Abstract
Purpose
To evaluate the differences of cervical alignment between standing cervical lateral radiograph and whole-spine lateral radiograph with clavicle position.
Methods
We prospectively evaluated 101 asymptomatic adults from whom standing cervical lateral radiograph with hands on both side followed by whole-spine lateral radiographs with clavicle position were obtained from April 2012 to December 2013. On two radiographs, cervical sagittal alignment from C2 to C7 was analyzed by Gore angle (GA) and Cobb angle (CA); head position was evaluated using the translation distance (TD, distance of the anterior tubercle of C1 compared with the vertical line through the posterior-inferior body of C7) and McGregor angle (MA, angle between the McGregor and horizontal lines). T1-slope was also evaluated.
Results
Cervical alignment on the cervical radiograph (GA −13.59° [−15.58 to −11.60], CA −9.76° [−11.65 to −7.86]) was significantly more lordotic than that on whole-spine radiographs (GA −6.28° [−8.65 to −3.91] and −4.14° [−6.40 to −1.89]). TD and MA on cervical radiographs (TD 34.98 mm [33.22–36.75]; MA 7.20° [6.35–8.35]) were meaningfully higher than those on whole-spine radiographs (TD 31.31 mm [29.47–33.16]; MA 6.32° [5.25–7.39]), but the MA values were not significant (p = 0.064). T1-slope was significantly lower in whole-spine radiographs (20.11° [18.88–21.35]) than in cervical radiographs (24.37° [23.14–25.6]). Values are expressed as mean (95 % confidence interval).
Conclusions
Clavicle position during whole-spine radiograph caused a substantial decrease in the T1-slope; head position posteriorly translated followed by the cervical sagittal alignment became more hypo-lordotic, with slight downward gazing in comparison with the cervical radiograph.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The whole-spine lateral radiograph is a key image to evaluate global sagittal spinal alignment. While the radiograph is being taken, a relaxed standing position with the arms on either side of the body is the optimal posture to evaluate global spinal sagittal alignment [1]. However, the presence of the arms on either side of the body obstructs proper radiographic visualization of thoracic and lumbar spine [1, 2]. Therefore, variable flexed arm positions for taking the radiograph have been suggested, and such positions could influence the sagittal vertical axis and some studies have reported the effects of the radiographic postures on thoracic and lumbar spine alignments [1–5]. However, there has been much less information about the cervical alignment on whole-spine lateral radiographs [2, 6, 7], whereas most of the studies on cervical sagittal alignment have used the cervical lateral radiograph with the patient in the relaxed standing position [8–11].
To the best of our knowledge, no study has demonstrated the differences in cervical alignment between a standing cervical lateral radiograph and a whole-spine lateral radiograph and investigated the significance of cervical alignment on a whole-spine lateral radiograph. Therefore, we hypothesized that the clavicle position while a whole-spine lateral radiograph is taken could affect cervical alignment more than an extended arm and hand position on both sides during a standing cervical lateral radiograph, and we evaluated the differences in cervical alignments between the two radiographs in a subject prospectively.
Materials and methods
This study protocol was approved by the Institutional Review Board, and informed consent was obtained from each subject who agreed to participate in the study. We prospectively evaluated 112 normal volunteers from whom standing cervical lateral radiographs followed by standing whole-spine lateral radiographs were obtained from April 2012 to December 2013. Among the volunteers, three had sigmoid curvature of the cervical spine and four had thoracic scoliosis more than 10° of the Cobb angle. Four volunteers had incomplete radiographs. Therefore, 101 volunteers were included in our study.
Radiographic postures
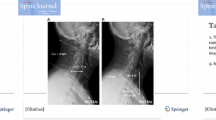
First, cervical lateral radiograph was taken with the head in a comfortable resting position with a horizontal gaze while the volunteers were standing with the arms extended and hands on either side. The tube was centered on the central line pointed to C4 (Fig. 1a). Subsequently, whole-spine lateral radiograph was acquired with the same patient in the most stable and relaxed position; volunteer stood with the knees locked and feet shoulder-width apart. In addition, the volunteer was looking straight ahead with their elbows bent, wrists flexed, and hands relaxed with the fingers in the supraclavicular fossa [2]. This positioning places the volunteers’ arms at approximately a 30° angle to the vertical axis of body. The tube was centered on the level of the center of the xiphoid process (Fig. 1b). The tube-to-subject distances in both radiographs were 182.9 cm.
