Abstract
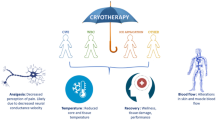
Cryotherapy is utilized as a physical intervention in the treatment of injury and exercise recovery. Traditionally, ice is used in the treatment of musculoskeletal injury while cold water immersion or whole-body cryotherapy is used for recovery from exercise. In humans, the primary benefit of traditional cryotherapy is reduced pain following injury or soreness following exercise. Cryotherapy-induced reductions in metabolism, inflammation, and tissue damage have been demonstrated in animal models of muscle injury; however, comparable evidence in humans is lacking. This absence is likely due to the inadequate duration of application of traditional cryotherapy modalities. Traditional cryotherapy application must be repeated to overcome this limitation. Recently, the novel application of cooling with 15 °C phase change material (PCM), has been administered for 3–6 h with success following exercise. Although evidence suggests that chronic use of cryotherapy during resistance training blunts the anabolic training effect, recovery using PCM does not compromise acute adaptation. Therefore, following exercise, cryotherapy is indicated when rapid recovery is required between exercise bouts, as opposed to after routine training. Ultimately, the effectiveness of cryotherapy as a recovery modality is dependent upon its ability to maintain a reduction in muscle temperature and on the timing of treatment with respect to when the injury occurred, or the exercise ceased. Therefore, to limit the proliferation of secondary tissue damage that occurs in the hours after an injury or a strenuous exercise bout, it is imperative that cryotherapy be applied in abundance within the first few hours of structural damage.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cryotherapy, the reduction of tissue temperature by the withdrawal of heat from the body (Michlovitz 1990), has been utilised in the treatment of injury for centuries. Hippocrates, who mentioned the use of snow and ice in his work to reduce oedema with good results, has been credited as the grandfather of the cryotherapy movement (Rivenburgh 1992). In the 1960s, cryotherapy in the form of ice was recommended for use in the treatment of musculoskeletal injury (Grant 1964; Hayden 1964). In the 1970s, Knight broke down the series of events that follow athletic injuries into primary and secondary-injury classifications (Knight 1976), and went on to investigate and detail the application of ice for its ability to retard secondary injury (Knight 1985, 1995; Knight et al. 2000). The tenets of Knight’s original model were updated in the early 2000s with a specific focus on the role of cryotherapy in the injury sequelae (Merrick 2002).
Ultimately, the processes that transpire within the muscle during injury or exercise are both defined by damage of the myofilament structures (Fig. 1), are initiated rapidly, and occur in several stages (Armstrong 1990; Armstrong et al. 1991; Huard et al. 2002; Järvinen et al. 2005; Lieber 2018). These events can be divided into the initial damage response, followed by a secondary damage response, and culminating in a regenerative/repair phase. Since the initial phase occurs during the injury or exercise, administering a recovery modality at this stage is not possible. The subsequent secondary stage involves a proliferation of the initial muscle injury, coupled with an inflammatory response surrounding the damaged area (Knight 1976; Merrick 2002). Following the natural course of catabolic events, the muscle fibre returns to its pre-exercise condition, and cellular homeostasis and physiological function are restored. The time course of this cycle is dependent on the magnitude of damage (Huard et al. 2002; Paulsen et al. 2012). Based on what is known about the post-injury (McArdle and Jackson 1997; Abrams 1997; Huard et al. 2002) and post-exercise (Kendall and Eston 2002; Lapointe et al. 2002; Peake et al. 2005; Howatson and van Someren 2008) cellular response, it is at the secondary stage where the application of cryotherapy might be advantageous in diminishing the proliferation of initial damage (Knight 1995; Merrick 2002; Enwemeka et al. 2002; Bleakley et al. 2012b; Ihsan et al. 2013), reducing secondary muscle damage (Knight 1985, 1995; Swenson et al. 1996; Merrick et al. 1999; Knight et al. 2000), and enhancing the regenerative response (Järvinen et al. 2005; Dykstra et al. 2009). As a result, the application of cryotherapy has been adopted for use not only by clinicians to treat injuries (Barnes 1979; Hubbard and Denegar 2004; Bleakley et al. 2004, 2011; Collins 2008; Carvalho et al. 2010; Bleakley and Davison 2010a; Tiidus 2015; Page 2018), but also by athletes to facilitate recovery from exercise (Bishop et al. 2008; Robson-Ansley et al. 2009; Nédélec et al. 2012; Versey et al. 2013; Kovacs and Baker 2014; Dupuy et al. 2018; Peake 2019).
One direct pathway to injury induced structural damage and three indirect pathways to exercise-induced structural damage. Localized soft tissue injury is always the result of a direct insult to the area (e.g. blunt force trauma, sheer stress, etc.) On the other hand, during exercise, three indirect pathways exist which all result in exercise-induced structural damage. (1) Mechanical stress, occurring from an increase in the net mechanical stress per muscle fibre (Enoka 1996), causes structural damage to the muscle fibre directly due to a failure in the myofibrils during eccentric contractions. (2) Exercise of prolonged duration and/or high metabolic intensity, such as marathon running results in metabolic stress. In the metabolic damage model, the initial events resulting in structural damage are caused by metabolic deficiencies which increase the vulnerability of the muscle fibre to mechanical stress (Tee et al. 2007). Metabolic stress and (3) the increase in temperature which occurs during exercise cause structural damage indirectly through an increase in the metabolic rate and nicotinamide adenine dinucleotide phosphate oxidase (NOX) activity, respectively. Both result in an increase in mitochondrial reactive oxygen species (ROS) activity. Cryotherapy cannot influence the primary damage response. However, if applied immediately following primary damage, and ideally prior to the potentiation of secondary damage, cryotherapy might minimise the risk of further damage to the musculature by mitigating the impairments typically occurring following injury or exercise
In practice, ice packs have become ubiquitous in training rooms. There is a longstanding tradition of applying ice (I), compression (C), and elevation (E), or ICE, and its many derivatives (Bleakley et al. 2012a), in the treatment of acute musculoskeletal injury (Merrick et al. 1993, 2003; Barlas et al. 1996; Block 2010; Tomchuk et al. 2010; Bleakley and Davison 2010a; Gillette and Merrick 2018). Although icing remains the standard of care following injury and despite its widespread use, evidence to support its use is limited (Knight 1995; Bleakley and Davison 2010a). Furthermore, no conclusive clinical evidence exists in humans in favour of ice, or the use of cryotherapy in any form for that matter, following injury (Block 2010). Additionally, there is a growing trend throughout the literature recommending against icing injuries so as not to blunt the natural healing response (Takagi et al. 2011; White and Wells 2013). As a result, there has recently been much debate amongst clinicians about best practice following injury (Mirkin 2014; Page 2018), with some recomending that cryotherapy be removed entirely from the standard management of soft-tissue injuries (Dubois and Esculier 2020).
Comparably, several other cryotherapy modalities varying in convenience and expense, traditionally in the form of whole-body cryotherapy (WBC) and cold-water immersion (CWI), and more recently phase change material (PCM), are omnipresent throughout professional, collegiate, and recreational athletic training facilities, spas, and even the home. Modalities that can be administered to larger areas of the body at a time are more commonly implemented than ice in an attempt to accelerate recovery following exercise. There are data showing beneficial effects, no benefits and even detrimental effects when cryotherapy is used in this context (Bleakley et al. 2010; Leeder et al. 2012; Poppendieck et al. 2013; Hohenauer et al. 2015) and evidence suggests that repeated use of cryotherapy attenuates strength gains following resistance training (Yamane et al. 2015; Roberts et al. 2015b; Fyfe et al. 2019; Hyldahl and Peake 2020).
Although the physiological effects and mechanisms associated with cryotherapy in humans have been investigated (Wilcock et al. 2006; White and Wells 2013; Ihsan et al. 2016; Bongers et al. 2017) and while some advances have recently been made in the understanding of the molecular response to cryotherapy (Broatch et al. 2018), the lack of consistent and unanimous evidence has resulted in controversy over the efficacy of most cryotherapy interventions following both injury and exercise. There remains a large gap in the scientific basis for the use of cryotherapy for recovery in humans, particularly because recommendations for optimal protocols stem from evidence demonstrated in animal models (Bleakley and Davison 2010b). Evidence is specifically lacking to identify and provide guidelines concerning cryotherapy treatment application, duration, and frequency (MacAuley 2001; Bleakley et al. 2004), following both injury and exercise. Furthermore, exactly how cryotherapy might diminish the secondary damage response following either injury or exercise remains unknown, and whether the application of cryotherapy has the same effects on secondary damage following injury as it does following exercise remains unknown. Finally, the effects, or lack thereof, of post-injury or post-exercise cryotherapy on muscle metabolism and inflammation in humans remain to be elucidated.
The role of cryotherapy in the treatment of and recovery from injury must be revisited, and its use for recovery from exercise must be reviewed. Specifically, the effect of cryotherapy on reducing metabolism and inflammation, and the mechanisms through which cryotherapy might achieve these effects in humans, must be addressed. Thus, the purpose of this narrative review will be to clarify and summarize the current best available evidence in support of the effects of various cryotherapy modalities in injury treatment and exercise recovery, and to provide evidence-based recommendations for the application of cryotherapy modalities in both injury treatment and exercise recovery scenarios. Importantly, providing a summary on the use of cooling techniques prior to (pre-cooling) or during (per-cooling) exercise is beyond the scope of this review.
The effects of cryotherapy interventions on metabolism and inflammation
There exists a long-standing belief that cryotherapy reduces the metabolic rate and thus the inflammation that occurs after the acute structural trauma by reducing temperature and blood flow at the site of injury or muscle damage. Suppressing local metabolic demand (Ho et al. 1995; Merrick 2002; Schaser et al. 2006) and limiting the inflammatory response (Ciolek 1985; Knigh 1985, 1995; Swenson et al. 1996; Merrick Rankin Andres and Hinman 1999; Merrick 2002; Schaser et al. 2006) are believed to diminish the proliferation and magnitude of the secondary injury occurring within the skeletal muscle and the surrounding site of injury (Meeusen and Lievens 1986; Knight 1995; Eston and Peters 1999; Merrick et al. 1999; Merrick and McBrier 2010). However, the scientific basis for administering cryotherapy to reduce metabolism and inflammation following both injury and exercise comes from evidence demonstrated in animal models. Animal models suggest that the optimum tissue temperature range for a reduction in cellular metabolic activity (Osterman et al. 1984; Sapega et al. 1988) and oxygen demand (Fuhrman 1959; Fuhrman et al. 1961) without causing tissue damage, is in the range of 10–15 °C (absolute temperature; Sapega et al. 1988). Tissue temperatures in excess of 15 °C have also shown suppressed metabolic activity (Puntel et al. 2012), reduced oedema formation (Smith et al. 1993; Dolan et al. 1997; Deal et al. 2002; Lee et al. 2005; Schaser et al. 2006), and reduced tissue damage (Merrick et al. 1999; Schaser et al. 2007; Bleakley and Hopkins 2010; Puntel et al. 2012) in animals. Similarly, animal models have demonstrated that cryotherapy is capable of reducing the inflammatory response that occurs following injury (Amon et al. 2003; Lee et al. 2005; Schaser et al. 2006, 2007; Puntel et al. 2012; Vieira Ramos et al. 2016). Although these effects demonstrated in animal models have formed the basis for the application of cryotherapy in humans, in vivo intramuscular temperatures below 20 °C during cryotherapy in humans have not been reported (Bleakley and Hopkins 2010; Bleakley et al. 2012b).
