Abstract
Presently applied methods to identify and quantify human satellite cells (SCs) give discrepant results. We introduce a new immunofluorescence method that simultaneously monitors two SC markers (NCAM and Pax7), the basal lamina and nuclei. Biopsies from power-lifters, power-lifters using anabolic substances and untrained subjects were re-examined. Significantly different results from those with staining for NCAM and nuclei were observed. There were three subtypes of SCs; NCAM+/Pax7+ (94%), NCAM+/Pax7− (4%) and NCAM−/Pax7+ (1%) but large individual variability existed. The proportion of SCs per nuclei within the basal lamina of myofibres (SC/N) was similar for all groups reflecting a balance between the number of SCs and myonuclei to maintain homeostasis. We emphasise that it is important to quantify both SC/N and the number of SCs per fibre. Our multiple marker method is more reliable for SC identification and quantification and can be used to evaluate other markers of muscle progenitor cells.
Similar content being viewed by others

Avoid common mistakes on your manuscript.
Introduction
Skeletal muscle satellite cells (SCs) are, by definition, cells located between the plasma membrane and the basal lamina of muscle fibres. They were first identified by electron microscopy and suggested to be “dormant myoblasts that failed to fuse with other myoblasts and are ready to recapitulate the embryonic development of the skeletal muscle fibre when the main multinucleate cell is damaged” (Mauro 1961). Indeed, their proposed functions in repair and regeneration of damaged muscle fibres have been confirmed (Bischoff 1975; Lipton and Schultz 1979; Snow 1978). In addition, SCs are also involved in muscle growth during foetal and postnatal development and are essential for both muscle fibre hypertrophy and maintenance of muscle mass in the adult (Buckingham 2006; Zammit 2008).
Immunohistochemistry and the development of antibodies (abs) to different molecular markers for SCs have made their identification possible using light microscopy. The body of knowledge on SC biology is at present mainly based on studies on mice. SCs are heterogeneous in their expression of different markers and composed of subpopulations with different self-renewal capacity (Buckingham and Montarras 2008; Kuang et al. 2007; Kuang and Rudnicki 2008; Zammit et al. 2006a; Zammit 2008). Furthermore, other stem cells resident in muscle as well as circulating stem cells may contribute to cells in the SC position and may participate in muscle regeneration and repair, see reviews (Cooper et al. 2006; Peault et al. 2007; Shefer and Yablonka-Reuveni 2007).
In human muscle, the use of molecular markers for identification of SCs began in 1989 when abs to the Leu-19 antigen, a 200- to 220-kDa surface glycoprotein, were shown to label SCs (Schubert et al. 1989). However, myotubes, myotube projections in regions of muscle fibre repair and periodically organised fibrillar structures in areas of regeneration were also labelled (Schubert et al. 1989). Subsequent studies showed that the Leu-19 antigen, CD56 and neural cell adhesion molecule (NCAM) have the same immunological properties (Lanier et al. 1989; Mechtersheimer et al. 1992) and that corresponding abs give identical staining patterns (Illa et al. 1992). In most studies on human SCs abs against the Leu-19 antigen or NCAM have been used. Cells located at the periphery of myofibres showing a NCAM stained rim around a nucleus have been judged as SCs (Charifi et al. 2003; Crameri et al. 2004, 2007; Kadi et al. 1999a, 1999b, 2004a, b, 2006; Kadi and Thornell 2000; Mackey et al. 2007a, b; Olsen et al. 2006; Petrella et al. 2006, 2008; Renault et al. 2002b; Verney et al. 2008).
Two other markers which also have been used to identify SCs in human muscle are the cell adhesion protein M-cadherin (M-cad) (Reimann et al. 2004; Sajko et al. 2004), and the paired-box transcription factor Pax7 (Crameri et al. 2007; Reimann et al. 2004; Verdijk et al. 2007). M-cad is an established marker for SCs in mice and was introduced by Irintchev et al. (1994), who showed that M-cad was present in SCs in normal mice muscle. As enhanced staining was seen at the sites of contact between SCs and the parent muscle fibre they also suggested an additional, spatially restricted expression of M-cad in the parent muscle fibres. When the staining patterns of M-cad and NCAM were compared, co-localisation of the abs was seen in nearly all SCs of denervated muscles, while <12% SCs were stained by NCAM in normal muscles (Irintchev et al. 1994). It is not clear whether the fraction of M-cad and NCAM stained SCs differs in human muscle (Sajko et al. 2004).
Pax7 is expressed in the nuclei of myogenic progenitor cells during development and is specifically expressed by SCs in mature muscle (Oustanina et al. 2004; Seale et al. 2000). Pax7 has been widely used to identify SCs in animal studies (Day et al. 2006; Ishido et al. 2009; Kuang et al. 2006; Olguin and Olwin 2004; Relaix et al. 2006; Shefer et al. 2006; Zammit et al. 2006b) and has been proposed to be the most reliable marker for SC in mice (Kuang and Rudnicki 2008; Zammit 2008). The staining of M-cad and Pax7 has been compared in biopsies of normal and pathological human muscles (Reimann et al. 2004). M-cad was, as in mice, present at the interface between the myofibre and the SC in normal muscle, but was in pathological muscle occasionally also seen in mononuclear cells outside the basal lamina of muscle fibres, in myotubes and in regenerating muscle fibres. Since anti-Pax7 reactivity was not found in all M-cad stained SCs and was also observed in some myonuclei, these authors argued against the use of abs against Pax7 alone as a SC “marker” in human muscle (Reimann et al. 2004). On the other hand, Verdijk et al. (2007) recently used Pax7 abs for SC quantification in favour for NCAM abs and reported that, in the human vastus lateralis muscle co-localisation of Pax7 and NCAM staining occurred in approximately 96% of the SCs in both young and elderly subjects.
In our laboratory we have used staining for NCAM as the main marker for SCs (Eriksson et al. 2005; Kadi et al. 1999a, b, 2000; Renault et al. 2002a; b; Thornell et al. 2003). During the years, we have tested the different markers recommended for SC identification in mice to evaluate and improve our method for SC identification and quantification in human muscle. With the exception of anti-Pax7, other markers for SCs used in mice (Zammit 2008) have in our hands not been useful for SC quantification in human muscle sections (Thornell et al. 2003; Lindström and Thornell unpublished).
In the present study we have used a multiple marker (MM) method to evaluate the staining for NCAM in relation to Pax7 in the same section, in order to determine whether the cells examined can unequivocally be identified with the two markers. To verify the position of the SCs and myonuclei we also included staining for laminin present in the myofibre basal lamina and around capillaries and staining for nuclei. Our MM method using both NCAM and Pax7 allows the detection of three SC subtypes in human muscle. Using this new method the SC frequency in the trapezius muscle of power-lifters differs substantially from that reported in our previous studies of the same muscle biopsies based on single immunoenzymatic/chromogen labelling of anti-NCAM and Mayers HTX (Eriksson 2006; Kadi et al. 1999a, b). We show that it is important to label the muscle fibre border in order to be able to establish whether stained cells are SCs or cells outside the muscle fibres.
