Abstract
Background
Retinal ganglion cell loss is considered to be a cause of visual impairment in Alzheimer`s patients. Alterations in amyloid precursor protein (APP) processing and amyloid-β (Aβ) accumulation, key molecules associated with Alzheimer`s disease pathogenesis, may therefore contribute to retinal damage. We therefore investigated retinal APP processing and eye morphology in Alzheimer`s transgenic mouse models.
Methods
Eyes and brain samples of 2- to 18-month-old transgenic mice expressing human APP with the double Swedish mutation (APPswe) (APP K595N/M596L)(Tg2576) were compared with eyes and brain tissue from wild-type background C57BL6xSJL controls. In addition, 6- to 12-month-old double transgenic mice over-expressing human APPswe and mutant presenilin 1 with exon 9 deletion (APPswe/PS1-dE9) were compared with background controls of C57BL6xC3H strain. Tissue samples were fixed in formalin for immunohistochemistry, and dissected retinal and cerebellar extracts were frozen for Western blotting and enzyme-linked immunosorbent assay (ELISA). Monoclonal antibodies 1E8 and WO2 were used for immunohistochemical detection of APP and Aβ, whereas Aβ 42/40 levels were assayed by ELISA. APP and processed fragments were detected biochemically by Western blotting with domain-specific antibodies, using antibody WO2 (Aβ) and rabbit antibody 369 to the C-terminal domain of APP.
Results
Immunocytochemistry revealed strong cytoplasmic expression of APP and possibly Aβ in retinal ganglion cells and inner nuclear layer cells, and in lens and corneal epithelia for APP transgenic mice. Retinas from the APP transgenic mouse strains contained 18 to 70 kDa APP proteolytic products that were not detected in the cerebellum. We found a higher proportion of APP α-secretase generated C-terminal fragments in transgenic retinal tissues than β-secretase-generated C-terminal fragments. Very low level Aβ was detected in transgenic retinas by ELISA; retinal Aβ 42 was 75 times less than for transgenic brain. Aβ was not detected in mouse retina by Western blotting in our study, indicating much less generation of Aβ in retina than brain tissue.
Conclusions
Alzheimer’s mouse model retinas present with different APP proteolytic products and have a significantly lower production of amyloidogenic Aβ than found in brain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is the most common cause of dementia, with 27 million individuals affected worldwide. Patients are mostly 65 or older, and display progressive cognitive impairment, reduced executive functions, and behavioural changes. Currently there is substantial interest related to changes in vision in Alzheimer’s patients. In some AD patients, visual impairment is more likely to be cortical and associated with impaired visuomotor integration and object recognition [1, 2], but there is still little information regarding alterations in visual perception that might originate in the retina or optic nerve.
Histological examination of retinas from AD patients has demonstrated thinning of the retinal nerve fiber layer (RNFL) and a reduction in macula volume in line with pathological electroretinograms [3, 4]. Loss of ganglion cells and their axons, with resultant thinning of the neuroretinal rim of the optic nerve, is a characteristic feature of glaucomatous optic neuropathy [5]. Ophthalmologic examinations in Alzheimer’s patients show an increased visual impairment with glaucoma in 25.9% of AD cases compared to 5.2% in age-matched controls [6]. Another common feature in AD patients is impaired colour vision, which is hypothesised to be caused by the loss of smaller-sized axons of the optic nerve [7].
The molecular pathology of AD is characterized by accumulation of amyloid-β peptide (Aβ) with extracellular plaque formation, tau aggregation within neurofibrillary tangles, and progressive neuronal loss [8, 9]. Aβ is formed sequentially from transmembrane APP through β− and γ-secretase cleavage. γ−secretase cleavage is critical in generating Aβ species of varied length, including the strongly aggregating amyloidogenic Aβ 1–42. Mutations in presenilin (PS1 or PS2), which forms the catalytic core of the γ-secretase complex, enhance Aβ 1–42 production, leading to early onset and higher severity of disease in affected families [10]. To date, there is minimal data about retinal APP processing, leading us to question whether there are differences between brain and retinal APP processing and Aβ accumulation, resembling Alzheimer’s pathology, in animal models. Aβ deposits have been reported in glaucomatous optic nerve heads, drusen of age-related macula degeneration, and cataractous lens [11–14]. Intravitreal injection of Aβ causes retinal ganglion cell damage, illustrating Aβ toxicity to retinal tissue [15]. For age-related macula degeneration, Aβ is presumed to be involved in inflammation and neovascularisation [13]. Studies on the DBA/2J mouse model of glaucoma showed that sustained intraocular pressure (IOP) leads to extracellular Aβ accumulation in optic nerve heads and ganglion cell loss [16].
