Abstract
The first ultrastructural investigations of Alzheimer’s disease noted the prominence of degenerating mitochondria in the dystrophic neurites of amyloid plaques, and speculated that this degeneration might be a major contributor to plaque pathogenesis. However, the fate of these organelles has received scant consideration in the intervening decades. A number of hypotheses for the formation and progression of amyloid plaques have since been suggested, including glial secretion of amyloid, somal and synaptic secretion of amyloid-beta protein from neurons, and endosomal–lysosomal aggregation of amyloid-beta protein in the cell bodies of neurons, but none of these hypotheses fully account for the focal accumulation of amyloid in plaques. In addition to Alzheimer’s disease, amyloid plaques occur in a variety of conditions, and these conditions are all accompanied by dystrophic neurites characteristic of disrupted axonal transport. The disruption of axonal transport results in the autophagocytosis of mitochondria without normal lysosomal degradation, and recent evidence from aging, traumatic injury, Alzheimer’s disease and transgenic mice models of Alzheimer’s disease, suggests that the degeneration of these autophagosomes may lead to amyloid production within dystrophic neurites. The theory of amyloid plaque pathogenesis has thus come full circle, back to the intuitions of the very first researchers in the field.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Deposits of extracellular amyloid with closely associated neuronal and glial pathology are commonly identified with Alzheimer’s disease, but amyloid plaques are found in many other conditions, including transmissible spongiform encephalopathies and traumatic brain injury. Amyloid plaques also commonly occur with aging in the absence of disease, injury or dementia. Plaques form in the cerebral cortex of aged primates [72, 184, 194], and in many non-primate species, but only rarely in aged rodents [257]. Animal models of amyloid pathology, created by inserting Alzheimer’s disease genes into mice, have rapidly expanded our knowledge in recent years, warranting a reconsideration of the mechanisms of amyloid plaque pathogenesis.
Amyloid is any proteinaceous polymer having a beta-pleated sheet conformation that accumulates extracellularly (for reviews see [205, 275]). In transmissible spongiform encephalopathies, such as mad cow disease, the amyloid is composed primarily of prion protein rather than the amyloid-beta (Aβ) peptide of Alzheimer’s disease. A number of prion diseases, including Creutzfeldt–Jakob disease, Gerstmann–Sträussler–Scheinker disease, kuru, and scrapie, exhibit amyloid plaque pathology similar to that of aging and Alzheimer’s disease [139]. A number of other cellular proteins may form amyloid in the brain, and all of these amyloids induce pathological changes [10, 31, 57, 168].
Amyloid plaques can result from traumatic brain injury in which axonal damage is distributed diffusely throughout the brain. Organelle accumulation in disrupted axons over a period of a few days post-injury leads to axotomy and plaque formation in animal models of traumatic injury [33, 219, 229]. Likewise in humans, traumatic brain injury with diffuse axonal damage leads to plaques containing Aβ protein [97, 218]. There is also evidence that amyloid plaques accumulate in the cerebral cortex of athletes involved in violent sports such as football and boxing [107, 177, 200].
The fact that insoluble extracellular deposits of fibrillar protein accumulate in a similar pattern in so many different conditions provides interesting clues to the mechanisms of pathogenesis. Pathogenesis likely involves a site of particular vulnerability that is disrupted by a variety of insults. Although amyloid is assembled from cellular proteins, where this assembly takes place is currently unknown. As reviewed below, several loci have been proposed for amyloid polymerization, including glia cells, neuronal lysosomes, and extracellular fluid, but the current evidence does not unequivocally endorse any of these loci. The early hypotheses of Fischer and Bonfiglio maintained that amyloid derives from degenerating axons (reviewed in [78]), and this alternative is reconsidered in light of the recently recognized importance of disrupted axonal transport in amyloid pathology [40, 77, 201, 226].
Amyloid plaque morphologies
Plaques are frequently identified by light microscopy using methods specific for fibrillar amyloid such as thioflavin-S or Congo Red staining. The commonly used descriptors “primitive” and “cored” describe the two main types of amyloid plaques revealed by this kind of histology and by electron microscopy. Several additional types of amyloid-related protein deposits have been more recently identified by immunohistochemistry (for a recent review see [241]).
Primitive plaques
Primitive plaques are composed of extracellular wisps of amyloid woven among a dense cluster of dystrophic neurites. The “dystrophic” label was given to these grossly swollen neurites because they resemble the spheroid enlargements of axons found in cases of malnutrition and in the infantile neuroaxonal dystrophy of Seitelberger [133]. Primitive plaques are sometimes called “neuritic” plaques because such dystrophic neurites are always present.
The term “dystrophic” is often mistakenly applied to the more fusiform, distorted neurites containing paired helical filaments (neurofibrillary tangles) of tau protein. Neurites with tau tangles are found in plaques in advanced Alzheimer’s disease, but they are absent from plaques in early disease stages [14, 41, 163, 232, 241, 265, 295]. Many non-human mammalian species develop amyloid plaques with aging but do not have neurites with tau inclusions [43, 212, 252]. Transgenic mice carrying Alzheimer’s disease mutations have amyloid plaques without tau tangles (for reviews see, [70, 221]) while mice engineered to also produce tau tangles initially form amyloid plaques without them [17, 170, 171]. This evidence establishes that plaques can form in the absence of neuritic tau accumulations, and that this type of neurite, while significant to Alzheimer’s disease progression, is not a general mechanism of amyloid plaque pathogenesis. In this review, the term “dystrophic neurite” is only used to refer to the globular type of swelling without tau tangles.
The term “neurite” is used because the distorted morphology makes it difficult to unequivocally identify the profiles as axonal or dendritic [148, 151]. However, evidence from transgenic mice demonstrates that most grossly swollen, dystrophic neurites are axons [17, 185, 222, 250, 299]. Dendrites passing through plaques often display spine loss, increased curvature, and a reduction in shaft diameter, while filopodial extensions and swellings are less frequently observed [81, 195]. The dystrophic swellings in plaques are more often diverticular offshoots from unmyelinated axons [63, 195]. Whether these dystrophic axons are degenerating or regenerating has been debated [2, 151, 258], but the fact that axon densities are reduced in plaques appears to favor degeneration [13, 52, 222].
By light microscopy, primitive plaques are observed to be spherical regions of pathology, usually 10–70 μm, but sometimes more than 100 μm, in diameter [6, 24]. Electron microscopy reveals many more small neuritic plaques than are apparent by light microscopic examination [239]. The smallest primitive plaques are clusters of just a few dystrophic neurites in the neuropil and do not involve cell bodies of any kind (Fig. 1). In addition to dystrophic neurites, the plaque region often contains normal-looking neuronal and glial processes, but the density of synapses is greatly reduced from that of normal neuropil [115, 125]. Occasionally, a dystrophic neurite is found to be the presynaptic partner of a synapse [75, 282], but claims that most dystrophic neurites are abnormal synaptic terminals are not supported by the available data. The frequency of synapses on dystrophic neurites in plaques has never been quantified, but immunolabeling for presynaptic proteins reveals that most dystrophic neurites lack the full synaptic machinery [18, 62].
A primitive neuritic plaque from layer III of prefrontal cortex of a 32-year-old rhesus monkey. Serial section electron microscopy shows that the plaque is a cluster of dystrophic neurites around darker extracellular deposits. This section from the center of the plaque shows the maximum diameter of approximately 12 μm. Surrounding the cluster of dystrophic neurites is normal-looking cortical neuropil in which glial and neuronal cell bodies are absent
The first ultrastructural studies of Alzheimer’s disease revealed that dystrophic neurites are swollen by abnormal accumulations of filaments, vesicles, tubules and mitochondria [115, 143, 238]. Transitional forms between mitochondria and additional mitochondrial-sized lamellar or dense bodies are obvious, and all of the early investigators, with the exception of Terry et al. [238], speculated that the numerous lamellar and dense bodies were degenerating mitochondria. Krigman et al. [125] further speculated that the degeneration of mitochondria in dystrophic neurites might ultimately lead to cored plaques. These inferences of progressive degeneration were partly motivated by the similarity of dystrophic neurites to axons undergoing Wallerian degeneration after transection [133, 134]. After Suzuki and Terry [233] found that the lamellar and dense bodies contained acid phosphatase, and classified these inclusions as lysosomes, little further consideration was given to their origin or fate until recently.
The terminology used to describe plaque types is not standardized, and some investigators use the term “diffuse plaque” to describe the distribution of amyloid in primitive plaques containing both amyloid fibrils and dystrophic neurites [54, 241, 252]. The adjective “diffuse” has also been applied to many other types of fibrillar and non-fibrillar deposits, so to avoid confusion “diffuse” will be avoided altogether in this review.
Cored plaques
Cored plaques differ from primitive plaques by containing a large central mass of amyloid. The central mass of amyloid makes these plaques easily identifiable with amyloid staining techniques, giving these plaques the moniker “classical”. The amyloid core sometimes has a star-shaped appearance with spokes of amyloid extending outward, and it is usually surrounded by a spherical cluster of dystrophic neurites and extracellular wisps of amyloid as in the primitive plaque.
Immediately around the core there may be a layer devoid of amyloid and neuritic processes. Ultrastructural studies reveal that this halo effect is created by glia that enclose the core [110, 150, 223, 257, 270, 296]. Cores of small plaques are enveloped by one or two activated microglia, while large plaque cores are surrounded by processes from dozens of microglia and astrocytes [268]. When cored plaques are not surrounded by dystrophic neurites and wisps of amyloid they are often referred to as compact or “burnt-out” plaques. Compact plaques are also enveloped by glial cells, in some cases entirely by astrocytes [115, 239].
Non-amyloid deposits
After the Aβ peptide was identified [152], it became possible to further examine the distributions of both fibrillar and non-fibrillar forms of Aβ in Alzheimer’s disease using immunohistochemistry. Immunolabeling revealed a more widespread deposition of the Aβ peptide than was seen previously with the classical stains for fibrillar amyloid [234, 281, 291]. Non-amyloid Aβ deposits, often called “diffuse plaques”, are frequently seen in the cerebral cortex, cerebellum, and striatum. The morphology of the deposits depends on the characteristics of the tissue. For example in the cerebellum, non-amyloid deposits extend vertically through the molecular layer, often appearing to loosely follow Purkinje neuron dendritic arbors [106, 264].
The Aβ immunoreactivity of non-amyloid deposits often extends over a large region 200 μm or more in diameter [234], which is largely devoid of dystrophic neurites or activated microglia, but occasional dystrophic neurites may be found on close inspection [18, 292]. While most of the immunoreactive region appears to lack amyloid, a sparse distribution of extracellular fibrils is sometimes revealed by electron microscopy [292], by Campbell–Switzer silver staining [241], or by weak thioflavin-S fluorescence [136]. Some investigations have concluded that amyloid fibrils are present in all deposits that are immunoreactive for fibrillogenic forms of the Aβ peptide, which would include most types of “non-fibrillar” deposits [49, 241, 242].
One issue with the identification of non-amyloid deposits is the use of formic acid pretreatment to enhance immunoreactivity [118]. This procedure defibrillates amyloid and solubilizes the constituent peptide, thus precluding amyloid staining by Congo Red or thioflavin-S [231]. Such treatment may also cause diffusion of the amyloid peptide within the tissue sample and may even extract amyloid protein from neurons [48, 174]. It is perhaps not surprising then that non-amyloid deposits are sometimes large, lake-like regions of Aβ immunoreactivity that are either peri-neuronal or extend beyond a central region of neuritic pathology. However, other investigators report that distributions of Aβ immunoreactivity are little changed by formic acid pretreatment [100, 106].
Numerous studies indicate that the molecular composition of non-amyloid deposits differs from that of primitive and cored plaques [80, 90, 158, 196, 245]. Non-amyloid deposits in the cerebellum, for example, are characterized by a preponderance of Aβ fragments in which the amino-terminal is truncated [100, 131]. This less fibrillogenic molecular profile was confirmed in aged canines [285], a species that develops non-amyloid Aβ deposits but not neuritic plaques [43]. Immunotherapy using antibodies directed at the amino-terminal of Aβ successfully removes fibrillar plaques but not non-amyloid deposits [183], further substantiating the difference in molecular composition. The relative lack of neuritic and microglial pathology in non-amyloid deposits may be related to this different composition.
Do plaque types reflect a progression of pathology?
Based on ultrastructural studies, Terry and Wisniewski [239, 240] proposed that small clusters of dystrophic neurites evolve into larger primitive plaques and, with the continual accumulation of extracellular amyloid, primitive plaques eventually evolve into cored plaques. While this plaque evolution hypothesis is certainly consistent with the structural evidence, it has met with criticism (reviewed in, [5]). An opposite progression has even been proposed, with cored plaques transitioning into primitive plaques to end up as non-amyloid deposits [269].
Struble et al. [230] found that as total plaque density increased in aged monkeys, there was a corresponding increase in cored plaques, suggesting that primitive plaques evolve into cored plaques. Evidence in favor of a plaque progression in Alzheimer’s disease has been less conclusive, however. Some studies have reported that primitive plaques precede cored plaques and that cored plaques accumulate as the disease progresses [244], but other studies have reported that primitive plaques increase with duration of the disease while cored plaques do not [54]. Supportive evidence for plaque progression comes from transgenic mice models of Alzheimer’s disease and from Down’s syndrome.
Transgenic mice expressing pathogenic forms of the Aβ precursor protein (APP) and its proteolytic enzymes exhibit increased production of Aβ from APP. Young mice first develop mostly small primitive plaques, but later numerous cored plaques appear [15, 85, 237]. The sizes of cored plaques and the number of invested microglial cells increase with age, and in the oldest transgenic mice, large plaques are often infiltrated by hypertrophic astrocytic processes [197, 268]. Older mice also exhibit more cored plaques with a “burnt-out” morphology in which dystrophic neurites are largely absent [15].
Down’s syndrome is manifested by an extra copy of chromosome 21, which leads to overexpression of APP and early onset of Alzheimer’s disease. The numerical density of amyloid plaques increases with age in Down’s syndrome [96, 136]. Non-amyloid deposits appear in the second and third decades of life, followed by neuritic and cored plaques in the fourth to fifth decades [87, 91, 136]. Primitive plaques predominate when Alzheimer’s disease first becomes identifiable, but with continued aging there is an increase in cored plaques. Protein aging studies confirm that the amyloid in the cores of classical plaques is older than the amyloid in primitive plaques, and the cores are surrounded by a halo of younger amyloid [9, 65].
