Abstract
The present study developed nonexercise models for predicting maximal oxygen uptake \(({\dot{{V}}}\hbox{O}_{\rm{2max}})\) using skeletal muscle (SM) mass and cardiac dimensions and to investigate the validity of these equations in healthy Japanese young men. Sixty healthy Japanese men were randomly separated into two groups: 40 in the development group and 20 in the validation group. \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) during treadmill running was measured using an automated breath-by-breath mass spectrometry system. Left ventricular internal dimensions at end-diastole (LVIDD) and at end-systole (LVIDS) were measured using M-mode ultrasound with a 2.5 MHz transducer. Stroke volume (SV) was calculated based on the Pombo rule. SM mass was predicted by B-mode ultrasound muscle thickness. Correlations were observed between \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) and predicted thigh (r = 0.74, P < 0.001) and lower leg SM mass (r = 0.55, P < 0.001). Furthermore, there were correlations between \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) and LVIDD (r = 0.74, P < 0.001) and SV (r = 0.72, P < 0.001). Stepwise regression analysis was applied to thigh SM mass and SV for prediction of \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in the development group, and these parameters were closely correlated with absolute measured \({\dot{{V}}}\hbox{O}_{\rm{2max}}\ ({R}^{2}=0.72, P < 0.001)\) by multiple regression analysis. When the \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) prediction equations were applied to the validation group, significant correlations were also observed between the measured and predicted \({\dot{{V}}}\hbox{O}_{\rm{2max}}\ ({R}^{2}=0.83, P < 0.001).\) These results suggested that nonexercise prediction of \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) using thigh SM mass and cardiac dimension is a valid method to predict \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in young Japanese adults.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Maximal oxygen uptake \(({\dot{{V}}}\hbox{O}_{\rm{2max}})\) is an important parameter related to cardiorespiratory fitness and quantifying training. \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) is used for quantifying training intensity for aerobic exercise prescription, evaluating the effects of aerobic exercise programs, and classifying individuals for health risks (American College of Sports Medicine 1995). Typically, a maximum graded exercise test performed on a treadmill or cycle ergometer is used to determine \({\dot{{V}}}\hbox{O}_{\rm{2max}}.\) However, this measurement method requires an extensive laboratory, specialized technicians, and considerable subject motivation.
A number of submaximal exercise tests have been developed to estimate \({\dot{{V}}}\hbox{O}_{\rm{2max}},\) based on heart rate during submaximal exercise (Astrand and Ryhming 1954; Cooper 1968; Fox 1973; McArdle et al. 1972; Ryhming 1953; Siconolfi et al. 1982). At present, estimation of maximal heart rate (e.g., the 220 minus age) is most commonly used to estimate \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) using the \({\dot{{V}}}\hbox{O}_{2}\)–heart rate relationship during submaximal exercise. However, type of exercise, fitness level, gender, body composition and age influence maximal heart rate. One standard deviation from the average of the maximal heart rate of the same-age subjects is ±10 beat min−1, and day-to-day heart rate validation averages ±5 beat min−1. This limitation indicates that \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) predicted from maximal/submaximal heart rate falls within 10–20% of the value for a given subject (McArdle 2001). Nonexercise prediction models of \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) use for anthropometry or physical activity (Davis et al. 2002; Fairbarn et al. 1994; Heil et al. 1995; Jackson et al. 1990; Jones et al. 1985; Matthews et al. 1999; Rosen et al. 1998). However, these methods fail to predict \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in certain subjects (Kolkhorst and Dolgener 1994; Malek et al. 2004; Whaley et al. 1995).
