Abstract
Background
Transient mutism as a consequence of posterior fossa surgery is a well-known phenomenon. However, it has rarely been reported after focal nonsurgically induced cerebellar damage.
Case report
We describe a 7-year-old child affected by a tumor arising from the quadrigeminal plate who developed transient cerebellar mutism after a spontaneous bleeding which extended to the upper cerebellar vermis. The recovery from mutism started about a week after the bleeding. At the time of the surgical treatment, 8 weeks after the spontaneous intratumoral bleeding, she was only dysarthric.
Discussion
To our knowledge, this is the first pediatric case of presurgical cerebellar mutism due to a hemorrhage of a neoplastic lesion. Moreover, the focality of bleeding allows the confirmation of the role played by the upper vermis in speech control as well as exclusion of surgically induced lesions commonly suggested as possible cause of the cerebellar mutism.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
Cerebellar mutism is a rare but well-described postoperative complication of the surgical treatment of posterior fossa lesions. It is characterized by a total absence of speech in awake and conscious patients after a symptom-free interval varying from a few hours to a couple of days, a subsequent dysarthric period, and a spontaneous recovery varying from a few days [4] to a couple of months [31]. Actually, almost all the cases reported in literature occur in the postoperative period, about 90% of them after tumor resection and, less frequently, following the resection of a vascular malformation [5].
Nonsurgical cases are very rare and usually present a traumatic or, less commonly, an infective etiology. Only three cases of preoperative mutism have been described so far, namely a spontaneous hemorrhage resulting from an arteriovenous malformation in two pediatric patients [2, 5] and a tumor-related mutism in an adult subject [1].
In the present report, we describe a case of presurgical, transient cerebellar mutism due to an upper vermis spontaneous bleeding from a tumor arising from the quadrigeminal plate and extending into superior cerebellum.
Case report
This 7-year-old girl from Togo suddenly developed severe cervical headache and vomit followed by loss of consciousness. She was taken to a local hospital where she was treated with unspecific antiparasitic and antibiotic agents. Eight days later, her clinical conditions improved and, when she regained consciousness, she was mute and unable to stand up. Ten days later, she was transferred to the main hospital of her country. At the admission, the neurological examination revealed severe gait instability, severe dysarthria, and head and four-limb tremor. Computed tomography (CT) scan of the brain, performed 2 weeks after the insult, showed a lesion arising from the inferior part of the quadrigeminal plate and extending into the superior cerebellum, with signs of a recent peritumoral hemorrhage involving the upper cerebellar vermis. The patient’s clinical condition continued to improve under dexamethasone administration. A new CT scan, performed 1 month later, did not disclose any additional finding.
She was transferred to our service on August 2007, 2 months after the ictal episode: at the admission, the neurological examination revealed ataxic gait, moderate dysarthria, and mild dysmetria, prevalent in the left side. The magnetic resonance imaging (MRI) examination of the brain confirmed the presence of an infiltrative lesion, arising from the inferior part of the quadrigeminal plate and the superior velum medullaris, involving the superior cerebellar vermis, with a superodorsal exophytic component. The lesion, 25 × 26 × 25 mm in diameters, showed a heterogeneous signal on T1-weighted images. It heterogeneously enhanced after gadolinium administration (Fig. 1). There was still evidence of the past hemorrhage around the posterior portion of the tumor and the upper vermis (Fig. 1). No hydrocephalus nor anomalies of the spinal cord were detected. The lesion was surgically excised through a suboccipital approach. No split of the cerebellar vermis was performed. Intraoperatively, the signs of the previous hemorrhage of the superior vermis were evident. The postoperative course was uneventful. A postoperative MRI study confirmed the apparently complete resection of the tumor and ruled out postoperative hydrocephalus. The pathological findings were consistent with pilocytic astrocytoma (World Health Organization grade I). When she was discharged, 1 week after surgical intervention, the patient showed good clinical condition and only mild dysarthria.
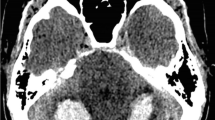
Preoperative MR imaging. Axial T2-weighted (a), sagittal T1-weighted (b), and coronal T2-weighted sequences (c) showing the tumor arising from the posterior part of the quadrigeminal plate and extending up to the superior vermis. The lesion shows a dishomogeneous signal on both T2 (hyperintense) and T1 sequences (hypointense). The remnants of the previous peritumoral hemorrhage (extracellular metahemoglobin) are evident within the posterior and inferior portion of the tumor and the upper vermis (c, d). The tumor dishomogeneously enhances after gadolinium administration (e, f)
Discussion
Cerebellar mutism is an unusual presentation of cerebellar injury. Characteristically, it occurs after a symptom-free interval and spontaneously regresses. In almost all the cases, the recovery is marked by a variable degree of dysarthria that explains why it is also known as “mutism and subsequent dysarthria” [34]. It occurs more often in children than in adults. When associated with behavioral abnormalities and personality changes, it configures the “posterior fossa syndrome.”
