Abstract
The objective of this study is to assess by echography and Doppler the Cerebral (Vmca), Aortic (Vao) and Femoral (Vfem) arterial flow velocity and calf vein (Tibial, Gastrocnemius) section (Tib, Gast) during orthostatic intolerance (OI) test after a 60-day, head down tilt bed rest (HDBR). Twenty-four women (25–40 years) underwent a 60-day HDBR at −6°: eight as control (Con), eight with exercise against lower body negative pressure (Ex-Lb) and eight with nutrition supplement (Nut). Before and after (R0) HDBR, all subjects underwent a 10-min, 80° tilt followed by progressive LBNP until presyncope. After the post-HDBR Tilt + LBNP test, two groups were identified: finishers (F, n = 11) who completed the Tilt and non-finishers (NF, n = 13). A higher percentage decrease in Vao flow, higher percentage distension of Tib vein and a lack of increase in Vmca/Vfem ratio during the post-HDBR Tilt + LBNP compared to pre-HDBR were correlated to OI, but not all of these abnormal responses were present in each of the NF subjects. Abnormal responses were more frequent in Con and Nut than in Ex-Lb subjects. (1) HDBR did not affect the cardiac, arterial and venous responses to the orthostatic test to the same extent in each subject. (2) Exercise within LBNP partially preserved the cardiovascular response to Tilt, while Nutrition supplementation had no efficacy. (3) Cerebral/femoral flow ratio and aortic flow were the parameters most closely related to OI. (4) Reduction in aortic flow was not the major hemodynamic change preceding syncope.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
After 60 days in head down tilt bed rest (HDBR), the cardiovascular system is affected morphologically (e.g., myocardial atrophy, altered carotid wall thickness, venous enlargment) and the hemodynamic responses to orthostatic and exercise activities are altered (Macias et al. 2007; Shoemaker et al. 1998; Hughson et al. 2004, Arbeille et al. 2008b; Bringard et al. 2010). Aerobic exercise countermeasures partially prevent muscular and cardiac atrophy and plasma volume loss (Macias et al. 2007; Dorfman et al. 2007; Trappe et al. 2007), while resistive exercise alone had a limited benefit on these processes (Alkner and Tesch 2004). Each mode of exercise countermeasure alone does not protect against OI. Lower body negative pressure (LBNP) in association with aerobic exercise not only restores plasma volume and myocardium thickness but also reduces peripheral vascular deconditioning and orthostatic intolerance during HDBR (Guell et al. 1991; Gharib et al. 1992; Arbeille et al. 1995; Macias et al. 2007; Watenpaugh et al. 2007). A nutrition countermeasure (daily amino acid supplementation) marginally maintains myocardium, but does not maintain orthostatic tolerance (Dorfman et al. 2007; Guinet et al. 2009; Arbeille et al. 2008b).
During HDBR studies, cardiovascular responses are evaluated using exercise (Bringard et al. 2010, Esposito et al. 2010) or orthostatic stress tests (LBNP, Stand, Tilt tests (Pavy-Le Traon et al. 1999). Usually the only cardiovascular parameters measured are HR and BP, with few studies measuring cerebral and femoral arterial flows. Recently, simultaneous assessment of femoral artery and portal vein flows before and after HDBR demonstrated that both vascular regions are affected more by HDBR in non-finishers during orthostatic stress than in finishers (Arbeille et al. 2008b). In addition, calf vein area increases more in non-finishers during a stand test after a HDBR compared to finishers (Belin de Chantemèle et al. 2004). These arterial and venous parameters have not been measured simultaneously during an orthostatic test (Stand or Tilt) in the same subject.
The hypotheses tested in this study are:
-
That HDBR may not affect cardiac, arterial and venous hemodynamic responses to the orthostatic test to the same extent in each subject.
-
That exercise within LBNP and a nutritional countermeasure prevent deconditioning of cardiac and peripheral responses to an orthostatic test (Tilt + LBNP) after HDBR.
-
Alterations of arterial and venous hemodynamic parameters in the leg changes are more closely related to orthostatic intolerance than the changes in cerebral or aortic blood flow. Thus, syncope is not mediated by a drop in cardiac output but rather by local vascular changes in the lower body.