Materials and methods
Biopsies from the descending part of the trapezius muscle from 11 male power-lifters and 8 sedentary controls (C) were primarily investigated. Five of the power-lifters had never used anabolic drugs (P) whereas six had used high doses of anabolic substances (PAS). To verify that the MM method also holds for other muscles, biopsies from the vastus lateralis from four of the PAS subjects were re-investigated. For a full description of the participant elite athletes, their training regime and the substances used for doping see Eriksson et al. (2005). Handling of biopsies and the detailed analysis of them with respect to muscle fibre types, muscle fibre area, muscle pathology and SC frequency on basis of NCAM staining have been reported previously (Eriksson 2006; Kadi et al. 1999a, b). In this study the analysed P and PAS subjects have the same individual label as previously used in Eriksson (2006). Written consent in accordance with the World Medical Association “Declaration of Helsinki” was obtained from all the subjects. The study was approved by the Ethical Committee of Umeå University.
Immunohistochemistry using multiple labelling
Five-μm thick muscle cross-sections were cut at −23°C using a Reichert Jung cryostat (Leica, Nussloch, Germany). The sections were collected on gelatine-coated slides and stored at −23°C until further processing the same day. The sections were brought to room temperature and post-fixed in 2% paraformaldehyde (PFA) for 8 min and then rinsed in 0.01 M phosphate buffered saline containing 0.05% Tween 20 (PBST) for 3 × 5 min.
In previous studies (Eriksson et al. 2005; Kadi et al. 1999a, b; Renault et al. 2002b) we had preferentially used unfixed sections sometimes cut in advance and stored at −20°C until the day of labelling. However, for immunofluorescence and multiple labelling as in the present study, this resulted in inadequate antigen and specimen preservation. The use of newly cut sections and post-fixation was therefore important. Improved staining results were obtained using 2% PFA for 6–10 min when compared to other fixatives such as acetone or methanol. The sections were immersed in 5% non-immune donkey serum (Jackson ImmunoResearch Laboratories. Inc, West Grove, PA, USA) for 15 min before each incubation with primary (+4°C overnight or 37°C for 60 min) and secondary (37°C for 30 min) abs and washed in PBST 3 × 5 min after all antibody incubations. Bound primary abs were visualised by indirect immunofluorescence using affinity-purified abs specifically prepared for multiple labelling and conjugated with fluorochromes with different emission spectra, fluorescein (FITC), Rhodamine Red-X (RRX) and Cyanine 5 (Cy5) (Jackson ImmunoResearch Laboratories. Inc, West Grove, PA, USA). Nuclei were identified with 4′,6-diamidino-2-phenylindole (DAPI) provided in the mounting medium (Vectashield®, Vector Laboratories Inc, Burlingame, CA 94010 USA). Control sections were treated as above except that the primary antibodies were exchanged with non-immune serum. A detailed scheme of the staining procedure is provided in Fig. 1.
Multiple labelling protocol of NCAM, Pax7, laminin and nuclei. The above protocol shows the labelling procedure used for the present experiments. Further experiments have shown that the procedure can be shortened by simultaneous labelling of the 2nd and 3rd primary abs and simultaneous labelling of their conjugated fluorochromes
Antibodies
For SC identification with the MM method we used the monoclonal antibody (mab) CD56/NCAM against the Leu-19 antigen (Becton Dickinson Immunocytochemistry Systems, San Jose, CA, USA) and the mab against Pax7 (Developmental Studies Hybridoma Bank, University of Iowa, Iowa City, IA, USA). The polyclonal antibody (pab) PC128 against human laminin (The Binding Site Ltd, Birmingham, UK) was used for identification of the basal lamina. On additional serial sections the mab NCL-Merosin against laminin alpha 2 chain (Novocastra Laboratories Ltd., UK) was used for identification of the myofibre basal lamina and the pab GTX15277 (Gene Tex, Inc) against dystrophin was used for detection of the myofibre plasma membrane.
Light microscopy and analysis of immunostained sections
The sections were evaluated using a Nikon eclipse E800 microscope (Nikon Inc., Melville, NY, USA) equipped with excitation filters for FITC (480 ± 15 nm), Texas Red (560 ± 20 nm), HQ Cy5 (620 ± 60 nm), dual-band filter for FITC and Texas Red and triple band filter for FITC, Texas Red and DAPI (Chroma Technology Corp., Rockingham, VT 05101 USA). A SPOT RT KE slider camera (Diagnostic Instruments Inc., Sterling Heights, MI, USA) was used for image acquisition. This camera uses three-shot digital technology to derive true, non-interpolated red, green, and blue values to the CCD and has a slide mechanism allowing light with longer wavelengths to reach the CCD, which allows the capture of emissions from Cy5 fluorescence to be displayed in black and white.
The sections were analysed using different filter cubes and ×20 and ×40 objectives. NCAM and Pax7 labelled SCs were visualised using the dual-band filter for FITC and RRX. The presence of a nucleus stained by DAPI was verified using the triple-band filter. The staining for NCAM alone was analysed using the FITC filter and a weak staining for Pax7 was controlled using the Texas Red filter since some fluorescence signal is lost when using the dual-band filter. To verify the SC position inside the myofibre basal lamina labelled by Cy5 an additional live image or a captured image was needed.
Two abs developed from the same source can be identified on the same section using indirect immuno-labelling technique if sequential labelling cycles are used and the antigens are known to be located in different histological structures such as NCAM in the cell membrane/cytoplasm and Pax7 in the cell nucleus. The order in which the primary mabs were applied was considered because the first primary antibody will be labelled by both secondary fluorochrome abs. NCAM was applied as the first primary mab since it was important that the thin and sometimes weak NCAM staining of the SC membrane could be analysed both separately in the FITC filter and together with labelling for Pax7 in the dual-band filter. Anti-Pax7 reactivity in a SC nucleus could be distinguished without any problem as a separate entity together with the NCAM labelled cell membrane using the dual-band filter or on merged images. The order of labelled fluorochromes, FITC before RRX resulted in SCs with yellow cell membranes and red nuclear staining. This gave a much better contrast than using the reversed order of the fluorochromes, which resulted in a yellow and green staining. Similarly this preferred combination also gave better staining for simultaneous visualisation of Pax7 and DAPI using the triple-band filter or on merged images. Since the emission of Cy5 only is detectable by the camera it was used for visualisation of the basal lamina. Different ways to analyse the frequency and staining pattern of SCs were considered and by experience we found the following to be most efficient: digital images were captured to cover the area of the section using the 20× objective. For each view, one image for each labelled fluorochrome was captured and used for merged image combinations. The images were used for detailed analysis and quantification using the Adobe Photoshop CS2 software (Adobe Systems Inc., Mountain View, CA, USA).
Identification of SCs
We identified a cell as a SC if the following criteria were fulfilled: the cell should be stained by NCAM or Pax7, contain a nucleus stained by DAPI and reside in a sublaminar position confirmed by the laminin staining. In addition, the SC should show staining for NCAM on the myofibre side of the nucleus. To exclude the presence of Pax7+ myonuclei we also analysed sections labelled by anti-Pax7, anti-dystrophin and DAPI. The staining pattern for anti-NCAM and anti-Pax7 identified SCs was analysed in detail on single and merged images using the zoom function of the software or under the microscope. The proportion of NCAM+/Pax7+, NCAM+/Pax7− and NCAM−/Pax7+ SCs was determined.
