67]. The reasons for this failure of NK cell responses in HCC patients are still under investigation. There is evidence that hepatoma cells can secrete a soluble form of MHC class I-related chain A (MICA) [68]. MICA is a ligand for the activating NK cell receptor NKG2D and a soluble form of this ligand might thus prevent proper NK cell activation at the tumor site. Other studies also revealed a role for MDSCs in suppression of NK cell function in HCC [69]. Thus, the functional impairment of immune cells is not restricted to CD8+ T cells but also comprises other cytotoxic cell types.
The role of CD4+ helper T cells in HCC remains elusive. A recent study in our group found that there is a pronounced lack of helper T cells specific for AFP in blood, liver, and tumors of HCC patients especially when compared to CD8+ T cell responses against the same antigen [70, 71]. Another recent study proposed that AFP specific CD4+ and CD8+ T cells expanded at different stages of disease [72]. However, the exact mechanism of this apparent insufficiency of helper T cells in HCC is still elusive and further research, especially for other TAAs, is still urgently required.
The mechanisms leading to an impairment of the immune response against HCC are summarized in Table 1. Taken together, many pathways have been shown to contribute to the apparent failure of the immune system in HCC. Further research is needed to better understand this failure and eventually be able to overcome it.
Perspectives for treatment
There is urgent need for additional therapeutic options for HCC. Liver transplantation is a curative option, but due to the shortage of donor organs, it is only applicable for a few patients. Instead, surgical removal of the tumor by liver resection is a frequently applied treatment. RFTA is another potentially curative treatment but only suitable for early stages of disease [6]. However, the frequent occurrence of recurrences limits the overall success rate of these approaches [73]. As shown earlier, the rate of recurrence is largely influenced by the lymphocyte infiltrate found within the tumor. Presumably, tumor-specific CD8+ T cells and NK cells are able to control the tumor cells remaining after resection and thus limit the rate of recurrence. A therapeutic approach that effectively enhances this tumor-specific immune response might thus be a very promising adjuvant approach to conventional surgical therapy. Indeed, the efficacy of autologous lymphocytes activated in vitro using anti-CD3 antibodies and recombinant human IL-2 in lowering recurrence rates and improving post-surgical survival could be demonstrated [74]. Clearly, this is one of the current aims of immunotherapy, although further research is still required.
Interestingly, recent studies also showed a role for some currently available therapeutic approaches in boosting the natural immune response against HCC. For example, it could be shown that RFTA increases the costimulatory capacity of antigen-presenting cells (APCs) and boosts NK cell activity [75, 76]. This is probably mediated by the release of tumor material by necrosis and thus in a pro-inflammatory context. This observation leads to the hypothesis that RFTA or similar ablative therapies could be applied prior to partial liver resection in an attempt to boost the immune response and thus limit the rate of recurrence after surgery. By this approach, the apparent power of the immune system could be used without the laborious and costly requirements of adoptive transfer of in vitro-activated cells, as described above. However, due to the novelty of some of these observations, this procedure has not been tested prospectively in the clinical setting.
With a better understanding of the underlying mechanisms of failure of the natural tumor-specific immune response, it might even become possible to apply immunotherapy as a first line of treatment [9]. However, thus far only a few trials testing immunotherapy of HCC have been published. Nevertheless, in mice, the general feasibility of such an approach could already be demonstrated using a DNA-based vaccine containing AFP [77]. In this trial, a partial tumor regression and improved survival coincided with the induction of AFP-specific immune responses. Furthermore, a phase I/II clinical trial using DCs pulsed with AFP peptides showed that immune responses to AFP were also inducible in humans although no clinical response was seen in this study [78]. However, a recent phase II clinical trial was able to show that autologous DCs primed with tumor lysate are well tolerated by HCC patients [79]. Additionally, this immunotherapeutic approach showed some anti-tumor effect as evidenced by stabilization of disease and a drop in serum AFP levels in some HCC patients.