Clinicians and athletes alike must recognize the challenge of directly translating the findings from the effects of cryotherapy treatment in animal studies to humans (Bleakley et al. 2012b). This is primarily because rodent muscle has different metabolic properties and responses to environmental stimuli than human skeletal muscle (Kowalski and Bruce 2014). Rodents are typically covered in hairy skin, which does not experience arterio-venous anastomoses (Greenfield 1963), and might experience a direct inhibitory effect on the normal vasoconstrictor response during local cooling (Faber 1988). Crucially, the magnitude of reduction in muscle temperature and blood flow induced by cryotherapy is significantly greater in animals because of the smaller subcutaneous adiposity and overall body size compared to humans. On this note, animal models caution that if sufficient muscle cooling is achieved following injury it might actually delay repair (Takagi et al. 2011; Singh et al. 2017; Miyakawa et al. 2020) and increase muscle scarring (Takagi et al. 2011) or slow muscle regeneration (Kawashima et al. 2021). However, it is highly unlikely that the degree of intramuscular cooling attained from 20 minutes of ice pack application in the rodents of Takagi et al.’s (2011) study would be achieved in humans. Indeed, in humans, cryotherapy-induced decrements in muscle metabolism and, or inflammation can be hindered by the magnitude of muscle damage, and by the effect of adipose tissue on heat extraction (Bleakley and Hopkins 2010). Therefore, results from animal studies cannot be directly applied to form the basis of cryotherapy application for recovery in humans.
In summary, based on the rationale derived from animal models, cryotherapy has been used in humans following both injury and exercise in an attempt to reduce metabolism and attenuate inflammation. However, the ability of cryotherapy to reduce muscle metabolism in humans has not been established. Only one study indirectly measuring muscle metabolism in humans has been able to demonstrate decreased muscle metabolic activity following post-exercise cooling (Ihsan et al. 2013). Similarly, in humans, there is only a handful of research that supports the use of cryotherapy for reducing the inflammatory response following exercise (Pournot et al. 2011; Ziemann et al. 2012; Guilhem et al. 2013) while most studies show no reduction in inflammation (Ingram et al. 2009; Pointon et al. 2011; Leeder et al. 2012; Pointon and Duffield 2012; Fragala et al. 2015; Peake et al. 2016). Others have demonstrated an exacerbated inflammatory response following post-exercise CWI (Gonzalez et al. 2014; Roberts et al. 2014; Jajtner et al. 2015) or topical cooling with a cold pack (Tseng et al. 2013). Recent evidence suggests that low tissue temperatures (8 °C) might accentuate the inflammatory response in deeper muscle tissues (Mawhinney et al. 2020).
The effects of cryotherapy interventions on tissue temperature
The mechanisms of cryotherapy were traditionally believed to be dependent on the cold induced vascular response, and that the cold‐induced reductions in muscle blood flow were responsible for reducing muscle metabolism, inflammation, and the subsequent secondary damage (Swenson et al. 1996; Merrick et al. 1999; Knight et al. 2000; Ihsan et al. 2016). However, cryotherapy-induced reductions in muscle blood flow are based on techniques that only allow for the indirect inference of hemodynamic or volume changes within the limb (Fiscus et al. 2005; Vaile et al. 2010; Ihsan et al. 2013; Roberts et al. 2015a; Choo et al. 2018; Stephens et al. 2018). It has more recently been established that the effectiveness of cryotherapy as a recovery modality is primarily dependent upon its ability to reduce muscle temperature, not muscle blood flow (Bleakley and Davison 2010a; Gregson et al. 2011; Mawhinney et al.2013, 2020).
The importance of achieving a clinically meaningful reduction in intramuscular temperature (Bleakley and Hopkins 2010) has been majorly overlooked but it is of greater significance for recovery than the vascular response (Swenson et al. 2007). This is because the physiological changes that occur following cryotherapy are dependent on the magnitude of muscle cooling, rather than a consequence of reduced muscle blood flow (Mawhinney et al. 2013, 2020). Recent evidence suggests that despite similar changes in muscle temperature following 8, 15, or 22 °C CWI for a period of 10 minutes, the change in muscle perfusion in the deep and superficial muscles was not uniform (Mawhinney et al. 2020). Skeletal muscle tissue perfusion is a reflexive mechanism from the skin. A reduction in muscle perfusion could potentially limit the inflammatory response while concomitantly preserving cellular oxygen supply, ultimately limiting hypoxic cell death and minimizing secondary damage (Wilcock et al. 2006; Merrick and McBrier 2010; Tipton et al. 2017). However, Mawhinney et al. (2020) speculated that 8–15 °C CWI resulted in shivering within the deep musculature which might have been responsible for the increase in deep muscle perfusion evident from the lower immersion temperatures in their study (Blondin et al. 2015). The authors suggested that a more tolerable treatment temperature could avoid the shivering response and the concomitant increase in deep tissue perfusion and might be a more effective option in the recovery process of soft tissue injury or exercise.
Importantly, although deep tissue intramuscular temperatures have been reduced by ~ 8–10 °C following cryotherapy in individuals at rest (Table 1; Kwiecien et al. 2019a: − 12.00 °C and − 10.90 °C at 3 cm during 30 min of ice treatment with elastic wrap and plastic wrap compression, respectively; Kwiecien et al. 2019b: − 7.59 °C at 3 cm during 180 min of 15 °C PCM treatment; Kwiecien et al. 2019b: − 7.20 °C at 3 cm during 15 min of 15 °C CWI treatment; Jutte et al. 2001: − 8.00 °C, Merrick et al. 1993: − 10.13 °C, Tomchuk et al. 2010: − 9.40 °C, all at 2 cm during 30 min of ice treatment with compression), only one study has demonstrated comparable reductions following exercise in hot conditions (Peiffer et al. 2009b: − 7.50 °C at 3 cm during 20 min of 14 °C CWI) while others have not (Freitag et al. 2021: − 1.61 °C at 3 cm during 10 min of 10 °C CWI). It is likely then that a greater cooling stimulus is necessary to reduce intramuscular temperature in an individual following exercise when the intramuscular temperature is elevated above baseline. Although musculoskeletal injury results in structural damage, this response is often localized and does not directly cause systemic elevations in temperature. Both the local and systemic elevations in tissue temperatures occurring during exercise have specific implications for how the dose of cryotherapy should be tailored following an exercise stimulus, but this also often overlooked. An important factor to consider that does not exist when implementing cryotherapy for the treatment of injury is that the rate of post-exercise recovery is related to the extent of the load imposed on the body by the exercise bout (Nédélec et al. 2012). Cryotherapy modalities capable of influencing systemic changes will be more successful at accelerating recovery following exercise during which the individual experienced a high thermal load (Bongers et al. 2017). Following exercise which elicited an increased thermal load, whole-body exposure to a cryotherapy medium, such as that occurring from CWI or WBC, may result in systemic effects to the whole body and produce a greater temperature gradient for tissue cooling. If the exercise induced a very minimal thermal load, local cold application using ice or more recently PCM might only produce local alterations in tissue temperature, but this local response might be sufficiently effective for recovery in this scenario.
The effect of cryotherapy treatment on tissue cooling has been well documented (Merrick et al. 1993; Zemke et al. 1998; Myrer et al. 1998, 2001; Jutte et al. 2001; Enwemeka et al. 2002; Yanagisawa et al. 2007). For a thorough review of the literature reporting on the rate and magnitude of tissue temperature reductions associated with popular cryotherapy dosages, we direct the reader’s attention to Bleakley and Hopkins (2010). In order for cryotherapy to effectively accelerate recovery following either injury or exercise resulting in structural damage, heat removal must occur within the target muscle and not just at the overlying skin (Bleakley and Hopkins 2010). In early cryotherapy literature, it was assumed that changes in intramuscular temperature were strongly related to changes in skin temperature. However, reductions in skin and intramuscular temperature are not strongly correlated (Merrick et al. 1993) and skin temperature is a poor predictor of deep tissue temperature (Bleakley and Hopkins 2010). Yet, when direct measures are unavailable, the efficacy of cryotherapy has often been assessed through measurements of skin surface temperature (Palmer and Knight 1996; Chesterton et al. 2002; Janwantanakul 2004, 2009; Kennet et al. 2007; Ihsan et al. 2013; Kwiecien et al. 2018; Estéfani et al. 2019). For this reason, clinicians, practitioners, and athletes alike often fail to understand that the magnitude of change in tissue temperature is extremely variable across the different tissue layers (e.g. skin, fat, superficial, and deep muscle), and that the skin and superficial tissues reach significantly lower temperatures than the deep muscle during cryotherapy application (for review we bring the readers attention to White and Wells 2013).
Skin is the first site to respond to cold exposure and its temperature decreases most rapidly (Merrick et al. 2003; White and Wells 2013). Skin is responsible for initiating thermoregulatory responses in the muscle because muscle lacks thermal receptors. During skin cooling, based on Fourier's law of heat conduction, deep muscle tissue loses heat mainly to the superficial muscle tissue (Bleakley and Hopkins 2010). Simultaneously incoming warm blood is diverted to the deeper tissues, thereby slowing down the cooling effect of the deep tissues (Pugh et al. 1960). Therefore, superficial muscle tissue cools faster, and to a greater magnitude than deeper muscle tissues (Merrick et al. 2003; Yanagisawa et al. 2007; Peiffer et al. 2009a, 2010; Gregson et al. 2011, 2013; Mawhinney et al. 2013; Roberts et al. 2014, 2015a; Mawhinney et al. 2017). Unfortunately, the magnitude of reduction in muscle temperature required in humans for optimally enhancing recovery remains unknown (Bleakley and Hopkins 2010).
The magnitude of change in muscle temperature is inversely correlated with subcutaneous adiposity (Myrer et al. 2001; Otte et al. 2002). Subcutaneous adipose tissue has low thermal conductivity and provides a layer of insulation, creating an insulating effect (Bleakley and Hopkins 2010). Convective heat loss that occurs from the musculature when cryotherapy is administered to the skin becomes limited as subcutaneous body fat increases (Stocks et al. 2004). Thus, the magnitude of reduction in intramuscular temperature will be less as skin-fold thickness increases (Selkow et al. 2012; Stephens et al. 2017). Subcutaneous tissue thickness should be taken into account when aiming to achieve a specific degree of intramuscular cooling (Selkow 2019). For example, to reduce muscle temperature by a standard amount in a heterogeneous group, Otte et al. (2002) demonstrated that an individual with a 31–40 mm skinfold thickness would have to apply ice for almost six times longer than an individual with 0–10 mm skin-fold thickness. Similarly, an individual with a 0–10 mm skin-fold thickness will achieve the same degree of intramuscular cooling as an individual with a 31–40 mm skin-fold thickness, but the cooling duration will take 10 min vs 60 min, respectively (Selkow 2019).
Similarly, the magnitude of change in muscle temperature is dependent on the thermal gradient between the muscle and the cryotherapy medium (Merrick et al. 2003), and on the duration of cryotherapy application. It has been well established that cold modalities with different thermodynamic properties produce different skin and intramuscular temperatures (Chesterton et al. 2002; Merrick et al. 2003; Vieira et al. 2013). Perhaps somewhat counterintuitive, modalities which melt from a solid to a liquid result in lower intramuscular temperatures than those which maintain the same phase (e.g. gel pack), even though a gel pack may initially be colder and reduce skin temperature faster than a bag of ice or frozen peas (Merrick et al. 2003). Indeed, modalities delivering cryotherapy at extremely low temperatures will rapidly reduce skin temperature but might increase muscle perfusion and would insufficiently reduce intramuscular temperature to a clinically relevant degree for a long enough time to have any influence on attenuating secondary damage. Reducing skin temperature without eliciting reductions in temperature of the deep muscle tissue will not only fail to induce clinically relevant changes in muscle metabolism or inflammation but can also result in cold related injury (Gage 1979; Wilke and Weiner 2003; Wilcock et al. 2006; Selfe et al. 2007; Brown and Hahn 2009; Costello et al. 2012; Tipton et al. 2017).
