Abstract
Purpose
There is rising impact of patient-reported outcome (PRO) measurement in joint arthroplasty over the past years. Bicruciate-retaining implants have shown more physiologic knee kinematics and provide superior proprioceptive capacities. The aim of this study was to evaluate if the functional properties of this new implant design lead to improved PRO results after total knee arthroplasty (TKA).
Methods
This prospective, controlled trial compares PRO of bicruciate-retaining total knee arthroplasty (BCR-TKA) to unicondylar knee arthroplasty (UKA) and standard posterior-stabilized total knee arthroplasty (PS-TKA). We evaluated 102 patients (34 patients in each group) 18 months postoperatively after knee arthroplasty. Primary outcome measure was the Forgotten Joint Score (FJS).
Results
The BCR-group showed the same level of joint awareness as the UKA-group (p = 0.999). The second control group of PS-TKA patients had a lower mean score value in the FJS compared to the BCR-group (p = 0.035) and UKA-group (p = 0.031). There was no correlation of age, gender, body mass index (BMI) and the FJS. No relevant floor- or ceiling effects occurred.
Conclusions
This study found reduced joint awareness for BCR-TKA compared to a standard total knee arthroplasty. The score values of the BCR-group were equal to the UKA-group. Further prospective, randomized studies to investigate long-term survivorship of bicruciate-retaining implants are needed.
Level of evidence
Level II.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
There is rising impact of patient-reported outcome (PRO) measurement in joint arthroplasty over the past years [5, 13, 14, 31, 43, 45]. PROM-questionnaires have become important tools to evaluate the disease-related quality of life. Conventional questionnaires focus on functional aspects like the range of motion or ligamentous stability [22, 41]. The concept of the “Forgotten Joint Score” (FJS) has revolutionized outcome assessment rating the loss of awareness of the artificial knee joint as the ultimate goal resulting in maximum patient satisfaction [5]. The FJS has shown a high validity and reliability and good responsiveness in patients after total knee arthroplasty (TKA) later than 12 months postoperative [4, 5, 9, 40, 42, 43].
In the treatment of advanced osteoarthritis, TKA with the sacrifice of the anterior cruciate ligament is the standard treatment. The sacrifice of the anterior cruciate ligament (ACL) can result in abnormal kinematics with functional limitations and reduced balance [44]. Anatomic studies have shown that especially the anterior cruciate ligament contains a considerable number of proprioceptive nerve cells [39]. Prior studies on proprioception have shown similar abilities after medial unicompartmental knee arthroplasty (UKA) with preservation of the ACL compared to healthy control subjects of the same age [18]. New implant designs for TKA with preservation of both cruciate ligaments have shown that these implants are associated with a higher “overall satisfaction” [35]. Recently, a prospective cohort study could demonstrate that bicruciate-retaining implants can provide a level of proprioception comparable to a medial unicondylar knee arthroplasty (UKA) [3]. Kinematic analyses have also demonstrated more physiologic knee joint biomechanics compared to total knee arthroplasty [24, 33, 44]. Abnormal kinematics and a loss of proprioceptive abilities can also be associated with non-specific pain and a functional deficit after joint replacement [10, 44].
The question remains if an improvement in these functional properties leads to a higher patient satisfaction. Prior studies on proprioception and patient satisfaction or kinematics and patient satisfaction were using conventional clinical scores and revealed inconsistent information. To date, there is no study on PROM of bicruciate-retaining total knee arthroplasty (BCR TKA).
The purpose of the study is to compare the PRO in patients with BCR TKA to patients with a medial bicruciate-retaining UKA and to patients with a total knee arthroplasty sacrificing both cruciate ligaments.
Materials and methods
Study design
A prospective, controlled trial was conducted to compare PRO in patients after arthroplasty of the knee for advanced osteoarthritis. Of the 1312 patients who underwent knee arthroplasty between December 2013 and November 2015, 102 consecutive patients were included in this study.
Preoperative evaluation included medical history, a standardized clinical examination and a radiographic analysis consisted of a weight-bearing long-leg view, a Rosenberg view and a lateral view of the knee. Since the FJS is not validated for preoperative osteoarthritic conditions, we used the Oxford Knee Score for preoperative functional assessment. Osteoarthritis was rated according to the Kellgren and Lawrence Score [23].
