Abstract
Purpose
Appendicitis and appendectomy(AA), when done at a young age, offer protection against inflammatory bowel disease (IBD) development in later life. However, IBD pathogenesis involves both immunological and vascular abnormalities. Using the first murine model of AA (developed by us), we aimed to determine the role of AA in modulating vascular remodelling mediated by endothelin activity in IBD.
Methods
Mice with two laparotomies each served as controls (sham-sham or SS). Distal colons were harvested (four AA group colons, four SS group colons), and RNA extracted from each. The RNA was subjected to microarray analysis and RT-PCR validation. Gene set enrichment analysis (GSEA) software was used to further analyze the microarray data.
Results
Gene expression of seven genes closely associated with endothelin activity was examined in distal colons 3 days post-AA and 28 days post-AA. While there were no gene expression changes 3 days post-AA, the genes EDN1 (0.7-fold), EDN2 (0.8-fold) and ECE2 (0.8-fold) were downregulated (*p value <0.05) 28 days post-AA. However, EDN3 (1.3-fold) was upregulated 28 days post-AA (*p value <0.05). GSEA analysis showed downregulation of 11 gene sets (stringent cut-offs—false discovery rate <5 % and p value <0.001) associated with endothelin and endothelin-converting enzyme genes by AA, in contrast to only 1 being upregulated.
Conclusions
AA induces a delayed but significant suppression of genes pertaining to endothelin activity. Elucidating the pathways involved in suppression of endothelin activity and manipulation of different genes/enzymes/proteins related to endothelin activity will significantly enhance the extant repertoire of therapeutic options in IBD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The appendix contains abundant lymphoid tissue and is perpetually exposed to intestinal flora. Inflammation of the appendix, appendicitis, is the most common gastrointestinal emergency requiring surgical intervention [1]. The highest occurrence of uncomplicated appendicitis is between 10 and 30 years [2].
The complex interplay between genetic predisposition, gastrointestinal bacteria and gut immunity in inflammatory bowel disease (or IBD, comprising Crohn’s disease and ulcerative colitis) is yet to be deciphered. It has been shown in over a dozen clinical studies that appendicitis and appendectomy (AA) limits or prevents ulcerative colitis from developing [3]. However, this protection is seen only in patients undergoing surgery before 20 years of age. In mice, the equivalent of the human appendix is the major caecal lymphoid patch. The development of experimental colitis was prevented by removal of the caecum in three murine colitis models, namely, T cell receptor-α mutants [4], dextran sulphate sodium (DSS) model [5] and adoptive T cell transfer colitis model [6]. The first murine model of AA was developed by our group [7]. In our model, appendiceal pathology resembles that of human appendicitis, and AA offers an age-, bacteria- and antigen-dependent protection against trinitrobenzene sulphonic acid (TNBS) colitis.
IBD pathogenesis involves both immunological and vascular abnormalities. Endothelins (ET-1, ET-2 and ET-3) are potent vasoconstrictor/pressors (Table 1) [8] originally obtained from porcine aortic endothelial cells [9]. Each endothelin consists of 21 amino acid residues with two sets of intra-chain disulphide linkages [9]. In addition to vasoconstrictor effects, endothelin produces a broad range of biological effects including stimulation of proliferation of vascular smooth muscle cells and fibroblasts (vascular remodelling), airway and intestinal smooth muscle contraction, increased force and rate of heart contraction, icosanoid release, increased atrial natriuretic peptide secretion from atrial cardiocytes, inhibition of renal renin release and sympathetic modulation [10]. The main functions of the endothelins, its activating (converting) enzymes, and their target receptors are summarized in Table 1.
In IBD patients, plasma endothelin is raised in IBD [11, 12], serum endothelin in ulcerative colitis [13] and plasma endothelin in ulcerative colitis [14]. Endothelin levels in colon samples, as assessed by radioimmunoassay (and immunohistochemistry), were significantly higher in IBD patients suggesting that endothelin production by local inflammatory cells may induce or aggravate IBD vasculitis via persistent vasoconstriction and intestinal ischaemia [15].