There is limited data demonstrating Αβ accumulation in human retinas of AD patients. Therefore, using AD animal models could be a useful tool for investigation of potential retinal changes caused by dysregulated APP processing. Several AD mouse models expressing mutant human AD related genes have been established. To mimic retinas afflicted by AD in this study, we used two well-established genetically modified mouse models, one over-expressing APP with the Swedish mutation (APPswe or Tg2576), the other being the APPswe and mutant presenilin 1 with exon 9 deletion (PS1-delE9). These mutations in humans cause Alzheimer’s disease, with individuals showing an early onset of disease [17, 18].
Two recent studies investigated retinal changes in AD mouse models. Ning et al. (2008) showed retinal degeneration in two APP/PS1 transgenic mouse lines with apoptotic cells detected in the retinal ganglion cell layer [19]. APP accumulation was reported in neurons of the inner nuclear layer and ganglion cells; Aβ deposits were reported in the nerve fiber layer and the retinal and choroidal vasculature, in an age-dependent manner. In addition, Shimazawa et al. found reduced retinal function in APP/PS1 transgenic mice with prolonged retinal visual potentials but reduced sensitivity to NMDA induced apoptosis [20].
In this study we investigated differences in APP metabolism in brain and retinal tissue. We compared the production of Aβ isoforms in brain and retina and investigated precursor cleavage products (APP CTFs) involved in APP breakdown by α- and β−secretase. Investigation of amyloidogenic APP processing in transgenic Alzheimer’s mouse retinas may give an indication whether toxic Αβ production in retina is likely to be sufficient to cause direct Aβ pathology in the eyes of Alzheimer’s patients.
Materials and methods
Animal models
The single transgenic (Tg2576) mice which contain the well-characterised hAPP695swe mutation were obtained from Karen Hsiao Ashe, Minnesota, USA [21]. Littermate wild-type C57Bl6/SJL controls were also utilized. Double transgenic mice over-expressing chimeric mouse/human APP695swe and presenilin1 exon-9 deletion (PS1-dE9) mutations were obtained from the Jackson Laboratory, Bar Harbor, ME, USA [22]. Both mutations are associated with familial Alzheimer’s disease. Background genotype mice, C57BL6/C3HeJ were compared with the double Tg mice. Mice aged 2 to 18 months were used for the study. Animals were housed in boxes (n = 3–5), with an ad libitum diet of standard mouse chow and a 12-hour light and dark cycle. Experimental protocols were approved by the animal ethics committee of the Department of Pathology, University of Melbourne, Australia.
Tissue collection
Mice were euthanized by CO2 asphyxiation. Brain and eyes were fixed in buffered formalin at 4°C for immunohistochemistry. Alternately brain and eyes were placed on dry ice, and further stored at −80°C for performing ELISA and western blot analyses.
Antibodies
Monoclonal mouse antibody WO2 detects residues 5–8 of human Aβ peptide [23]. For detection of carboxyl-terminal fragments (CTFs) we used the rabbit Ab 369 antibody raised to the cytoplasmic domain of human APP [24] (gift from Prof. S. Gandy, Philadelphia, PA, USA). Monoclonal mouse antibody 1E8 is raised to Aβ 17–24 [25]. G210 and G211 mouse monoclonal antibodies directed to the C-terminal ends of Aβ 40 and Aβ 42 were used in ELISA assay to assess the relative levels of these Aβ forms [26].
Immunohistochemical analysis
Formalin-fixed tissue was embedded in paraffin for sectioning. 5-μm sections were treated with 80% formic acid for 5 min at room temperature, then treated with 3% hydrogen peroxide for 5 minutes, and incubated in blocking buffer (50 mM Tris-HCl, 175 mM NaCl, pH 7.4, with 20% blocking serum corresponding to species for secondary Ab). Monoclonal 1E8 was used at 1:200 and WO2 at 1:1000 for 1 hour at room temperature. Sections were incubated with biotinylated secondary antibody (Dako LSAB) for 15 minutes at room temperature, followed by washing in PBS and incubation with streptavidin/horseradish peroxidase reagent (Dako LSAB) for 15 min at room temperature. After washing in PBS and water, sections were treated with chromagen (Dako DAB kit) and washed with water, then counterstained in Mayer`s Haematoxylin and mounted with DPX.
