Abstract
Purpose
To investigate the correlation between serum 25-hydroxyvitamin D (25-OH-VD) concentrations and metabolic parameters in obese and non-obese women with polycystic ovary syndrome (PCOS).
Methods
One hundred women with PCOS were divided into two groups, obese and non-obese, according to their body mass index (BMI). Waist-to-hip ratio (WHR), Ferriman–Gallwey score, homeostasis model assessment of insulin resistance (HOMA-IR), total cholesterol, triglycerides, calcium, 25-OH-VD, LH/FSH, total testosterone, and DHEAS were measured.
Results
The serum 25-OH-VD mean levels were 56.31% lower in the obese PCOS patients. There was an association of increased HOMA-IR, BMI, WHR, triglycerides, total testosterone, and DHEAS with decreased 25-OH-VD concentrations in the obese PCOS patients.
Conclusion
Low serum 25-OH-VD concentrations result from the presence of obesity and insulin resistance. However, the dependency between PCOS and hypovitaminosis D is questionable. Hypovitaminosis D should be kept in mind while managing obese women with PCOS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Polycystic ovarian syndrome (PCOS) is the most common hormonal disorder in women of reproductive age, characterized by hyperandrogenism and chronic anovulation; it is estimated to affect 5–10% of women [1]. A positive diagnosis is based on the patient presenting with any two of the following three features: oligo-ovulation/anovulation, clinical and/or biochemical signs of hyperandrogenism, and polycystic ovaries on ultrasound examination [2].
Insulin resistance stimulates the accumulation of more weight and induces hyperandrogenism and other symptoms of PCOS. The strong association between insulin resistance and ovarian hyperandrogenism suggests that insulin directly influences ovarian function [3]. Insulin resistance is a cardinal finding in the pathophysiology of PCOS [1] and increases with increasing body mass index (BMI) and waist circumference as a clinical sign of central obesity [4]. Obesity and, specifically, central obesity, is a common feature of PCOS that worsens the phenotype [5]. Insulin resistance is most commonly found in obese PCOS patients (65%), but can also occur in about 20% of lean PCOS patients [6].
Vitamin D deficiency has been shown to be associated with impaired glucose clearance and insulin secretion in both human [7] and animal [8] models. 25-Hydroxyvitamin D (25-OH-VD) is positively correlated with the insulin sensitivity and negatively with β-cell function [9]. The aim of this study was to investigate the correlation between low serum 25-OH-VD concentrations and metabolic parameters and IR in obese and non-obese women with PCOS.
Materials and methods
This prospective study analyzed 100 consecutive women with PCOS. The women enrolled had PCOS diagnosed according to the Rotterdam criteria [2], having two of the following three features: (1) oligo-ovulation or anovulation; (2) clinical and/or biochemical signs of hyperandrogenism; and (3) polycystic ovaries on ultrasound examination (defined as the presence of ≥ 12 follicles measuring 2–9 mm in diameter and/or ovarian volume > 10 cm3).
There was no age limit for inclusion. The exclusion criteria were Cushing’s syndrome, congenital adrenal hyperplasia, hyperprolactinemia, thyroid dysfunction, and virilizing tumors. The women who reported use of medication known to affect carbohydrate metabolism, plasma calcium concentrations, or endocrine parameters during the 3 months prior to the study were also excluded.
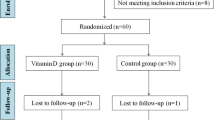
The patients were divided into two groups based on BMI: an obese group (BMI ≥ 25 kg/m2) and a non-obese group (BMI < 25 kg/m2). The numbers of obese and non-obese women with PCOS were 57 and 43, respectively. They were recruited from the outpatient clinics of the Department of Gynecology and Obstetrics, Yuzuncu Yil University School of Medicine (Van, Turkey) over an 8-month period between September 2007 and May 2008. The study was approved by the Yuzuncu Yil University Ethics Committee for Clinical and Laboratory Research. Written, informed consent to participate in the study was obtained from each patient.
Both BMI and waist-to-hip ratio (WHR) were measured for each patient. BMI was calculated as weight/height (kg/m2). The WHR was calculated by dividing the minimal waist circumference by the hip circumference at the level of the greater trochanters. The degree of hirsutism was determined using the Ferriman–Gallwey score [10].