The main objective of our study is to simultaneously quantify the hemodynamic response to a calibrated 10 min Tilt with additional LBNP at the heart (aortic flow), arterial (cerebral, femoral artery) and calf vein levels. The efficiency of two countermeasures for preventing cardiovascular degradation of the orthostatic response is also evaluated.
Methods
In 2005, a 60-day, 6° HDBR study [Women international space simulation for exploration (WISE) study] was organized by the MEDES Space Clinic at Rangueil Hospital, Toulouse, France. The experiment was approved by a French Committee for Health. Twenty-four healthy women signed a consent form after being informed of the risks of this long-term HDBR study. The population was randomly assigned to three groups, exercise within lower body negative pressure (Ex-Lb: n = 8) and nutrition (Nut: n = 8) countermeasure groups and controls (Con: n = 8). Exercise subjects performed flywheel resistance exercise in the 6° head down position (Alkner et al 2007; Trappe et al. 2007) every third day, plus 40-min supine treadmill exercise within LBNP (Macias et al. 2007) 3–4 days per week with interspersed rest days. The treadmill within LBNP exercise was followed by 10-min passive LBNP at 50 mmHg. Nutrition subjects consumed a daily supplement of protein (0.6 g/kg/day) during meals. This supplement included 3.6 g/day free leucine, 1.8 g/day valine and 1.8 g/day free isoleucine (Trappe et al. 2007).
Orthostatic tolerance test
A Tilt + LBNP test was performed pre-HDBR (Day −1) and after 60 days of HDBR (Day 0). After instrumentation with echographic and Doppler probes (see below) and collection of baseline data in supine position, the subject was tilted to +80° for 10 min and then LBNP was applied from −10 to −50 mmHg, where the pressure was reduced by 10 mmHg every 3 min until presyncope (sudden drop in SBP (>10 mmHg/min), sudden drop in HR (>15 bpm), SBP <70 mmHg, severe light headedness, or nausea). This tilt + LBNP protocol was used in previous studies allowing a precise determination of changes in orthostatic tolerance induced by bed rest (Watenpaugh et al. 2007).
Echographic and Doppler measurements
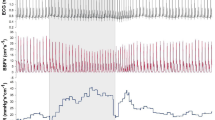
During the TILT + LBNP test, the maximal and mean aortic blood flow velocity (cm/s) (Aortic Flow) were measured from the aortic Doppler spectrum assuming an angle of 0° between the Doppler beam and the aortic axis (2 MHz pulsed Doppler). The aortic probe was fixed on a chest harness. Cerebral flow velocity (MCA Flow) was recorded using a 2 MHz transcranial Doppler probe fixed over the temporal window to insonate the right middle cerebral artery (MCA). The angle of insonation of the MCA was also 0°. The superficial femoral artery flow velocity (Fem Flow) was investigated using a flat Doppler probe of 4 MHz fixed by two straps passing around the upper part of the thigh and around the abdomen. The Doppler beam was steered at 45° from the front face of the probe, and the angle between the Doppler beam and the vessel axis remained unchanged during the session. All sensors worked during all Tilt and Tilt + LBNP tests. The Doppler spectrum was recorded and analysed by the Cardiolab ground module (ESA-CNES device). Based on an earlier report (Arbeille 1997), it was assumed that the diameter of these vessels remained constant during the orthostatic tolerance tests and that mean velocity changed in proportion with flow volume (ml/min) as calculated from velocity and vessel cross-section.
Changes in vascular resistance were estimated from the maximal (S) and minimal (D) flow velocities on the MCA (Cerebral resistance index CRI = [(S − D)/S)] and femoral artery (Femoral resistance index FRI = D/S), D being the amplitude of the reverse flow) (Adamson et al. 1990; Arbeille 1997). From these mean velocities, a Cerebral to Femoral flow ratio [CFR = (MCA flow/FEM flow)] that measures the proportion of flow supplying the leg and the brain was calculated. Calf veins were investigated using a 7.5 MHz ultrasound “T-shaped probe” attached to the upper posterior level of the left calf by an adhesive patch, and connected to the echograph by a 2 m long cable (Logic book GE France). The ultrasound probe was placed in order to visualize a transverse cross-section of the upper part of the posterior tibial vein (Tib) and one or two gastrocnemius veins (Gast) depending on the subject’s anatomy. Echographic views were digitized and recorded continuously during the test and processed on a program designed by our laboratory. The contours of the tibial and gastrocnemius veins were outlined on the images and vein cross-sectional area (CSA) was expressed in cm2.