For other malignancies, especially melanoma, immunotherapy is already several steps further into development. Importantly, a vaccine containing recombinant human NY-ESO-1 protein mixed with ISCOMATRIX adjuvant was able to achieve stabilization of disease in some patients [80]. As mentioned above, the immunogenicity of this antigen was also proven for HCC, raising hopes that vaccines developed for other malignancies might also be applicable for HCC patients. Other approaches in HCC immunotherapy focused on the immunomodulatory role of NKT cells in order to orchestrate a comprehensive immune response involving multiple effector arms [81, 82]. However, there is little data so far and this approach thus requires further investigation.
In conclusion, immunotherapy holds promise to become a useful adjuvant treatment to support current surgical regimens in the near future. The possible use of immunotherapy as a stand-alone therapy, however, still requires and warrants further investigation.
Summary
HCC is a malignancy of increasing importance due to a rising incidence accompanied by limited treatment options. The immune system plays a pivotal role in the development of HCC as chronic inflammation is one of the most important causes of HCC. Limiting such inflammations might thus be a promising approach to reduce the occurrence of this disease. However, once the tumor is established, the immune system is usually able to confer a certain level of protection against the tumor, at least against recurrence after surgical removal. Enhancing this natural anti-tumor immunity and breaking the immunosuppressive barriers established by HCC are central aims of immunotherapy and might in the future be of benefit for patients’ survival.
References
Calle EE, Rodriguez C, Walker-Thurmond K, Thun MJ (2003) Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U.S. adults. N Engl J Med 348(17):1625–1638. doi:10.1056/NEJMoa021423
Parkin DM (2001) Global cancer statistics in the year 2000. Lancet Oncol 2(9):533–543. doi:10.1016/S1470-2045(01)00486-7
El-Serag HB, Rudolph KL (2007) Hepatocellular carcinoma: epidemiology and molecular carcinogenesis. Gastroenterology 132(7):2557–2576. doi:10.1053/j.gastro.2007.04.061
Fattovich G, Stroffolini T, Zagni I, Donato F (2004) Hepatocellular carcinoma in cirrhosis: incidence and risk factors. Gastroenterology 127(5 Suppl 1):S35–S50
Blum HE, Spangenberg HC (2007) Hepatocellular carcinoma: an update. Arch Iran Med 10(3):361–371
El-Serag HB, Marrero JA, Rudolph L, Reddy KR (2008) Diagnosis and treatment of hepatocellular carcinoma. Gastroenterology 134(6):1752–1763. doi:10.1053/j.gastro.2008.02.090
Spangenberg HC, Thimme R, Blum HE (2009) Targeted therapy for hepatocellular carcinoma. Nat Rev Gastroenterol Hepatol 6(7):423–432. doi:10.1038/nrgastro.2009.86
Breous E, Thimme R (2010) Potential of immunotherapy for hepatocellular carcinoma. J Hepatol. doi:10.1016/j.jhep.2010.10.013
Couzin-Frankel J (2010) Immune therapy steps up the attack. Science 330(6003):440–443. doi:10.1126/science.330.6003.440