A morning blood sample was taken after an overnight fast of ≥ 12 h during the follicular phase (between days 3 and 5) of each patient’s spontaneous or progestin-induced menstrual cycle. The homeostasis model assessment of insulin resistance (HOMA-IR) was used to evaluate insulin resistance, using the following formula: [11] HOMA-IR = (IRI × FPG)/22.5, where IRI is fasting plasma immunoreactive insulin (μU/L) and FPG is fasting plasma glucose (mmol/L).
Serum 25-OH-VD levels were measured using the high-performance liquid chromatography (HPLC)-based Chromsystems diagnostic kit. Levels of calcium were determined using spectrophotometry. Levels of luteinizing hormone (LH), follicle-stimulating hormone (FSH), total testosterone, dehydroepiandrosterone sulfate (DHEAS), and insulin were determined by chemiluminescent immunoassay using an Immulite® 2000 analyzer (Diagnostic Products Corp., Los Angeles, CA, USA). Glucose, total cholesterol and triglycerides were measured by enzymatic colorimetric assay using a Roche–Hitachi PP Modular Analyzer (Roche–Hitachi, Tokyo, Japan) and its original reagents.
All data were analyzed using the Statistical Package for the Social Sciences for Windows 16.0 software (SPSS, Chicago, IL, USA). Data are presented as mean ± SD or as percentages. First, multivariate analysis of variance (MANOVA) was done for all variables. After obtaining a significant difference between two groups with MANOVA (P < 0.01), comparisons between obese PCOS and non-obese PCOS patients were analyzed by one-way analysis of variance (ANOVA). The variables that caused significant difference were determined by ANOVA. Correlations between variables were evaluated using Pearson’s correlation coefficient. Statistical significance was defined as P < 0.01.
Results
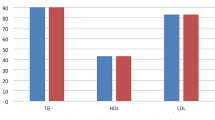
All PCOS patients in this study presented with menstrual disturbances (oligo/amenorrhea). Forty-three (43%) out of the 100 PCOS patients were non-obese, with a BMI < 25.00 kg/m2, and 57 (57%) were obese with a BMI ≥ 25.00 kg/m2. Metabolic characteristics of the non-obese and obese women with PCOS are shown in Table 1. The obese and non-obese women with PCOS who were studied had similar Ferriman–Gallwey scores, LH/FSH ratios, and calcium concentrations (P > 0.01). BMI, WHR, HOMA-IR, total cholesterol, triglycerides, total testosterone, and DHEAS were significantly higher in the obese women with PCOS compared with the non-obese women with PCOS (P < 0.01), whereas 25-OH-VD levels were significantly lower in the obese women with PCOS compared with the non-obese women with PCOS (P < 0.01) (Table 1).
The 25-OH-VD levels correlated negatively with BMI, WHR, HOMA-IR, total cholesterol, total testosterone, and DHEAS in the obese women with PCOS. No correlation was found between 25-OH-VD levels and age, LH/FSH ratio, or calcium levels in the obese women with PCOS. In contrast, there was a negative correlation between 25-OH-VD levels and LH/FSH ratio in the non-obese women with PCOS (Table 2). The serum 25-OH-VD mean levels were 56.31% lower in the obese PCOS patients.
Discussion
The primary defect in PCOS appears to be exaggerated androgen synthesis and secretion by the ovaries and adrenal glands [12]. PCOS is a unique, natural model for the study of the influence of androgen excess on bone mass among women [13]. In patients with PCOS, the deleterious effect on bone of amenorrhea is balanced by androgen overproduction [14]. Insulin resistance and systemic hyperinsulinism play a major role in the development of the hyperandrogenism characteristic of the syndrome. Insulin acts synergistically with LH to stimulate the synthesis of androgens by ovarian theca cells in vitro [6]. Insulin resistance, defined as reduced utilization of insulin-mediated glucose, has been found in 10–25% of the obese population in sophisticated, dynamic studies of insulin action [15]. There was also a tendency towards decreased insulin sensitivity in lean PCOS subjects, but only in obese women did these changes become statistically significant, suggesting that obesity, and particularly abdominal obesity, is an important contributor to the development of insulin resistance in PCOS [16, 17]. In our study, more than half of the PCOS patients were obese comparable to other study groups [18–20].
