Abstract
Pulmonary fat embolism (PFE) is frequently encountered in blunt trauma. The clinical manifestation ranges from no impairment in light cases to death due to right-sided heart failure or hypoxaemia in severe cases. Occasionally, pulmonary fat embolism can give rise to a fat embolism syndrome (FES), which is marked by multiorgan failure, respiratory disorders, petechiae and often death. It is well known that fractures of long bones can lead to PFE. Several authors have argued that PFE can arise due to mere soft tissue injury in the absence of fractures, a claim other authors disagree upon. In this study, we retrospectively examined 50 victims of blunt trauma with regard to grade and extent of fractures and crushing of subcutaneous fatty tissue and presence and severity of PFE. Our results indicate that PFE can arise due to mere crushing of subcutaneous fat and that the fracture grade correlated well with PFE severity (p = 0.011). The correlation between PFE and the fracture severity (body regions affected by fractures and fracture grade) showed a lesser significant correlation (p = 0.170). The survival time (p = 0.567), the amount of body regions affected by fat crushing (p = 0.336) and the fat crush grade (p = 0.485) did not correlate with the PFE grade, nor did the amount of body regions affected by fractures. These results may have clinical implications for the assessment of a possible FES development, as, if the risk of a PFE is known, preventive steps can be taken.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Fat embolism is a frequent phenomenon in blunt force trauma with incidences reported as ranging from 47% to 100% [1–5].
There are two main pathophysiological theories as to the development of fat embolism, the mechanical theory and the biochemical theory. The mechanical theory of Gossling et al. [6], states that fat droplets are released into the venous system and become lodged in the pulmonary capillary beds, from which they travel via arteriovenous shunts to other organs. The biochemical theory, on the other hand, assumes that hormonal changes caused by trauma or other disorders such as sepsis, release chylomicrons into the vascular system. According to Baker et al. [7], the local hydrolysis of fat emboli by pneumocytes generates free fatty acids, which enter other organs and cause multiorgan dysfunction. This biochemical theory may explain the presence of fat embolism in albeit rare non-traumatic cases [8].
Its importance in forensic pathology lies in two features, namely that its presence indicates that the victim had a blood circulation at the time of injury sustainment, i.e. was alive and that it can cause death due to a marked increase in pressure in the pulmonary vasculature with right heart damage and failure [9] or hypoxaemia. The severity of clinical symptoms of fat embolism may range between none and death due to cardiopulmonary collapse. The mere presence of embolised fat is not to be confused with a fat embolism syndrome (FES). This syndrome, which was first described by Zenker in 1862 and clinically diagnosed by von Bergmann in 1873 [10] represents a systemic affliction with multiorgan dysfunction, typically manifesting itself with pulmonary dysfunction and respiratory failure, petechiae and fever [11].
In the mechanical theory, it is generally assumed that the fat originates from osseous fractures [12–14] and is embolised into different organs, notably the lungs.
Several groups have found that pulmonary fat embolism (PFE) may occur in the absence of fractures, the origin of the fat being crushed soft tissue [5, 12, 15], a feature also witnessed regularly in our own autopsy case-load.
Mudd et al. [16] examined the occurrence of PFE in deaths after blunt trauma and concluded that there was no correlation of PFE and the number of fractures found and that soft tissue injury is to be considered the primary cause of PFE.
This contradicts Falzi et al. [17], who state that PFE severity correlates with the amount of osseous fractures and the survival time. According to this study, PFE in a brief survival time (minutes) was present in only 37% of the cases, while in a survival time of several hours, a 60 PFE positivity was noted. After a survival time of several days, the PFE rate sunk to 42%.
Therefore, according to the literature, several aspects of traumatic PFE seem unclear:
-
Can PFE arise in the absence of fractures?
-
Does the grade of PFE correlate to the extent of fractures?
-
Does a survival time dependency regarding PFE positivity exists?
In addition to these points, we asked ourselves, whether a correlation between the extent of fat crushing and PFE grade exists, and if so, does the abundance of subcutaneous fat as encountered in obese persons influence the PFE grade.
