Abstract
The current therapeutic regimen recommended by the European League against Rheumatism (EULAR) for anti-neutrophil cytoplasmic antibody-associated vasculitis (AAV) is continuation of initially administered doses of glucocorticoids (GCs) in combination with cyclophosphamide (CYC) for 1 month followed by gradual tapering. Considering the adverse effects of GCs, another tapering regimen of GCs with CYC, which was characterized by tapering GCs weekly, was reported by the British Society of Rheumatology (weekly-reduction regimen). The aim of the present study is to evaluate the safety and efficacy of this weekly-reduction regimen for Japanese AAV patients in comparison with the monthly-reduction regimen recommended by the EULAR. We retrospectively reviewed medical records of adult patients newly diagnosed with AAV during the period from April 2000 to December 2010. The outcome measures were rates of remission, relapse, infection, and GC-induced diabetes mellitus during the first 12 months. Clinical data in the two groups and categorial variables with a possible relation to the outcomes were compared by using the t test and chi-square test, respectively. Twenty-four patients were enrolled in our study. All of the patients achieved remission, and the rates of relapse during the first 12 months were not statistically different between the two groups (P = 0.16). Patients treated with the weekly-reduction regimen were less liable to have infection (P = 0.03) and impaired glucose tolerance (P = 0.017), compared with those treated with the monthly-reduction regimen. A therapeutic strategy using the weekly-reduction regimen of GCs would be effective and would have fewer side effects than the monthly-reduction regimen.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The current therapeutic regimen recommended by the European League against Rheumatism (EULAR) for anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV) is treatment with high-dose glucocorticoids (GCs) in combination with cyclophosphamide (CYC). According to the recommendation, initial dose of GCs (1 mg/kg/day of prednisolone) in combination with CYC should be continued for 1 month followed by gradual tapering [1]. However, the appropriate dose and duration of administration of GCs for the treatment of AAV have not yet been determined. Long-term use of high-dose GCs increases the risk of various complications including infection, which is one of the main causes of morbidity and mortality in patients with rheumatic diseases [2–9]. Moreover, high-dose GCs have been reported to be responsible for the progression of impaired glucose tolerance [10–13]. Considering the effects of GCs on morbidity and mortality, another tapering regimen of GCs in combination with CYC was reported in guidelines published by the British Society of Rheumatology (BSR) in 2007 [14]. This regimen is characterized by tapering GCs weekly. In recent randomized controlled studies by the EULAR and other European researchers, this weekly-reduction regimen of GCs in combination with CYC has been used instead of 1-month continuation of initial high-dose GCs (monthly-reduction regimen) [15–19]. However, the efficacy and safety of this weekly-reduction regimen compared to the monthly-reduction regimen for AAV patients have yet to be elucidated.
The aim of the present study was to determine the safety and efficacy of the weekly-reduction regimen of GCs with CYC for AAV patients in Japan in comparison with the previous protocol, i.e., monthly-reduction regimen of GCs with CYC.
Patients and methods
Subjects
We retrospectively reviewed medical records of adult patients with AAV who were admitted to Okayama University Hospital during the period from April 2000 to December 2010. Patients newly diagnosed with microscopic polyangiitis (MPA) or Wegener’s granulomatosis (WG) who were treated with GCs in combination with intravenous CYC (IVCY) were enrolled in our study. Patients were classified as MPA or WG with the European Medicines Agency (EMEA) algorithm (2007) [20]. Since the purpose of our study was to compare two regimens with a focus on how to taper GCs in combination with IVCY, patients who were administered IVCY more than three times were enrolled in our study. This study was approved by the Ethics Committee of Okayama University Hospital.
Study protocol
Both regimens consisted of oral prednisolone and monthly IVCY. As recommended by the EULAR in 2009, the dose of CYC was reduced in patients with impaired renal function and in patients older than 60 years of age. In the weekly group (treated with the weekly-reduction regimen), prednisolone was tapered according to the BSR guideline (Table 1). Initial dose of prednisolone in the monthly group (treated with the monthly-reduction regimen) was maintained for at least 1 month and then tapered gradually. Administration of IVCY was continued for 3 months after disease remission in both groups. We used prophylaxis for Pneumocystis jiroveci and fungal infection in patients enrolled in our study.