Quantification of NCAM and Pax7 stained SCs, myofibres and myonuclei
The number of cross-sectioned myofibres and associated SCs were marked and counted on separate image layers using either an image reconstruction of the whole section (merged images of NCAM, Pax7, DAPI and Laminin) or of each image area separately. If the image areas were analysed separately, morphometric principles to bridge variation in myofibre size were used for the quantification of myofibres, SCs and myonuclei (Gundersen 1986). In one case, two sections of the same specimen obtained at different levels were used for the quantitative analysis in order to increase the number of fibres analysed to ≥200 fibres. Regenerating muscle fibres having a basal lamina but lacking a dystrophin labelled plasma membrane (verified in a serial section labelled with anti-dystrophin) or fibres with incomplete basal lamina were not included in the analysis.
The number of sublaminar nuclei (i.e. all nuclei enclosed by the basal lamina) per fibre (N/F) was determined from randomly selected images of the basal lamina and nuclei visualised by staining for laminin and DAPI. The number of nuclei was obtained in more than 75 fibres in C and more than 100 fibres in P and PAS, however, with the exception of one biopsy (PAS1) where only 60 fibres were available. The number of N/F for each individual was used to calculate the number of SCs expressed as a proportion of all nuclei (myonuclei + SC nuclei) inside the myofibre basal lamina (number of SCs/((N/F) × number of F) × 100) and the size of myofibre CSA per nucleus i.e. nuclear domain (myofibre CSA/(((N/F) × number of F) − number of SCs)).
Statistics
All statistical analyses were performed using SPSS standard Version 17.0 (SPSS, Chicago, Illinois, USA). Residual analyses revealed no strong discrepancies from the one-way analysis of variance (ANOVA) assumptions, except for a large difference in variance between the groups in the mean fibre cross-sectional area, and the number of SCs per mm2. To compare the group means for those variables, since the Kruskal–Wallis test suggested statistical differences, independent sample t tests not assuming equal variances was used for the mean fibre cross-sectional area and Mann–Whitney test was used for the number of SCs per mm2. For the other variables, between-group differences were tested using ANOVA. When the ANOVA test suggested statistical differences, the Tukey post-hoc test was applied to establish the contribution of each group to the apparent significance. Paired samples t test was used for repeated measurements. A Chi-square test was used to evaluate if observed frequency of SC subpopulations was related to group characteristics. Statistical significance for all analyses was accepted at p < 0.05. Data are reported as means ± SD.
Results
Immunoreactivity for NCAM, Pax7 and laminin
When the sections were examined in the dual-filter set for both NCAM and Pax7 or the triple-filter set including DAPI staining of nuclei, it was obvious that Pax7 was present in nuclei, as expected, and that these nuclei in general were related to a rim of NCAM staining. Staining for laminin revealed that these cells were in a sublaminar position, i.e. SCs (Fig. 2). A Pax7+ nucleus was never observed inside the dystrophin labelled myofibre plasma membrane, i.e., myonuclei were always unstained for Pax7 (Fig. 3). However, we sometimes observed dystrophin staining surrounding a Pax7+ nucleus found in SC position (Fig. 3b–f).
Multiple labelled muscle cross-section for identification of SCs with immunofluorescence microscopy. Cross-section from a control subject stained with anti-NCAM, anti-Pax7, anti-laminin and DAPI shown in single and merged images: a NCAM (green); b NCAM (green + red = yellow) and Pax7 (red); c NCAM (yellow), Pax7 (red), Laminin (white) and DAPI (blue); d Laminin (white). Three SCs are indicated with arrows in a and shown in higher magnification in corresponding insets (a–c). Note the difference in degree of anti-NCAM staining between the SCs. SC (a) would have been difficult to identify without the positive reaction for Pax7. Note NCAM stained structures not related to the SCs present between myofibres (large arrowheads a and d) and autofluorescent lipofuscin granules (small arrowheads in a and d). Capillaries (*). Bar 50 μm and insets 10 μm
Pax7 staining and myonuclei. Control section from a C subject stained for Pax7 (red), dystrophin (green), and DAPI (blue) to examine whether Pax7 might also stain myonuclei, i.e. nuclei located interior to the anti-dystrophin staining of myofibres. a Pax7+ nucleus (red) located in a SC position exterior to the myofibre plasma membrane (green). d Pax7+ nucleus (red) surrounded by staining for anti-dystrophin. b and e Merged images also showing nuclei stained by DAPI (blue). c and f Anti-dystrophin. Arrows show the thin rim of labelling interior to (e) and around (f) the SCs. Lipofuscin granules (arrowheads). Bar 20 μm
There was a variation in the intensity of the staining for both NCAM and Pax7 in the SCs from intense to lack of detectable staining (Figs. 2 and 4). Sometimes a weak staining for laminin was noticed between a NCAM+/Pax7+ stained cell and the myofibre (Fig. 5b). Such cells were included in the quantification as SCs, whereas occasional NCAM+/Pax7+cells with a distinct anti-laminin reaction around the cell separating it from the myofibre were not assessed as SCs (Fig. 5c–d). A few mono-nucleated NCAM+/Pax7− cells with positive laminin staining were also observed between the myofibres (Fig. 5e–f). NCAM and Pax7 staining was also present in cell clusters within injured myofibres (Fig. 6), the latter deduced from the presence of a basal lamina (Fig. 6b) and the lack of a plasma membrane, i.e. no staining for dystrophin (Fig. 6c). These clusters represented cells involved in myofibre repair i.e. macrophages (verified by immunolabelling for CD68, not shown) and SC progeny in various stages of myogenic differentiation; staining for NCAM and Pax7 differed with more cells stained for only NCAM (Fig. 6d–e) and some cells showed staining for desmin and developmental myosin heavy chains (Eriksson et al. 2006). In other areas and sections, staining for NCAM could also be seen at the contour of muscle fibres, in structures in between muscle fibres and in the sarcoplasm of some very small to normal sized muscle fibres (Fig. 7).
