Abstract
The use of dermal substitutes is increasingly widespread but the outcomes of substitute-assisted healing remain functionally deficient. Presently, the most successful scaffolds are acellular polymer matrices, prepared through lyophilization and phase separation techniques, designed to mimic the dermal extracellular matrix. The application of scaffolds containing viable cells has proven to be problematic due to short shelf-life, high cost and death of transplanted cells as a result of immune rejection and apoptosis. Recent advances in biomaterial science have made new techniques available capable of increasing scaffold complexity, allowing the creation of 3D microenvironments that actively control cell behaviour. Importantly, it may be possible through these sophisticated novel techniques, including bio-printing and electrospinning, to accurately direct stem cell behaviour. This complex proposal involves the incorporation of cell-matrix, cell-cell, mechanical cues and soluble factors delivered in a spatially and temporally pertinent manner. This requires accurate modelling of three-dimensional stem cell interactions within niche environments to identify key signalling molecules and mechanisms. The application of stem cells within substitutes containing such environments may result in greatly improved transplanted cell viability. Ultimately this may increase cellular organization and complexity of skin substitutes. This review discusses progress made in improving the efficacy of cellular dermal substitutes for the treatment of cutaneous defects and the potential of evolving new technology to improve current results.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tissue engineering and regenerative medicine are necessitated by the limited reparative capacity of post-natal tissues and organs. In the treatment of cutaneous defects, the use of tissue-engineered dermal substitutes, in their various forms, is increasingly routine, particularly as a life saving tool following acute thermal trauma. However, at present, even the most successful amongst these, cannot restore the full functionality and appearance of uninjured dermis.
Dermal substitute construction is variable and a range of materials, designs and cell sources have been investigated. Most commercially available products are based around polymer matrices, derived from both natural and synthetic sources. The majority of these, however, were developed during the 1990s and are designed to mimic the basic properties of the extracellular matrix (ECM).
Physiologically, on the simplest level, the ECM supplies the structural and organizational framework of developing and mature dermal tissue. This framework is created in the main through highly hydrated insoluble macromolecules such as fibrillar proteins (e.g. collagens), glycoproteins (e.g. elastin or fibronectin) and proteoglycans with associated glycosaminoglycans (e.g. versican). The tunability of this system is such that cells are able to create cell-specific micro-environments through bidirectional interaction with, and remodelling of, the ECM surrounding them.
Following damage to or destruction of dermal tissue, granulation tissue is formed. This loosely woven immature neomatrix is deposited by invading monocytes (mainly macrophages) and fibroblasts following platelet-mediated establishment of haemostasis. The early granulation tissue contains large quantities of fibrin, fibronectin, hyaluronan and also collagen types I and III [165]. Several growth factors have been identified as important for cell invasion of the site, proliferation and matrix deposition/remodelling including transforming growth factor (TGF)-β [164], platelet derived growth factor (PDGF) [85, 109, 142], fibroblast growth factors (FGFs) [85, 160] and matrikines released by matrix damage and remodelling. This early tissue provides the framework for the deposition of neodermis. Within a few weeks the fibronectin-rich matrix disappears. Hyaluronan is reduced and collagen type I/III fibres are slowly remodelled to contain less collagen III and reorganized into large bundles. The anisotropic architecture of the mature fibrillar matrix consists of both rigid supporting collagens, flexible elastic networks of elastin, and molecular connectors. This arrangement not only confers important mechanical properties but influences cell behaviour by the manner in which cells bind to, and therefore sense their microenvironment [134].
Cells adhere to the different ECM components either directly through cell surface receptors (e.g. integrins) or via intermediate factors with varying degrees of specificity and affinity. The density and number of specific cell surface receptors that bind the ligand initiates corresponding intracellular signalling events. These specific interactions, in part, control cell survival, cell phenotypes and drive cell fate decision [44, 66, 94]. Of additional importance is the spatial orientation of activated cell surface receptors. In some cases three-dimensional integrin activation is required to initiate a cellular response. An example of this is the regulation of MMP-13 production through 3D activation of α1β1 and α2β1 integrins in collagen substrates, which results in the coordinated stimulation of three MAPK classes (ERK1/2, JNK and p38). In this example, it is the balance between the p38 (activating) and ERK1/2 (suppressing) pathways through integrin-mediated ECM-cell signalling that affects the rate of enzymatic degradation of the matrix [134].
The extent and complexity of the inherent bioactivity of native dermal ECM has only recently been fully realized and is not yet understood fully. The ECM environment, which a transplanted cell is subjected to, influences cell survival and behaviour. The current gap in knowledge into what specific environmental cues are required for maximizing therapeutic efficacy of transplanted cells could explain the failure of early cellular dermal substitutes to behave as designed once in the wound bed [78, 79, 98]. It is probable that a more detailed knowledge of the complex interactions involved will allow improved substitute design. Recent advances in material synthesis and processing have facilitated a developmental move towards more sophisticated bio-inspired materials and away from educated trial and error bio-mimicry [43, 79, 176].
This review will discuss the current status of dermal substitutes and the biomaterial design that they are based on. The use of stem cells in regenerative medicine is reviewed in this context along with the characteristics and potential of various stem cell sources for application in this field. The article then moves on to focus on novel emerging techniques and materials that are likely to become important in future dermal substitutes, in particular, those containing stem cells.
Biomaterials
Perhaps unsurprisingly, given its natural prevalence, collagen is the most widely utilized scaffold biopolymer available for use in skin substitutes. It is obtained from allogeneic or xenogeneic sources, with sufficient molecular homology existing to prevent a significantly detrimental immune response in most cases [16]. The collagen in these scaffolds is often reconstituted into porous, fibrous and hydrogel structures with physical properties that can be controlled through manufacture conditions, such as chemical cross-linking to prevent degradation. However, such treatments may compromise effectiveness, for example extensive cross-linking increases matrix rigidity and reduces cell attachment and viability [24, 143]. In its natural state, collagen has a superior degradation rate (up to 6 weeks) in comparison to reconstituted collagen (1 week) [19, 62, 72].
Numerous other natural materials have been used in scaffolds for engineered dermis including hyaluronic acid [25], fibrin [2], laminin [51] and elastin [60]. These materials are usually processed into porous scaffolds through lyophilization (freeze-drying) or phase separation processes. (Fig. 1) Naturally occurring ECM molecules are considered advantageous due to their cell interaction, adhesion and signalling properties. These interactions could include direct matrix-cell interactions, through the uptake of soluble factors or through the interaction of enzymatically degraded fragments, or matrikines, with cell surface receptors [17, 20, 154]. However, with the exception of elastin, the mechanical properties of these materials are often poor in comparison to the properties of synthetic materials, which can be tailored across a broad spectrum. Even elastin, with a half life of around 70 years [27], must be organized into its naturally occurring network to function properly and retain its stability [27]. When using natural materials disease transmission and immunogenicity remain a concern. In addition to these concerns, further complications include the availability of materials; especially allogeneic material, purification of selected materials, and batch-to-batch and source variability. These also serve to increase the cost of utilizing some raw materials, meaning substitutes developed from these materials are potentially more expensive. A possible way of side stepping these problems could be through the use of recombinant technology in their production. Due to these issues, there is a desire to develop synthetic materials that can be designed to best mimic the natural ECM.
Current strategies for the production of dermal substitutes. Current scaffolds tend to be in several main forms: a Hydrogels, b porous sponge (lyophilization/particulate leaching/phase separation), c non-woven fibre, d woven fibre, e honey comb mesh. These can be inserted as acellular scaffolds or can be seeded with autologous/allogeneic cells harvested from bioposy or cell line. Alternatively cell suspensions can be directly applied to skin defects as a liquid or spray
Synthetic materials offer the possibility of improving material control, reducing batch variation, eliminating disease transmission and providing more cost-effective scalability. Synthetic materials investigated as scaffold materials include polyurethane (PU), polypropylene (PP) [138], poly(ethylene glycol), polyglycolide (PGA), polylactide (PLA) and polylactide-coglycolide (PLGA) [29, 101, 108], polytetra fluoroethylene (PTFE), polycaprolactone (PCL)[119], polyethylene terephthalate (PET), Poly(l-lactide) (PLLA)[169] and poly(ethyleneglycolterephthalate)-poly(butylenes terephthalate) (PEGT/PBT) [21, 39], [157] Despite their ease of manipulation and manufacture, the safety of these materials remains a concern [57]. Although they may not be directly toxic, the use of synthetic materials has in some cases been found to lead to a foreign body response and fibrous capsule formation surrounding the material [138, 155]. Even though, cell interaction with these materials can be limited; they can often be easily and effectively modified through the attachment of growth factors, attachment sites or coating with ECM molecules to improve cellular performance. Zisch et al. [176] covalently decorated PEG hydrogels with vascular endothelial growth factor (VEGF) which led to improved vascularization following grafting to chick chorioallontoic membrane and subcutaneous implantation in rats. A more simplistic approach was applied by Chen et al. [29] who investigated a hybridized PLGA/collagen mesh as a 3D culture system for tissue engineering skin and found that hybridization resulted in improved cell attachment and ECM deposition of dermal fibroblasts.