Hanahan D, Weinberg RA (2000) The hallmarks of cancer. Cell 100(1):57–70
Aravalli RN, Steer CJ, Cressman EN (2008) Molecular mechanisms of hepatocellular carcinoma. Hepatology 48(6):2047–2063. doi:10.1002/hep.22580
Minguez B, Tovar V, Chiang D, Villanueva A, Llovet JM (2009) Pathogenesis of hepatocellular carcinoma and molecular therapies. Curr Opin Gastroenterol 25(3):186–194. doi:10.1097/MOG.0b013e32832962a1
Nam SW, Park JY, Ramasamy A, Shevade S, Islam A, Long PM, Park CK, Park SE, Kim SY, Lee SH, Park WS, Yoo NJ, Liu ET, Miller LD, Lee JY (2005) Molecular changes from dysplastic nodule to hepatocellular carcinoma through gene expression profiling. Hepatology 42(4):809–818. doi:10.1002/hep.20878
Huang H, Fujii H, Sankila A, Mahler-Araujo BM, Matsuda M, Cathomas G, Ohgaki H (1999) Beta-catenin mutations are frequent in human hepatocellular carcinomas associated with hepatitis C virus infection. Am J Pathol 155(6):1795–1801
Cheng WT, Xu K, Tian DY, Zhang ZG, Liu LJ, Chen Y (2009) Role of Hedgehog signaling pathway in proliferation and invasiveness of hepatocellular carcinoma cells. Int J Oncol 34(3):829–836
Castello G, Scala S, Palmieri G, Curley SA, Izzo F (2010) HCV-related hepatocellular carcinoma: from chronic inflammation to cancer. Clin Immunol 134(3):237–250. doi:10.1016/j.clim.2009.10.007
Bartosch B, Thimme R, Blum HE, Zoulim F (2009) Hepatitis C virus-induced hepatocarcinogenesis. J Hepatol 51(4):810–820. doi:10.1016/j.jhep.2009.05.008
Moradpour D, Blum HE (2005) Pathogenesis of hepatocellular carcinoma. Eur J Gastroenterol Hepatol 17(5):477–483. doi:00042737-200505000-00002
Nakamoto Y, Guidotti LG, Kuhlen CV, Fowler P, Chisari FV (1998) Immune pathogenesis of hepatocellular carcinoma. J Exp Med 188(2):341–350
Mantovani A, Allavena P, Sica A, Balkwill F (2008) Cancer-related inflammation. Nature 454(7203):436–444. doi:10.1038/nature07205
Haybaeck J, Zeller N, Wolf MJ, Weber A, Wagner U, Kurrer MO, Bremer J, Iezzi G, Graf R, Clavien PA, Thimme R, Blum H, Nedospasov SA, Zatloukal K, Ramzan M, Ciesek S, Pietschmann T, Marche PN, Karin M, Kopf M, Browning JL, Aguzzi A, Heikenwalder M (2009) A lymphotoxin-driven pathway to hepatocellular carcinoma. Cancer Cell 16(4):295–308. doi:10.1016/j.ccr.2009.08.021
Barash H, RG E, Edrei Y, Ella E, Israel A, Cohen I, Corchia N, Ben-Moshe T, Pappo O, Pikarsky E, Goldenberg D, Shiloh Y, Galun E, Abramovitch R (2010) Accelerated carcinogenesis following liver regeneration is associated with chronic inflammation-induced double-strand DNA breaks. Proc Natl Acad Sci USA 107(5):2207–2212. doi:10.1073/pnas.0908867107
French SW, Oliva J, French BA, Li J, Bardag-Gorce F (2010) Alcohol, nutrition and liver cancer: role of Toll-like receptor signaling. World J Gastroenterol 16(11):1344–1348
Heine H, Lien E (2003) Toll-like receptors and their function in innate and adaptive immunity. Int Arch Allergy Immunol 130(3):180–192. doi:10.1159/000069517IAA30180
Tanaka J, Sugimoto K, Shiraki K, Tameda M, Kusagawa S, Nojiri K, Beppu T, Yoneda K, Yamamoto N, Uchida K, Kojima T, Takei Y (2010) Functional cell surface expression of toll-like receptor 9 promotes cell proliferation and survival in human hepatocellular carcinomas. Int J Oncol 37(4):805–814