Western blot analysis
Frozen eyes were microscopically dissected on ice to conserve retinal extracts. Brain samples and 2–3 dissected pooled retinas were diluted in 400 μl phosphate-buffered saline containing protease inhibitors (Sigma P-2714) then sonicated with a Virsonic600 Probe (Virtis, NY) (3x30 sec bursts on ice). Total protein concentrations of the suspension were determined with a BCA assay (Pierce biotechnology, Rockford, IL, USA). Western blotting with APP and Aβ antibodies (WO2, Ab 369) was preformed as previously described [27]. Samples (20 μg protein) were mixed with SDS sample buffer containing β-mercaptoethanol, heated to 95°C for 5 minutes and then electrophoresed on 15% Tris-Tricine polyacrylamide gels. Proteins were transferred to nitrocellulose membrane (Bio-Rad, Regents Park, NSW, Australia). Western blots were developed with chemiluminescence (PerkinElmer).
ELISA analysis of Aβ isoforms
Enzyme-linked immunosorbent assay (ELISA) was performed for quantification of Aβ 1–40 and 1–42 peptides. Retinal homogenates from three different Tg 2576 mice were compared with wild-type mouse (C57Bl6/SJL) retinas (n = 4). Cerebellum from 8 Tg2576 and eight wild-type controls were also analysed. Samples were analysed as described previously using Aβ40- and Aβ42-specific G210 and G211 antibodies for capture and WO2 antibody for detection [26]. Data are presented as means ± SEM (Table 1).
Results
Localization of APP and Aβ expression in eyes from Alzheimer`s mouse models
APP and processed product distribution was examined by immunolabelling of paraffin-embedded tissue sections. Staining with antibody WO2 indicated robust expression of APP in Tg2576 retina at 14 months of age; there was strong cytoplasmic labelling of the ganglion cell layer and inner nuclear layer (Fig. 1a–c). Minimal APP was detected in the photoreceptor or pigmented retinal epithelial cell layers. There was also strong cytoplasmic expression of APP in the epithelial cell layers of the cornea and lens of these mice detected with antibody WO2 (not shown). Further labelling with Aβ antibody 1E8 indicated APP and possibly cytoplasmic Aβ labelling in the same regions (Fig. 1d–g). Positive Aβ labelling in peripheral retina within vacuolar structures of the ganglion cell layer indicate damaged capillaries (Fig. 1f). Retinas from age-matched wild-type background strain mice C57Bl6/SJL showed no reactivity for these Aβ antibodies, which are specific for the human APP and its derived Aβ sequence (Fig. 1h,i). Aβ 1E8 antibody-reactive “plaque-like” structures were not detected in the transgenic mouse eyes examined. Cortical brain plaques from Tg2576 mice showed positive labelling with the Aβ 1E8 antibody (Fig. 1j).
Expression and locallization of APP and derived products in eyes from Tg2576 mice. a,b,c Sections from 14-month-old transgenic mice labelled with WO2 antibody had strong cytoplasmic labelling of retinal ganglion cells (GCL, ganglion cell layer) and neurons of the inner nuclear layer (INL). The inner plexiform layer (IPL), outer plexiform layer (OPL), outer nuclear layer (ONL), photoreceptors (PR) and pigmented epithelial layer in c, (RPE) had minimal immunoreactivity. d,e 1E8 Aβ antibody positive labelling of corneal (d) and lens (e) epithelial cytoplasm in 14 month Tg2576 mouse sections. f,g 1E8 immunoreactivity had a similar pattern, with positive labelling of the cytoplasm of ganglion cells and the INL for 14-month-old Tg2576 retina, with a labelled capillary in peripheral region in f, and central region imaged in g. h,i 1E8 labelling of 14-month-old non-transgenic C57Bl6/SJL retina was negative. j 1E8 positive labelling of plaques in cortex from Tg2576 18-month-old brain. Bars, 20 μm
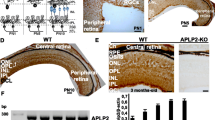
Eyes from 9-month-old TgAPP/PS1 mice had similar intracellular Aβ antibody labelling in the cytoplasmic compartment of retinal ganglion cells and inner nuclear layer cells, and in the epithelia of cornea and lens (Fig. 2a–d). These mice had possible small Aβ deposits associated with damaged capillaries within the ganglion cell layer and the inner nuclear layer (Fig. 2a,b); the inner plexiform and outer plexiform layers of the retinas had moderate immunoreactivity with the 1E8 antibody. Transgenic APP/PS1 brain cortex accumulate many brain plaque structures of various size that can be detected with the 1E8 antibody, as shown in Fig. 2e.