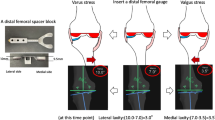
The BCR-implant (Vanguard XP, Biomet Inc., Warsaw, USA) used in this study is a recently developed TKA with a U-shaped tibial component to retain the anterior and posterior cruciate ligament. The anterior portion of the tibial component consists of a broad bar to provide sufficient rotating beam fatigue strength. The femoral component has also a new generation design with a funnel-shaped narrowed anterior femoral flange. For the TKA control group (PS) we used the Genesis II PS (Smith & Nephew plc, London, UK) since this is the ‘gold standard’ in our institution. The indications for implantation of a BCR- or PS-TKA were OA of more than one compartment. Both TKA-groups comprised patients with a manually correctable deformity of less than 10° of axis deviation (varus or valgus). Preoperative clinical examination included a Lachman test to exclude patients with relevant a–p instability. ACL deficiency was a contraindication for implantation of a BCR-TKA, which was visualized intraoperatively. Isolated medial compartment osteoarthritis was an indication for a medial unicompartmental arthroplasty according to the criteria by Berend [6]. Exclusion criteria were instability of the anterior cruciate ligament or varus/valgus deformity of more than 10°. Patients with another impairing locomotor disorder of the lower extremity, a mental disorder, or a lack of informed consent were also excluded.
There were three groups of patients (34 patients each):
-
The study group (BCR-group) consisted of patients with bi-compartmental osteoarthritis undergoing a bicruciate-retaining total knee arthroplasty (Vanguard XP, Biomet Inc., Warsaw, USA).
-
One control group (UKA-group) consisted of patients with isolated medial compartment osteoarthritis undergoing implantation of a medial unicompartmental knee arthroplasty using a mobile bearing (Oxford, Biomet Inc., Warsaw, USA).
-
The second control group (PS-group) consisted of patients with bi-compartmental osteoarthritis undergoing posterior stabilized total knee arthroplasty (Genesis II PS, Smith&Nephew plc, London, UK).
The patient population comprised 53 women (52.0%) and 49 men. The mean age was 62.3 ± 9.5 years (range 38–81). Fifty-five patients involved the right knee (54.0%), 47 patients the left knee (Table 1). All patients had primary implantation performed by the senior author (C.T.). We used a medial sub-vastus approach for implantation of UKA and a mid-vastus approach for total joint replacements (BCR-group and PS-group). Implantation was performed in a highly standardized setting using tourniquet control and cementation of all implants. We reserve a patello-femoral resurfacing (PFR) for cases of severe patello-femoral degenerations. Postoperative care was equal for all patients: analgesia, continuous passive motion (CPM) and physiotherapy with immediate full weight bearing. All patients had a routine follow-up including a standardized clinical and radiological examination within the first year. We did not see any intraoperative fracture like island fracture of the intercondylar eminence. At 18 months postoperative, all patients completed a questionnaire consisting of the FJS, the EQ-5D, a visual analog scale (VAS), a functional assessment, a complication analysis, and a subjective rating by the patient. We collected all data prospectively. Primary outcome measure was the FJS 18 months postoperative.
Forgotten Joint Score (FJS)
The FJS score is a self-administrated questionnaire comprising 12 items concerning on the patient’s ability to forget the artificial joint in everyday life. The loss of awareness of an artificial joint is seen as the ultimate goal in arthroplasty of the knee. It is assumed that the ‘forgotten joint’ goes along with maximum patient satisfaction [5]. The “Forgotten Joint Score” was developed in 2012 and has shown a high internal consistency, construct validity and responsiveness later than 12 months postoperative after TKA [4, 5, 40, 42, 43]. The score is reported on a scale from 0 to 100, whereas 100 represents the best outcome indicating that the patient is not aware of the artificial joint in everyday life. Table 2 shows the questions included in the FJS.
Statistical analysis
Statistical analysis was performed using the software package SPSS (Version 23, SPSS Inc, Chicago, Illinois). Unless otherwise stated, descriptive data are given as mean ± standard deviation. The level of significance was at p < 0.05 for all tests.
Since there is no previous data on joint awareness in BCR-TKA, this preliminary study was designed as an exploratory pilot study without any a priori sample size calculation based on a primary endpoint. Based on the sample size in studies PRO after TKA 100 patients were considered feasible and expected to have enough power to discover clinically relevant differences between the groups.