Cryotherapy modalities used for recovery from injury and exercise
Cryotherapy, in the form of ice, is a mainstay treatment in the management of or rehabilitation from strains, sprains, contusions, as well as fractures, and immediately after acute musculoskeletal soft tissue injury (Barnes 1979; Knight 1985, 1995; Meeusen and Lievens 1986; Swenson et al. 1996; Knight et al. 2000; Beiner and Jokl 2001; Bleakley et al. 2004). Ice has traditionally been applied in the immediate stage following injury for its ability to exert an acute local analgesic effect (Mac Auley 2001; Hubbard and Denegar 2004) by inhibiting nerve conduction velocity (Knight et al. 2000; Chesterton et al. 2002; Algafly and George 2007), and to restrict oedema formation (Meeusen and Lievens 1986). Similarly, intermittent cryo-compression therapy has gained popularity and is most commonly implemented in the immediate stages following injury or at the conclusion of an operative procedure for its purported ability to reduce oedema (Chleboun et al. 1995; Meeusen et al. 1998; Block 2010) and restore function (Schröder and Pässler 1994; Dervin et al. 1998; Waterman et al. 2012; Murgier and Cassard 2014). When used in the management of acute soft tissue injuries or post-surgery, cryotherapy might improve outcomes by limiting haemorrhage formation and secondary cell death (Bleakley et al. 2004), but only if it is instituted soon after the injury has occurred (Collins 2008). Importantly, controlled trials implementing its use following musculoskeletal injuries do not exist so evidence in support of its use for accelerating recovery following injury in humans is equivocal (Table 2).
Following exercise, studies investigating the effect of a single application of ice have shown no effect on recovery of soreness (Yackzan et al. 1984; Gulick et al. 1996). A recent meta-analysis concluded that, following exercise, local cryotherapy in the form of ice does not diminish soreness or accelerate the recovery strength (Nogueira et al. 2019). Since ice is applied locally and is typically limited to treatment durations of less than 30 min, it is unlikely that a single ice treatment over a small area would provide a sufficient cooling stimulus to elicit any systemic effects to accelerate whole body recovery following exercise. For this reason, and as is commonplace following injury (Knight 1995), repeat applications at frequent intervals over several hours should in theory be implemented to enhance the magnitude of cooling (Palmer and Knight 1996). However, this rate of treatment, particularly within the first 12–24 h following exercise, is not commonplace amongst athletes as they are unlikely to comply with such a demanding treatment schedule. Studies investigating repeat applications of ice following exercise are limited and inconclusive. Some studies have shown a positive effect at 48 h on the recovery of soreness (Oakley et al. 2013) and blood markers of muscle damage (Howatson and Van Someren 2003); while others have shown no effect (Howatson et al. 2005) or a delay in the recovery of both soreness and adaptation to exercise training (Isabell et al. 1992; Tseng et al. 2013). Therefore, ice is generally not an effective cryotherapy modality when used for recovery from exercise (Table 2).
Exposing the body to very cold air (− 110 °C to − 140 °C) for durations of 2–4 min while minimally dressed, known as WBC, has become a popular recovery modality following intensive training and competition (Banfi et al. 2010; Costello et al. 2015). The physiological, neuromuscular, and perceptual effects of WBC for accelerating recovery following exercise have been well reviewed (Bleakley et al. 2014). Studies indicate that WBC may successfully accelerate subjective recovery of soreness following exercise (Hausswirth et al. 2011; Pournot et al. 2011; Ziemann et al. 2012; Fonda and Sarabon 2013; Bleakley et al. 2014; Costello et al. 2015; Rose et al. 2017). Evidence further suggests that WBC might effectively suppress the acute inflammatory response following exercise (Banfi et al. 2009, 2010; Hervé Pournot et al. 2011; Ziemann et al. 2012; Guilhem et al. 2013; Ferreira-Junior et al. 2015). However, more recent research demonstrated no effect on inflammation (Krueger et al. 2019). Similarly, evidence for the effect of WBC on functional recovery is mixed, with some studies concluding that WBC positively influenced muscle function or performance capacities (Hausswirth et al. 2011; Ziemann et al. 2012; Fonda and Sarabon 2013; Krüger et al. 2015; Ferreira-Junior et al. 2015), while others have shown no effect on the ability of WBC to improve functional recovery (Bleakley et al. 2014). There is some evidence that WBC augments training-induced aerobic adaptations and performance (Costello et al. 2011; Vieira et al. 2015; Broatch et al. 2019 see Table 2 for a summary of the evidence for accelerated recovery following injury and exercise from WBC in humans).
Water immersion typically in water temperatures of 15 °C or less for a single duration of 15 min or less, known as CWI, is not only the most popular cryotherapy strategy but also one of the most popular recovery strategies used by athletes following exercise (Leeder et al. 2012). The role of CWI for accelerating recovery has been studied following isolated eccentric exercise (Vaile et al. 2007; Machado et al. 2016), endurance exercise (Yeargin et al. 2006; Brophy-Williams et al. 2011; Wilson et al. 2018), resistance exercise (Roberts et al. 2015a), laboratory cycling protocols (Lane and Wenger 2004; Halson et al. 2008; Vaile et al., 2007, 2008, 2010; Peiffer et al. 2010) and team-sport exercise (Montgomery et al. 2008; Rowsell et al. 2009, 2011; Webb et al. 2013; Garcia da Mota and Marocolo 2016; Leeder et al. 2019). Evidence supports the use of CWI for reducing soreness (Montgomery et al. 2008; Ingram et al. 2009; Pournot et al. 2010; Pointon et al. 2011; Hausswirth and Le Meur 2011; Pointon and Duffield 2012; Poppendieck et al. 2013; Minett et al. 2014; Hohenauer et al. 2015; Machado et al. 2015; Siqueira et al. 2018). Meta-analyses have demonstrated clear but limited efficacy of CWI for alleviating soreness for up to 96 h post-exercise (Bleakley et al. 2010; Leeder et al. 2012; Versey et al. 2013). There is also some evidence to support the use of CWI for reducing blood markers of muscle damage (Leeder et al. 2012; Hohenauer et al. 2015; Vieira et al. 2016; Dupuy et al. 2018) and inflammation (Dupuy et al. 2018). Although evidence to support its use for accelerating recovery of strength loss following exercise remains equivocal (Bleakley et al. 2010; Leeder et al. 2012; Poppendieck et al. 2013; Versey et al. 2013; Machado et al. 2015; Hohenauer et al. 2015), it might have some efficacy in recovery of functional performance (Vaile et al. 2008; Leeder et al. 2012; Leeder et al. 2019; see Table 2 for a summary of the evidence for accelerated recovery following injury and exercise from CWI in humans).
The disparity in results can be explained by the variability in immersion temperature and, or duration of CWI protocols implemented throughout the literature. For example, immersion temperature is extremely variable, ranging between 5 and 20 °C (Bleakley et al. 2010; Versey et al. 2013). Some have suggested that lower temperatures might have beneficial effects on recovery following exercise (Rowsell et al. 2009, 2011; Anderson et al. 2018; Dupuy et al. 2018). However, the evidence has demonstrated that reducing water temperature does not produce additional recovery benefits (Sellwood et al. 2007; Corbett et al. 2012; Poppendieck et al. 2013), and it is likely to result in increased discomfort (Bailey et al. 2007; Vaile et al. 2008; Versey et al. 2011). Immersion duration is of greater importance than immersion temperature because, along with frequency of immersions and mode of immersion continuous vs intermittent (White et al. 2013; Hohenauer et al. 2015; Machado et al. 2016; Vieira et al. 2016), it is more strongly correlated with the magnitude of change in muscle temperature (Peiffer et al. 2009a). However, immersion duration is limited by the water temperature as colder temperatures are poorly tolerated. Immersion does not commonly exceed 30 min (Bleakley et al. 2010; Versey et al. 2013; Machado et al. 2015) because it can result in cold induced injury or hypothermia. With this in mind, ~ 10-min durations repeated at frequent intervals are likely to yield best results. However, until best practices are defined, and there is more consistency in how CWI is used, the true magnitude of its efficacy for exercise recovery will elude us (Merrick 2013).
Ice compression elevation, WBC, and CWI are all limited by their treatment duration. Although no consensus exists for optimal treatment criteria, a critical level of tissue cooling must be achieved to optimize the clinical effectiveness of cryotherapy (Bleakley and Hopkins 2010). This can only be achieved by implementing repeat treatments when using traditional forms of cryotherapy (Fig. 2). The duration of cryotherapy can be prolonged while maintaining a comfortable, constant temperature by utilising a cooling medium called phase change material (PCM; for thorough review see Kwiecien et al. 2020a). Ice is technically the most commonly utilized PCM for recovery. Unfortunately, the latent phase, the period of phase change but no detectible temperature change, of 0 °C limits ice from maintaining a cooling capacity for prolonged durations. The latent phase of any PCM can be manipulated and the duration of the latent phase can be prolonged as the phase point increases above 0 °C. This is traditionally achieved by adjusting the ratio of salt hydrate, fatty acids and esters, and, or paraffins that make up the PCM. However, it is imperative to understand that the phase point will dictate the duration that any PCM can hold a given temperature. Compared with conventional cryotherapy interventions, PCM with a phase transition point greater than 0 °C can overcome the limitation of short treatment durations that traditional cryotherapy modalities face. Furthermore, the use of PCM offers a substitute to other more traditional modes of cryotherapy as it allows for the safe manipulation of the frequency, duration, and temperature.
Cryotherapy duration and its effect on duration of tissue temperature reduction. The duration of tissue temperature reduction is limited during single applications of traditional cryotherapy modalities [whole-body cryotherapy (WBC), cold-water immersion (CWI), or ice]. This limitation can be overcome by administering repeat treatments to prolong the duration of reduced tissue temperature. However, this is often logistically impractical, and patients or athletes are unlikely to comply to a rigorous treatment schedule. The duration of tissue temperature reduction is prolonged by administering a single dose of phase change material (PCM) cooling. Alternatively, traditional cryotherapy modalities can be immediately followed by PCM application to prolong the duration of tissue temperature reduction. Although speculative, a critical level of tissue cooling is more likely to be achieved by prolonging the duration of cryotherapy application (through 1. repeat treatments of traditional cryotherapy, 2. Combining a single treatment using traditional methods with PCM cooling immediately after, or 3. Single prolonged treatment using PCM). Prolonging the duration of tissue temperature reduction, particularly during the stage of secondary damage, might optimize the clinical effectiveness of cryotherapy
In particular, the PCM packs we have utilized throughout our research ‘freeze’ at a temperature of 15 °C (Glacier Tek USDA BioPreferred PureTemp PCM, Plymouth, MN, USA), and are advantageous because they can be safely administered for durations of 3 h at a time in one dose (Kwiecien et al. 2019b). Studies examining the effects of 15 °C PCM cooling on indices of recovery from exercise-induced muscle damage have demonstrated that 6 h of 15 °C PCM cooling accelerated recovery of strength and soreness following isolated eccentric exercise of the quadriceps in untrained (Kwiecien et al. 2018) and trained (Kwiecien et al. 2020c) individuals (see Table 2 for summary). Importantly, the protection provided by PCM cooling after an initial bout of eccentric exercise did not interfere with the adaptive response when the exercise was repeated (Kwiecien et al. 2020c). Three hours of PCM cooling has also been shown to accelerate recovery of strength (Clifford et al. 2018; Brownstein et al. 2019) and soreness (Clifford et al. 2018) following soccer match play and baseball pitching (Mullaney et al. 2020), but not following a marathon run (Kwiecien et al. 2020b). Since the ultimate indicator of post-exercise recovery is the ability of the muscle to produce force (Minett et al. 2014), the ability of PCM to alleviate not only soreness but also strength loss could allow athletes to achieve better performance in subsequent games, matches, or routines. The efficacy of prolonged PCM cooling for accelerating recovery from injury remains to be investigated.