Animal models involving endothelin appraisal include DSS colitis and TNBS colitis. DSS colitis increases colonic endothelin, and the endothelin-converting enzyme inhibitor SM-19712 significantly diminishes DSS-induced increases in colonic endothelin staining [16]. Exogenous application of the endothelin-1 receptor A antagonist LU-135252 ameliorates TNBS colitis [17]. The non-selective endothelin receptor antagonist Bosentan ameliorates TNBS colitis [18–20] and DSS colitis [21]. In TNBS colitis, endothelin receptor-mediated antagonism occurs via endothelin receptor A, but not endothelin receptor B [19].
Individual gene expression differences between two experimental groups have been successfully elucidated by various gene expression methodologies. Unfortunately, this simplistic approach does not take into account the biological reality of cellular processes cohesively or contiguously effecting changes as groups of genes (gene sets). These changes may be minimal when individual genes per se are examined but are poignantly obvious when corresponding gene sets are examined. We have previously demonstrated the utility of this approach in exploring mechanisms of immune protection in the colon [22–24]. This study uses microarray analysis and gene set enrichment analysis (GSEA) [25] to identify and characterize the role of endothelin activity-related gene expression in the amelioration of colitis by AA in our murine model.
Materials and methods
Animal experiments
Specific pathogen-free Balb/c mice (male, 5 weeks) were purchased from the Animal Resource Centre, Perth, Western Australia, and kept in the University of New South Wales holding and care facility. All experiments were approved and monitored by the University of New South Wales Animal Care and Ethics Committee. Mice were anaesthetized intraperitoneally with xylazine (5 mg/kg; Sigma-Aldrich, X1251) and ketamine (100 mg/kg; Sigma-Aldrich, K1884), followed by allocation into two treatment groups, the appendicitis group or the sham surgery group [7]. Mice were randomized to have either appendicitis or sham operation. Appendicitis was induced by constructing an appendiceal pouch (using a sterile rubber band) from the caecal lymphoid patch. Sham surgery entailed a similar procedure but without continuous obstruction by band ligation of the caecal patch and the placement of a sterile rubber band in the abdominal cavity as a control for foreign body reaction. Seven days following initial surgery, appendicitis mice underwent appendectomy (AA group) while sham mice underwent a second sham surgery (sham and sham, SS, group). All mice were monitored daily.
Processing of colonic specimens for RNA extraction
Transmural distal colonic segments were cleaned of faecal contents with normal saline and immediately transferred to TRIzol® reagent (50–75 mg of tissue in 600 μL of TRIzol® reagent; Invitrogen Australia Pty Limited, 15596-026), snap-frozen in liquid nitrogen and stored at −80 °C until the microarray analysis. Further extraction entailed chloroform and isopropanol treatment and centrifugation followed by washing the resultant pellet with 75 % ethanol, air-drying and final re-constitution in nuclease-free H2O. Concentration and purity of RNA were determined by automated optical density evaluation (OD 260/OD 280 ≥ 1.8 and OD 260/OD 230 ≥ 1.8) using Nanodrop ND-1000 (Nanodrop Technologies, Wilmington, DE, USA). The degree of RNA degradation was analyzed by the Agilent electrophoresis bioanalyzer 2100 (Agilent Technologies Inc., Santa Clara, CA, USA) with the RNA integrity number (RIN) values consistently above 7.