Measured parameters
To evaluate cervical sagittal alignment from C2 to C7, the Gore angle (GA) [12, 13] and the Cobb angle (CA) [14] were measured. The GA is the angle between two lines drawn at the C2 and C7 posterior body margins, and CA is defined as the angle between two lines on inferior endplates of C2 and C7 that are extended until they intersect. The positive value indicates kyphotic alignment, whereas the negative value means lordotic alignment. The translation distance (TD) is defined as the distance from the anterior tubercle of C1 to the vertical lines passing through the posteroinferior body corner of C7 to evaluate the anteroposterior translation of the head position [15]. The McGregor line angle (MA) is defined as the angle between McGregor line that is drawn from the posterosuperior edge of the hard palate to the most caudal point of the occipital curve and the horizontal line to investigate superoinferior head tilting. Superior head tilting relative to the horizontal line was defined as a positive value. T1-slope, which is the angle between a horizontal line and a line parallel to the superior endplate of T1, was also evaluated (Fig. 2) [16, 17]. All parameters were independently measured by two orthopedic surgeons (with 2 and 3 years of experience) on a computer monitor with a diagonal length of 68.58 cm, showing the cervical lateral radiograph and magnified cervical spine portion of the whole-spine lateral radiograph, which was similar in size to the cervical lateral radiograph, measured using PACS (Picture Archiving and Communications System; General Electric, Chicago, IL, USA).
Measurements of cervical parameters on a cervical lateral radiograph (a) and magnified cervical spine of a whole-spine lateral radiograph (b). The cervical sagittal alignment of C2–7 using the Gore and Cobb methods, translation distance of C1–7, McGregor angle, and T1-slope were evaluated in one computer monitor with a diagonal length of 68.58 cm
Statistics
Statistical analysis was performed using SPSS version 18.0 (IBM Corp., Armonk, NY, USA). First, the distribution of the collected data was evaluated for normality using the Shapiro–Wilk test. Because all the variables were normally distributed, data were analyzed using a paired t test. The interobserver reliability of the measurements was evaluated using interclass correlation coefficients (ICCs) and 95 % confidence interval (95 % CI). A p value less than 0.05 was considered statistically significant.
Results
Fifty males and fifty-one females were included in the study, and the average age of the patients was 29.1 years (range 22–52 years). The subjects’ mean body mass index (BMI) was 22.3 kg/m2 (range 15.7–31.5 kg/m2). The ICC values of all measurements for the interobserver reliability in both radiographs were all in excellent range (Table 1).
Cervical alignment between two radiographs (Table 1)
The mean values of GA and CA on the cervical radiograph were −13.59° (95 % CI −15.58 to −11.60) and −9.76° (95 % CI −11.65 to −7.86), and −6.28° (95 % CI −8.65 to −3.91) and −4.14° (95 % CI −6.40 to −1.89) on the whole-spine radiograph. These values indicated that the cervical radiograph showed substantially lordotic cervical alignment compared with the whole-spine radiograph (GA p < 0.001; CA p < 0.001) (Fig. 3a, b).
Head position and T1-slope between two radiographs (Table 1)
The mean values of TD were 34.98 mm (95 % CI 33.22–36.75) on the cervical radiograph and 31.31 mm (95 % CI 29.47–33.16) on the whole-spine radiograph. The value was significantly lower on the whole-spine radiograph (p < 0.001) (Fig. 3c). This means that the head position on the whole-spine radiograph was substantially translated posteriorly than on the cervical radiograph. The MA (mean 7.20°; 95 % CI 6.35–8.35) in the cervical radiograph showed a higher angle than the value (mean 6.32°; 95 % CI 5.25–7.39) in the whole-spine radiograph, but the difference was not statistically significant (p = 0.064) (Fig. 3d). This finding demonstrates that the head position on the whole-spine radiograph had a tendency toward more inferior tilted gazing than the head position on the cervical radiograph. T1-slope was significantly lower in the whole-spine radiograph (mean 20.11°; 95 % CI 18.88–21.35) than in the cervical radiograph (mean 24.37°; 95 % CI 23.14–25.60) (Fig. 3e).
Discussion
Using the whole-spine lateral radiograph to evaluate global sagittal alignment, the effects of different arm positions for better visualization of the thoracic and the lumbar spine on sagittal alignment have been widely examined [1–5, 18]. Among the arm positions while the radiograph is obtained, the clavicle position has been considered superior to other positions for better visualization of T2, T12, and overall rating without external support, which may affect sagittal alignment [2, 4]. However, there has been no study to evaluate the effects of the clavicle position on the whole-spine lateral radiograph for cervical alignment.
