Abstract
Recent experimental research has shown that metallic gold releases charged gold atoms when placed intracerebrally and that the liberated gold ions affect inflammation in the brain. The observations suggest that metallic gold can be used as a safe suppressor of inflammation in the central nervous system.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Inflammation in the central nervous system (CNS) has been found to resemble the inflammatory processes taking place in other tissues, and the CNS is therefore no longer considered an immunologically privileged organ (Barker and Widner 2004). Although inflammation is a natural response to damage in the CNS the associated processes unavoidably result in often permanent morphological and physiological changes and are not seldom succeeded by functional disturbances (Whitney et al. 2009). Microglia are considered the resident immune cells of the CNS and the immune response is believed to be ignited by a combined action of microglia, microglia derivated macrophages and invading monocytes/macrophages. The activated microglia, i.e. microglia derivated macrophages, secrete a variety of proinflammatory and neurotoxic factors that apart from igniting the inflammatory cascade are believed to induce and/or exacerbate neurodegeneration (Stoll et al. 1998; Liu and Hong 2003; Mhatre et al. 2004; Chew et al. 2006). Products of the reactive microglia derivated macrophages mediate both the activation of astrocytes, recruiting of lymphocytes and granulocytes and the neuronal injury (Giulian et al. 1993).
It is well known that neuroinflammation regardless of cause, i.e. stroke, traumatic brain injury or neurodegenerative maladies like Alzheimer’s disease and multiple sclerosis (MS), includes loss of neural tissue (for details see Back and Schüler 2004; Pantano et al. 2006; Aktas et al. 2007). In MS, microglia are activated by auto-reactive T cells that peak during the acute disease causing a collapse of the blood–brain barrier and introducing an invasion of all the members of a full-scale immune response (Rasmussen et al. 2007).
Metallic gold plates were used to reconstruct skull defects over 3,000 years ago (Habal 1979), and in the beginning of the nineteenth century gold salts were claimed to be effective in the treatment of depression, epilepsy, migraine, alcoholism, and even impotence. Gold salts got a reputation of being a “nervine” pharmacological element (Richards et al. 2002). However, gold salts were first introduced to modern medicine in 1890 when Robert Koch, Nobel Laureate from 1905, discovered that Mycobacterium tuberculosis could not live in the presence of gold ions in an in vitro setup. This started a not very successful use of gold compounds as a remedy for tuberculosis, but in the slipstream of its use as an antibiotic, clinical knowledge leading to recognition of the immuno-modulatory effects of gold ions accumulated. Hence, since 1927 gold salts have been used in the treatment of rheumatic arthritis, and when more recent medication fails gold thio salts are still used (see also Hashimoto et al. 1992; Yamaguchi et al. 2001).
Although the underlying mechanisms of gold ions are still not fully clarified it has been recognized that gold ions are powerful inhibitors of macrophages and polymorphonuclear leucocytes (Vernon-Roberts 1979; Fleming et al. 1996; Hostýnek 1997). In the 1960s it was demonstrated that gold inhibits the lysosomal enzymes of phagocytotic cells in the inflamed synovial tissue (Persellin and Ziff 1966; Yanni et al. 1994), and gold ions were found to inhibit antigen processing, to suppress NF-κ B-binding activity and I-κ B-kinase activation, and in turn to reduce production of proinflammatory cytokines (Yang et al. 1995; Traber et al. 1999; Yoshida et al. 1999). How gold ions induce their antinociceptive effects is, however, still not known.
The use of gold compounds in medicine has been limited because of their adverse effects. Both parenterally and perorally administered gold compounds can give rise to pronounced nephrotoxicity, and careful monitoring is therefore needed when administering the traditional gold compounds (Hashimoto et al. 1992; Tozman and Gottlieb 1987; Felson et al. 1990; Merchant 1998). Gold thio salts have only occasionally been suggested to cause neurotoxicity, most likely because the blood–brain barrier seems to exclude gold ions from the CNS. However, gold thioglucose, a little used gold compound in the twentieth century, has been associated with significant tissue loss in brain and medulla oblongata (Debons et al. 1982a, b; McGirr et al. 1984). These toxic effects of gold ions relate to the massive whole body exposure that results from treatment with gold compounds in order to obtain a therapeutic level at the inflamed joint(s). This problem can, however, be by-passed by making metallic gold particles/implants the source of gold ions, i.e. by placing a local depot of gold in the inflamed tissue. This “auromedication” is practicable because metallic gold is not, as it has been thought, an inert metal, but is slowly dissolved in the organism by a process coined dissolucytosis (Danscher 2002; Larsen et al. 2007).