Li YW, Qiu SJ, Fan J, Zhou J, Gao Q, Xiao YS, Xu YF (2010) Intratumoral neutrophils: a poor prognostic factor for hepatocellular carcinoma following resection. J Hepatol. doi:10.1016/j.jhep.2010.07.044
Gomez D, Farid S, Malik HZ, Young AL, Toogood GJ, Lodge JP, Prasad KR (2008) Preoperative neutrophil-to-lymphocyte ratio as a prognostic predictor after curative resection for hepatocellular carcinoma. World J Surg 32(8):1757–1762. doi:10.1007/s00268-008-9552-6
Kuang DM, Zhao Q, Wu Y, Peng C, Wang J, Xu Z, Yin XY, Zheng L (2010) Peritumoral neutrophils link inflammatory response to disease progression by fostering angiogenesis in hepatocellular carcinoma. J Hepatol. doi:10.1016/j.jhep.2010.08.041
Yu JJ, Gaffen SL (2008) Interleukin-17: a novel inflammatory cytokine that bridges innate and adaptive immunity. Front Biosci 13:170–177
Zhang JP, Yan J, Xu J, Pang XH, Chen MS, Li L, Wu C, Li SP, Zheng L (2009) Increased intratumoral IL-17-producing cells correlate with poor survival in hepatocellular carcinoma patients. J Hepatol 50(5):980–989. doi:10.1016/j.jhep.2008.12.033
Kuang DM, Peng C, Zhao Q, Wu Y, Zhu LY, Wang J, Yin XY, Li L, Zheng L (2010) Tumor-activated monocytes promote expansion of IL-17-producing CD8+ T cells in hepatocellular carcinoma patients. J Immunol 185(3):1544–1549. doi:10.4049/jimmunol.0904094
Kuang DM, Peng C, Zhao Q, Wu Y, Chen MS, Zheng L (2010) Activated monocytes in peritumoral stroma of hepatocellular carcinoma promote expansion of memory T helper 17 cells. Hepatology 51(1):154–164. doi:10.1002/hep.23291
Wada Y, Nakashima O, Kutami R, Yamamoto O, Kojiro M (1998) Clinicopathological study on hepatocellular carcinoma with lymphocytic infiltration. Hepatology 27(2):407–414. doi:10.1002/hep.510270214
Unitt E, Marshall A, Gelson W, Rushbrook SM, Davies S, Vowler SL, Morris LS, Coleman N, Alexander GJ (2006) Tumour lymphocytic infiltrate and recurrence of hepatocellular carcinoma following liver transplantation. J Hepatol 45(2):246–253. doi:10.1016/j.jhep.2005.12.027
Gao Q, Qiu SJ, Fan J, Zhou J, Wang XY, Xiao YS, Xu Y, Li YW, Tang ZY (2007) Intratumoral balance of regulatory and cytotoxic T cells is associated with prognosis of hepatocellular carcinoma after resection. J Clin Oncol 25(18):2586–2593. doi:10.1200/JCO.2006.09.4565
Hirano S, Iwashita Y, Sasaki A, Kai S, Ohta M, Kitano S (2007) Increased mRNA expression of chemokines in hepatocellular carcinoma with tumor-infiltrating lymphocytes. J Gastroenterol Hepatol 22(5):690–696. doi:10.1111/j.1440-1746.2006.04551.x
Chew V, Tow C, Teo M, Wong HL, Chan J, Gehring A, Loh M, Bolze A, Quek R, Lee VK, Lee KH, Abastado JP, Toh HC, Nardin A (2010) Inflammatory tumour microenvironment is associated with superior survival in hepatocellular carcinoma patients. J Hepatol 52(3):370–379. doi:10.1016/j.jhep.2009.07.013