Evidence for the detrimental effects occurring during and from cryotherapy interventions
Inflammation following injury or damaging exercise is both beneficial and detrimental (Chazaud 2020), creating secondary tissue damage while, at the same time, resulting in the structural and functional repair of damaged tissues (Tidball 2005). There is a growing trend throughout the literature recommending against icing so as not to delay or impair the regeneration process or the natural healing response that occurs following injury and exercise (Takagi et al. 2011; White and Wells 2013; Tiidus 2015; Dubois and Esculier 2020). Most recently, the pioneer of the original rest, ice, compression, elevation (RICE) method (Mirkin and Hoffman 1978), rescinded his recommendation of the practice because it may delay healing, instead of facilitating it (Mirkin 2014). The logic behind this theory is that the healing process requires potentiation of the inflammatory response (Smith 1991; Smith et al. 2008; Paulsen et al. 2012). Research in animal models has demonstrated that cryotherapy attenuated neutrophil (Singh et al. 2017) and macrophage infiltration (Takagi et al. 2011; Vieira Ramos et al. 2016; Singh et al. 2017; Miyakawa et al. 2020) to the injured area which might be harmful for muscle regeneration (Kawashima et al. 2021). Dubois and Esculier (2020) suggest that cryotherapy, in particular ice, could potentially disrupt inflammation which may lead to impaired tissue repair and redundant collagen synthesis. However, the only evidence they cite in support of this impaired response comes from animal models (Singh et al. 2017). Other animal models have also demonstrated an exacerbated remodelling phase (excessive collagen response and excessive fibrosis) occurring as a result of acute cryotherapy application (Takagi et al. 2011). By contrast, chronic icing repeated up to 48 h post-injury reduced inflammation but did not influence muscle regeneration or fibrosis (Vieira Ramos et al. 2016). The discrepancy in these results could be due to the acute versus chronic application of cryotherapy, or a result of the different means through which injury was induced (crush injury method, Takagi et al. 2011; freeze injury method to simulate contusion, Vieira Ramos et al. 2016). Notably, both the artificially induced injury and magnitude of cooling that occurred in the animal models of the two aforementioned studies are not and should not be directly comparable to what would occur in humans following injury or exercise. It remains crucial for practitioners and athletes to understand that comparable detrimental effects on the healing processes in humans have not been demonstrated.
It has also recently become evident that cryotherapy, in particular CWI, can have detrimental effects on muscle mass and strength gains (Yamane et al. 2015; Roberts et al. 2015b; Fyfe et al. 2019), and can impair muscle protein synthesis rates (Roberts et al. 2015b; Fuchs et al. 2020) if performed regularly as part of a post-exercise regime. These findings indicate that cryotherapy blunts chronic skeletal muscle adaptations from resistance exercise (Hyldahl and Peake 2020). This effect has recently been attributed to the cryotherapy-induced reduction of intramuscular temperature, which impairs the glutamine-induced anabolic response (Rantala and Chaillou 2019). Others have proposed that the reduction in protein accumulation and protein synthesis within the muscle fibres are a consequence of reduced blood flow to the exercised muscle (Figueiredo and von Walden 2020). An attenuation in the molecular mechanisms regulating resistance training adaptations have also been suggested as one of the proposed mechanisms behind these detrimental effects (Roberts et al. 2015b; Lindsay et al. 2015, 2016; Figueiredo et al. 2016; Broatch et al. 2018; Earp et al. 2019). Specifically, chronic CWI exposures have been shown to effect long-term adaptation to training by suppressing the cellular signalling required for adaptation (Lindsay et al. 2016) and activation and deregulation of the inflammatory process (Lindsay et al. 2015).
While the evidence continues to support the detrimental effects from cryotherapy on chronic adaptation, acute use of cryotherapy (PCM) for 6 consecutive hours did not blunt the naturally occurring adaptive mechanism known as the repeated bout effect (Kwiecien et al. 2020c). Deyhle et al. (2016) recently demonstrated that an initial bout of eccentric exercise resulted in little change to intramuscular markers of inflammation, a second bout, resulted in marked increases in multiple proinflammatory cytokines and significant macrophage and T-cell infiltration. Given this, and since an enhanced and more targeted acute inflammatory response may actually help speed recovery of muscle after repeated bouts of exercise (Hyldahl et al. 2017), it is possible that cryotherapy only blunts the inflammatory response when used following chronic exercise, but not following a single bout of exercise. These findings ultimately suggest that chronic, repeated use of CWI attenuates recovery following traditional resistance training but a single PCM cooling treatment following one exercise bout does not compromise the adaptation that provides protection from damage after a repeated bout of eccentric exercise (the repeated bout effect). Whether or not this effect is related to the amount of area exposed to the cryotherapy stimulus (whole body versus local cooling) remains to be elucidated.
Any detrimental effects from cryotherapy that occur following resistance exercise can be easily avoided if cryotherapy is not implemented during the training or pre-season phase of an athlete season. In fact, cryotherapy should be primarily adopted by athletes during the regular season when anabolic training adaptations are not being induced and the goal of in-season management of the athlete is to facilitate recovery and avoid catabolism following particularly strenuous bouts of exercise. During the in-season or competition scenarios, athletes commonly participate in multiple exercise sessions within a condensed window, often within 24 h. In the event of multiple games occurring within short periods of each other, or an evening game followed by a morning practice, accelerating recovery is a priority over muscle adaptation. The benefits of PCM for providing acute recovery of strength loss might increase an athlete’s total time training or the overall training load in subsequent sessions during intense athlete schedules. Additionally, cryotherapy may be employed at the beginning of pre-season following an initial exercise bout to blunt the damage response to an aggressive return to activity in deconditioned athletes (Kwiecien et al. 2020b). Thereafter it should be removed to optimize pre-season training adaptations until the athlete enters the regular season.
Conclusion
Traditional cryotherapy modalities have generally been shown to provide pain relief when applied following soft tissue injury and to reduce soreness when applied after damaging exercise. The effects on functional recovery and other measures of injury or muscle damage have been mixed. Although cryotherapy remains a widely accepted recovery strategy, and although a plethora of research exists on its use, the current best available evidence is often misunderstood or misconstrued. This has resulted in the end user (clinician, practitioner, and/or athlete) potentially believing in the myths as opposed to understanding the facts surrounding cryotherapy and its application (Table 3). Ultimately, the efficacy of any particular cryotherapy intervention is dependent on the timing and duration of the intervention. The primary goal of cryotherapy should be to maintain a reduction in intramuscular temperature for as long as possible in the immediate stages following both injury and exercise to hinder the proliferation of secondary damage. It is quite possible that cryotherapy’s potential benefits have been limited by the short duration of application with traditional cryotherapy modalities. However, repeated or prolonged cryotherapy is often impractical, may be poorly tolerated, and can pose safety concerns. In this regard, recent studies showing no adverse events indicate that prolonged cooling with PCM may be a safe and practical alternative to traditional short duration cryotherapy modalities. Nevertheless, cryotherapy in any form should not be employed routinely during normal training as it can hinder training adaptations. On the other hand, cryotherapy can and should be implemented as a recovery modality when there is inadequate time for recovery to occur naturally and when subsequent performance could be impaired. Finally, it is noteworthy that while cryotherapy is often applied with the goal of reducing local metabolism and the inflammatory response, there is insufficient supporting evidence for such an effect to occur in humans.
Abbreviations
- CWI:
-
Cold-water immersion
- ICE:
-
Ice compression elevation
- PCM:
-
Phase change material
- WBC:
-
Whole-body cryotherapy
References
Abrams G (1997) Response of the body to injury: inflammation and repair. In: pathophysiology: clinical concepts of disease processes. (5th ed), 38–58
Algafly AA, George KP, Herrington L (2007) The effect of cryotherapy on nerve conduction velocity, pain threshold and pain tolerance * commentary. Br J Sports Med 41(6):365–369. https://doi.org/10.1136/bjsm.2006.031237
Amon M, Menger MD, Vollmar B (2003) Heme oxygenase and nitric oxide synthase mediate cooling-associated protection against TNF-α-induced microcirculatory dysfunction and apoptotic cell death. FASEB J 17(2):175–185. https://doi.org/10.1096/fj.02-0368com
Armstrong RB (1990) Initial events in exercise-induced muscular injury. Med Sci Sports Exerc 22(4):429–435
Armstrong RB, Warren GL, Warren JA (1991) Mechanisms of exercise-induced muscle fibre injury. Sports Med 12(3):184–207
Bailey DM, Erith SJ, Griffin PJ, Dowson A, Brewer DS, Gant N, Williams C (2007) Influence of cold-water immersion on indices of muscle damage following prolonged intermittent shuttle running. J Sports Sci 25(11):1163–1170. https://doi.org/10.1080/02640410600982659
Banfi G, Melegati G, Barassi A, Dogliotti G, Melzi d’Eril G, Dugué B, Corsi MM (2009) Effects of whole-body cryotherapy on serum mediators of inflammation and serum muscle enzymes in athletes. J Therm Biol 34(2):55–59. https://doi.org/10.1016/j.jtherbio.2008.10.003
Banfi G, Lombardi G, Colombini A, Melegati G (2010) Whole-body cryotherapy in athletes. Sports Med 40(6):509–517. https://doi.org/10.2165/11531940-000000000-00000
Barnes L (1979) Cryotherapy—putting injury on ice. Phys Sports Med 7(6):130–136. https://doi.org/10.1080/00913847.1979.11710883
Beiner JM, Jokl P (2001) Muscle contusion injuries: current treatment options. JAAOS 9(4):227–237
Bishop PA, Jones E, Woods AK (2008) Recovery from training: a brief review. J Strength Cond Res 22(3):1015–1024. https://doi.org/10.1519/jsc.0b013e31816eb518