Aside from manufactured matrices, several products exist that consist of intact de-cellularized dermal matrices of allogenic or xenogeneic origin (e.g. Alloderm™, Oasis™, FortaFlex™, Repliform™). The hypothesis being that these matrices offer an ideal scaffold environment for the migration and proliferation of dermal cells through the retention of structure, attachment sites and matrix-bound growth factors. Reports demonstrate that 3D adhesions are formed rapidly in cells seeded to tissue-, or cell-derived acellular matrices [33]. This suggests that these matrices if processed competently may retain and present important information that promotes attachment, proliferation and migration to a further extent than other three-dimensional and two-dimensional materials [33]. However, problems can arise when using harsh de-cellularization protocols that may remove or denature growth factors and damage matrix architecture [30, 69]. Conversely, mild protocols may fail to remove cellular material efficiently, resulting in a subsequent immune reaction in response to retained foreign cell fragments [34, 52, 166]. Of the commercially available products mentioned above; Alloderm™ and Oasis™ have had relative success in their clinical application in the treatment of chronic ulcers and as dressings for split thickness graft donor sites. Accelerated healing and decreased pain were reported in some cases in comparison to conventional treatments [88, 111, 121, 136, 158, 159]. It is worth noting that intact de-cellularized ECM represents a mature end-point structure, both in terms of architecture and molecular composition. It is possible that this environment is not ideal for inducing a regenerative wound healing response from host cells. Finally, although a scaffold material can be designed as “permanent”, generally it is considered desirable that the transplanted scaffold can be safely assimilated into the body as new matrix is generated by the populating cells.
Stem cells
Currently, the transplantation of cells in regenerative medicine is limited by the poor survival rates and persistence of the transplanted material [83, 129]. The cellular constituents of current dermal substitutes only remain present for approximately 1 month after application with only a few percent of cells surviving initial engraftment [31, 147]. If cellular dermal substitutes are to succeed, further improvements need to be made. This could be achieved through the delivery of stem and progenitor cell populations within protective and bioinstructive environments [3].
Stem cells are defined by their ability to self-replicate and produce more specialized progeny [87, 141]. Their incorporation into dermal substitutes could lead to improved therapeutic activity by directly contributing to cellular content of the healing wound, the release of paracrine factors and activation of host stem and somatic cell populations [3]. Furthermore due to their plasticity, it may be possible to increase the non-fibroblastic cell content of substitutes without the need to incorporate several different cell populations. Previous work has sought to identify suitable stem or progenitor populations for tissue engineering applications. Several candidate populations have been identified drawing from embryonic stem cell (ESC), adult stem cell (ASC) sources and more recently through induced pluripotent stem cells (iPS cells) (Table 1). Each source has advantageous characteristics, though none are without disadvantages.
Embryonic stem cells are pluripotent stem cells derived from the inner cell mass of the blastocyst, which forms several days after fertilization [152]. Due to their pluripotency, and unique ability to maintain pluripotency in long-term culture, these cells make an attractive single source to generate cells of multiple, diverse lineages [18]. However, the use of ESCs has attracted widespread public controversy leading to complex and stringent regulations governing their use. Additional safety concerns exist with the use of these cells due to reports of teratoma formation [172]. However, since the generation of the first human ESC line in 1998, at least 225 subsequent human ESC lines have been generated [64, 152].
The physiological function of ASCs is the maintenance and repair of the tissues in which they reside. ASC populations reside within niches in tissue incorporating cell-cell, cell-matrix, soluble cues, mechanical properties and soluble factor gradients to maintain steady numbers of stem cells in a stable undifferentiated state within them [161] (Fig. 2). It was previously thought that ASCs were lineage restricted to their host-tissue. However, recent work has shown that some populations of these cells are multipotent and possibly even pluripotent [74], and, therefore, capable of differentiation into a wider range of cells than anticipated [84, 130]. Certain populations of these stem cells have characteristics such as abundance and ease of extraction, facilitating their use in regenerative medicine and tissue engineering [63]. Of these, bone marrow-derived mesenchymal stem cells (BM-MSCs) and adipose-derived stem cells (Ad-MSCs) are perhaps the most promising candidates for stem cell therapy. BM-MSCs are the most characterized ASC population [23, 54]. They are present in bone marrow in low density (~1 MSC per 5 × 103 mononuclear cells) [77]. Although no single BM-MSC specific marker has been identified positive expression of CD73, CD90 and CD105, when not expressing CD34, CD14 and CD45 has been used to identify MSCs from mixed populations [7, 153]. Bone marrow-derived stem cells have been used clinically in the treatment of cutaneous defects, showing improved healing outcomes in comparison to conventional treatments [13, 42].
Schematic representation of adult stem cell niche and factors involved in controlling stem cell behaviour within it. The undifferentiated stem cell (blue) is situated within the niche surrounded by supporting cells (red), specific extracellular matrix molecules and in proximity to microvasculature. The fate of the stem cell is controlled within the niche through direct interactions with the ECM and supporting somatic cells. Further to this, the release of paracrine and autocrine factors alters the behaviour of the resident stem cells. The release of these factors can be influenced by cytokine/growth factor release and/or neuronal signalling (green cell) to tune stem cell behaviour to the tissue requirements, e.g. increased division and migration during wound healing
Adipose-derived stem cells offer an attractive alternative to BM-MSCs. Adipose tissue has the highest abundance of stem cells of any tissue in the body, which can be easily harvested through liposuction surgery and demonstrate multipotency in vitro [55, 179]. Flow cytometric analyses of Ad-MSCs have revealed that they share similar surface receptors with BM-MSCs. This importantly includes the activated lymphocyte adhesion molecule CD166, which has been shown to identify BM-MSC populations with multipotent differentiation potential, and integrin β1 which is also associated with the cells in the epidermal stem cell compartment [53, 75, 89]. Ad-MSCs have yet to be used in the clinic to treat cutaneous injury but have shown promise in animal wound healing models [5].
Hair follicle-derived stem cell (HFSC) populations offer a further option for application in stem cell therapy due to their natural position and roles within the skin, their ease of extraction and multipotency [4, 32, 70, 135]. Of the discussed ASC populations HFSC have been least investigated for tissue engineering skin. However, they may represent an important future resource in the development of dermal substitutes.
Another candidate population of cells for use in the development of cell instructive dermal substitutes would be the newly promising iPS cells. Since the discovery by Takahashi and Yamanaka [150] that pluripotency could be induced in somatic cells through the delivery of several growth factors, the field of iPS cells has rapidly expanded. Their research elegantly demonstrated the direct reprogramming of mouse embryonic fibroblasts through the enforced expression of four transcription factor genes (Oct3/4, Sox2, Klf4 and c-Myc) [112, 150]. Since this initial work, several groups have confirmed and improved this technique and generated human iPS cells that are epigenetically and developmentally indistinguishable from ES cells [92, 97, 123, 124, 162]. The c-Myc gene has since been shown to be dispensible for reprogramming which has resulted in reduced incidence of malignant transformation in iPS derivatives [112]. Recently, virus-free generation of iPS cells was achieved by Zhou et al. [174] and Kim et al. [80] using recombinant proteins. Zhou et al. [174] used polyarginine protein transduction domain tagged proteins repeatedly added to culture media containing valproic acid (VPA) to reprogramme murine fibroblasts. In a similar way, Kim et al. [80] used proteins tagged with a highly basic peptide sequence derived from human immunodeficiency virus-TAT protein to reprogramme human fibroblasts. These tagged proteins were released from HEK293 (human embryonic kidney) cells engineered to over express them [80]. The virus free reprogramming of cells, removes the major safety concern of retroviral gene transfer-induced mutagenesis. This technique potentially means that a tailor made population of pluripotent stem cells can be constructed rapidly from a small sample of the patient’s own somatic cells. Several safety concerns, such as tumor formation potential, remain to be addressed prior to clinical application of stem cells from this source. Although this field is progressing rapidly, akin to other breakthroughs, it is likely to be some time before the transition from laboratory to clinic is made possible [12, 28, 112].