\({\dot{{V}}}\hbox{O}_{\rm{2max}}\) is associated with central and peripheral factors. Central factors include pulmonary diffusing capacity, cardiac output [stroke volume (SV) times heart rate], and oxygen-carrying capacity of the blood (Bassett and Howley 2000), of which SV can be evaluated from cardiac dimensions (Pombo et al. 1971). The relationship between cardiac dimensions using echocardiography and \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) is reported (Osborne et al. 1992; Saito and Matushita 2004; Yamazaki et al. 2000), however, there is no imfomation on the prediction of \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) using both central and peripheral factors. Peripheral factors include skeletal muscle (SM) characteristics, such as SM mass. The absolute quantity of muscle mass activated during exercise is an important factor in achieving a high \({\dot{{V}}}\hbox{O}_{\rm{2max}}.\) Ultrasound-derived prediction equations are capable of taking measurements in the field and are valid in predicting total and regional SM mass in both men and women (Sanada et al. 2005). We hypothesized that if central and peripheral factors of SV and SM mass were included in a prediction model of \({\dot{{V}}}\hbox{O}_{\rm{2max}},\) the accuracy may be improved. The purpose of this study was to develop a nonexercise model to predict \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) using cardiac dimensions and SM mass, and to investigate the validity of these equations in Japanese young adults.
Methods
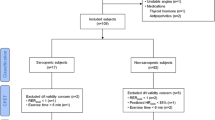
Sixty healthy young Japanese men were separated randomly into two groups: 40 in the development group and 20 in the validation group (Table 1). They participated in college club activities, such as football, swimming, track and field, karate, and engaged in continuous aerobic exercise for at least one session per week for a minimum of 1 h per session. All subjects were physically active but were not specially trained athletes. The purpose, procedures, and risks of the study were explained to each subject prior to inclusion, and all subjects gave their written informed consent prior to participation in the study. The Tokyo Metropolitan University Departmental Ethical Commission approved this study.
Physical activity
All participants wore a uniaxial accelerometer (Lifecorder; Suzuken, Nagoya, Japan) on the left side of the body for 24 h, except when sleeping and showering. Each subject was tested over 7 days, and the per-day mean number of steps (steps day−1), physical activity (kJ day−1), and physical intensity (kJ steps−1 day−1) were recorded. The NASA/JSC physical activity scale (PA-R), a questionnaire, was used to survey the subject’s physical activity.
\({\dot{{V}}}\hbox{O}_{\rm{2max}}\)
\({\dot{{V}}}\hbox{O}_{2}\) during treadmill running was measured using an automated breath-by-breath mass spectrometry system (Aeromonitor AE-280S, Minato Medical Science, Tokyo, Japan). The subjects warmed up at 180 or 190 m min−1 at fixed 0° grade for 5 min. The treadmill speed increased at a rate of 10 m min−1 for each successive 1 min of running until fatigue, defined as the speed at which the subject could no longer continue to keep up with the treadmill. \({\dot{{V}}}\hbox{O}_{2}\) and the respiratory gas exchange ratio were measured every 30 s. Heart rate was also measured every 30 s during exercise using a monitor (Vantage XL, Polar Electro, Kempele, Finland). The range of perceived exertion (RPE) was expressed every 1 min. \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) was recorded as the highest value of \({\dot{{V}}}\hbox{O}_{2}\) for 30 s during each exercise test. The following criteria were used to establish that maximum effort had been achieved: \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) appeared as a plateau in \({\dot{{V}}}\hbox{O}_{2}\) despite an increase in treadmill speed (increased \({\dot{{V}}}\hbox{O}_{2}\) within 150 ml min−1), maximum heart rate within ±11 beats min−1 of the age-predicted maximum (220 minus age), and a maximum respiratory exchange ratio above 1.15 (Howley et al. 1995).
Cardiac dimensions
Left ventricular echocardiograms were obtained by an experienced technician, with subjects in the resting state and in the left lateral decubitus position. The left ventricle was observed in the two-dimension long-axis plane with a 2.5 MHz transducer. M-mode recording were derived from a cursor line crossing the left ventricle below the tips of the mitral valve leaflets. Left ventricular internal dimension at end-diastole (LVIDD) and left ventricular internal dimension at end-systole (LVIDS) were mesured, and the SV was calculated according to Pombo et al. (1971); SV = LVIDD3−LVIDS3. The inter-observer differences in LVIDD and LVIDS (analysis of five separate M-mode scans in five male subjects) were 2.0 ± 1.4 and 1.9 ± 1.9%, respectively, and the intra-observer differences in LVIDD and LVIDS (comparisons of the same images in five male subjects analyzed by two observers) were 2.4 ± 0.8 and 3.0 ± 1.4%, respectively.