All foreign bodies are met by responses from the immune system and, if it is a gold particle or a gold implant, a disintegrating chemical attack will be orchestrated by macrophages that home in on the surface of the implant. Because gold ions have immunosuppressive characteristics that include involvement of macrophages, the bio-released gold ions will affect the dissolution causing macrophages and condition a dampening down of the inflammatory process. The level of suppression depends on the amount of released gold ions that again depends on (1) the size of the available gold surfaces, (2) the number of attacking macrophages, and (3) whether the macrophages are activated or not. Therefore, a metallic implant will serve as a “depot of gold ions” from which immuno-modulatory gold ions will be released at a speed depending on the immunological state of the tissue.
Treatment with gold compounds as e.g. aurothiomalate, i.e. Myocrisin®, is an approach very different from auromedication. When Myocrisin® is applied it causes a spread of gold ions to all parts of the body apart from the CNS and an exposure of all cells, but as the injected gold ions are taken up within a very short period of time by a rather broad spectrum of cells in the whole body, the therapeutic effect on the activated macrophages of the joint(s) suffering from autoimmune inflammation is short. Therefore, the treatment has to be repeated again and again in order to maintain a therapeutic level in the inflamed joint(s). The uptake of gold ions in the cells of the proximal tubules in the nephrons is an important element in the toxicity profile of gold ions (Ogura et al. 1996).
Auromedication on the other hand, based as it is on a relatively sparse bio-liberation of gold ions from a depot of metallic gold implants, releases gold ions locally on a permanent basis, i.e. establishes a local therapeutic level of gold ions. As only insignificant amounts of gold ions will find their way into lymph and blood vessels, no damage will occur to the epithelial cells of the nephrons in kidney (Danscher 2002). These qualities make auromedication a safe treatment from a toxicological point of view. The possibility of a local allergic reaction, i.e. contact allergy towards gold implants/particles made of 99.99% pure gold has to be studied in order to fence conceivable problems. Unwanted reactions of gold ions have been studied in patients that had evolved skin rashes in relation to treatment with gold thio compounds (Hashizume et al. 2008). In patients with gilded stents for stenosis of the cardiac vessels contact allergy has been observed (Svedman et al. 2009), while another study finds that gold-plated stents appear to produce fewer macroscopic and histopathologic changes in the aorta than other types of stents and concludes that gold is a useful intravascular material because it reacts only minimally with the vessel wall (Tanigawa et al. 1995). In summary it is fair to say that gold and gilded implants are intensively used in a multitude of surgery approaches with great success, including as a remedy for lagophthalmos (Choi and Driscoll 2004).
An important benefit from using the auromedication approach is that the release of gold ions seems to be dependent on the degree of inflammation adjacent to gold implants, i.e. whether the local macrophages are activated or not. While auromedicated tissues that are not inflamed will release only tiny amounts of gold ions, immunologically active tissue releases manifold more. The data pointing to such an inflammation depending bio-release of gold ions were gained from a pilot experiment involving transplantation of hearts in rats (Danscher 2010). More research to confirm these findings is underway in our laboratory. If confirmed, the consequences are that a given gold depot can control inflammation in the area of implantation for a very long time, as an activation of the local microglia and monocyte derivated macrophages will cause an increased release of gold ions that again will down regulate the inflammation making the autoimmune event short-lived because the inflammatory cascade might not unfold at all.
Auromedication in the brain of mice with cryo-lesions has ignited a hope of finding ways of suppressing inflammation in the brain (Larsen et al. 2008; Pedersen et al. 2009a, b). By inserting a local depot of metallic gold, that can be made removable, in an area of the brain prone to inflammation it might be possible, in a safe way, to secure a control of the immunological processes in that particular area as long as it is found needed.
Autometallographic (AMG) studies have revealed that gold ions originating from gold salts have their metabolic end station in the lysosomal compartment, and the excess accumulation of gold containing macromolecules causes rupture of the lysosomal membrane (Davies et al. 1971, Burkhardt et al. 1978; Danscher 1981, 1991; Brunk et al. 1997; Møller-Madsen et al. 1984). Gold ions resulting from gold salts have also been shown to be transported over the placental barrier and into the human embryo (Møller-Madsen et al. 1987) and to accumulate in the dorsal root ganglia (Schiønning et al. 1992).