Parameters display
Arterial and venous parameter changes (in percent from supine) during the whole orthostatic test (Tilt + LBNP) and the absolute values of the vein CSA (in cm2) were displayed as mean ± SD for the three groups (Con; Ex-Lb and Nut) and also for the two groups, finishers and non-finishers. These data were also analysed subject by subject to predict OI, but only during the 10-min TILT as none of the non-finishers reached the first LBNP level. For the subject-by-subject analysis, OI parameters were compared as the percent change during post-HDBR tilt to the percent change during pre-HDBR tilt. For example, the difference in aortic flow drop between R0 and pre-HDBR TILT was [Δ%Ao flow = (percent drop in Ao flow at R0 TILT) minus (percent drop in Ao flow pre-HDBR TILT)]. Thus Δ%Ao flow <0 signifies that there was a higher drop in aortic flow post-HDBR Tilt compared to pre-HDBR Tilt. In addition, Δ%CFR = (Δ%CFR R0 − Δ%CFR pre) < 0 signifies that the blood flow redistribution towards the brain was less efficient post-HDBR Tilt (less vasoconstriction on the leg vascular area). Finally, Δ%Tib csa or Δ%Gast csa > 0 signifies that the vein distension was higher during the post-HDBR Tilt.
Statistical analyses
In the Tilt + LBNP data analysis (time to presyncope), the absolute values at REST and the percent change from supine to the end of the Tilt + LBNP were analysed with the data grouped according to (a) HDBR effect, (b) the countermeasure used, and (c) whether they finished (F) the post-HDT 10-min Tilt test or not (NF). In the figures, values were presented as mean ± SD. Statistical comparisons were performed using two-factor analysis of variance with main effects of group (Finishers, Non-finishers), HDBR (pre-HDBR and post-HDBR). Differences were significant for P < 0.05.
The accuracy of the flow redistribution parameters (%MCA flow, %Ao flow, %CFR = %[MCA flow/(FEM flows)], %Tib csa) to predict OI by the end of the HDBR was determined on the basis of the sensitivity (SS) and specificity (SP) of their response to the Tilt test. Each parameter was expressed as positive (PPV) and negative (NPV) predictive values. In NF subjects lower aortic flow velocity, or femoral resistance, or lower increase in CFR, or higher vein distension, at post-HDBR tilt compared to pre-HDBR, was considered as a “true positive response”, while the opposite was considered a “false negative response”. Conversely, in F subjects, lower aortic flow velocity, lower femoral resistance, lower CFR, or higher vein distension at post-HDBR tilt (compare to pre-HDBR), was considered false positive responses while the opposite was considered as a true negative value.
Results
Table 1 shows that the basic cardiac volume and mass parameters were significantly reduced at post-HDBR compared to pre-HDBR on the NF subject. There was a significant increase in supine resting HR measured prior to the tilt for both the F and NF subjects, but no change in SBP or DBP during this supine baseline period comparing the pre- versus post-HDBR tilt tests.
Average cardiac, arterial and venous changes during the last 3 min of the Tilt + LBNP test in, F and NF groups (Fig. 1 : mean ± SD)
Pre-HDBR 22 subjects reached the Tilt + LBNP −20 mmHg level (1Co and 1Nut did not), while post-HDBR 5 subjects stopped the test at −10 mmHg (2 Ex, 1 Co and 2 Nut) and 6 subjects stopped at −20 mmHg (Ex 4, Co 1, Nut 1).
