Abstract
Introduction
We describe an extra-articular, extra-rotator cuff entry point for antegrade humeral nailing, which preserves the articular surface and rotator cuff integrity.
Material and methods
Thirty-two patients with humeral shaft fractures underwent antegrade intramedullary nailing using a modified insertion point located 1 cm below the crest of the greater tuberosity, in a region outside the articular surface and rotator cuff area.
Results
In all cases, nailing was done successfully, without any perforation of the humeral inner cortex by the nail. Extension of the fracture line to the distal metaphysis happened intraoperatively in one case of a distal diaphysis fracture. In the remainder of the patients, postoperative reduction of the fracture was successful, with no sign of an iatrogenic incident of fracture comminution. Excellent active shoulder function and full early functional recovery of the shoulder joint (to 16th week postoperatively) were established in 98% of the patients. All fractures were united in a mean period of 14 weeks.
Conclusion
We suggest an extra-articular, extra-rotator cuff entry point for antegrade humeral nailing as a possible and safe technique with beneficial results for the shoulder’s postoperative function.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Intramedullary nailing for humeral shaft fractures has been recently established as a reliable method of fixation when surgical intervention is needed [3, 5, 9, 11, 14]. The most common technical modalities include antegrade nail insertion at a point medial to the greater tuberosity, through the rotator cuff, and retrograde application of the nail proximal to the olecranon fossa, both combined by interlocking screw fixation to ensure tortional stability. Although there are few reports evaluating the retrograde technique, the complication of a distal humerus fracture around the site of nail insertion is always possible and has recently been reported [13, 16, 17, 19]. On the other hand, the potential compromise of rotator cuff function after the typical intra-articular insertion of antegrade nailing is currently under consideration. Analyzing the functional results of recent reports, it seems that there is a higher incidence of shoulder pain, impingement, and limitation of shoulder joint function after antegrade nail insertion [1, 7, 8, 13, 18]. Antegrade nail insertion predisposes opening of the intramedullary canal at the proximal end of the humerus through the rotator cuff and joint surface, creating problems for the function of the joint like pain and/or stiffness, as well as lengthening the rehabilitation period, leading to unsatisfactory results, despite the solid fusion at the fracture side. Considering these significant complications, we proposed an alternative technique using an extra-articular and extra-rotator cuff entry point of the nail, located 1 cm bellow the crest of the greater tuberosity, which preserves the articular surface and the rotator cuff.
Patients and methods
Thirty-two patients (18 male and 14 female, mean age 45.3 years) with humeral shaft fractures underwent antegrade intramedullary nailing according to the proposed modified technique in a 12-year period (1990–2002) in our department. According to the AO classification, there were 13 type A fractures, 11 type B, and 5 type C. Three fractures were pathologic. Fourteen were located at the mid-diaphysis, 10 extended to the proximal third of the diaphysis, and 5 to the distal third. Open reduction was necessary in 10 cases.
The Russell–Taylor humeral nail (Smith and Nephew, Richards) was used in all patients. For antegrade nail insertion, the patient is placed in a semi-sited position on a radiolucent table. C-arm image intensifier control was used in all cases. With the patient under general anesthesia, a standard longitudinal skin incision (3–5 cm) from the most lateral point of the acromion is used, centered over the tip of the greater tuberosity. Incision of the fascia, longitudinal splitting of the deltoid, and palpation of the greater tuberosity are the next steps. With the small curved awl, the entry portal site is established 1 cm below the tip of the greater tuberosity, just under the insertion of the rotator cuff (Fig. 1). Advancement of the curved awl is confirmed under image intensification, with both anteroposterior and lateral views to ensure that the nail will be in the midplane of the humerus.
Withdrawal of the curved awl is followed by the 2.4-mm, ball-tipped reamer guide rod insertion, which advanced down to the medullary canal at about 1–2 cm proximal to the olecranon fossa; the correct placement is confirmed again by image intensification. Proper nail length is verified with the guide rod method; with the distal end of the rod 1–2 cm proximal to the olecranon fossa; a second guide rod of equal length is overlapped, extending proximally from the humeral entry portal. Subtracting the length (in millimeters) of the overlapped guide rod from the total length, one can accurately determine the correct length of the nail. The proximal metaphysis of the humerus, including the entry point, is reamed thereafter to a diameter of 10 mm, for approximately 4 cm, to enlarge the proximal medullary canal (Fig. 2).
With the guide rod in place, the nail (diameter 7–8 mm) is gently advanced over it to the fracture, with the least possible angle between the nail’s axis and diaphysis axis, in order to avoid penetration of the inner cortex of the humerus on the site opposite to the entry point (Fig. 3). Confirmation of fracture reduction by image identification is always necessary in this step, followed by gentle passage of the nail to the distal fragment and removal of the guide rod. The nail is impacted 1–2 cm proximal to the olecranon fossa, at the cone-shaped diaphyseal flute of the distal humerus, ensuring rotational stability distally to the fracture area, and no distal locking screws are used. Finally, the nail is proximally locked with one 4-mm locking screw, using the proximal drill guide, which allows adjustment of the screw angle to 20 deg to obtain the best purchase in the cortical bone of the medial humeral metaphysis (Fig. 4).