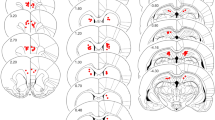
Bio-released gold ions behave predictably as gold ions originating from gold compounds and they likewise pile up in the lysosomes (Danscher 2002; Larsen et al. 2007). This uptake of gold in the lysosomal compartment after exposure to metallic gold implants or gold particles has been confirmed in tissues from rats and mice (Danscher 2002; Larsen et al. 2007, 2008). In the brain, gold ions released from a metallic depot, e.g. gold particles, are taken up by both glia cells and neurons and accumulate in lysosomes (Fig. 1). If gold particles are placed in the cerebral ventricles they are attacked by small macrophages most likely originating from nearby microglia cells (Fig. 2). We have termed this foreign body reaction ‘dissolucytosis’ defined as the extracellular liberation of metal ions from the surface of metallic implants and metal particles bigger than 20 μm, i.e. particles that cannot be phagocytosed by macrophages. The process is believed to be initiated by a macrophage-induced reorganization of the bio-film that envelops any foreign body that is introduced in the organism (Larsen et al. 2007; Sennerby et al. 1993; Roach et al. 1998). The elaborated dissolution membrane makes it operational for the macrophages to control the chemical events at the gold surface, and the dissolucytosis of gold ions involves most likely the capacity of macrophages to release cyanide ions and to alter the oxygen tension and the pH in their vicinity (Amatore et al. 2008). As mentioned, vide supra, the dissolucytotic process is limited by the size of the gold surface facing the tissue, the amount of dissolucytotic macrophages, and their state of activity. The relatively slow speed of the process results in a limited liberation of gold ions securing that they are taken up almost exclusively by cells close to the implant.
Micrographs of 25 μm gold particles in cryo-lesioned neocortex containing tiny autometallographic (AMG) grains in adjacent cells. The grains result from AMG enhancement of gold nanoparticles created by accumulation of the bio-released gold ions in lysosomes. a 30-μm-thick cryo section showing two AMG enhanced gold particles in the inflammatory cerebral tissue. Scale bar 50 μm. b A neighbour section to section in a, but at a higher magnification. Note the heavy load of gold particularly in glia cells. Scale bar 20 μm. c High magnification of the cellular uptake of bio-released gold ion in a semi-thin Epon section. Scale bar 10 μm. d Electron micrograph of AMG silver enhanced gold ions located in lysosomes (arrows). Scale bar 1 μm
In a recent study we injected 20–45 μm gold particles into the neocortex of mice before generating a cryo-injury. We found that the released gold ions reduced microgliosis and neuronal apoptosis, inflicted a transient astrogliosis, and increased the neural stem cell (NSC) response (Larsen et al. 2008). Following unilateral treatment with gold particles, NSC stimulation with increased M-CSF expression was seen. The metallic gold treatment significantly increased the expression of the growth factors VEGF, FGF, LIF and neurotrophin-4 (Pedersen et al. 2009a, 2010). Furthermore metallic gold has been found to reduce TNFα expression, oxidative DNA damage and pro-apoptotic signals after experimental brain injury, while at the same time an increase in the expression of the neuroprotective proteins MTI + II was recorded (Pedersen et al. 2009b). As the bio-liberated gold ions have been shown to possess pronounced anti-inflammatory, neuroprotective and neurostimulatory capacities in the mouse brain a guarded conclusion would be that metallic gold might have clinical potentials.
Neuroprotection and regeneratory qualities of metallic gold were seen as a reduction of apoptotic cell death at both the early and the late phase, and NSE and TUNEL staining confirmed a gold dependant circumvention of apoptosis in neurons (Larsen et al. 2008).
The amount of gold injected into the neocortex of the mice was 5.4 mg pure gold and the amount of released gold ions is so low that only the most sensitive quantitative technique can trace such small amounts. The tool that has made it possible to observe the dissolucytotic activities leading to liberation of gold ions is the histochemical technique autometallography (AMG) (Danscher 1981; Danscher and Stoltenberg 2006) (Figs. 3, 4). As gold nannocrystals/quantum dots (QD) composed of only a few gold atoms are sufficient to initiate the AMG process, the technique is unique in its field and far more sensitive than any of the available laser and diffraction techniques. The capacity of tracing gold in intact tissue makes the technique the tool for establishing the exact morphological location of gold nanoparticles at all magnifications including the highest ultrastructural levels. With the extraordinary sensitivity follows, however, that the technique is rather sensitive to catalytic impurities in the chemicals used. It is imperative, therefore, that the utensils are cleaned carefully in 10% Farmer solution (see protocols) in order to obtain optimal results.