Bleakley CM, Davison G (2010a) Management of acute soft tissue injury using protection rest ice compression and elevation: recommendations from the Association of Chartered Physiotherapists in Sports and Exercise Medicine (ACPSM) [Executive Summary]. Association of Chartered Physiotherapists in Sports and Exercise Medicine, pp 1–24
Bleakley CM, Davison GW (2010b) Cryotherapy and inflammation: evidence beyond the cardinal signs. Phys Ther Rev 15(6):430–435. https://doi.org/10.1179/1743288X10Y.0000000014
Bleakley CM, Hopkins JT (2010) Is it possible to achieve optimal levels of tissue cooling in cryotherapy? Phys Ther Rev 15(4):344–350. https://doi.org/10.1179/174328810x12786297204873
Bleakley CM, McDonough S, MacAuley D (2004) The use of ice in the treatment of acute soft-tissue injury. Am J Sports Med 32(1):251–261. https://doi.org/10.1177/0363546503260757
Bleakley CM, McDonough S, Gardner E, Hopkins JT, Glasgow P, Davison GW, Baxter GD, Hopkins JT, Davison GW (2010) Cold-water immersion (cryotherapy) for preventing and treating muscle soreness after exercise. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.cd008262
Bleakley CM, Glasgow P, MacAuley DC (2012a) PRICE needs updating, should we call the POLICE. Br J Sports Med 46(4):220–221. https://doi.org/10.1136/bjsports-2011-090297
Bleakley CM, Glasgow P, Webb MJ (2012b) Cooling an acute muscle injury: can basic scientific theory translate into the clinical setting? Br J Sports Med 46(4):296–298. https://doi.org/10.1136/bjsm.2011.086116
Bleakley CM, Bieuzen F, Davison GW, Costello JT (2014) Whole-body cryotherapy: empirical evidence and theoretical perspectives. Open Access J Sports Med 5:25–36. https://doi.org/10.2147/OAJSM.S41655
Block J (2010) Cold and compression in the management of musculoskeletal injuries and orthopedic operative procedures: a narrative review. Open Access J Sports Med 1:105. https://doi.org/10.2147/oajsm.s11102
Blondin DP, Labbé SM, Phoenix S, Guérin B, Turcotte EE, Richard D, Carpentier AC, Haman F (2015) Contributions of white and brown adipose tissues and skeletal muscles to acute cold-induced metabolic responses in healthy men. J Physiol 593(3):701–714
Bongers CCWG, Hopman MTE, Eijsvogels TMH (2017) Cooling interventions for athletes: an overview of effectiveness, physiological mechanisms, and practical considerations. Temperature 4(1):60–78
Broatch JR, Petersen A, Bishop DJ (2018) The influence of post-exercise cold-water immersion on adaptive responses to exercise: a review of the literature. Sports Med 48(6):1369–1387. https://doi.org/10.1007/s40279-018-0910-8
Broatch JR, Poignard M, Hausswirth C, Bishop DJ, Bieuzen F (2019) Whole-body cryotherapy does not augment adaptations to high-intensity interval training. Sci Rep 9(1):1–11. https://doi.org/10.1038/s41598-019-48518-1
Brophy-Williams N, Landers G, Wallman K (2011) Effect of immediate and delayed cold water immersion after a high intensity exercise session on subsequent run performance. J Sports Sci Med 10(4):665–670
Brown WC, Hahn DB (2009) Frostbite of the feet after cryotherapy: a report of two cases. J Foot Ankle Surg 48(5):577–580
Brownstein CG, Ansdell P, Škarabot J, McHugh MP, Howatson G, Goodall S, Thomas K (2019) The effect of phase change material on recovery of neuromuscular function following competitive soccer match-play. Front Physiol. https://doi.org/10.3389/fphys.2019.00647
Carvalho N, Puntel G, Correa P, Gubert P, Amaral G, Morais J, Royes L, da Rocha J, Soares F (2010) Protective effects of therapeutic cold and heat against the oxidative damage induced by a muscle strain injury in rats. J Sports Sci 28(9):923–935. https://doi.org/10.1080/02640414.2010.481722
Chazaud B (2020) Inflammation and skeletal muscle regeneration: leave it to the macrophages! Trends Immunol 41(6):481–492. https://doi.org/10.1016/j.it.2020.04.006
Chesterton LS, Foster NE, Ross L (2002) Skin temperature response to cryotherapy. Arch Phys Med Rehabil 83(4):543–549. https://doi.org/10.1053/apmr.2002.30926
Chleboun GS, Howell JN, Baker HL, Ballard TN, Graham JL, Hallman HL, Perkins LE, Schauss JH, Conatser RR (1995) Intermittent pneumatic compression effect on eccentric exercise-induced swelling, stiffness, and strength loss. Arch Phys Med Rehabil 76(8):744–749
Choo HC, Nosaka K, Peiffer JJ, Ihsan M, Yeo CC, Abbiss CR (2018) Peripheral blood flow changes in response to postexercise cold water immersion. Clin Physiol Funct Imaging 38(1):46–55
Ciolek JJ (1985) Cryotherapy. Review of physiological effects and clinical application. Clevel Clin Quart 52(2):193–201. https://doi.org/10.3949/ccjm.52.2.193
Clifford T, Abbott W, Kwiecien SY, Howatson G, McHugh MP (2018) Cryotherapy reinvented: application of phase change material for recovery in elite soccer. Int J Sports Physiol Perform. https://doi.org/10.1123/ijspp.2017-0334
Collins NC (2008) Is ice right? Does cryotherapy improve outcome for acute soft tissue injury? Emerg Med J 25(2):65–68. https://doi.org/10.1136/emj.2007.051664
Corbett J, Barwood MJ, Lunt HC, Milner A, Tipton MJ (2012) Water immersion as a recovery aid from intermittent shuttle running exercise. Eur J Sport Sci 12(6):509–514. https://doi.org/10.1080/17461391.2011.570380
Costello JT, Algar LA, Donnelly AE (2011) Effects of whole-body cryotherapy (−110 °C) on proprioception and indices of muscle damage. Scand J Med Sci Sports 22(2):190–198. https://doi.org/10.1111/j.1600-0838.2011.01292.x
Costello JT, Culligan K, Selfe J, Donnelly AE (2012) Muscle, skin and core temperature after −110 °C cold air and 8 °C water treatment. PLoS ONE 7(11):e48190. https://doi.org/10.1371/journal.pone.0048190
Costello JT, Baker PRA, Minett GM, Bieuzen F, Stewart IB, Bleakley C (2015) Cochrane review: whole-body cryotherapy (extreme cold air exposure) for preventing and treating muscle soreness after exercise in adults. Cochrane Database Syst Rev 9(1):43–44. https://doi.org/10.1111/jebm.12187
de Estéfani D, Ruschel C, Benincá IL, dos Santos Haupenthal DP, de Avelar NCP, Haupenthal A (2019) Volume of water added to crushed ice affects the efficacy of cryotherapy: a randomised, single-blind, crossover trial. Physiotherapy. https://doi.org/10.1016/j.physio.2019.12.005
Deal DN, Tipton J, Rosencrance E, Curl WW, Smith TL (2002) Ice reduces edema: a study of microvascular permeability in rats. J Bone Joint Surg 84(9):1573–1578
Dervin GF, Taylor DE, Keene GCR (1998) Effects of cold and compression dressings on early postoperative outcomes for the arthroscopic anterior cruciate ligament reconstruction patient. J Orthop Sports Phys Ther 27(6):403–406. https://doi.org/10.2519/jospt.1998.27.6.403
Deyhle MR, Gier AM, Evens KC, Eggett DL, Nelson WB, Parcell AC, Hyldahl RD (2016) Skeletal muscle inflammation following repeated bouts of lengthening contractions in humans. Front Physiol 6:424. https://doi.org/10.3389/fphys.2015.00424
Dolan MG, Thornton RM, Fish DR, Mendel FC (1997) Effects of cold water immersion on edema formation after blunt injury to the hind limbs of rats. J Athl Train 32(3):233–237
Dubois B, Esculier JF (2020) Soft-tissue injuries simple need peace and love. Br J Sports Med 54(2):3–5. https://doi.org/10.1136/bjsports-2019-101253
Dupuy O, Douzi W, Theurot D, Bosquet L, Dugué B (2018) An evidence-based approach for choosing post-exercise recovery techniques to reduce markers of muscle damage, soreness, fatigue, and inflammation: a systematic review with meta-analysis. Front Physiol. https://doi.org/10.3389/fphys.2018.00403
Dykstra JH, Hill HM, Miller MG, Cheatham CC, Michael TJ, Baker RJ (2009) Comparisons of cubed ice, crushed ice, and wetted ice on intramuscular and surface temperature changes. J Athl Train 44(2):136–141
Earp JE, Hatfield DL, Sherman A, Lee EC, Kraemer WJ (2019) Cold-water immersion blunts and delays increases in circulating testosterone and cytokines post-resistance exercise. Eur J Appl Physiol 119(8):1901–1907. https://doi.org/10.1007/s00421-019-04178-7
Enoka RM (1996) Eccentric contractions require unique activation strategies by the nervous system. J Appl Physiol 81(6):2339–2346
Enwemeka CS, Allen C, Avila P, Bina J, Konrade J, Munns S (2002) Soft tissue thermodynamics before, during, and after cold pack therapy. Med Sci Sports Exerc 34(1):45–50. https://doi.org/10.1097/00005768-200201000-00008
Eston R, Peters D (1999) Effects of cold water immersion on the symptoms of exercise-induced muscle damage. J Sports Sci 17(3):231–238. https://doi.org/10.1080/026404199366136
Faber JE (1988) Effect of local tissue cooling on microvascular smooth muscle and postjunctional alpha 2-adrenoceptors. Am J Physiol Heart Circulatory Physiol 255(1):H121–H130
Ferreira-Junior JB, Bottaro M, Vieira A, Siqueira AF, Vieira CA, Durigan JLQ, Cadore EL, Coelho LGM, Simões HG, Bemben MG (2015) One session of partial-body cryotherapy (− 110 °C) improves muscle damage recovery. Scand J Med Sci Sports 25(5):e524-530. https://doi.org/10.1111/sms.12353
Figueiredo VC, von Walden F (2020) Freezing translation at multiple levels one session at a time. J Physiol 598(8):1441–1442
Figueiredo VC, Roberts LA, Markworth JF, Barnett MPG, Coombes JS, Raastad T, Peake JM, Cameron-Smith D (2016) Impact of resistance exercise on ribosome biogenesis is acutely regulated by post-exercise recovery strategies. Physiol Rep 4(2):e12670. https://doi.org/10.14814/phy2.12670
Fiscus KA, Kaminski TW, Powers ME (2005) Changes in lower-leg blood flow during warm, cold, and contrast-water therapy. Arch Phys Med Rehabil 86(7):1404–1410. https://doi.org/10.1016/j.apmr.2004.11.046
Fonda B, Sarabon N (2013) Effects of whole-body cryotherapy on recovery after hamstring damaging exercise: a crossover study. Scand J Med Sci Sports. https://doi.org/10.1111/sms.12074
Fragala MS, Jajtner AR, Townsend JR, Gonzalez AM, Wells AJ, Oliveira LP, Hoffman JAYR, Stout JR, Fukuda DH (2015) Leukocyte IGF-1 receptor expression during muscle recovery. Med Sci Sports Exerc 47(1):92–99. https://doi.org/10.1249/mss.0000000000000392
Freitag L, Clijsen R, Deflorin C, Taube W, Hohenauer E (2021) Intramuscular temperature changes in the quadriceps femoris muscle after post-exercise cold-water immersion (10°C for 10 min): a systematic review with meta-analysis. Front Sports Act Living. https://doi.org/10.3389/fspor.2021.660092
Fuchs CJ, Kouw IWK, Churchward-Venne TA, Smeets JSJ, Senden JM, van Marken Lichtenbelt WD, Verdijk LB, van Loon LJC (2020) Postexercise cooling impairs muscle protein synthesis rates in recreational athletes. J Physiol 598(4):755–772
Fuhrman GJ (1959) Oxygen consumption of animals and tissues as a function of temperature. J Gen Physiol 42(4):715–722. https://doi.org/10.1085/jgp.42.4.715
Fuhrman FA, Fuhrman GJ, Farr DA, Fail JH (1961) Relationship between tissue respiration and total metabolic rate in hypo and normothermic rats. Am J Physiol Legacy Content 201(2):231–234. https://doi.org/10.1152/ajplegacy.1961.201.2.231
Fyfe JJ, Broatch JR, Trewin AJ, Hanson ED, Argus CK, Garnham AP, Halson SL, Polman RC, Bishop DJ, Petersen AC (2019) Cold water immersion attenuates anabolic signalling and skeletal muscle fiber hypertrophy, but not strength gain, following whole-body resistance training. J Appl Physiol. https://doi.org/10.1152/japplphysiol.00127.2019
Gage AA (1979) Cryo corner: what temperature is lethal for cells? J Dermatol Surg Oncol 5(6):459–464. https://doi.org/10.1111/j.1524-4725.1979.tb00695.x