Given the multifarious nature of non-amyloid deposits, it is difficult to assign them a specific role in the progression of pathology. Extracellular deposits containing mostly soluble Aβ protein are often assumed to represent the first step in amyloid plaque pathogenesis [53, 210, 234]. The best evidence supporting this contention is usually taken to be the sequence of pathology reported in Down’s syndrome [5], but recent evidence from transgenic mice is not confirmatory. Non-amyloid deposits appear months after fibrillar plaques in most transgenic mice with one or more Alzheimer’s disease mutations [76, 85, 114, 155, 197, 198]. However, when transgenic mice are engineered to overexpress APP without mutations, similar to Down’s syndrome, they initially develop non-amyloid deposits [89]. Non-amyloid deposits in the cerebellum and striatum, which are highly insoluble, do not appear to evolve into neuritic plaques over the course of Alzheimer’s disease [286] or over a lifetime with Down’s syndrome [147]. The existence of a “pre-amyloid” type of deposit therefore, remains controversial.
Proposed mechanisms of plaque pathogenesis
A key attribute of all plaques is the focal deposition of amyloid in a local, typically spherical, region. The evidence for temporal evolution suggests that primitive plaques mature into cored plaques, and then stabilize as large, spherical areas of pathology around this focus of fibrillar amyloid [36]. Although several different mechanisms for the focal deposition of amyloid have been proposed (Fig. 2), the issue of how plaques form is still unresolved.
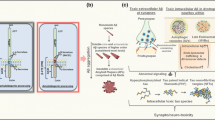
Competing hypotheses for the locus of amyloid production and the pathogenesis of neuritic plaques. a Amyloid deposition is initiated from blood vessels that release Aβ (1) which spontaneously fibrillates (2) in the perivascular space and creates a toxic environment for axons, leading to dystrophy (3). b Amyloid deposition is initiated by glia that secrete Aβ (1) which spontaneously fibrillates (2) and produces axonal dystrophy (3). c Aβ is secreted from somato-dendritic regions or synaptic terminals of neurons (1). The protein spontaneously aggregates (2) into amyloid filaments that activate microglia (3). Activated microglia secrete toxins that cause axonal dystrophy (4). d Aβ is secreted by neurons (1) and processed extracellularly into amyloid filaments by microglia (2). Amyloid toxicity leads to axonal dystrophy (3). e Aβ or its precursor protein is internalized through endocytosis and aggregated in lysosomal compartments in the cell body of neurons (1). Lysis of the cell (2) leads to extracellular deposition, which activates microglia (3). Activated microglia poison axons leading to dystrophy (4). f Amyloid is formed in autophagosomes (1) trapped in axonal dystrophies and deposited by rupture of the swelling (2). Extracellular amyloid leads to the formation of more dystrophies (3) by disrupting axonal transport, and provokes a glial reaction (4)
Blood vessel origin
Amyloid plaques are frequently accompanied by cerebral amyloid angiopathy in which amyloid is deposited around cerebral and leptomeningeal blood vessels. The cause of cerebral amyloid angiopathy is unknown (for review see [23]), but similarities in the distributions of amyloid angiopathy and plaques suggest that blood vessels might be involved in amyloid plaque formation [4, 58, 260]. The severity of Alzheimer’s disease pathology correlates with the severity of co-occurring cerebral amyloid angiopathy [7, 8], and large cored plaques are often in close proximity to blood vessels with amyloid deposits [126, 127], further suggesting that brain amyloid might originate from systemic circulation or from the cells of the blood vessel walls [56, 105]. However, small plaques are frequently far from blood vessels [4, 111], ruling out a nidus of origin involving blood vessels for these plaques.
Neuron-specific expression of Alzheimer’s disease mutations in mice causes parenchymal amyloid plaques to form prior to significant perivascular amyloid deposition [197], making it unlikely that Aβ originates from blood or blood vessel walls. Rather, cerebral amyloid angiopathy appears to develop from neuronal APP, since it also occurs in APP-null mice expressing mutant APP only in neurons [25]. In addition, amyloid angiopathy occurs in the thalamus, even though neurons in the thalamus do not express the transgenes, indicating that the transgene products are transported from cortex, possibly by axons [25].
Glial production of amyloid
All cored plaques contain activated microglia that surround and interdigitate with the central mass of amyloid. On single sections, bundles of amyloid are often completely surrounded by microglial profiles, giving the appearance that amyloid lies within membranous compartments in the microglia cytoplasm. This appearance led to the supposition that fibrillar amyloid is secreted by microglia [160, 238]. Some investigators speculated that amyloid fibrils are formed within the endoplasmic reticulum of microglia and exocytosed to the extracellular space [284]. But evidence from serial section electron microscopy shows that the amyloid fibrils in cored plaques that appear to lie within microglia are in fact entirely extracellular [204, 223, 257, 268].
The proteolytic enzymes responsible for production of Aβ from APP, as well as APP itself, are most strongly expressed in neurons [42, 44, 124, 215, 256]. Therefore, glia are unlikely producers of the Aβ that forms plaques. The glial secretion hypothesis was accordingly modified to propose that Aβ from neurons is processed into amyloid at the plasma membrane of microglia cells [148, 165]. Support for this hypothesis comes from studies showing activated microglia in plaques from the onset of amyloid pathology in transgenic mice [88, 197, 224, 268].
The production of amyloid principally at the surface of microglia gives a definite nidus to amyloid plaque formation, every plaque would originate at a microglial cell. But if each microglial cell is independently capable of forming a plaque, it is unclear why large numbers of microglia cluster around single plaque cores [224]. Furthermore, although cultured microglia respond to plaques of synthetic amyloid [98], they do not process synthetic Aβ into amyloid plaques [26]. Another difficulty with this hypothesis is that the earliest amyloid plaques would be expected to be compact plaques produced by activated microglia, which would evolve first into classical plaques, and then into primitive plaques when microglia retract and astrocytes infiltrate the amyloid core [269]. Obviously, this evolution is at odds with the sequence of plaque progression in transgenic mice models of Alzheimer’s disease, and some of the earliest, primitive plaques may be devoid of microglia [42, 47, 228].
Microglia and astrocytes may be consumers of amyloid rather than producers, since cultured microglia internalize aggregates of Aβ peptide and rapidly phagocytose plaque cores [51, 66, 181]. There is also some evidence of phagocytosis and digestion of amyloid by microglia in vivo [102, 153, 273], and astrocytes have been shown to migrate to and degrade amyloid plaques [288]. Consistent with consumption of amyloid instead of production, inhibition of microglial responses in transgenic mice leads to more rapid development of amyloid pathology [59, 289].
Neuronal secretion of Aβ
Neurons in culture secrete Aβ, and extracellular, soluble Aβ peptide has been proposed to be sufficient to initiate plaque formation [209]. In a simple version of this hypothesis, abnormal proteolysis of APP at the surface of neurons releases Aβ peptide directly into the extracellular space. However, the proteolytic enzymes that generate Aβ from APP appear to operate in intracellular compartments rather than at the neuron plasma membrane (for reviews see [217, 276]). Many different compartments have been proposed as principal sites of pathogenic cleavage prior to secretion, including rough endoplasmic reticulum, golgi secretory apparatus, and endosomes that recycle to the plasma membrane. Whatever the compartment, non-fibrillar deposits generated by the secretion of soluble Aβ would be centered on neurons, in agreement with data showing some Aβ immunoreactivity centered on the cell bodies and primary dendrites of neurons in Alzheimer’s disease and aging [178, 179, 271]. In the cerebella of Alzheimer’s disease patients, non-fibrillar deposits are often closely associated with accumulations of Aβ inside the somata and dendrites of Purkinje neurons [264].
In conflict with the hypothesis that the neuron soma is the primary nidus of amyloid plaque formation, many amyloid plaques are not centered on neuron cell bodies. As shown by electron microscopy, small plaques are often located in the synaptic neuropil and involve only neurites and glial processes without any neuronal cell bodies or large proximal dendrites (Fig. 1). The soma is often not the nidus of plaque formation even when it is the source of Aβ. This is evident in mice with genetic constructs designed to secrete Aβ through the golgi pathway. In these mice amyloid plaques form in the molecular layers of the cerebellum and hippocampus rather than only in cell body layers [154].
APP is trafficked down the axon [108, 123], suggesting that Aβ is produced in synaptic terminals rather than in the somato-dendritic compartment. One hypothesis based on this idea is that normal synaptic transmission secretes Aβ, which if not cleared quickly leads to pathogenesis [211]. Recent experiments in transgenic mice demonstrate that extracellular levels of Aβ rise with epileptiform activity and decrease when synaptic transmission is blocked [38]. Additional support for an axonal locus of production comes from studies in transgenic mice showing that the transection of axons of the perforant pathway to the hippocampal dentate gyrus reduces the amount of Aβ protein deposited in this brain region [135, 213, 254]. Unlike somatic secretion however, there is no obvious nidus of fibrillation with synaptic secretion. Synaptic release of soluble peptide would disperse Aβ widely throughout the neuropil of the cerebral cortex.
Spontaneous extracellular fibrillogenesis
One proposal for how soluble Aβ triggers plaque pathogenesis is that the peptide spontaneously begins to form fibrils as the extracellular concentration of Aβ reaches high levels [53, 210, 241]. To explain the formation of a neuritic plaque, it is assumed that the extracellular amyloid attracts microglia, which release molecules toxic to nearby axons and dendrites, causing them to swell and degenerate. Since microglia and amyloid precede dystrophic neurites in this hypothesis, it is in conflict with the sequence of plaque progression discussed above.
Although solutions of synthetic Aβ spontaneously fibrillate in vitro under certain conditions, the extent to which this happens in vivo is unclear. Comparable concentrations of Aβ peptide are found in the extracellular fluid of normal mice and transgenics with amyloid pathology [37], and this concentration appears to be orders of magnitude less than the concentration required for spontaneous fibrillation in vitro [141, 180]. Moreover, the presence of a high concentration of Aβ appears to be insufficient for both fibrillation and plaque pathogenesis in vivo, since intracerebral injections of Aβ rarely produce plaques [156, 214, 277 but see 216].
Additional evidence indicates that oligomerization begins intraneuronally, with secretion of soluble oligomers rather than monomers of Aβ [263]. Pathogenesis may require this prior aggregation of Aβ into oligomers or protofibrils, since the Aβ peptide is much less toxic to neurons than these multimers (reviewed in [262]). Experiments with transgenic mice suggest that soluble Aβ oligomers may be involved in the cognitive decline of Alzheimer’s disease [39, 137], but there is still little evidence for the formation of focal, neuritic amyloid plaques directly from these oligomers. Intracerebral injections of Aβ dimers, oligomers or polymers at physiological concentrations produces little or no seeding of amyloid plaques, even in transgenic mice predisposed to amyloid pathology [156]. However, injection of extracts from brains with extant amyloid pathology does seed plaques, suggesting that factors in addition to Aβ protein are involved in plaque pathogenesis [11, 109, 156].
Neuronal accumulation and lysis
Several groups proposed that Aβ aggregation within the cell bodies of neurons is prerequisite to deposition in the extracellular space (for reviews see [78, 129, 276, 279]). In Down’s syndrome, granular accumulations of Aβ can be seen in neuronal cell bodies prior to the appearance of plaques or perineuronal deposits [82, 162], and Aβ peptide accumulates in a granular pattern in the cell bodies of neurons in Alzheimer’s disease [46, 79]. Transgenic mice with amyloid pathology also exhibit intraneuronal granules of Aβ immunoreactivity [15, 171, 278, 280]. In mice with highly accelerated pathology, fibrillar amyloid accumulates in neurons along with Aβ prior to deposition of the protein in the extracellular space [169].
Aβ could accumulate inside any of the intracellular compartments where it is cleaved from APP but not secreted. Two likely candidates are endoplasmic reticulum [86, 247], and lysosomes [29, 30, 182]. To reach the lysosomal pathway, Aβ might be produced inside endosomes by proteolytic processing of internalized APP, or Aβ might be endocytosed from an extracellular pool of soluble protein [119]. Normal processing of endosomal compartments would then lead to aggregation of the Aβ within lysosomes.
Amyloid plaques might be created when lysosome-laden neurons die and release amyloid into the extracellular space [46, 74]. In this hypothesis, every plaque is centered on a dying neuron. Although there is evidence for somal and lysosomal remnants in some plaques [28, 30, 46], plaques are not necessarily concentrated in cell body layers, and transgenic mice engineered to accumulate Aβ in neuronal somata exhibit neurodegeneration but not plaques [130]. Further emphasizing that somata are not niduses of all plaques, non-transgenic brain tissue grafted into transgenic mice develops amyloid plaques before the rest of the hippocampus even though the neurons expressing amyloidogenic mutations reside outside the graft [157].
As noted above, many small plaques are clusters of dystrophic axons and amyloid in neuropil distant from cell bodies (Fig. 1). Consequently, the somal accumulation hypothesis has been extended to include the possible transportation of amyloid-filled endosomes or lysosomes from the soma into neurites [74, 78], where they would presumably accumulate as the lamellar and dense bodies in dystrophic swellings. Dystrophic axonal swellings are often far from the soma, and while evidence shows that endosomal and lamellar bodies are retrogradely transported along axons to the soma [94], there is little evidence for anterograde transportation of lysosomes to distal axons.
Disruption of axonal transport
Disruption of fast axonal transport leads to focal swellings filled with organelles [95, 251], which resemble Wallerian degeneration [267]. Similarities to Alzheimer’s disease pathology led many investigators to surmise that disrupted axonal transport is responsible for the formation of dystrophic neurites in amyloid plaques [69, 115, 134, 192, 240]. Terry and Wisniewski [240], in the vein of Fischer and Bonfiglio, suggested that the earliest precursor of a senile plaque was an axonal swelling, but the mechanism by which an axonal swelling might serve as a nidus of amyloid deposition and plaque formation has remained elusive. Renewed interest in this possibility (as exemplified by [77, 226]) is largely due to recent findings in transgenic mice models of Alzheimer’s disease.
Transgenic mice with amyloid pathology exhibit swellings along the lengths of axons long before amyloid deposition is detectable [227, 250]. These non-synaptic, non-terminal axonal swellings are filled with mitochondria, vesicles, and mitochondrial-sized lamellar and dense bodies, consistent with disrupted axonal transport. Furthermore, reduced expression of microtubule motor proteins in these mice increases the number of axonal swellings, as well as the number of amyloid plaques later in the disease, reinforcing the supposition that disrupted axonal transport contributes to the formation of amyloid plaques [227].
Traumatic brain injury produces axonal swellings similar in appearance to plaque dystrophic neurites [33, 219, 229], and these swellings are believed to arise as a result of impaired axonal transport (reviewed in [22, 190]). Axon swellings appear within 1–2 h post-injury and demonstrate intense APP immunoreactivity, consistent with interruption of the normal axonal transport of this protein [186, 218]. Some swellings also exhibit immunoreactivity for Aβ peptide and stain for fibrillar amyloid, suggesting that amyloid plaques are sequelae of the deposition of amyloid from axon swellings after traumatic injury [34, 186].
APP-immunoreactive dystrophic neurites that resemble those of traumatic injury are likewise found in the amyloid plaques of Alzheimer’s disease [42, 44, 112, 153, 215]. Some investigators hypothesize that extracellular amyloid causes structural injury to axons in the same manner as traumatic injury [117, 287]. However, evidence for amyloid inside axon swellings following traumatic injury also supports the opposite relationship, namely that dystrophic neurites in plaques produce amyloid.