The transplantation of stem cells, notwithstanding the source of the cells, has encountered several obstacles, in particular, controlling the fate of the engrafted cells once applied to the wounded dermis. Several schemes have been suggested such as those by Discher et al. in which materials could be engineered to contain stem cells within niche environments designed to maintain the ‘stemness’ of the cells. As progenitor cells move out from this niche environment, differentiation could be directed through engineered ECM design, as in natural tissue [9, 106, 156]. An alternative approach could be to attract circulating native stem cell populations once a scaffold is transplanted. This could be achieved through incorporation of some homing signal and/or specific binding sites to mobilize resident stem cell populations and encourage residence within the substitute [35]. Sasaki et al. [139] investigated whether systemically delivered MSCs are able to differentiate into multiple skin types and contribute to wound healing in murine models. They found that wound-site intradermal injection of the chemokine SLC/CCL21 increased MSC homing to the defect and resulted in accelerated wound repair. A related factor, stromal cell-derived factor-1 (SDF-1), is rapidly overexpressed following tissue injury [10] and is known to recruit endothelial progenitor cells to wound sites [14, 15, 46]. Recently, Rabbany et al. [132] investigated the effects of a SDF-1-releasing alginate scaffold on cutaneous wound healing in a porcine model [132]. The authors reported that wounds treated with SDF-1 fully closed without scar formation. Interestingly, they go on to link this finding to the sonic hedgehog (Shh)-Gli pathway, which is responsible for regulating foetal organ development and implicated in scarless wound healing [36]. Sonic hedgehog has been shown to upregulate SDF-1 and also enhance SDF-1’s recruitment of progenitor cells to wound sites [8, 86]. The authors suggest that Shh-mediated SDF-1 upregulation may be the mechanism by which decreased scarring is achieved in foetal wound healing and could be exploited to achieve similar results in adult tissues [132]. Materials designed to deliver these chemokines and other factors in conjunction with stem cell transplantation could result in increased efficacy of stem cell treatments.
Aside from the delivery of soluble factors, substrate stiffness is now recognized as an important factor affecting the lineage commitment of stem cells [41, 137]. Engler et al. [41] and Saha et al. [137] demonstrated that in 2D culture. MSCs cultured on soft substrates commit to neurogenic fates, on moderately soft substrates commit to myogenic fates and on rigid substrates commit to osteogenic fates. Recently, Pek et al. [125] demonstrated that substrate stiffness has a similar effect on MSCs cultured in 3D systems. By utilizing an inert thixotropic polyethylene glycol–silica nanocomposite gel, Pek et al. [125] were able to demonstrate the direct effect of matrix stiffness whilst controlling the biological cues presented to the cells within the system, in particular, the effect of integrin-ligand binding mediated cell responses [125].
Current strategies for stem cell-assisted cutaneous repair
It is hypothesized that stem cells can improve healing through three basic mechanisms; (1) creation of an environment that enhances the regenerative capacity of endogenous cells, (2) transdifferentiation, and (3) cell fusion [99, 131, 145, 146]. Numerous studies have demonstrated the potential of transplanted ASCs to improve wound healing rates in animal models and clinical trials [5, 42, 47, 48, 114, 133]. These early trials have shown that cell preparation and delivery methods alter the therapeutic efficacy of the transplanted stem cells leading to contrasting reports in the literature [5]. For example, a murine model treating dermal wounds in diabetic mice with human adipose-derived stem cells, found that when the cells were delivered as a suspension, no advantageous healing effect was observed [5]. However, when cells were delivered as three-dimensional aggregates, wound healing was significantly accelerated [5]. Other studies deliver Ad-MSCs [3, 117, 120] and BMSCs [59, 93, 99, 107, 114, 173] in dermal substitutes. One reason for the observed benefit of cells delivered in this way could be that the harsh, necrotic environment of the wound may lack the appropriate milieu to support the transplanted stem cells. It is clear that the environment in which the cells are delivered must confer some level of protection to maintain viability whilst allowing direct contact with, and migration into, the wound environment.
Designing 3D biomaterials to control stem cell-assisted dermal regeneration
The challenge, thus, lies in the identification, design and manufacture of dermal scaffolds which maximize the healing potential of transplanted stem cells. Effectively manipulating the enormously complex cell interactions and regulators of cell fate in three dimensions still represents a significant problem even in vitro. The majority of information that we have about cell signalling networks and interactions has been derived from 2D in vitro culture systems. It is a challenge, therefore, to micro-engineer a 3D environment when mechanisms of intra- and inter-cellular signalling networks in this setting are not well known [95]. This situation is exacerbated by the tissue-dependent variability of the niche itself down to the molecular level and the dissimilar responses of stem cells from different sources to similar materials and microenvironments [118]. The materials present may as a result have a differential effect depending on cell source. This, and the lack of understanding of how dimensionality affects signal transduction pathways could be addressed with the development of quantitative models [95, 96]. Using high throughput techniques to test biologically driven assumptions into cell behaviour through accurate creation of specific cell-matrix interactions is likely to be an efficient method for the development of materials with the complexity needed to accurately direct cellular processes [6, 45, 100, 115].
Several materials and fabrication techniques have been developed or recently applied to tissue engineering that have the potential to make the manufacture of such complex materials possible (Table 2; Fig. 3). The presentation and release of growth factors as a means of instructing cell behaviour is an area which has received considerable interest. Micro- and nano-spheres incorporated into matrices of various forms can be designed with release profiles to deliver factors in a concentration and time-specific manner [148, 163, 170]. This approach also protects the growth factors from degradation. Alternative approaches tether growth factors to scaffold polymers to be released and activated through cell-mediated enzymatic action. One example of this cell-demanded release, pioneered by Hubbell, involves VEGF covalently bound to poly (ethylene glycol) hydrogel matrices [38, 177, 178]. This couples growth factor concentration directly to cell remodelling and was shown to induce controlled, natural-like blood vessel growth and formation in chick chorioallontoic membrane and rats [38].
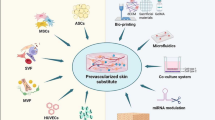
Flow chart representing some of the design considerations for next generation dermal substitutes. The design of dermal substitutes starts with the choice of substrate material which can be from a biological source or a synthetic material. The grey box represents selected instructive cues and promising methods of incorporation into substrates. This instructive scaffold may then be inserted as an acellular substitute or cells may be introduced (purple box). The incorporation of viable cells into the designed substrate is also an important design consideration with several populations to select from. The 3D spatial positioning of these cells within scaffolds should improve the speed and functionality of substitute assisted healing. The efficacy of transplanted cells is dependent on delivery method and scaffold material design
Matrix tethering and micro/nano-sphere incorporation could also be used to create spatial and temporal concentration gradients in three dimensions [144]. Gradients of bioinstructive molecules presented in these ways, effectively reduce the amount of the particular molecular factors needed to produce the desired cellular response [144]. Aside from chemical gradients, the incorporation of other gradients such as (but not exclusive to) pore size, substrate stiffness and cell attachment site distribution or type are also important. Spatial patterning of some or all of these physical and biological cues mimics the natural composition of dermis and other tissues. For example, the recreation of the dermal–epidermal bilayer could be facilitated by gradients of keratinocyte/fibroblast-specific attachment sites, growth factors, differentiation factors and scaffold properties. These factors could work synergistically to induce correct cell fate decisions from transplanted and endogenous stem and progenitor populations for rapid, successful wound healing.
One of the promising novel techniques to emerge in recent times is bioprinting. Bioprinting can be defined as the automated, computer-aided deposition of biological materials and cells in a predesigned pattern [102]. It is possible through this relatively new technique to construct 3D-engineered tissues via layer-by-layer deposition. The layered structure of the skin may mean that this technique is particularly applicable to the creation of dermal substitutes.
The term bioprinting encompasses a number of techniques including inkjet [116, 167], laser guidance direct write [122], laser-induced forward transfer (LIFT) [65], extrusion-based printing [168] and electrostatic-based jetting [58]. These techniques have several characteristics that can be harnessed for the creation of next generation dermal substitutes. The computer-aided nature of the technique means that precision deposition of cells, ECM and bioactive agents in defined amounts is possible with relative ease [116]. Importantly, through the different ink dispensers of printers, it is possible to use multiple ECM components simultaneously. Non-contact processes, where a jet is formed for microsecond time-scales, also mean that the deposition of bio-ink can be made on a variety of substrates and even liquid [37]. Ink-jet delivery systems have received particular attention but several limitations currently exist such as high shear stress on extrusion and high impact on deposition of the bio-ink droplet [104]. In bio-printing cells, maintaining viability and gene expression profiles represents a challenge, with some success reported [56, 113, 116]. The viscosities, surface tensions and densities of the bio-inks used in these systems are limited by the process requirements, restricting the concentrations of some ECM molecules that may be used [104]. This becomes important in the construction of 3D bio-printed substitutes where deposited material must be capable of retaining shape and offering structural support. At present 3D construction relies on either layer-by-layer deposition of bio-inks which can be gelified or through the use of a 2D ‘bio-paper’ material which is then stacked sequentially to give a 3D structure [105, 116]. It has been suggested that the latter method may be the only feasible solution to mechanical problems arising when using direct 3D gel-based approaches [56]. This approach could also improve general handling properties for clinical application of dermal bio-printed constructs. In addition, the form of bio-paper utilized for 3D construction may allow the combination of bio-printing with another emerging processing technique, electrospinning. Ultimately it may be possible to develop in situ bio-printing clinical tools. This technology could feasibly allow the direct regeneration of cutaneous injury [103].