Validation and analysis of gene expression with RT-PCR
Reverse transcription to produce cDNA was performed using RT2 First-Strand Kits (SA Biosciences, MD, USA) according to the manufacturer’s instructions. RT-PCR was performed utilizing the LightCycler 480 Real-Time PCR System (Roche Applied Science, Mannheim, Germany): with RT2 SYBR Green PCR Master Mix according to the manufacture’s protocol (SA Biosciences). Predesigned primers for genes of interest (slpi, s100A8, lbp, CD68, IL18R1, IL33, ccl8, cxcl10, ccl12, pf4, cxcl5, ccl7, fpr1 and ccr5) were obtained from SA Biosciences (Frederick, MD, USA). For reference genes, we evaluated three candidates, β-actin, β-glucuronidase and 18S rRNA. Beta-glucuronidase was selected based on similar expression patterns to most of our genes of interest and also because it was invariantly expressed between the groups. Hence, each sample was normalized on the basis of its β-glucuronidase content. Thermal cycling was performed as follows: initial denaturation at 95 °C for 10 min, followed by 40 cycles of 95 °C for 15 s and 60 °C for 1 min. Each assay was performed in duplicate. The quantification points generated from qRT-PCR were normalized against a reference gene using this formula: normalised value of Gene of interest with β-glucuronidase = 2−(QP GOI −QP RG), where QP = quantitative point, GOI = gene of interest and RG = reference gene (i.e. β-glucuronidase).
Experimental design of microarray study
All experiments were designed to be compliant with minimum information about a microarray experiment (MIAME) standards [26, 27]. For Affymetrix array experiments, four individual test samples (for 3-day post-SS/AA time point) or three individual test samples (for 28-day post-SS/AA time point) were used per group (AA group versus SS group; one colonic sample per mouse) with each sample hybridized to an individual slide.
Affymetrix array process—labelling, hybridization, scanning and normalization
RNA from each mouse distal colonic tissue specimen was taken individually through the microarray process. For Affymetrix arrays, 100 ng of RNA from each sample was labelled using the Whole Transcript Sense Target Labelling Assay as described (Affymetrix). Labelled cRNA samples were then hybridized to Affymetrix Mouse Gene 1.0 ST Arrays (28,853 well-annotated genes) (Ramaciotti Centre for Gene Function Analysis, University of New South Wales) before being scanned using an Affymetrix GCS3000 7G four-colour Gene Array scanner with autoloader (Affymetrix). The Gene Expression Omnibus accession number for microarray data reported here, inclusive of MIAME-compliant experimental details [26, 27], is GSE23914.
Microarray preprocessing and filtering
All non-control probesets from the eight arrays were imported into Partek (Version 6.4, Partek Inc) and then normalized using RMA [28]. The probability of each probeset being expressed was determined using the detected above background procedure, using Affymetrix Power Tools (v1.10.2), excluding 13 probes from probeset 10338063 which had very low GC, and thus did not have matched controls. Probesets were excluded if none of the samples were detected above background (P = 10−5). To assess the degree of differential expression between AA and SS groups, a two-way ANOVA on treatment and batch was fitted to each probeset using Partek. To correct for multiple hypothesis testing, we used the q value/positive false discovery rate (FDR) [29].
Gene set enrichment analysis
We compared gene expression profiles to the c2_all collection of curated gene sets from the molecular signature database (version 2.5) [25]. This collection contains gene sets that are experimentally derived, as well as from expert-curated pathway databases. A pre-ranked file was created, containing the average difference between AA and SS for each probeset, sorted from most upregulated in SS to most downregulated. We used the na28 annotation csv file from www.affymetrix.com to determine the gene symbol for each probeset and collapsed probesets to unique genes using the default, max_probe option, resulting in 18,600 unique genes. GSEA (version 2.0) [25] was run in pre-ranked mode, using default parameters (gene set sizes between 15 and 500 leaving 1,387 gene sets, 1,000 permutations, images on the top 50 gene sets).
Enrichment of endothelin activity-associated gene sets
We utilized GSEA, developed by Mootha [30] which merges data from groups of gene sets previously described in the literature to detect significant expression differences. We utilized stringent statistical cut-offs (FDR values <5 % and p value <0.001) to delineate endothelin pathway-associated gene sets which were consistently altered in the distal colons of all AA mice when compared to control SS mice. Endothelin pathway-associated gene sets were divided into those pertaining to the following: (1) endothelin genes and endothelin-converting enzyme genes and (2) endothelin receptor genes.