When the focal lesions are considered, thus excluding infective processes that diffusely involve the cerebellum, the cerebellar damage resulting in mutism occurs almost always after surgery. Actually, the cerebellar mutism is thought to result from a surgical procedure and its consequences (cerebellar edema or contusion). To date, the occurrence of cerebellar mutism before a surgical operation has been reported only in two pediatric cases affected by cerebellar arteriovenous malformation (AVM) [2, 5] and in an adult patient harboring a cerebellar cystic hemangioblastoma [1]. The clinical onset of our patient was characterized by severe acute headache and quickly progressing loss of consciousness due to the sudden bleeding, like in the other two preoperative pediatric cases. Differently from them, however, the cause was not represented by a vascular malformation but by a low-grade astrocytoma that is rarely burdened by intratumoral bleeding and was not reported as cause of preoperative cerebellar mutism yet.
The pathogenesis of the cerebellar mutism is still unknown, despite the large number of publications on this subject [14, 18, 23, 27]. The most important pathogenetic hypothesis and the sites of lesion proposed as anatomical substrate of cerebellar mutism are summarized on Table 1.
One of the possible mechanisms explaining the occurrence of mutism after a cerebellar hemorrhage is the posthemorrhagic spasm of the cerebellar arteries and the subsequent edema, as proposed by some authors [15, 25]. Such a mechanism could justify the presence of a mutism-free interval, as occurred in the case reported by Baillieux and coworkers [5]. The authors described a pediatric patient who presented a brief loss of consciousness after bleeding of a cerebellar AVM and showed mutism after 1-day free interval. In the other pediatric preoperative case from the literature, described by Al-Anazi et al. [2], as well as in the present one, the patient appeared mute after regaining consciousness. In these instances, the absence of a mutism-free interval could be justified by the longer comatose period (5 and 8 days, respectively).
In the two previously published cases, the cerebellar hemorrhage extended to the dentate nucleus that is believed to be involved in the occurrence of cerebellar mutism when damaged [3, 6, 16]. This hypothesis is not shared by all the authors [11, 15, 24]. In our case, actually, the hemorrhage involved the upper cerebellar vermis, sparing the dentate nucleus. The shared feature among the cases here considered is the involvement of the midline cerebellar structures and we could speculate about their possible role in the pathogenesis of preoperative mutism. Damage of midline cerebellar or brain stem structures, indeed, is reported to increase the risk of developing postoperative cerebellar mutism, occurring in 91.5% of the pediatric cases and in 69.2% of the adult ones [23], although it is not considered to be an independent risk factor [8, 29].
The role of hydrocephalus as possible cause of mutism is debated [14, 18, 22, 30]. The adult patient reported by Akil et al. [1] showed a preoperative cerebellar mutism resulting from a hemangioblastoma of the left cerebellar hemisphere, exerting only a compression on the vermis with its cystic component, and from the associated severe hydrocephalus (no signs of hemorrhage were present). Hydrocephalus, however, was missing in our patient as well as in the two other aforementioned children.
Because of the very small number of cases of preoperative mutism and their inhomogeneous clinical and radiological features, it is very hard to give some hypotheses about the pathogenesis of the speech disturbance. However, the case here presented appears to confirm the role of the upper cerebellar vermis in speech while excluding the involvement of the dentate nucleus as essential cause of cerebellar mutism.
References
Akil H, Statham PFX, Gotz M, Bramley P, Whittle IR (2006) Adult cerebellar mutism and cognitive–affective syndrome caused by cystic hemangioblastoma. Acta Neurochir (Wien) 148:597–598
Al-Anazi A, Hassounah M, Sheikh B, Barayan S (2001) Cerebellar mutism by arteriovenous malformation of the vermis. Br J Neurosurg 15:47–50
Ammirati M, Mirzai S, Samii M (1989) Transient mutism following removal of a cerebellar tumor: a case report and review of the literature. Childs Nerv Syst 5:12–14
Asamoto M, Ito H, Suzuki N, Oiwa Y, Sito K, Haraoka J (1994) Transient mutism after posterior fossa surgery. Child Nerv Syst 10:275–278
Baillieux H, Weyns F, Paquier P, De Deyn PP, Marien P (2007) Posterior fossa syndrome after a vermian stroke: a new case and review of the literature. Pediatr Neurosurg 43:386–395
Cakir Y, Karakisi D, Koçanaogullari O (1994) Cerebellar mutism in an adult: case report. Surg Neurol 41:342–344