Electrospinning supplies a simple, cost-effective method to construct porous scaffolds with uniform fibres in the nano-scale [22]. The process involves charging a polymer solution or melt to a high potential and injecting it through a blunt needle towards a grounded collector, typically 10–30 cm away. The electrical potential of the resulting fibre drives it across the air gap between the needle and collector, with the solvent evaporating during this transit. This results on the formation of dry polymer fibres on the collector [11]. The scale of the fibres can be produced in these scaffolds corresponds to the natural ECM, with reports demonstrating that they promote normal cell-cell and cell-matrix interactions [61, 91]. The majority of the natural and synthetic biomaterials used to construct nanofibrous scaffolds are those previously used to construct scaffolds by other methods. Electrospun scaffolds have been shown to promote fibroblast proliferation in vitro [175]. Working on full thickness wounds in mice, superior ‘take’ and levels of contraction were observed in collagen electrospun scaffolds in comparison to freeze-dried scaffolds [128].
The electrospinning technique lends itself to the creation of sequentially layered scaffolds [11]. Through altering the spin parameters, physical properties such as fibre diameter, porosity and fibre alignment (anisotropy) can be adjusted. As an example, fibre diameter, alignment and density could be adjusted to create a scaffold that structurally mimic the reticular and papillary dermis. Yang et al. [171] electrospun a collagen-PCL multi-layered scaffold containing viable human dermal fibroblasts and keratinocytes deposited directly through the electrospinning process. Although viability of the cells was maintained it has been suggested that care needs to be taken when spinning cells directly due to exposure to high electrical field and organic solvents often used in the process [11]. To create biologically instructive scaffolds growth factors may be directly added to the polymer solution prior to spinning with studies indicating that biological activity is maintained in vitro and in vivo [49].
Conclusion
Over recent years, biomaterials science has developed novel techniques which can be applied to tissue engineering and regenerative medicine. Amongst these newly emerging techniques, bio-printing and electrospinning have the potential to produce scaffolds which incorporate instructive factors and viable cells. A number of studies have demonstrated the principles of viable cell positioning and bioactive molecule patterning [73, 116] and managed to control stem cell fate [76, 127]. The translation from these improved scaffolds to instructive three-dimensional dermal substitutes is not a simple task. Mimicking the complexity of the natural matrix may not be a practical option when producing commercial dermal substitutes. Which factors and properties are essential to create a niche for stem cells conducive for the regeneration of dermal tissue requires further investigation. The precise positioning of molecules and cells may allow the construction of differentiated structures currently lacking from dermal substitutes like nerves, sweat glands and pilosebaceous units. The precise and automated nature of bio-printing makes it a particularly attractive choice for the fabrication of dermal substitutes containing stem cells. In the future, it may even be possible to bio-print bespoke dermal substitutes in situ.
References
Aggarwal S, Pittenger MF (2005) Human mesenchymal stem cells modulate allogeneic immune cell responses. Blood 105(4):1815
Ahmed TAE, Dare EV, Hincke M (2008) Fibrin: a versatile scaffold for tissue engineering applications. Tissue Eng Part B Rev 14(2):199–215
Altman AM, Matthias N, Yan Y, Song YH, Bai X, Chiu ES, Slakey DP, Alt EU (2008) Dermal matrix as a carrier for in vivo delivery of human adipose-derived stem cells. Biomaterials 29(10):1431–1442
Amoh Y, Li L, Campillo R, Kawahara K, Katsuoka K, Penman S, Hoffman RM (2005) Implanted hair follicle stem cells form Schwann cells that support repair of severed peripheral nerves. Pro Natl Acad Sci USA 102(49):17734–17738
Amos PJ, Kapur SK, Stapor PC, Shang H, Bekiranov S, Khurgel M, Rodeheaver GT, Peirce SM, Katz AJ (2010) Human adipose-derived stromal cells accelerate diabetic wound healing: impact of cell formulation and delivery. Tissue Eng Part A 16(5):1595–1606
Anderson DG, Levenberg S, Langer R (2004) Nanoliter-scale synthesis of arrayed biomaterials and application to human embryonic stem cells. Nat Biotechnol 22(7):863–866
Arthur A, Zannettino A, Gronthos S (2009) The therapeutic applications of multipotential mesenchymal/stromal stem cells in skeletal tissue repair. J Cell Physiol 218(2):237–245
Asai J, Takenaka H, Kusano KF, Ii M, Luedemann C, Curry C, Eaton E, Iwakura A, Tsutsumi Y, Hamada H, Kishimoto S, Thorne T, Kishore R, Losordo DW (2006) Topical sonic hedgehog gene therapy accelerates wound healing in diabetes by enhancing endothelial progenitor cell-mediated microvascular remodeling. Circulation 113(20):2413–2424
Ashton BA, Eaglesom CC, Bab I, Owen ME (1984) Distribution of fibroblastic colony-forming cells in rabbit bone marrow and assay of their osteogenic potential by an in vivo diffusion chamber method. Calcif Tissue Int 36(1):83–86
Askari AT, Unzek S, Popovic ZB, Goldman CK, Forudi F, Kiedrowski M, Rovner A, Ellis SG, Thomas JD, DiCorleto PE, Topol EJ, Penn MS (2003) Effect of stromal-cell-derived factor 1 on stem-cell homing and tissue regeneration in ischaemic cardiomyopathy. Lancet 362(9385):697–703
Ayres CE, Jha BS, Sell SA, Bowlin GL, Simpson DG (2010) Nanotechnology in the design of soft tissue scaffolds: innovations in structure and function. Wiley Interdiscip Rev Nanomed Nanobiotechnol 2(1):20–34
Bach FH, Albertini RJ, Joo P, Anderson JL, Bortin MM (1968) Bone-marrow transplantation in a patient with the Wiskott-Aldrich syndrome. Lancet 2(7583):1364–1366
Badiavas EV, Falanga V (2003) Treatment of chronic wounds with bone marrow-derived cells. Arch Dermatol 139(4):510–516
Badillo AT, Chung S, Zhang L, Zoltick P, Liechty KW (2007) Lentiviral gene transfer of SDF-1 [alpha] to wounds improves diabetic wound healing. J Surg Res 143(1):35–42
Badillo AT, Zhang L, Liechty KW (2008) Stromal progenitor cells promote leukocyte migration through production of stromal-derived growth factor 1alpha: a potential mechanism for stromal progenitor cell-mediated enhancement of cellular recruitment to wounds. J Pediatr Surg 43(6):1128–1133
Baumann LS, Shamban A, Lupo MP, Monheit GD, Thomas JA, Murphy DK, Walker PS (2007) Comparison of smooth-gel hyaluronic acid dermal fillers with cross-linked bovine collagen: a multicenter, double-masked, randomized, within-subject study. Dermatol Surg 33(2):S128–S135
Beattie AJ, Gilbert TW, Guyot JP, Yates AJ, Badylak SF (2008) Chemoattraction of progenitor cells by remodeling extracellular matrix scaffolds. Tissue Eng Part A 15(5):1119–1125
Beddington RS, Robertson EJ (1989) An assessment of the developmental potential of embryonic stem cells in the midgestation mouse embryo. Development 105(4):733–737
Bell E, Ivarsson B, Merrill C (1979) Production of a tissue-like structure by contraction of collagen lattices by human fibroblasts of different proliferative potential in vitro. Proc Natl Acad Sci USA 76(3):1274–1278
Bellon G, Martiny L, Robinet A (2004) Matrix metalloproteinases and matrikines in angiogenesis. Crit Rev Oncol Hematol 49(3):203–220