“Camera lucida” representation of the autometallographic process. When the hydroquinone molecules (hexagonal molecules, being the reductor molecules of the AMG developer) adhere to the gold quantum dots (stained gold), electrons are released into the QD, and this event builds up energy in the valence cloud that forms the attraction forces of the nanocrystal. The higher energy level brought about by the surplus electrons increases the statistical probability that silver ions (stained blue) that have attached themselves to the nanocrystal lattices of the IQ dots catch an electron and are turned into a silver atom (stained silver in the drawing). The “new” silver atom shares valence electrons with the valence cloud of the original nanocrystals and is therefore a genuine part of the original gold quantum dot. When the AMG enhanced QD’s have reached the most optimal size for electron, respectively, light microscopic analysis the process is stopped by the developer being replaced by a 5% sodium thiosulphate solution that removes silver ions from the section. Proton-induced X-ray emission spectroscopic analysis (PIXE) of the tissue surrounding gold implants confirms that gold ions are liberated, i.e. that the AMG observations are valid (Danscher 2002; Danscher et al. 1984)
Autometallographic enhancement of gold nanoparticles can be performed in two different ways. To the left an AMG solution is poured into jars containing glass slides with the tissue sections, or the AMG developer is dripped directly onto the individual section. To the right the slides are first dipped into an autoradiographic emulsion, allowed to dry for 10 min and then placed in jars filled with a common chemical developer. Both approaches result in the tissue sections being permeated with a solution of reducing molecules and silver ions. As the gold nanocrystals in the tissue sections catalyse the reduction of silver ions to metallic silver on their surfaces either of the techniques will result in the gold quantum dots/gold nanocrystals becoming encapsulated in metallic silver and thereby made visible at EM and LM levels, i.e. the gold nanoparticle has graphed its own position in the tissue section (modified from Danscher and Stoltenberg 2006)
When it was published that gold nanocrystals can be enlarged by AMG (Danscher 1981; Danscher and Nørgaard 1985) the technique rapidly became industrialized since colloidal gold particles had been introduced as markers of antibodies for ultrastructural analysis (Faulk and Taylor 1971; Bendayan 1980). The latter technique, however, did not allow histopathological/immunohistochemical evaluation of survey sections at light microscopic levels, and the AMG technique therefore came as a welcome solution of this problem. The AMG enhanced gold particles are easily identified at LM levels thanks to the black/brown stain resulting from nanocrystals being encapsulated in silver.
The size of the AMG grains is determined by the original size of the gold particles, the length of development, and the temperature at which the process takes place. The AMG enhanced gold particles are easily identified at LM levels thanks to the black/brown stain of the AMG grains (Danscher and Nørgaard 1985). This quality facilitates screening of sections at low magnifications and promotes the speed by which the diagnosis can be made. Image analysis can contribute to increase the amount of information that can be extracted from the sections. The AMG emulsion technique accentuates that when autoradiography is used for tracing radioactive isotopes in tissue sections it is necessary that these are free of AMG catalytic nanocrystals.
AMG was simultaneously introduced as an enhancer of targeting colloidal gold particles in immunohistochemistry (Holgate et al. 1983) and enzyme histochemistry (Danscher and Nørgaard 1983), and soon thereafter several different AMG developers and a wide assortment of gold-tagged molecules became commercially available.
Although auromedication in some form may lay a decade or more ahead, intra-cerebral application of metallic gold as a pharmaceutical source of gold ions represents a new medical concept that bypasses the blood–brain barrier and allows a direct depot drug delivery to inflamed brain tissue. Loss of nervous tissue is primarily the result of neuroinflammation following traumatic injuries, cerebral thrombosis and haemorrhage, and diseases like Alzheimer’s and MS (Inglese et al. 2004), and the marked impact of gold ions on the inflammatory response in our model includes an increased glia fibrillary acidic protein, GFAP, activity in the early phase along with an over time stable reduction in the number of microglia/macrophages and a significant reduction of ramified macrophages at day 14 (Larsen et al. 2008).