Study endpoints
The primary endpoints were the rates of remission and relapse during the first 12 months after commencement of treatment, and the secondary endpoints were the rate of infection during the first 12 months, and the proportion of patients who had developed and required treatment intervention for GC-induced diabetes mellitus (GC-induced DM) during the first 12 months. The Vasculitis Damage Index (VDI), which scores cumulative damage from any cause since disease onset, was also assessed at 6 and 12 months after commencement of treatment.
Study definitions
We defined disease remission as the absence of new or worse signs of disease activity, with the Birmingham Vasculitis Activity Score (BVAS) index of 0. BVAS indicates manifestations of vasculitis activity during a period of 4 weeks before the date of assessment [21]. We also defined relapse as the recurrence or first appearance of at least one BVAS item.
As in previous studies, infections were confirmed by the existence of supportive clinical features, laboratory findings, positive cultures, and radiographic evidence. When causal organisms were not identified, diagnosis of infections was made on the basis of clinical findings in combination with improvement following antimicrobial therapy [4, 22].
GC-induced DM was defined as hyperglycemia described in the guidelines of the World Health Organization being detected continuously and requiring treatment [23]. Continuous elevation of blood glucose levels (fasting glucose levels ≧126 mg/dl and/or random glucose levels ≧200 mg/dl) was regarded as hyperglycemia.
Statistical analysis
Statistical analysis was performed with JMP® 7 (SAS Institute Inc, USA). Clinical data in the two groups were compared by using the t test, and categorial variables with a possible relation to the outcomes were compared by using the nonparametric chi-square test. Statistical significance was defined as a P value of less than 0.05, two-tailed.
Results
Baseline characteristics
In the period from April 2000 to December 2010, 24 patients were enrolled in our study. Baseline characteristics of the patients in each group are shown in Table 2. The mean ± SEM ages at diagnosis were 72.3 ± 1.9 years in the monthly group and 71.4 ± 1.3 years in the weekly group (P = 0.75). Except for the frequency and types of AAV, the differences between the two groups were not statistically significant. The numbers of patients with diabetes mellitus before treatment were 1 (6.7%) in the monthly group and 3 (33.3%) in the weekly group. Fasting glucose levels and postprandial glucose levels before treatment were similar in the two groups, but HbA1c level before treatment was higher in the weekly group.
Treatment in the two groups
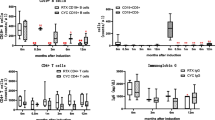
The initial dose of prednisolone in the weekly group was higher than that in the monthly group (0.97 ± 0.05 mg/kg/day vs. 0.67 ± 0.03 mg/kg/day, P < 0.0001), while the daily dose of prednisolone 1 month after the commencement of treatment in the weekly group was lower than that in the monthly group (0.41 ± 0.02 mg/kg/day vs. 0.57 ± 0.03 mg/kg/day, P = 0.0007) (Fig. 1). In addition, the cumulative dose of prednisolone during the first 12 months in the weekly group was lower than that in the monthly group, whereas the cumulative dose of CYC during the first 12 months in the weekly group was higher than that in the monthly group (Table 2).
Disease remission and relapse
All of our patients achieved remission within the first 6 months. During the first 12 months, 13.3% in the monthly group and none in the weekly group had relapse (P = 0.16). VDIs at 6 months (2.7 ± 0.4 in the monthly group and 2.4 ± 0.5 in the weekly group, P = 0.72) and those at 12 months (2.6 ± 0.4 in the monthly group and 2.3 ± 0.6 in the weekly group, P = 0.71) were not statistically different.
Infectious complications
The rate of infectious episodes during the first 12 months in the weekly group was lower than that in the monthly group (10 of the 15 patients in the monthly group and 2 of the 9 patients in the weekly group, P = 0.03) (Table 3). About half of the infections were severe or life-threatening (in 4 of the 10 patients in the monthly group and in both of the 2 patients in the weekly group). The most frequent infection in our study was respiratory infection. No patient died from infectious complications.