Catsman-Berrevoets CE, VanDongen HR, Zwetsloot CP (1992) Transient loss of speech followed by dysarthria after removal of posterior fossa tumour. Dev Med Child Neurol 34:1102–1109
Catsman-Berrevoets CE, VanDongen HR, Mulder PGH, Paz y Geuze M, Paquier PF, Lequin MH (1999) Tumour type and size are high risk factors for the syndrome of cerebellar mutism and subsequent dysarthria. J Neurol Neurosurg Psychiatry 67:755–757
Crutchfeld JS, Sawaya R, Meyers CA, Moore BD III (1994) Postoperative mutism in neurosurgery. J Neurosurg 81:115–121
Dailey AT, McKhann GM, Berger MS (1995) The pathophysiology of oral pharyngeal apraxia and mutism following posterior fossa tumor resection in children. J Neurosurg 83:467–475
Dietze DD, Mickle JP (1990–1991) Cerebellar mutism after posterior fossa surgery. Pediat Neurosurg 16:25–31
Ersahin Y (1998) Is splitting of the vermis responsible for cerebellar mutism? Pediatr Neurosurg 28:328
Ersahin Y, Mutluer S, Cagli S, Duman Y (1996) Cerebellar mutism: report of seven cases and review of the literature. Neurosurg 38:60–65
Ersahin Y, Muttluer S, Saydam S, Barçin E (1997) Cerebellar mutism: report of two unusual cases and review of the literature. Clin Neur Neurosurg 99:130–134
Ferrante L, Mastronardi L, Acqui M, Fortuna A (1990) Mutism after posterior fossa in children. J Neurosurg 72:959–963
Fraioli B, Guidetti B (1975) Effect of stereotactic lesions of the dentate nucleus of the cerebellum in man. Appl Neurophysiol 38:81–90
Frim DM, Ogilvy CS (1995) Mutism and cerebellar dysarthria after brain stem surgery: case report. Neurosurg 36:854–857
Gelabert-Gonzalez M, Fernandez-Villa J (2001) Mutism after posterior fossa surgery. Review of the literature. Clin Neurol Neurosurg 103:111–114
Germanò A, Baldari S, Caruso G, Caffo M, Montemagno G, Cardia E, Tomasello F (1998) Reversible cerebral perfusion alterations in children with transient mutism after posterior fossa surgery. Childs Nerv Syst 14:114–119
Hirsch JF, Renier D, Czernichow P, Benveniste L, Pierre-Khan A (1979) Medulloblastoma in childhood. Survival and functional results. Acta Neurochir (Wien) 48:1–15
Holmes G (1917) The symptoms of acute cerebellar injuries due to gunshot injuries. Brain 40:461–535
Humphreys RP (1989) Mutism after posterior fossa surgery. In: Marlin AE (ed) Concepts in pediatric neurosurgery, vol. 9. Karger, Basel, pp 57–64
Ildan F, Tuna M, Erman T, Goçer AI, Zeren M, Cetinalp E (2002) The evaluation and comparison of cerebellar mutism in children and adults after posterior fossa surgery: report of two adult cases and review of the literature. Acta Neurochir (Wien) 144:463–473
Lechtemberg R, Gilman S (1978) Speech disorders in cerebellar disease. Ann Neurol 3:285–290
Nagatani K, Waga S, Nakagawa Y (1991) Mutism after removal of a vermian medulloblastoma: cerebellar mutism. Surg Neurol 36:307–309
Ozek M, Pamir N, Alptekin B (1993) Mutism after total removal of an exophytic pontine glioma. Turk Neurosurg 3:37–39
Ozgur BM, Berberian J, Aryan HE, Meltzer HS, Levy ML (2006) The pathophysiologic mechanism of cerebellar mutism. Surg Neurol 66:18–25
Pollack IF, Polinko P, Albright LA, Towbin R, Fitz C (1995) Mutism and pseudobulbar symptoms after resection of posterior fossa tumors in children: incidence and pathophysiology. Neurosurg 37:885–893
Robertson PL, Muraszko KM, Holmes E, Sposto R, Packer RJ, Gajjar A, Dias MS, Allen JC (2006) Incidence and severity of postoperative cerebellar mutism syndrome in children with medulloblastoma: a prospective study by the Children’s Oncology Group. J Neurosurg 105(6 Suppl Pediatrics):444–451
Salvati M, Missori P, Lunardi P, Orlando ER (1991) Transient cerebellar mutism after posterior cranial fossa surgery in an adult. Clin Neurol Neurosurg 93:313–316
Siffert J, Poussaint TY, Goumnerova LC, Scott RM, LaValley B, Tarbell NJ, Pomeroy SL (2000) Neurological dysfunction associated with postoperative cerebellar mutism. J Neur Oncol 48:75–81
Stein BM, Fraser RAR, Tenner MS (1972) Normal pressure hydrocephalus: complication of posterior fossa surgery in children. Pediatrics 49:50–58
Turgut M (1998) Transient cerebellar mutism. Childs Nerv Syst 14:161–166
VanDongen HR, Catsman-Berrevoets CE, VanMourik M (1994) The syndrome of ‘cerebellar’ mutism and subsequent dysarthria. Neurology 44:2040–2046
Conflict of interest statement
The authors do not report any conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Frassanito, P., Massimi, L., Caldarelli, M. et al. Cerebellar mutism after spontaneous intratumoral bleeding involving the upper cerebellar vermis: a contribution to the physiopathogenic interpretation. Childs Nerv Syst 25, 7–11 (2009). https://doi.org/10.1007/s00381-008-0711-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-008-0711-8