Autophagic production of amyloid
Dystrophic axons clearly accumulate APP, and cleavage of APP to Aβ protein likely occurs within these swellings as well, because the enzymes responsible for this proteolysis also accumulate there [21, 34, 248, 299]. One candidate compartment for this proteolysis is the early endosome. Although there is scant evidence for significant endocytosis within dystrophic neurites of amyloid plaques, endosomes might be trafficked into dystrophic swellings from the distal axon [166]. However, immuno-electron microscopy of Aβ has thus far failed to localize the Aβ protein to clearly identifiable endosomal compartments within dystrophic neurites [120–122, 235, 236].
Another candidate site for Aβ production in dystrophic neurites is within autophagic vacuoles, which have recently been implicated in Alzheimer’s and other neurodegenerative diseases (for review see [202]). Analysis of biopsy material reveals that Alzheimer’s disease brains contain many more autophagosomes than normal brains [167], and a similar abnormal accumulation of autophagosomes occurs in transgenic mice with amyloid pathology [297]. The majority of these autophagosomes are concentrated in the dystrophic neurites of amyloid plaques, but a few are found in the somato-dendritic compartment. These autophagic vacuoles appear to be a prominent locus of Aβ production [297, 298]. In cultured cells overexpressing APP, suppression of autophagy reduces Aβ secretion while induction of autophagy increases Aβ release [297].
The substrate of autophagy is unclear, but recent data indicate that autophagocytosis of mitochondria is increased in Alzheimer’s disease [161]. Autophagocytosis followed by lysosomal processing is the major degradative pathway for mitochondria, a process sometimes abbreviated as “mitophagy” (for reviews see [20, 116]). Moreover, the autophagocytosis of mitochondria would account for the transitional forms between normal mitochondria and the lamellar bodies in dystrophic neurites of amyloid plaques [63, 239, 283]. Amyloid may be produced by dysfunctional mitophagy, and this possibility is supported by immuno-electron microscopy showing that APP accumulates in the mitochondria and lamellar bodies of dystrophic neurites [17, 50, 112, 148, 215]. Proteolytic enzymes necessary for the production of Aβ from APP have also been identified in mitochondria and autophagosomes [84, 297, 298], as have the Aβ peptide and its oligomers [27, 120, 121, 144, 146, 218, 293, 297].
A synthesis of mechanisms
One curious aspect of most proposed mechanisms of plaque formation is that the central cellular pathology of primitive plaques, the dystrophic neurite, plays no role in pathogenesis (Fig. 2). Dystrophic neurites are often considered to be an incidental consequence of amyloid deposition or microglial activation, but not active participants in plaque pathogenesis. In other words, most hypotheses assume that extracellular Aβ peptide and microglial activation are all that is needed to create a classical amyloid plaque. The data discussed above, however, suggests that plaques form in close conjunction with amyloid protein processing in dystrophic neurites. When considered in synthesis with the mechanisms of disrupted axonal transport, mitochondrial malfunction and oxidative stress, autophagy, impaired lysosomal processing, and intraneuronal production of Aβ, all of which have been implicated in Alzheimer’s disease, the dystrophic neurite is a likely nidus of plaque pathogenesis (Fig. 2f).
Dystrophic axons are antecedents of pathology
The data from traumatic injury, Alzheimer’s disease and transgenic mice, discussed above, are consistent with axonal dystrophy playing a key role in plaque formation. Numerous studies report that the smallest amyloid deposits are closely associated with dystrophic neurites [15, 176, 199, 227, 283]. In addition, isolated dystrophic neurites are found widely scattered throughout the cortical neuropil in all conditions leading to amyloid pathology, including normal aging [113, 149], traumatic brain injury [218, 229], prion diseases [140], and Alzheimer’s disease [41, 167, 215, 227, 283].
Any insult that disassembles axonal microtubules and disrupts retrograde transport would be an additional candidate for initiating plaque pathogenesis, due to the expected formation of dystrophic swellings. This would include excitotoxic injury for example, since high concentrations of extracellular potassium and glutamate have been shown to disrupt axonal transport and induce dystrophic swellings [92, 93]. Relatively few studies have made an association between amyloid plaques and excitotoxic injury, but there is evidence that mediators of excitotoxicity such as hypoxia/ischemia can result in the initial stages of amyloid pathogenesis [32, 104, 189, 255].
Amyloid plaques might also be expected as an outcome of any number of pathological conditions in which dystrophic neurites commonly occur (for reviews see [103, 140]). However, depositions of amyloid are not consistently found in most of these conditions, emphasizing that additional factors are involved, such as overproduction of fibrillogenic fragments of APP. In familial Alzheimer’s disease, the genetic defects leading to overproduction of fibrillogenic Aβ protein may cause relatively benign axonal dystrophies to become potent seeds of pathology. Likewise, in late-onset, sporadic forms of Alzheimer’s disease, the increased frequency of axonal dystrophies with aging may conspire with other factors to increase the probability of amyloid plaque formation.
Mitophagy follows disruption of axonal transport
The organelles that accumulate most during inhibition of retrograde axonal transport are mitochondria [251], because these organelles are normally trafficked from the distal axon to the soma for lysosomal degradation after they become metabolically dysfunctional [188]. Dystrophic neurites in plaques likewise accumulate large numbers of mitochondria, which are metabolically compromised but unable to reach the soma for lysosomal processing [15, 63]. These stranded mitochondria consequently enter a mitophagic pathology leading to production of large numbers of autophagosomes. Autophagosomes might also be trafficked into dystrophic swellings from the distal axon, along with endosomes and amyloid-related proteins, since autophagosomes are also retrogradely transported [94]. In any case, the large numbers of mitochondria, and the transitional forms between these mitochondria and the autophagic vacuoles, indicate that mitochondria are the main substrate of autophagy in dystrophic neurites [63, 115, 233, 239, 240].
As discussed above, autophagosomes appear to be a principal site of Aβ generation in Alzheimer’s disease, but direct evidence of amyloid production by autophagosomes in dystrophic neurites is still lacking. Amyloid fibrillogenesis in vitro has been shown to have an intermediate stage involving a 5 nm-wide protofibril [3, 261], and recent ultrastructural evidence reveals that clusters of autophagosomes in some dystrophic neurites degenerate into loose bundles of 5 nm filaments [63]. This suggests that amyloid fibrillogenesis may occur in some dystrophic neurites (Fig. 3), but verification of the molecular nature of these filaments awaits further studies.
Dystrophic neurites in a primitive neuritic plaque from layer III of prefrontal cortex of a 32-year-old rhesus monkey. Degenerated mitochondria form lamellar bodies that in advanced stages of degeneration form tight clusters (asterisks). These clusters appear to degenerate further (star) into loose 5 nm-wide filaments within the cytoplasm (arrows). Dystrophic neurites with accumulations of filaments and degenerated organelles form a dense matrix (flag) that is similar in appearance to the filamentous material found in the extracellular spaces of the plaque (arrowheads). Scale bar: 0.5 microns
Amyloid disrupts axonal transport and neurite integrity
Extracellular amyloid protein has detrimental effects on neuron integrity. Multimers of Aβ are toxic to neurons [67, 132, 142], and in high enough concentration Aβ peptide can kill cultured neurons, possibly due to the spontaneous formation of such aggregates [45]. Significantly, application of Aβ protein to the axons of cultured neurons induces local swelling and degeneration [99, 187, 220], consistent with the evidence that extracellular amyloid protein disrupts axonal transport [92] and strands mitochondria [203]. The disruption of axonal transport may be due to the formation of calcium-permeable channels by multimers of Aβ [141], since a pathological influx of calcium can completely disassemble microtubules [64, 207, 266].
The effects of intracellular amyloid on neuronal integrity are less well established, but it has been shown that intracellular accumulation of Aβ can lead to loss of membrane integrity and eventual neuron degeneration [55, 130, 294]. Internal aggregation of Aβ could thus lead to disintegration of a dystrophic neurite and spilling of its cytoplasmic contents into the extracellular space, as proposed by Kawai et al. [112], Chen et al. [34], and others. Neuritic lysis in plaques is consistent with evidence of neuronal cytoplasmic and organellar proteins, mRNAs, and membranous organelles among the extracellular amyloid of plaques [28, 30, 63, 73, 138, 191, 193]. These spilled cytoplasmic contents may be part of the plaque seeding mechanism, which would help explain why brain extracts, but not synthetic amyloids, seed plaques [156].
Pathogenesis involves local positive feedback
To account for the focal nature of plaque growth, the primary pathogenic mechanism likely involves local positive feedback between the damage caused by extracellular amyloid and the intracellular production of amyloidogenic proteins. Of the mechanisms considered (Fig. 2), only the production and release of amyloid from dystrophic neurites due to dysfunctional mitophagy appears to fully satisfy this condition. In this scenario, the neuritic plaque is generated by a chain reaction of pathology in a local region of the neuropil, as proposed by Wisniewski and Terry [283], Stokin and Goldstein [226], and others. Rupture of an amyloid-laden swelling would expose neighboring healthy axons to the toxic effects of amyloid, disrupt microtubule-based transport, and cause them to become dystrophic. Such a process would explain why dystrophic neurites are clustered tightly together in plaques [18, 259].
Studies of neuritic plaques in transgenic mice reveal that both human and mouse Aβ is present, with human Aβ concentrated in amyloid cores due to the fibrillogenic transgenes and wild-type mouse Aβ concentrated more in the dystrophic neurites [253], consistent with extracellular amyloid causing swellings and Aβ production in neighboring axons. The rapid formation of neuritic plaques in just a few days, as observed by in vivo imaging studies of transgenic mice [71], indicates that a positive feedback mechanism is responsible for plaque formation. Moreover, the swelling of neurites in plaques recovers just as rapidly upon removal of extracellular amyloid [19, 71, 206], consistent with a restoration of axonal transport.
Intracellular amyloid accumulation
The implication is that dystrophic axons with localized accumulations of APP precede amyloid plaques, as observed [227]. However, as mentioned above, intraneuronal aggregations of Aβ in somata and axon initial segments also precede extracellular Aβ deposition [169]. What is the relationship between the Aβ formed in dystrophic neurites to that accumulating in the somata of neurons? One possibility is that neuronal cell bodies endocytose Aβ that has been released from nearby dystrophic axons. This is consistent with data showing that the intrasomal Aβ accumulation is cleared after immunotherapy removes extracellular deposits [172].
Another possibility is that intracellular Aβ production in dystrophic neurites contributes directly to accumulation in the cell body, by the retrograde transportation of autophagosomes formed in dystrophic neurites [297]. Such an explanation is more parsimonious than supposing that lysosomes migrate from somata to distal dystrophic neurites. This possibility is also supported by electron microscopic evidence that the clusters of lamellar bodies, normally found in axonal dystrophies where normal microtubule-based transport is disrupted, are also occasionally found nearby in the non-dystrophic part of the axon where retrograde transport is possible (e.g. Fig. 2b of [63]). Another interpretation of the finding that immunotherapy clears both plaques and intraneuronal Aβ [172], would be that removal of extracellular amyloid allows the recovery of dystrophic neurites (as shown in [19]) and so removes the intracellular source of Aβ from the lysosomal pathway.
Role of glia in plaque pathogenesis
The progressive deposition of amyloid from dystrophic neurites would activate glia to migrate into the developing plaque. As plaques accumulate extracellular amyloid, microglia invade the amyloid deposit and perhaps facilitate its compaction into a central mass by removing cellular debris. A plaque may stop growing when neighboring neurites are no longer easily disrupted by exposure to amyloid, due to enclosure of amyloid by glia and reduced exposure of healthy neurites to amyloid protofibrils. Amyloid plaques appear to be remarkably stable once mature [12, 36, 101, 145].
Astrocytes may participate in the removal of amyloid plaques, as evidenced by plaque-like regions of gliosis, 40–100 μm in diameter, with little extracellular amyloid and few dystrophic neurites. These “remnant” or “vanishing” plaques as they are sometimes called, are composed of numerous astrocytes with intracellular granules of Aβ immunoreactivity [68, 243, 246, 290]. They appear to be the final resolution of cored plaques because their density increases with disease duration in Alzheimer’s disease [175]. Because astrocytes accumulate Aβ in this manner during advanced stages of amyloid pathology, it has been further suggested that these Aβ-laden astrocytes might serve as secondary niduses for plaque formation by cell lysis [164, 165].
Relationship of dystrophic neurites to non-amyloid deposits
Each dystrophic neurite may experience a unique life history that depends, in part, on the accumulation and processing of amyloidogenic proteins. Many axons may swell but remain intact, while others may generate highly disruptive aggregates of Aβ. Dystrophic neurites accumulating non-fibrillogenic, but relatively insoluble, fragments of Aβ, may disgorge their contents without triggering additional neuritic degeneration, glial activation, or plaque growth. For example, a type of deposit known as a “cotton–wool plaque” is associated with particular presenilin-1 mutations that predispose neurons to produce amino-terminal truncated fragments of Aβ [128, 225]. Accumulations of amino-terminal truncated forms of Aβ have been seen in single dystrophic neurites scattered throughout the neuropil in Alzheimer’s disease [90], substantiating the idea that particular types of dystrophic neurites are niduses of non-amyloid deposits.
Relevance to other brain amyloid pathologies
Remarkably, the above synthesis appears to also account for the formation of amyloid plaques by the proteins involved in prion disease and in the familial British and Danish dementias. Like APP, prion protein is trafficked along the axon and accumulates in dystrophic neurites along with mitochondria and APP [16, 61, 140, 173]. The amyloidogenic proteins in familial British and Danish dementias show similar properties, including fast axonal transportation [35] and accumulation in dystrophic neurites [1]. Like Aβ protein, multimers of these other proteins are also toxic to neurons, possibly by acting as calcium ionophores that disrupt microtubules [57, 168]. Thus, amyloid plaques in a variety of diseases may be produced by dystrophic axons that accumulate amyloidogenic protein. This common mechanism of pathogenesis is supported by data showing that the different types of amyloidogenic proteins are often deposited together in plaques [61, 83, 159, 208, 249].
Amyloidogenic proteins subject to axonal trafficking may also be contributors to cerebral amyloid angiopathy. Axons appear to play a role in delivering the amyloid protein that leads to angiopathy, as mentioned above [25]. Whether some type of axonal secretion is involved remains unclear, but dystrophic swellings are found adjacent to the perivascular amyloid [25]. Amyloid angiopathy is also found in leptomeningeal vessels outside of the neuropil, which is much less likely to have a direct neuronal origin. Non-neuronal hypotheses for amyloid angiopathy include diffusion of Aβ along perivascular drainage pathways [274], microglial or smooth muscle production of amyloid [271, 272], and few others [23].