Glucocorticoid-induced diabetes mellitus (GC-induced DM)
Comparison of patients who developed GC-induced DM in the two groups is shown in Table 4. During the first 12 months, 13 of 14 patients in the monthly group and 2 of 6 patients in the weekly group without DM before treatment developed GC-induced DM (92.9% in the monthly group and 33.3% in the weekly group, P = 0.017). Interestingly, all of these patients were diagnosed as having GC-induced DM by elevation of postprandial glucose levels ≧200 mg/dl, not by fasting glucose levels ≧126 mg/dl, and GC-induced DM occurred in all patients within the first month (20.3 ± 4.6 days in the monthly group and 10.5 ± 11.8 days in the weekly group) (Table 4). Glucose levels after lunch were drastically elevated by treatment with prednisolone, while fasting glucose and HbA1c levels were not changed (data not shown). Three patients in the monthly group, but none in the weekly group, with GC-induced DM were treated with insulin. Notably, about 50% of the patients with GC-induced DM were treated with anti-diabetic drugs continuously at the end of the observation period.
Discussion
In the present study, all of the patients achieved remission during the first 6 months. In addition, the rates of relapse during the first 12 months and the VDIs at 6 and 12 months after the commencement of treatment were not statistically different between the two groups. In six previous studies, the mean rate of remission induction during the first 6 months was 87% (range, 68–93%) [15–19, 24] and the rate of relapse during the first 12 months was approximately 10% [16]. Although the mean BVAS in our weekly group was almost the same as that in our monthly group and in the six previous studies (17.6 ± 1.6 in the monthly group, 15.0 ± 2.1 in the weekly group, and 18.9 in the CYCAZAREM study group) [16], the rates of remission and relapse in the weekly group were not inferior to those in the monthly group or those in the previous studies. Thus, the efficacy of the weekly-reduction regimen was not inferior to that of the monthly-reduction regimen.
The rate of infectious episodes during the first 12 months in the weekly group was significantly lower than that in the monthly group (Table 3). A review of patients in the European Vasculitis Study Group (EUVAS) trials showed that infection occurred during the first 12 months in 24% of the patients [25], almost the same rate as that in our weekly group, and that 50% of deaths within the first year were caused by infection [25, 26]. Another study showed that a high cumulative dose of CYC increases the risk of infection in AAV patients [27]. Although the cumulative dose of CYC during the first 12 months in the weekly group was high compared to that in the monthly group, the rate of infection in the weekly group was not higher than that in the monthly group. Lower rate of infectious episodes in the weekly group indicated that early reduction in the doses of GCs might reduce infection-related mortality.
We also investigated the safety of the weekly-reduction regimen with a focus on GC-induced DM. The number of patients with GC-induced DM during the first 12 months in the weekly group was smaller than that in the monthly group (Table 4). In previous studies, the rates of GC-induced DM in patients with connective tissue diseases were between 0.4 and 54% [28–33], almost the same as that in our weekly group but lower than that in our monthly group. The large variability in the rate of GC-induced DM may be due to differences in study populations, observation periods, and other factors, including doses of GCs and age, which are known to influence the risk of GG-induced DM [30, 33–40]. The mean age of patients in our study (over 65 years) was more advanced than that of patients in previous studies [16, 41], and our patients were therefore more liable to have impaired glucose tolerance when treated with GCs. Nevertheless, the rate of GC-induced DM in the weekly group was not larger than that in previous studies, suggesting that early reduction in the doses of GCs may reduce GC-induced DM.
Second, all of our patients who had developed GC-induced DM were diagnosed by postprandial glucose levels ≧200 mg/dl within the first month. Iwamoto et al. reported that GC-induced DM was diagnosed in most patients by elevation of postprandial glucose levels, not by fasting glucose and HbA1c levels [33]. The results of their study suggested that measuring only fasting glucose and HbA1c levels is not sufficient to diagnose GC-induced DM, particularly in the early phase of the treatment. Postprandial hyperglycemia is a risk factor for acute inflammation and endothelial dysfunction, leading to cardiovascular diseases [42–45]. However, a clear definition of GC-induced DM was not given in most previous reports on the use of high-dose GCs, and the proportion of patients with GC-induced DM, which should be diagnosed by postprandial hyperglycemia, might have been underestimated. Continuous measurement with a focus on postprandial hyperglycemia is necessary in order not to overlook occult GC-induced DM.