Variability in NCAM/Pax7 staining in SCs. Images of selected SCs from multiple labelled muscle cross-sections stained with anti-NCAM, anti-Pax7, anti-laminin and DAPI (Rows a–f). Merged images are shown in columns 2–4. 1st column NCAM (green), 2nd NCAM (green + red = yellow) and Pax7 (red); 3rd DAPI staining (blue) is added; 4th staining for laminin (white) is added and the 5th laminin (alone). a SC with strong staining for both NCAM and Pax7. b Two NCAM stained SCs. One has weak staining for Pax7 (arrow). c Pax7 stained SC with weak staining for NCAM. d Two NCAM stained profiles; (a) NCAM staining is seen towards the basal lamina but not between the myofibre and the Pax7 negative nucleus, not counted as a SC, whereas (b) was counted as a SC, a tip of a nucleus negative with anti-Pax7 staining, but DAPI staining is observed. e NCAM stained SC with no staining for Pax7. f Pax7 stained SC with undetectable staining for NCAM. Autofluorescent lipofuscin granules are seen in all columns, some examples are marked (arrowheads) in the 5th column. (a: P subject and b–f: C subjects). Capillaries (*). Bar 20 μm
Necessity of labelled basal lamina for reliable detection of NCAM and Pax7 stained SCs. Images of selected NCAM stained cells from sections multiple labelled with anti-NCAM, anti-Pax7, anti-laminin and DAPI (Rows a–f). Merged images are shown in columns 2–4. 1st column NCAM (green), 2nd NCAM (green + red = yellow) and Pax7 (red); 3rd DAPI staining (blue) is added; 4th staining for laminin (white) is added and the 5th laminin (alone). a NCAM+/Pax7+ SC in a sublaminar position. b–d NCAM+/Pax7+ cells with variable degrees of laminin staining towards the myofibre: b weak staining for laminin (arrow) was counted as a SC. c and d distinct staining for laminin (arrows) were not counted as SCs. e One NCAM+/Pax7+ and one NCAM+/Pax7− cell. The NCAM+/Pax7+ cell is a SC inside the myofibre basal lamina whereas the NCAM+/Pax7− cell is stained by laminin and is separated from the myofibre (arrow). The latter is not considered to be a SC. f NCAM+/Pax7− cell with its own basal lamina (arrows) located in the space between myofibres close to two capillaries. Not considered to be a SC. Capillaries (*). (a–c and e, f from PAS subjects, d from C subject). Bar 20 μm
Injured myofibre under early repair. Muscle cross-section from a PAS subject stained for NCAM (yellow), Pax7 (red), laminin (white) and DAPI (blue) a Merged image of all four markers showing a cluster of cells related to a myofibre under repair (*) and three SCs (arrows). b Laminin staining of myofibre basal lamina and capillaries. Note presence of an intact basal lamina around the fibre under repair. c Adjacent section stained with anti-dystrophin (red) and DAPI (blue) to verify that the muscle fibre under repair lacks an intact plasma membrane. Bar 50 μm. d and e The injured fibre shown in higher magnification to reveal the heterogeneity in staining for NCAM and Pax7. d NCAM (yellow) and Pax7 (red). e NCAM (yellow), Pax7 (red) and DAPI (blue). Note that some nuclei are neither Pax7+ nor NCAM+. Bar 20 μm
NCAM staining of muscle fibres. Multiple labelled cross-section from a PAS subject. Merged images are shown. a NCAM (yellow) and Pax7 (red), b staining for DAPI (blue) and laminin (white) is added. Staining for NCAM, apart from being present in three Pax7+ SCs (arrows) is also seen with variable degree in the cytoplasm of muscle fibres of different size. Note the small sized myofibre (arrowhead) which in the absence of additional staining for the basal lamina and nuclei might have been misinterpreted to be a SC. Bar 50 μm
A number of fluorescent structures often granular in shape present close to SCs or being sublaminar were seen in all sections and with all filters (Figs. 2–4). These structures are autofluorescent lipofuscin granules (Thornell et al. 1983).
Proportion of NCAM and Pax7 stained SCs
The majority (94–95%) of SCs was stained for both NCAM and Pax7 in all groups. The mean proportion of SCs identified by NCAM staining only was 4.3% in the C group, 2.5% in the P group and 5.4% in the PAS group. Few SCs showed Pax7 staining only (mean 1.4% all groups) but with high individual variability (range 0–11.3%). The highest frequency was seen in one biopsy from a power-lifter (P2) (Table 1). The observed frequencies of NCAM+/Pax7+, NCAM+/Pax7− and NCAM−/Pax7+ SC subpopulations in the C, P and PAS groups were significantly different from expected frequencies if occurred by chance (p = 0.0027). The largest discrepancy between the observed and expected frequencies was found in NCAM+/Pax7− and NCAM−/Pax7+ SCs in the P and PAS groups (Table 2).
The number of N/F, SC frequency and nuclear domains
In Table 3 the mean fibre cross-sectional area (CSA), N/F, the number of analysed fibres and SC data expressed as the number of SC per fibre (SC/F) or relative to sublaminar nuclei (SC/N) are given.
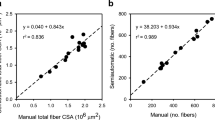
The mean number of N/F was of the same magnitude in the P (4.2 ± 0.5) and PAS (4.0 ± 0.9) groups but significantly higher than the C group (2.7 ± 0.5) (p < 0.01). The mean number of N/F was plotted against the mean fibre CSA for all subjects. A significant correlation was observed r = 0.74 (p < 0.01) (Fig. 8a).
The number of SC/F was of the same magnitude in the P and PAS groups, but differed significantly from that in the C group (p ≤ 0.01). In other terms, the P and PAS groups had approximately 6–7 more SCs per 100 fibres or about 50% more SCs than the C group. A positive correlation was found between the number of SC/F and the mean fibre CSA r = 0.65 (p < 0.01) (Fig. 8b). There was no difference between the groups when the number of SCs was expressed as SC/N. The number of SCs per mm2 was lower for the PAS group (19.9 ± 5) compared to the P (28.4 ± 12.2) and C (25.2 ± 3.7) groups but not significantly different. The size of the nuclear domains differed significantly for the PAS group (2575 ± 540 μm2) versus that of the P (1727 ± 350 μm2) and C (1819 ± 223 μm2) groups (p < 0.01).
SC frequency identified by NCAM and Pax7 compared to NCAM + Mayers HTX
With the present MM method we found almost half the number of SC/F (mean difference −0.16 SC/F) compared to the previously reported results for the samples in the P and PAS groups (Table 4). Only one sample (P2) showed slightly higher and more similar number of SC/F (+0.04 SC/F) with the new method. In this individual the highest number of NCAM−/PAX7+ SCs was observed (11.3%). Also when the number of SC/N was compared to previously reported data a considerable difference (p < 0.01) was observed for the P and PAS subjects. For the C groups comparable proportions were observed (Table 4).
Verification of the MM method in another muscle
Biopsies from the vastus lateralis muscle from four of the PAS subjects were investigated to examine if the number of SCs using the MM method differed from our previous results based on staining for NCAM + Mayers HTX. Our new method showed a fourfold difference in the number of SC/F compared to previously reported data for the same subjects: 0.15 ± 0.05 vs. 0.63 ± 0.41 SC/F. The individual new data versus the old data were: PAS1 (0.20 vs. 0.49), PAS2 (0.18 vs. 1.17), PAS5 (0.12 vs. 0.64) and PAS6 (0.09 vs. 0.20).
From our staining results, it seems possible that NCAM stained profiles, without the additional markers of the MM method could easily have given rise to misinterpretations and included in the analysis without fulfilling the criteria as SCs (Fig. 9).