References
Aktas O, Waiczies S, Zipp F (2007) Neurodegeneration in autoimmune demyelination: recent mechanistic insights reveal novel therapeutic targets. J Neuroimmunol 184:17–26
Amatore C, Arbault S, Bouton C, Drapier JC, Ghandour H, Koh AC (2008) Real-time amperometric analysis of reactive oxygen and nitrogen species released by single immunostimulated macrophages. Chembiochem 9:1472–1480
Back T, Schüler OG (2004) The natural course of lesion development in brain ischemia. Acta Neurochir Suppl 89:55–61
Barker RA, Widner H (2004) Immune problems in central nervous system cell therapy. NeuroRx 1:472–481
Bendayan M (1980) Use of the protein A-gold technique for the morphological study of vascular permeability. J Histochem Cytochem 28:1251–1254
Brunk UT, Dalen H, Roberg K, Hellquist HB (1997) Photo-oxidative disruption of lysosomal membranes causes apoptosis of cultured human fibroblasts. Free Radic Biol Med 23:616–626
Burkhardt D, Stephens RW, Ghosh P, Taylor TK (1978) Inhibition of synovial fluid lysosomal glycosidases by anti-arthritic gold preparations. Agents Actions 8:251–257
Chew LJ, Takanohashi A, Bell M (2006) Microglia and inflammation: impact on developmental brain injuries. Ment Retard Dev Disabil Res Rev 12:105–112
Choi M, Driscoll CF (2004) Fabrication of a custom eyelid implant prosthesis: a clinical report. J Prosthodont 13:101–103
Danscher G (1981) Localization of gold in biological tissue. A photochemical method for light and electron microscopy. Histochemistry 71:81–88
Danscher G (1991) Histochemical tracing of zinc, mercury, silver and gold. Prog Histochem Cytochem 23:273–285
Danscher G (2002) In vivo liberation of gold ions from gold implants. Autometallographic tracing of gold in cells adjacent to metallic gold. Histochem Cell Biol 117:447–452
Danscher G (2010) Medicament and method of treatment of patients with heavy metals. United States Patent 7,655,261 B2, 2 Feb 2010
Danscher G, Nørgaard JOR (1983) Light microscopic visualization of colloidal gold on resin-embedded tissue. J Histochem Cytochem 31:1394–1398
Danscher G, Nørgaard JOR (1985) Ultrastructural autometallography: a method for silver amplification of catalytic metals. J Histochem Cytochem 33:706–710
Danscher G, Stoltenberg M (2006) Autometallography (AMG). Silver enhancement of quantum dots resulting from 1) metabolism of toxic metals in animals and humans, 2) in vivo, in vitro and immersion created zinc-sulphur/zinc-selenium nanocrystals, 3) metal ions liberated from metal implants and particles. Prog Histochem Cytochem 41:57–140
Danscher G, Hansen HJ, Møller-Madsen B (1984) Energy dispersive X-ray analysis of tissue gold after silver amplification by physical development. Histochemistry 81:283–285
Davies M, Lloyd JB, Beck F (1971) The effect of trypan blue, suramin and aurothiomalate on the breakdown of 125 I-labelled albumin within rat liver lysosomes. Biochem J 121:21–26
Debons AF, Das KC, Fuhr B, Siclari E (1982a) Inhibition by hypophysectomy of the hyperphagia and obesity following gold thioglucose. Physiol Behav 29:695–699
Debons AF, Siclari E, Das KC, Fuhr B (1982b) Gold thioglucose-induced hypothalamic damage, hyperphagia, and obesity: dependence on the adrenal gland. Endocrinology 110:2024–2029
Faulk WP, Taylor GM (1971) An immunocolloid method for the electron microscope. Immunochemistry 8:1081–1083
Felson DT, Anderson JJ, Meenan RF (1990) The comparative efficacy and toxicity of second-line drugs in rheumatoid arthritis. Results of two metaanalyses. Arthritis Rheum 33:1449–1461
Fleming CJ, Salisbury EL, Kirwan P, Painter DM, Barnetson RS (1996) Chrysiasis after low-dose gold and UV light exposure. J Am Acad Dermatol 34:349–351