Conclusions
Amyloid deposits in the brain may be produced through multiple mechanisms (Fig. 2), but recent data support the intuitions of the early ultrastructural investigators that degenerating mitochondria in dystrophic axons are significant contributors to amyloid pathology. Rupture of a dystrophic neurite that contains amyloid protofibrils may seed a neuritic plaque, particularly when this occurs in a region dense with unmyelinated axons susceptible to further disruption by the deposited amyloid. Of course, secreted soluble Aβ might contribute to further plaque growth once a plaque is seeded [60], and some plaques may be seeded by lysis of cell bodies or other mechanisms. Further investigations into the processes of degeneration in dystrophic axons across the full spectrum of conditions exhibiting amyloid pathology are needed to fully explicate the role of this common aspect in the development and progression of disease.
References
Akiyama H, Kondo H, Arai T, Ikeda K, Kato M, Iseki E, Schwab C, McGeer PL (2004) Expression of BRI, the normal precursor of the amyloid protein of familial British dementia, in human brain. Acta Neuropathol (Berl) 107:53–58
Arendt T (2003) Synaptic plasticity and cell cycle activation in neurons are alternative effector pathways: the ‘Dr. Jekyll and Mr. Hyde concept’ of Alzheimer’s disease or the yin and yang of neuroplasticity. Prog Neurobiol 71:83–248
Arimon M, Diez-Perez I, Kogan MJ, Durany N, Giralt E, Sanz F, Fernandez-Busquets X (2006) Fine structure study of Aβ1–42 fibrillogenesis with atomic force microscopy. FASEB J 19:1344–1346
Armstrong RA (1995) Is the clustering of beta-amyloid (A beta) deposits in the frontal cortex of Alzheimer patients determined by blood vessels? Neurosci Lett 195:121–124
Armstrong RA (1998) Beta-amyloid plaques: stages in life history or independent origin? Dement Geriatr Cogn Disord 9:227–238
Armstrong RA (1999) Do beta-amyloid (Abeta) deposits in patients with Alzheimer’s disease and Down’s syndrome grow according to the log-normal model? Neurosci Lett 261:97–100
Attems J, Jellinger KA, Lintner F (2005) Alzheimer’s disease pathology influences severity and topographical distribution of cerebral amyloid angiopathy. Acta Neuropathol (Berl) 110:222–231
Attems J, Quass M, Jellinger KA, Lintner F (2007) Topographical distribution of cerebral amyloid angiopathy and its effect on cognitive decline are influenced by Alzheimer disease pathology. J Neurol Sci 257:49–55
Azizeh BY, Head E, Ibrahim MA, Torp R, Tenner AJ, Kim RC, Lott IT, Cotman CW (2000) Molecular dating of senile plaques in the brains of individuals with Down syndrome and in aged dogs. Exp Neurol 163:111–122
Baglioni S, Casamenti F, Bucciantini M, Luheshi LM, Taddei N, Chiti F, Dobson CM, Stefani M (2006) Prefibrillar amyloid aggregates could be generic toxins in higher organisms. J Neurosci 26:8160–8167
Baker HF, Ridley RM, Duchen LW, Crow TJ, Bruton CJ (1993) Experimental induction of beta-amyloid plaques and cerebral angiopathy in primates. Ann NY Acad Sci 695:228–231
Beer RE, Ulrich J (1993) Alzheimer plaque density and duration of dementia. Arch Gerontol Geriatr 16:1–7
Benes FM, Farol PA, Majocha RE, Marotta CA, Bird ED (1991) Evidence for axonal loss in regions occupied by senile plaques in Alzheimer cortex. Neuroscience 42:651–660
Benzing WC, Brady DR, Mufson EJ, Armstrong DM (1993) Evidence that transmitter-containing dystrophic neurites precede those containing paired helical filaments within senile plaques in the entorhinal cortex of nondemented elderly and Alzheimer’s disease patients. Brain Res 619:55–68
Blanchard V, Moussaoui S, Czech C, Touchet N, Bonici B, Planche M, Canton T, Jedidi I, Gohin M, Wirths O, Bayer TA, Langui D, Duyckaerts C, Tremp G, Pradier L (2003) Time sequence of maturation of dystrophic neurites associated with Abeta deposits in APP/PS1 transgenic mice. Exp Neurol 184(1):247–263
Borchelt DR, Koliatsos VE, Guarnieri M, Pardo CA, Sisodia SS, Price DL (1994) Rapid anterograde axonal transport of the cellular prion glycoprotein in the peripheral and central nervous systems. J Biol Chem 269:14711–14714
Boutajangout A, Authelet M, Blanchard V, Touchet N, Tremp G, Pradier L, Brion JP (2004) Characterisation of cytoskeletal abnormalities in mice transgenic for wild-type human tau and familial Alzheimer’s disease mutants of APP and presenilin-1. Neurobiol Dis 15:47–60
Brendza RP, O’Brien C, Simmons K, McKeel DW, Bales KR, Paul SM, Olney JW, Sanes JR, Holtzman DM (2003) PDAPP, YFP double transgenic mice: a tool to study amyloid-beta associated changes in axonal, dendritic, and synaptic structures. J Comp Neurol 456:375–383
Brendza RP, Bacskai BJ, Cirrito JR, Simmons KA, Skoch JM, Klunk WE, Mathis CA, Bales KR, Paul SM, Hyman BT, Holtzman DM (2005) Anti-Abeta antibody treatment promotes the rapid recovery of amyloid-associated neuritic dystrophy in PDAPP transgenic mice. J Clin Invest 115:428–433
Brunk UT, Terman A (2002) The mitochondrial–lysosomal axis theory of aging: accumulation of damaged mitochondria as a result of imperfect autophagocytosis. Eur J Biochem 269:1996–2002
Busciglio J, Hartmann H, Lorenzo A, Wong C, Baumann K, Sommer B, Staufenbiel M, Yankner BA (1997) Neuronal localization of presenilin-1 and association with amyloid plaques and neurofibrillary tangles in Alzheimer’s disease. J Neurosci 17:5101–5107
Büki A, Povlishock JT (2006) All roads lead to disconnection? Traumatic axonal injury revisited. Acta Neurochir (Wien) 148:181–194
Burgermeister P, Calhoun ME, Winkler DT, Jucker M (2000) Mechanisms of cerebrovascular amyloid deposition. Lessons from mouse models. Ann NY Acad Sci 903:307–316
Bussiere T, Bard F, Barbour R, Grajeda H, Guido T, Khan K, Schenk D, Games D, Seubert P, Buttini M (2004) Morphological characterization of Thioflavin-S-positive amyloid plaques in transgenic Alzheimer mice and effect of passive Abeta immunotherapy on their clearance. Am J Pathol 165(3):987–995
Calhoun ME, Burgermeister P, Phinney AL, Stalder M, Tolnay M, Wiederhold KH, Abramowski D, Sturchler-Pierrat C, Sommer B, Staufenbiel M, Jucker M (1999) Neuronal overexpression of mutant amyloid precursor protein results in prominent deposition of cerebrovascular amyloid. Proc Natl Acad Sci USA 96:14088–14093
Casal C, Serratosa J, Tusell JM (2002) Relationship between beta-AP peptide aggregation and microglial activation. Brain Res 928:76–84
Caspersen C, Wang N, Yao J, Sosunov A, Chen X, Lustbader JW, Xu HW, Stern D, McKhann G, Yan SD (2005) Mitochondrial Aβ: a potential focal point for neuronal metabolic dysfunction in Alzheimer’s disease. FASEB J 19:2040–2041
Cataldo AM, Barnett JL, Mann DM, Nixon RA (1996) Colocalization of lysosomal hydrolase and beta-amyloid in diffuse plaques of the cerebellum and striatum in Alzheimer’s disease and Down’s syndrome. J Neuropathol Exp Neurol 55:704–715
Cataldo AM, Hamilton DJ, Barnett JL, Paskevich PA, Nixon RA (1996) Properties of the endosomal–lysosomal system in the human central nervous system: disturbances mark most neurons in populations at risk to degenerate in Alzheimer’s disease. J Neurosci 16:186–199
Cataldo AM, Thayer CY, Bird ED, Wheelock TR, Nixon RA (1990) Lysosomal proteinase antigens are prominently localized within senile plaques of Alzheimer’s disease: evidence for a neuronal origin. Brain Res 513:181–192
Caughey B, Lansbury PT Jr (2003) Protofibrils, pores, fibrils, and neurodegeneration: separating the responsible protein aggregates from the innocent bystanders. Ann Rev Neurosci 26:267–298
Chen GJ, Xu J, Lahousse SA, Caggiano NL, de la Monte SM (2003) Transient hypoxia causes Alzheimer-type molecular and biochemical abnormalities in cortical neurons: potential strategies for neuroprotection. J Alzheimers Dis 5:209–228
Chen X-H, Meaney DF, Xu B-N, Nonaka M, McIntosh TK, Wolf JA, Saatman KE, Smith DH (1999) Evolution of neurofilament subtype accumulation in axons following diffuse brain injury in the pig. J Neuropathol Exp Neurol 58:588–596
Chen XH, Siman R, Iwata A, Meaney DF, Trojanowski JQ, Smith DH (2004) Long-term accumulation of amyloid-beta, beta-secretase, presenilin-1, and caspase-3 in damaged axons following brain trauma. Am J Pathol 165:357–371
Choi SI, Vidal R, Frangione B, Levy E (2004) Axonal transport of British and Danish amyloid peptides via secretory vesicles. FASEB J 18:373–375
Christie RH, Bacskai BJ, Zipfel WR, Williams RM, Kajdasz ST, Webb WW, Hyman BT (2001) Growth arrest of individual senile plaques in a model of Alzheimer’s disease observed by in vivo multiphoton microscopy. J Neurosci 21(3):858–864
Cirrito JR, May PC, O’Dell MA, Taylor JW, Parsadanian M, Cramer JW, Audia JE, Nissen JS, Bales KR, Paul SM, DeMattos RB, Holtzman DM (2003) In vivo assessment of brain interstitial fluid with microdialysis reveals plaque-associated changes in amyloid-beta metabolism and half-life. J Neurosci 23:8844–8853
Cirrito JR, Yamada KA, Finn MB, Sloviter RS, Bales KR, May PC, Schoepp DD, Paul SM, Mennerick S, Holtzman DM (2005) Synaptic activity regulates interstitial fluid amyloid-beta levels in vivo. Neuron 48:913–922
Cleary JP, Walsh DM, Hofmeister JJ, Shankar GM, Kuskowski MA, Selkoe DJ, Ashe KH (2005) Natural oligomers of the amyloid-beta protein specifically disrupt cognitive function. Nat Neurosci 8:79–84
Coleman M (2005) Axon degeneration mechanisms: commonality amid diversity. Nat Rev Neurosci 6:889–898
Cras P, Kawai M, Lowery D, Gonzalez-DeWhitt P, Greenberg B, Perry G (1991) Senile plaque neurites in Alzheimer disease accumulate amyloid precursor protein. Proc Natl Acad Sci USA 88:7552–7556
Cras P, Kawai M, Siedlak S, Mulvihill P, Gambetti P, Lowery D, Gonzalez-DeWhitt P, Greenberg B, Perry G (1990) Neuronal and microglial involvement in beta-amyloid protein deposition in Alzheimer’s disease. Am J Pathol 137:241–246
Cummings BJ, Su JH, Cotman CW, White R, Russell MJ (1993) Beta-amyloid accumulation in aged canine brain: a model of early plaque formation in Alzheimer’s disease. Neurobiol Aging 14:547–560
Cummings BJ, Su JH, Geddes JW, Van Nostrand WE, Wagner SL, Cunningham DD, Cotman CW (1992) Aggregation of the amyloid precursor protein within degenerating neurons and dystrophic neurites in Alzheimer’s disease. Neuroscience 48:763–777
Dahlgren KN, Manelli AM, Stine WB Jr, Baker LK, Krafft GA, LaDu MJ (2002) Oligomeric and fibrillar species of amyloid-beta peptides differentially affect neuronal viability. J Biol Chem 277:32046–32053
D’Andrea MR, Nagele RG, Wang H-Y, Peterson PA, Lee DHS (2001) Evidence that neurons accumulating amyloid can undergo lysis to form amyloid plaques in Alzheimer’s disease. Histopathology 38:120–134
D’Andrea MR, Reiser PA, Gumula NA, Hertzog BM, Andrade-Gordon P (2001) Application of triple immunohistochemistry to characterize amyloid plaque-associated inflammation in brains with Alzheimer’s disease. Biotech Histochem 76:97–106
D’Andrea MR, Reiser PA, Polkovitch DA, Gumula NA, Branchide B, Hertzog BM, Schmidheiser D, Belkowski S, Gastard MC, Andrade-Gordon P (2003) The use of formic acid to embellish amyloid plaque detection in Alzheimer’s disease tissues misguides key observations. Neurosci Lett 342:114–118
Davies CA, Mann DM (1993) Is the “preamyloid” of diffuse plaques in Alzheimer’s disease really nonfibrillar? Am J Pathol 143(6):1594–1605
Devi L, Prabhu BM, Galati DF, Avadhani NG, Anandatheerthavarada HK (2006) Accumulation of amyloid precursor protein in the mitochondrial import channels of human Alzheimer’s disease brain is associated with mitochondrial dysfunction. J Neurosci 26:9057–9068
DeWitt DA, Perry G, Cohen M, Doller C, Silver J (1998) Astrocytes regulate microglial phagocytosis of senile plaque cores of Alzheimer’s disease. Exp Neurol 149:329–340
DeWitt DA, Silver J (1996) Regenerative failure: a potential mechanism for neuritic dystrophy in Alzheimer’s disease. Exp Neurol 142:103–110
Dickson DW (1997) The pathogenesis of senile plaques. J Neuropathol Exp Neurol 56:321–339
Dickson TC, Vickers JC (2001) The morphological phenotype of beta-amyloid plaques and associated neuritic changes in Alzheimer’s disease. Neuroscience 105:99–107
Ditaranto K, Tekirian TL, Yang AJ (2001) Lysosomal membrane damage in soluble Abeta-mediated cell death in Alzheimer’s disease. Neurobiol Dis 8:19–31
Donahue JE, Flaherty SL, Johanson CE, Duncan JA 3rd, Silverberg GD, Miller MC, Tavares R, Yang W, Wu Q, Sabo E, Hovanesian V, Stopa EG (2006) RAGE, LRP-1, and amyloid-beta protein in Alzheimer’s disease. Acta Neuropathol (Berl) 112:405–415