Misinterpretation of SCs. Cross-section from vastus lateralis muscle of a PAS subject stained with anti-NCAM, anti-Pax7, anti-laminin and DAPI. Single and merged images are shown. a and a1–d1 NCAM (green). a2–d2 NCAM (green + red = yellow) and Pax7 (red). b and a3–d3 All markers; staining for laminin (white) and DAPI (blue) added. a4–d4 laminin staining (white). Note a number of NCAM stained profiles (a–b). Those surrounding a nucleus stained by DAPI are marked with (arrows) if Pax7+ and with (arrowheads) if Pax7−. Two NCAM+/Pax7+ cells (a–b) and two NCAM+/Pax7− (c–d) are shown at higher magnification. a1–a4 Cell interpreted as a SC: NCAM+/Pax7+, with a nucleus in sublaminar position. b1–b4 NCAM+/Pax7+ cell enclosed by laminin staining and separated from the myofibre. This cell is a muscle progenitor cell but not a SC by definition. c1–c4 NCAM+/Pax7− cell enclosed by laminin staining and separated from the myofibre. The cell is not a SC by definition. It may be myogenic but its status is unknown. d1–d4 NCAM+ structure close to a Pax7− nucleus, possibly an unmyelinated nerve located between the muscle fibres. Further classification is not possible with current data. a–b bar 50 μm and (a1–d4) bar 10 μm
Discussion
In the present study we have described a new and robust immunofluorescence MM method to identify and quantify SCs in human muscle. The method allows the distinction of SC subtypes and is unquestionably more accurate for the identification and quantification of SCs than our previous methods. We demonstrate that cells in the SC position in the human trapezius muscle form a heterogeneous cell population. The vast majority of the SCs (94%) were stained for both markers approximately 5% were only stained for NCAM and 1% only for Pax7. Thus, staining for NCAM identified more SCs than staining for Pax7. This was true for 18 of the 19 subjects, whereas in one biopsy (P2) 11.3% of the SCs were only stained with Pax7. Importantly, a more complete description of the number and identity of SCs was obtained with the use of both markers. We envision that the MM method has a great potential also for further studies on human muscle SCs and other cells in situ in normal, experimental and pathological conditions as it can be used for the evaluation of other markers for determination, quiescence, activation, proliferation or differentiation.
Disadvantages with anti-NCAM and anti-Pax7 as single markers for SC quantification
Staining for NCAM has been used in a number of studies to identify SCs and it has been regarded as a reliable marker for SCs in human muscle (Charifi et al. 2003; Eriksson et al. 2005; Kadi et al. 1999a, b, 2004b, 2006; Mackey et al. 2007a, b; Olsen et al. 2006; Petrella et al. 2006, 2008; Verney et al. 2008). However, NCAM is expressed not only in SCs but also on/in myoblasts, myotubes and muscle fibres during development and in adults in regenerating or newly denervated muscle fibres (Illa et al. 1992). NCAM is also abundant along unmyelinated intramuscular nerves and at the surface of motor nerve terminals and Schwann cells related to neuromuscular junctions (Cashman et al. 1987; Mechtersheimer et al. 1992). Thus, it is of utmost importance that stained SCs can be reliably separated from other structures stained by NCAM.
It is conceivable that the synthesis and degradation of NCAM and NCAM isoforms may vary in relation to the degree of physical activity and other factors. This may be reflected in variability in degree of NCAM staining. Differences in the specificity of different NCAM abs may also be a problem. Studies in which the present antibody to NCAM has been used report 4.3–5% SC/N for the vastus lateralis muscle in sedentary young individuals (Mackey et al. 2007b; Olsen et al. 2006; Petrella et al. 2006), whereas in studies using other abs to NCAM the mean proportion of SC/N is just 2.5–2.86% (Crameri et al. 2004, 2007; Dreyer et al. 2006).
Pax7, unlike NCAM and M-cad, is proposed to be expressed only in SCs in mature muscle (Kuang and Rudnicki 2008) and thus Pax7 ought to be an ideal marker for SCs. However, the use of Pax7 as a single marker for SCs in human muscle was not recommended by Reimann et al. (2004), who found a discrepancy between M-cad and Pax7 stained SCs in normal and pathological muscle biopsies. In their study staining for Pax7 identified about 95% of the SCs in two normal muscles i.e., 5% were Pax7−/M-cad+, whereas in pathological biopsies Pax7−/M-cad+ SCs ranged from 1.6% to 15.2%. In addition, the use of Pax7 as a marker for SCs in ageing muscle warrants further caution as a decline in Pax7 reactivity has been reported in muscle of aged mice (Zammit 2008). Nevertheless, anti-Pax7 staining was recently used to assess the fibre type specific SC content in the vastus lateralis muscle of young and elderly men (Verdijk et al. 2007). As a control they compared the staining of Pax7 with NCAM in three young and three old subjects. More than 96% of the NCAM+ SCs showed also staining for Pax7, values in agreement with our present study. However, their SC quantification using Pax7, laminin and DAPI stained sections resulted in a considerably lower proportion of SC/N (<3%) for the young subjects compared to the results reported in other studies when the same NCAM ab has been used (Mackey et al. 2007b; Olsen et al. 2006; Petrella et al. 2006). Variation in SC frequency between different muscles or age groups may be explained by different properties of individual muscles, different physical activity or by factors related to normal ageing (Thornell et al. 2003). However, the large variation reported during normal conditions for the same muscles and age in different studies is more puzzling. Although such discrepancies could reflect interindividual variations, in light of the present results, they may also reflect the lack of a standardised method to identify and count the SCs.
Comparison of the MM method and previous NCAM results
When the proportion of SC/N for the power-lifters and control group was compared in our previous studies using only NCAM as the SC marker, the proportion of SC/N was significantly larger in the P and PAS groups than in the C group (Kadi et al. 1999a, b). When the MM method was used, the proportion of SC/N for the P and PAS groups was very different from that previously reported for the same individuals P (4.5% vs. 7.1%) and PAS (4.7% vs. 7.1%). On the other hand, the proportion of SC/N for the C groups was similar (4.4% vs. 4.0%). Thus, the proportion of SC/N did not differ between the P, PAS and C groups using the MM method. This indicates that the proportion of SC/N was overestimated in the strength-trained subjects in our previous studies (Kadi et al. 1999a, b). An overestimation of NCAM identified SCs is supported by the fact that the number of SC/F for the power-lifters with the MM method was approximately half of the values previously calculated on basis of the old method (Eriksson 2006). Different results in the power-lifters but similar results in untrained subjects indicate that the number of SC/N identified by NCAM and Mayers-HTX staining for the power-lifters was influenced by the exercise and/or the morphology of the biopsies reflecting years of strength training with and without stimulating substances. We know that strength training undoubtedly will influence repair and growth of muscle fibres which results in a partly myopathic appearance of the biopsies (Eriksson et al. 2005, 2006; Kadi 2000; Kadi et al. 1999a). An overestimation of SCs (as an explanation for the different results) in the trained subjects was verified through the analysis of biopsies from the vastus lateralis of four of the PAS subjects where the MM-method resulted in a four times lower figure than previously reported (0.15 SC/F vs. 0.63 SC/F). The advantage of the MM method in this context, except for using two SC markers and the possibility to exclude staining for nuclei, can be explained by the fact that staining for the basal lamina allowed the separation of cells which were outside the basal lamina from those inside the basal lamina (e.g., Fig. 9 where evident NCAM stained structures located outside the basal lamina of muscle fibres might easily have been counted as SCs). Thus, although our previous studies were done with the stringency and accuracy permitted by the method used at that time and with blinded personal data, the same person doing the measurements etc, it is obvious that the accuracy of the measurements has been improved using our new technique.