Giulian D, Corpuz M, Chapman S, Mansouri M, Robertson C (1993) Reactive mononuclear phagocytes release neurotoxins after ischemic and traumatic injury to the central nervous system. J Neurosci Res 36:681–693
Habal MB (1979) Current status of biomaterial’s clinical applications in plastic and reconstructive surgery. Biomater Med Devices Artif Organs 7:229–241
Hashimoto K, Whitehurst CE, Matsubara T, Hirohata K, Lipsky PE (1992) Immunomodulatory effects of therapeutic gold compounds. Gold sodium thiomalate inhibits the activity of T cell protein kinase C. J Clin Invest 89:1839–1848
Hashizume H, Seo N, Ito T, Takigawa M, Yagi H (2008) Promiscuous interaction between gold-specific T cells and APCs in gold allergy. J Immunol 181:8096–8102
Holgate CS, Jackson P, Cowen PN, Bird CC (1983) Immunogold-silver staining: new method of immunostaining with enhanced sensitivity. J Histochem Cytochem 31:938–944
Hostýnek JJ (1997) Gold: an allergen of growing significance. Food Chem Toxicol 35:839–844
Inglese M, Mancardi GL, Pagani E, Rocca MA, Murialdo A, Saccardi R, Comi G, Filippi M (2004) Brain tissue loss occurs after suppression of enhancement in patients with multiple sclerosis treated with autologous haematopoietic stem cell transplantation. J Neurol Neurosurg Psychiatry 75:643–644
Larsen A, Stoltenberg M, Danscher G (2007) In vitro liberation of charged gold atoms: autometallographic tracing of gold ions released by macrophages grown on metallic gold surfaces. Histochem Cell Biol 128:1–6
Larsen A, Kolind K, Pedersen DS, Doering P, Pedersen MO, Danscher G, Penkowa M, Stoltenberg M (2008) Gold ions bio-released from metallic gold particles reduce inflammation and apoptosis and increase the regenerative responses in focal brain injury. Histochem Cell Biol 130:681–692
Liu B, Hong JS (2003) Neuroprotective effect of naloxone in inflammation-mediated dopaminergic neurodegeneration. Dissociation from the involvement of opioid receptors. Methods Mol Med 79:43–54
McGirr EE, Browne CD, Champion GD, Day RO, Sambrook PN (1984) Aurothioglucose in rheumatoid arthritis. Outcome of treatment in patients intolerant of sodium aurothiomalate. Med J Aust 141:349–351
Merchant B (1998) Gold, the noble metal and the paradoxes of its toxicology. Biologicals 26:49–59
Mhatre AN, Li Y, Feng L, Gasperin A, Lalwani AK (2004) SDHB, SDHC, and SDHD mutation screen in sporadic and familial head and neck paragangliomas. Clin Genet 66:461–466
Møller-Madsen B, Mogensen SC, Danscher G (1984) Ultrastructural localization of gold in macrophages and mast cells exposed to aurothioglucose. Exp Mol Pathol 40:148–154
Møller-Madsen B, Danscher G, Uldbjerg N, Allen JG (1987) Autometallographic demonstration of gold in human fetal liver and placenta. Rheumatol Int 7:47–48
Ogura T, Takaoka M, Yamauchi T, Oishi T, Mimura Y, Hashimoto M, Asano N, Yamamura M, Otsuka F, Makino H, Ota Z, Takahashi K (1996) Changes in urinary enzyme activity and histochemical findings in experimental tubular injury induced by gold sodium thiomalate. J Med 27:41–55
Pantano P, Mainero C, Caramia F (2006) Functional brain reorganization in multiple sclerosis: evidence from fMRI studies. J Neuroimaging 16:104–114
Pedersen MO, Larsen A, Pedersen DS, Stoltenberg M, Penkova M (2009a) Metallic gold treatment reduces proliferation of inflammatory cells, increases expression of VEGF and FGF, and stimulates cell proliferation in the subventricular zone following experimental traumatic brain injury. Histol Histopathol 24:573–586
Pedersen MO, Larsen A, Pedersen DS, Stoltenberg M, Penkowa M (2009b) Metallic gold reduces TNFα expression, oxidative DNA damage and pro-apoptotic signals after experimental brain injury. Brain Res 1271:103–113
Pedersen MO, Larsen A, Stoltenberg M, Penkowa M (2010) Bio-released gold ions modulate expression of neuroprotective and hematopoietic factors after brain injury. Brain Res 1307:1–13