Arterial flow velocity and venous cross-sectional area average change in response to TILT and Tilt + LBNP (mean ± SD). NF did not reach Tilt + Lb post-HDBR. (Asterisk inside the bar: significant compared to Tilt, Asterisk between 2 bars: significant compared to pre-HDBR p < 0.05) a Middle cerebral mean flow velocity drop (Vmca): percent drop from supine to Tilt and Tilt + Lb (pre and post) in finishers (F) and non-finisher (NF) gr. b Aortic mean flow velocity (Vao): percent drop from supine to Tilt or Tilt + Lb (pre and post) in finishers (F) and non-finishers (NF). c Femoral mean flow velocity (Vfem): percent drop from supine to Tilt or Tilt + Lb (pre and post) finishers (F) and non-finishers (NF). d Cerebral to femoral flow velocity ratio (Vmca/Vfem): percent increase from supine to Tilt or Tilt + Lb (pre and post) finishers (F) and non-finishers (NF) e Femoral Resistance index (FRI): percent change from supine (pre and post) finishers (F) and non-finishers (NF) f Tibial vein cross-section (Tib): percent increase from supine to Tilt (pre and post) finishers (F) and non-finishers (NF) g Gastrocnemius vein cross-section (Gast): percent increase from supine to Tilt or Tilt + Lb (pre and post) finishers (F) and non-finishers (NF)
Thus, the analysis of the cardiovascular changes during the post-HDBR test in relation with OI was limited to Tilt for the NF and to Tilt + LBNP at −20 mmHg for the F. The impact of the CMs on cardiovascular responses to the orthostatic test was analysed using only the Tilt data.
In the F and NF groups during the pre-HDBR Tilt + LBNP
The changes in Vmca; Vao, Vfem, CFR (Vmca/Vfem), FRI, Tib csa, Gast csa were similar for the two groups (Fig. 1).
In the F group during post-HDBR Tilt + LBNP
Vmca decreased significantly more during Tilt + LBNP at −20 mmHg (p < 0.05) compared to the end of Tilt but not compared to pre-HDBR LBNP-20 mmHg, Vao also decreased significantly more at LBNP-20 mmHg (p < 0.05) compared to end of Tilt, while Vfem, CFR, FRI, Tib csa and Gast csa changed similarly as compared to pre-HDBR at each level.
In the NF group during post-HDBR Tilt
Vmca decreased significantly more compared to pre-HDBR (−30 vs. −8% pre, p < 0.05), Vao decreased significantly more (−30 vs. −10%, p < 0.05), Vfem decreased similarly (−42 vs. −33% ns), CFR (Vmca/Vfem) increased less (+23 vs. +43%, p < 0.05), FRI increased less (+20 vs. +30%, p < 0.05), Tib csa increased more (+300 vs. +180%, p < 0.05) and Gast csa increased more (pre +380 vs. +280%, p < 0.05).
Individual cardiac, arterial and venous changes during Tilt: NF versus F (Fig. 2)
For Vao, 8 of 13 NF had a greater decrease post-HDBR (>10% compared to pre), but 5 of 11 F also had a greater decrease. A greater increase in Gast Vein was observed in 8 of 13 NF as well as 5 of 11 F. For the Tib Vein, 7 of 13 NF and 7 of 11 F had a greater increase post-HDBR. For CFR, 9 of 13 NF had a smaller increase of CFR post-HDBR, but only 2 of 11 F had a smaller increase. At least one of these abnormal responses was present in 12 of 13 NF and in 8 of 11 F. In 12 of 13 NF there was either a greater drop in Vao or lack of CFR increase and similar changes were also observed in 4 of 11 F. Three abnormal responses were present in 4 of 13 NF, but only 1 F. Systolic Vfem and Vao changed proportionately in each subjects.