For comparison of mean values of the FJS, we performed an analysis of variances (ANOVA). In the case of a significant effect, Tukey adjusted post hoc pairwise comparisons were calculated.
The Ethics Committee at the University of Regensburg approved the study in May 2014 (Institutional Review Board Number 14-101-0135). A written informed consent was obtained from every patient in accordance with the declaration of Helsinki.
Results
Table 1 shows demographic data recorded in 102 patients. The patient groups were comparable regarding preoperative medical condition (Table 3). The preoperative OKS was missing in three PS-patients, two UKA-patients, and one BCR-patient. Table 4 shows intraoperative data. In the BCR-group 5 patients had additional PFR and 4 of 34 patients in the PS-group had undergone PFR (Table 4). Nine BCR-patients had undergone lateral release of the patella, and 15 patients of the PS-group. Of course, none of these additional procedures were performed in the UKA-group. We did not see any intraoperative fracture of the intercondylar tibial eminence as described for BCR-TKA. There was one case of arthroscopic debridement 3 months postoperatively for a limited range of motion of 0–10–90° in the BCR-group. After debridement, she exhibited ROM of 0–0–110°. No other implantation-related complications (infection or loosening) occurred. One patient sustained a periprosthetic femur fracture Rorabeck type II [37] with a stable femoral component when she slipped on a sheet of ice 3 months after primary implantation. She received minimal invasive plate osteosynthesis.
Table 2 shows the raw score results for each question of the FJS for each group. We found differences mainly for activities like walking/hiking and stair climbing (Table 2). We investigated a possible impact of age, gender, and BMI for each question of the FJS. There was only a correlation between age and the FJS result of question 11 (hiking) and 12 (sports activity). There was no evidence for a correlation of age, gender, or BMI and all other questions or the total score result of the FJS. We found no difference between the FJS score in patients with or without PFR. One patient scored the minimum score of 0 and two patients scored a maximum of 100 points in the FJS. Therefore, relevant floor- or ceiling effects did not occur.
Table 5 shows the results for the FJS, the EQ-5D, and VAS for each of the three patient groups. We recorded a higher FJS for the BCR-group (p = 0.035) and the UKA-group (p = 0.031) compared to the PS-group (Table 5). Hence, the primary outcome measure was significantly different between the bicruciate-retaining implants (BCR and UKA) compared to the cruciate-sacrificing implant (PS).
Discussion
This is the first study to report on PRO after BCR-TKA finding a reduced joint awareness compared to a standard total knee arthroplasty sacrificing both cruciate ligaments.
There is a high proportion of patients who report residual knee symptoms after TKA without any objectifiable clinical or radiological reasons [7, 32]. There is an ongoing discussion about the value of preservation of cruciate ligaments in arthroplasty of the knee. Apart from the restoration of the natural kinematic behavior, the major reason for the development of bicruciate-retaining designs was the preservation of the nerve vessels in the anterior cruciate ligament, and as such a better proprioception. 18/102 patients included in this study were investigated in a proprioceptive analysis proving superior balance ability for bicruciate-retaining implants [3]. Besides that, there is some data showing superior proprioceptive capacity and improved knee kinematics after BCR-TKA compared to standard TKA [3, 10, 24, 30, 33, 34, 44]. Recently, Peersman et al. [33] showed that changes introduced to tibiofemoral kinematics by removal of the conforming meniscus and cartilage are of more impact than different inlay sizes and their combinations for a BCR TKA. However, they confirmed very close to normal knee kinematics for BCR-TKA. There are also studies supporting superior patient satisfaction after BCR-TKA. Cloutier et al. [11] were the first to develop a bicruciate-retaining total knee arthroplasty (BCR-TKA). He reported excellent clinical results with a survivorship rate of 95% after 10 years and 82% rate after 22 years [12, 38]. The largest long-term series of bicruciate-retaining total knee arthroplasty patients is presented by Pritchett [35]. He reported on 214 knees in 160 patients with a minimum follow-up of 20 years. The Kaplan–Meier survivorship was 89% (95% CI 82–93%) with revision for any reason as an endpoint. Despite these promising long-term results, the bicruciate-retaining implant design is not the current standard of care.