This is the first report on evaluation of a weekly-reduction regimen of GCs compared to a monthly-reduction regimen in combination with CYC for AAV in Japanese patients. The weekly-reduction regimen may be as effective as the monthly-reduction regimen in inducing remission without increase in relapse. In addition, earlier reduction in the doses of GCs is beneficial for reducing onset of infection and diabetes due to decreases in both daily dose and cumulative dose of GCs. Our findings indicate that a therapeutic strategy using the weekly-reduction regimen of GCs would be effective and would have fewer side effects than the monthly-reduction regimen due to decreased risks of infection and diabetes. However, our retrospective study has limitations including selection bias, incompleteness of medical records, and short observation period. A future prospective study with a larger number of AAV patients is needed to confirm our findings and to determine the ideal and cost-beneficial therapeutic regimen for patients suffering from disease activity and adverse effects.
References
Mukhtyar C, Guillevin L, Cid MC, Dasgupta B, de Groot K, Gross W et al (2009) EULAR recommendations for the management of primary small and medium vessel vasculitis. Ann Rheum Dis 68:310–317. doi:10.1136/ard.2008.088096
Noel V, Lortholary O, Casassus P, Cohen P, Genereau T, Andre MH et al (2001) Risk factors and prognostic influence of infection in a single cohort of 87 adults with systemic lupus erythematosus. Ann Rheum Dis 60:1141–1144
Pryor BD, Bologna SG, Kahl LE (1996) Risk factors for serious infection during treatment with cyclophosphamide and high-dose corticosteroids for systemic lupus erythematosus. Arthritis Rheum 39:1475–1482
Bosch X, Guilabert A, Pallares L, Cerveral R, Ramos-Casals M, Bove A et al (2006) Infections in systemic lupus erythematosus: a prospective and controlled study of 110 patients. Lupus 15:584–589
Gladman DD, Hussain F, Ibanez D, Urowitz MB (2002) The nature and outcome of infection in systemic lupus erythematosus. Lupus 11:234–239
Settipane GA, Pudupakkam RK, McGowan JH (1978) Corticosteroid effect on immunoglobulins. J Allergy Clin Immunol 62:162–166
Weiler JM, Packard BD (1982) Methylprednisolone inhibits the alternative and amplification pathways of complement. Infect Immun 38:122–126
Nair MP, Schwartz SA (1984) Immunomodulatory effects of corticosteroids on natural killer and antibody-dependent cellular cytotoxic activities of human lymphocytes. J Immunol 132:2876–2882
Schuyler MR, Gerblich A, Urda G (1984) Prednisone and T-cell subpopulations. Arch Intern Med 144:973–975
Gulliford MC, Charlton J, Latinovic R (2006) Risk of diabetes associated with prescribed glucocorticoids in a large population. Diabetes Care 29:2728–2729. doi:10.2337/dc06-1499
Gurwitz JH, Bohn RL, Glynn RJ, Monane M, Mogun H, Avorn J (1994) Glucocorticoids and the risk for initiation of hypoglycemic therapy. Arch Intern Med 154:97–101
Conn HO, Poynard T (1994) Corticosteroids and peptic ulcer: meta-analysis of adverse events during steroid therapy. J Intern Med 236:619–632
Blackburn D, Hux J, Mamdani M (2002) Quantification of the risk of corticosteroid-induced diabetes mellitus among the elderly. J Gen Intern Med 17:717–720
Lapraik C, Watts R, Bacon P, Carruthers D, Chakravarty K, D’Cruz D et al (2007) BSR and BHPR guidelines for the management of adults with ANCA associated vasculitis. Rheumatology (Oxford) 46:1615–1616. doi:10.1093/rheumatology/kem146a