Skeletal muscle mass
Muscle thickness (MTH) determined by B-mode ultrasound was measured at nine sites from the anterior and posterior surfaces of the body (Abe et al. 1994): lateral forearm, anterior and posterior upper arm, abdomen, subscapula, anterior and posterior thigh, and anterior and posterior lower leg. Ultrasonographic evaluation of the MTH was performed using a real-time linear electronic scanner with a 5-MHz scanning head (SSD-500, Aloka, Tokyo, Japan). The scanning head with water-soluble transmission gel provided acoustic contact without depression of the skin surface and placed perpendicular to the tissue interface under the marked sites. The MTHs were measured directly and were determined as the distance from the adipose tissue–muscle interface to the muscle–bone interface. Total and regional SM mass were estimated using the equations of Sanada et al. (2006). The MTHs were converted to mass units in kilograms by ultrasound-derived prediction equations using site-matched MTH × height, which calculated the arm, trunk, thigh, and lower leg SM mass.
Fat free mass
Fat free mass (FFM) was estimated from body density using the subcutaneous fat measurements from B-mode ultrasound (Abe et al. 1994). The body density estimated by nine sites subcutaneous fat layer (the measurement sites described in Ultrasound MTH and measurements). The SE of the estimate of body density using ultrasound equations is ∼0.006 gm l−1 (−2.5% body fat) for men and women. Body fat percentage was calculated from the body density using the equation of Brozek et al. (1963). FFM was the difference between body mass and fat mass.
Statistical analysis
Measured and calculated values are expressed as means ± standard deviation (SD). Student’s t test was used for comparison of variables between the development and validation groups. Pearson’s product correlations were calculated between the prediction variables (anthropometric measurements, physical activity, cardiac dimensions, and total and regional SM mass) and \({\dot{{V}}}\hbox{O}_{\rm{2max}}.\) Stepwise multiple regression analyses were performed for these prediction variables and \({\dot{{V}}}\hbox{O}_{\rm{2max}}.\) The prediction equations obtained from the model-development group were then validated in the cross-validation group using the Bland and Altman approach (Bland and Altman 1986). The alpha level for testing significance was set at P < 0.05. All statistical analyses were completed using Stat View v5.0 for Windows (SYS Institute).
Results
Correlations were observed between \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) and predicted thigh (r = 0.74, P < 0.001) and lower leg SM mass (r = 0.55, P < 0.001) in the development group (Table 2). Furthermore, there were correlations between \({{\dot{{V}}}\hbox{O}_{\rm{2max}}}\) and LVIDD (r = 0.74, P < 0.001) and SV (r = 0.72, P < 0.001, Table 3). A correlation was observed between SV and thigh SM mass (r = 0.50, P < 0.01). There were correlations between \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) and body mass, PA-R, and total energy expenditure (P < 0.001, Table 4). Moreover, Stepwise regression analysis was applied to the predicted thigh SM mass and SV to predict \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in the development group, and the values were closely correlated with absolute measured \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) (n = 40, R 2 = 0.72, P < 0.001, SEE = 0.39 l min−1).
When the \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) prediction equations were applied to the validation group, correlations were also observed between the predicted and measured \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) (n = 20, R 2 = 0.83, P < 0.001, Fig. 1a). There was not any bias in prediction of \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) for the validation group (Fig. 1b). The predicted \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in the validation group was 3.70 ± 0.61 l min−1 and was not significantly different from the measured \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) of 3.66 ± 0.55 l min−1 (Table 5).