Generally, the implantation of a BCR-implant is a challenging procedure. Compared to a cruciate-sacrificing arthroplasty, anatomic positioning with a precise reconstruction of the joint line and ligamentous tension is even more important to achieve natural knee kinematics [1, 11, 20, 21, 26, 34, 35, 38, 44]. Furthermore, there are reports of intraoperative island fractures because implantation of BCR implants leaves only a narrow bony base for the insertion of the cruciate ligaments. Lombardi [26] reported a prospective multicenter study with early stage results (90 days postoperative) of 383 patients with a BCR-TKA. He found 11 cases of island fracture in the first 119 patients and only 5 cases in the following 264 patients. He interpreted this as a sign of a learning curve. In our study, only one surgeon performed all surgeries in a highly specialized setting. To date, we have seen no island fractures. We also reserve patella-femoral resurfacing (PFR) to cases of symptomatic severe patella-femoral degeneration. However, there is ongoing discussion about alteration of patella-femoral pressure with PFR [8].
In recent studies, the main argument supporting the use of bicruciate-retaining implants was a more natural feeling knee and an overall higher patient satisfaction [11, 18, 26, 30]. Unfortunately, none of these studies have given an objective parameter to substantiate this assumption. PRO has a rising influence in clinical decision-making. The concept of the “Forgotten Joint Score” (FJS) with rating the loss of awareness of the artificial knee joint as the ultimate goal is a new dimension in measuring the patient’s satisfaction [5]. The FJS has shown a high validity and reliability and good responsiveness in patients after TKA [4, 5, 40, 42, 43]. The FJS was originally developed for evaluation at least 12 months after implantation and has shown some limitations regarding responsiveness within the first year [4]. Several authors have investigated PRO during the first 2 years after TKA and found no relevant change later than 12 months postoperatively [16, 36, 43]. Accordingly, an evaluation 18 months postoperatively seems to be an appropriate time for measurement of PRO. One major advantage of the FJS is the absence of floor- or ceiling effects which is important to discern between good and excellent results. In our population, no relevant floor- or ceiling effects occurred.
Several studies have proven superior functional abilities and patient satisfaction for a UKA preserving both cruciate ligaments [15, 17, 19, 27,28,29]. However, the number of dissatisfied patients is a lot higher after TKA [7, 32]. We were aiming for high methodical quality when we designed this prospective, controlled trial. Therefore, we decided to investigate two control groups. A control group with a posterior cruciate-retaining implant would have been feasible. Since the PS-design is the gold standard in our institution we are most familiar with this type of implant making it reasonable to choose these patients as a control group. Additionally, recent literature shows no relevant difference between posterior cruciate-retaining and posterior stabilized implants concerning clinical or functional results [32, 33]. Recently, a study by Zuiderbaan [45] showed a 14 points difference in the FJS when comparing UKA to TKA 1.5 years after implantation. Although the total score in our patient population was lower compared to the results by Zuiderbaan, we also recorded a 14 points difference between UKA and standard TKA. However, the mean score in our BCR group was equal to the UKA-group in our population.
There is an ongoing discussion about the impact of demographic characteristics like age, gender, or BMI on the outcome after knee arthroplasty. Large registry studies using conventional outcome measurement tools could not confirm a relation between age, gender, or obesity and the postoperative outcome [2, 27]. There are also studies using the FJS which show that there is no correlation between baseline characteristics and the postoperative outcome [42, 43, 45]. Although we were not able to randomize the patients, preoperative data regarding deformity, KLS, and OKS were homogeneous which can be seen as a strength of this study. Recently, Li et al. [25] presented data on the preoperative FJS of people requiring TKA and indicated a correlation between the FJS and pre-operative age, gender and body mass index (BMI). However, we did not see any correlation between these parameters in our patient population.
This study has some limitations. Surely, the main limitation is the non-randomized design of the study. Since bicruciate-retaining arthroplasty is not yet a standard treatment option, a randomization would not have been conformable to ethical standards. Under these circumstances, it is difficult to assemble equally comprised patient groups. However, this reflects clinical reality. Additionally, the period of dates of surgery is unequal for the three groups. The recruitment period for the BCR group was longer due to logistic reasons. However, there was no specific patient selection and no other relevant change in treatment protocol except the choice of implant. The study focuses on measuring the PRO after arthroplasty. Further studies are needed to investigate if the preservation of the ACL or the physiologic knee kinematics or both are responsible for the patient’s improved perception of the joint. Therefore, we advocate for further randomized studies on the comparison of bicruciate-retaining and standard implants in knee osteoarthritis.