Individual subject results: aortic flow change during Tilt: (%Ao at Tilt post—%Ao at Tilt pre) <0 = > greater Ao decrease at post-HDBR. CFR = (Vmca/Vfem) change during Tilt: (%CFR increase at TILT post—%CFR at Tilt Pre) <0 = > loss in CFR increase (vasoconstriction) at post-HDBR—Tib csa change during Tilt: (%Tib increase during TILT post HDR—%Tib at Tilt Pre) >0 = > higher vein distension during post-HDBR Tilt. The arrows identify the subjects who presented the 3 abnormal responses at the cardiac and lower limb arterial and venous areas (4 NF and 1 F, all 5 Non-Ex-Lb subjects)
Individual cardiac, arterial and venous changes during Tilt (Counter measure gr, Fig. 2)
For Vao, 8 of 16 Non-Ex-Lb had a greater decrease and this was also observed in 4 of 8 Ex-Lb. For Gast vein, 11 of 16 Non-Ex-Lb had a greater increase, but only 2 of 8 Ex-Lb had this response. For Tib vein, 11of 16 Non-Ex-Lb and 3 of 8 Ex-Lb had a greater increase. For CFR, 9 of 16 Non-Ex-Lb had a lack of increase, while this was observed in 2 of 8 Ex-Lb. One of these abnormal responses was present in 15 of 16 Non-Ex-Lb and 5 of 8 Ex-Lb. 7 of 16 Non-Ex-Lb had Tib vein increase and lack of CFR increase, but none of the 8 Ex-Lb had this response. All three of these abnormal responses were present in 4 of 16 Non-Ex, but in none of the 8 Ex-Lb.
Discussion
The primary vascular responses we found during the Tilt + LBNP test were that in the NF and Non-Ex-Lb groups, the drop in aortic flow and Tib-Gast vein distension were greater and the average increase in cerebral to femoral flow ratio (CFR) was smaller compared to the F and Ex-Lb groups. Thus we could expect that the cardiac, arterial and venous responses to an orthostatic test may be more affected in each NF and Non-Ex-Lb subject after HDBR, while none of these responses may be altered in the F or Ex-Lb groups. In fact, the analyses of the mean data among the NF and Non-Ex-Lb subgroups demonstrated that each of the cardiac, arterial and venous abnormal responses were only modestly related to OI or to CM, while the subject-by-subject analyses found that not all of these abnormal responses were present simultaneously in each of the NF or Non-Ex-Lb subjects. This suggests that there is not ONE specific cardiovascular region or function more affected by the HDBR or involved in the development of OI. Thus central and peripheral organs or systems involved in the cardiovascular dysregulation after HDBR are neither affected to the same extent nor in the same order for all subjects.
Most of the changes in cardiovascular variables found during the present Tilt + LBNP test were similar to the changes during a supine LBNP orthostatic test after 55 days of HDBR (Arbeille et al. 2008a, b). Nevertheless, none of these supine LBNP subjects approached the pre-syncope level and thus the supine LBNP results could not provide information on the aortic, cerebral, femoral arterial and calf changes during presyncope.
Cardiac, arterial and venous responses to (Tilt + LBNP during the last 3 min), pre- and post-HDBR in relation with OI
During post-HDBR test in the F group, the added LBNP stress caused a greater decrease in cerebral flow velocity (Vmca) compared to Tilt, but of smaller amplitude than in the NF. Despite the fact that these F subjects finished the 10 min Tilt, their cardiovascular responses were already affected in various territories (leg) by the HDBR, while cerebral autoregulation as reflected by the limited drop in Vmca was still operational and not affected by the HDBR. Previous studies have reported that autoregulation is neither significantly affected by HDBR nor by the reduction in plasma volume that accompanied LBNP, which supports the present observation (Brown et al. 2003; Guo et al. 2006; Kuriyama et al. 2000).
The greater decrease in aortic flow (Vao) during post-HDBR Tilt in the NF group (compared to F) is consistent with an altered venous return as discussed below and may be due to a reduced leg vasoconstriction and increased venous distension. The lack of CFR smaller increase at post-HDBR Tilt compared to pre-, in the NF group expresses the lesser reduction of femoral flow (Vfem) (lack of vasoconstriction) and its consequence on the decrease in cerebral blood flow (Vmca). The intra-muscular gastrocnemius vein and the tibial vein in regions deeper and free from the muscle showed similar and significant increase in vein cross-sectional area at post-HDBR Tilt compared to pre-HDBR Tilt in the NF subjects. Stand tests after a 90-day HDBR (Belin de Chantemèle et al. 2004) and WISE HDBR 55-day supine LBNP showed significant increase in vein distension in the NF subjects (Arbeille et al. 2008a).