El-Agnaf O, Gibson G, Lee M, Wright A, Austen BM (2004) Properties of neurotoxic peptides related to the Bri gene. Protein Pept Lett 11:207–212
Elfenbein HA, Rosen RF, Stephens SL, Switzer RC, Smith Y, Pare J, Mehta PD, Warzok R, Walker LC (2007) Cerebral beta-amyloid angiopathy in aged squirrel monkeys. Histol Histopathol 22:155–167
El Khoury J, Toft M, Hickman SE, Means TK, Terada K, Geula C, Luster AD (2007) CCR2 deficiency impairs microglial accumulation and accelerates progression of Alzheimer-like disease. Nat Med 13:432–438
Esler WP, Stimson ER, Ghilardi JR, Vinters HV, Lee JP, Mantyh PW, Maggio JE (1996) In vitro growth of Alzheimer’s disease beta-amyloid plaques displays first-order kinetics. Biochemistry 35:749–757
Ferrer I, Blanco R, Carmona M, Puig B, Ribera R, Rey MJ, Ribalta T (2001) Prion protein expression in senile plaques in Alzheimer’s disease. Acta Neuropathol (Berl) 101:49–56
Ferrer I, Marti E, Tortosa A, Blasi J (1998) Dystrophic neurites of senile plaques are defective in proteins involved in exocytosis and neurotransmission. J Neuropathol Exp Neurol 57(3):218–225
Fiala JC, Feinberg MD, Peters A, Barbas H (2007) Mitochondrial degeneration in dystrophic neurites of senile plaques may lead to extracellular deposition of fine filaments. Brain Struct Funct doi:10.1007/s00429-007-0153-1
Fiala JC, Kirov SA, Feinberg MD, Petrak LJ, George P, Goddard CA, Harris KM (2003) Timing of neuronal and glial ultrastructure disruption during brain slice preparation and recovery in vitro. J Comp Neurol 465:90–103
Fonseca MI, Head E, Velazquez P, Cotman CW, Tenner AJ (1999) The presence of isoaspartic acid in beta-amyloid plaques indicates plaque age. Exp Neurol 157:277–288
Frackowiak J, Wisniewski HM, Wegiel J, Merz GS, Iqbal K, Wang KC (1992) Ultrastructure of the microglia that phagocytose amyloid and the microglia that produce beta-amyloid fibrils. Acta Neuropathol (Berl) 84(3):225–233
Fraser PE, Levesque L, McLachlan DR (1994) Alzheimer A beta amyloid forms an inhibitory neuronal substrate. J Neurochem 62:1227–1230
Funato H, Yoshimura M, Yamazaki T, Saido TC, Ito Y, Yokofujita J, Okeda R, Ihara Y (1998) Astrocytes containing amyloid beta-protein (Abeta)-positive granules are associated with Abeta40-positive diffuse plaques in the aged human brain. Am J Pathol 152:983–992
Gajdusek DC (1985) Hypothesis: interference with axonal transport of neurofilament as a common pathogenetic mechanism in certain diseases of the central nervous system. N Engl J Med 312:714–719
Games D, Buttini M, Kobayashi D, Schenk D, Seubert P (2006) Mice as models: transgenic approaches and Alzheimer’s disease. J Alzheimers Dis 9(3 Suppl):133–149
Garcia-Alloza M, Borrelli LA, Rozkalne A, Hyman BT, Bacskai BJ (2007) Curcumin labels amyloid pathology in vivo, disrupts existing plaques, and partially restores distorted neurites in an Alzheimer mouse model. J Neurochem doi:10.1111/j.1471–4159.2007.04613.x
Giannakopoulos P, Hof PR, Michel JP, Guimon J, Bouras C (1997) Cerebral cortex pathology in aging and Alzheimer’s disease: a quantitative survey of large hospital-based geriatric and psychiatric cohorts. Brain Res Rev 25(2):217–245
Ginsberg SD, Crino PB, Hemby SE, Weingarten JA, Lee VM, Eberwine JH, Trojanowski JQ (1999) Predominance of neuronal mRNAs in individual Alzheimer’s disease senile plaques. Ann Neurol 45:174–181
Glabe C (2001) Intracellular mechanisms of amyloid accumulation and pathogenesis in Alzheimer’s disease. J Mol Neurosci 17:137–145
Gonatas NK, Anderson W, Evangelista I (1967) The contribution of altered synapses in the senile plaque: an electron microscopic study in Alzheimer’s dementia. J Neuropathol Exp Neurol 26(1):25–39
Gordon MN, Holcomb LA, Jantzen PT, DiCarlo G, Wilcock D, Boyett KW, Connor K, Melachrino J, O’Callaghan JP, Morgan D (2002) Time course of the development of Alzheimer-like pathology in the doubly transgenic PS1+APP mouse. Exp Neurol 173:183–195
Götz J, Ittner LM, Kins S (2006) Do axonal defects in tau and amyloid precursor protein transgenic animals model axonopathy in Alzheimer’s disease? J Neurochem 98:993–1106
Gouras GK, Almeida CG, Takahashi RH (2005) Intraneuronal Aβ accumulation and origin of plaques in Alzheimer’s disease. Neurobiol Aging 26:1235–1244
Gouras GK, Tsai J, Naslund J, Vincent B, Edgar M, Checler F, Greenfield JP, Haroutunian V, Buxbaum JD, Xu H, Greengard P, Relkin NR (2000) Intraneuronal Abeta42 accumulation in human brain. Am J Pathol 156:15–20
Gowing E, Roher AE, Woods AS, Cotter RJ, Chaney M, Little SP, Ball MJ (1994) Chemical characterization of Abeta 17–42 peptide, a component of diffuse amyloid deposits of Alzheimer disease. J Biol Chem 269:10987–10990
Grutzendler J, Helmin K, Tsai J, Gan WB (2007) Various dendritic abnormalities are associated with fibrillar amyloid deposits in Alzheimer’s disease. Ann NY Acad Sci 1097:30–39
Gyure KA, Durham R, Stewart WF, Smialek JE, Troncoso JC (2001) Intraneuronal abeta-amyloid precedes development of amyloid plaques in Down syndrome. Arch Pathol Lab Med 125:489–492
Hainfellner JA, Wanschitz J, Jellinger K, Liberski PP, Gullotta F, Budka H (1998) Coexistence of Alzheimer-type neuropathology in Creutzfeldt–Jakob disease. Acta Neuropathol (Berl) 96:116–122
Hansson CA, Frykman S, Farmery MR, Tjernberg LO, Nilsberth C, Pursglove SE, Ito A, Winblad B, Cowburn RF, Thyberg J, Ankarcrona M (2004) Nicastrin, presenilin, APH-1, and PEN-2 form active gamma-secretase complexes in mitochondria. J Biol Chem 279:51654–51660
Harigaya Y, Tomidokoro Y, Ikeda M, Sasaki A, Kawarabayashi T, Matsubara E, Kanai M, Saido TC, Younkin SG, Shoji M (2006) Type-specific evolution of amyloid plaque and angiopathy in APPsw mice. Neurosci Lett 395:37–41
Hartmann T, Bieger SC, Bruhl B, Tienari PJ, Ida N, Allsop D, Roberts GW, Masters CL, Dotti CG, Unsicker K, Beyreuther K (1997) Distinct sites of intracellular production for Alzheimer’s disease Abeta40/42 amyloid peptides. Nat Med 3:1016–1020
Head E, Azizeh BY, Lott IT, Tenner AJ, Cotman CW, Cribbs DH (2001) Complement association with neurons and beta-amyloid deposition in the brains of aged individuals with Down Syndrome. Neurobiol Dis 8:252–265
Heneka MT, Sastre M, Dumitrescu-Ozimek L, Dewachter I, Walter J, Klockgether T, Van Leuven F (2005) Focal glial activation coincides with increased BACE1 activation and precedes amyloid plaque deposition in APP[V717I] transgenic mice. J Neuroinflammation 2:22
Higgins LS, Holtzman DM, Rabin J, Mobley WC, Cordell B (1994) Transgenic mouse brain histopathology resembles early Alzheimer’s disease. Ann Neurol 35:598–607
Higgins LS, Murphy GM Jr, Forno LS, Catalano R, Cordell B (1996) P3 beta-amyloid peptide has a unique and potentially pathogenic immunohistochemical profile in Alzheimer’s disease brain. Am J Pathol 149:585–596
Hirayama A, Horikoshi Y, Maeda M, Ito M, Takashima S (2003) Characteristic developmental expression of amyloid beta40, 42 and 43 in patients with Down syndrome. Brain Dev 25:180–185
Hiruma H, Katakura T, Takahashi S, Ichikawa T, Kawakami T (2003) Glutamate and amyloid beta-protein rapidly inhibit fast axonal transport in cultured rat hippocampal neurons by different mechanisms. J Neurosci 23:8967–8677
Hiruma H, Nishida S, Katakura T, Kusakabe T, Takenaka T, Kawakami T (1999) Extracellular potassium rapidly inhibits axonal transport of particles in cultured mouse dorsal root ganglion neurites. J Neurobiol 38:225–233
Hollenbeck PJ (1993) Products of endocytosis and autophagy are retrieved from axons by regulated retrograde organelle transport. J Cell Biol 121:305–315
Horie H, Takenaka T, Kaiho M (1983) Effects of disruption of microtubules on translocation of particles and morphology in tissue cultured neurites. Brain Res 288:85–93
Hyman BT, West HL, Rebeck GW, Lai F, Mann DM (1995) Neuropathological changes in Down’s syndrome hippocampal formation. Effect of age and apolipoprotein E genotype. Arch Neurol 52:373–378
Ikonomovic MD, Uryu K, Abrahamson EE, Ciallella JR, Trojanowski JQ, Lee VM, Clark RS, Marion DW, Wisniewski SR, DeKosky ST (2004) Alzheimer’s pathology in human temporal cortex surgically excised after severe brain injury. Exp Neurol 190:192–203
Isobe I, Yanagisawa K, Michikawa M (2000) A possible model of senile plaques using synthetic amyloid beta-protein and rat glial culture. Exp Neurol 162:51–60
Ivins KJ, Bui ET, Cotman CW (1998) Beta-amyloid induces local neurite degeneration in cultured hippocampal neurons: evidence for neuritic apoptosis. Neurobiol Dis 5:365–378
Iwatsubo T, Saido TC, Mann DM, Lee VM, Trojanowski JQ (1996) Full-length amyloid-beta (1–42(43)) and amino-terminally modified and truncated amyloid-beta 42(43) deposit in diffuse plaques. Am J Pathol 149:1823–1830
Jankowsky JL, Slunt HH, Gonzales V, Savonenko AV, Wen JC, Jenkins NA, Copeland NG, Younkin LH, Lester HA, Younkin SG, Borchelt DR (2005) Persistent amyloidosis following suppression of Abeta production in a transgenic model of Alzheimer disease. PLoS Med 2:e355
Jeffrey M, Goodsir CM, Bruce ME, McBride PA, Farquhar C (1994) Morphogenesis of amyloid plaques in 87V murine scrapie. Neuropathol Appl Neurobiol 20:535–542
Jellinger K (1973) Neuroaxonal dystrophy: its natural history and related disorders. In: Zimmerman HM (ed) Progress in neuropathology. vol. II. Grune & Stratton, New York, pp 129–180
Jendroska K, Poewe W, Daniel SE, Pluess J, Iwerssen-Schmidt H, Paulsen J, Barthel S, Schelosky L, Cervos-Navarro J, DeArmond SJ (1995) Ischemic stress induces deposition of amyloid beta immunoreactivity in human brain. Acta Neuropathol (Berl) 90:461–466
Jeynes B, Provias J (2006) The possible role of capillary cerebral amyloid angiopathy in Alzheimer lesion development: a regional comparison. Acta Neuropathol (Berl) 112:417–427
Joachim CL, Morris JH, Selkoe DJ (1989) Diffuse senile plaques occur commonly in the cerebellum in Alzheimer’s disease. Am J Pathol 135:309–319
Jordan BD (2000) Chronic traumatic brain injury associated with boxing. Semin Neurol 20:179–185
Kamal A, Almenar-Queralt A, LeBlanc JF, Roberts EA, Goldstein LSB (2001) Kinesin-mediated axonal transport of a membrane compartment containing secretase and presenilin-1 requires APP. Nature 414:643–648
Kane MD, Lipinski WJ, Callahan MJ, Bian F, Durham RA, Schwarz RD, Roher AE, Walker LC (2000) Evidence for seeding of beta-amyloid by intracerebral infusion of Alzheimer brain extracts in beta-amyloid precursor protein-transgenic mice. J Neurosci 20:3606–3611
Kato S, Gondo T, Hoshii Y, Takahashi M, Yamada M, Ishihara T (1998) Confocal observation of senile plaques in Alzheimer’s disease: senile plaque morphology and relationship between senile plaques and astrocytes. Pathol Int 48:332–340
Kawai M, Cras P, Perry G (1992) Serial reconstruction of beta-protein amyloid plaques: relationship to microvessels and size distribution. Brain Res 592:278–282
Kawai M, Cras P, Richey P, Tabaton M, Lowery DE, Gonzalez-DeWhitt PA, Greenberg BD, Gambetti P, Perry G (1992) Subcellular localization of amyloid precursor protein in senile plaques of Alzheimer’s disease. Am J Pathol 140:947–958
Kawarabayashi T, Shoji M, Yamaguchi H, Tanaka M, Harigaya Y, Ishiguro K, Hirai S (1993) Amyloid beta protein precursor accumulates in swollen neurites throughout rat brain with aging. Neurosci Lett 153:73–76
Kawarabayashi T, Younkin LH, Saido TC, Shoji M, Ashe KH, Younkin SG (2001) Age-dependent changes in brain, CSF, and plasma amyloid (beta) protein in the Tg2576 transgenic mouse model of Alzheimer’s disease. J Neurosci 21:372–381
Kidd M (1964) Alzheimer’s disease: an electron microscopical study. Brain 87:307–320
Kim I, Rodriguez-Enriquez S, Lemasters JJ (2007) Selective degradation of mitochondria by mitophagy. Arch Biochem Biophys 462:245–253
King CE, Adlard PA, Dickson TC, Vickers JC (2000) Neuronal response to physical injury and its relationship to the pathology of Alzheimer’s disease. Clin Exp Pharmacol Physiol 27:548–552
Kitamoto T, Ogomori K, Tateishi J, Prusiner SB (1987) Formic acid pretreatment enhances immunostaining of cerebral and systemic amyloids. Lab Invest 57:230–236
Knauer MF, Soreghan B, Burdick D, Kosmoski J, Glabe CG (1992) Intracellular accumulation and resistance to degradation of the Alzheimer amyloid A4/beta protein. Proc Natl Acad Sci USA 89:7437–7441
Kokubo H, Kayed R, Glabe CG, Saido TC, Iwata N, Helms JB, Yamaguchi H (2005) Oligomeric proteins ultrastructurally localize to cell processes, especially to axon terminals with higher density, but not to lipid rafts in Tg2576 mouse brain. Brain Res 1045:224–228