Relationship between the measured and predicted absolute \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) values in the validation group (a), and Bland–Altman analysis of the validation group (b). Differences between the measured and predicted \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) values plotted against the measured and predicted \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) values
Discussion
Several indirect methods of estimating \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) based on heart rate responses to submaximal exercise have been developed (Astrand and Ryhming 1954; Cooper 1968; Fox 1973; McArdle et al. 1972; Ryhming 1953; Siconolfi et al. 1982). These methods show good prediction accuracy, with high R 2 value, low SEE, and SEE% of the measured value. Siconolfi et al. (1982) reported R 2 = 0.73, SEE of 0.36 l min−1, and SEE% of 14% using their multiple regression equation during submaximal cycle ergometry exercise; \({\dot{{V}}}\hbox{O}_{\rm{2max}}=0.348\ {\dot{{V}}}\hbox{O}_{2}\) of Astrand–Ryhming test −0.035 × age. Fox et al. (1973) also reported a prediction equation based on linear regression analysis relating \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) to submaximal heart rate during the fifth minute of bicycle exercise at 150 W. Their regression equation, R 2, SEE, and SEE% were: \({\dot{{V}}}\hbox{O}_{\rm{2max}}=19.26 \times\) submaximal heart rate at 150 W + 6,300; 0.58; 0.246 l min−1; 7.8% of the measured value. In a field study using walk-run performance, SEE% of predicted \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) from submaximal tests averaged about 8–10% of the measured value (McArdle 2001). The SEE and SEE% values of the nonexercise prediction model in the present study (two variables) were 0.39 l min−1 and 10.5% of the measured value (Table 4), respectively, and were similar to the SEE and SEE% reported for exercise-based prediction models.
Nonexercise tests have been developed based on body composition, including percent of body fat or body mass index, and physical activity determined by a questionnaire method (NASA/JSC physical activity scale; PA-R, Table 5). Excluding the report of Fairbarn et al. (1994), most of the nonexercise prediction models described lower results than the measured \({\dot{{V}}}\hbox{O}_{\rm{2max}}.\) Kolkhorst and Dolgener (1994) also reported that the nonexercise prediction model using the equations of Jackson et al. (1990) significantly underestimated aerobic capacity in college students with high \({\dot{{V}}}\hbox{O}_{\rm{2max}}\). Malek et al. (2004) developed a nonexercise model of \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) using exercise duration and intensity based on a self-questionnaire in aerobically trained women. They reported R 2, SEE, and SEE% values of 0.58, 0.26 l min−1, and 10%, respectively. Although they suggested that the prediction equation is a valid method, their study used six predictors and no statistical selection, such as stepwise regression analysis, was performed. In contrast to previous nonexercise prediction models, the predicted \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) (validation group) was not significantly different from the measured \({\dot{{V}}}\hbox{O}_{\rm{2max}},\) and the derivation of the nonexercise prediction models resulted in a validity coefficient of R 2 = 0.83 and SEE of 0.39 l min−1 (Fig. 1).