Expression of APP and products in TgAPP/PS1 9-month-old mouse eye. a,b 1E8 labelling had a similar expression pattern of immunoreactivity as seen for Tg2576 with labelling of cells in GCL and INL as well as moderate labelling of IPL and OPL, ONL and PR labelling was minimal for central retina (a) and outer retina (b). Again corneal epithelium (c) and lens epithelium (d) showed strong cytoplasmic labelling with the 1E8 antibody. e 1E8 positive labelling of TgAPP/PS1 brain cortical plaques of a 12-month-old mouse. Bars, 20 μm
Biochemical analysis of retinal and brain APP processing in Tg2576 and TgAPP/PS1 mice
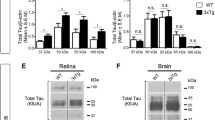
To investigate APP processing we used antibody WO2 for detection of human full length APP and Aβ sequence-containing cleavage products. Aged Tg2576 mouse retinal extracts were compared with age-matched cerebellum brain extracts and corresponding wild-type controls Fig. 3a,b). Double transgenic APP/PS1 retinas were analysed in parallel. Tg2576 retinas showed additional cleavage products between 18 and 70 kDa that were not prominent in brain extracts. 4 kDa Aβ was not detectable by Western blotting in these retinal extracts. In transgenic brain there was a very strong signal for Aβ at the expected apparent mobility of 4 kDa (Fig. 3b, lane 4).
Western blot analysis of APP processing in APP transgenic retina and brain. a,b Protein from total homogenates of retina, cerebellum, and optic nerve was analysed by electrophoresis and blotted with WO2 antibody which detects full length human APP (APP FL), the APP CTFβ proteolytic intermediate, and Aβ peptide. APP and CTFβ were detected in Tg2576 cerebellum (CB) for 11 and 16 months of age; Aβ was strongly detected only in the 16-month-old brain sample (b, lane 4). Comparison of retina and optic nerve (ON, b lanes 1 and 2) revealed a similar pattern of APP processing as for retina. Detection of APP and products was weaker for the retina from TgAPP/PS1 mouse (a, lane 6). *Proteolytic products of APP between 18 -70 kDa were detected in retina and not the brain samples. c,d Parallel samples as used for a,b were blotted with antibody to the cytoplasmic domain of APP (Ab 369) to compare APP CTF processing intermediates. This shows strong detection of CTFα in retina of Tg2576 (c, lane 3; d, lane 8). Cerebellum from Tg2576 and wild-type mice had a much higher level of CTFβ than produced by retina (c, lane 1; d, lanes 3 and 4)
Retinal extracts of transgenic 6-month-old APP/PS1 mice showed a pattern similar to that of the single transgenic Tg2576 mice with fragments between 13 and 70 kDa, but with an overall weaker signal pattern compared to retinas from Tg2576 mice (Fig. 3a, lane 6). As for the Tg2576 line, we have not detected the Aβ peptide in retinal extracts from the double transgenic mouse line by Western blotting (Fig. 3a,b).
APP undergoes an initial cleavage step by α- or β-secretase to yield the corresponding intermediate C-terminal fragments containing the complete Aβ (CTFβ) or truncated Aβ sequence (CTFα). These intermediate proteolytic precursors were analysed by Western blotting with the rabbit Ab 369 to the cytoplasmic C-terminal region of APP (Fig. 3 C,D). This revealed that the Tg2576 retinas produce more CTFα than CTFβ, leading to an increased ratio of CTFα/CTFβ compared to that found in brain tissue from Tg2576 or the background wild-type cerebellum. This low level of detectable intermediate Aβ precursor is in agreement with minimal Aβ peptide detection in the retinas.