Implications of the MM method
Pax7 and NCAM staining patterns
We observed that the Pax7 antigen is sensitive to degradation as well as to strong fixation. For unfixed biopsies, the sections need to be immediately used and lightly fixed to prevent protein degradation and to preserve antigenicity of Pax7 and other antigens as well as nuclei morphology. This may explain why several groups have encountered difficulties with staining for anti-Pax7 (Personal communication).
The observed variation in the staining intensity for Pax7 may be explained by higher or lower expression of Pax7 in the nucleus, uneven distribution of Pax7 in the nucleus or different proportions of the nucleus being present in the stained section. SCs stained with NCAM but with undetectable staining for Pax7 were in a few cases obviously cut close to the edge of the nucleus, which render the possibility that a small part of a nucleus is detectable by DAPI but may not have sufficient anti-Pax7 reactivity to be noticed. One might therefore speculate whether the only reason for the reduced number of SCs identified by Pax7 is a consequence of it being expressed in the nucleus instead of a protein expressed on the surface or in the cytoplasm of the cell. However, NCAM+/Pax7− SCs with a nucleus of normal size were identified, which unequivocally confirms the existence of a NCAM+/Pax7− population of SCs. Nevertheless, the proportion of SCs that express both markers may be somewhat larger than the observed (94%). One explanation to Pax7 negative cells can be that SCs progressing into terminal differentiation will lose Pax7 expression (Olguin and Olwin 2004; Reimann et al. 2004; Zammit et al. 2004). This is certainly the case in areas of muscle damage and repair, e.g., Fig. 5, where there is a large discrepancy between cells stained for NCAM alone versus NCAM and Pax7. Further studies are underway to explore markers for myogenic progression such as the myogenic regulatory factors Myf5, MyoD and myogenin as well as other molecular markers for SCs in mice (Gnocchi et al. 2009).
Importance of staining of the basal lamina
In our present study we sometimes observed a weak staining of the basal lamina in the space between the myofibre and the SC. This might reflect that the SC is in a process of leaving the SC niche, an interpretation supported by the presence of some NCAM+/Pax7+ cells and small myofibres which had an unquestionable basal lamina of their own and which were adhering to or located close to the myofibre. These cells most likely correspond to our observation of some Pax7+ nuclei surrounded by dystrophin staining. Similar features of SCs leaving the niche have been presented in ultrastructural studies of SCs (Roth et al. 2000). In the present study, the SCs were often seen in close association to capillaries but clearly separated from them e.g., (Figs. 2, 4 and 9). On the contrary, Zheng et al. (2007) recently reported that human SCs (Pax7+or NCAM+) were observed to co-express endothelial cell markers in approximately 10% of the cells. These cells were located between muscle fibres (Zheng et al. 2007), thus their definition for a SC differs from the classical one. The authors added in parenthesis “co-expressed or are located close to cells that express endothelial antigens”. In our view, it is apparent that an additional marker, e.g. staining for laminin, would have been needed to verify the identity of those cells.
Our present results emphasise the importance of being able to separate the nuclei inside the basal lamina from nuclei outside the myofibres. We observed that the use of DAPI in combination with a marker for the myofibre basal lamina gave a significantly lower number of N/F compared to our previous results (P + PAS, p < 0.01) (Eriksson 2006). Still the result of the MM method showed that the mean number of N/F was clearly correlated to the mean fibre CSA, in agreement with previous studies (Eriksson et al. 2005; Kadi et al. 1999a, b; Kadi and Thornell 2000). This supports that upon muscle hypertrophy, when the muscle fibre cross-sectional area increases there is a need for more myonuclei to maintain the size of nuclear domains (Allen et al. 1999). Petrella et al. (2008) have studied three different groups of subjects who performed 16 w of resistance training. One group responded with a robust skeletal muscle hypertrophy, one with modest hypertrophy and one did not respond at all. The hypertrophy responder group showed a significant increase in SC/N, SC/F and number of myonuclei per fibre in agreement with the need of myonuclear addition via SC recruitment for myofibre expansion. Our elite power-lifters are certainly responders to intensive training for a long period. In this respect are our new results of a similar ratio between the number of SCs and the number of myonuclei in both controls and strength-trained subjects of interest. This shows that the increase in myonuclei in hypertrophic muscles physically accustomed to heavy load is balanced by a proportional increase in SCs.
Interestingly the mean nuclear domain in the PAS group was significantly larger than for the P and C groups. Several studies have speculated about a threshold for the size of a nuclear domain (Kadi et al. 2004b; Petrella et al. 2006). Our results support that one effect of the use of anabolic steroids might be to enhance the function of the nuclei allowing a more effective protein synthesis (Kadi 2008) thereby giving rise to larger nuclear domains than what has previously been noted in trained people (Petrella et al. 2008).
Lipofuscin granules
Autofluorescent lipofuscin pigment granules, often localised close to the SC nucleus and myonuclei is a feature which might be of inconvenience when using an immunofluorescence-based method. However, in addition to their characteristic shape and size they can always be distinguished from the specific fluorescence signal as they show fluorescence irrespective of the filter type.
How should the frequency of SCs be expressed?
In the past when the only way to identify SCs was to use electron microscopy, it was feasible to quantify SCs in relation to the number of myonuclei (Schmalbruch and Hellhammer 1976). Quantification of SCs in relation to number of myonuclei has prevailed even in light microscopy based approaches (Crameri et al. 2004, 2007; Eriksson et al. 2005; Kadi et al. 1999a, b, 2000; Mackey et al. 2007b; Sinha-Hikim et al. 2006). Another way to quantify SCs has been to relate the number of SC per mm length of muscle fibre (Sajko et al. 2004; Sinha-Hikim et al. 2003). Lately, several papers have also used the number of SC/F as a measure (Charifi et al. 2003; Dreyer et al. 2006; Kadi et al. 2004a, 2006; Olsen et al. 2006; Petrella et al. 2006; Renault et al. 2002a; Verdijk et al. 2007; Verney et al. 2008). Our new results show that the number of SC/N did not differ between the C group and power-lifter groups whereas, the number of SC/F was significantly higher in the power-lifters and positively correlated to the mean muscle fibre CSA. In our view the number of SC/F seems to be a more relevant expression for the SC frequency. It will not be influenced by uncertainties in the quantification of myonuclei or changes in the number of myonuclei due to muscle growth, pathological processes or ageing (Sajko et al. 2004). Nevertheless, until more information clarifying the discrepancies between different investigations is available, we recommend that both variables be used.
Conclusion
With regard to the increasing complexity in cell and molecular biology of SCs and other muscle progenitor cells, there is a definite need of a method, which allows a reliable identification and quantification of SCs and subtypes in sections of human muscle. The MM method as shown in the present study fulfils such criteria.
