Abstract
Introduction
The inability to visualize the sternum tip and T1 vertebra on radiographs may decrease the accuracy of the measurements of cervical sagittal parameters. The object of this study is to investigate the value of MRI to measure cervical sagittal parameters and to compare the data of cervical sagittal parameters on radiographs and MR images.
Materials and methods
Fifty-two asymptomatic adults were recruited. Each subject had both an MRI and radiographs of the cervical spine. Data, including C2–7 lordosis (CL), T1 slope (T1S), thoracic inlet angle (TIA), neck tilt (NT), and T1S minus C2–7 lordosis (T1S-CL), on radiographs and MRI were collected and analyzed.
Results
There were significant differences in CL, T1S, and T1S-CL, between X-ray and MR imaging, but not in TIA and NT. Each of the radiographic cervical sagittal parameters had a significant relationship with the corresponding value on MRI, and the correlation between radiographic and MRI measurement of TIA was the most significant of all parameters.
Conclusions
Positional change may significantly influence most sagittal parameters. Supine MRI cannot substitute for upright cervical radiographs to measure most cervical sagittal parameters except for TIA in an asymptomatic population.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Cervical sagittal parameters, especially thoracic inlet angle (TIA), neck tilt (NT), and T1 slope, have been considered previously as important factors influencing cervical sagittal balance. Lee et al. initially reported that the TI alignment significantly correlated with cervical sagittal balance. To preserve physiological NT around 44°, a large TIA increased T1 slope, and thereby cervical lordosis, and vice versa for smaller TIAs. TIA and T1 slope can be used as parameters to predict physiological alignment of the cervical spine [1–3]. Recently, several studies also showed that T1 slope minus C2–C7 lordosis, similar to PI-LL, significantly correlated with cervical sagittal alignment, the neck disability index (NDI), and patient-reported health-related quality-of-life (HRQOL) scores following cervical surgery [4, 5].
Although cervical sagittal parameters have shown their importance in cervical sagittal balance and predicting postoperative clinical outcomes, the inability to visualize the sternum tip and T1 vertebra on radiographs is a critical defect, preventing T1 slope, NT, and TIA from being clearly measured, and may decrease the accuracy of the measurements.
To overcome this defect of radiographs, we studied the cervical sagittal parameters of an asymptomatic population measured via cervical MRI, which can accurately demonstrate the sternum tip and T1 vertebra. To the best of our knowledge, this is the first study to investigate the value of MRI to measure cervical sagittal parameters of an asymptomatic population and the relationship of cervical sagittal parameters between cervical MRI and radiographical data. Two previous studies only focused on adolescent idiopathic scoliosis (AIS) patients and considered MRI as a reliable substitute for X-ray imaging in adolescent idiopathic scoliosis (AIS) patients; however, we found different results in asymptomatic population.
Materials and methods
One hundred asymptomatic adults who visited the outpatient department or physical examination center of our hospital between September 2013 and September 2015 were reviewed. Each individual had both an MRI and radiographs of the cervical spine. The study was approved by the Ethics Committee of our institution.
The inclusion criteria are as follows: (1) age ≥20 years; (2) no history of diagnosis or treatment related to any part of the spine, all of them underwent both MRI and cervical radiographs due to exclusion of the possibility of cervical spine disease and patients strongly claim; (3) no evidence of cervical deformity on radiographs. The exclusion criterion was as follows: T1 vertebral body and/or upper end of sternum were not clearly visible on lateral radiograph (obscured by overlapping soft and bony tissues). A total of 52 subjects met the study criteria and were included.
A standing lateral radiograph of the cervical spine was obtained with the subject in a neutral standing position, looking straight ahead. Cervical MRI was obtained with the subject in a comfortable supine position. The parameters, including T1 slope, TIA, neck tilt, and C2–C7 lordosis, were measured on the cervical radiograph and cervical MRI.
Cervical parameters
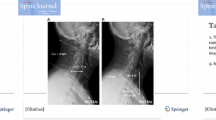
C2–7 lordosis (CL): the Cobb angle between the lower endplates of C2 and C7 (Fig. 1).
T1 slope (T1S): the angle between the upper endplate of T1 (T1UEP) and the horizontal (Fig. 1).
Thoracic inlet angle (TIA): an angle formed by a vertical line from the center of the T1UEP, and a line connecting the center of the T1UEP and the upper end of the sternum (Fig. 1).
Neck tilt (NT): an angle formed by a vertical line from the sternum tip and a line connecting the center of the T1UEP and the upper end of the sternum (Fig. 1).
T1S minus C2–7 lordosis (T1S-CL): the T1S angle minus the C2–7 lordosis.
The above acronyms followed by an ‘X’ denote X-ray imaging parameters, and followed by an ‘M’ denote MRI parameters, for example, CLX and CLM for C2-7 lordosis on X-ray and MR imaging, respectively.