ELISA analysis of Aβ 1–40 and 1–42 levels in Tg2576 retina and cerebellum
To further investigate expression of Aβ isoforms 1–40 and 1–42 in retinas and brain fractions from Tg2576 mice, we performed a sandwich ELISA with Aβ C-terminal antibodies specific for Aβ1–40 (G210) and Aβ 1–42 (G211), as used in previous studies from our laboratory [26]. In wild-type retinas, Aβ 1–40 was below detectable limits (Table 1). In comparison we detected 14.1 pmol/g protein of Aβ 1–42 in retinal extracts of Tg2576; wt retina had significantly less Aβ 1–42 of 8.53 pmol/g protein. Tg2576 retina Aβ 1–40 levels of 0.19 pmol/g protein were significantly lower than the Aβ 1–42 level. However, we note that the Tg2576 retina had a similar level of Aβ to that detectable in cerebellum from non-transgenic mice, which do not produce Aβ plaques, again indicating that the retinas are not producing Aβ at a significant level, and would be unlikely to accumulate as microscopically visible Aβ aggregates.
In comparison, human cortical tissue and Tg2576 cerebellar tissue revealed considerably greater production of the Aβ peptide both for 1–40 and 1–42 (Table 1). Level of Aβ 1−42 was 75 times greater for Tg2576 cerebellum than for Tg2576 retina.
Discussion
We analysed APP metabolism and assessed Aβ production in retinal tissue from two well-established Alzheimer’s mouse models. Overexpression of the human APP Swedish mutant gene in the Tg2576 mouse results in age-dependent accumulation of brain Aβ. These animals develop amyloid plaque deposition and ultimately memory deficits at 10 months of age [21]. The second transgenic line, with APPswe/PS1-del9 transgenes, produces earlier deposition of Aβ in brain plaques, and develops memory deficits from the age of 6 months.
Recent studies have demonstrated retinal degeneration, utilising TUNEL staining for identification of apoptotic cells; this group also reported Aβ accumulation in these Alzheimer’s mouse models [19]. In addition, Shimazawa et al. looked at functional changes, finding delayed latency of electroretinal potential conduction in APP/PS1 mice compared with wild-type controls [20]. Despite these largely histological studies, it was unclear whether the Alzheimer’s mice produce sufficient quantities of Aβ peptide aggregates to affect retinal integrity. Using two Aβ antibodies for detection of APP, CTFβ, and/or Aβ, we found significant cytoplasmic labelling of the ganglion cells and cell bodies of the inner nuclear layer. In addition, both WO2 and 1E8 Aβ antibodies strongly labelled the epithelial cells of the cornea and lens of both transgenic lines, consistent with the finding of Aβ in lens of Alzheimer’s patients [14]. Labelling with these antibodies was negligible in wild-type control tissues, since the antibodies are raised to regions of the Aβ peptide only found in the human APP sequence. There was no significant immunolabelling of the photoreceptor cells in retinas in our transgenic lines.
Our study, in agreement with previous investigations [19], did not find Aβ amyloid plaque-like formation in retina like the plaques which accumulate in the brains of these mice. Therefore, differences in APP gene expression and peptide formation between brain and retinal tissue are to be anticipated.
This is the first report of APP proteolytic products (apart from Aβ) in retinas of AD mouse models. APP and products were detected in retinal and cerebral extracts analysed by gel electrophoresis and Western blotting, using WO2 Aβ and APP cytoplasmic domain antibodies. Significant APP was detected in retina from both transgenic strains. The pattern of APP products showed several differences between transgenic brains and retinal extracts. In particular, we detected additional apparent proteolytic products between 70 and 18 kDa in the transgenic retinas. This indicates that APP may undergo alternative processing in the retina compared with brain tissue. More work will be needed to clarify the features and origin of these protein products. Interestingly, Aβ was only detectable in transgenic brain in the Western blot analysis, and this correlated with prominent expression of Aβ plaques in brains of these mice.
In contrast, there was apparent detection of Aβ by ELISA in all of our samples, reflecting increased sensitivity of detection by this method. The ELISA data however, reveal significantly lower Aβ levels in retina than in brain tissue, with Aβ levels in transgenic mouse retina being still well above wild-type controls. We consider that these low levels are caused by low expression of retinal β-secretase. β-secretase is known to be a crucial factor contributing to amyloidogenic APP proteolytic processing, as it generates the N-terminus of Aβ. Brain contains high expression of β-secretase activity, which is elevated in Alzheimer’s disease [28, 29]. Although there may be abundant full-length APP expression, peripheral tissue β-secretase activity is considerably lower, resulting in only minor Aβ production in most non-brain tissues [30].