De Groot K, Rasmussen N, Bacon PA, Tervaert JW, Feighery C, Gregorini G et al (2005) Randomized trial of cyclophosphamide versus methotrexate for induction of remission in early systemic antineutrophil cytoplasmic antibody-associated vasculitis. Arthritis Rheum 52:2461–2469. doi:10.1002/art.21142
Jayne D, Rasmussen N, Andrassy K, Bacon P, Tervaert JW, Dadoniene J et al (2003) A randomized trial of maintenance therapy for vasculitis associated with antineutrophil cytoplasmic autoantibodies. N Engl J Med 349:36–44. doi:10.1056/NEJMoa020286
Gordon M, Luqmani RA, Adu D, Greaves I, Richards N, Michael J et al (1993) Relapses in patients with a systemic vasculitis. Q J Med 86:779–789
Guillevin L, Cordier JF, Lhote F, Cohen P, Jarrousse B, Royer I et al (1997) A prospective, multicenter, randomized trial comparing steroids and pulse cyclophosphamide versus steroids and oral cyclophosphamide in the treatment of generalized Wegener’s granulomatosis. Arthritis Rheum 40:2187–2198. doi:10.1002/1529-0131(199712)40:12<2187:AID-ART12>3.0.CO;2-H
Haubitz M, Schellong S, Gobel U, Schurek HJ, Schaumann D, Koch KM et al (1998) Intravenous pulse administration of cyclophosphamide versus daily oral treatment in patients with antineutrophil cytoplasmic antibody-associated vasculitis and renal involvement: a prospective, randomized study. Arthritis Rheum 41:1835–1844. doi:10.1002/1529-0131(199810)41:10<1835:AID-ART16>3.0.CO;2-Q
Watts R, Lane S, Hanslik T, Hauser T, Hellmich B, Koldingsnes W et al (2007) Development and validation of a consensus methodology for the classification of the ANCA-associated vasculitides and polyarteritis nodosa for epidemiological studies. Ann Rheum Dis 66:222–227. doi:10.1136/ard.2006.054593
Luqmani RA, Bacon PA, Moots RJ, Janssen BA, Pall A, Emery P et al (1994) Birmingham Vasculitis Activity Score (BVAS) in systemic necrotizing vasculitis. Qjm 87:671–678
Yuhara T, Takemura H, Akama T, Suzuki H, Yamane K, Kashiwagi H (1996) Predicting infection in hospitalized patients with systemic lupus erythematosus. Intern Med 35:629–636
World Health Organization (2006) Definition and diagnosis of diabetes mellitus and intermediate hyperglycemia. Report of a WHO consultation. WHO, Geneva
Carruthers D, Sherlock J (2009) Evidence-based management of ANCA vasculitis. Best Pract Res Clin Rheumatol 23:367–378. doi:10.1016/j.berh.2008.12.003
Turnbull J, Harper L (2009) Adverse effects of therapy for ANCA-associated vasculitis. Best Pract Res Clin Rheumatol 23:391–401. doi:10.1016/j.berh.2009.04.002
Booth AD, Almond MK, Burns A, Ellis P, Gaskin G, Neild GH et al (2003) Outcome of ANCA-associated renal vasculitis: a 5-year retrospective study. Am J Kidney Dis 41:776–784
Charlier C, Henegar C, Launay O, Pagnoux C, Berezne A, Bienvenu B et al (2009) Risk factors for major infections in Wegener granulomatosis: analysis of 113 patients. Ann Rheum Dis 68:658–663. doi:10.1136/ard.2008.088302
Kim SY, Yoo CG, Lee CT, Chung HS, Kim YW, Han SK et al (2011) Incidence and risk factors of steroid-induced diabetes in patients with respiratory disease. J Korean Med Sci 26:264–267. doi:10.3346/jkms.2011.26.2.264
Montori VM, Basu A, Erwin PJ, Velosa JA, Gabriel SE, Kudva YC (2002) Posttransplantation diabetes: a systematic review of the literature. Diabetes Care 25:583–592
Panthakalam S, Bhatnagar D, Klimiuk P (2004) The prevalence and management of hyperglycaemia in patients with rheumatoid arthritis on corticosteroid therapy. Scott Med J 49:139–141