Hiroishi K, Eguchi J, Baba T, Shimazaki T, Ishii S, Hiraide A, Sakaki M, Doi H, Uozumi S, Omori R, Matsumura T, Yanagawa T, Ito T, Imawari M (2010) Strong CD8(+) T-cell responses against tumor-associated antigens prolong the recurrence-free interval after tumor treatment in patients with hepatocellular carcinoma. J Gastroenterol 45(4):451–458. doi:10.1007/s00535-009-0155-2
Komita H, Homma S, Saotome H, Zeniya M, Ohno T, Toda G (2006) Interferon-gamma produced by interleukin-12-activated tumor infiltrating CD8+ T cells directly induces apoptosis of mouse hepatocellular carcinoma. J Hepatol 45(5):662–672. doi:10.1016/j.jhep.2006.05.018
Caligiuri MA (2008) Human natural killer cells. Blood 112(3):461–469. doi:10.1182/blood-2007-09-077438
Taketomi A, Shimada M, Shirabe K, Kajiyama K, Gion T, Sugimachi K (1998) Natural killer cell activity in patients with hepatocellular carcinoma: a new prognostic indicator after hepatectomy. Cancer 83(1):58–63. doi:10.1002/(SICI)1097-0142(19980701)83:1<58::AID-CNCR8>3.0.CO;2-A
Chuang WL, Liu HW, Chang WY (1990) Natural killer cell activity in patients with hepatocellular carcinoma relative to early development and tumor invasion. Cancer 65(4):926–930
Miyagi T, Takehara T, Tatsumi T, Kanto T, Suzuki T, Jinushi M, Sugimoto Y, Sasaki Y, Hori M, Hayashi N (2003) CD1d-mediated stimulation of natural killer T cells selectively activates hepatic natural killer cells to eliminate experimentally disseminated hepatoma cells in murine liver. Int J Cancer 106(1):81–89. doi:10.1002/ijc.11163
Chen X, Fu S, Chen F, Chen H, Chen Z (2008) Identification of tumor-associated antigens in human hepatocellular carcinoma by autoantibodies. Oncol Rep 20(4):979–985
Heo CK, Woo MK, Yu DY, Lee JY, Yoo JS, Yoo HS, Ko JH, Kim JM, Choi JY, Kim IG, Paik SG, Cho EW (2010) Identification of autoantibody against fatty acid synthase in hepatocellular carcinoma mouse model and its application to diagnosis of HCC. Int J Oncol 36(6):1453–1459
Nakano K, Orita T, Nezu J, Yoshino T, Ohizumi I, Sugimoto M, Furugaki K, Kinoshita Y, Ishiguro T, Hamakubo T, Kodama T, Aburatani H, Yamada-Okabe H, Tsuchiya M (2009) Anti-glypican 3 antibodies cause ADCC against human hepatocellular carcinoma cells. Biochem Biophys Res Commun 378(2):279–284. doi:10.1016/j.bbrc.2008.11.033
Dunn GP, Koebel CM, Schreiber RD (2006) Interferons, immunity and cancer immunoediting. Nat Rev Immunol 6(11):836–848. doi:10.1038/nri1961
Smyth MJ, Crowe NY, Godfrey DI (2001) NK cells and NKT cells collaborate in host protection from methylcholanthrene-induced fibrosarcoma. Int Immunol 13(4):459–463
Dunn GP, Old LJ, Schreiber RD (2004) The immunobiology of cancer immunosurveillance and immunoediting. Immunity 21(2):137–148. doi:10.1016/j.immuni.2004.07.017
Nagao M, Nakajima Y, Hisanaga M, Kayagaki N, Kanehiro H, Aomatsu Y, Ko S, Yagita H, Yamada T, Okumura K, Nakano H (1999) The alteration of Fas receptor and ligand system in hepatocellular carcinomas: how do hepatoma cells escape from the host immune surveillance in vivo? Hepatology 30(2):413–421. doi:10.1002/hep.510300237