We directly compared CTFα and CTFβ levels in Tg2576 and the double transgenic mouse lines. We found similar CTFα and CTFβ levels in Tg2576 brain tissue. In comparison, Tg2576 retinas have high CTFα but only very low CTFβ expression levels, indicating minimal activation of amyloidogenic β-secretase activity [10]. It is known that the α-secretase APP degradation pathway predominates in peripheral tissues [31]. These results were also in agreement with the work of Lehmann et al., who described a high APP CTFα/CTFβ ratio in whole eye and other peripheral tissues in homogenates from another mutant APP mouse model (R1.40) [30]. Our TgAPP/PS1 model showed minimal APPα or CTFβ expression levels in retina (Fig. 3 A,C lane 6).
Our findings indicate only trace amounts of Aβ in retina, even in transgenic mice over-expressing APP. In combination with low CTFβ detection in these studies, we consider that Alzheimer retinal tissue may be less affected by Aβ toxicity than suggested by other immunochemical studies alone. To date, there are only limited biochemical reports implicating accumulation of Aβ in retina from AD patients.
Whether visual impairment in Alzheimer’s patients is due to retinal pathology or due to extraretinal ocular pathology remains unclear. Bayer et al. measured a high occurrence rate of elevated intraocular pressure in Alzheimer’s patients [6]. Glaucoma is defined by retinal papillary changes, as well as elevated pressure. Other studies showed glaucoma-like thinning of the nerve fibre layer in Alzheimer cases using optical coherence tomography [4, 32]. Possible association of APP and Aβ deposition in the anterior eye segment with these changes is unknown. Our immunohistochemistry revealed high expression of APP in the lens and the corneal epithelial cell layers of the transgenic mouse models. Strong expression of APP in the lens epithelium of APP transgenic mice correlates with reported deposits of Aβ peptides in the cytoplasm of lens cells from AD patients [14]. Examination of trabecular meshwork properties and anterior chamber depth in Alzheimer’s patients and AD mouse models may be a future approach to further investigate visual disturbances in Alzheimer’s disease patients in the future.
References
Mendez MF, Mendez MA, Martin R, Smyth KA, Whitehouse PJ (1990) Complex visual disturbances in Alzheimer’s disease. Neurology 40:439–443
Tippett WJ, Krajewski A, Sergio LE (2007) Visuomotor integration is compromised in Alzheimer’s disease patients reaching for remembered targets. Eur Neurol 58:1–114. doi:10.1159/000102160
Gary (1989) Abnormal pattern electroretinograms in patients with sede dementia of the alzheimer type. Ann Neurol 26:226–231
Iseri PK, Altinas O, Tokay T, Yuksel N (2006) Relationship between cognitive impairment and retinal morphological and visual functional abnormalities in Alzheimer disease. J Neuroophthalmol 26:18–24. doi:10.1097/01.wno.0000204645.56873.26
Ojima T, Tanabe T, Hangai M, Yu S, Morishita S, Yoshimura N (2007) Measurement of retinal nerve fiber layer thickness and macular volume for glaucoma detection using optical coherence tomography. Jpn J Ophthalmol 51:197–203. doi:10.1007/s10384–006-0433-y
Bayer AU, Keller ON, Ferrari F, Maag KP (2002) Association of glaucoma with neurodegenerative diseases with apoptotic cell death: Alzheimer’s disease and Parkinson’s disease. Am J Ophthalmol 133:135–137. doi:10.1016/S0002-9394(01)01196-5
Syed AB, Armstrong RA, Smith CU (2005) A quantitative analysis of optic nerve axons in elderly control subjects and patients with Alzheimer’s disease. Folia Neuropathol 43:1–69