In our prospective cohort study, the clavicle position during whole-spine radiograph resulted in a substantially decreased T1-slope, posteriorly translated head position, and hypo-lordotic or kyphotic cervical alignment compared with the standing cervical lateral radiograph with arms extended and hands on either side. The MA to estimate the degree of superoinferior tilting of horizontal gaze had a tendency toward a value that was lower in the whole-spine radiograph (p = 0.064). Such like findings could be expected by the following sequences. The clavicle position while the whole-spine radiograph was obtained caused extended thoracic inlet (decreased T1-slope and head position posteriorly translated), then cervical sagittal alignment was changed into hypo-lordotic or kyphotic alignment to compensate for the gravity line and sustain horizontal gaze in the standing radiographic posture (Fig. 4). Although it was not statistically significant, some inferior tilted gazing was observed on the whole-spine radiograph for compensation of extended thoracic inlet to maintain horizontal gaze.
The schematic figure demonstrates the effects of clavicle position on the changes of parameters. The clavicle position results in decreased T1-slope and translation distance, which means thoracic inlet is extended and head position is translated posteriorly, followed by secondary cervical kyphosis occurs
The aforementioned findings could also be expected by the results of previous reports [1–5], demonstrating that these whole-spine lateral radiographic postures with arms forward-flexed or in the clavicle position could theoretically result in posterior shift of the sagittal vertical axis to counterbalance the lever arm because of an increase in lumbar lordosis, decreased thoracic kyphosis, and posteriorly shifted thoracic spine. Considering effects of the radiographic postures, the decreased T1-slope and posteriorly translated head position followed by secondary cervical kyphotic change to balance the head over the trunk can also be expected.
A relaxed standing posture with the arms on either side of the body is a functional and easily assumed position during a cervical standing lateral radiograph. Aota et al. [3] demonstrated that both the fist-on-clavicles and arms forward-flexion positions produced substantial negative shift of the sagittal vertical axis than did the relaxed standing posture. Horton et al. [2] reported there were no significant differences of cervical alignment among whole-spine radiographs taken at 60°, 90° arms-flexed, and the clavicle position. Therefore, the same secondary cervical kyphotic change could be expected in other arm-flexed positions, even if they were not included in this study.
In previous reports on cervical alignment of asymptomatic subjects on cervical lateral radiographs from relaxed subjects standing and facing forward, Yukawa et al. [8] reported a mean Cobb angle of C2–7 that was −13.9° ± 12.3° in 1,230 asymptomatic volunteers, and Gore et al. [13] reported the mean Gore angle of C2–7 was −21.2° ± 14.6° in 200 asymptomatic subjects. These mean values demonstrate slight lordotic alignment compared to our values [19] (Table 2). Park et al. [6] measured cervical sagittal alignment on a whole-spine lateral radiograph with the arms in clavicle position to determine age-related changes in cervical alignment. In their study, as the head pitches forward (a more positive sagittal vertical axis), cervical alignment became more lordotic for horizontal gazing and T1-slope decreased to allow for compensatory cervical lordosis. In contrast, with a more negative sagittal vertical axis of the clavicle position while taking a whole-spine radiograph, T1-slope was decreased, which means that thoracic inlet was extended. The cervical alignment appeared to be hypo-lordotic or kyphotic to maintain horizontal gazing, and our findings are consistent with the results of Knott et al. [20] which show that more positive sagittal balance was associated with greater T1-slope, as demonstrated in Fig. 4.
Conclusion
Our results showed the clavicle position, first, causes substantial decrease in T1-slope and posterior translation of head position and then, the secondary compensation of cervical spine, which allows the widest regional range of motion, occurs to maintain horizontal gaze. The cervical sagittal alignment becomes substantially more hypo-lordotic or kyphotic, and slightly inferior gazing can occur. Therefore, in evaluating cervical alignment on a whole-spine lateral radiograph with clavicle position, the alignment is not true sagittal alignment but compensatory alignment and it could not be data expressing normative cervical alignment [6, 7]. The true cervical sagittal alignment should be evaluated in cervical lateral radiograph with the subject in a neutral relaxed position.