We therefore undertook to examine whether the severity of a PFE correlates with subcutaneous fat contusion, fracture severity, age, body mass index and survival time.
Method and materials
Cases
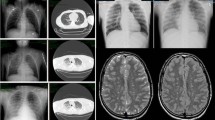
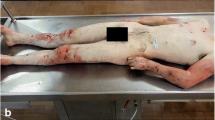
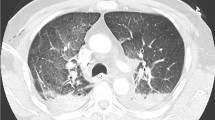
We retrospectively selected 50 cases delivered to our institute for forensic autopsy, which fulfilled the following criteria: (a) all cases must have suffered a blunt trauma; (b) the corpses underwent full body dissection, i.e. dissection not only of the organs of the head, and trunk, but also of the soft tissues of the back and the extremities; (c) no laceration of the right atrium or ventricle was present as such damage to the right heart may inhibit it from pumping fat-laden blood into the pulmonary vasculature, thus preventing a PFE; (d) no intense cardiac resuscitation was performed, as such resuscitation attempts may give rise to a PFE. This means that—to our knowledge—no emergency crews or laypersons performed a CPR and that no CPR typical signs (electroshock burns, rib fractures lacking surrounding haemorrhage at typical resuscitation sites) were present. Intubation and administration of vasoactive drugs did not constitute exclusion criteria. However, unknown layperson resuscitation attempts without signs of a forceful (intense) resuscitation could not be ruled out. In 29 cases, computed tomography was performed during lifetime and/or post-mortem.
Autopsy protocols of 50 cases, which fulfilled inclusion and exclusion criteria, were studied. In these protocols, the state of the skull, spine, rib cage, pelvis and extremity skeleton were described with regard to fractures as were the soft tissues of the head, trunk and extremities regarding fat crushing. The face, hands and feet were not dissected in these autopsies. Here, we relied on the computer tomography reports in 29 of 50 cases and in the remaining 21 cases on the accounts in the autopsy protocols that the skeletal structures were stable. Obviously, small, non-dislocated fractures of the face, hands and feet may have been missed in these cases. However, according to our experience, direct trauma to these regions is generally seen even without dissection.
The cases were analysed regarding the presence and severity of PFE, injuries, age, sex, body mass index and survival time. The study population consisted of 34 males (mean age: 47.8 years, SD: 20.4) and 16 females (mean age: 54.3 years, SD: 26.7) corpses.
Survival time
The survival time was estimated based on the information given on the course of the incident and given in hours, or quarters of an hour. A survival time of “0.1 h” indicates that death occurred very rapidly, within minutes, but not immediately.
PFE
PFE was assessed by retrospectively studying the autopsy protocols. The initial diagnosis was made on thin unfixed, haemolysed lung samples (mean width 1.6 mm) which were stained with Sudan III. Histological grading of these samples was performed by board-certified forensic pathologists according to Falzi and collaborators [17] (Table 1). We also awarded half grades of PFE. A PFE of, for example, 2–3 was graded as “2.5”.
Injuries
Injuries were divided into fractures and crushing of the subcutaneous fatty tissue. Injuries of the inner organs were not examined in this study.
Fat crushing
Every affected body region (Table 2) received one point, i.e. no crushed body region resulted in zero points and a crushing of every body region equalled five points. The fat crushing was graded as shown in Table 3. The severity of the fat crushing was calculated as being the amount of body regions affected multiplied by the crush grade.
Fractures
In analogy to fat crushing grading, the body was divided into five regions (Table 4), in which either no fracture, isolated or extensive/comminute fractures were seen (Table 5). All long bones as well as vertebrae and flat bones such as the skull and pelvis were examined. The overall severity of the fracturing was calculated as being the body region affected multiplied by the fracture grade per region.
Statistics
The statistical package PASW 18, SPSS Inc., was used for the analysis of the data. According to the Kolmogorov–Smirnov test of normality, the variables “survival time”, “crushed body region”, “crushed severity”, “crushed region × severity”, “fracture severity”, “fracture body region” and “fracture severity × body region” are not normally distributed (p < 0.05). Therefore, we used non-parametric statistical techniques. Relationships were explored between variables.