Beumer GJ, Van Blitterswijk CA, Bakker D, Ponec M (1993) Cell-seeding and in vitro biocompatibility evaluation of polymeric matrices of PEO/PBT copolymers and PLLA. Biomaterials 14(8):598–604
Bhardwaj N, Kundu SC (2010) Electrospinning: a fascinating fiber fabrication technique. Biotechnol Adv 28(3):325–347
Bianco P, Riminucci M, Gronthos S, Robey PG (2001) Bone marrow stromal stem cells: nature, biology, and potential applications. Stem Cells 19(3):180–192
Brusselaers N, Pirayesh A, Hoeksema H, Richters CD, Verbelen J, Beele H, Blot SI, Monstrey S (2010) Skin replacement in burn wounds. J Trauma 68(2):490–501
Caravaggi C, De Giglio R, Pritelli C, Sommaria M, Dalla Noce S, Faglia E, Mantero M, Clerici G, Fratino P, Dalla Paola L, Mariani G, Mingardi R, Morabito A (2003) HYAFF 11-based autologous dermal and epidermal grafts in the treatment of noninfected diabetic plantar and dorsal foot ulcers. Diabetes Care 26(10):2853–2859
Carpenter MK, Frey-Vasconcells J, Rao MS (2009) Developing safe therapies from human pluripotent stem cells. Nat Biotech 27(7):606–613
Casasco M, Casasco A, Icaro Cornaglia A, Farina A, Calligaro A (2004) Differential distribution of elastic tissue in human natural skin and tissue-engineered skin. J Mol Histol 35(4):421–428
Cavazzana-Calvo M, Hacein-Bey S, Basile GS, Gross F, Yvon E, Nusbaum P, Selz F, Hue C, Certain S, Casanova JL, Bousso P, Deist FL, Fischer A (2000) Gene therapy of human severe combined immunodeficiency (SCID)-X1 disease. Science 288(5466):669–672
Chen G, Sato T, Ohgushi H, Ushida T, Tateishi T, Tanaka J (2005) Culturing of skin fibroblasts in a thin PLGA-collagen hybrid mesh. Biomaterials 26(15):2559–2566
Chen RN, Ho HO, Tsai YT, Sheu MT (2004) Process development of an acellular dermal matrix (ADM) for biomedical applications. Biomaterials 25(13):2679–2686
Clark RAF, Ghosh K, Tonnesen MG (2007) Tissue engineering for cutaneous wounds. J Invest Dermatol 127(5):1018–1029
Cotsarelis G, Sun TT, Lavker RM (1990) Label-retaining cells reside in the bulge area of pilosebaceous unit: implications for follicular stem cells, hair cycle, and skin carcinogenesis. Cell 61(7):1329–1337
Cukierman E, Pankov R, Stevens DR, Yamada KM (2001) Taking cell-matrix adhesions to the third dimension. Science 294(5547):1708–1712
Dahl SLM, Koh J, Prabhakar V, Niklason LE (2003) Decellularized native and engineered arterial scaffolds for transplantation. Cell Transplant 12(6):659–666
Discher DE, Mooney DJ, Zandstra PW (2009) Growth factors, matrices, and forces combine and control stem cells. Science 324(5935):1673–1677
Drossopoulou G, Lewis KE, Sanz-Ezquerro JJ, Nikbakht N, McMahon AP, Hofmann C, Tickle C (2000) A model for anteroposterior patterning of the vertebrate limb based on sequential long-and short-range SHH signalling and BMP signalling. Development 127(7):1337–1348
Duocastella M, Fernández-Pradas J, Serra P, Morenza J (2008) Jet formation in the laser forward transfer of liquids. Appl Phys A Mater Sci Process 93(2):453–456
Ehrbar M, Djonov VG, Schnell C, Tschanz SA, Martiny-Baron G, Schenk U, Wood J, Burri PH, Hubbell JA, Zisch AH (2004) Cell-demanded liberation of VEGF121 from fibrin implants induces local and controlled blood vessel growth. Circ Res 94(8):1124–1132
El Ghalbzouri A, Lamme EN, van Blitterswijk C, Koopman J, Ponec M (2004) The use of PEGT/PBT as a dermal scaffold for skin tissue engineering. Biomaterials 25(15):2987–2996
Elcin YM, Dixit V, Gitnick G (2001) Extensive in vivo angiogenesis following controlled release of human vascular endothelial cell growth factor: implications for tissue engineering and wound healing. Artif Organs 25(7):558–565
Engler AJ, Sen S, Sweeney HL, Discher DE (2006) Matrix elasticity directs stem cell lineage specification. Cell 126(4):677–689
Falanga V, Iwamoto S, Chartier M, Yufit T, Butmarc J, Kouttab N, Shrayer D, Carson P (2007) Autologous bone marrow-derived cultured mesenchymal stem cells delivered in a fibrin spray accelerate healing in murine and human cutaneous wounds. Tissue Eng 13(6):1299–1312
Fan VH, Au A, Tamama K, Littrell R, Richardson LB, Wright JW, Wells A, Griffith LG (2007) Tethered epidermal growth factor provides a survival advantage to mesenchymal stem cells. Stem Cells 25(5):1241–1251
Fisher OZ, Khademhosseini A, Langer R, Peppas NA (2010) Bioinspired materials for controlling stem cell fate. Acc Chem Res 43(3):419–428
Flaim CJ, Chien S, Bhatia SN (2005) An extracellular matrix microarray for probing cellular differentiation. Nat Methods 2(2):119–125
Fox A, Smythe J, Fisher N, Tyler MPH, McGrouther DA, Watt SM, Harris AL (2008) Mobilization of endothelial progenitor cells into the circulation in burned patients. Br J Surg 95(2):244–251
Fu X, Fang L, Li X, Cheng B, Sheng Z (2006) Enhanced wound healing quality with bone marrow mesenchymal stem cells autografting after skin injury. Wound Repair Regen 14(3):325–335
Fu XB, Fang LJ, Wang YX, Sun TZ, Cheng B (2004) Enhancing the repair quality of skin injury on porcine after autografting with the bone marrow mesenchymal stem cells. Zhonghua Yi Xue Za Zhi 84(11):9204
Fu YC, Nie H, Ho ML, Wang CK, Wang CH (2008) Optimized bone regeneration based on sustained release from three-dimensional fibrous PLGA/HAp composite scaffolds loaded with BMP-2. Biotechnol Bioeng 99(4):996–1006
Gimble JM, Guilak F (2003) Adipose-derived adult stem cells: isolation, characterization, and differentiation potential. Cytotherapy 5(5):362–369
Goetz AK, Scheffler B, Chen HX, Wang S, Suslov O, Xiang H, Brüstle O, Roper SN, Steindler DA (2006) Temporally restricted substrate interactions direct fate and specification of neural precursors derived from embryonic stem cells. Proc Natl Acad Sci USA 103(29):11063–11068
Goissis G, Suzigan S, Parreira DR, Maniglia JV, Braile DM, Raymundo S (2000) Preparation and characterization of collagen elastin matrices from blood vessels intended as small diameter vascular grafts. Artif Organs 24(3):217–223
Gronthos S, Franklin DM, Leddy HA, Robey PG, Storms RW, Gimble JM (2001) Surface protein characterization of human adipose tissue-derived stromal cells. J Cell Physiol 189(1):54–63
Gronthos S, Zannettino ACW, Hay SJ, Shi S, Graves SE, Kortesidis A, Simmons PJ (2003) Molecular and cellular characterisation of highly purified stromal stem cells derived from human bone marrow. J Cell Sci 116:1827–1835
Guilak F, Lott KE, Awad HA, Cao Q, Hicok KC, Fermor B, Gimble JM (2006) Clonal analysis of the differentiation potential of human adipose-derived adult stem cells. J Cell Physiol 206(1):229–237
Guillemot F, Souquet A, Catros S, Guillotin B, Lopez J, Faucon M, Pippenger B, Bareille R, Rémy M, Bellance S, Chabassier P, Fricain JC, Amedee J (2010) High-throughput laser printing of cells and biomaterials for tissue engineering. Acta Biomater 6(7):2494–2500
Gunatillake PA, Adhikari R (2003) Biodegradable synthetic polymers for tissue engineering. Eur Cell Mater 5(1):1–16
Gupta A, Seifalian AM, Ahmad Z, Edirisinghe MJ, Winslet MC (2007) Novel electrohydrodynamic printing of nanocomposite biopolymer scaffolds. J Bioact Compat Polym 22(3):265–280
Hanson SE, Bentz ML, Hematti P (2010) Mesenchymal stem cell therapy for nonhealing cutaneous wounds. Plast Reconstr Surg 125(2):510–516
Haslik W, Kamolz LP, Nathschläger G, Andel H, Meissl G, Frey M (2007) First experiences with the collagen-elastin matrix Matriderm® as a dermal substitute in severe burn injuries of the hand. Burns 33(3):364–368