References
Marks MC, Stanford CF, Mahar AT, Newton PO (2003) Standing lateral radiographic positioning does not represent customary standing balance. Spine 28:1176–1182
Horton WC, Brown CW, Bridwell KH, Glassman SD, Suk SI, Cha CW (2005) Is there an optimal patient stance for obtaining a lateral 36″ radiograph? A critical comparison of three techniques. Spine 30:427–433
Aota Y, Saito T, Uesugi M, Ishida K, Shinoda K, Mizuma K (2009) Does the fists-on-clavicles position represent a functional standing position? Spine 34:808–812
Faro FD, Marks MC, Pawelek J, Newton PO (2004) Evaluation of a functional position for lateral radiograph acquisition in adolescent idiopathic scoliosis. Spine 29:2284–2289
Vedantam R, Lenke LG, Bridwell KH, Linville DL, Blanke K (2000) The effect of variation in arm position on sagittal spinal alignment. Spine 25:2204–2209
Park MS, Moon SH, Lee HM, Kim SW, Kim TH, Lee SY, Riew KD (2013) The effect of age on cervical sagittal alignment: normative data on 100 asymptomatic subjects. Spine 38:E458–E463
Lee CS, Noh H, Lee DH, Hwang CJ, Kim H, Cho SK (2012) Analysis of sagittal spinal alignment in 181 asymptomatic children. J Spinal Disord Tech 25:E259–E263
Yukawa Y, Kato F, Suda K, Yamagata M, Ueta T (2012) Age-related changes in osseous anatomy, alignment, and range of motion of the cervical spine. Part I: radiographic data from over 1,200 asymptomatic subjects. Eur Spine J 21:1492–1498
Nojiri K, Matsumoto M, Chiba K, Maruiwa H, Nakamura M, Nishizawa T, Toyama Y (2003) Relationship between alignment of upper and lower cervical spine in asymptomatic individuals. J Neurosurg 99:80–83
Villavicencio AT, Babuska JM, Ashton A, Busch E, Roeca C, Nelson EL, Mason A, Burneikiene S (2011) Prospective, randomized, double-blind clinical study evaluating the correlation of clinical outcomes and cervical sagittal alignment. Neurosurgery 68:1309–1316
Silber JS, Lipetz JS, Hayes VM, Lonner BS (2004) Measurement variability in the assessment of sagittal alignment of the cervical spine: a comparison of the gore and cobb methods. J Spinal Disord Tech 17:301–305
Scheer JK, Tang JA, Smith JS, Acosta FL Jr, Protopsaltis TS, Blondel B, Bess S, Shaffrey CI, Deviren V, Lafage V, Schwab F, Ames CP (2013) Cervical spine alignment, sagittal deformity, and clinical implications. J Neurosurg Spine 19:141–159
Gore DR, Sepic SB, Gardner GM (1986) Roentgenographic findings of the cervical spine in asymptomatic people. Spine 11:521–524
Cobb JR (1948) Outline for the study of scoliosis. Instr Course Lect 5:261–275
Harrison DE, Harrison DD, Cailliet R, Troyanovich SJ, Janik TJ, Holland B (2000) Cobb method or Harrison posterior tangent method: which to choose for lateral cervical radiographic analysis. Spine 25:2072–2078
Armijo-Olivo S, Jara X, Castillo N, Alfonso L, Schilling A, Valenzuela E, Frugone R, Magee D (2006) A comparison of the head and cervical posture between the self-balanced position and the Frankfurt method. J Oral Rehabil 33:194–201
Rocabado M (1983) Biomechanical relationship of the cranial, cervical, and hyoid regions. J Craniomandibular Pract 1:61–66
Suzuki H, Endo K, Mizuochi J, Kobayashi H, Tanaka H, Yamamoto K (2010) Clasped position for measurement of sagittal spinal alignment. Eur Spine J 19:782–786
Ct Kuntz, Levin LS, Ondra SL, Shaffrey CI, Morgan CJ (2007) Neutral upright sagittal spinal alignment from the occiput to the pelvis in asymptomatic adults: a review and resynthesis of the literature. J Neurosurg Spine 6:104–112
Knott PT, Mardjetko SM, Techy F (2010) The use of the T1 sagittal angle in predicting overall sagittal balance of the spine. Spine J 10:994–998
Acknowledgments
This study was approved by Institutional Review Board in Chung-Ang University in Seoul, Korea of Republic (C2012039(734)).
Conflict of interest
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (2013R1A1A2009322).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Park, SM., Song, KS., Park, SH. et al. Does whole-spine lateral radiograph with clavicle positioning reflect the correct cervical sagittal alignment?. Eur Spine J 24, 57–62 (2015). https://doi.org/10.1007/s00586-014-3525-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3525-2