On the other hand, the CFR which is the ratio between the cerebral and femoral flow increased similarly during pre- and post-HDBR both during Tilt and Tilt + LBNP in the F group. This suggests that the femoral flow was reduced more than cerebral flow and that the regulating systems (baro-reflexes, cerebral auto-regulation, local leg and splanchnic vasoconstriction) were still operational in this group even after long-term HDBR. This was also observed during supine LBNP or stand tests after long duration HDBR (Arbeille et al. 2005, 2008b).
One may notice that most of the NF subjects were hypovolemic and had myocardial atrophy (Dorfman et al. 2007; Macias et al. 2007) which also may contribute to the drop in aortic flow during an orthostatic test. The greater Ao flow decrease post-HDBR during Tilt + LBNP-20 mmHg (compared to pre-HDBR) in the F group suggests that cardiac function in this group was also partially altered by the HDBR, even though these subjects had no significant reduction in left ventricle volume and had no significant decrease in cardiac mass.
Individual subject analysis in the 3 min preceding pre-syncope and test termination post-HDBR compared to the last 3 min in Tilt at pre-HDBR
The results from individual subjects indicated that a greater aortic flow decrease, higher Tib vein distension and a lack of increase in CFR (less efficient flow redistribution), during post-HDBR Tilt compared to pre, did not occur in all NF subjects (4/13 NF and 1/11 F). A significant drop in aortic flow just before syncope (test end point), insufficient vasoconstriction (too low CFR increase) or higher vein distension was present in half of the whole population, but most of the time only one of these conditions was present.
The flow redistribution ratio (CFR) in relation with the lower limb flow and resistance (FRI) change and the aortic flow drop were the parameters that most correlated to OI (SS 75%; SP 88%). Higher leg vein distension was less correlated to OI. These observations are in agreement with those reported by Goswami et al. (2009) concerning changes in blood pressure, heart rate and cardiac output (CO impedance measurements) during LBNP. These authors observed that the differences in HR, BP and CO responses between subjects indicated that the preferred activation of selected pathways of blood pressure control differed among individuals, but that the preferential mechanisms were highly conserved and reproducible within the same individual.
Conversely others suggest that hypotension (presyncope) during routine tilt testing is always cardiac output mediated, which challenges the conventional idea of insufficient vasoconstriction or systemic vasodilation (vasovagal response) as the overriding cause of hypotension during postural syncope. But they directly measured neither cardiac output nor peripheral flow and vascular resistance changes (Verheyden et al. 2008; Gisolf et al. 2004) which may explain why this explanation is in contradiction with our present results.
On the other hand, all except one of the Non-Ex-Lb subjects had at least one of these abnormal responses during Tilt but only half of the Ex-Lb subjects, which suggests that the Ex-Lb CM partially prevented the cardiac, arterial and/or venous deconditioning induced by the HDBR. Thus, the Ex-Lb CM may have different effects on each of the central and peripheral cardiovascular parameters. The combination of “greater venous distension and lack of CFR increase” was present in half of the Non-Ex-Lb subjects but in none of the Ex-Lb subjects. This suggests that the vascular parameters were most altered by the HDBR and most protected by the Ex-Lb CM in the lower limb arteries and veins (SS 86%; SP 59%).
During this same WISE study Guinet et al. (2009) observed from the heart rate, blood pressure and the duration of the Tilt-LBNP test that the Ex-Lb CM did not significantly improve orthostatic tolerance but protected blood volume and cardiovascular responses to sub-tolerance levels of orthostatic stress. Nevertheless, the Ex-Lb group in the present study had better regional arterial and venous responses to the post-HDBR orthostatic tests. This is not in contradiction with the Guinet et al. results, as HR and BP are systemic parameters which express the summation of peripheral arterial and venous responses. Again, this is in agreement with the fact that not all NF subjects had similar alterations in the various peripheral regions, yet all had an earlier drop in BP post-HDBR compared to pre-HDBR.
Limitations of the study
Carotid artery and Femoral artery diameter were measured with the subject in supine and in tilt positions and these values were used for the calculation of flow volume. Although the common carotid diameter tended to decrease and the femoral diameter to increase, these changes were not significant and did not significantly affect the flow volume calculation. One reason for this lack of effect was that the diameter squared (cross-section area) is used for the calculation of flow volume. The error on the cross-section area is twice as high as the error on the diameter measurement which also results in a twofold greater error on the flow volume than for the diameter. This is true for any kind of vessel but especially for small vessels (MCA). Conversely the changes in mean velocity from supine to tilt were significant. Therefore we used the change in flow velocity for assessing a change in flow volume.