Passive shoulder and elbow mobilization were started on the 2nd postoperative day, followed by active assisted mobilization (2nd to 4th postoperative week) and muscular strengthening (after 4th postoperative week).
Results
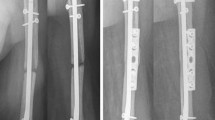
The mean follow-up period was 32 months (minimum 12 months). The outcome was evaluated according to the Constant-Murley shoulder scoring system, Mayo Elbow Score, clinical documentation at the fracture area, and radiological representation. Three patients with pathological fractures were lost before the last follow-up evaluation. The remaining 29 fractures were united between the 2nd and 4th postoperative months, in a mean period of 14 weeks (range 12–20 weeks), without any need of further surgical intervention (Fig. 5). In one case of an AO type C fracture of the distal diaphysis, an extension of the fracture line to the distal metaphysis was detected after nail insertion, and a Sarmiento cast was applied for 4 weeks. In the other cases, no tortional or rotational instability, fracture displacement, or loss of distal impaction was found, even if the fracture line extended to the distal part of the shaft (Fig. 6). There were two postoperative radial nerve palsies, which fully recovered after 3 and 4 months postoperatively. There were no cases of deep infection, implant failure, or proximal nail migration. Assessment of shoulder function using the Constant-Murley score was performed at the 2nd, 4th, 8th and 16th postoperative week (Table 1). Full passive range of shoulder motion was achieved in all patients between the 2nd and 4th postoperative week. Six patients had minor complaints of pain at the entry point of the nail after the 16th postoperative week, which gradually resolved by the 6th postoperative month. The average Mayo Elbow Score was excellent (95.8/100).
Discussion
Intramedullary fixation for humeral shaft fractures has gained in popularity in recent years for many reasons, including improved image intensification, relatively percutaneous insertion techniques, the need for proficiency in plate application, and the overall good results with intramedullary nails for fractures of the other long bones. In comparison with compression plate fixation, intramedullary nailing is associated with a shorter operating time, no need of external support, reduced blood loss, low infection rate, and early recovery of function [2, 13, 14, 20, 21]. The rates of fracture union are particular satisfactory and remarkably high as well.
However, literature reports of intramedullary nailing vary from great enthusiasm to strong criticism [15]. This criticism is based on concerns regarding the type of the nail, the insertion techniques, the inability to achieve rotational stability, migration of the nail, and problems with shoulder function. Shoulder pain, decreased muscular strength, and joint stiffness sometimes requiring manipulation under anesthesia are some of the complications following the standard nail insertion entry point [4, 6, 8, 10]. When the nail is inserted at the level of the anatomical neck, the resultant tear in rotator cuff tendons must be carefully sutured, whereas if the insertion point is located directly at the crest of the greater tuberosity, the insertion of the rotator cuff is damaged and is difficult to repair because of the poor blood supply to this area. In several cases, this ‘iatrogenic’ injury of rotator cuff insertion during the insertion of the awl, reaming, application or withdrawal of the nail is extremely extensive, resulting in a severe compromise of shoulder function during the rehabilitation period. Even in patients with minimal rotator cuff trauma, the time of functional rehabilitation of the shoulder is usually prolonged up to 3 months postoperatively, as well as the patient’s functional deficiency and morbidity. Moreover, subacromial impingement caused by nail migration is not an uncommon complication [13], requiring material removal, whereas in cases of nail extraction from the same entry point, the injury to the rotator cuff becomes constant and progressively leads to permanent pain, cuff tear, and shoulder disability.
Retrograde insertion of the humeral nail is quite reasonable [10, 16, 17], but it has not gained in popularity for many reasons including the bulky targeting device, the solitary interlocking possibility proximally and distally, and the lack of intrafragmentary compression.
Taking into consideration all these problems creating a lot of concern regarding the efficacy of intramedullary nailing in the treatment of humeral diaphyseal fractures, we suggest a modification in the surgical technique of antegrade intramedullary nailing: a less traumatic entry point that preserves and retains the shoulder anatomy. Based on our experience, we believe that the proposed entry point, 1 cm below the crest of the greater tuberosity, is a safe method which preserves the articular surface of the humeral head and the rotator cuff insertion from damage. Using the Russell–Taylor humeral nail according to this technique, we did not face any case of penetration or splitting fracture of the inner cortex opposite to the entry point. It is essential to ensure enlargement of the entry hole and the proximal canal in order to facilitate the slipping of the nail on the inner cortex and over the guide wire before its promotion distally. After the application of the nail, reduction of the fracture was achieved in all cases, and no fracture gap exceeding 1 mm was detected. Another benefit of this technique is the ability to fix the proximal locking screw in cortical bone so that migration of the screw can be avoided. Passive, painless, full range of motion of the shoulder and elbow joint could be initiated from the second postoperative day, followed by early active motion while the healing process was going on.