It is of interest how the central and peripheral factors contribute to the \({\dot{{V}}}\hbox{O}_{\rm{2max}}\). In the present study, the R 2 value of the estimated SV was similar to the thigh SM mass, with values of 0.52 and 0.55, respectively. The sum of these values was >1.00 because the variables interact with each other (R 2 = 0.25, P < 0.05). The R 2 value in the development group was 0.72 (Table 4), and the remaining 28% variation may be associated with other peripheral factors (e.g. peripheral diffusion gradients) or pulmonary diffusing capacity (Bassett and Howley 2000). Although \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) is limited by cardiac output, i.e., the oxygen-delivery capacity, the MRI-measured lower body SM mass was correlated with \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) during running (R 2 = 0.90), independent of body or fat-free body mass (Sanada et al. 2005). SM mass is an important determinant of exercise capacity in patients with chronic heart failure (Cicoira et al. 2001; Lang et al. 1997). Lang et al. (1997) reported that there was a significant linear correlation between leg lean mass measured by dual-energy X-ray absorptiometry and \({\dot{{V}}}\hbox{O}_{\rm{2max}}\;({R}^{2} = 0.47, P < 0.001)\) in stable ambulatory patients with heart failure. This R 2 value was similar to that in healthy subjects in the present study. On the other hand, the left ventricular dimension also closely correlated with \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in a cross-sectional study in 142 men (R 2 = 0.64, P < 0.001) and in a meta-analysis in 762 men (R 2 = 0.52, P < 0.001) (Osborne et al. 1992). The R 2 value was similar to the value in the present study. Osborne et al. (1992) noted that the LVIDD was correlated with \({\dot{{V}}}\hbox{O}_{\rm{2max}}\;({R}^{2}=0.71, P < 0.001),\) but not the LVIDS. The observations of Takahashi et al. (2003) support these results. Osborne et al. (1992) explained these findings by noting that endurance training involves high-intensity exercise bouts in which left ventricular cardiac output and SV are increased for up to several hours per day. These results suggest that the thigh SM mass and cardiac dimensions are important determinants of \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in healthy young men.
References
Abe T, Kondo M, Kawakami Y, Fukunaga T (1994) Prediction equations for body composition of Japanese adults by B-mode ultrasound. Am J Hum Biol 6:161–170
American College of Sports Medicine (1995) Guidelines for exercise testing and prescription. Lippincott Williams & Wilkins, Philadelphia
Astrand PO, Ryhming I (1954) A nomogram for calculation of aerobic capacity (physical fitness) from pulse rate during sub-maximal work. J Appl Physiol 7:218–221
Bassett DR Jr, Howley ET (2000) Limiting factors for maximum oxygen uptake and determinants of endurance performance. Med Sci Sports Exerc 32:70–84
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Brozek J, Grande F, Anderson JT, Keys A (1963) Densitometric analysis of body composition: revision of some quantitative assumptions. Ann NY Acad Sci 110:113–140
Cicoira M, Zanolla L, Franceschini L, Rossi A, Golia G, Zamboni M, Tosoni P, Zardini P (2001) Skeletal muscle mass independently predicts peak oxygen consumption and ventilatory response during exercise in noncachectic patients with chronic heart failure. J Am Coll Cardiol 37:2080–2085
Cooper KH (1968) A means of assessing maximal oxygen intake. Correlation between field and treadmill testing. JAMA 203:201–204
Davis JA, Storer TW, Caiozzo VJ, Pham PH (2002) Lower reference limit for maximal oxygen uptake in men and women. Clin Physiol Funct Imaging 22:332–338
Fairbarn MS, Blackie SP, McElvaney NG, Wiggs BR, Pare PD, Pardy RL (1994) Prediction of heart rate and oxygen uptake during incremental and maximal exercise in healthy adults. Chest 105:1365–1369
Fox EL (1973) A simple, accurate technique for predicting maximal aerobic power. J Appl Physiol 35:914–916
Heil DP, Freedson PS, Ahlquist LE, Price J, Rippe JM (1995) Nonexercise regression models to estimate peak oxygen consumption. Med Sci Sports Exerc 27:599–606