In the present Tilt-LBNP test splanchnic flow was not investigated because too many sensors already were placed on the subject and it would have required additional operators touching the subject during the test. The important role of this vascular area in the expression of OI has been documented during supine LBNP (Arbeille et al. 2008b) and such information would have helped for understanding the complete vascular response to the present orthostatic test.
Conclusion
The present study confirms that: (1) HDBR did not affect to the same extent the cardiac, arterial and venous hemodynamic responses to the orthostatic test in each subject. (2) The exercise within LBNP countermeasure, partially preserved the cardiovascular responses to Tilt, while the Nutrition countermeasure had no benefit on orthostatic tolerance. (3) The cerebral/femoral flow ratio and the aortic flow responses were the parameters that most closely related to OI after HDBR, (4) but the reduction in aortic flow was not the major hemodynamic change preceding the onset of syncope.
References
Adamson SL, Morrow RJ, Languille BL (1990). Side dependent effect of increase in placental vascular resistance on the umbilical arterial velocity waveform in fetal sheep. Ultrasound Med Biol6:19–27
Alkner BA, Tesch PA (2004) Knee extensor and plantar flexor muscle size and function following 90 days of bed rest with or without resistance exercise. Eur J Appl Physiol 93(3):294–305
Arbeille P (1997) Doppler sensors and harnesses for cardiac and peripheral arterial flow monitoring. Ultrasound Med Biol 3:415–423
Arbeille P, Pavy-leTraon A, Fomina G, Vasseur P, Guell A (1995) Femoral artery flow response to LBNP, as an indicator of orthostatic tolerance. Application to long term head down tilt, & spaceflight. Aviat Space Environ Med 66:131–136
Arbeille P, Besnard S, Kerbeci P, Pascaud L, Mohty D (2005) Portal vein cross-sectional area and flow, and orthostatic tolerance—a 90-day bed-rest study. Am J Applied Physiol (5):1853–1857
Arbeille P, Kerbeci P, Mattar L, Shoemaker JK, Hughson RL (2008a) WISE-2005—Tibial & gastrocnemius vein, and calf tissue response to LBNP after a 60 day bedrest with & without counter-measures. J Appl Physiol 104(4):938–943
Arbeille P, Kerbeci P, Mattar L, Shoemaker JK, Hughson R (2008b) Insufficient flow reduction during LBNP in both splanchnic & lower limb areas is associated with orthostatic intolerance after bedrest. Am J Physiol Heart Circ 295(5):1846–1854
Belin de Chantemèle E, Ludovic Pascaud, Custaud M, Capri A, Louisy F, Blanc S, Ferretti G, Gharib C, Arbeille P (2004) Calf volume and vein cross section during stand-test after a 90 day bed rest study with/without exercise counter-measure. J Physiol (Lond) 561(2):611–622
Bringard A, Pogliaghi S, Adami A, De Roia G, Lador F, Lucini D, Pizzinelli P, Capelli C, Ferretti G (2010) Cardiovascular determinants of maximal oxygen consumption in upright and supine posture at the end of prolonged bed rest in humans. Respir Physiol Neurobiol 172(1–2):53–62
Brown CM, Dütsch M, Hecht MJ, Neundörfer B, Hilz MJ (2003) Assessment of cerebrovascular and cardiovascular responses to lower body negative pressure as a test of cerebral autoregulation. J Neurol Sci 15;208(1–2):71–78
Dorfman TA, Levine BD, Tillery T, Peshock RM, Hastings JL, Schneider SM, Macias BR, Biolo G, Hargens AR (2007) Cardiac atrophy in women following bed rest. J Appl Physiol 103(1):8–16
Esposito F, Limonta E, Alberti G, Veicsteinas A, Ferretti G (2010). Effect of respiratory muscle training on maximum aerobic power in normoxia and hypoxia. Respir Physiol Neurobiol 31;170(3):268–272