Garcia C, da Mota G, Marocolo M (2016) Cold water immersion is acutely detrimental but increases performance post-12 h in rugby players. Int J Sports Med 37(08):619–624. https://doi.org/10.1055/s-0035-1565200
Gillette CM, Merrick MA (2018) The effect of elevation on intramuscular tissue temperatures. J Sport Rehabil 27(6):526–529. https://doi.org/10.1123/jsr.2016-0239
Gonzalez AM, Stout JR, Jajtner AR, Townsend JR, Wells AJ, Beyer KS, Boone CH, Pruna GJ, Mangine GT, Scanlon TM, Bohner JD, Oliveira LP, Fragala MS, Hoffman JR (2014) Effects of β-hydroxy-β-methylbutyrate free acid and cold water immersion on post-exercise markers of muscle damage. Amino Acids 46(6):1501–1511. https://doi.org/10.1007/s00726-014-1722-2
Grant AE (1964) Massage with ice (cryokinetics) in the treatment of painful conditions of the musculoskeletal system. Arch Phys Med Rehabil 45:233–238
Greenfield A (1963) The circulation through the skin. Circulation 2:1325–1351
Gregson W, Black MA, Jones H, Milson J, Morton J, Dawson B, Atkinson G, Green DJ (2011) Influence of cold water immersion on limb and cutaneous blood flow at rest. Am J Sports Med 39(6):1316–1323. https://doi.org/10.1177/0363546510395497
Gregson W, Allan R, Holden S, Phibbs P, Doran D, Campbell I, Waldron S, Joo C, Morton J (2013) Postexercise cold-water immersion does not attenuate muscle glycogen resynthesis. Med Sci Sports Exerc 45(6):1174–1181. https://doi.org/10.1249/MSS.0b013e3182814462
Guilhem G, Hug F, Couturier A, Regnault S, Bournat L, Filliard J-R, Dorel S (2013) Effects of air-pulsed cryotherapy on neuromuscular recovery subsequent to exercise-induced muscle damage. Am J Sports Med 41(8):1942–1951. https://doi.org/10.1177/0363546513490648
Gulick DT, Kimura IF, Sitler M, Paolone A, Kelly JD (1996) Various treatment techniques on signs and symptoms of delayed onset muscle soreness. J Athl Train 31(2):145–152
Halson SL, Quod MJ, Martin DT, Gardner AS, Ebert TR, Laursen PB (2008) Physiological responses to cold water immersion following cycling in the heat. Int J Sports Physiol Perform 3(3):331–346. https://doi.org/10.1123/ijspp.3.3.331
Hausswirth C, Le Meur Y (2011) Physiological and nutritional aspects of post-exercise recovery. Sports Med 41(10):861–882. https://doi.org/10.2165/11593180-000000000-00000
Hausswirth C, Louis J, Bieuzen F, Pournot H, Fournier J, Filliard J-R, Brisswalter J (2011) Effects of whole-body cryotherapy vs far-infrared vs passive modalities on recovery from exercise-induced muscle damage in highly-trained runners. PLoS ONE 6(12):e27749. https://doi.org/10.1371/journal.pone.0027749
Hayden CA (1964) Cryokinetics in an early treatment program. Phys Ther 44:990–993. https://doi.org/10.1093/ptj/44.11.990
Ho SS, Illgen RL, Meyer RW, Torok PJ, Cooper MD, Reider B (1995) Comparison of various icing times in decreasing bone metabolism and blood flow in the knee. Am J Sports Med 23(1):74–76. https://doi.org/10.1177/036354659502300112
Hohenauer E, Taeymans J, Baeyens J-P, Clarys P, Clijsen R (2015) The effect of post-exercise cryotherapy on recovery characteristics: a systematic review and meta-analysis. PLoS ONE 10(9):e0139028. https://doi.org/10.1371/journal.pone.0139028
Howatson G, Van Someren KA (2003) Ice massage: effects on exercise-induced muscle damage. J Sports Med Phys Fitness 43(4):500–505
Howatson G, van Someren KA (2008) The prevention and treatment of exercise-induced muscle damage. Sports Med 38(6):483–503. https://doi.org/10.2165/00007256-200838060-00004
Howatson G, Gaze D, van Someren KA (2005) The efficacy of ice massage in the treatment of exercise-induced muscle damage. Scand J Med Sci Sports 15(6):416–422. https://doi.org/10.1111/j.1600-0838.2005.00437.x
Huard J, Li Y, Fu FH (2002) Muscle injuries and repair: current trends in research. J Bone Joint Surg 84(5):822–832
Hubbard TJ, Denegar CR (2004) Does cryotherapy improve outcomes with soft tissue injury? J Athl Train 39(3):278–279
Hyldahl RD, Peake JM (2020) Combining cooling or heating applications with exercise training to enhance performance and muscle adaptations. J Appl Physiol 129(2):353–365
Hyldahl RD, Chen TC, Nosaka K (2017) Mechanisms and mediators of the skeletal muscle repeated bout effect. Exerc Sport Sci Rev 45(1):24–33. https://doi.org/10.1249/jes.0000000000000095
Ihsan M, Watson G, Lipski M, Abbiss CR (2013) Influence of postexercise cooling on muscle oxygenation and blood volume changes. Med Sci Sports Exerc 45(5):876–882. https://doi.org/10.1249/mss.0b013e31827e13a2
Ihsan M, Watson G, Abbiss CR (2016) What are the physiological mechanisms for post-exercise cold water immersion in the recovery from prolonged endurance and intermittent exercise? Sports Med 46(8):1095–1109. https://doi.org/10.1007/s40279-016-0483-3
Ingram J, Dawson B, Goodman C, Wallman K, Beilby J (2009) Effect of water immersion methods on post-exercise recovery from simulated team sport exercise. J Sci Med Sport 12(3):417–421. https://doi.org/10.1016/j.jsams.2007.12.011
Isabell WK, Durrant E, Myrer W, Anderson S (1992) The effects of ice massage, ice massage with exercise, and exercise on the prevention and treatment of delayed onset muscle soreness. J Athl Train 27(3):208–217
Jajtner AR, Hoffman JR, Gonzalez AM, Worts PR, Fragala MS, Stout JR (2015) Comparison of the effects of electrical stimulation and cold-water immersion on muscle soreness after resistance exercise. J Sport Rehabil 24(2):99–108. https://doi.org/10.1123/jsr.2013-0113
Janwantanakul P (2004) Different rate of cooling time and magnitude of cooling temperature during ice bag treatment with and without damp towel wrap. Phys Ther Sport 5(3):156–161
Janwantanakul P (2009) The effect of quantity of ice and size of contact area on ice pack/skin interface temperature. Physiotherapy 95(2):120–125. https://doi.org/10.1016/j.physio.2009.01.004
Järvinen TAH, Järvinen TLN, Kääriäinen M, Kalimo H, Järvinen M (2005) Muscle injuries: biology and treatment. Am J Sports Med 33(5):745–764. https://doi.org/10.1177/0363546505274714
Jutte LS, Merrick MA, Ingersoll CD, Edwards JE (2001) The relationship between intramuscular temperature, skin temperature, and adipose thickness during cryotherapy and rewarming. Arch Phys Med Rehabil 82(6):845–850. https://doi.org/10.1053/apmr.2001.23195
Kawashima M, Kawanishi N, Tominaga T, Suzuki K, Miyazaki A, Nagata I, Miyoshi M, Miyakawa M, Sakuraya T, Sonomura T, Arakawa T (2021) Icing after eccentric contraction-induced muscle damage perturbs the disappearance of necrotic muscle fibers and phenotypic dynamics of macrophages in mice. J Appl Physiol. https://doi.org/10.1152/japplphysiol.01069.2020
Kendall B, Eston R (2002) Exercise-induced muscle damage and the potential protective role of estrogen. Sports Med 32(2):103–123. https://doi.org/10.2165/00007256-200232020-00003
Kennet J, Hardaker N, Hobbs S, Selfe J (2007) Cooling efficiency of 4 common cryotherapeutic agents. J Athl Train 42(3):343
Knight KL (1976) Effects of hypothermia on inflammation and swelling. Athl Train 11:7–10
Knight KL (1985) Cryotherapy: theory, technique, and physiology. Chattanooga Corp., Education Division
Knight KL (1995) Cryotherapy in sport injury management. Human Kinetics
Knight KL, Brucker JB, Stoneman PD, Rubley MD (2000) Muscle injury management with cryotherapy. Athlet Ther Today 5(4):26–30. https://doi.org/10.1123/att.5.4.26
Kovacs MS, Baker LB (2014) Recovery interventions and strategies for improved tennis performance. Br J Sports Med 48(Suppl 1):i18–i21. https://doi.org/10.1136/bjsports-2013-093223
Kowalski GM, Bruce CR (2014) The regulation of glucose metabolism: implications and considerations for the assessment of glucose homeostasis in rodents. Am J Physiol Endocrinol Metabol 307(10):E859–E871. https://doi.org/10.1152/ajpendo.00165.2014
Krueger M, Costello JT, Achtzehn S, Dittmar K-H, Mester J (2019) Whole-body cryotherapy (− 110 °C) following high-intensity intermittent exercise does not alter hormonal, inflammatory or muscle damage biomarkers in trained males. Cytokine 113:277–284. https://doi.org/10.1016/j.cyto.2018.07.018
Krüger M, de Mareés M, Dittmar K-H, Sperlich B, Mester J (2015) Whole-body cryotherapy’s enhancement of acute recovery of running performance in well-trained athletes. Int J Sports Physiol Perform 10(5):605–612. https://doi.org/10.1123/ijspp.2014-0392
Kwiecien SY, McHugh MP, Howatson G (2018) The efficacy of cooling with phase change material for the treatment of exercise-induced muscle damage: pilot study. J Sports Sci 36(4):407–413. https://doi.org/10.1080/02640414.2017.1312492
Kwiecien SY, Mathew S, Howatson G, McHugh MP (2019a) The effect of varying degrees of compression from elastic vs plastic wrap on quadriceps intramuscular temperature during wetted ice application. SMS 29(8):13430. https://doi.org/10.1111/sms.13430
Kwiecien SY, McHugh MP, Goodall S, Hicks KM, Hunter AM, Howatson G (2019b) Exploring the efficacy of a safe cryotherapy alternative: physiological temperature changes from cold-water immersion versus prolonged cooling of phase-change material. Int J Sports Physiol Perform. https://doi.org/10.1123/ijspp.2018-0763
Kwiecien SY, O’Hara DJ, McHugh MP, Howatson G (2020c) Prolonged cooling with phase change material enhances recovery and does not affect the subsequent repeated bout effect following exercise. Eur J Appl Physiol 120(2):413–423. https://doi.org/10.1007/s00421-019-04285-5
Kwiecien SY, Mchugh MP, Howatson G (2020a) Don’t Lose Your Cool with Cryotherapy: the application of phase change material for prolonged cooling in athletic recovery and beyond. Front Sports Act Living. https://doi.org/10.3389/fspor.20.00118
Kwiecien SY, McHugh MP, Hicks KM, Keane KM, Howatson G (2020b) Prolonging the duration of cooling does not enhance recovery following a marathon. Scand J Med Sci Sports. https://doi.org/10.1111/sms.13822
Lane KN, Wenger HA (2004) Effect of selected recovery conditions on performance of repeated bouts of intermittent cycling separated by 24 hours. J Strength Condition Res 18(4):855. https://doi.org/10.1519/14183.1
Lapointe BM, Frenette J, Côté CH (2002) Lengthening contraction-induced inflammation is linked to secondary damage but devoid of neutrophil invasion. J Appl Physiol 92(5):1995–2004
Lee H, Natsui H, Akimoto T, Yanagi K, Ohshima N, Kono I (2005) Effects of cryotherapy after contusion using real-time intravital microscopy. Med Sci Sports Exerc 37(7):1093–1098. https://doi.org/10.1249/01.mss.0000169611.21671.2e
Leeder JDC, Gissane C, van Someren K, Gregson W, Howatson G (2012) Cold water immersion and recovery from strenuous exercise: a meta-analysis. Br J Sports Med 46(4):233–240. https://doi.org/10.1136/bjsports-2011-090061
Leeder JDC, Godfrey M, Gibbon D, Gaze D, Davison GW, van Someren KA, Howatson G (2019) Cold water immersion improves recovery of sprint speed following a simulated tournament. Eur J Sport Sci. https://doi.org/10.1080/17461391.2019.1585478
Lieber RL (2018) Biomechanical response of skeletal muscle to eccentric contractions. J Sport Health Sci 7(3):294–309. https://doi.org/10.1016/j.jshs.2018.06.005