Dunaif et al. [21] suggested that women with PCOS have significant insulin resistance that is independent of obesity, changes in body composition, and impairment of glucose tolerance. On the other hand, the 1991–1992 Annual Report of the Committee for Reproductive and Endocrine (Japan Society of Obstetrics and Gynecology) [22] demonstrated a significant difference in insulin resistance between non-obese and obese women with PCOS; it suggested that obesity was the factor that affected insulin resistance most strongly and that insulin resistance in Japanese PCOS sufferers was a consequence of obesity rather than a feature of PCOS itself.
Hyperinsulinemia and abdominal obesity may have complementary effects in the pathogenesis of PCOS. Low calcium intake has been identified as a potential contributing factor to obesity [23]. In contrast, in the present study, we did not find a significant difference in calcium levels between obese women with PCOS and non-obese women with PCOS.
In obese perimenopausal women, serum 25-OH-D3 levels were significantly lower in comparison with healthy controls. The low level of 25-OH-D3 in obese subjects may be caused by the decreased exposure to sunlight (limited mobility of obese patients), excessive storage of vitamin D in adipose tissue and inhibition of its synthesis in liver by the increased level of 1,25-dihydroxyvitamin D [24]. Vitamin D insufficiency associated with obesity is likely to be functionally significant, as compensatory hyperparathyroidism has been observed in obese adults with low 25-OH-VD levels [25].
Hahn et al. [19] demonstrated that in PCOS patients increased body weight had a significant negative correlation on 25-hydroxyvitamin D concentrations, as in our study. The low concentration of 25-OH-VD could be a factor triggering insulin resistance and diabetes [26]. Zella et al. [27] have shown that oral administration of 1,25-dihydroxyvitamin D3 protected non-obese diabetic mice from developing insulin-dependent diabetes mellitus.
Women with PCOS are known to be at increased risk for the development of impaired glucose tolerance and type 2 diabetes mellitus (T2DM) [18]. A high prevalence of vitamin D deficiency has been shown in women with T2DM [28]. Insulin sensitivity has been shown to be increased by vitamin D supplementation [29].
In our study, low serum concentrations of 25-OH-VD were also shown to be associated with higher BMI values and total cholesterol. We also confirmed the association between abdominal obesity, hyperandrogenism, and insulin resistance by the correlation between HOMA-IR, WHR, FGS and total testosterone, and DHEAS concentrations in obese PCOS patients. Vitamin D levels below 20 ng/mL are considered to indicate hypovitaminosis D [9]. In our study, 67% of PCOS patients presented with vitamin D levels below 20 ng/mL. Vitamin D could be an alternative treatment to support insulin sensitivity. Vitamin D deficiency decreases the biosynthesis and release of insulin [8].
Vitamin D supplementation could be an element in the complex treatment of PCOS patients presenting with obesity and hypovitaminosis D, not only to ameliorate insulin resistance but also to prevent other serious health consequences. Randomized, controlled, prospective trials are needed to address this possible positive effect of vitamin D supplementation in obese patients with and without PCOS, especially whether vitamin D could prevent type 2 [19] and type 1 diabetes mellitus [30]. There was an inverse association between vitamin D levels and diabetes [26]. In a non-randomized controlled trial, Thys-Jacobs et al. [31] anticipated that the combination of dietary calcium insufficiency and vitamin D deficiency may well be largely responsible for the menstrual abnormalities associated with PCOS.
Abdominal obesity is a contributor to the development of insulin resistance in PCOS. Obesity and insulin resistance aggravate hyperandrogenism. Serum vitamin D is significantly lower in obese than in non-obese individuals and may contribute to lower serum 25-hydroxyvitamin D in obesity [32]. Hypovitaminosis D results from the presence of obesity but is independent of the presence of PCOS. The results of our study were in agreement with the previous studies supporting an association of increased HOMA-IR and BMI with decreased 25-OH-VD concentrations in women with PCOS. Although managing obese women with PCOS, low concentrations of 25-OH-VD should be kept in mind. Vitamin D supplementation can be useful in the treatment of obese women with PCOS.