Kokubo H, Kayed R, Glabe CG, Yamaguchi H (2005) Soluble Abeta oligomers ultrastructurally localize to cell processes and might be related to synaptic dysfunction in Alzheimer’s disease brain. Brain Res 1031:222–228
Kokubo H, Saido TC, Iwata N, Helms JB, Shinohara R, Yamaguchi H (2005) Part of membrane-bound Abeta exists in rafts within senile plaques in Tg2576 mouse brain. Neurobiol Aging 26:409–418
Koo EH, Sisodia SS, Archer DR, Martin LJ, Weidemann A, Beyreuther K, Fischer P, Masters CL, Price DL (1990) Precursor of amyloid protein in Alzheimer disease undergoes fast anterograde axonal transport. Proc Natl Acad Sci USA 87:1561–1565
Kovacs DM, Fausett HJ, Page KJ, Kim TW, Moir RD, Merriam DE, Hollister RD, Hallmark OG, Mancini R, Felsenstein KM, Hyman BT, Tanzi RE, Wasco W (1996) Alzheimer-associated presenilins 1 and 2: neuronal expression in brain and localization to intracellular membranes in mammalian cells. Nat Med 2:224–229
Krigman MR, Feldman RG, Bensch K (1965) Alzheimer’s presenile dementia: a histochemical and electron microscopic study. Lab Invest 14:381–396
Kumar-Singh S, Cras P, Wang R, Kros JM, van Swieten J, Lubke U, Ceuterick C, Serneels S, Vennekens K, Timmermans JP, Van Marck E, Martin JJ, van Duijn CM, Van Broeckhoven C (2002) Dense-core senile plaques in the Flemish variant of Alzheimer’s disease are vasocentric. Am J Pathol 161:507–520
Kumar-Singh S, Pirici D, McGowan E, Serneels S, Ceuterick C, Hardy J, Duff K, Dickson D, Van Broeckhoven C (2005) Dense-core plaques in Tg2576 and PSAPP mouse models of Alzheimer’s disease are centered on vessel walls. Am J Pathol 167:527–543
Kwok JB, Halliday GM, Brooks WS, Dolios G, Laudon H, Murayama O, Hallupp M, Badenhop RF, Vickers J, Wang R, Naslund J, Takashima A, Gandy SE, Schofield PR (2003) Presenilin-1 mutation L271V results in altered exon 8 splicing and Alzheimer’s disease with non-cored plaques and no neuritic dystrophy. J Biol Chem 278:6748–6754
LaFerla FM, Green KN, Oddo S (2007) Intracellular amyloid-beta in Alzheimer’s disease. Nat Rev Neurosci 8:499–509
LaFerla FM, Tinkle BT, Bieberich CJ, Haudenschild CC, Jay G (1995) The Alzheimer’s Abeta peptide induces neurodegeneration and apoptotic cell death in transgenic mice. Nat Genet 9:21–30
Lalowski M, Golabek A, Lemere CA, Selkoe DJ, Wisniewski HM, Beavis RC, Frangione B, Wisniewski T (1996) The “nonamyloidogenic” p3 fragment (amyloid beta17–42) is a major constituent of Down’s syndrome cerebellar preamyloid. J Biol Chem 271:33623–33631
Lambert MP, Barlow AK, Chromy BA, Edwards C, Freed R, Liosatos M, Morgan TE, Rozovsky I, Trommer B, Viola KL, Wals P, Zhang C, Finch CE, Krafft GA, Klein WL (1998) Diffusible, nonfibrillar ligands derived from Abeta1–42 are potent central nervous system neurotoxins. Proc Natl Acad Sci USA 95:6448–6453
Lampert PW (1967) A comparative electron microscopic study of reactive, degenerating, regenerating, and dystrophic axons. J Neuropathol Exp Neurol 26:345–368
Lampert PW (1971) Fine structural changes of neurites in Alzheimer’s disease. Acta Neuropathol (Berl.) Suppl. V:49–53
Lazarov O, Lee M, Peterson DA, Sisodia SS (2002) Evidence that synaptically released beta-amyloid accumulates as extracellular deposits in the hippocampus of transgenic mice. J Neurosci 22:9785–9793
Lemere CA, Blusztajn JK, Yamaguchi H, Wisniewski T, Saido TC, Selkoe DJ (1996) Sequence of deposition of heterogeneous amyloid beta-peptides and APO E in Down syndrome: implications for initial events in amyloid plaque formation. Neurobiol Dis 3:16–32
Lesne S, Koh MT, Kotilinek L, Kayed R, Glabe CG, Yang A, Gallagher M, Ashe KH (2006) A specific amyloid-beta protein assembly in the brain impairs memory. Nature 440:352–357
Liao L, Cheng D, Wang J, Duong DM, Losik TG, Gearing M, Rees HD, Lah JJ, Levey AI, Peng J (2004) Proteomic characterization of postmortem amyloid plaques isolated by laser capture microdissection. J Biol Chem 279:37061–37068
Liberski PP (2004) Amyloid plaques in transmissible spongiform encephalopathies (prion diseases). Folia Neuropathol 42(Suppl B):109–119
Liberski PP, Yanagihara R, Gibbs CJ Jr, Gajdusek DC (1989) Scrapie as a model for neuroaxonal dystrophy: ultrastructural studies. Exp Neurol 106:133–141
Lin H, Bhatia R, Lal R (2001) Amyloid β protein forms ion channels: implications for Alzheimer’s disease pathophysiology. FASEB J 15:2433–2444
Lorenzo A, Yankner BA (1994) Beta-amyloid neurotoxicity requires fibril formation and is inhibited by congo red. Proc Natl Acad Sci USA 91:12243–12247
Luse SA, Smith KR Jr (1964) The ultrastructure of senile plaques. Am J Pathol 44:553–563
Lustbader JW, Cirilli M, Lin C, Xu HW, Takuma K, Wang N, Caspersen C, Chen X, Pollack S, Chaney M, Trinchese F, Liu S, Gunn-Moore F, Lue L-F, Walker DG, Kuppusamy P, Zewier ZL, Arancio O, Stern D, Yan SS, Wu H (2004) ABAD directly links Aβ to mitochondrial toxicity in Alzheimer’s disease. Science 304:448–452
Mackenzie IR (1994) Senile plaques do not progressively accumulate with normal aging. Acta Neuropathol (Berl) 87:520–525
Manczak M, Anekonda TS, Henson E, Park BS, Quinn J, Reddy PH (2006) Mitochondria are a direct site of Aβ accumulation in Alzheimer’s disease neurons: implications for free radical generation and oxidative damage in disease progression. Human Mol Genet 15:1437–1449
Mann DM, Iwatsubo T (1996) Diffuse plaques in the cerebellum and corpus striatum in Down’s syndrome contain amyloid beta protein (Abeta) only in the form of Abeta 42(43). Neurodegeneration 5:115–120
Martin LJ, Pardo CA, Cork LC, Price DL (1994) Synaptic pathology and glial responses to neuronal injury precede the formation of senile plaques and amyloid deposits in the aging cerebral cortex. Am J Pathol 145:1358–1381
Martin LJ, Sisodia SS, Koo EH, Cork LC, Dellovade TL, Weidemann A, Beyreuther K, Masters C, Price DL (1991) Amyloid precursor protein in aged nonhuman primates. Proc Natl Acad Sci USA 88:1461–1465
Masliah E, Mallory M, Deerinck T, DeTeresa R, Lamont S, Miller A, Terry RD, Carragher B, Ellisman M (1993) Re-evaluation of the structural organization of neuritic plaques in Alzheimer’s disease. J Neuropathol Exp Neurol 52:619–632
Masliah E, Miller A, Terry RD (1993) The synaptic organization of the neocortex in Alzheimer’s disease. Med Hypoth 41:334–340
Masters CL, Simms G, Weinman NA, Multhaup G, McDonald BL, Beyreuther K (1985) Amyloid plaque core protein in Alzheimer disease and Down syndrome. Proc Natl Acad Sci USA 82:4245–4249
McGeer PL, Akiyama H, Kawamata T, Yamada T, Walker DG, Ishii T (1992) Immunohistochemical localization of beta-amyloid precursor protein sequences in Alzheimer and normal brain tissue by light and electron microscopy. J Neurosci Res 31:428–442
McGowan E, Pickford F, Kim J, Onstead L, Eriksen J, Yu C, Skipper L, Murphy MP, Beard J, Das P, Jansen K, Delucia M, Lin WL, Dolios G, Wang R, Eckman CB, Dickson DW, Hutton M, Hardy J, Golde T (2005) Abeta42 is essential for parenchymal and vascular amyloid deposition in mice. Neuron 47:191–199
McGowan E, Sanders S, Iwatsubo T, Takeuchi A, Saido T, Zehr C, Yu X, Uljon S, Wang R, Mann D, Dickson D, Duff K (1999) Amyloid phenotype characterization of transgenic mice overexpressing both mutant amyloid precursor protein and mutant presenilin 1 transgenes. Neurobiol Dis 6:231–244
Meyer-Luehmann M, Coomaraswamy J, Bolmont T, Kaeser S, Schaefer C, Kilger E, Neuenschwander A, Abramowski D, Frey P, Jaton AL, Vigouret JM, Paganetti P, Walsh DM, Mathews PM, Ghiso J, Staufenbiel M, Walker LC, Jucker M (2006) Exogenous induction of cerebral beta-amyloidogenesis is governed by agent and host. Science 313:1781–1784
Meyer-Luehmann M, Stalder M, Herzig MC, Kaeser SA, Kohler E, Pfeifer M, Boncristiano S, Mathews PM, Mercken M, Abramowski D, Staufenbiel M, Jucker M (2003) Extracellular amyloid formation and associated pathology in neural grafts. Nat Neurosci 6:370–377
Miravalle L, Calero M, Takao M, Roher AE, Ghetti B, Vidal R (2005) Amino-terminally truncated Abeta peptide species are the main component of cotton wool plaques. Biochemistry 44:10810–10821
Miyazono M, Kitamoto T, Iwaki T, Tateishi J (1992) Colocalization of prion protein and beta protein in the same amyloid plaques in patients with Gerstmann-Straussler syndrome. Acta Neuropathol (Berl) 83:333–339
Mochizuki A, Peterson JW, Mufson EJ, Trapp BD (1996) Amyloid load and neural elements in Alzheimer’s disease and nondemented individuals with high amyloid plaque density. Exp Neurol 142:89–102
Moreira PI, Siedlak SL, Wang X, Santos MS, Oliveira CR, Tabaton M, Nunomura A, Szweda LI, Aliev G, Smith MA, Zhu X, Perry G (2007) Autophagocytosis of Mitochondria Is Prominent in Alzheimer Disease. J Neuropathol Exp Neurol 66:525–532
Mori C, Spooner ET, Wisniewsk KE, Wisniewski TM, Yamaguch H, Saido TC, Tolan DR, Selkoe DJ, Lemere CA (2002) Intraneuronal Abeta42 accumulation in Down syndrome brain. Amyloid 9:88–102
Mukaetova-Ladinska EB, Garcia-Siera F, Hurt J, Gertz HJ, Xuereb JH, Hills R, Brayne C, Huppert FA, Paykel ES, McGee M, Jakes R, Honer WG, Harrington CR, Wischik CM (2000) Staging of cytoskeletal and beta-amyloid changes in human isocortex reveals biphasic synaptic protein response during progression of Alzheimer’s disease. Am J Pathol 157:623–636
Nagele RG, D’Andrea MR, Lee H, Venkataraman V, Wang HY (2003) Astrocytes accumulate Abeta 42 and give rise to astrocytic amyloid plaques in Alzheimer disease brains. Brain Res 971:197–209
Nagele RG, Wegiel J, Venkataraman V, Imaki H, Wang KC, Wegiel J (2004) Contribution of glial cells to the development of amyloid plaques in Alzheimer’s disease. Neurobiol Aging 25:663–674
Nixon RA, Cataldo AM (2006) Lysosomal system pathways: genes to neurodegeneration in Alzheimer’s disease. J Alzheimer Dis 9:277–289
Nixon RA, Wegiel J, Kumar A, Yu WH, Peterhoff C, Cataldo A, Cuervo AM (2005) Extensive involvement of autophagy in Alzheimer disease: an immuno-electron microscopy study. J Neuropathol Exp Neurol 64:113–122
Novitskaya V, Bocharova OV, Bronstein I, Baskakov IV (2006) Amyloid fibrils of mammalian prion protein are highly toxic to cultured cells and primary neurons. J Biol Chem 281:13828–13836
Oakley H, Cole SL, Logan S, Maus E, Shao P, Craft J, Guillozet-Bongaarts A, Ohno M, Disterhoft J, Eldik LV, Berry R, Vassar R (2006) Intraneuronal beta-amyloid aggregates, neurodegeneration, and neuron loss in transgenic mice with five familial Alzheimer’s disease mutations: potential factors in amyloid plaque formation. J Neurosci 26:10129–10140
Oddo S, Billings L, Kesslak JP, Cribbs DH, LaFerla FM (2004) Abeta immunotherapy leads to clearance of early, but not late, hyperphosphorylated tau aggregates via the proteasome. Neuron 43:321–332
Oddo S, Caccamo A, Shepherd JD, Murphy MP, Golde TE, Kayed R, Metherate R, Mattson MP, Akbari Y, LaFerla FM (2003) Triple-transgenic model of Alzheimer’s disease with plaques and tangles: intracellular Abeta and synaptic dysfunction. Neuron 39:409–421
Oddo S, Caccamo A, Smith IF, Green KN, LaFerla FM (2006) A dynamic relationship between intracellular and extracellular pools of Abeta. Am J Pathol 168:184–194
Ohgami T, Kitamoto T, Weidmann A, Beyreuther K, Tateishi J (1991) Alzheimer’s amyloid precursor protein-positive degenerative neurites exist even within kuru plaques not specific to Alzheimer’s disease. Am J Pathol 139:1245–1250
Ohyagi Y, Tsuruta Y, Motomura K, Miyoshi K, Kikuchi H, Iwaki T, Taniwaki T, Kira J (2007) Intraneuronal amyloid beta42 enhanced by heating but counteracted by formic acid. J Neurosci Methods 159:134–138
Oide T, Kinoshita T, Arima K (2006) Regression stage senile plaques in the natural course of Alzheimer’s disease. Neuropathol Appl Neurobiol 32:539–556
Okamoto K, Yamaguchi H, Hirai S, Shoji M, Inoue K, Takatama M (1989) Immunogold electron microscopic study of cerebrovascular and senile plaque amyloid using anti-beta protein antibody. Prog Clin Biol Res 317:953–963
Omalu BI, DeKosky ST, Minster RL, Kamboh MI, Hamilton RL, Wecht CH (2005) Chronic traumatic encephalopathy in a National Football League player. Neurosurgery 57:128–134
Pappolla MA, Omar RA, Sambamurti K, Anderson JP, Robakis NK (1992) The genesis of the senile plaque. Further evidence in support of its neuronal origin. Am J Pathol 141:1151–1159
Pappolla MA, Omar RA, Vinters HV (1991) Image analysis microspectroscopy shows that neurons participate in the genesis of a subset of early primitive (diffuse) senile plaques. Am J Pathol 139:599–607