Nagao M, Nakajima Y, Kanehiro H, Hisanaga M, Aomatsu Y, Ko S, Tatekawa Y, Ikeda N, Kanokogi H, Urizono Y, Kobayashi T, Shibaji T, Kanamura T, Ogawa S, Nakano H (2000) The impact of interferon gamma receptor expression on the mechanism of escape from host immune surveillance in hepatocellular carcinoma. Hepatology 32(3):491–500. doi:10.1053/jhep.2000.16470
Gehring AJ, Ho ZZ, Tan AT, Aung MO, Lee KH, Tan KC, Lim SG, Bertoletti A (2009) Profile of tumor antigen-specific CD8 T cells in patients with hepatitis B virus-related hepatocellular carcinoma. Gastroenterology 137(2):682–690. doi:10.1053/j.gastro.2009.04.045
Hsu PN, Yang TC, Kao JT, Cheng KS, Lee YJ, Wang YM, Hsieh CT, Lin CW, Wu YY (2010) Increased PD-1 and decreased CD28 expression in chronic hepatitis B patients with advanced hepatocellular carcinoma. Liver Int 30(9):1379–1386. doi:10.1111/j.1478-3231.2010.02323.x
Maki A, Matsuda M, Asakawa M, Kono H, Fujii H, Matsumoto Y (2004) Decreased expression of CD28 coincides with the down-modulation of CD3zeta and augmentation of caspase-3 activity in T cells from hepatocellular carcinoma-bearing patients and hepatitis C virus-infected patients. J Gastroenterol Hepatol 19(12):1348–1356. doi:10.1111/j.1440-1746.2004.03455.x
Shi F, Shi M, Zeng Z, Qi RZ, Liu ZW, Zhang JY, Yang YP, Tien P, Wang FS (2011) PD-1 and PD-L1 upregulation promotes CD8(+) T-cell apoptosis and postoperative recurrence in hepatocellular carcinoma patients. Int J Cancer 128(4):887–896. doi:10.1002/ijc.25397
Wu K, Kryczek I, Chen L, Zou W, Welling TH (2009) Kupffer cell suppression of CD8+ T cells in human hepatocellular carcinoma is mediated by B7-H1/programmed death-1 interactions. Cancer Res 69(20):8067–8075. doi:10.1158/0008-5472.CAN-09-0901
Ormandy LA, Farber A, Cantz T, Petrykowska S, Wedemeyer H, Horning M, Lehner F, Manns MP, Korangy F, Greten TF (2006) Direct ex vivo analysis of dendritic cells in patients with hepatocellular carcinoma. World J Gastroenterol 12(20):3275–3282
Ormandy LA, Hillemann T, Wedemeyer H, Manns MP, Greten TF, Korangy F (2005) Increased populations of regulatory T cells in peripheral blood of patients with hepatocellular carcinoma. Cancer Res 65(6):2457–2464. doi:10.1158/0008-5472.CAN-04-3232
Yang XH, Yamagiwa S, Ichida T, Matsuda Y, Sugahara S, Watanabe H, Sato Y, Abo T, Horwitz DA, Aoyagi Y (2006) Increase of CD4+ CD25+ regulatory T-cells in the liver of patients with hepatocellular carcinoma. J Hepatol 45(2):254–262. doi:10.1016/j.jhep.2006.01.036
Unitt E, Rushbrook SM, Marshall A, Davies S, Gibbs P, Morris LS, Coleman N, Alexander GJ (2005) Compromised lymphocytes infiltrate hepatocellular carcinoma: the role of T-regulatory cells. Hepatology 41(4):722–730. doi:10.1002/hep.20644
Fu J, Xu D, Liu Z, Shi M, Zhao P, Fu B, Zhang Z, Yang H, Zhang H, Zhou C, Yao J, Jin L, Wang H, Yang Y, Fu YX, Wang FS (2007) Increased regulatory T cells correlate with CD8 T-cell impairment and poor survival in hepatocellular carcinoma patients. Gastroenterology 132(7):2328–2339. doi:10.1053/j.gastro.2007.03.102
Kobayashi N, Hiraoka N, Yamagami W, Ojima H, Kanai Y, Kosuge T, Nakajima A, Hirohashi S (2007) FOXP3+ regulatory T cells affect the development and progression of hepatocarcinogenesis. Clin Cancer Res 13(3):902–911. doi:10.1158/1078-0432.CCR-06-2363