He W, Horn SW, Hussain MD (2007) Improved bioavailability of orally administered mifepristone from PLGA nanoparticles. Int J Pharm 334(1–2):173–178
de Vries HJ, Middelkoop E, Mekkes JR, Dutrieux RP, Wildevuur CH, Westerhof H (1994) Dermal regeneration in native non-cross-linked collagen sponges with different extracellular matrix molecules. Wound Repair Regen 2(1):37–47
Hodgkinson T, Yuan XF, Bayat A (2009) Adult stem cells in tissue engineering. Expert Rev Med Devices 6(6):621–640
Hoffman LM, Carpenter MK (2005) Characterization and culture of human embryonic stem cells. Nat Biotechnol 23(6):699–708
Hopp B, Smausz T, Kresz N, Barna N, Bor Z, Kolozsvari L, Chrisey D, Szabó A, Nógrádi A (2005) Survival and proliferative ability of various living cell types after laser-induced forward transfer. Tissue Eng 11(11–12):1817–1823
Huang S, Chen CS, Ingber DE (1998) Control of cyclin D1, p27Kip1, and cell cycle progression in human capillary endothelial cells by cell shape and cytoskeletal tension. Mol Biol Cell 9(11):3179–3193
Huang S, Xu Y, Wu C, Sha D, Fu X (2010) In vitro constitution and in vivo implantation of engineered skin constructs with sweat glands. Biomaterials 31(21):5520–5525
Huang S, Zhang Y, Tang L, Deng Z, Lu W, Feng F, Xu X, Jin Y (2009) Functional bilayered skin substitute constructed by tissue-engineered extracellular matrix and microsphere-incorporated gelatin hydrogel for wound repair. Tissue Eng Part A 15(9):2617–2624
Hudson TW, Liu SY, Schmidt CE (2004) Engineering an improved acellular nerve graft via optimized chemical processing. Tissue Eng 10(9–10):1346–1358
Jahoda CA (2003) Cell movement in the hair follicle dermis—more than a two-way street? J Invest Dermatol 121(6):ix–xi
Jahoda CAB, Whitehouse CJ, Reynolds AJ, Hole N (2003) Hair follicle dermal cells differentiate into adipogenic and osteogenic lineages. Exp Dermatol 12(6):849–859
Pachence JM (1996) Collagen-based devices for soft tissue repair. J Biomed Mater Res 33(1):35–40
Jayasinghe SN, Irvine S, McEwan JR (2007) Cell electrospinning highly concentrated cellular suspensions containing primary living organisms into cell-bearing threads and scaffolds. Nanomedicine 2(4):555–567
Jiang Y, Jahagirdar BN, Reinhardt RL, Schwartz RE, Keene CD, Ortiz-Gonzalez XR, Reyes M, Lenvik T, Lund T, Blackstad M, Du J, Aldrich S, Lisberg A, Low WC, Largaespada DA, Verfaillie CM (2002) Pluripotency of mesenchymal stem cells derived from adult marrow. Nature 418(6893):41–49
Jones PH, Watt FM (1993) Separation of human epidermal stem cells from transit amplifying cells on the basis of differences in integrin function and expression. Cell 73(4):713–724
Kang X, Xie Y, Powell HM, James Lee L, Belury MA, Lannutti JJ, Kniss DA (2007) Adipogenesis of murine embryonic stem cells in a three-dimensional culture system using electrospun polymer scaffolds. Biomaterials 28(3):450–458
Kastrinaki MC, Sidiropoulos P, Roche S, Ringe J, Lehmann S, Kritikos H, Vlahava VM, Delorme B, Eliopoulos GD, Jorgensen C (2008) Functional, molecular and proteomic characterisation of bone marrow mesenchymal stem cells in rheumatoid arthritis. Ann Rheum Dis 67(6):741–749
Kearney JN (2001) Clinical evaluation of skin substitutes. Burns 27(5):545–551
Kemp P (2006) History of regenerative medicine: looking backwards to move forwards. Regen Med 1(5):653–669
Kim D, Kim CH, Moon JI, Chung YG, Chang MY, Han BS, Ko S, Yang E, Cha KY, Lanza R, Kim KS (2009) Generation of human induced pluripotent stem cells by direct delivery of reprogramming proteins. Cell Stem Cell 4(6):472–476
Kim MS, Bhang SH, Yang HS, Rim NG, Jun I, Kim SI, Kim BS, Shin H (2010) Development of functional fibrous matrices for the controlled release of basic fibroblast growth factor to improve therapeutic angiogenesis. Tissue Eng Part A 16(10):2999–3010
Knoepfler PS (2009) Deconstructing stem cell tumorigenicity: a roadmap to safe regenerative medicine. Stem Cells 27(5):1050–1056
Kolokol’chikova EG, Budkevich LI, Bobrovnikov AE, Badikova AK, Tumanov VP (2001) Morphological changes in burn wounds after transplantation of allogenic fibroblasts. Bull Exp Biol Med 131(1):89–93
Kotton DN, Fine A (2003) Derivation of lung epithelium from bone marrow cells. Cytotherapy 5(2):169–173
Kumar RK, O’Grady R, Li W, Smith LW, Rhodes GC (1991) Primary culture of adult mouse lung fibroblasts in serum-free medium: responses to growth factors. Exp Cell Res 193(2):398–404
Kusano KF, Pola R, Murayama T, Curry C, Kawamoto A, Iwakura A, Shintani S, Ii M, Asai J, Tkebuchava T, Thorne T, Takenaka H, Aikawa R, Goukassian D, von Samson P, Hamada H, Yoon YS, Silver M, Eaton E, Ma H, Heyd L, Kearney M, Munger W, Porter JA, Kishore R, Losordo DW (2005) Sonic hedgehog myocardial gene therapy: tissue repair through transient reconstitution of embryonic signaling. Nat Med 11(11):1197–1204
Lajtha LG (2006) Stem cell concepts. Differentiation 14(1–3):23–33
Lattari V, Jones LM, Varcelotti JR, Latenser BA, Sherman HF, Barrette RR (1997) The use of a permanent dermal allograft in full-thickness burns of the hand and foot: a report of three cases. J Burn Care Rehabil 18(2):147–155
Lee RH, Kim BC, Choi IS, Kim H, Choi HS, Suh KT, Bae YC, Jung JS (2004) Characterization and expression analysis of mesenchymal stem cells from human bone marrow and adipose tissue. Cell Physiol Biochem 14(4–6):311–324
Li C, Vepari C, Jin HJ, Kim HJ, Kaplan DL (2006) Electrospun silk-BMP-2 scaffolds for bone tissue engineering. Biomaterials 27(16):3115–3124
Li WJ, Laurencin CT, Caterson EJ, Tuan RS, Ko FK (2002) Electrospun nanofibrous structure: a novel scaffold for tissue engineering. J Biomed Mater Res Part A 60(4):613–621
Liu H, Zhu F, Yong J, Zhang P, Hou P, Li H, Jiang W, Cai J, Liu M, Cui K, Qu X, Xiang T, Lu D, Chi X, Gao G, Ji W, Ding M, Deng H (2008) Generation of induced pluripotent stem cells from adult rhesus monkey fibroblasts. Cell Stem Cell 3(6):587–590
Liu P, Deng Z, Han S, Liu T, Wen N, Lu W, Geng X, Huang S, Jin Y (2008) Tissue-engineered skin containing mesenchymal stem cells improves burn wounds. Artif Organs 32(12):925–931
Lukashev ME, Werb Z (1998) ECM signalling: orchestrating cell behaviour and misbehaviour. Trends Cell Biol 8(11):437–441
Lund AW, Yener B, Stegemann JP, Plopper GE (2009) The natural and engineered 3D microenvironment as a regulatory cue during stem cell fate determination. Tissue Eng Part B Rev 15(3):371–380
Lutolf MP, Hubbell JA (2005) Synthetic biomaterials as instructive extracellular microenvironments for morphogenesis in tissue engineering. Nat Biotechnol 23(1):47–55
Maherali N, Sridharan R, Xie W, Utikal J, Eminli S, Arnold K, Stadtfeld M, Yachechko R, Tchieu J, Jaenisch R (2007) Directly reprogrammed fibroblasts show global epigenetic remodeling and widespread tissue contribution. Cell Stem Cell 1(1):55–70
Mansbridge J, Liu K, Patch R, Symons K, Pinney E (1998) Three-dimensional fibroblast culture implant for the treatment of diabetic foot ulcers: metabolic activity and therapeutic range. Tissue Eng 4(4):403–414
Mansilla E, Marin GH, Sturla F, Drago HE, Gil MA, Salas E, Gardiner MC, Piccinelli G, Bossi S, Petrelli L, Iorio G, Ramos CA, Soratti C (2005) Human mesenchymal stem cells are tolerized by mice and improve skin and spinal cord injuries. Transplant Proc 37(1):292–294
Mei Y, Gerecht S, Taylor M, Urquhart AJ, Bogatyrev SR, Cho SW, Davies MC, Alexander MR, Langer RS, Anderson DG (2009) Mapping the interactions among biomaterials, adsorbed proteins, and human embryonic stem cells. Adv Mater 21(27):2781–2786