Parbhu A, Lin H, Thimm J, Lal R (2002) Imaging real-time aggregation of amyloid beta protein (1–42) by atomic force microscopy. Peptides 23:1265–1270
Paresce DM, Ghosh RN, Maxfield FR (1996) Microglial cells internalize aggregates of Alzheimer’s disease amyloid b-protein via a scavenger receptor. Neuron 17:553–565
Pasternak SH, Bagshaw RD, Guiral M, Zhang S, Ackerley CA, Pak BJ, Callahan JW, Mahuran DJ (2003) Presenilin-1, nicastrin, amyloid precursor protein, and gamma-secretase activity are co-localized in the lysosomal membrane. J Biol Chem 278:26687–26694
Patton RL, Kalback WM, Esh CL, Kokjohn TA, Van Vickle GD, Luehrs DC, Kuo YM, Lopez J, Brune D, Ferrer I, Masliah E, Newel AJ, Beach TG, Castano EM, Roher AE (2006) Amyloid-beta peptide remnants in AN-1792-immunized Alzheimer’s disease patients: a biochemical analysis. Am J Pathol 169:1048–1063
Peters A (1991) Aging in monkey cerebral cortex. In: Peters A, Jones EG (eds) Cerebral cortex. vol. 9. Normal and altered states of function. Plenum, New York, pp 485–510
Phinney AL, Deller T, Stalder M, Calhoun ME, Frotscher M, Sommer B, Staufenbiel M, Jucker M (1999) Cerebral amyloid induces aberrant axonal sprouting and ectopic terminal formation in amyloid precursor protein transgenic mice. J Neurosci 19:8552–8559
Pierce JE, Trojanowski JQ, Graham DI, Smith DH, McIntosh TK (1996) Immunohistochemical characterization of alterations in the distribution of amyloid precursor proteins and beta-amyloid peptide after experimental brain injury in the rat. J Neurosci 16:1083–1090
Pike CJ, Cummings BJ, Cotman CW (1992) beta-Amyloid induces neuritic dystrophy in vitro: similarities with Alzheimer pathology. Neuroreport 3:769–772
Pilling AD, Horiuchi D, Lively CM, Saxton WM (2006) Kinesin-1 and dynein are the primary motors for fast axonal transport of mitochondria in Drosophila motor axons. Mol Biol Cell 17:2057–2068
Pluta R, Kida E, Lossinsky AS, Golabek AA, Mossakowski MJ, Wisniewski HM (1994) Complete cerebral ischemia with short-term survival in rats induced by cardiac arrest. I. Extracellular accumulation of Alzheimer’s beta-amyloid protein precursor in the brain. Brain Res 649:323–328
Povlishock JT (1992) Traumatically induced axonal injury: pathogenesis and pathobiological implications. Brain Pathol 2:1–12
Powers JM, Skeen JT (1988) Ultrastructural heterogeneity in cerebral amyloid of Alzheimer’s disease. Acta Neuropathol (Berl) 76:613–623
Praprotnik D, Smith MA, Richey PL, Vinters HV, Perry G (1996) Filament heterogeneity within the dystrophic neurites of senile plaques suggests blockage of fast axonal transport in Alzheimer’s disease. Acta Neuropathol (Berl) 91:226–235
Praprotnik D, Smith MA, Richey PL, Vinters HV, Perry G (1996) Plasma membrane fragility in dystrophic neurites in senile plaques of Alzheimer’s disease: an index of oxidative stress. Acta Neuropathol (Berl) 91:1–5
Price DL, Martin LJ, Sisodia SS, Wagster MV, Koo EH, Walker LC, Koliatsos VE, Cork LC (1991) Aged non-human primates: an animal model of age-associated neurodegenerative disease. Brain Pathol 1:287–296
Probst A, Basler V, Bron B, Ulrich J (1983) Neuritic plaques in senile dementia of Alzheimer type: a golgi analysis in the hippocampal region. Brain Res 268:249–254
Rabano A, Jimenez-Huete A, Acevedo B, Calero M, Ghiso J, Valdes I, Gavilondo J, Frangione B, Mendez E (2005) Diversity of senile plaques in Alzheimer’s disease as revealed by a new monoclonal antibody that recognizes an internal sequence of the Abeta peptide. Curr Alzheimer Res 2:409–417
Radde R, Bolmont T, Kaeser SA, Coomaraswamy J, Lindau D, Stoltze L, Calhoun ME, Jaggi F, Wolburg H, Gengler S, Haass C, Ghetti B, Czech C, Holscher C, Mathews PM, Jucker M (2006) Abeta42-driven cerebral amyloidosis in transgenic mice reveals early and robust pathology. EMBO Rep 7:940–946
Reilly JF, Games D, Rydel RE, Freedman S, Schenk D, Young WG, Morrison JH, Bloom FE (2003) Amyloid deposition in the hippocampus and entorhinal cortex: quantitative analysis of a transgenic mouse model. Proc Natl Acad Sci USA 100:4837–4842
Rifenburg RP, Perry G (1995) Dystrophic neurites define diffuse as well as core-containing senile plaques in Alzheimer’s disease. Neurodegeneration 4:235–237
Roberts GW, Allsop D, Bruton C (1990) The occult aftermath of boxing. J Neurol Neurosurg Psychiatry 53:373–378
Roy S, Zhang B, Lee VM, Trojanowski JQ (2005) Axonal transport defects: a common theme in neurodegenerative diseases. Acta Neuropathol (Berl) 109:5–13
Rubinsztein DC, DiFiglia M, Heintz N, Nixon RA, Qin ZH, Ravikumar B, Stefanis L, Tolkovsky A (2005) Autophagy and its possible roles in nervous system diseases, damage and repair. Autophagy 1:11–22
Rui Y, Tiwari P, Xie Z, Zheng JQ (2006) Acute impairment of mitochondrial trafficking by β-amyloid peptides in hippocampal neurons. J Neurosci 26:10480–10487
Sasaki A, Shoji M, Harigaya Y, Kawarabayashi T, Ikeda M, Naito M, Matsubara E, Abe K, Nakazato Y (2002) Amyloid cored plaques in Tg2576 transgenic mice are characterized by giant plaques, slightly activated microglia, and the lack of paired helical filament-typed, dystrophic neurites. Virchows Arch 441:358–367
Sawaya MR, Sambashivan S, Nelson R, Ivanova MI, Sievers SA, Apostol MI, Thompson MJ, Balbirnie M, Wiltzius JJ, McFarlane HT, Madsen AO, Riekel C, Eisenberg D (2007) Atomic structures of amyloid cross-beta spines reveal varied steric zippers. Nature 447:453–457
Schenk D, Barbour R, Dunn W, Gordon G, Grajeda H, Guido T, Hu K, Huang J, Johnson-Wood K, Khan K, Kholodenko D, Lee M, Liao Z, Lieberburg I, Motter R, Mutter L, Soriano F, Shopp G, Vasquez N, Vandevert C, Walker S, Wogulis M, Yednock T, Games D, Seubert P (1999) Immunization with amyloid-beta attenuates Alzheimer-disease-like pathology in the PDAPP mouse. Nature 400:173–177
Schlaepfer WW (1977) Structural alterations of peripheral nerve induced by the calcium ionophore A23187. Brain Res 136:1–9
Schwarze-Eicker K, Keyvani K, Gortz N, Westaway D, Sachser N, Paulus W (2005) Prion protein (PrPc) promotes beta-amyloid plaque formation. Neurobiol Aging 26:1177–1182
Selkoe DJ (1996) Amyloid beta-protein and the genetics of Alzheimer’s disease. J Biol Chem 271:18295–18298
Selkoe DJ (2000) Toward a comprehensive theory for Alzheimer’s disease: hypothesis: Alzheimer’s disease is caused by the cerebral accumulation and cytotoxicity of amyloid beta-protein. Ann NY Acad Sci 924:17–25
Selkoe DJ (2006) The ups and downs of Abeta. Nat Med 12:758–759
Selkoe DJ, Bell DS, Podlisny MB, Price DL, Cork LC (1987) Conservation of brain amyloid proteins in aged mammals and humans with Alzheimer’s disease. Science 235:873–877
Sheng JG, Price DL, Koliatsos VE (2002) Disruption of corticocortical connections ameliorates amyloid burden in terminal fields in a transgenic model of Abeta amyloidosis. J Neurosci 22:9794–9799
Shin RW, Ogino K, Kondo A, Saido TC, Trojanowski JQ, Kitamoto T, Tateishi J (1997) Amyloid beta-protein (Abeta) 1–40 but not Abeta1–42 contributes to the experimental formation of Alzheimer disease amyloid fibrils in rat brain. J Neurosci 17:8187–8193
Shoji M, Kawarabayashi T, Matsubara E, Ikeda M, Ishiguro K, Harigaya Y, Okamoto K (2000) Distribution of amyloid beta protein precursor in the Alzheimer’s disease brain. Psychiatry Clin Neurosci 54:45–54
Sipos E, Kurunczi A, Kasza A, Horvath J, Felszeghy K, Laroche S, Toldi J, Parducz A, Penke B, Penke Z (2007) beta-Amyloid pathology in the entorhinal cortex of rats induces memory deficits: implications for Alzheimer’s disease. Neuroscience 147:28–36
Small SA, Gandy S (2006) Sorting through the cell biology of Alzheimer’s disease: intracellular pathways to pathogenesis. Neuron 52:15–31
Smith DH, Chen X-H, Iwata A, Graham DI (2003) Amyloid β accumulation in axons after traumatic brain injury in humans. J Neurosurg 98:1072–1077
Smith DH, Chen X-H, Nonaka M, Trojanowski JQ, Lee VM-Y, Saatman KE, Leoni MJ, Wolf JA, Meaney DF (1999) Accumulation of amyloid β and tau and the formation of neurofilament inclusions following diffuse brain injury in the pig. J Neuropathol Exp Neurol 58:982–992
Song M-S, Saavedra L, Posse de Chaves EI (2006) Apoptosis is secondary to non-apoptotic axonal degeneration in neurons exposed to Aβ in distal axons. Neurobiol Aging 27:1224–1238
Spires TL, Hyman BT (2005) Transgenic models of Alzheimer’s disease: learning from animals. NeuroRx 2:423–437
Spires TL, Meyer-Luehmann M, Stern EA, McLean PJ, Skoch J, Nguyen PT, Bacskai BJ, Hyman BT (2005) Dendritic spine abnormalities in amyloid precursor protein transgenic mice demonstrated by gene transfer and intravital multiphoton microscopy. J Neurosci 25:7278–7287
Stalder M, Deller T, Staufenbiel M, Jucker M (2001) 3D-reconstruction of microglia and amyloid in APP23 transgenic mice: no evidence of intracellular amyloid. Neurobiol Aging 22:427–434
Stalder M, Phinney A, Probst A, Sommer B, Staufenbiel M, Jucker M (1999) Association of microglia with amyloid plaques in brains of APP23 transgenic mice. Am J Pathol 154:1673–1684
Steiner H, Revesz T, Neumann M, Romig H, Grim MG, Pesold B, Kretzschmar HA, Hardy J, Holton JL, Baumeister R, Houlden H, Haass C (2001) A pathogenic presenilin-1 deletion causes abberrant Abeta 42 production in the absence of congophilic amyloid plaques. J Biol Chem 276:7233–7239
Stokin GB, Goldstein LSB (2006) Axonal transport and Alzheimer’s disease. Ann Rev Biochem 75:607–627
Stokin GB, Lillo C, Falzone TL, Brusch RG, Rockenstein E, Mount SL, Raman R, Davies P, Masliah E, Williams DS, Goldstein LSB (2005) Axonopathy and transport deficits in the pathogenesis of Alzheimer’s disease. Science 307:1282–1288
Stoltzner SE, Grenfell TJ, Mori C, Wisniewski KE, Wisniewski TM, Selkoe DJ, Lemere CA (2000) Temporal accrual of complement proteins in amyloid plaques in Down’s syndrome with Alzheimer’s disease. Am J Pathol 156:489–499
Stone JR, Singleton RH, Povlishock JT (2001) Intra-axonal neurofilament compaction does not evoke local axonal swelling in all traumatically injured axons. Exp Neurol 172:320–331
Struble RG, Price DL, Cork LC, Price DL (1985) Senile plaques in cortex of aged normal monkeys. Brain Res 361:267–275
Styren SD, Hamilton RL, Styren GC, Klunk WE (2000) X-34, a fluorescent derivative of Congo red: a novel histochemical stain for Alzheimer’s disease pathology. J Histochem Cytochem 48:1223–1232
Su JH, Cummings BJ, Cotman CW (1998) Plaque biogenesis in brain aging and Alzheimer’s disease. II. Progressive transformation and developmental sequence of dystrophic neurites. Acta Neuropathol (Berl) 96:463–471
Suzuki K, Terry RD (1967) Fine structural localization of acid phosphatase in senile plaques in Alzheimer’s disease presenile dementia. Acta Neuropathol 8:276–284
Tagliavini F, Giaccone G, Frangione B, Bugiani O (1988) Preamyloid deposits in the cerebral cortex of patients with Alzheimer’s disease and nondemented individuals. Neurosci Lett 93:191–196
Takahashi RH, Almeida CG, Kearney PF, Yu F, Lin MT, Milner TA, Gouras GK (2004) Oligomerization of Alzheimer’s beta-amyloid within processes and synapses of cultured neurons and brain. J Neurosci 24:3592–3599
Takahashi RH, Milner TA, Li F, Nam EE, Edgar MA, Yamaguchi H, Beal MF, Xu H, Greengard P, Gouras GK (2002) Intraneuronal Alzheimer abeta42 accumulates in multivesicular bodies and is associated with synaptic pathology. Am J Pathol 161:1869–1879
Takeuchi A, Irizarry MC, Duff K, Saido TC, Hsiao Ashe K, Hasegawa M, Mann DM, Hyman BT, Iwatsubo T (2000) Age-related amyloid beta deposition in transgenic mice overexpressing both Alzheimer mutant presenilin 1 and amyloid beta precursor protein Swedish mutant is not associated with global neuronal loss. Am J Pathol 157:331–339
Terry RD, Gonatas NK, Weiss M (1964) Ultrastructural studies in Alzheimer’s presenile dementia. Am J Pathol 44:269–297
Terry RD, Wisniewski HM (1970) The ultrastructure of the neurofibrillary tangle and the senile plaque. In: Wolstenholme GEW, O’Connor M (eds) Alzheimer’s disease and related conditions. J & A Churchill, London pp 145–168
Terry RD, Wisniewski HM (1972) Ultrastructure of senile dementia and of experimental analogs. In: Gaitz CM (ed) Aging and the brain. Plenum, New York, pp 89–116
Thal DR, Capetillo-Zarate E, Del Tredici K, Braak H (2006) The development of amyloid beta protein deposits in the aged brain. Sci Aging Knowledge Environ 2006(6):re1