Masters CL, Simms G, Weinman NA, Multhaup G, McDonald BL, Beyreuther K (1985) Amyloid plaque core protein in Alzheimer disease and Down syndrome. Proc Natl Acad Sci USA 82:4245–4249. doi:10.1073/pnas.82.12.4245
Hanger DP, Brion JP, Gallo JM, Cairns NJ, Luthert PJ, Anderton BH (1991) Tau in Alzheimer’s disease and Down’s syndrome is insoluble and abnormally phosphorylated. Biochem J 275(Pt 1):99–104
Evin G, Weidemann A (2002) Biogenesis and metabolism of Alzheimer’s disease Abeta amyloid peptides. Peptides 23:1285–1297. doi:10.1016/S0196-9781(02)00063-3
Janciauskiene S, Krakau T (2001) Alzheimer’s peptide: a possible link between glaucoma, exfoliation syndrome and Alzheimer’s disease. Acta Ophthalmol Scand 79:328–329. doi:10.1034/j.1600-0420.2001.790327.x
Janciauskiene S, Krakau T (2003) Alzheimer’s peptide and serine proteinase inhibitors in glaucoma and exfoliation syndrome. Doc Ophthalmol 106:215–223. doi:10.1023/A:1022949121078
Yoshida T, Ohno-Matsui K, Ichinose S, Sato T, Iwata N, Saido TC, Hisatomi T, Mochizuki M, Morita I (2005) The potential role of amyloid beta in the pathogenesis of age-related macular degeneration. J Clin Invest 115:2793–2800. doi:10.1172/JCI24635
Goldstein LE, Muffat JA, Cherny RA, Moir RD, Ericsson MH, Huang X, Mavros C, Coccia JA, Faget KY, Fitch KA, Masters CL, Tanzi RE, Chylack LT Jr, Bush AI (2003) Cytosolic beta-amyloid deposition and supranuclear cataracts in lenses from people with Alzheimer’s disease. Lancet 361:1258–1265. doi:10.1016/S0140-6736(03)12981-9
Guo L, Salt TE, Luong V, Wood N, Cheung W, Maass A, Ferrari G, Russo-Marie F, Sillito AM, Cheetham ME, Moss SE, Fitzke FW, Cordeiro MF (2007) Targeting amyloid-beta in glaucoma treatment. Proc Natl Acad Sci USA 104:13444–13449. doi:10.1073/pnas.0703707104
Goldblum D, Kipfer-Kauer A, Sarra GM, Wolf S, Frueh BE (2007) Distribution of amyloid precursor protein and amyloid-beta immunoreactivity in DBA/2J glaucomatous mouse retinas. Invest Ophthalmol Vis Sci 48:5085–5090. doi:10.1167/iovs.06-1249
Haass C, Lemere CA, Capell A, Citron M, Seubert P, Schenk D, Lannfelt L, Selkoe DJ (1995) The Swedish mutation causes early-onset Alzheimer’s disease by beta-secretase cleavage within the secretory pathway. Nat Med 1:1291–1296. doi:10.1038/nm1295-1291
Prihar G, Verkkoniem A, Perez-Tur J, Crook R, Lincoln S, Houlden H, Somer M, Paetau A, Kalimo H, Grover A, Myllykangas L, Hutton M, Hardy J, Haltia M (1999) Alzheimer disease PS-1 exon 9 deletion defined. Nat Med 5:1090. doi:10.1038/13383
Ning A, Cui JZ, To E, Hsiao Ashe K, Matsubara JA (2008) Amyloid beta deposits lead to retinal degeneration in a mouse model of alzheimer disease. Invest Ophthalmol Vis Sci
Shimazawa M, Inokuchi Y, Okuno T, Nakajima Y, Sakaguchi G, Kato A, Oku H, Sugiyama T, Kudo T, Ikeda T, Takeda M, Hara H (2008) Reduced retinal function in amyloid precursor protein-over-expressing transgenic mice via attenuating glutamate-N-methyl-d-aspartate receptor signaling. J Neurochem 107:279–290. doi:10.1111/j.1471-4159.2008.05606.x
Hsiao K, Chapman P, Nilsen S, Eckman C, Harigaya Y, Younkin S, Yang F, Cole G (1996) Correlative memory deficits, Abeta elevation, and amyloid plaques in transgenic mice. Science 274:99–102. doi:10.1126/science.274.5284.99
Jankowsky JL, Slunt HH, Ratovitski T, Jenkins NA, Copeland NG, Borchelt DR (2001) Co-expression of multiple transgenes in mouse CNS: a comparison of strategies. Biomol Eng 17:157–165. doi:10.1016/S1389-0344(01)00067-3