Statistics
Group comparisons were analyzed using the Mann-Whitney U test with GraphPad Prism (Graphpad software, San Diego, CA, USA). Data are expressed as mean ± standard error of mean, and the differences were considered to be significant if p < 0.05.
Results
Quantitative RT-PCR validation of our gene expression study
We selected 14 genes for confirmation of our gene expression studies. They broadly belonged to four major groups: innate immunity (slpi, s100A8, lbp, CD68), immune mediators (IL18R1, IL33), cell migration chemokines (ccl8, cxcl10, ccl12 or mcp5, pf4, cxcl5, ccl7 or mcp3) and cell migration receptors (fpr1, ccr5). The RT-PCR results, which have already been published [22], indicate that 8 of the total 14 genes tested were significantly upregulated in the AA group; 3 of these genes just missed statistical significance, and 3 genes showed no difference between the SS and AA groups.
Individual distal colonic gene expression of endothelin activity-associated genes
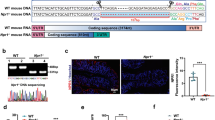
Seven genes associated with endothelin activity—EDN1, EDN2, EDN3, ECE1, ECE2, EDNRA and EDNRB (Table 1)—were examined for gene expression levels in distal colons 3 days post-AA and 28 days post-AA. There were no significant changes 3 days after AA. At the 28-day post-AA time point, EDN1 (0.7-fold), EDN2 (0.8-fold) and ECE2 (0.8-fold) were significantly downregulated (*p value <0.05). At the same time point, EDN2 (1.3-fold) was significantly upregulated (*p value <0.05).
Enrichment of endothelin activity-associated gene sets
Utilizing stringent statistical cut-offs for GSEA (FDR values <5 % and p value <0.001), we delineated 28-day post-AA endothelin activity-associated gene sets which were also consistently altered in the distal colons of each of the AA mice when compared to that from each of the control SS mice (Table 2). While 11 gene sets associated with endothelin and endothelin-converting enzyme genes were downregulated in the AA group, only 1 was upregulated. While three gene sets associated with endothelin receptors were upregulated in the AA group, only one was downregulated.
Discussion
Using a murine appendicitis model developed by us [7], we earlier delineated genetic pathways involved in the AA-induced protection against TNBS colitis via microarray analyses, GSEA and RT-PCR validation [22]. The novelty of our study is that the most distal regions of the large gut sustain major persistent changes (protective against colitis), by manipulation at the caecum, the most proximal region of the large gut. Distal colonic gene expression studies, 3 days after surgery or 28 days after surgery, reveal the various genes and gene sets that are associated with the durable protective effect of AA against colitis [22]. The gene expression data obtained from our microarray study get more distinct between the time points (days 3 and 28) and stabilise around day 28. Although observable in our overall microarray results, these are visually appraised better in the RT-PCR time curves (days 3, 14 and 28) of selected genes in our previous paper [22].
Seven well-known genes closely associated with endothelin activity (Table 1) were examined for gene expression levels in distal colons 3 days post-AA and 28 days post-AA (Table 1). At the 28-day post-AA time point, EDN1 (0.7-fold), EDN2 (0.8-fold) and ECE2 (0.8-fold) were significantly downregulated (Table 1, Fig. 1). Overall, AA induces a delayed but significant suppression of genes pertaining to endothelin activity, although EDN3 (1.3-fold) was upregulated. The upregulation of EDN3 could be attributed to compensatory activity or feedback control loops.
The most intriguing aspect of these findings is the fact that there were no significant changes 3 days after AA but significant and concerted endothelin activity suppressive expression changes 28 days after AA. Does this mean that AA-induced delayed, but sustained long-lasting endothelin suppression activity, leads to “vascular remodelling” that may augment the anti-colitis protection seen after AA? Further studies (contingent on funding) including competitive inhibition of endothelin activity pathways in our AA model and extended time course experiments are required to delve into this.