Statistical analysis
All measurements were determined using the picture archiving and communication system in the hospital, both by a spine surgeon and a radiologist. Each reader evaluated each image twice at different time points and their average values were adopted. Quantitative data were analyzed using a paired t test, and the correlations between parameters of the cervical radiographs and MRI were analyzed using the Pearson correlation coefficient. Statistical analyses were performed using SPSS 22.0 (SPSS Inc., Chicago, IL, USA) and P < 0.05 was considered significant.
Results
Forty-five subjects of 100 subjects were excluded, because it was difficult to evaluate the sternum and T1 vertebral body accurately on X-ray imaging, and three subjects were excluded due to the absence of the sternum from the MR image. A total of 52 subjects were included. There were 27 male and 25 female subjects, with a mean age of 32.3 ± 8.9 years.
Comparison of the cervical sagittal parameter measurements on MR and X-ray imaging yielded significant differences in CL, T1S, and T1S-CL. The mean radiographic CL was significantly greater than that on MRI (19.1°± 12.0° versus 3.3°± 9.8°, P < 0.01), the mean radiographic T1S was significantly greater than on MRI (25.7°± 5.0° versus 22.6°± 6.4°, P < 0.01) while the mean radiographic T1S-CL was significantly lower than on MRI (6.6°± 9.9° versus 19.3°± 8.3°, P < 0.01). The difference between the means of CLX and CLM (CLX − CLM), T1SX and T1SM (T1SX − T1SM), and T1S-CLX and T1S-CLM (T1S-CLX − T1S-CLM), was 15.9°± 12.2°, 3.1°± 6.5°, and −12.7°± 10.5°, respectively. There was no significant difference in TIA and NT between X-ray and MR imaging (Table 1).
Each of the radiographic cervical sagittal parameters had a significant relationship with that of MRI. The Pearson correlation coefficient of CLX and CLM, TIAX and TIAM, T1SX and T1SM, NTX and NTM, T1S-CLX, and T1S-CLM, was 0.387, 0.563, 0.367, 0.357, and 0.307, respectively. There were also significant correlations with other parameters. CLX significantly correlated with TIAX, T1SX, T1S-CLX, and T1S-CLM (r = 0.299, 0.591, −0.913, −0.278, respectively). TIAX significantly correlated with T1SX, NTX, CLM, T1SM, and NTM (r = 0.476, 0.684, 0.377, 0.305, 0.330, respectively). T1SX significantly correlated with TIAX, NTX, and TIAM (r = 0.476, −0.313, 0.280, respectively). NTX significantly correlated with TIAX, T1SX, and TIAM (r = 0.684, -0.313, 0.370, respectively). T1S-CLX significantly correlated with CLX and CLM (r = −0.913, −0.361, respectively). Parameters on MRI, similar to those on X-ray imaging, also had significant correlations with others (Table 2).
Discussion
In the previous studies, cervical sagittal parameter showed promise for similar relationships to be found in the lumbar spine. TIA, T1S, and NT were considered as critical parameters that account for cervical sagittal balance. A cervical balance mechanism in an asymptomatic population was confirmed, whereby a larger TIA increases T1S and subsequently increases CL, to obtain a horizontal gaze and sagittal alignment of cervical spine with minimum energy expenditure [1]. Furthermore, increasing values of T1S had been correlated with worse outcomes after posterior cervical surgery and T1S-CL was also found to significantly correlate with HRQOL scores following cervical surgery [6].
However, the previous studies based on unclear cervical X-ray radiographs could not accurately measure TIA, T1S, and NT due to the invisible sternum tip and T1 vertebra [7]. In this study, a similar issue was encountered. Nearly half of the subjects (45 of 100) were excluded due to difficulty measuring accurately. We initially compared MRI cervical sagittal parameters in an asymptomatic population with the data measured on X-ray images. The purpose of this study was to investigate the capability to analyze cervical sagittal parameters via MRI. The merit of MRI was that we could easily visualize the sternum tip and T1 vertebra and accurately measure cervical sagittal parameters. However, as cervical X-ray was obtained with the subject in a neutral standing position, while cervical MRI was obtained with the subject in a supine position, several parameters significantly changed, probably because of positioning [8, 9]. The mean T1S and CL on X-ray imaging were significantly greater than on MRI, while the mean T1S-CL was significantly lower. TIA did not change significantly in different positions (70.2 ± 6.6 versus 68.9 ± 8.5, P = 0.236).