Results
The results gleamed from the autopsy data are shown in Table 6. The results of the statistical analysis (Spearman’s rho correlation coefficient and p value) are shown in Table 7.
Five cases presented fat crushing in the absence of fractures, and of these, only three displayed a PFE. On the other hand, three cases presented with fractures but without detectable fat crushing had a PFE.
There is a statistically significant correlation (p < 0.05) between grade of PFE and fracture grade.
The significances of the correlation coefficients remained the same, even after controlling the influence of the age, height, weight and BMI. Still, the only statistically significant correlation was that between PFE and the fracture grade.
After splitting the cases in two sex groups, the significances remained as shown above in the male group. The significance of the PFE fracture grade correlation became even stronger (p < 0.01). In the female group however, this significant correlation disappears (p > 0.05).
Although the overall fracture distribution correlated better to PFE than fat crushing, it was not significant (p = 0.170). Indeed, only the fracture grade per body region showed a statistically relevant correlation with the PFE grade (p = 0.011).
Nineteen cases had a very short survival time of a maximum of a few minutes (Δt = 0.1 h in Table 6). Of these, 14 (73.7%) were PFE positive, whereas 5 (26.3%) were PFE negative. There was, however, no significant correlation between the PFE grade and the survival time (p = 0.567).
Although our results tended to show that more PFE was seen when several body regions experienced fat crushing, there was no significant statistical correlation (p = 0.336).
The grade of fat crushing correlated even less with the PFE grade (p = 0.485) and the crush severity (affected body regions × fat crushing grade) showed an even less significant correlation (p = 0.616).
Similarly, insignificant results were obtained when comparing the PFE grade with the amount of body regions displaying fractures.
Discussion
The presented study consists of a small study group and has two shortcomings, namely that we cannot fully exclude a cardiopulmonary resuscitation by laypersons and that in several cases, the faces, hands and feet could not be examined other than by external inspection.
Nevertheless, the following conclusions may be drawn from our results:
Existence of traumatic PFE without osseous fractures
According to our data, traumatic PFE can occur due to fat crushing in the absence of fractures. Three cases with fat crushing showed PFE without detectable fractures. Although this constellation proved to be rare, it coincided with the results of other groups [5, 12, 15].
Correlation of PFE with fractures
Falzi et al. [17] showed a correlation of the amount of fractures with the prevalence of PFE. Our results underlined this observation and showed a significant correlation between PFE and the fracture grade. In other words, according to our results, the more comminute a fracture is, the higher the PFE grade will be. These results may be explained by the local energy necessary for the development of severe, comminute fractures; for such fractures to develop, very high impact energy is necessary. This high impact energy may force fat into the vascular bed, and ultimately give rise to a PFE.
After gender separation, this significance became even stronger in the male group. However, the female groups’ significance dropped after gender separation. This significance drop may be due to the small female group size of 16 cases versus 34 in the male group and may rise in a larger study population.
In addition to this, a certain relationship between the fracture grade on several body regions and PFE could be observed. Therefore, the more high-grade (i.e. more comminute) fractures are distributed over more body regions, the higher the PFE grade will be. However, this correlation did not prove to be highly significant (p = 0.170).
Interestingly, our results did not show a correlation between the PFE grade and the fracture-affected body regions. This is indeed surprising, as one would have expected more less severe fractures to eventually amount to less, but more comminute fractures. A possible explanation may be, that comminute fractures arise due to higher impact energies than non-comminute fractures, and that impact energy may be a key aspect to PFE development.
Survival time and PFE
Falzi et al. [17] postulated a correlation between survival time and PFE positivity. According to these group results, cases with a survival time of only a few minutes were PFE positive in only 37% of the cases. Our results do not back this observation. In our cases with very brief survival times, we noted a positive PFE in almost 74%. The reason for this discrepancy is unclear. One possibility is that we also included cases, in which, unknown to us, a layperson resuscitation was performed which influenced PFE positivity. However, Falzi’s group must have included resuscitated individuals, so that the most likely reason for the discrepancy is a more sensitive examination method.