During GSEA analysis (Table 2), owing to the obvious fact that endothelin receptor expression may not be proportional to endothelin activity, as a result of negative feedback regulation of endothelin receptor expression by endothelin (Fig. 1), endothelin pathway-associated gene sets were divided into those pertaining to the following: (1) endothelin genes and endothelin-converting enzyme genes and (2) endothelin receptor genes. While 11 gene sets associated with endothelin and endothelin-converting enzyme genes were downregulated in the AA group, only 1 was upregulated (Table 2). While three gene sets associated with endothelin receptors were upregulated in the AA group, only one was downregulated (Table 2). Overall, a significant suppression of gene sets pertaining to endothelin activity is seen.
Colonic endothelin was far higher in IBD patients [15], animal models of colitis (DSS colitis and TNBS colitis) demonstrate increased colonic endothelin and blocking endothelin activity at different levels ameliorates colitis (Table 3). Endothelin production by local inflammatory cells may induce or aggravate IBD vasculitis via persistent vasoconstriction and intestinal ischaemia. Our data indicates that AA in the most proximal colon substantially curbs endothelin activity-related gene expression in the most distal colon, this being delayed by 4 weeks after AA (but not soon after AA). This AA-mediated suppression of endothelin activity-related gene expression (Fig. 1) would suppress endothelin vasoactivity-mediated immunopathologial damage in inflammatory colitis. Specific immunohistochemical analyses and “functional confirmation” using one or more endothelin-associated gene knockouts would be our next logical step to pursue. Endothelin activity, owing to its pivotal role in gut homeostasis, vasoconstriction, vascular remodelling, IBD and colon cancer, is an attractive therapeutic target. Elucidating the pathways involved in suppression of endothelin activity using our unique murine AA model [7, 22–24] will enhance the development of approaches and techniques to manipulate different genes, enzymes and proteins related to endothelin activity, towards improving therapeutic options in IBD. Investigating strategies, involving monoclonal antibodies, combinatorial peptides and small molecules (identified by high throughput screening) to manipulate and modulate different aspects of endothelin activity, would augment the development of new therapeutic options to manage IBD.
References
Addiss DG, Shaffer N, Fowler BS, Tauxe RV (1990) The epidemiology of appendicitis and appendectomy in the United States. Am J Epidemiol 132:910–925
Marudanayagam R, Williams GT, Rees BI (2006) Review of the pathological results of 2660 appendicectomy specimens. J Gastroenterol 41:745–749
Koutroubakis IE, Vlachonikolis IG, Kouroumalis EA (2002) Role of appendicitis and appendectomy in the pathogenesis of ulcerative colitis: a critical review. Inflamm Bowel Dis 8:277–286
Mizoguchi A, Mizoguchi E, Chiba C, Spiekermann GM, Tonegawa S, Nagler-Anderson C, Bhan AK (1996) Cytokine imbalance and autoantibody production in T cell receptor-alpha mutant mice with inflammatory bowel disease. J Exp Med 183:847–856
Krieglstein CF, Cerwinka WH, Laroux FS, Grisham MB, Schurmann G, Bruwer M, Granger DN (2001) Role of appendix and spleen in experimental colitis. J Surg Res 101:166–175
Farkas SA, Hornung M, Sattler C, Steinbauer M, Anthuber M, Obermeier F, Herfarth H, Schlitt HJ, Geissler EK (2005) Preferential migration of CD62L cells into the appendix in mice with experimental chronic colitis. Eur Surg Res 37:115–122