Lindsay A, Carr S, Othman MI, Marks E, Davies S, Petersen C, Draper N, Gieseg SP (2015) The physiological and mononuclear cell activation response to cryotherapy following a mixed martial arts contest: a pilot study. Pteridines. https://doi.org/10.1515/pterid-2015-0010
Lindsay A, Othman MI, Prebble H, Davies S, Gieseg SP (2016) Repetitive cryotherapy attenuates the in vitro and in vivo mononuclear cell activation response. Exp Physiol 101(7):851–865. https://doi.org/10.1113/EP085795
Mac Auley DC (2001) Ice therapy: how good is the evidence? Int J Sports Med 22(5):379–384. https://doi.org/10.1055/s-2001-15656
Machado AF, Ferreira PH, Micheletti JK, de Almeida AC, Lemes ÍR, Vanderlei FM, Netto Junior J, Pastre CM (2015) Can water temperature and immersion time influence the effect of cold water immersion on muscle soreness? A systematic review and meta-analysis. Sports Med 46(4):503–514. https://doi.org/10.1007/s40279-015-0431-7
Machado AF, Almeida AC, Micheletti JK, Vanderlei FM, Tribst MF, Netto Junior J, Pastre CM (2016) Dosages of cold-water immersion post exercise on functional and clinical responses: a randomized controlled trial. Scand J Med Sci Sports 27(11):1356–1363. https://doi.org/10.1111/sms.12734
Mawhinney C, Jones H, Joo CH, Low DA, Green DJ, Gregson W (2013) Influence of cold-water immersion on limb and cutaneous blood flow after exercise. Med Sci Sports Exerc 45(12):2277–2285. https://doi.org/10.1249/mss.0b013e31829d8e2e
Mawhinney C, Low DA, Jones H, Green DJ, Costello JT, Gregson W (2017) Cold water mediates greater reductions in limb blood flow than whole body cryotherapy. Med Sci Sports Exerc 49(6):1252–1260. https://doi.org/10.1249/mss.0000000000001223
Mawhinney C, Heinonen I, Low DA, Han C, Jones H, Kalliokoski KK, Kirjavainen A, Kemppainen J, Di Salvo V, Weston M, Cable T, Gregson W (2020) Changes in quadriceps femoris muscle perfusion following different degrees of cold-water immersion. J Appl Physiol. https://doi.org/10.1152/japplphysiol.00833.2019
McArdle A, Jackson MJ (1997) Intracellular mechanisms involved in skeletal muscle damage. Oxford Medical Publications, NY
Meeusen R, Lievens P (1986) The use of cryotherapy in sports injuries. Sports Med 3(6):398–414. https://doi.org/10.2165/00007256-198603060-00002
Meeusen R, Joos E, Roeykens J, Bossuyt A, De KM (1998) The influence of cold and compression on lymph flow at the ankle. Clin J Sport Med 8(4):266–271
Merrick MA (2002) Secondary injury after musculoskeletal trauma: a review and update. J Athl Train 37(2):209–217
Merrick MA (2013) Cold water immersion to improve postexercise recovery: a meta-analysis. Clin J Sport Med 23(3):242–243
Merrick MA, McBrier NM (2010) Progression of secondary injury after musculoskeletal trauma—a window of opportunity? J Sport Rehabil 19(4):380–388. https://doi.org/10.1123/jsr.19.4.380
Merrick MA, Knight KL, Ingersoll CD, Potteiger JA (1993) The effects of ice and compression wraps on intramuscular temperatures at various depths. J Athl Train 28(3):236–245
Merrick MA, Rankin JM, Andres FA, Hinman CL (1999) A preliminary examination of cryotherapy and secondary injury in skeletal muscle. Med Sci Sports Exerc 31(11):1516. https://doi.org/10.1097/00005768-199911000-00004
Merrick MA, Jutte LS, Smith ME (2003) Cold modalities with different thermodynamic properties produce different surface and intramuscular temperatures. J Athl Train 38(1):28–33
Michlovitz SL (1990) Thermal agents in rehabilitation. Davis Company, Davis
Minett GM, Duffield R, Billaut F, Cannon J, Portus MR, Marino FE (2014) Cold-water immersion decreases cerebral oxygenation but improves recovery after intermittent-sprint exercise in the heat. Scand J Med Sci Sports 24(4):656–666. https://doi.org/10.1111/sms.12060
Mirkin G (2014) Why ice delays recovery [online] (pp 1–2)
Mirkin G, Hoffman M (1978) The sports medicine book. Little Brown
Miyakawa M, Kawashima M, Haba D, Sugiyama M, Taniguchi K, Arakawa T (2020) Inhibition of the migration of MCP-1 positive cells by icing applied soon after crush injury to rat skeletal muscle. Acta Histochem 122(3):151511. https://doi.org/10.1016/j.acthis.2020.151511
Montgomery PG, Pyne DB, Hopkins WG, Dorman JC, Cook K, Minahan CL (2008) The effect of recovery strategies on physical performance and cumulative fatigue in competitive basketball. J Sports Sci 26(11):1135–1145. https://doi.org/10.1080/02640410802104912
Mullaney MJ, McHugh MP, Kwiecien SY, Ioviero N, Fink A, Howatson G (2020) Accelerated muscle recovery in baseball pitchers using phase change material cooling. Med Sci Sports Exerc. https://doi.org/10.1249/mss.0000000000002447
Murgier J, Cassard X (2014) Cryotherapy with dynamic intermittent compression for analgesia after anterior cruciate ligament reconstruction preliminary study. Orthop Traumatol 100(3):309–312. https://doi.org/10.1016/j.otsr.2013.12.019
Myrer JW, Measom G, Fellingham GW (1998) Temperature changes in the human leg during and after two methods of cryotherapy. J Athl Train 33(1):25–29
Myrer WJ, Myrer KA, Measom GJ, Fellingham GW, Evers SL (2001) Muscle temperature is affected by overlying adipose when cryotherapy is administered. J Athl Train 36(1):32–36
Nédélec M, McCall A, Carling C, Legall F, Berthoin S, Dupont G (2012) Recovery in soccer. Sports Med 43(1):9–22. https://doi.org/10.1007/s40279-012-0002-0
Nogueira NM, Felappi CJ, Lima CS, Medeiros DM (2019) Effects of local cryotherapy for recovery of delayed onset muscle soreness and strength following exercise-induced muscle damage: systematic review and meta-analysis. Sport Sci Health. https://doi.org/10.1007/s11332-019-00571-z
Oakley ET, Pardeiro RB, Powell JW, Millar AL (2013) The effects of multiple daily applications of ice to the hamstrings on biochemical measures, signs, and symptoms associated with exercise-induced muscle damage. J Strength Cond Res 27(10):2743–2751. https://doi.org/10.1519/jsc.0b013e31828830df
Osterman AL, Heppenstall RB, Sapega AA, Katz M, Chance B, Sokolow D (1984) Muscle Ischemia and Hypothermia: a bioenergetic study using 31phosphorus nuclear magnetic resonance spectroscopy. J Trauma 24(9):811–817. https://doi.org/10.1097/00005373-198409000-00006
Otte JW, Merrick MA, Ingersoll CD, Cordova ML (2002) Subcutaneous adipose tissue thickness alters cooling time during cryotherapy. Arch Phys Med Rehabil 83(11):1501–1505. https://doi.org/10.1053/apmr.2002.34833
Page P (2018) To ice or not to ice: that is the question|cramer sports medicine. https://www.cramersportsmed.com/first-aider/to-ice-or-not-to-ice-that-is-the-question.html
Palmer JE, Knight KL (1996) Ankle and thigh skin surface temperature changes with repeated ice pack application. J Athl rain 31(4):319
Paulsen G, Mikkelsen UR, Raastad T, Peake JM (2012) Leucocytes, cytokines and satellite cells: what role do they play in muscle damage and regeneration following eccentric exercise? Exerc Immunol Rev 18:42–97
Peake JM (2019) Recovery after exercise: what is the current state of play? Curr Opin Physio 10:17–26
Peake J, Nosaka KK, Suzuki K (2005) Characterization of inflammatory responses to eccentric exercise in humans. Exerc Immunol Rev 11:64–85
Peake JM, Roberts LA, Figueiredo VC, Egner I, Krog S, Aas SN, Suzuki K, Markworth JF, Coombes JS, Cameron-Smith D, Raastad T (2016) The effects of cold water immersion and active recovery on inflammation and cell stress responses in human skeletal muscle after resistance exercise. J Physiol 595(3):695–711. https://doi.org/10.1113/jp272881
Peiffer JJ, Abbiss CR, Nosaka K, Peake JM, Laursen PB (2009a) Effect of cold water immersion after exercise in the heat on muscle function, body temperatures, and vessel diameter. J Sci Med Sport 12(1):91–96. https://doi.org/10.1016/j.jsams.2007.10.011
Peiffer JJ, Abbiss CR, Watson G, Nosaka K, Laursen PB (2009b) Effect of cold-water immersion duration on body temperature and muscle function. J Sports Sci 27(10):987–993. https://doi.org/10.1080/02640410903207424
Peiffer JJ, Abbiss CR, Watson G, Nosaka K, Laursen PB (2010) Effect of a 5-min cold-water immersion recovery on exercise performance in the heat. Br J Sports Med 44(6):461–465. https://doi.org/10.1136/bjsm.2008.048173
Pointon M, Duffield R (2012) Cold water immersion recovery after simulated collision sport exercise. Med Sci Sports Exerc 44(2):206–216. https://doi.org/10.1249/mss.0b013e31822b0977
Pointon M, Duffield R, Cannon J, Marino FE (2011) Cold water immersion recovery following intermittent-sprint exercise in the heat. Eur J Appl Physiol 112(7):2483–2494. https://doi.org/10.1007/s00421-011-2218-3
Poppendieck W, Faude O, Wegmann M, Meyer T (2013) Cooling and performance recovery of trained athletes: a meta-analytical review. Int J Sports Physiol Perform 8(3):227–242. https://doi.org/10.1123/ijspp.8.3.227
Pournot H, Bieuzen F, Duffield R, Lepretre P-M, Cozzolino C, Hausswirth C (2010) Short term effects of various water immersions on recovery from exhaustive intermittent exercise. Eur J Appl Physiol 111(7):1287–1295. https://doi.org/10.1007/s00421-010-1754-6
Pournot H, Bieuzen F, Louis J, Fillard J-R, Barbiche E, Hausswirth C (2011) Time-course of changes in inflammatory response after whole-body cryotherapy multi exposures following severe exercise. PLoS ONE 6(7):e22748. https://doi.org/10.1371/journal.pone.0022748
Pugh LG, Edholm OG, Fox RH, Wolff HS, Hervey GR, Hammond WH, Tanner JM, Whitehouse RH (1960) A physiological study of channel swimming. Clin Sci 19:257–273
Puntel GO, Carvalho NR, Dobrachinski F, Salgueiro ACF, Puntel RL, Folmer V, Barbosa NBV, Royes LFF, Rocha JBT, Soares FAA (2012) Cryotherapy reduces skeletal muscle damage after ischemia/reperfusion in rats. J Anat 222(2):223–230. https://doi.org/10.1111/joa.12009
Rantala R, Chaillou T (2019) Mild hypothermia affects the morphology and impairs glutamine-induced anabolic response in human primary myotubes. Am J Physiol Cell Physiol 317(1):C101–C110
Rivenburgh DW (1992) Physical modalities in the treatment of tendon injuries. Clin Sports Med 11(3):645–659
Roberts LA, Nosaka K, Coombes JS, Peake JM (2014) Cold water immersion enhances recovery of submaximal muscle function after resistance exercise. Am J Physiol Reg Integr Comp Physiol 307(8):R998–R1008. https://doi.org/10.1152/ajpregu.00180.2014
Roberts LA, Muthalib M, Stanley J, Lichtwark G, Nosaka K, Coombes JS, Peake JM (2015a) Effects of cold water immersion and active recovery on hemodynamics and recovery of muscle strength following resistance exercise. Am J Physiol Reg Integr Comp Physiol 309(4):R389–R398. https://doi.org/10.1152/ajpregu.00151.2015
Roberts LA, Raastad T, Markworth JF, Figueiredo VC, Egner IM, Shield A, Cameron-Smith D, Coombes JS, Peake JM (2015b) Post-exercise cold water immersion attenuates acute anabolic signalling and long-term adaptations in muscle to strength training. J Physiol 593(18):4285–4301. https://doi.org/10.1113/jp270570
Robson-Ansley PJ, Gleeson M, Ansley L (2009) Fatigue management in the preparation of olympic athletes. J Sports Sci 27(13):1409–1420. https://doi.org/10.1080/02640410802702186
Rose C, Edwards KM, Siegler JC, Graham K, Caillaud C (2017) Whole-body cryotherapy as a recovery technique after exercise: a review of the literature. Int J Sports Med 38(14):1049–1060