Smyllie HC, Connolly CK (1968) Incidence of serious complications of corticosteroid therapy in respiratory disease. A retrospective survey of patients in the Brompton hospital. Thorax 23:571–581
Uzu T, Harada T, Sakaguchi M, Kanasaki M, Isshiki K, Araki S et al (2007) Glucocorticoid-induced diabetes mellitus: prevalence and risk factors in primary renal diseases. Nephron Clin Pract 105:c54–c57. doi:10.1159/000097598
Iwamoto T, Kagawa Y, Naito Y, Kuzuhara S, Kojima M (2004) Steroid-induced diabetes mellitus and related risk factors in patients with neurologic diseases. Pharmacotherapy 24:508–514
Clore JN, Thurby-Hay L (2009) Glucocorticoid-induced hyperglycemia. Endocr Pract 15:469–474. doi:10.4158/EP08331.RAR
Arner P, Gunnarsson R, Blomdahl S, Groth CG (1983) Some characteristics of steroid diabetes: a study in renal-transplant recipients receiving high-dose corticosteroid therapy. Diabetes Care 6:23–25
Willi SM, Kennedy A, Brant BP, Wallace P, Rogers NL, Garvey WT (2002) Effective use of thiazolidinediones for the treatment of glucocorticoid-induced diabetes. Diabetes Res Clin Pract 58:87–96
Pagano G, Cavallo-Perin P, Cassader M, Bruno A, Ozzello A, Masciola P et al (1983) An in vivo and in vitro study of the mechanism of prednisone-induced insulin resistance in healthy subjects. J Clin Invest 72:1814–1820. doi:10.1172/JCI111141
Elphick MC (1968) Modified colorimetric ultramicro method for estimating Nefa in serum. J Clin Pathol 21:567–570
Spiegelman BM (1998) PPAR-gamma: adipogenic regulator and thiazolidinedione receptor. Diabetes 47:507–514
Okumura S, Takeda N, Takami K, Yoshino K, Hattori J, Nakashima K et al (1998) Effects of troglitazone on dexamethasone-induced insulin resistance in rats. Metabolism 47:351–354
de Groot K, Harper L, Jayne DR, Flores Suarez LF, Gregorini G, Gross WL et al (2009) Pulse versus daily oral cyclophosphamide for induction of remission in antineutrophil cytoplasmic antibody-associated vasculitis: a randomized trial. Ann Intern Med 150:670–680
Temelkova-Kurktschiev TS, Koehler C, Henkel E, Leonhardt W, Fuecker K, Hanefeld M (2000) Postchallenge plasma glucose and glycemic spikes are more strongly associated with atherosclerosis than fasting glucose or HbA1c level. Diabetes Care 23:1830–1834
Barrett-Connor E, Ferrara A (1998) Isolated postchallenge hyperglycemia and the risk of fatal cardiovascular disease in older women and men. The Rancho Bernardo Study. Diabetes Care 21:1236–1239
Tominaga M, Eguchi H, Manaka H, Igarashi K, Kato T, Sekikawa A (1999) Impaired glucose tolerance is a risk factor for cardiovascular disease, but not impaired fasting glucose. The Funagata Diabetes Study. Diabetes Care 22:920–924
Ceriello A, Esposito K, Piconi L, Ihnat MA, Thorpe JE, Testa R et al (2008) Oscillating glucose is more deleterious to endothelial function and oxidative stress than mean glucose in normal and type 2 diabetic patients. Diabetes 57:1349–1354. doi:10.2337/db08-0063
Acknowledgments
This work was supported in part by grants from the Ministry of Health, Labour and Welfare, Japan.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Matsumoto, Y., Sada, Ke., Otsuka, F. et al. Evaluation of weekly-reduction regimen of glucocorticoids in combination with cyclophosphamide for anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis in Japanese patients. Rheumatol Int 32, 2999–3005 (2012). https://doi.org/10.1007/s00296-011-2136-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-011-2136-z