Watson Ng WS, Hampartzoumian T, Lloyd AR, Grimm MC (2007) A murine model of appendicitis and the impact of inflammation on appendiceal lymphocyte constituents. Clin Exp Immunol 150:169–178
Inoue A, Yanagisawa M, Kimura S, Kasuya Y, Miyauchi T, Goto K, Masaki T (1989) The human endothelin family: three structurally and pharmacologically distinct isopeptides predicted by three separate genes. Proc Natl Acad Sci U S A 86:2863–2867
Yanagisawa M, Kurihara H, Kimura S, Goto K, Masaki T (1988) A novel peptide vasoconstrictor, endothelin, is produced by vascular endothelium and modulates smooth muscle Ca2+ channels. J Hypertens Suppl 6:S188–S191
Leppaluoto J, Ruskoaho H (1992) Endothelin peptides: biological activities, cellular signalling and clinical significance. Ann Med 24:153–161
Kanazawa S, Tsunoda T, Onuma E, Majima T, Kagiyama M, Kikuchi K (2001) VEGF, basic-FGF, and TGF-beta in Crohn's disease and ulcerative colitis: a novel mechanism of chronic intestinal inflammation. Am J Gastroenterol 96:822–828
Letizia C, Boirivant M, De Toma G, Cerci S, Subioli S, Scuro L, Ferrari P, Pallone F (1998) Plasma levels of endothelin-1 in patients with Crohn’s disease and ulcerative colitis. Ital J Gastroenterol Hepatol 30:266–269
Wang JY, Wang XY, Sun HY (2012) Study on the correlation between the pulmonary injury and the ET-1 serum level in ulcerative colitis patients. Zhongguo Zhong Xi Yi Jie He Za Zhi 32:455–459
Nakamura T, Kawagoe Y, Matsuda T, Ueda A, Ueda Y, Takahashi Y, Tanaka A, Koide H (2004) Effect of granulocyte and monocyte adsorption apheresis on urinary albumin excretion and plasma endothelin-1 concentration in patients with active ulcerative colitis. Blood Purif 22:499–504
Murch SH, Braegger CP, Sessa WC, MacDonald TT (1992) High endothelin-1 immunoreactivity in Crohn's disease and ulcerative colitis. Lancet 339:381–385
Lee S, Carter PR, Watts MN, Bao JR, Harris NR (2009) Effects of the endothelin-converting enzyme inhibitor SM-19712 in a mouse model of dextran sodium sulfate-induced colitis. Inflamm Bowel Dis 15:1007–1013
Kruschewski M, Anderson T, Loddenkemper C, Buhr HJ (2006) Endothelin-1 receptor antagonist (LU-135252) improves the microcirculation and course of TNBS colitis in rats. Dig Dis Sci 51:1461–1470
Hogaboam CM, Muller MJ, Collins SM, Hunt RH (1996) An orally active non-selective endothelin receptor antagonist, bosentan, markedly reduces injury in a rat model of colitis. Eur J Pharmacol 309:261–269
Deniz M, Cetinel S, Kurtel H (2004) Blood flow alterations in TNBS-induced colitis: role of endothelin receptors. Inflamm Res 53:329–336
Gulluoglu BM, Kurtel H, Gulluoglu MG, Yegen C, Aktan AO, Dizdaroglu F, Yalin R, Yegen BC (1999) Role of endothelins in trinitrobenzene sulfonic acid-induced colitis in rats. Digestion 60:484–492
Anthoni C, Mennigen RB, Rijcken EJ, Laukotter MG, Spiegel HU, Senninger N, Schurmann G, Krieglstein CF (2006) Bosentan, an endothelin receptor antagonist, reduces leucocyte adhesion and inflammation in a murine model of inflammatory bowel disease. Int J Color Dis 21:409–418
Cheluvappa R, Luo AS, Palmer C, Grimm MC (2011) Protective pathways against colitis mediated by appendicitis and appendectomy. Clin Exp Immunol 165:393–400
Cheluvappa R, Luo AS, Grimm MC (2014) T helper type 17 pathway suppression by appendicitis and appendectomy protects against colitis. Clin Exp Immunol 175:316–322