Thal DR, Capetillo-Zarate E, Schultz C, Rub U, Saido TC, Yamaguchi H, Haass C, Griffin WS, Del Tredici K, Braak H, Ghebremedhin E (2005) Apolipoprotein E co-localizes with newly formed amyloid beta-protein (Abeta) deposits lacking immunoreactivity against N-terminal epitopes of Abeta in a genotype-dependent manner. Acta Neuropathol (Berl) 110:459–471
Thal DR, Hartig W, Schober R (1999) Diffuse plaques in the molecular layer show intracellular Abeta(8–17)-immunoreactive deposits in subpial astrocytes. Clin Neuropathol 18:226–231
Thal DR, Rub U, Schultz C, Sassin I, Ghebremedhin E, Del Tredici K, Braak E, Braak H (2000) Sequence of Abeta-protein deposition in the human medial temporal lobe. J Neuropathol Exp Neurol 59:733–748
Thal DR, Sassin I, Schultz C, Haass C, Braak E, Braak H (1999) Fleecy amyloid deposits in the internal layers of the human entorhinal cortex are comprised of N-terminal truncated fragments of Abeta. J Neuropathol Exp Neurol 58:210–216
Thal DR, Schultz C, Dehghani F, Yamaguchi H, Braak H, Braak E (2000) Amyloid beta-protein (Abeta)-containing astrocytes are located preferentially near N-terminal-truncated Abeta deposits in the human entorhinal cortex. Acta Neuropathol (Berl) 100:608–617
Tienari PJ, Ida N, Ikonen E, Simons M, Weidemann A, Multhaup G, Masters CL, Dotti CG, Beyreuther K (1997) Intracellular and secreted Alzheimer beta-amyloid species are generated by distinct mechanisms in cultured hippocampal neurons. Proc Natl Acad Sci USA 94:4125–4130
Tomidokoro Y, Harigaya Y, Matsubara E, Ikeda M, Kawarabayashi T, Shirao T, Ishiguro K, Okamoto K, Younkin SG, Shoji M (2001) Brain Abeta amyloidosis in APPsw mice induces accumulation of presenilin-1 and tau. J Pathol 194:500–506
Tomidokoro Y, Lashley T, Rostagno A, Neubert TA, Bojsen-Moller M, Braendgaard H, Plant G, Holton J, Frangione B, Revesz T, Ghiso J (2005) Familial Danish dementia: co-existence of Danish and Alzheimer amyloid subunits (ADan AND A{beta}) in the absence of compact plaques. J Biol Chem 280:36883–36894
Tsai J, Grutzendler J, Duff K, Gan W-B (2004) Fibrillar amyloid deposition leads to synaptic abnormalities and breakage of neuronal branches. Nat Neurosci 7:1181–1183
Tsukita S, Ishikawa H (1980) The movement of membranous organelles in axons: electron microscopic identification of anterogradely and retrogradely transported organelles. J Cell Biol 84:513–530
Uno H, Alsum PB, Dong S, Richardson R, Zimbric ML, Thieme CS, Houser WD (1996) Cerebral amyloid angiopathy and plaques, and visceral amyloidosis in aged macaques. Neurobiol Aging 17:275–281
van Groen T, Kiliaan AJ, Kadish I (2006) Deposition of mouse amyloid beta in human APP/PS1 double and single AD model transgenic mice. Neurobiol Dis 23:653–662
van Groen T, Liu L, Ikonen S, Kadish I (2003) Diffuse amyloid deposition, but not plaque number, is reduced in amyloid precursor protein/presenilin 1 double-transgenic mice by pathway lesions. Neuroscience 119:1185–1197
van Groen T, Puurunen K, Maki HM, Sivenius J, Jolkkonen J (2005) Transformation of diffuse beta-amyloid precursor protein and beta-amyloid deposits to plaques in the thalamus after transient occlusion of the middle cerebral artery in rats. Stroke 36:1551–1556
Vassar R, Bennett BD, Babu-Khan S, Kahn S, Mendiaz EA, Denis P, Teplow DB, Ross S, Amarante P, Loeloff R, Luo Y, Fisher S, Fuller J, Edenson S, Lile J, Jarosinski MA, Biere AL, Curran E, Burgess T, Louis JC, Collins F, Treanor J, Rogers G, Citron M (1999) Beta-secretase cleavage of Alzheimer’s amyloid precursor protein by the transmembrane aspartic protease BACE. Science 286:735–741
Vaughan DW, Peters A (1981) The structure of neuritic plaques in the cerebral cortex of aged rats. J Neuropathol Exp Neurol 40:472–487
Vickers JC (1997) A cellular mechanism for the neuronal changes underlying Alzheimer’s disease. Neuroscience 78:629–639
Vickers JC, Chin D, Edwards AM, Sampson V, Harper C, Morrison J (1996) Dystrophic neurite formation associated with age-related beta amyloid deposition in the neocortex: clues to the genesis of neurofibrillary pathology. Exp Neurol 141:1–11
Vinters HV, Pardridge WM (1986) The blood-brain barrier in Alzheimer’s disease. Can J Neurol Sci 13(4 Suppl):446–448
Walsh DM, Hartley DM, Kusumoto Y, Fezoui Y, Condron MM, Lomakin A, Benedek GB, Selkoe DJ, Teplow DB (1999) Amyloid β-protein fibrillogenesis: structure and biological activity of protofibrillar intermediates. J Biol Chem 274:25945–25952
Walsh DM, Selkoe DJ (2007) A beta oligomers––a decade of discovery. J Neurochem 101:1172–1184
Walsh DM, Tseng BP, Rydel RE, Podlisny MB, Selkoe DJ (2000) The oligomerization of amyloid beta-protein begins intracellularly in cells derived from human brain. Biochemistry 39:10831–10839
Wang HY, D’Andrea MR, Nagele RG (2002) Cerebellar diffuse amyloid plaques are derived from dendritic Abeta42 accumulations in Purkinje cells. Neurobiol Aging 23:213–223
Wang D, Munoz DG (1995) Qualitative and quantitative differences in senile plaque dystrophic neurites of Alzheimer’s disease and normal aged brain. J Neuropathol Exp Neurol 54:548–556
Waxman SG, Black JA, Ransom BR, Stys PK (1993) Protection of the axonal cytoskeleton in anoxic optic nerve by decreased extracellular calcium. Brain Res 614:137–145
Webster HD (1962) Transient, focal accumulation of axonal mitochondria during the early stages of Wallerian degeneration. J Cell Biol 12:361–383
Wegiel J, Wang KC, Imaki H, Rubenstein R, Wronska A, Osuchowski M, Lipinski WJ, Walker LC, LeVine H (2001) The role of microglial cells and astrocytes in fibrillar plaque evolution in transgenic APPsw mice. Neurobiol Aging 22:49–61
Wegiel J, Wang KC, Tarnawski M, Lach B (2000) Microglia cells are the driving force in fibrillar plaque formation, whereas astrocytes are a leading factor in plague degradation. Acta Neuropathol (Berl) 100:356–364
Wegiel J, Wisniewski HM (1990) The complex of microglial cells and amyloid star in three-dimensional reconstruction. Acta Neuropathol (Berl) 81:116–124
Wegiel J, Wisniewski HM (1999) β-Amyloidosis in Alzheimer’s disease. In: de Leon MJ (ed) An atlas of Alzheimer’s disease. Parthenon Publishing Group, New York, pp 89–107
Wegiel J, Wisniewski HM, Dziewiatkowski J, Tarnawski M, Nowakowski J, Dziewiatkowska A, Soltysiak Z (1995) The origin of amyloid in cerebral vessels of aged dogs. Brain Res 705:225–234
Weldon DT, Rogers SD, Ghilardi JR, Finke MP, Cleary JP, O’Hare E, Esler WP, Maggio JE, Mantyh PW (1998) Fibrillar beta-amyloid induces microglial phagocytosis, expression of inducible nitric oxide synthase, and loss of a select population of neurons in the rat CNS in vivo. J Neurosci 18:2161–2173
Weller RO, Massey A, Newman TA, Hutchings M, Kuo YM, Roher AE (1998) Cerebral amyloid angiopathy: amyloid beta accumulates in putative interstitial fluid drainage pathways in Alzheimer’s disease. Am J Pathol 153:725–733
Westermark P (2005) Aspects on human amyloid forms and their fibril polypeptides. FEBS J 272:5942–5949
Wilson CA, Doms RW, Lee VM (1999) Intracellular APP processing and Abeta production in Alzheimer disease. J Neuropathol Exp Neurol 58:787–794
Winkler J, Connor DJ, Frautschy SA, Behl C, Waite JJ, Cole GM, Thal LJ (1994) Lack of long-term effects after beta-amyloid protein injections in rat brain. Neurobiol Aging 15:601–607
Wirths O, Multhaup G, Czech C, Blanchard V, Moussaoui S, Tremp G, Pradier L, Beyreuther K, Bayer TA (2001) Intraneuronal Abeta accumulation precedes plaque formation in beta-amyloid precursor protein and presenilin-1 double-transgenic mice. Neurosci Lett 306:116–120
Wirths O, Multhaup G, Bayer TA (2004) A modified beta-amyloid hypothesis: intraneuronal accumulation of the beta-amyloid peptide––the first step of a fatal cascade. J Neurochem 91:513–520
Wirths O, Weis J, Szczygielski J, Multhaup G, Bayer TA (2006) Axonopathy in an APP/PS1 transgenic mouse model of Alzheimer’s disease. Acta Neuropathol (Berl) 111:312–319
Wisniewski HM, Bancher C, Barcikowski M, Wen GY, Currie J (1989) Spectrum of morphological appearance of amyloid deposits in Alzheimer’s disease. Acta Neuropathol 78:337–347
Wisniewski HM, Ghetti B, Terry RD (1973) Neuritic (senile) plaques and filamentous changes in aged rhesus monkeys. J Neuropathol Exp Neurol 32:566–584
Wisniewski HM, Terry RD (1973) Reexamination of the pathogenesis of the senile plaque. In: Zimmerman HM (ed) Progress in neuropathology. Vol. II. Grune & Stratton, New York, pp 1–26
Wisniewski HM, Wegiel J, Wang KC, Kujawa M, Lach B (1989) Ultrastructural studies of the cells forming amyloid fibers in classical plaques. Can J Neurol Sci 16(4 Suppl):535–542
Wisniewski T, Lalowski M, Bobik M, Russell M, Strosznajder J, Frangione B (1996) Amyloid beta 1–42 deposits do not lead to Alzheimer’s neuritic plaques in aged dogs. Biochem J 313:575–580
Wolf DS, Gearing M, Snowdon DA, Mori H, Markesbery WR, Mirra SS (1999) Progression of regional neuropathology in Alzheimer disease and normal elderly: findings from the Nun study. Alzheimer Dis Assoc Disord 13:226–231
Woodhouse A, West AK, Chuckowree JA, Vickers JC, Dickson TC (2005) Does beta-amyloid plaque formation cause structural injury to neuronal processes? Neurotox Res 7:5–15
Wyss-Coray T, Loike JD, Brionne TC, Lu E, Anankov R, Yan F, Silverstein SC, Husemann J (2003) Adult mouse astrocytes degrade amyloid-beta in vitro and in situ. Nat Med 9:453–457
Wyss-Coray T, Yan F, Lin AH, Lambris JD, Alexander JJ, Quigg RJ, Masliah E (2002) Prominent neurodegeneration and increased plaque formation in complement-inhibited Alzheimer’s mice. Proc Natl Acad Sci USA 99:10837–10842
Yamaguchi H, Sugihara S, Ogawa A, Saido TC, Ihara Y (1998) Diffuse plaques associated with astroglial amyloid beta protein, possibly showing a disappearing stage of senile plaques. Acta Neuropathol (Berl) 95:217–222
Yamaguchi H, Hirai S, Shoji M, Harigaya Y, Okamoto Y, Nakazato Y (1989) Alzheimer type dementia: diffuse type of senile plaques demonstrated by beta protein immunostaining. Prog Clin Biol Res 317:467–474
Yamaguchi H, Nakazato Y, Shoji M, Takatama M, Hirai S (1991) Ultrastructure of diffuse plaques in senile dementia of the Alzheimer type: comparison with primitive plaques. Acta Neuropathol 82:13–20
Yan SD, Xiong W-C, Stern DM (2006) Mitochondrial amyloid-beta peptide: pathogenesis or late-phase development. J Alz Dis 9:127–137
Yang AJ, Chandswangbhuvana D, Margol L, Glabe CG (1998) Loss of endosomal/lysosomal membrane impermeability is an early event in amyloid Abeta1–42 pathogenesis. J Neurosci Res 52:691–698
Yasuhara O, Kawamata T, Aimi Y, McGeer EG, McGeer PL (1994) Two types of dystrophic neurites in senile plaques of Alzheimer disease and elderly non-demented cases. Neurosci Lett 171:73–76
Ye W, Zhou JN, Hu XY, Liu JW, He JH, Tang XW (2003) Reconstruction of the three-dimensional structure of senile plaques in Alzheimer disease. Sheng Wu Hua Xue Yu Sheng Wu Wu Li Xue Bao (Shanghai) 35:449–453
Yu WH, Cuervo AM, Kumar A, Peterhoff CM, Schmidt SD, Lee JH, Mohan PS, Mercken M, Farmery MR, Tjernberg LO, Jiang Y, Duff K, Uchiyama Y, Naslund J, Mathews PM, Cataldo AM, Nixon RA (2005) Macroautophagy––a novel Beta-amyloid peptide-generating pathway activated in Alzheimer’s disease. J Cell Biol 171:87–98
Yu WH, Kumar A, Peterhoff C, Shapiro Kulnane L, Uchiyama Y, Lamb BT, Cuervo AM, Nixon RA (2004) Autophagic vacuoles are enriched in amyloid precursor protein-secretase activities: implications for beta-amyloid peptide over-production and localization in Alzheimer’s disease. Int J Biochem Cell Biol 36:2531–2540
Zhao J, Fu Y, Yasvoina M, Shao P, Hitt B, O’Connor T, Logan S, Maus E, Citron M, Berry R, Binder L, Vassar R (2007) β-Site amyloid precursor protein cleaving enzyme 1 levels become elevated in neurons around amyloid plaques: implications for Alzheimer’s disease pathogenesis. J Neurosci 27:3639–3649
Acknowledgments
Thanks to Alan Peters for providing the aged monkey tissue used for Figs. 1 and 3, and to Marcia Feinberg for electron microscopy. Thanks also to Helen Barbas, Alan Peters, and the reviewers for many helpful suggestions on earlier versions of the manuscript.
This work was supported by grants from National Institute of Mental Health (RO1 MH057414) and National Institute of Neurological Disorders and Stroke (RO1 NS024760), from the National Institute on Aging (P01 AG00001), and from the Dudley Allen Sargent Research Fund, Boston University.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fiala, J.C. Mechanisms of amyloid plaque pathogenesis. Acta Neuropathol 114, 551–571 (2007). https://doi.org/10.1007/s00401-007-0284-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-007-0284-8