Since the balance of the cervical spine is acquired in an upright position during a human’s daily life, parameters derived from a supine MRI might not suitable for assessing this directly. However, the capability of MRI to evaluate cervical sagittal balance is still of interest. In this study, we found the similar correlation of parameters on both X-ray and MR images, and that a large TIA led to a large T1S, and large CL (Fig. 1). Meanwhile, each of the radiographic cervical sagittal parameters had a significant correlation with that on MRI. We wondered whether parameters on MRI could substitute for those on radiographs in instances where it was difficult to determine the location of the sternum tip and T1 vertebra. Therefore, we analyzed a linear regression model of cervical sagittal parameters derived from MR and X-ray imaging (Fig. 2). There was a significant correlation in TIA between radiographs and MRI (r = 0.563); however, no obvious correlations were found in other parameters. Cervical sagittal parameters might be influenced by different positions. As a result, the value of T1S, CL, and T1S-CL showed significant differences and no obvious correlation between the two imaging modalities. Although NT showed no significant difference between modalities, and was not influenced by positional change as a previous study reported [10], the correlation was not as significant as that of TIA (r = 0.367 versus 0.563). We could not apply MRI as a substitute to measure any of the parameters except TIA. The value of TIA on MRI was not identical to that on X-ray images, and the correlation (r = 0.563) between MRI and radiographs was not as high as expected, similar to the result on supine CT [9], indicating that it might not be considered as constant a morphological parameter as previously reported [10], we suggest that MRI should be used for measuring TIA only if the sternum tip and T1 vertebra were not evident on the lateral radiograph. We also noticed some other studies consider MRI as a reliable substitute for X-ray imaging, since no significant difference was noted in terms of TIA, T1S, NT, and the sagittal alignment of the upper thoracic spine [11, 12]; however, subjects in those studies were adolescent idiopathic scoliosis (AIS) patients with a deformative, rigid, and activity-restricted spine, and therefore, positional change might not significantly affect the data of cervical sagittal parameters and the result was not applicable to an asymptomatic population with a normal spine.
Conclusion
In this study, we initially investigated the value of MRI to measure cervical sagittal parameters in an asymptomatic population via comparison to the data measured on radiographs. TIA was the only cervical sagittal parameter that showed no significant differences and a significant correlation between X-ray and MR imaging. Our results indicate that supine MRI cannot substitute for upright radiographs to measure most cervical parameters, except TIA, in an asymptomatic population. We suggest that MRI supersedes for measuring TIA only if the sternum tip and T1 vertebra are not visible on radiographs.
References
Lee SH, Kim KT, Seo EM, Suk KS, Kwack YH, Son ES (2012) The influence of thoracic inlet alignment on the craniocervical sagittal balance in asymptomatic adults. Clin Spine Surg 25(2):E41–E47
Lee SH, Son ES, Seo EM, Suk KS, Kim KT (2015) Factors determining cervical spine sagittal balance in asymptomatic adults: correlation with spinopelvic balance and thoracic inlet alignment. Spine J 15(4):705–712
Knott PT, Mardjetko SM, Techy F (2010) The use of the T1 sagittal angle in predicting overall sagittal balance of the spine. Spine J 10(11):994–998
Iyer S, Nemani VM, Nguyen J, Elysee J, Burapachaisri A, Ames CP, Kim HJ (2016) Impact of cervical sagittal alignment parameters on neck disability. Spine 41(5):371–377
Hyun SJ, Kim KJ, Jahng TA, Kim HJ (2016) Relationship between T1 slope and cervical alignment following multilevel posterior cervical fusion surgery: impact of T1 slope minus cervical lordosis. Spine 41(7):E396–E402
Kim TH, Lee SY, Kim YC, Park MS, Kim SW (2013) T1 slope as a predictor of kyphotic alignment change after laminoplasty in patients with cervical myelopathy. Spine 38(16):E992–E997
Jang J, J. S, Lee SH, Min JH, Kim SK, Han KM, Maeng DH (2007) Surgical treatment of failed back surgery syndrome due to sagittal imbalance. Spine 32(26):3081–3087
Park SM, Song KS, Park SH, Kang H, Riew KD (2015) Does whole-spine lateral radiograph with clavicle positioning reflect the correct cervical sagittal alignment? Eur Spine J 24(1):57–62
Jun HS, Chang IB, Song JH, Kim TH, Park MS, Kim SW, Oh JK (2014) Is it possible to evaluate the parameters of cervical sagittal alignment on cervical computed tomographic scans? Spine 39(10):E630–E636
Janusz P, Tyrakowski M, Glowka P, Offoha R, Siemionow K (2015) Influence of cervical spine position on the radiographic parameters of the thoracic inlet alignment. Eur Spine J 24(12):2880–2884
Wang F, Sun X, Mao S, Liu Z, Qiao J, Zhu F, Qiu Y et al (2013) MR imaging may serve as a valid alternative to standing radiography in evaluating the sagittal alignment of the upper thoracic spine. J Spinal Disord Tech 11:582–585
Qiao J, Zhu F, Liu Z, Xu L, Zhu Z, Qian B, Qiu Y et al (2015) Measurement of thoracic inlet alignment on MRI: reliability and the influence of body position. J Spinal Disord Techn. doi:10.1097/BSD.0000000000000306
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
This work was sponsored by the Natural Science Foundation of China (81372002, 31170925) and a research grant from the Shanghai Hospital Development Center (SHDC12014102).
Ethical approval
The study was approved by the Ethics Committee of Zhongshan Hospital Fudan University. The manuscript submitted does not contain information about medical device(s)/drug(s).
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xing, R., Zhou, G., Chen, Q. et al. MRI to measure cervical sagittal parameters: a comparison with plain radiographs. Arch Orthop Trauma Surg 137, 451–455 (2017). https://doi.org/10.1007/s00402-017-2639-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-017-2639-5