Abstract
Introduction
The peritoneal cavity is the most common site of cerebrospinal fluid absorption in hydrocephalus treatment. Many distal catheter complications are the result of this type of treatment, and these have been extensively described in the neurosurgical literature.
Materials and methods
In our study, six cases of distal catheter migration with visceral perforation and/or extrusion are presented: three through the umbilicus, two through the scrotum, and one through the anus. An extensive review of the literature was performed.
Results
The studies of peritoneal dialysis models for the treatment of chronic renal failure patients provide important data about solute absorption in the peritoneal cavity and reactivity of the peritoneal membrane.
Conclusion
This model, when compared to distal catheter complications on a ventriculoperitoneal (VP) shunt, presents similarities that could help understand the mechanism of the nonfunctional complications of the distal VP catheter (complication with functional shunt), providing valuable data to support an inflammatory mechanism.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The peritoneal cavity is the most common site for cerebrospinal fluid (CSF) absorption on hydrocephalus treatment. It was first used by Ferguson (1898), through a lumboperitoneal shunt system, and it was later popularized by Nulsen and Spitz (1952) and Holter and Pudenz (1956) [7]. With the advent of the silicon rubber (silicon elastomer) as a biocompatible material and one-way valvular systems, a new age on hydrocephalus treatment had begun [23].
Much knowledge was acquired about CSF physiology on hydrocephalus, and advancements in image techniques improved diagnosis and prognosis, creating a great expectation in the neurosurgical population. However, the diversion of CSF from the ventricles to the peritoneal cavity is still the most common treatment modality. One could expect an immediate recovery of the CSF physiology after ventriculoperitoneal (VP) shunting, but a high morbidity and mortality rate is frequently observed due to several complications.
There are no available studies in the literature to provide some useful data about how the CSF is absorbed in the peritoneal cavity because there are no reports showing the relationships between the silicon catheter, the CSF and its contents (especially glucose and proteins), and the structures in the peritoneal cavity (mainly the peritoneal membrane).
Abdominal complications related to distal catheter migration and visceral perforation and/or extrusion [1, 3, 5, 6, 15, 17, 18, 21, 25–30, 32, 35–37], ascitis [2, 16], and peritoneal pseudocysts [14, 34] have been recognized and treated in neurosurgical practice, and these complications can be grouped and named as “nonfunctional abdominal complication of distal catheter” once the VP shunt still works, although their mechanisms are still not well established.
Most papers related to the peritoneal dialysis model (PDM) for the treatment of patients with chronic renal failure provide interesting data about absorption and solute exchange in the peritoneal cavity, as well as about peritoneal membrane reactivity to the presence of foreign bodies, like silicon elastomer [4, 9, 22, 24, 31].
The goals of our study are:
-
To share our experience in the treatment of six patients with abdominal complications related to VP shunt system (distal catheter migration and/or visceral perforation) for the treatment of hydrocephalus (Table 1).
-
To perform an extensive review about these complications from all papers published in the literature from 1966 to 2003 (Table 2).
-
To study the PDM for the treatment of chronic renal failure and to compare with abdominal complications of VP shunt system in hydrocephalus treatment.
-
To group all abdominal complications of distal catheter in hydrocephalus treatment with migrations, perforation and/or extrusion, and ascitis and peritoneal pseudocyst, and classify as “No functional abdominal complications of the distal catheter.”
Materials and methods
Two hundred eighty-two pediatric patients with hydrocephalus from several etiologies were studied retrospectively from October 1995 to March 2003 (data obtained from the Neurosurgery Service of Hospital “Dr. José de Carvalho Florence” in São José dos Campos City, São Paulo, Brazil). All children were submitted to VP shunting, and six patients presented no functional abdominal complications related to the abdominal catheter (migration, visceral perforation and/or distal catheter extrusion through the anus, vagina, umbilical scar, and scrotum), as shown in Table 1.
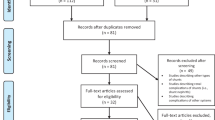
After an extensive review of all papers published from 1966 to 2003, 84 papers related to these complications were found, performing a total of 159 cases (Table 2). A study on PDM was also carried out.
Results
After reviewing the literature, a prevalence in men for these complications (47.5%) over women (26.9%) was found, performing a total of 119 cases. In 25.62% of the cases, gender was not referred by the authors.
The age of the first VP shunt on each patient varied from a few days to 58 years. In 66.7% of the patients, they were less than 1 year old (usually between the first and tenth month of life). In 22.98% of the patients, the age varied between 1 and 10 years, with only 10.34% of them older than 10 years, performing a total of 87 described cases. In 72 patients, there was no reference to their age (45.3%).