Cao M, Cabrera R, Xu Y, Firpi R, Zhu H, Liu C, Nelson DR (2007) Hepatocellular carcinoma cell supernatants increase expansion and function of CD4(+)CD25(+) regulatory T cells. Lab Invest 87(6):582–590. doi:10.1038/labinvest.3700540
Zhou J, Ding T, Pan W, Zhu LY, Li L, Zheng L (2009) Increased intratumoral regulatory T cells are related to intratumoral macrophages and poor prognosis in hepatocellular carcinoma patients. Int J Cancer 125(7):1640–1648. doi:10.1002/ijc.24556
Hoechst B, Ormandy LA, Ballmaier M, Lehner F, Kruger C, Manns MP, Greten TF, Korangy F (2008) A new population of myeloid-derived suppressor cells in hepatocellular carcinoma patients induces CD4(+)CD25(+)Foxp3(+) T cells. Gastroenterology 135(1):234–243. doi:10.1053/j.gastro.2008.03.020
Chu MH, Chien SC, Hu CP, Wang CY, Lee SD, Tsai YT, Wu JC, Han SH, Chang CM (1988) Natural and activated cytotoxic lymphocytes reactivity to human hepatocellular carcinoma cell lines in hepatocellular carcinoma patients. Liver 8(4):198–207
Cai L, Zhang Z, Zhou L, Wang H, Fu J, Zhang S, Shi M, Zhang H, Yang Y, Wu H, Tien P, Wang FS (2008) Functional impairment in circulating and intrahepatic NK cells and relative mechanism in hepatocellular carcinoma patients. Clin Immunol 129(3):428–437. doi:10.1016/j.clim.2008.08.012
Jinushi M, Takehara T, Tatsumi T, Hiramatsu N, Sakamori R, Yamaguchi S, Hayashi N (2005) Impairment of natural killer cell and dendritic cell functions by the soluble form of MHC class I-related chain A in advanced human hepatocellular carcinomas. J Hepatol 43(6):1013–1020. doi:10.1016/j.jhep.2005.05.026
Hoechst B, Voigtlaender T, Ormandy L, Gamrekelashvili J, Zhao F, Wedemeyer H, Lehner F, Manns MP, Greten TF, Korangy F (2009) Myeloid derived suppressor cells inhibit natural killer cells in patients with hepatocellular carcinoma via the NKp30 receptor. Hepatology 50(3):799–807. doi:10.1002/hep.23054
Witkowski M, Spangenberg HC, Neumann-Haefelin C, Buttner N, Breous E, Kersting N, Drognitz O, Hopt UT, Blum HE, Semmo N, Thimme R (2010) Lack of ex vivo peripheral and intrahepatic alpha-fetoprotein-specific CD4+ responses in hepatocellular carcinoma. Int J Cancer. doi:10.1002/ijc.25866
Thimme R, Neagu M, Boettler T, Neumann-Haefelin C, Kersting N, Geissler M, Makowiec F, Obermaier R, Hopt UT, Blum HE, Spangenberg HC (2008) Comprehensive analysis of the alpha-fetoprotein-specific CD8+ T cell responses in patients with hepatocellular carcinoma. Hepatology 48(6):1821–1833. doi:10.1002/hep.22535
Behboudi S, Alisa A, Boswell S, Anastassiou J, Pathan AA, Williams R (2010) Expansion of anti-AFP Th1 and Tc1 responses in hepatocellular carcinoma occur in different stages of disease. Br J Cancer 102(4):748–753. doi:10.1038/sj.bjc.6605526
Yang Y, Nagano H, Ota H, Morimoto O, Nakamura M, Wada H, Noda T, Damdinsuren B, Marubashi S, Miyamoto A, Takeda Y, Dono K, Umeshita K, Nakamori S, Wakasa K, Sakon M, Monden M (2007) Patterns and clinicopathologic features of extrahepatic recurrence of hepatocellular carcinoma after curative resection. Surgery 141(2):196–202. doi:10.1016/j.surg.2006.06.033