Mikos AG, Bao Y, Cima LG, Ingber DE, Vacanti JP, Langer R (1993) Preparation of poly (glycolic acid) bonded fiber structures for cell attachment and transplantation. J Biomed Mater Res 27(2):183–189
Mironov V, Boland T, Trusk T, Forgacs G, Markwald RR (2003) Organ printing: computer-aided jet-based 3D tissue engineering. Trends Biotechnol 21(4):157–161
Mironov V, Kasyanov V, Drake C, Markwald RR (2008) Organ printing: promises and challenges. Regen Med 3(1):93–103
Mironov V, Reis N, Derby B (2006) Review: bioprinting: a beginning. Tissue Eng 12(4):631–634
Mironov V, Visconti RP, Kasyanov V, Forgacs G, Drake CJ, Markwald RR (2009) Organ printing: tissue spheroids as building blocks. Biomaterials 30(12):2164–2174
Mitsiadis TA, Barrandon O, Rochat A, Barrandon Y, De Bari C (2007) Stem cell niches in mammals. Exp Cell Res 313(16):3377–3385
Mizuno H, Miyamoto M, Shimamoto M, Koike S, Hyakusoku H, Kuroyanagi Y (2010) Therapeutic angiogenesis by autologous bone marrow cell implantation together with allogeneic cultured dermal substitute for intractable ulcers in critical limb ischaemia. J Plast Reconstr Aesthet Surg 63(11):1875–1882
Mooney DJ, Baldwin DF, Suh NP, Vacanti JP, Langer R (1996) Novel approach to fabricate porous sponges of poly (-lactic-co-glycolic acid) without the use of organic solvents. Biomaterials 17(14):1417–1422
Moriyama K, Shimokawa H, Susami T, Sasaki S, Kuroda T (1991) Effects of growth factors on mucosal scar fibroblasts in culture—a possible role of growth factors in scar formation. Matrix 11(3):190
Morris RJ, Liu Y, Marles L, Yang Z, Trempus C, Li S, Lin JS, Sawicki JA, Cotsarelis G (2004) Capturing and profiling adult hair follicle stem cells. Nat Biotechnol 22(4):411–417
Mostow EN, Haraway GD, Dalsing M, Hodde JP, King D (2005) Effectiveness of an extracellular matrix graft (OASIS Wound Matrix) in the treatment of chronic leg ulcers: a randomized clinical trial. J Vasc Surg 41(5):837–843
Müller LUW, Daley GQ, Williams DA (2009) Upping the ante: recent advances in direct reprogramming. Mol Ther 17(6):947–953
Nair K, Gandhi M, Khalil S, Yan KC, Marcolongo M, Barbee K, Sun W (2009) Characterization of cell viability during bioprinting processes. Biotechnol J 4(8):1168–1177
Nakagawa H, Akita S, Fukui M, Fujii T, Akino K (2005) Human mesenchymal stem cells successfully improve skin-substitute wound healing. Br J Dermatol 153(1):29–36
Nakajima M, Ishimuro T, Kato K, Ko IK, Hirata I, Arima Y, Iwata H (2007) Combinatorial protein display for the cell-based screening of biomaterials that direct neural stem cell differentiation. Biomaterials 28(6):1048–1060
Nakamura M, Kobayashi A, Takagi F, Watanabe A, Hiruma Y, Ohuchi K, Iwasaki Y, Horie M, Morita I, Takatani S (2005) Biocompatible inkjet printing technique for designed seeding of individual living cells. Tissue Eng 11(11–12):1658–1666
Nambu M, Kishimoto S, Nakamura S, Mizuno H, Yanagibayashi S, Yamamoto N, Azuma R, Kiyosawa T, Ishihara M (2009) Accelerated wound healing in healing-impaired db/db mice by autologous adipose tissue-derived stromal cells combined with atelocollagen matrix. Ann Plast Surg 62(3):317–321
Neuss S, Apel C, Buttler P, Denecke B, Dhanasingh A, Ding X, Grafahrend D, Groger A, Hemmrich K, Herr A (2008) Assessment of stem cell/biomaterial combinations for stem cell-based tissue engineering. Biomaterials 29(3):302–313
Ng KW, Hutmacher DW, Schantz JT, Ng CS, Too HP, Lim TC, Phan TT, Teoh SH (2001) Evaluation of ultra-thin poly (-caprolactone) films for tissue-engineered skin. Tissue Eng 7(4):441–455
Nie C, Yang D, Morris SF (2009) Local delivery of adipose-derived stem cells via acellular dermal matrix as a scaffold: a new promising strategy to accelerate wound healing. Med Hypotheses 72(6):679–682
Niezgoda JA, Van Gils CC, Frykberg RG, Hodde JP (2005) Randomized clinical trial comparing OASIS Wound Matrix to Regranex Gel for diabetic ulcers. Adv Skin Wound Care 18(5):258–266
Odde D, Renn M (2000) Laser-guided direct writing of living cells. Biotechnol Bioeng 67(3):312–318
Okita K, Ichisaka T, Yamanaka S (2007) Generation of germline-competent induced pluripotent stem cells. Nature 448(7151):313–317
Park IH, Zhao R, West JA, Yabuuchi A, Huo H, Ince TA, Lerou PH, Lensch MW, Daley GQ (2007) Reprogramming of human somatic cells to pluripotency with defined factors. Nature 451(7175):141–146
Pek YS, Wan ACA, Ying JY (2010) The effect of matrix stiffness on mesenchymal stem cell differentiation in a 3D thixotropic gel. Biomaterials 31(3):385–391
Pessina A, Gribaldo L (2006) The key role of adult stem cells: therapeutic perspectives. Curr Med Res Opin 22(11):2287–2300
Phillippi JA, Miller E, Weiss L, Huard J, Waggoner A, Campbell P (2008) Microenvironments engineered by inkjet bioprinting spatially direct adult stem cells toward muscle-and bone-like subpopulations. Stem Cells 26(1):127–134
Powell HM, Supp DM, Boyce ST (2008) Influence of electrospun collagen on wound contraction of engineered skin substitutes. Biomaterials 29(7):834–843
Price RD, Das-Gupta V, Harris PA, Leigh IM, Navsaria HA (2004) The role of allogenic fibroblasts in an acute wound healing model. Plast Reconstr Surg 113(6):1719–1729
Prockop DJ (1997) Marrow stromal cells as stem cells for nonhematopoietic tissues. Science 276(5309):71–74
Prockop DJ, Gregory CA, Spees JL (2003) One strategy for cell and gene therapy: harnessing the power of adult stem cells to repair tissues. Proc Natl Acad Sci USA 100(Suppl 1):11917–11923
Rabbany SY, Pastore J, Yamamoto M, Miller T, Rafii S, Aras R, Penn M (2010) Continuous delivery of stromal cell-derived factor-1 from alginate scaffolds accelerates wound healing. Cell Transplant 19(4):399–408
Rasulov MF, Vasil’chenkov AV, Onishchenko NA, Krasheninnikov ME, Kravchenko VI, Gorshenin TL, Pidtsan RE, Potapov IV (2005) First experience in the use of bone marrow mesenchymal stem cells for the treatment of a patient with deep skin burns. Bull Exp Biol Med 139(1):141–144
Ravanti L, Heino J, López-Ot n C, Kähäri VM (1999) Induction of collagenase-3 (MMP-13) expression in human skin fibroblasts by three-dimensional collagen is mediated by p38 mitogen-activated protein kinase. J Biol Chem 274(4):2446–2455
Richardson GD, Arnott EC, Whitehouse CJ, Lawrence CM, Reynolds AJ, Hole N, Jahoda CAB (2005) Plasticity of rodent and human hair follicle dermal cells: implications for cell therapy and tissue engineering. J Investig Dermatol Symp Proc 10(3):180–183
Romanelli M, Dini V, Bertone M, Barbanera S, Brilli C (2007) OASIS® wound matrix versus Hyaloskin® in the treatment of difficult to heal wounds of mixed arterial/venous aetiology. Int Wound J 4(1):3–7
Saha K, Keung AJ, Irwin EF, Li Y, Little L, Schaffer DV, Healy KE (2008) Substrate modulus directs neural stem cell behavior. Biophys J 95(9):4426–4438
Sanders JE, Stiles CE, Hayes CL (2000) Tissue response to single-polymer fibers of varying diameters: evaluation of fibrous encapsulation and macrophage density. J Biomed Mater Res 52(1):231–237
Sasaki M, Abe R, Fujita Y, Ando S, Inokuma D, Shimizu H (2008) Mesenchymal stem cells are recruited into wounded skin and contribute to wound repair by transdifferentiation into multiple skin cell type. J Immunol 180(4):2581–2587
Schlüter H, Kaur P (2009) Bioengineered human skin from embryonic stem cells. Lancet 374(9703):1725–1726
Schofield R (1978) The relationship between the spleen colony-forming cell and the haemopoietic stem cell. Blood Cells 4(1–2):7