References
Franks S (1995) Polycystic ovary syndrome. N Engl J Med 333:853–861. doi:10.1056/NEJM199509283331307
Rotterdam ESHRE/ASRM-sponsored PCOS Consensus Workshop Group (2003) Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS). Hum Reprod 19:41–47. doi:10.1093/humrep/deh098
Utsunomiya T, Taniguchi I, Sadanaga A et al (1993) Insulin resistance in non-obese patients with polycystic ovary syndrome. Jpn J Fertil Steri 38:77–81
Aronne LJ, Segal KR (2002) Adiposity and fat distribution outcome measures: assessment and clinical implications. Obes Res 10(Suppl 1):14S–21S. doi:10.1038/oby.2002.184
Gambineri A, Pelusi C, Vicennati V et al (2002) Obesity and the polycystic ovary syndrome. Int J Obes 26:883–896. doi:10.1038/sj.ijo.0801994
Dale PO, Tanbo T, Vaaler S et al (1992) Body weight, hyperinsulinemia, and gonadotropin levels in the polycystic ovarian syndrome: evidence of two distinct populations. Fertil Steril 58:487–491
Ortlepp JR, Metrikat J, Albrecht M, von Korff A, Hanrath P, Hoffmann R (2003) The vitamin D receptor gene variant and physical activity predicts fasting glucose levels in healthy young men. Diabet Med 20:451–454. doi:10.1046/j.1464-5491.2003.00971.x
Bourlon PM, Billaudel B, Faure–Dussert A (1999) Influence of vitamin D3 deficiency and 1, 25 dihydroxyvitamin D3 on de novo insulin biosynthesis in the islets of the rat endocrine pancreas. J Endocrinol 160:87–95. doi:10.1677/joe.0.1600087
Chiu KC, Chu A, Go VL, Saad MF (2004) Hypovitaminosis D is associated with insulin resistance and beta cell dysfunction. Am J Clin Nutr 79:820–825
Ferriman D, Gallwey JD (1961) Clinical assessment of body hair growth in women. J Clin Endocrinol Metab 21:1440–1447
Matthews DR, Hosker JP, Rudenski AS et al (1985) Homeostasis model assessment: insulin resistance and β-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28:412–419. doi:10.1007/BF00280883
Wickenheisser JK, Nelson–DeGrave VL, McAllister JM (2006) Human ovarian theca cells in culture. Trends Endocrinol Metab 17:65–71. doi:10.1016/j.tem.2006.01.003
Zborowski JV, Talbott EO, Cauley JA (2001) Polycystic ovary syndrome, androgen excess, and the impact on bone. Obstet Gynecol Clin North Am 28:135–151, vii–viii. doi:10.1016/S0889-8545(05)70190-X
Adami S, Zamberlan N, Castello R, Tosi F, Gatti D, Moghetti P (1998) Effect of hyperandrogenism and menstrual cycle abnormalities on bone mass and bone turnover in young women. Clin Endocrinol (Oxf) 48:169–173. doi:10.1046/j.1365-2265.1998.3691182.x
Ferrannini E, Natali A, Bell P et al (1997) Insulin resistance and hypersecretion in obesity group for the study of insulin resistance (EGIR). J Clin Invest 100:1166–1173. doi:10.1172/JCI119628
Morin-Papunen LC, Vauhkonen I, Koivunen RM, Ruokonen A, Tapanainen JS (2000) Insulin sensitivity, insulin secretion, and metabolic and hormonal parameters in healthy women and women with polycystic ovarian syndrome. Hum Reprod 15:1266–1274. doi:10.1093/humrep/15.6.1266
Pasquali R, Casimirri F (1993) The impact of obesity on hyperandrogenism and polycystic ovary syndrome in premenopausal women. Clin Endocrinol (Oxf) 39:1–16. doi:10.1111/j.1365-2265.1993.tb01744.x
Ehrmann DA, Barnes RB, Rosenfield RL, Cavaghan MK, Imperial J (1999) Prevalence of impaired glucose tolerance and diabetes in women with polycystic ovary syndrome. Diabetes Care 22:141–146. doi:10.2337/diacare.22.1.141