Howley ET, Bassett DR Jr, Welch HG (1995) Criteria for maximal oxygen uptake: review and commentary. Med Sci Sports Exerc 27:1292–1301
Jackson AS, Blair SN, Mahar MT, Wier LT, Ross RM, Stuteville JE (1990) Prediction of functional aerobic capacity without exercise testing. Med Sci Sports Exerc 22:863–870
Jones NL, Makrides L, Hitchcock C, Chypchar T, McCartney N (1985) Normal standards for an incremental progressive cycle ergometer test. Am Rev Respir Dis 131:700–708
Kolkhorst FW, Dolgener FA (1994) Nonexercise model fails to predict aerobic capacity in college students with high \(\dot{{V}}\hbox{O}_{2}\) peak. Res Q Exerc Sport 65:78–83
Lang CC, Chomsky DB, Rayos G, Yeoh TK, Wilson JR (1997) Skeletal muscle mass and exercise performance in stable ambulatory patients with heart failure. J Appl Physiol 82:257–261
Malek MH, Housh TJ, Berger DE, Coburn JW, Beck TW (2004) A new nonexercise-based \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) equation for aerobically trained females. Med Sci Sports Exerc 36:1804–1810
Matthews CE, Heil DP, Freedson PS, Pastides H (1999) Classification of cardiorespiratory fitness without exercise testing. Med Sci Sports Exerc 31:486–493
McArdle WD, Katch FI, Pechar GS, Jacobson L, Ruck S (1972) Reliability and interrelationships between maximal oxygen intake, physical work capacity and step-test scores in college women. Med Sci Sports 4:182–186
McArdle WD, Katch FI, Katch VL (2001) Individual differences and measurement of energy capacities. In: Exercise physiology: energy, nutrition, and human performance, Lippincott Williams & Wilkins, Philadelphia
Osborne G, Wolfe LA, Burggraf GW, Norman R (1992) Relationships between cardiac dimensions, anthropometric characteristics and maximal aerobic power \(({\dot{{V}}}\hbox{O}_{\rm{2max}})\) in young men. Int J Sports Med 13:219–224
Pombo JF, Troy BL, Russell RO Jr (1971) Left ventricular volumes and ejection fraction by echocardiography. Circulation 43:480–490
Rosen MJ, Sorkin JD, Goldberg AP, Hagberg JM, Katzel LI (1998) Predictors of age-associated decline in maximal aerobic capacity: a comparison of four statistical models. J Appl Physiol 84:2163–2170
Ryhming I (1953) A modified Harvard step test for the evaluation of physical fitness. Arbeitsphysiologie 15:235–250
Saito K, Matushita M (2004) The contribution of left ventricular mass to maximal oxygen uptake in female college rowers. Int J Sports Med 25:27–31
Sanada K, Kearns CF, Kojima K, Abe T (2005) Peak oxygen uptake during running and arm cranking normalized to total and regional skeletal muscle mass measured by magnetic resonance imaging. Eur J Appl Physiol 93:687–693
Sanada K, Kearns CF, Midorikawa T, Abe T (2006) Prediction and validation of total and regional skeletal muscle mass by ultrasound in Japanese adults. Eur J Appl Physiol 96:24–31
Siconolfi SF, Cullinane EM, Carleton RA, Thompson PD (1982) Assessing \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) in epidemiologic studies: modification of the Astrand–Rhyming test. Med Sci Sports Exerc 14:335–338
Takahashi K, Miyachi M, Fujimoto K, Takamoto T, Yamazaki K, Matsueda S, Yamamoto K, Yuzuki O (2003) Maximal oxygen uptake is associated with dimensions in left ventricle and aorta (in Japanese). Japan J Phys Educ Health Sport Sci 48:691–703
Whaley MH, Kaminsky LA, Dwyer GB, Getchell LH (1995) Failure of predicted \({\dot{{V}}}\hbox{O}_{\rm{2max}}\) to discriminate physical fitness in epidemiological studies. Med Sci Sports Exerc 27:85–91
Yamazaki H, Onishi S, Katsukawa F, Ishida H, Kinoshita N (2000) Peak aerobic performance and left ventricular morphological characteristics in university students. Clin J Sport Med 10:286–290
Acknowledgments
The authors thank Dr Motohiko Miyachi (Division of Health Promotion and Exercise, National Institute of Health and Nutrition) for helpful discussion and comments. We also gratefully acknowledge the dedicated men who participated in this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sanada, K., Midorikawa, T., Yasuda, T. et al. Development of nonexercise prediction models of maximal oxygen uptake in healthy Japanese young men. Eur J Appl Physiol 99, 143–148 (2007). https://doi.org/10.1007/s00421-006-0325-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-006-0325-3