Seppä H, Grotendorst G, Seppä S, Schiffmann E, Martin GR (1982) Platelet-derived growth factor in chemotactic for fibroblasts. J Cell Biol 92(2):584–588
Shigehiko S, Katsuya K, Faramartz A, Naoki M, Yoshihiko N, Yoshito I (2000) Long-term follow-up study of artificial dermis composed of outer silicone layerand inner collagen sponge. Br J Plast Surg 53(8):659–666
Singh M, Berkland C, Detamore MS (2008) Strategies and applications for incorporating physical and chemical signal gradients in tissue engineering. Tissue Eng Part B Rev 14(4):341–366
Spees JL, Olson SD, Ylostalo J, Lynch PJ, Smith J, Perry A, Peister A, Wang MY, Prockop DJ (2003) Differentiation, cell fusion, and nuclear fusion during ex vivo repair of epithelium by human adult stem cells from bone marrow stroma. Proc Natl Acad Sci USA 100(5):2397–2402
Stoff A, Rivera AA, Banerjee NS, Moore ST, Numnum TM, Espinosa-de-los-Monteros A, Richter DF, Siegal GP, Chow LT, Feldman D (2008) Promotion of incisional wound repair by human mesenchymal stem cell transplantation. Exp Dermatol 18(4):362–369
Strande LF, Foley ST, Doolin EJ, Hewitt CW (1997) In vitro bioartificial skin culture model of tissue rejection and inflammatory/immune mechanisms. Transplant Proc 29(4):2118–2119
Tabata Y (2003) Tissue regeneration based on growth factor release. Tissue Eng 9(1):5–15
Takahashi K, Tanabe K, Ohnuki M, Narita M, Ichisaka T, Tomoda K, Yamanaka S (2007) Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell 131(5):861–872
Takahashi K, Yamanaka S (2006) Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126(4):663–676
Takemoto S, Morimoto N, Kimura Y, Taira T, Kitagawa T, Tomihata K, Tabata Y, Suzuki S (2008) Preparation of collagen/gelatin sponge scaffold for sustained release of bFGF. Tissue Eng Part A 14(10):1629–1638
Thomson JA, Itskovitz-Eldor J, Shapiro SS, Waknitz MA, Swiergiel JJ, Marshall VS, Jones JM (1998) Embryonic stem cell lines derived from human blastocysts. Science 282(5391):1145–1147
Tögel F, Westenfelder C (2007) Adult bone marrow-derived stem cells for organ regeneration and repair. Dev Dyn 236(12):3321–3331
Tran KT, Lamb P, Deng JS (2005) Matrikines and matricryptins: implications for cutaneous cancers and skin repair. J Dermatol Sci 40(1):11–20
Uzunismail A, Duman A, Perk C, Findik H, Beyhan G (2008) The effects of acellular dermal allograft (AlloDerm®) interface on silicone-related capsule formation—experimental study. Eur J Plast Surg 31(4):179–185
van der Flier LG, Clevers H (2009) Stem cells, self-renewal, and differentiation in the intestinal epithelium. Annu Rev Physiol 71:241–260
Vats A, Tolley NS, Polak JM, Gough JE (2003) Scaffolds and biomaterials for tissue engineering: a review of clinical applications. Clin Otolaryngol Allied Sci 28(3):165–172
Wainwright D, Madden M, Luterman A, Hunt J, Monafo W, Heimbach D, Kagan R, Sittig K, Dimick A, Herndon D (1996) Clinical evaluation of an acellular allograft dermal matrix in full-thickness burns. J Burn Care Rehabil 17(2):124–136
Wainwright DJ (1995) Use of an acellular allograft dermal matrix (AlloDerm) in the management of full-thickness burns. Burns 21(4):243–248
Watanabe S, Wang XEN, Hirose M, Oide H, Kitamura T, Miyazaki A, Sato N (1995) Basic fibroblast growth factor accelerates gastric mucosal restoration in vitro by promoting mesenchymal cell migration and proliferation. J Gastroenterol Hepatol 10(6):627–632
Watt FM, Hogan BL (2000) Out of Eden: stem cells and their niches. Science 287(5457):1427–1430
Wernig M, Meissner A, Foreman R, Brambrink T, Ku M, Hochedlinger K, Bernstein BE, Jaenisch R (2007) In vitro reprogramming of fibroblasts into a pluripotent ES-cell-like state. Nature 448(7151):318–324
Whitaker MJ, Quirk RA, Howdle SM, Shakesheff KM (2001) Growth factor release from tissue engineering scaffolds. J Pharm Pharmacol 53(11):1427–1437
Wiseman DM, Polverini PJ, Kamp DW, Leibovich SJ (1988) Transforming growth factor-beta (TGF [beta]) is chemotactic for human monocytes and induces their expression of angiogenic activity. Biochem Biophys Res Commun 157(2):793–800
Witte MB, Barbul A (1997) General principles of wound healing. Surg Clin North Am 77(3):509–528
Woods T, Gratzer PF (2005) Effectiveness of three extraction techniques in the development of a decellularized bone-anterior cruciate ligament-bone graft. Biomaterials 26(35):7339–7349
Xu T, Jin J, Gregory C, Hickman J, Boland T (2005) Inkjet printing of viable mammalian cells. Biomaterials 26(1):93–99
Yan Y, Wang X, Pan Y, Liu H, Cheng J, Xiong Z, Lin F, Wu R, Zhang R, Lu Q (2005) Fabrication of viable tissue-engineered constructs with 3D cell-assembly technique. Biomaterials 26(29):5864–5871
Yang J, Shi G, Bei J, Wang S, Cao Y, Shang Q, Yang G, Wang W (2002) Fabrication and surface modification of macroporous poly (L lactic acid) and poly (L lactic co glycolic acid) (70/30) cell scaffolds for human skin fibroblast cell culture. J Biomed Mater Res 62(3):438–446
Yang S, Leong KF, Du Z, Chua CK (2001) The design of scaffolds for use in tissue engineering. Part I. Traditional factors. Tissue Eng 7(6):679–689
Yang X, Shah JD, Wang H (2009) Nanofiber enabled layer-by-layer approach toward three-dimensional tissue formation. Tissue Eng Part A 15(4):945–956
Yao S, Chen S, Clark J, Hao E, Beattie GM, Hayek A, Ding S (2006) Long-term self-renewal and directed differentiation of human embryonic stem cells in chemically defined conditions. Proc Natl Acad Sci USA 103(18):6907–6912
Yoshikawa T, Mitsuno H, Nonaka I, Sen Y, Kawanishi K, Inada Y, Takakura Y, Okuchi K, Nonomura A (2008) Wound therapy by marrow mesenchymal cell transplantation. Plast Reconstr Surg 121(3):860–877
Zhou H, Wu S, Joo JY, Zhu S, Han DW, Lin T, Trauger S, Bien G, Yao S, Zhu Y (2009) Generation of induced pluripotent stem cells using recombinant proteins. Cell Stem Cell 4(5):381–384
Zhu X, Cui W, Li X, Jin Y (2008) Electrospun fibrous mats with high porosity as potential scaffolds for skin tissue engineering. Biomacromolecules 9(7):1795–1801
Zisch AH, Lutolf MP, Ehrbar M, Raeber GP, Rizzi SC, Davies N, Schmokel H, Bezuidenhout D, Djonov V, Zilla P, Hubbell JA (2003) Cell-demanded release of VEGF from synthetic, biointeractive cell-ingrowth matrices for vascularized tissue growth. FASEB J 17(5):2260–2262
Zisch AH, Lutolf MP, Hubbell JA (2003) Biopolymeric delivery matrices for angiogenic growth factors. Cardiovasc Pathol 12(6):295–310
Zisch AH, Schenk U, Schense JC, Sakiyama-Elbert SE, Hubbell JA (2001) Covalently conjugated VEGF-fibrin matrices for endothelialization. J Control Release 72(1–3):101–113
Zuk PA, Zhu M, Ashjian P, De Ugarte DA, Huang JI, Mizuno H, Alfonso ZC, Fraser JK, Benhaim P, Hedrick MH (2002) Human adipose tissue is a source of multipotent stem cells. Mol Biol Cell 13(12):4279–4295
Related articles recently published in Archives of Dermatological Research (selected by the journal’s editorial staff)
Kim WS, Park BS, Sung JH (2009) Protective role of adipose-derived stem cells and their soluble factors in photoaging. Arch Dermatol Res 301:329–336
Salvolini E, Lucarini G, Zizzi A, Orciani M, Di Benedetto G, Di Primio R (2010) Human skin-derived mesenchymal stem cells as a source of VEGF and nitric oxide. Arch Dermatol Res 302:367–374
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hodgkinson, T., Bayat, A. Dermal substitute-assisted healing: enhancing stem cell therapy with novel biomaterial design. Arch Dermatol Res 303, 301–315 (2011). https://doi.org/10.1007/s00403-011-1131-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-011-1131-2