Conclusion
Our study is the first to compare PRO in BCR-TKA to UKA and standard TKA. We found a reduced joint awareness for BCR-TKA compared to a standard total knee arthroplasty. The score values of the BCR-group was equal to the UKA-group. Further studies are needed to investigate long-term survivorship of BCR-implants.
References
Amiri S, Wilson DR (2012) A computational modeling approach for investigating soft tissue balancing in bicruciate retaining knee arthroplasty. Comput Math Methods Med 2012:652865. https://doi.org/10.1155/2012/652865
Baker P, Petheram T, Jameson S, Reed M, Gregg P, Deehan D (2012) The association between body mass index and the outcomes of total knee arthroplasty. J Bone Jt Surg Am Vol 94(16):1501–1508. https://doi.org/10.2106/JBJS.K.01180
Baumann F, Bahadin O, Krutsch W, Zellner J, Nerlich M, Angele P, Tibesku CO (2016) Proprioception after bicruciate-retaining total knee arthroplasty is comparable to unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-016-4121-2
Baumann F, Ernstberger T, Loibl M, Zeman F, Nerlich M, Tibesku C (2016) Validation of the German Forgotten Joint Score (G-FJS) according to the COSMIN checklist: does a reduction in joint awareness indicate clinical improvement after arthroplasty of the knee? Arch Orthop Trauma Surg 136(2):257–264. https://doi.org/10.1007/s00402-015-2372-x
Behrend H, Giesinger K, Giesinger JM, Kuster MS (2012) The “forgotten joint” as the ultimate goal in joint arthroplasty: validation of a new patient-reported outcome measure. J Arthroplasty 27(3):430–436 e431. https://doi.org/10.1016/j.arth.2011.06.035
Berend KR, Berend ME, Dalury DF, Argenson JN, Dodd CA, Scott RD (2015) Consensus statement on indications and contraindications for medial unicompartmental knee arthroplasty. J Surg Orthop Adv 24(4):252–256
Bourne RB, Chesworth BM, Davis AM, Mahomed NN, Charron KD (2010) Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res 468(1):57–63. https://doi.org/10.1007/s11999-009-1119-9
Calliess T, Ettinger M, Schado S, Becher C, Hurschler C, Ostermeier S (2016) Patella tracking and patella contact pressure in modular patellofemoral arthroplasty: a biomechanical in vitro analysis. Arch Orthop Trauma Surg 136(6):849–855. https://doi.org/10.1007/s00402-016-2451-7
Cao S, Liu N, Han W, Zi Y, Peng F, Li L, Fu Q, Chen Y, Zheng W, Qian Q (2017) Simplified Chinese version of the Forgotten Joint Score (FJS) for patients who underwent joint arthroplasty: cross-cultural adaptation and validation. J Orthop Surg Res 12(1):6. https://doi.org/10.1186/s13018-016-0508-5
Cherian JJ, Kapadia BH, Banerjee S, Jauregui JJ, Harwin SF, Mont MA (2014) Bicruciate-retaining total knee arthroplasty: a review. J Knee Surg 27(3):199–205. https://doi.org/10.1055/s-0034-1374812
Cloutier JM (1983) Results of total knee arthroplasty with a non-constrained prosthesis. J Bone Jt Surg Am Vol 65(7):906–919
Cloutier JM, Sabouret P, Deghrar A (1999) Total knee arthroplasty with retention of both cruciate ligaments. A nine to eleven-year follow-up study. J Bone Jt Surg Am Vol 81(5):697–702
Collins NJ, Misra D, Felson DT, Crossley KM, Roos EM (2011) Measures of knee function: International Knee Documentation Committee (IKDC) Subjective Knee Evaluation Form, Knee Injury and Osteoarthritis Outcome Score (KOOS), Knee Injury and Osteoarthritis Outcome Score Physical Function Short Form (KOOS-PS), Knee Outcome Survey Activities of Daily Living Scale (KOS-ADL), Lysholm Knee Scoring Scale, Oxford Knee Score (OKS), Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC), Activity Rating Scale (ARS), and Tegner Activity Score (TAS). Arthritis Care Res 63(Suppl 11):S208-228. https://doi.org/10.1002/acr.20632
Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Jt Surg Br Vol 80(1):63–69
Ettinger M, Zoch JM, Becher C, Hurschler C, Stukenborg-Colsman C, Claassen L, Ostermeier S, Calliess T (2015) In vitro kinematics of fixed versus mobile bearing in unicondylar knee arthroplasty. Arch Orthop Trauma Surg 135(6):871–877. https://doi.org/10.1007/s00402-015-2214-x
Fitzgerald JD, Orav EJ, Lee TH, Marcantonio ER, Poss R, Goldman L, Mangione CM (2004) Patient quality of life during the 12 months following joint replacement surgery. Arthritis Rheum 51(1):100–109. https://doi.org/10.1002/art.20090
Fuchs S, Frisse D, Laass H, Thorwesten L, Tibesku CO (2004) Muscle strength in patients with unicompartmental arthroplasty. Am J Phys Med Rehabil Assoc Acad Phys 83(8):650–654 quiz 655–657, 662
Fuchs S, Frisse D, Tibesku CO, Laass H, Rosenbaum D (2002) Proprioceptive function, clinical results, and quality of life after unicondylar sledge prostheses. Am J Phys Med Rehabil Assoc Acad Physiatr 81(7):478–482
Fuchs S, Tibesku CO, Frisse D, Genkinger M, Laass H, Rosenbaum D (2005) Clinical and functional comparison of uni- and bicondylar sledge prostheses. Knee Surg Sports Traumatol Arthrosc 13(3):197–202. https://doi.org/10.1007/s00167-004-0580-y
Fuchs S, Tibesku CO, Genkinger M, Laass H, Rosenbaum D (2003) Proprioception with bicondylar sledge prostheses retaining cruciate ligaments. Clin Orthop Relat Res 406:148–154. https://doi.org/10.1097/01.blo.0000038053.29678.a5
Goutallier D, Manicom O, Van Driessche S (2008) Total knee arthroplasty with bicruciate preservation: comparison versus the same posterostabilized design at eight years follow-up. Revue de chirurgie orthopedique et reparatrice de l’appareil moteur 94(6):585–595. https://doi.org/10.1016/j.rco.2008.04.012
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the knee society clinical rating system. Clin Orthop Relat Res 248:13–14
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16(4):494–502
Komistek RD, Allain J, Anderson DT, Dennis DA, Goutallier D (2002) In vivo kinematics for subjects with and without an anterior cruciate ligament. Clin Orthop Relat Res 404:315–325
Li D, Troelsen A, Ingelsrud L, Husted H, Gromov K (2017) Females, younger patients and patients with high BMI have the highest pre-operative knee awareness measured using the Forgotten Joint Score. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4446-5
Lombardi AV (2015) THE BI-CRUCIATE RETAINING TKA: “A THING OF BEAUTY IS A JOY FOREVER”—AFFIRMS. Bone Jt J Orthop Proc Suppl 97-B(SUPP 1):69
Lygre SH, Espehaug B, Havelin LI, Furnes O, Vollset SE (2010) Pain and function in patients after primary unicompartmental and total knee arthroplasty. J Bone Jt Surg Am Vol 92(18):2890–2897. https://doi.org/10.2106/JBJS.I.00917
Lyons MC, MacDonald SJ, Somerville LE, Naudie DD, McCalden RW (2012) Unicompartmental versus total knee arthroplasty database analysis: is there a winner? Clin Orthop Relat Res 470(1):84–90. https://doi.org/10.1007/s11999-011-2144-z
Matthews DJ, Hossain FS, Patel S, Haddad FS (2013) A Cohort Study Predicts Better Functional Outcomes and Equivalent Patient Satisfaction Following UKR Compared with TKR. HSS J Musculoskelet J Hosp Special Surg 9(1):21–24. https://doi.org/10.1007/s11420-012-9326-4
Moro-oka TA, Muenchinger M, Canciani JP, Banks SA (2007) Comparing in vivo kinematics of anterior cruciate-retaining and posterior cruciate-retaining total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 15(1):93–99. doi:https://doi.org/10.1007/s00167-006-0134-6