References
Allen DL, Roy RR, Edgerton VR (1999) Myonuclear domains in muscle adaptation and disease. Muscle Nerve 22:1350–1360
Bischoff R (1975) Regeneration of single skeletal muscle fibers in vitro. Anat Rec 182:215–235
Buckingham M (2006) Myogenic progenitor cells and skeletal myogenesis in vertebrates. Curr Opin Genet Dev 16:525–532
Buckingham M, Montarras D (2008) Skeletal muscle stem cells. Curr Opin Genet Dev 18:330–336
Cashman NR, Covault J, Wollman RL, Sanes JR (1987) Neural cell adhesion molecule in normal, denervated, and myopathic human muscle. Ann Neurol 21:481–489
Charifi N, Kadi F, Feasson L, Denis C (2003) Effects of endurance training on satellite cell frequency in skeletal muscle of old men. Muscle Nerve 28:87–92
Cooper RN, Butler-Browne GS, Mouly V (2006) Human muscle stem cells. Curr Opin Pharmacol 6:295–300
Crameri RM, Langberg H, Magnusson P, Jensen CH, Schroder HD, Olesen JL, Suetta C, Teisner B, Kjaer M (2004) Changes in satellite cells in human skeletal muscle after a single bout of high intensity exercise. J Physiol 558:333–340
Crameri RM, Aagaard P, Qvortrup K, Langberg H, Olesen J, Kjaer M (2007) Myofibre damage in human skeletal muscle: effects of electrical stimulation vs voluntary contraction. J Physiol 583:365–380
Day K, Shefer G, Richardson JB, Enikolopov G, Yablonka-Reuveni Z (2006) Nestin-GFP reporter expression defines the quiescent state of skeletal muscle satellite cells. Dev Biol 304:246–259
Dreyer HC, Blanco CE, Sattler FR, Schroeder ET, Wiswell RA (2006) Satellite cell numbers in young and older men 24 hours after eccentric exercise. Muscle Nerve 33:242–253
Eriksson A (2006) Strength training and anabolic steroids. The Department of Integrative Medical Biology, Section for Anatomy, Umeå University, Sweden and The Department of Health Science, Section for Medical Science, Luleå University of Technology, Sweden
Eriksson A, Kadi F, Malm C, Thornell LE (2005) Skeletal muscle morphology in power-lifters with and without anabolic steroids. Histochem Cell Biol 124:167–175
Eriksson A, Lindstrom M, Carlsson L, Thornell LE (2006) Hypertrophic muscle fibers with fissures in power-lifters; fiber splitting or defect regeneration? Histochem Cell Biol 126:409–417
Gnocchi VF, White RB, Ono Y, Ellis JA, Zammit PS (2009) Further characterisation of the molecular signature of quiescent and activated mouse muscle satellite cells. PLoS ONE 4:e5205
Gundersen HJ (1986) Stereology of arbitrary particles. A review of unbiased number and size estimators and the presentation of some new ones, in memory of William R. Thompson. J Microsc 143:3–45
Illa I, Leon-Monzon M, Dalakas MC (1992) Regenerating and denervated human muscle fibers and satellite cells express neural cell adhesion molecule recognized by monoclonal antibodies to natural killer cells. Ann Neurol 31:46–52
Irintchev A, Zeschnigk M, Starzinski-Powitz A, Wernig A (1994) Expression pattern of M-cadherin in normal, denervated, and regenerating mouse muscles. Dev Dyn 199:326–337
Ishido M, Uda M, Kasuga N, Masuhara M (2009) The expression patterns of Pax7 in satellite cells during overload-induced rat adult skeletal muscle hypertrophy. Acta Physiol (Oxf) 195:459–469
Kadi F (2000) Adaptation of human skeletal muscle to training and anabolic steroids. Acta Physiol Scand Suppl 646:1–52
Kadi F (2008) Cellular and molecular mechanisms responsible for the action of testosterone on human skeletal muscle. A basis for illegal performance enhancement. Br J Pharmacol 154:522–528
Kadi F, Thornell LE (2000) Concomitant increases in myonuclear and satellite cell content in female trapezius muscle following strength training. Histochem Cell Biol 113:99–103
Kadi F, Eriksson A, Holmner S, Butler-Browne GS, Thornell LE (1999a) Cellular adaptation of the trapezius muscle in strength-trained athletes. Histochem Cell Biol 111:189–195
Kadi F, Eriksson A, Holmner S, Thornell LE (1999b) Effects of anabolic steroids on the muscle cells of strength-trained athletes. Med Sci Sports Exerc 31:1528–1534
Kadi F, Ahlgren C, Waling K, Sundelin G, Thornell LE (2000) The effects of different training programs on the trapezius muscle of women with work-related neck and shoulder myalgia. Acta Neuropathol 100:253–258
Kadi F, Charifi N, Denis C, Lexell J (2004a) Satellite cells and myonuclei in young and elderly women and men. Muscle Nerve 29:120–127
Kadi F, Schjerling P, Andersen LL, Charifi N, Madsen JL, Christensen LR, Andersen JL (2004b) The effects of heavy resistance training and detraining on satellite cells in human skeletal muscles. J Physiol 558:1005–1012
Kadi F, Charifi N, Henriksson J (2006) The number of satellite cells in slow and fast fibres from human vastus lateralis muscle. Histochem Cell Biol 126:83–87
Kuang S, Rudnicki MA (2008) The emerging biology of satellite cells and their therapeutic potential. Trends Mol Med 14:82–91
Kuang S, Charge SB, Seale P, Huh M, Rudnicki MA (2006) Distinct roles for Pax7 and Pax3 in adult regenerative myogenesis. J Cell Biol 172:103–113
Kuang S, Kuroda K, Le Grand F, Rudnicki MA (2007) Asymmetric self-renewal and commitment of satellite stem cells in muscle. Cell 129:999–1010
Lanier LL, Testi R, Bindl J, Phillips JH (1989) Identity of Leu-19 (CD56) leukocyte differentiation antigen and neural cell adhesion molecule. J Exp Med 169:2233–2238
Lipton BH, Schultz E (1979) Developmental fate of skeletal muscle satellite cells. Science 205:1292–1294
Mackey AL, Esmarck B, Kadi F, Koskinen SO, Kongsgaard M, Sylvestersen A, Hansen JJ, Larsen G, Kjaer M (2007a) Enhanced satellite cell proliferation with resistance training in elderly men and women. Scand J Med Sci Sports 17:34–42
Mackey AL, Kjaer M, Dandanell S, Mikkelsen KH, Holm L, Dossing S, Kadi F, Koskinen SO, Jensen CH, Schroder HD, Langberg H (2007b) The influence of anti-inflammatory medication on exercise-induced myogenic precursor cell responses in humans. J Appl Physiol 103:425–431
Mauro A (1961) Satellite cell of skeletal muscle fibers. J Biophys Biochem Cytol 9:493–495
Mechtersheimer G, Staudter M, Moller P (1992) Expression of the natural killer (NK) cell-associated antigen CD56 (Leu-19), which is identical to the 140-kDa isoform of N-CAM, in neural and skeletal muscle cells and tumors derived therefrom. Ann N Y Acad Sci 650:311–316
Olguin HC, Olwin BB (2004) Pax-7 up-regulation inhibits myogenesis and cell cycle progression in satellite cells: a potential mechanism for self-renewal. Dev Biol 275:375–388