The children’s age at the time of each complication varied from a few days to 1 year in 30% of the patients. The age at the time of complication varied from 11 months to 10 years in 46.7% of the patients, while the complications occurred after 10 years in only 22.22% of the patients (90 cases). In 69 (43.4%) patients, there was no reference to age.
The time relation between the first VP shunt and its complication occurred in 57.5% of the patients in the 1st year after VP shunt implantation, 22.5% in the 2nd year after VP shunt implantation, and 20% between the 3rd and 12th year after VP shunt implantation (a total of 80 cases). In 49.7% of patients, we had no such information.
The analysis of the available data has identified the presence of fibrosis around the distal catheter and at the site where it was originally placed in the peritoneal cavity as the common factor to all these complications, and many authors also mentioned multiple VP shunt reviews and previous abdominal surgeries as possible factors related to complications, as well as the length of the distal catheter. However, the mechanism leading to fibrosis formation was not conclusive [1, 2, 16, 17, 33–35, 37].
Discussion
Hydrocephalus treatment remains a great challenge to neurosurgeons, and CSF diverting from the ventricular system to the peritoneal cavity is still the most common treatment modality.
Ventriculoperitoneal shunts usually provide an immediate relief of intracranial hypertension, and it is quite simple to be performed. Unfortunately, the complication rate is high, mostly related to infection (skin, ventricle system, subcutaneous space, and peritoneal cavity) and due to obstruction (of the proximal catheter by choroids plexus, ventricular wall, cerebral parenchyma, blood, and other debris) [11]. The catheters may fracture in its long trajectory at the subcutaneous tissue [13] or by a biodegradation process that occurs during system implantation, posttrauma [8, 10], or by the formation of a bacterial biofilm on the catheter surface [12]. Many abnormalities are found on the catheter surface implanted after long periods, and these can be responsible by bacterial adhesion (data assessed by electronic microscopy) [19, 20]. There is also evidence that CSF proteins are absorbed at the catheters and act as another responsible factor for biodegradation and bacterial adhesion [11].
Little importance is given in the literature to the peritoneal cavity in relation to how CSF is absorbed. Although the silicon elastomer is considered an inert material and designed to remain in the body for very long periods, the CSF will probably be absorbed by the same mechanisms involved in the normal peritoneal liquid absorption, through the specialized structures called stomata, especially at the diaphragm site [4, 9].
The PDM, especially the chronic ambulatory peritoneal dialysis (CAPD) for the treatment of chronic renal failure, employs foreign material such as Tenckhoff & Schecter catheter (silicon) and dialysis solution (saline solution containing dextrose) into the peritoneal cavity for long periods of time for removing toxic substances by means of diffusion and ultrafiltration [4, 9, 31].
The ultrafiltration process is the mechanism by which liquids are removed from the blood through an osmotic pressure gradient (primary mechanism) to the dialyzed solution by hydrostatic pressure mechanism. The studies confirm the presence of small pores, which are responsible for the flow of low molecular weight substances such as urea, creatinine, glucose, as well as the presence of large pores, which are responsible for the flow of high molecular weight substances. Larger pores, so-called “aquapores,” were identified and therefore facilitate the passage of substances with higher molecular weight [4, 9, 31].
The CAPD cycle varies from 4 to 8 continuous hours and employs a total of 56 l of dialysis solution per week. This continuous exposure of the peritoneal membrane to the dialysis solution can result in significant changes on its morphology and ultrastructure with a potential risk of peritoneal fibrosis, documented at PDM studies [24].
In fact, the success of this kind of treatment depends on the functional integrity of the peritoneal membrane and of the vascular mesothelium. The abnormalities described in the morphology and ultrastructure of the peritoneal membrane occur especially at the peritoneal mesothelium, with an increased development of the wrinkled endoplasmatic reticulum and a decrease in membrane microvilosities (responsible for the increase in its surface area), micropinocytic vesicles, and changes on the submesothelial layer, leading to a rare sclerosis effect on the connective tissue.
It is speculated that the glucose present in the dialysis fluid could be potentially toxic to the mesothelial cells in animal models. The glucose passes through the mesothelium easily in extremely high concentration and can lead to damage of mesothelium and vascular changes in the peritoneal tissue [24].
The absorption rate of the peritoneal fluid through the lymphatics ranges from 0.5 to 1.5 ml/min, with the peak absorption occurring through diaphragmatic lymphatics, especially at the subdiaphragmatic region, where there are open intracellular channels or so-called “stomata.” These are conducted to the mediastimal lymphatic and localized before the right lymphatic duct, so it can then reach the right internal jugular and subclavian veins [9].