Gharib C, Maillet A, Gauquelin G, Allevard A, Guell A, Cartier R, Arbeille PH (1992) Results of a 4 week HDT with and without LBNP countermeasure: (I) Volume regulating hormones. Aviat Space Environ Med 63:3–8
Gisolf J, Westerhof BE, van Dijk N, Wesseling KH, Wieling W, Karemaker JM (2004) Sublingual nitroglycerin used in routine Tilt testing provokes a cardiac output-mediated vasovagal response. J Am Coll Cardiol 44(3):588–593
Goswami N, Roessler A, Lackner HK, Schneditz D, Grasser E, Hinghofer-Szalkay HG (2009) Heart rate and stroke volume response patterns to augmented orthostatic stress. Clin Auton Res 19(3):157–165
Guell A, Braak L, Pavy-le Traon A, Gharib C (1991) Cardiovascular adaptation during simulated microgravity: lower body negative pressure to counter orthostatic hypotension. Aviat Space Environ Med 62:331–335
Guinet P, Schneider SM, Macias BR, Watenpaugh DE, Hughson RL, Le Traon AP, Bansard JY, Hargens AR (2009) WISE-2005: effect of aerobic and resistive exercises on orthostatic tolerance during 60 days bed rest in women. Eur J Appl Physiol 106(2):217–227
Guo H, Tierney N, Schaller F, Raven PB, Smith SA, Shi X (2006) Cerebral autoregulation is preserved during orthostatic stress superimposed with systemic hypotension. J Appl Physiol 100(6):1785–1792
Hughson RL, Shoemaker JK, Arbeille P, O’Leary DD, Pissolitto KS, Hughes MD (2004) Splanchnic and peripheral vascular resistance during lower body negative pressure (LBNP) and Tilt. Gravit Physiol 11(2):95–96
Kuriyama K, Ueno T, Ballard RE, Cowings PS, Toscano WB, Watenpaugh DE, Hargens AR (2000) Cerebrovascular responses during lower body negative pressure-induced presyncope. Aviat Space Environ Med 71(10):1033–1038
Macias BR, Cao P, Watenpaugh DE, Hargens AR (2007) LBNP treadmill exercise maintains spine function and muscle strength in identical twins during 28-day simulated microgravity. J Appl Physiol 102(6):2274–2278
Pavy-Le Traon A, Louisy F, Vasseur-Clausen P, Güell A, Gharib C (1999) Contributory factors to orthostatic intolerance after simulated weightlessness. Clin Physiol 19(5):360–368
Shoemaker JK, Hogeman CS, Silber DH, Gray K, Herr M, Sinoway LI (1998) Head-down tilt bed rest alters forearm vasodilator and vasoconstrictor responses. J Appl Physiol 84:1756–1762
Trappe TA, Burd NA, Louis ES, Lee GA, Trappe SW (2007) Influence of concurrent exercise or nutrition countermeasures on thigh and calf muscle size and function during 60 days of bed rest in women. Acta Physiol (Oxf) 191(2):147–159
Verheyden B, Liu J, van Dijk N, Westerhof BE, Reybrouck T, Aubert AE, Wieling W (2008) Steep fall in cardiac output is main determinant of hypotension during drug-free and nitroglycerine-induced orthostatic vasovagal syncope. Heart Rhythm 5(12):1695–1701
Watenpaugh DE, O’Leary DD, Schneider SM, Lee SM, Macias BR, Tanaka K, Hughson RL, Hargens AR (2007) Lower body negative pressure exercise plus brief postexercise lower body negative pressure improve post-bed rest orthostatic tolerance. J Appl Physiol 103:1964–1972
Acknowledgments
The authors acknowledge the sonographers from Tours University Hospital (Maryannick Porcher, Valerie Moreau, Frederic Salez and Joel Blouin) for their active participation on the capture of the Echographic and Doppler data.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Guido Ferrett.
Rights and permissions
About this article
Cite this article
Arbeille, P., Shoemaker, K., Kerbeci, P. et al. Aortic, cerebral and lower limb arterial and venous response to orthostatic stress after a 60-day bedrest. Eur J Appl Physiol 112, 277–284 (2012). https://doi.org/10.1007/s00421-011-1935-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-011-1935-y