Correlation of PFE and fat crushing
If one follows the biomechanical hypothesis, one would expect a more grievous crushing of fatty tissue, be it the crush grade or the amount of affected body regions, to have an influence on the development of PFE, i.e. the more severe the crushing, the more severe the PFE should be. Our study does not support this hypothesis; indeed, although a (statistically insignificant) tendency toward a higher PFE grade was seen when several body regions experienced fat crushing. The grade of fat crushing did not correlate with the PFE grade, nor did the crush severity. These results suggest that other factors, perhaps the localisation of the crush site on the body, may play a role in the fat crushing development of PFE.
Conclusions
-
Traumatic PFE may occur in the absence of fractures.
-
Survival time does not correlate with the PFE grade.
-
Neither the amount of body regions affected by fat crushing, nor the grade of fat crushing nor the severity of fat crushing showed significant correlation with the PFE grade.
-
The grade of a fracture, i.e. whether multiple/comminute or isolated—possibly as a result of the impact energy—correlated with the grade of the PFE. This may have clinical implications for the assessment of possible FES, as, if the risk of a FES is known, preventive steps can be taken in order to prevent this potentially lethal disorder.
References
Vance BM (1931) The significance of fat embolism. Arch Surg 23:425–465
Robb-Smith AHT (1941) Pulmonary fat embolism. Lancet 1:135–141
Denman FR, Gragg L (1948) Fat embolism: a diagnostic enigma. Arch Surg 57:325–332
Wyatt JP, Khoo P (1950) Fat embolism in trauma. J Clin Pathol 120:637–640
Hiss J, Kahana T, Kugel C (1996) Beaten to death: why do they die? J Trauma 40:27–30
Gossling HR, Pellegrini VD Jr (1982) Fat embolism syndrome: a review of the pathophysiology and physiological basis of treatment. Clin Orthop Relat Res 165:68–82
Baker PL, Pazell JA, Peltier LF (1971) Free fatty acids, catecholamines, and arterial hypoxia in patients with fat embolism. J Trauma 12:1026–1030
Shapiro MP, Hayes JA (1984) Fat embolism in sickle cell disease. Report of a case with brief review of the literature. Arch Intern Med 144:181–182
Fracasso T, Karger B, Pfeiffer H, Sauerland C, Schmeling A (2010) Immunohistochemical identification of prevalent right ventricular ischemia causing right heart failure in cases of pulmonary fat embolism. Int J Leg Med 124:537–542
Von Bergmann E (1873) Ein fall von tödlicher Fettembolie. Berl Klin Wochenschr 10:385
Gurd AR, Wilson RE (1974) The FES. J Bone Joint Surg Br 56:408–416
Scully RE (1956) Fat embolism in Korean battle casualties: its incidence, clinical aspects and pathologic aspects. Am J Pathol 32:379–397
Palmovic V, McCarroll JR (1965) Fat embolism in trauma. Arch Pathol 80:630–635
Tedeschi CG, Walter LG (1968) Shock and fat embolism: an appraisal. Surg Clin North Am 48:431–452
Nichols GR II, Corey TS, Davis GJ (1990) Nonfracture-associated fatal fat embolism in a case of a child abuse. J Forensic Sci 35:493–499
Mudd KL, Hunt A, Matherly RC, Goldsmith LJ, Campbell FR, Nichols GR 2nd, Rink RD (2000) Analysis of pulmonary fat embolism in blunt force fatalities. J Trauma 48:711–715
Falzi G, Henn R, Spann W (1964) Über pulmonale Fettembolie nach Traumen mit verschieden langer Überlebenszeit. Münch Med Wochenschr 106:978–981
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bolliger, S.A., Muehlematter, K., Thali, M.J. et al. Correlation of fat embolism severity and subcutaneous fatty tissue crushing and bone fractures. Int J Legal Med 125, 453–458 (2011). https://doi.org/10.1007/s00414-011-0563-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00414-011-0563-8