Ida N, Hartmann T, Pantel J, Schroder J, Zerfass R, Forstl H, Sandbrink R, Masters CL, Beyreuther K (1996) Analysis of heterogeneous A4 peptides in human cerebrospinal fluid and blood by a newly developed sensitive Western blot assay. J Biol Chem 271:22908–22914. doi:10.1074/jbc.271.37.22908
Buxbaum JD, Gandy SE, Cicchetti P, Ehrlich ME, Czernik AJ, Fracasso RP, Ramabhadran TV, Unterbeck AJ, Greengard P (1990) Processing of Alzheimer beta/A4 amyloid precursor protein: modulation by agents that regulate protein phosphorylation. Proc Natl Acad Sci USA 87:6003–6006. doi:10.1073/pnas.87.15.6003
Culvenor JG, Henry A, Hartmann T, Evin G, Galatis D, Friedhuber A, Jayasena UL, Underwood JR, Beyreuther K, Masters CL, Cappai R (1998) Subcellular localization of the Alzheimer’s disease amyloid precursor protein and derived polypeptides expressed in a recombinant yeast system. Amyloid 5:79–89
Fodero-Tavoletti MT, Smith DP, McLean CA, Adlard PA, Barnham KJ, Foster LE, Leone L, Perez K, Cortes M, Culvenor JG, Li QX, Laughton KM, Rowe CC, Masters CL, Cappai R, Villemagne VL (2007) In vitro characterization of Pittsburgh compound-B binding to Lewy bodies. J Neurosci 27:10365–10371. doi:10.1523/JNEUROSCI.0630-07.2007
Culvenor JG, McLean CA, Cutt S, Campbell BC, Maher F, Jakala P, Hartmann T, Beyreuther K, Masters CL, Li QX (1999) Non-Abeta component of Alzheimer’s disease amyloid (NAC) revisited. NAC and alpha-synuclein are not associated with Abeta amyloid. Am J Pathol 155:1173–1181
Vassar R, Bennett BD, Babu-Khan S, Kahn S, Mendiaz EA, Denis P, Teplow DB, Ross S, Amarante P, Loeloff R, Luo Y, Fisher S, Fuller J, Edenson S, Lile J, Jarosinski MA, Biere AL, Curran E, Burgess T, Louis JC, Collins F, Treanor J, Rogers G, Citron M (1999) Beta-secretase cleavage of Alzheimer’s amyloid precursor protein by the transmembrane aspartic protease BACE. Science 286:735–741. doi:10.1126/science.286.5440.735
Holsinger RM, McLean CA, Beyreuther K, Masters CL, Evin G (2002) Increased expression of the amyloid precursor beta-secretase in Alzheimer’s disease. Ann Neurol 51:783–786. doi:10.1002/ana.10208
Lehman EJ, Kulnane LS, Lamb BT (2003) Alterations in beta-amyloid production and deposition in brain regions of two transgenic models. Neurobiol Aging 24:645–653. doi:10.1016/S0197-4580(02)00153-7
Evin G, Zhu A, Holsinger RM, Masters CL, Li QX (2003) Proteolytic processing of the Alzheimer’s disease amyloid precursor protein in brain and platelets. J Neurosci Res 74:386–392. doi:10.1002/jnr.10745
Paquet C, Boissonnot M, Roger F, Dighiero P, Gil R, Hugon J (2007) Abnormal retinal thickness in patients with mild cognitive impairment and Alzheimer’s disease. Neurosci Lett 420:97–99. doi:10.1016/j.neulet.2007.02.090
Acknowledgments
We thank Karen Hsiao Ashe for the Tg2576 mice, Laura Leone for assistance with histology, and Katrina Laughton for ELISA assays. We thank the Bethlehem Griffiths Research Foundation, Victoria and the Australian National Health and Medical Research Council for funding support.
Author information
Authors and Affiliations
Corresponding author
Additional information
The authors have full control of all primary data, and allow Graefe’s Archive for Clinical and Experimental Opthalmology to review such data upon request.
Rights and permissions
About this article
Cite this article
Dutescu, R.M., Li, QX., Crowston, J. et al. Amyloid precursor protein processing and retinal pathology in mouse models of Alzheimer’s disease. Graefes Arch Clin Exp Ophthalmol 247, 1213–1221 (2009). https://doi.org/10.1007/s00417-009-1060-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-009-1060-3