Takayama T, Sekine T, Makuuchi M, Yamasaki S, Kosuge T, Yamamoto J, Shimada K, Sakamoto M, Hirohashi S, Ohashi Y, Kakizoe T (2000) Adoptive immunotherapy to lower postsurgical recurrence rates of hepatocellular carcinoma: a randomised trial. Lancet 356(9232):802–807. doi:10.1016/S0140-6736(00)02654-4
Zerbini A, Pilli M, Laccabue D, Pelosi G, Molinari A, Negri E, Cerioni S, Fagnoni F, Soliani P, Ferrari C, Missale G (2010) Radiofrequency thermal ablation for hepatocellular carcinoma stimulates autologous NK-cell response. Gastroenterology 138(5):1931–1942. doi:10.1053/j.gastro.2009.12.051
Zerbini A, Pilli M, Fagnoni F, Pelosi G, Pizzi MG, Schivazappa S, Laccabue D, Cavallo C, Schianchi C, Ferrari C, Missale G (2008) Increased immunostimulatory activity conferred to antigen-presenting cells by exposure to antigen extract from hepatocellular carcinoma after radiofrequency thermal ablation. J Immunother 31(3):271–282. doi:10.1097/CJI.0b013e318160ff1c
Grimm CF, Ortmann D, Mohr L, Michalak S, Krohne TU, Meckel S, Eisele S, Encke J, Blum HE, Geissler M (2000) Mouse alpha-fetoprotein-specific DNA-based immunotherapy of hepatocellular carcinoma leads to tumor regression in mice. Gastroenterology 119(4):1104–1112
Butterfield LH, Ribas A, Dissette VB, Lee Y, Yang JQ, De la Rocha P, Duran SD, Hernandez J, Seja E, Potter DM, McBride WH, Finn R, Glaspy JA, Economou JS (2006) A phase I/II trial testing immunization of hepatocellular carcinoma patients with dendritic cells pulsed with four alpha-fetoprotein peptides. Clin Cancer Res 12(9):2817–2825. doi:10.1158/1078-0432.CCR-05-2856
Palmer DH, Midgley RS, Mirza N, Torr EE, Ahmed F, Steele JC, Steven NM, Kerr DJ, Young LS, Adams DH (2009) A phase II study of adoptive immunotherapy using dendritic cells pulsed with tumor lysate in patients with hepatocellular carcinoma. Hepatology 49(1):124–132. doi:10.1002/hep.22626
Jager E, Gnjatic S, Nagata Y, Stockert E, Jager D, Karbach J, Neumann A, Rieckenberg J, Chen YT, Ritter G, Hoffman E, Arand M, Old LJ, Knuth A (2000) Induction of primary NY-ESO-1 immunity: CD8+ T lymphocyte and antibody responses in peptide-vaccinated patients with NY-ESO-1+ cancers. Proc Natl Acad Sci USA 97(22):12198–12203. doi:10.1073/pnas.220413497220413497
Shibolet O, Alper R, Zlotogarov L, Thalenfeld B, Engelhardt D, Rabbani E, Ilan Y (2003) NKT and CD8 lymphocytes mediate suppression of hepatocellular carcinoma growth via tumor antigen-pulsed dendritic cells. Int J Cancer 106(2):236–243. doi:10.1002/ijc.11201
Margalit M, Shibolet O, Klein A, Elinav E, Alper R, Thalenfeld B, Engelhardt D, Rabbani E, Ilan Y (2005) Suppression of hepatocellular carcinoma by transplantation of ex-vivo immune-modulated NKT lymphocytes. Int J Cancer 115(3):443–449. doi:10.1002/ijc.20889
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Flecken, T., Spangenberg, H.C. & Thimme, R. Immunobiology of hepatocellular carcinoma. Langenbecks Arch Surg 397, 673–680 (2012). https://doi.org/10.1007/s00423-011-0783-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-011-0783-x