Rowsell GJ, Coutts AJ, Reaburn P, Hill-Haas S (2009) Effects of cold-water immersion on physical performance between successive matches in high-performance junior male soccer players. J Sports Sci 27(6):565–573. https://doi.org/10.1080/02640410802603855
Rowsell GJ, Coutts AJ, Reaburn P, Hill-Haas S (2011) Effect of post-match cold-water immersion on subsequent match running performance in junior soccer players during tournament play. J Sports Sci 29(1):1–6. https://doi.org/10.1080/02640414.2010.512640
Sapega AA, Heppenstall RB, Sokolow DP, Graham TJ, Maris JM, Ghosh AK, Chance B, Osterman AL (1988) The bioenergetics of preservation of limbs before replantation. The rationale for intermediate hypothermia. J Bone Joint Surg 70(10):1500–1513. https://doi.org/10.2106/00004623-198870100-00010
Schaser KD, Stover JF, Melcher I, Lauffer A, Haas NP, Bail HJ, Stöckle U, Puhl G, Mittlmeier TW (2006) Local cooling restores microcirculatory hemodynamics after closed soft-tissue trauma in rats. J Trauma 61(3):642–649. https://doi.org/10.1097/01.ta.0000174922.08781.2f
Schaser KD, Disch AC, Stover JF, Lauffer A, Bail HJ, Mittlmeier T (2007) Prolonged superficial local cryotherapy attenuates microcirculatory impairment, regional inflammation, and muscle necrosis after closed soft tissue injury in rats. Am J Sports Med 35(1):93–102. https://doi.org/10.1177/0363546506294569
Schröder D, Pässler HH (1994) Combination of cold and compression after knee surgery—a prospective randomized study. Knee Surg Sports Traumatol Arthrosc 2(3):158–165. https://doi.org/10.1007/BF01467918
Selfe J, Hardaker N, Whitaker J, Hayes C (2007) Thermal imaging of an ice burn over the patella following clinically relevant cryotherapy application during a clinical research study. Phys Ther Sport 8(3):153–158. https://doi.org/10.1016/j.ptsp.2007.04.001
Selkow NM (2019) Cooling of lower extremity muscles according to subcutaneous tissue thickness. J Athl Train 54(12):1304–1307. https://doi.org/10.4085/1062-6050-550-18
Selkow NM, Day C, Liu Z, Hart JM, Hertel JAY, Saliba SA (2012) Microvascular perfusion and intramuscular temperature of the calf during cooling. Med Sci Sports Exerc 44(5):850–856. https://doi.org/10.1249/mss.0b013e31823bced9
Singh DP, Barani Lonbani Z, Woodruff MA, Parker TJ, Steck R, Peake JM (2017) Effects of topical icing on inflammation, angiogenesis, revascularization, and myofiber regeneration in skeletal muscle following contusion injury. Front Physiol. https://doi.org/10.3389/fphys.2017.00093
Siqueira AF, Vieira A, Bottaro M, Ferreira-Júnior JB, Nóbrega O, Souza VC, Marqueti RC, Babault N, Durigan JLQ (2018) Multiple cold-water immersions attenuate muscle damage but not alter systemic inflammation and muscle function recovery: a parallel randomized controlled trial. Sci Rep 8(1):10961. https://doi.org/10.1038/s41598-018-28942-5
Smith LL (1991) Acute inflammation. Med Sci Sports Exerc 23(5):542–551. https://doi.org/10.1249/00005768-199105000-00006
Smith TL, Curl WW, Smith BP, Holden MB, Wise T, Marr A, Andrew Koman L (1993) New skeletal muscle model for the longitudinal study of alterations in microcirculation following contusion and cryotherapy. Microsurgery 14(8):487–493. https://doi.org/10.1002/micr.1920140805
Smith C, Kruger MJ, Smith RM, Myburgh KH (2008) The inflammatory response to skeletal muscle injury: illuminating complexities. Sports Med 38(11):947–969. https://doi.org/10.2165/00007256-200838110-00005
Stephens JM, Halson S, Miller J, Slater GJ, Askew CD (2017) Cold-water immersion for athletic recovery: one size does not fit all. Int J Sports Physiol Perform 12(1):2–9. https://doi.org/10.1123/ijspp.2016-0095
Stephens JM, Halson SL, Miller J, Slater GJ, Askew CD (2018) Influence of body composition on physiological responses to post-exercise hydrotherapy. J Sports Sci 36(9):1044–1053. https://doi.org/10.1080/02640414.2017.1355062
Stocks JM, Patterson MJ, Hyde DE, Jenkins AB, Mittleman KD, Taylor NAS (2004) Effects of immersion water temperature on wholebody fluid distribution in humans. Acta Physiol Scand 182(1):3–10. https://doi.org/10.1111/j.1365-201x.2004.01302.x
Swenson C, Swärd L, Karlsson J (2007) Cryotherapy in sports medicine. Scand J Med Sci Sports 6(4):193–200. https://doi.org/10.1111/j.1600-0838.1996.tb00090.x
Takagi R, Fujita N, Arakawa T, Kawada S, Ishii N, Miki A (2011) Influence of icing on muscle regeneration after crush injury to skeletal muscles in rats. J Appl Physiol 110(2):382–388. https://doi.org/10.1152/japplphysiol.01187.2010
Tee JC, Bosch AN, Lambert MI (2007) Metabolic consequences of exercise-induced muscle damage. Sports Med 37(10):827–836. https://doi.org/10.2165/00007256-200737100-00001
Tidball JG (2005) Inflammatory processes in muscle injury and repair. Am J Physiol Reg Integr Compar Physiol 288(2):R345–R353. https://doi.org/10.1152/ajpregu.00454.2004
Tiidus PM (2015) Alternative treatments for muscle injury: massage, cryotherapy, and hyperbaric oxygen. Curr Rev Musculoskelet Med 8(2):162–167. https://doi.org/10.1007/s12178-015-9261-3
Tipton MJ, Collier N, Massey H, Corbett J, Harper M (2017) Cold water immersion: kill or cure? Exp Physiol 102(11):1335–1355. https://doi.org/10.1113/EP086283
Tomchuk D, Rubley MD, Holcomb WR, Guadagnoli M, Tarno JM (2010) The magnitude of tissue cooling during cryotherapy with varied types of compression. J Athl Train 45(3):230–237. https://doi.org/10.4085/1062-6050-45.3.230
Tseng C-Y, Lee J-P, Tsai Y-S, Lee S-D, Kao C-L, Liu T-C, Lai C-H, Harris MB, Kuo C-H (2013) Topical cooling (icing) delays recovery from eccentric exercise-induced muscle damage. J Strength Cond Res 27(5):1354–1361. https://doi.org/10.1519/jsc.0b013e318267a22c
Vaile J, Halson S, Gill N, Dawson B (2007) Effect of hydrotherapy on the signs and symptoms of delayed onset muscle soreness. Eur J Appl Physiol 102(4):447–455. https://doi.org/10.1007/s00421-007-0605-6
Vaile J, Halson S, Gill N, Dawson B (2008) Effect of cold water immersion on repeat cycling performance and thermoregulation in the heat. J Sports Sci 26(5):431–440. https://doi.org/10.1080/02640410701567425
Vaile J, O’Hagan C, Stefanovic B, Walker M, Gill N, Askew CD (2010) Effect of cold water immersion on repeated cycling performance and limb blood flow. Br J Sports Med 45(10):825–829. https://doi.org/10.1136/bjsm.2009.067272
Versey N, Halson S, Dawson B (2011) Effect of contrast water therapy duration on recovery of cycling performance: a dose-response study. Eur J Appl Physiol 111(1):37–46. https://doi.org/10.1007/s00421-010-1614-4
Versey NG, Halson SL, Dawson BT (2013) Water immersion recovery for athletes: effect on exercise performance and practical recommendations. Sports Med 43(11):1101–1130. https://doi.org/10.1007/s40279-013-0063-8
Vieira A, Oliveira AB, Costa R, Herrera E, Salvini T (2013) Cold modalities with different thermodynamic properties have similar effects on muscular performance and activation. Int J Sports Med 34(10):873–880. https://doi.org/10.1055/s-0032-1333283
Vieira A, Bottaro M, Ferreira-Junior JB, Vieira C, Cleto VA, Cadore EL, Simões HG, Carmo JD, Brown LE (2015) Does whole-body cryotherapy improve vertical jump recovery following a high-intensity exercise bout? Open Access J Sports Med 6:49–54. https://doi.org/10.2147/OAJSM.S70263
Vieira A, Siqueira A, Ferreira-Junior J, CarmoDuriganBlazevichBottaro JJAM (2016) The effect of water temperature during cold-water immersion on recovery from exercise-induced muscle damage. Int J Sports Med 37(12):937–943. https://doi.org/10.1055/s-0042-111438
Vieira Ramos G, Pinheiro CM, Messa SP, Delfino GB, de Marqueti R (2016) Cryotherapy reduces inflammatory response without altering muscle regeneration process and extracellular matrix remodeling of rat muscle. Sci Rep. https://doi.org/10.1038/srep18525
Waterman B, Walker JJ, Swaims C, Shortt M, Todd MS, Machen SM, Owens BD (2012) The efficacy of combined cryotherapy and compression compared with cryotherapy alone following anterior cruciate ligament reconstruction. J Knee Surg 25(2):155–160. https://doi.org/10.1055/s-0031-1299650
Webb NP, Harris NK, Cronin JB, Walker C (2013) The relative efficacy of three recovery modalities after professional Rugby league matches. J Strength Cond Res 27(9):2449–2455. https://doi.org/10.1519/jsc.0b013e31827f5253
White GE, Wells GD (2013) Cold-water immersion and other forms of cryotherapy: physiological changes potentially affecting recovery from high-intensity exercise. Extreme Physiol Med 2(1):26. https://doi.org/10.1186/2046-7648-2-26
Wilcock IM, Cronin JB, Hing WA (2006) Physiological response to water immersion. Sports Med 36(9):747–765. https://doi.org/10.2165/00007256-200636090-00003
Wilke B, Weiner RD (2003) Postoperative cryotherapy: risks versus benefits of continuous-flow cryotherapy units. Clin Podiatr Med Surg 20(2):307–322. https://doi.org/10.1016/s0891-8422(03)00009-0
Wilson LJ, Cockburn E, Paice K, Sinclair S, Faki T, Hills FA, Gondek MB, Wood A, Dimitriou L (2018) Recovery following a marathon: a comparison of cold water immersion, whole body cryotherapy and a placebo control. Eur J Appl Physiol 118(1):153–163. https://doi.org/10.1007/s00421-017-3757-z
Yackzan L, Adams C, Francis KT (1984) The effects of ice massage on delayed muscle soreness. Am J Sports Med 12(2):159–165. https://doi.org/10.1177/036354658401200214
Yamane M, Ohnishi N, Matsumoto T (2015) Does regular post-exercise cold application attenuate trained muscle adaptation? Int J Sports Med 36(08):647–653. https://doi.org/10.1055/s-0034-1398652
Yanagisawa O, Homma T, Okuwaki T, Shimao D, Takahashi H (2007) Effects of cooling on human skin and skeletal muscle. Eur J Appl Physiol 100(6):737–745. https://doi.org/10.1007/s00421-007-0470-3
Yeargin SW, Casa DJ, McClung JM, Knight JC, Healey JC, Goss PJ, Harvard WR, Hipp GR (2006) Body cooling between two bouts of exercise in the heat enhances subsequent performance. J Strength Cond Res 20(2):383. https://doi.org/10.1519/r-18075.1
Zemke JE, Andersen JC, Guion WK, McMillan J, Joyner AB (1998) Intramuscular temperature responses in the human leg to two forms of cryotherapy: ice massage and ice bag. J Orthop Sports Phys Ther 27(4):301–307. https://doi.org/10.2519/jospt.1998.27.4.301
Ziemann E, Olek RA, Kujach S, Grzywacz T, Antosiewicz J, Garsztka T, Laskowski R (2012) Five-day whole-body cryostimulation, blood inflammatory markers, and performance in high-ranking professional tennis players. J Athl Train 47(6):664–672. https://doi.org/10.4085/1062-6050-47.6.13
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
SYK and MPM conceptualized the manuscript. SYK performed the literature review and drafter the original manuscript. MPM reviewed the manuscript. SYK and MPM edited the manuscript and critically revising the work. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Additional information
Communicated by Michael Lindinger .
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kwiecien, S.Y., McHugh, M.P. The cold truth: the role of cryotherapy in the treatment of injury and recovery from exercise. Eur J Appl Physiol 121, 2125–2142 (2021). https://doi.org/10.1007/s00421-021-04683-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-021-04683-8