Olsen S, Aagaard P, Kadi F, Tufekovic G, Verney J, Olesen JL, Suetta C, Kjaer M (2006) Creatine supplementation augments the increase in satellite cell and myonuclei number in human skeletal muscle induced by strength training. J Physiol 573:525–534
Oustanina S, Hause G, Braun T (2004) Pax7 directs postnatal renewal and propagation of myogenic satellite cells but not their specification. Embo J 23:3430–3439
Peault B, Rudnicki M, Torrente Y, Cossu G, Tremblay JP, Partridge T, Gussoni E, Kunkel LM, Huard J (2007) Stem and progenitor cells in skeletal muscle development, maintenance, and therapy. Mol Ther 15:867–877
Petrella JK, Kim JS, Cross JM, Kosek DJ, Bamman MM (2006) Efficacy of myonuclear addition may explain differential myofiber growth among resistance-trained young and older men and women. Am J Physiol Endocrinol Metab 291:E937–E946
Petrella JK, Kim JS, Mayhew DL, Cross JM, Bamman MM (2008) Potent myofiber hypertrophy during resistance training in humans is associated with satellite cell-mediated myonuclear addition: a cluster analysis. J Appl Physiol 104:1736–1742
Reimann J, Brimah K, Schroder R, Wernig A, Beauchamp JR, Partridge TA (2004) Pax7 distribution in human skeletal muscle biopsies and myogenic tissue cultures. Cell Tissue Res 315:233–242
Relaix F, Montarras D, Zaffran S, Gayraud-Morel B, Rocancourt D, Tajbakhsh S, Mansouri A, Cumano A, Buckingham M (2006) Pax3 and Pax7 have distinct and overlapping functions in adult muscle progenitor cells. J Cell Biol 172:91–102
Renault V, Rolland E, Thornell LE, Mouly V, Butler-Browne G (2002a) Distribution of satellite cells in the human vastus lateralis muscle during aging. Exp Gerontol 37:1513–1514
Renault V, Thornell LE, Eriksson PO, Butler-Browne G, Mouly V (2002b) Regenerative potential of human skeletal muscle during aging. Aging Cell 1:132–139
Roth SM, Martel GF, Ivey FM, Lemmer JT, Metter EJ, Hurley BF, Rogers MA (2000) Skeletal muscle satellite cell populations in healthy young and older men and women. Anat Rec 260:351–358
Sajko S, Kubinova L, Cvetko E, Kreft M, Wernig A, Erzen I (2004) Frequency of M-cadherin-stained satellite cells declines in human muscles during aging. J Histochem Cytochem 52:179–185
Schmalbruch H, Hellhammer U (1976) The number of satellite cells in normal human muscle. Anat Rec 185:279–287
Schubert W, Zimmermann K, Cramer M, Starzinski-Powitz A (1989) Lymphocyte antigen Leu-19 as a molecular marker of regeneration in human skeletal muscle. Proc Natl Acad Sci U S A 86:307–311
Seale P, Sabourin LA, Girgis-Gabardo A, Mansouri A, Gruss P, Rudnicki MA (2000) Pax7 is required for the specification of myogenic satellite cells. Cell 102:777–786
Shefer G, Yablonka-Reuveni Z (2007) Reflections on lineage potential of skeletal muscle satellite cells: do they sometimes go MAD? Crit Rev Eukaryot Gene Expr 17:13–29
Shefer G, Van de Mark DP, Richardson JB, Yablonka-Reuveni Z (2006) Satellite-cell pool size does matter: defining the myogenic potency of aging skeletal muscle. Dev Biol 294:50–66
Sinha-Hikim I, Roth SM, Lee MI, Bhasin S (2003) Testosterone-induced muscle hypertrophy is associated with an increase in satellite cell number in healthy, young men. Am J Physiol Endocrinol Metab 285:E197–E205
Sinha-Hikim I, Cornford M, Gaytan H, Lee ML, Bhasin S (2006) Effects of testosterone supplementation on skeletal muscle fiber hypertrophy and satellite cells in community-dwelling older men. J Clin Endocrinol Metab 91:3024–3033
Snow MH (1978) An autoradiographic study of satellite cell differentiation into regenerating myotubes following transplantation of muscles in young rats. Cell Tissue Res 186:535–540
Thornell L-E, Eriksson A, Edström L (1983) Intermediate filaments in human myophaties. Dowben RM, Shay JW (eds) Cell and muscle motility, vol 4. Plenum Press, New York, pp 85–136
Thornell LE, Lindstrom M, Renault V, Mouly V, Butler-Browne GS (2003) Satellite cells and training in the elderly. Scand J Med Sci Sports 13:48–55
Verdijk LB, Koopman R, Schaart G, Meijer K, Savelberg HH, van Loon LJ (2007) Satellite cell content is specifically reduced in type II skeletal muscle fibers in the elderly. Am J Physiol Endocrinol Metab 292:E151–E157
Verney J, Kadi F, Charifi N, Feasson L, Saafi MA, Castells J, Piehl-Aulin K, Denis C (2008) Effects of combined lower body endurance and upper body resistance training on the satellite cell pool in elderly subjects. Muscle Nerve 38:1147–1154
Zammit PS (2008) The muscle satellite cell: the story of a cell on the edge. In: Schiaffino S, Partridge T (eds) Skeletal muscle repair and regeneration. Springer, pp 45–64
Zammit PS, Golding JP, Nagata Y, Hudon V, Partridge TA, Beauchamp JR (2004) Muscle satellite cells adopt divergent fates: a mechanism for self-renewal? J Cell Biol 166:347–357
Zammit PS, Partridge TA, Yablonka-Reuveni Z (2006a) The skeletal muscle satellite cell: the stem cell that came in from the cold. J Histochem Cytochem 54:1177–1191
Zammit PS, Relaix F, Nagata Y, Perez Ruiz A, Collins CA, Partridge TA, Beauchamp JR (2006b) Pax7 and myogenic progression in skeletal muscle satellite cells. J Cell Sci 119:1824–1832
Zheng B, Cao B, Crisan M, Sun B, Li G, Logar A, Yap S, Pollett JB, Drowley L, Cassino T, Gharaibeh B, Deasy BM, Huard J, Peault B (2007) Prospective identification of myogenic endothelial cells in human skeletal muscle. Nat Biotechnol 25:1025–1034
Acknowledgments
We wish to thank Mrs. Anna-Karin Olofsson and Margaretha Enerstedt for excellent technical assistance, Asst. profs Peter Anton and Leif Nilsson for statistical support, Ph.D Lena Carlsson and Prof. Fatima Pedrosa Domellöf for valuable comments on the manuscript and Ph.D Anders Eriksson for referring the power-lifter subjects to us. This study was supported by grants from the Association Française contre les Myopathies, MYORES Network of Excellence (contract 511978) of the European Union, the Swedish Research Council (12x3934), the Swedish National Centre for Research in Sports (108/08, 99/09) and the Medical Faculty of Umeå University, Sweden.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lindström, M., Thornell, LE. New multiple labelling method for improved satellite cell identification in human muscle: application to a cohort of power-lifters and sedentary men. Histochem Cell Biol 132, 141–157 (2009). https://doi.org/10.1007/s00418-009-0606-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-009-0606-0