In conclusion, antegrade intramedullary nailing is a reliable and beneficial surgical procedure for the treatment of humeral shaft fractures, regarding union and functional recovery of the upper extremity. However, several complications like intraoperative shoulder joint injuries and other technical difficulties inhibit the acceptance of the method by orthopedic surgeons. In order to avoid those problems, an extra-articular insertion of the nail at a lower entry point, preserving the rotator cuff and articular surface, should be selected. Possible future modifications of the humeral nailing systems to facilitate this antegrade insertion through the proposed entry point form the next step for the further development of this technique.
References
Ajmal M, O’Sullivan M, McCabe J, Curtin W (2001) Antegrade locked intramedullary nailing in humeral shaft fractures. Injury 32:692–694
Brumback RJ, Bosse MJ, Poka A et al (1986) Intramedullary stabilization of humeral shaft fractures in patients with multiple trauma. J Bone Joint Surg Am 68:960–970
Chapman JR, Henley MB, Agel J, Benca PJ (2000) Randomized prospective study of humeral shaft fracture fixation: intramedullary nails versus plates. J Orthop Trauma 14:162–166
Cox MA, Dolan M, Synnott K, McElwain JP (2000) Closed interlocking nailing of humeral shaft fractures with the Russell-Taylor nail. J Orthop Trauma 14:349–353
Crolla RMPH, Vries LS de, Clevers GJ (1993) Locked intramedullary nailing of humeral fractures. Injury 24:403–406
Farragos AF, Schemitsch EH, McKee MD (1999) Complications of intramedullary nailing for fractures of the humeral shaft: a review. J Orthop Trauma 13:258–267
Flinkkila T, Hyvonen P, Lakovaara M, Linden T, Ristiniemi J, Hamalainen M (1999) Intramedullary nailing of humeral shaft fractures. A retrospective study of 126 cases. Acta Orthop Scand 70:133–136
Gregory P, Sanders R (1997) Compression plating versus intramedullary fixation of humeral shaft fractures. J Am Acad Orthop Surg 5:215–223
Heim D, Herkert F, Hess P, Regazzoni P (1993) Surgical treatment of humeral shaft fractures: the Basel experience. J Trauma 35:226–232
Henley MB, Chapman JR, Claudi BF (1992) Closed retrograde Hackethal nail stabilization of humeral shaft fractures. J Orthop Trauma 6:18–24
Ikpeme JO (1994) Intramedullary interlocking nailing for humeral fractures: experiences with the Russell–Taylor humeral nail. Injury 25:447–455
Ingman AM, Waters DA (1994) Locked intramedullary nailing of humeral shaft fractures: implant design, surgical techniques and clinical results. J Bone Joint Surg Br 76:23–29
Lin J, Shen PW, Hou SM (2003) Complications of locked nailing in humeral shaft fractures. J Trauma 54:943–949
Lin J, Hou SM (2003) Locked nailing of severely comminuted or segmental humeral fractures. Clin Orthop 406:195–204
Riemer BL, Foglesong ME, Burke CJ III, Butterfield SL (1994) Complications of Seidel intramedullary nailing of narrow diameter humeral diaphyseal fractures. Orthopedics 17:19–29
Rommens PM, Blum J, Runkel M (1998) Retrograde nailing of humeral shaft fractures. Clin Orthop 350:29–39
Rommens PM, Verbruggen J, Broos PL (1995) Retrograde locked nailing of humeral shaft fractures: a review of 39 patients. J Bone Joint Surg Br 77:84–89
Sanzana ES, Dummer RE, Castro JP, Diaz EA (2002) Intramedullary nailing of humeral shaft fractures. Int Orthop 26:211–213
Scheerlinck T, Handelberg F (2002) Functional outcome after intramedullary nailing of humeral shaft fractures: comparison between retrograde Marchetti-Vicenzi and unreamed AO antegrade nailing. J Trauma 52:60–71
Vecsei N, Kolonja A, Mousavi M, Vecsei V (2001) Intramedullary fixation of humerus shaft fractures. An analysis of complications of 2 implants with special reference to outcome after management with the unreamed humerus interlocking nail. Wien Klin Wochenschr 113:597–604
Watanabe RS (1993) Intramedullary fixation of complicated fractures of the humeral shaft. Clin Orthop 292:255–263
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dimakopoulos, P., Papadopoulos, A.X., Papas, M. et al. Modified extra rotator-cuff entry point in antegrade humeral nailing. Arch Orthop Trauma Surg 125, 27–32 (2005). https://doi.org/10.1007/s00402-004-0757-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-004-0757-3