Hahn S, Haselhorst U, Tan S, Quadbeck B, Schmidt M, Roesler S, Kimmig R, Mann K, Janssen OE (2006) Low serum 25-hydroxyvitamin D concentrations are associated with insulin resistance and obesity in women with polycystic ovary syndrome. Exp Clin Endocrinol Diabetes 114:577–583. doi:10.1055/s-2006-948308
Goodarzi MO, Erickson S, Port SC, Jennrich RI, Korenman SG (2003) Relative impact of insulin resistance and obesity on cardiovascular risk factors in polycystic ovary syndrome. Metabolism 52:713–719. doi:10.1016/S0026-0495(03)00031-3
Dunaif A, Segal KR, Futterweit W et al (1989) Profound peripheral insulin resistance, independent of obesity, in polycystic ovary syndrome. Diabetes 38:1165–1174. doi:10.2337/diabetes.38.9.1165
The Committee for Reproductive and Endocrine in Japan Society of Obstetrics and Gynecology (1993) Annual report (1991–1992) for the determination of diagnostic criteria for polycystic ovary syndrome. Acta Obstet Gynaecol Jpn 45:1359–1367 (in Japanese)
Zemel MB (2002) Regulation of adiposity and obesity risk by dietary calcium: mechanisms and implications. J Am Coll Nutr 21:146S–151S
Holecki M, Zahorska-Markiewicz B, Janowska J, Mizia-Stec K, Zak-Golab A, Olszanecka-Glinianowicz M, Wojaczynska-Stanek K, Nieszporek T, Wiecek A (2007) Osteoprotegerin—does it play a protective role in the pathogenesis of bone loss in obese perimenopausal women? Endokrynol Pol 58:7–10
Yanoff LB, Parikh SJ, Spitalnik A et al (2006) The prevalence of hypovitaminosis D and secondary hyperparathyroidism in obese black Americans. Clin Endocrinol (Oxf) 64:523–529. doi:10.1111/j.1365-2265.2006.02502.x
Scragg R, Sowers M, Bell C (2004) Serum 25-hydroxyvitamin D, diabetes, and ethnicity in the Third National Health and Nutrition Examination Survey. Diabetes Care 27:2813–2818. doi:10.2337/diacare.27.12.2813
Zella JB, McCary LC, DeLuca HF (2003) Oral administration of 1, 25-dihydroxyvitamin D3 completely protects NOD mice from insulin dependent diabetes mellitus. Arch Biochem Biophys 417:77–80. doi:10.1016/S0003-9861(03)00338-2
Isaia G, Giorgino R, Adami S (2001) High prevalence of hypovitaminosis D in female type 2 diabetic population. Diabetes Care 24:1496. doi:10.2337/diacare.24.8.1496
Kotsa K, Yavropoulou MP, Anastasiou O, Yovos JG (2008) Role of vitamin D treatment in glucose metabolism in polycystic ovary syndrome. Fertil Steril Oct 16 (Epub ahead of print) PMID: 18930208.
Baynes KC, Boucher BJ, Feskens EJ, Kromhout D (1997) Vitamin D, glucose tolerance and insulinaemia in elderly men. Diabetologia 40:344–347. Published erratum appears in Diabetologia 1997 40(7):870. doi:10.1007/s001250050685
Thys-Jacobs S, Donovan D, Papadopoulos A, Sarrel P, Bilezikian JP (1999) Vitamin D and calcium dysregulation in the polycystic ovarian syndrome. Steroids 64:430–435. doi:10.1016/S0039-128X(99)00012-4
Liel Y, Ulmer E, Shary J, Hollis BW, Bell NH (1988) Low circulating vitamin D in obesity. Calcif Tissue Int 43:199–201. doi:10.1007/BF02555135
Conflict of interest statement
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yildizhan, R., Kurdoglu, M., Adali, E. et al. Serum 25-hydroxyvitamin D concentrations in obese and non-obese women with polycystic ovary syndrome. Arch Gynecol Obstet 280, 559–563 (2009). https://doi.org/10.1007/s00404-009-0958-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-009-0958-7