Cheluvappa R, Luo AS, Grimm MC (2014) Autophagy suppression by appendicitis and appendectomy protects against colitis. Inflamm Bowel Dis 20:847–855
Subramanian A, Tamayo P, Mootha VK, Mukherjee S, Ebert BL, Gillette MA, Paulovich A, Pomeroy SL, Golub TR, Lander ES, Mesirov JP (2005) Gene set enrichment analysis: a knowledge-based approach for interpreting genome-wide expression profiles. Proc Natl Acad Sci U S A 102:15545–15550
Brazma A (2009) Minimum information about a microarray experiment (MIAME)—successes, failures, challenges. ScientificWorldJournal 9:420–423
Brazma A, Hingamp P, Quackenbush J, Sherlock G, Spellman P, Stoeckert C, Aach J, Ansorge W, Ball CA, Causton HC, Gaasterland T, Glenisson P, Holstege FC, Kim IF, Markowitz V, Matese JC, Parkinson H, Robinson A, Sarkans U, Schulze-Kremer S, Stewart J, Taylor R, Vilo J, Vingron M (2001) Minimum information about a microarray experiment (MIAME)-toward standards for microarray data. Nat Genet 29:365–371
Irizarry RA, Bolstad BM, Collin F, Cope LM, Hobbs B, Speed TP (2003) Summaries of Affymetrix GeneChip probe level data. Nucleic Acids Res 31:e15
Storey JD, Tibshirani R (2003) Statistical significance for genomewide studies. Proc Natl Acad Sci U S A 100:9440–9445
Mootha VK, Lindgren CM, Eriksson KF, Subramanian A, Sihag S, Lehar J, Puigserver P, Carlsson E, Ridderstrale M, Laurila E, Houstis N, Daly MJ, Patterson N, Mesirov JP, Golub TR, Tamayo P, Spiegelman B, Lander ES, Hirschhorn JN, Altshuler D, Groop LC (2003) PGC-1alpha-responsive genes involved in oxidative phosphorylation are coordinately downregulated in human diabetes. Nat Genet 34:267–273
Kuruppu S, Smith AI (2012) Endothelin converting enzyme-1 phosphorylation and trafficking. FEBS Lett 586:2212–2217
Davenport AP, Kuc RE (2000) Cellular expression of isoforms of endothelin-converting enzyme-1 (ECE-1c, ECE-1b and ECE-1a) and endothelin-converting enzyme-2. J Cardiovasc Pharmacol 36:S12–S14
Paasche JD, Attramadal T, Kristiansen K, Oksvold MP, Johansen HK, Huitfeldt HS, Dahl SG, Attramadal H (2005) Subtype-specific sorting of the ETA endothelin receptor by a novel endocytic recycling signal for G protein-coupled receptors. Mol Pharmacol 67:1581–1590
Grossmann S, Higashiyama S, Oksche A, Schaefer M, Tannert A (2009) Localisation of endothelin B receptor variants to plasma membrane microdomains and its effects on downstream signalling. Mol Membr Biol 26:279–292
McCartney SA, Ballinger AB, Vojnovic I, Farthing MJ, Warner TD (2002) Endothelin in human inflammatory bowel disease: comparison to rat trinitrobenzenesulphonic acid-induced colitis. Life Sci 71:1893–1904
Padol I, Huang JQ, Hogaboam CM, Hunt RH (2000) Therapeutic effects of the endothelin receptor antagonist Ro 48-5695 in the TNBS/DNBS rat model of colitis. Eur J Gastroenterol Hepatol 12:257–265
Addenda
The raw microarray data are available in Gene Expression Omnibus. The accession number for microarray data reported here is GSE23914, and the relevant link is http://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE23914.
Conflicts of interest
None to report.
Funding
National Health and Medical Research Council (NHMRC)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cheluvappa, R., Eri, R., Luo, A.S. et al. Endothelin and vascular remodelling in colitis pathogenesis—Appendicitis and appendectomy limit colitis by suppressing endothelin pathways. Int J Colorectal Dis 29, 1321–1328 (2014). https://doi.org/10.1007/s00384-014-1974-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-014-1974-z