The studies on cell biology of isolated peritoneal membrane in humans explore the potential that these cells have to yield immunomediation in response to a proinflammatory reaction. The presence of foreign bodies inside the peritoneal cavity activates macrophages (first defense line) and monocytes, which stimulate mesothelial cells to produce immunomediators [interleukins (IL)]. Initially, macrophages and monocytes are activated, which results in primary immunomediation such as IL-β1, a tumor necrosis factor alpha (TNF-α), as well as prostaglandin 2 (PGE-2) and prostacyclin 2 (PGI-2). These primary immunomediators activate IL-6 and IL-8, which are found in great amounts in dialyzed patients with peritonitis. The IL-8 attracts neutrophils to the inflammatory site, while the IL-6, PGE-2, and PGI-2 act as a limitary of the inflammatory reaction. It is postulated that IL-β1 yielded by monocytes and macrophages may have an important role in physiopathology of peritoneal fibrosis and can therefore increase collagen synthesis to an elevated level of procollagen in fibroblasts. There are evidences that indicate that peritoneal fibroblasts (second on the defense line) may respond to inflammatory stimuli by spreading and increasing the extracellular matrix compounds, with a potential contribution for the development of peritoneal fibrosis in patients undergoing CAPD [9, 22].
Curiously, in most publications related to complications such as migration, perforation, and/or extrusion of the distal catheter through the anus, a strong fibrosis reaction surrounding the distal catheters and structures was verified by the authors at the sites where the perforations had occurred [1, 33, 36, 37]; however, it was not clear how this process occurred or if there was enough time for the fibrosis to develop and why it happens in only some patients.
Bowel peristaltic movements and increased intra-abdominal pressures are referred by the authors as a constant source of mechanical pressure before perforation due to necrosis at the site of the anchoring [1, 33]. It is also mentioned that the weakness of certain peritoneal areas and the umbilical end of the vitellointestinal duct and the processus vaginalis into the scrotum might have remained patent, which could act as a facilitating mechanism for perforation [6, 25, 32].
Conclusion
Based on the existing data, we concluded that the PDM may be as an important parameter for a more detailed study about CSF absorption in the peritoneal cavity, and there may be an important interaction between the silicon tubes of a VP shunt system, the CSF contents (especially the glucose and the proteins), and the reactivity of the peritoneal membrane for the production of well-known immunomediators involved in the inflammatory reaction associated to foreign body response in the peritoneum.
The inflammatory reactions can damage the ultrastructure of the peritoneal membrane and impair CSF absorption (ascitis for example), the anchoring mechanisms of the fibrosis on the tip of the distal catheter (peritoneal pseudocyst for example), at the viscerae (the bowel for example) and in weak parts of the peritoneum (the vagina for example), or in sites where ducts are still patent (processus vaginalis into the scrotum and vitellointestinal duct), aided by intra-abdominal pressure and peristalsis movement. All these factors together may act as a “common factor” and are responsible for the “nonfunctional abdominal complication related to the distal catheter” and a possible chronic inflammatory nature in different stages.
References
Abu-Dalu K, Pode D, Hadani M, Sahar A (1987) Colonic complications of ventriculoperitoneal shunts. Neurosurgery 13(2):167–169
Adegbite AB, Khan M (1982) Role of protein content in CSF ascitis following ventriculoperitoneal shunting. J Neurosurg 57:423–425
Adeloye A (1973) Spontaneous extrusion of the abdominal tube through the umbilicus complicating peritoneal shunt for hydrocephalus. J Neurosurg 38:758–760
Alexander SR (1994) Peritoneal dialysis. In: Holliday MA, Barratt TM, Avner ED (eds) Pediatric nephrology, 3rd edn. Williams & Wilkins, Baltimore, pp 1339–1353
Alonso-Vanegas M, Alvarez JL, Delgado L, Mendizábal R, Jiménez JL, Sanches-Cabrera JM (1994) Gastric perforation due to ventriculoperitoneal shunt. Pediatr Neurosurg 21:192–194
Antunes ACM, Ribeiro TR (1975) Spontaneous umbilical fístula from ventriculoperitoneal shunt drainage. J Neurosurg 43:481–482
Aronyk KE (1993) The history and classification of hydrocephalus. Neurosurg Clin N Am 4(4):599–609