Nielsen KA, Thomsen MG, Latifi R, Kallemose T, Husted H, Troelsen A (2016) Does post-operative knee awareness differ between knees in bilateral simultaneous total knee arthroplasty? Predictors of high or low knee awareness. Knee Surg Sports Traumatol Arthrosc 24(10):3352–3358. https://doi.org/10.1007/s00167-016-4013-5
Parvizi J, Nunley RM, Berend KR, Lombardi AV Jr, Ruh EL, Clohisy JC, Hamilton WG, Della Valle CJ, Barrack RL (2014) High level of residual symptoms in young patients after total knee arthroplasty. Clin Orthop Relat Res 472(1):133–137. https://doi.org/10.1007/s11999-013-3229-7
Peersman G, Slane J, Dirckx M, Vandevyver A, Dworschak P, Heyse TJ, Scheys L (2017) The influence of polyethylene bearing thickness on the tibiofemoral kinematics of a bicruciate retaining total knee arthroplasty. Knee 24(4):751–760. https://doi.org/10.1016/j.knee.2017.03.010
Pritchett JW (2011) Patients prefer a bicruciate-retaining or the medial pivot total knee prosthesis. J Arthroplasty 26(2):224–228. https://doi.org/10.1016/j.arth.2010.02.012
Pritchett JW (2015) Bicruciate-retaining total knee replacement provides satisfactory function and implant survivorship at 23 years. Clin Orthop Relat Res 473(7):2327–2333. https://doi.org/10.1007/s11999-015-4219-8
Pynsent PB, Adams DJ, Disney SP (2005) The Oxford hip and knee outcome questionnaires for arthroplasty. J Bone Jt Surg Br Vol 87(2):241–248
Rorabeck CH, Taylor JW (1999) Classification of periprosthetic fractures complicating total knee arthroplasty. Orthop Clin N Am 30(2):209–214
Sabouret P, Lavoie F, Cloutier JM (2013) Total knee replacement with retention of both cruciate ligaments: a 22-year follow-up study. Bone Jt J 95-B(7):917–922. https://doi.org/10.1302/0301-620X.95B7.30904
Schultz RA, Miller DC, Kerr CS, Micheli L (1984) Mechanoreceptors in human cruciate ligaments. A histological study. J Bone Jt Surg Am Vol 66(7):1072–1076
Shadid MB, Vinken NS, Marting LN, Wolterbeek N (2016) The Dutch version of the Forgotten Joint Score: test–retesting reliability and validation. Acta Orthop Belg 82(1):112–118
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 198:43–49
Thienpont E, Opsomer G, Koninckx A, Houssiau F (2014) Joint awareness in different types of knee arthroplasty evaluated with the Forgotten Joint score. J Arthroplasty 29(1):48–51. https://doi.org/10.1016/j.arth.2013.04.024
Thomsen MG, Latifi R, Kallemose T, Husted H, Troelsen A (2016) Does knee awareness differ between different knee arthroplasty prostheses? A matched, case-control, cross-sectional study. BMC Musculoskelet Disord 17:141. https://doi.org/10.1186/s12891-016-1001-3
Ward TR, Burns AW, Gillespie MJ, Scarvell JM, Smith PN (2011) Bicruciate-stabilised total knee replacements produce more normal sagittal plane kinematics than posterior-stabilised designs. J Bone Jt Surg Br Vol 93(7):907–913. https://doi.org/10.1302/0301-620X.93B7.26208
Zuiderbaan HA, van der List JP, Khamaisy S, Nawabi DH, Thein R, Ishmael C, Paul S, Pearle AD (2017) Unicompartmental knee arthroplasty versus total knee arthroplasty: Which type of artificial joint do patients forget? Knee Surg Sports Traumatol Arthrosc 3:681–686. https://doi.org/10.1007/s00167-015-3868-1
Acknowledgements
This study was supported by the European Knee Society.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Baumann, F., Krutsch, W., Worlicek, M. et al. Reduced joint-awareness in bicruciate-retaining total knee arthroplasty compared to cruciate-sacrificing total knee arthroplasty. Arch Orthop Trauma Surg 138, 273–279 (2018). https://doi.org/10.1007/s00402-017-2839-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-017-2839-z