Persellin RH, Ziff M (1966) The effect of gold salt on lysosomal enzymes of the peritoneal macrophage. Arthritis Rheum 9:57–65
Rasmussen S, Wang Y, Kivisäkk P, Bronson RT, Meyer M, Imitola J, Khoury SJ (2007) Persistent activation of microglia is associated with neuronal dysfunction of callosal projecting pathways and multiple sclerosis-like lesions in relapsing—remitting experimental autoimmune encephalomyelitis. Brain 130:2816–2829
Richards DG, McMillin DL, Mein EA, Nelson CD (2002) Gold and its relationship to neurological/glandular conditions. Int J Neurosci 112:31–53
Roach TI, Slater SE, White LS, Zhang X, Majerus PW, Brown EJ, Thomas ML (1998) The protein tyrosine phosphatase SHP-1 regulates integrin-mediated adhesion of macrophages. Curr Biol 8:1035–1038
Schiønning JD, Poulsen EH, Møller-Madsen B, Danscher G (1992) Autometallographic detection of gold in dorsal root ganglia of rats treated with sodium aurothiomalate. Exp Mol Pathol 56:239–247
Sennerby L, Kälebo P, Thomsen P, Albrektsson T (1993) Influence of indomethacin on the regeneration of cortical bone within titanium implants in rabbits. Biomaterials 14:156–158
Stierhof YD, Humbel BM, Schwarz H (1991) Suitability of different silver enhancement methods applied to 1 nm colloidal gold particles: an immunoelectron microscopic study. J Electron Microsc Tech 17:336–343
Stoll G, Jander S, Schroeter M (1998) Inflammation and glial responses in ischemic brain lesions. Prog Neurobiol 56:149–171
Svedman C, Ekqvist S, Möller H, Björk J, Pripp CM, Gruvberger B, Holmström E, Gustavsson CG, Bruze M (2009) A correlation found between contact allergy to stent material and restenosis of the coronary arteries. Contact Dermat 60(3):158–164
Tanigawa N, Sawada S, Kobayashi M (1995) Reaction of the aortic wall to six metallic stent materials. Acad Radiol 2:379–384
Tozman EC, Gottlieb NL (1987) Adverse reactions with oral and parenteral gold preparations. Med Toxicol 2:177–189
Traber KE, Okamoto H, Kurono C, Baba M, Saliou C, Soji T, Packer L, Okamoto T (1999) Anti-rheumatic compound aurothioglucose inhibits tumor necrosis factor-alpha-induced HIV-1 replication in latently infected OM10.1 and Ach2 cells. Int Immunol 11:143–150
Vernon-Roberts B (1979) Action of gold salts on the inflammatory response and inflammatory cell function. J Rheumatol Suppl 5:120–129
Whitney NP, Eidem TM, Peng H, Huang Y, Zheng JC (2009) Inflammation mediates varying effects in neurogenesis: relevance to the pathogenesis of brain injury and neurodegenerative disorders. J Neurochem 108(6):1343–1359
Yamaguchi K, Ushijima H, Hisano M, Inoue Y, Shimamura T, Hirano T, Müller WE (2001) Immunomodulatory effect of gold sodium thiomalate on murine acquired immunodeficiency syndrome. Microbiol Immunol 45:549–555
Yang JP, Merin JP, Nakano T, Kato T, Kitade Y, Okamoto T (1995) Inhibition of the DNA-binding activity of NF-kappa B by gold compounds in vitro. FEBS Lett 361:89–96
Yanni G, Nabil M, Farahat MR, Poston RN, Panayi GS (1994) Intramuscular gold decreases cytokine expression and macrophage numbers in the rheumatoid synovial membrane. Ann Rheum Dis 53:315–322
Yoshida S, Kato T, Sakurada S, Kurono C, Yang JP, Matsui N, Soji T, Okamoto T (1999) Inhibition of IL-6 and IL-8 induction from cultured rheumatoid synovial fibroblasts by treatment with aurothioglucose. Int Immunol 11:151–158
Acknowledgments
The authors acknowledge the technical assistance of Mrs. Karin Wiedemann and Mr. Albert Meier.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Danscher, G., Larsen, A. Effects of dissolucytotic gold ions on recovering brain lesions. Histochem Cell Biol 133, 367–373 (2010). https://doi.org/10.1007/s00418-010-0681-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-010-0681-2