Bouch AL, Hermelin E, Sainte-Rose C, Sgouros S (1998) Mechanical dysfunction of ventriculoperitoneal shunts caused by calcification of silicone rubber catheter. J Neurosurg 88:975–982
Burkart JM (2002) Peritoneal dialysis. In: Brenner BM, Rectors FC Jr (eds) The kidney, vol 2, 5th edn. Saunders, Philadelphia, pp 2454–2517
Cuka GM, Helbusch LC (1995) Fractures of the peritoneal catheter of cerebrospinal fluid shunts. Pediatr Neurosurg 22:101–103
Del Bigio MR (1998) Biological reaction to cerebrospinal fluid shunts devices: a review of the cellular pathology. Neurosurgery 42(2):319–325
Drake JM, Sainte-Rose C (1995) The shunt book. Blackwell, Cambridge, pp 123–192
Elisevich K, Mattar AG, Cheeseman F (1994) Biodegradation of distal shunt catheter. Pediatr Neurosurg 21:71–76
Er°ahin Y, Mutluer S, Tekeli G (1996) Abdominal cerebrospinal fluid pseudocysts. Childs Nerv Syst 12:755–758
Fermin S, Fernández-Guerra RA, Sureda PJ (1996) Extrusion of peritoneal catheter through the mouth. Childs Nerv Syst 12:553–555
Gil Z, Beni-Adani L, Siomin V, Nagar H, Dvir R, Constantini S (2001) Ascitis following ventriculoperitoneal shunting in children with chiasma-hypothalamic glioma. Childs Nerv Syst 17:395–398
Giuffrè R, Di Lorenzo N (1975) Two unusual complications of ventriculo-peritoneal shunt in the same infant. Surg Neurol 3:23–24
Gelabert González M (1987) Extrusion of peritoneal catheter through the anus. Childs Nerv Syst 3:183–184
Guevara JA, La Torre J, Denoya CD, Zúccaro G (1981) Microscopic studies in shunts for hydrocephalus. Childs Brain 8:193–284
Guevara JA, Zúccaro G, Trevisán A, Denoya CD (1987) Bacterial adhesion to cerebrospinal fluid shunts. J Neurosurg 67:438–445
Johnson MC, Maxwell MS (1995) Delayed intrapleural migration of a ventriculo-peritoneal shunt. Childs Nerv Syst 11:348–350
Jörres A, Ludat K, Sander K, Dunkel K, Lorenz F, Keck H, Frei U, Gahl GM (1996) The peritoneal fibroblast and the control of peritoneal inflammation. Kidney Int 50(Suppl 56):S22–S27
Kalousdian S, Karlan MS, Willians MA (1998) Silicone elastomer cerebrospinal fluid shunt systems. Neurosurgery 42(4):887–892
Krediet RT (1999) The peritoneal membrane in chronic peritoneal dialysis. Kidney Int 55:341–356
Kwork CK, Yes CP, Wen HL (1989) Bilateral scrotal migration catheter: a rare complication of ventriculoperitoneal shunt. Surg Neurol 31:330–331
Lortat-Jacob S et al (1984) Complications abdominals des shunts ventriculo-péritoneaux chez l’enfant: 65 observations. Chir Pediatr 25:17–21
Martin LM, Donaldson-Hugh ME, Cameron MM (1997) Cerebrospinal fluid hydrothorax caused by transdiaphragmatic migration of a ventriculo-peritoneal catheter through the foramen of Bochdalek. Childs Nerv Syst 13:282–284
McAulay D, Dick AC, Paterson A (2001) Peritoneography in the assessment of peritoneal cerebrospinal fluid absorption. Neurosurgery 49(5):1267–1269
Mozingo JR, Cauthen JC (1974) Vaginal perforation by a Raimondi peritoneal catheter in a adult. Surg Neurol 2:195–196
Nagulic M, Djordjevic M, Samardzie M (1996) Peritoneo-vulvar catheter extrusion after shunt operation. Childs Nerv Syst 12(4):222–223
Nolph KD (1991) Peritoneal dialysis. In: Brenner BM, Rector FC Jr (eds) The kidney, vol 2, 4th edn. Saunders, Philadelphia, pp 2299–2335
Ramani PS (1974) Extrusion of abdominal catheter of ventriculoperitoneal shunt into the scrotum. J Neurosurg 40:772–773
Rubin RC, Ghatak NR Visudhipan P (1972) Asymptomatic perforated viscus and gram-negative ventriculitis as a complication of valve-regulated ventriculoperitoneal shunts. J Neurosurg 37:616–618
Salomão JF, Leibinger RD (1999) Abdominal pseudocysts complicating CSF shunting in infant and children: report of 18 cases. Pediatr Neurosurg 31:274–278
Schulhof LA, Worth M, Kalsbeck JE (1975) Bowel perforation due to peritoneal shunt: a report of seven cases and review of the literature. Surg Neurol 3:265–269
Snow RB, Lavyne MH, Fraser RAR (1986) Colonic perforation by ventriculoperitoneal shunts. Surg Neurol 25:173–177
Wilson CB, Bertan V (1966) Perforation of the bowel complicating peritoneal shunt for hydrocephalus. Am Surg 32(9):601–603
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Aquino, H.B., Carelli, E.F., Borges Neto, A.G. et al. Nonfunctional abdominal complications of the distal catheter on the treatment of hydrocephalus: an inflammatory hypothesis?. Childs Nerv Syst 22, 1225–1230 (2006). https://doi.org/10.1007/s00381-005-0025-z
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-005-0025-z