Abstract
Background
The life prognosis of elderly patients with myeloperoxidase–anti-neutrophil cytoplasmic antibodies-associated vasculitis (MPO-AAV) has been improved by reducing the corticosteroid or cyclophosphamide dose to avoid opportunistic infection. However, many elderly MPO-AAV patients experience recurrence and renal death. An effective and safer maintenance treatment method is necessary to improve the renal prognosis of MPO-AAV.
Methods
Patients with MPO-AAV who reached complete or incomplete remission after induction therapy were prospectively and randomly divided into mizoribine (MZR; n = 25) and control (n = 28) groups. The primary endpoint was relapse of MPO-AAV. The patients’ serum MZR concentration was measured before (C0) and 3 h after taking the MZR. The maximum drug concentration (Cmax) and the serum MZR concentration curves were determined using population pharmacokinetics parameters. We also assessed the relationship between the MZR concentrations and adverse events. The observation period was 12 months.
Results
Fifty-eight MPO-AAV patients from 16 hospitals in Japan were enrolled. Ten patients relapsed (MZR group, n = 6; control group, n = 4; a nonsignificant between-group difference). Changes in the serum MZR concentration could be estimated for 22 of the 25 MZR-treated patients: 2 of the 11 patients who reached a Cmax of 3 μg/mL relapsed, whereas 4 of the 11 patients who did not reach this Cmax relapsed. The treatment of one patient with C0 > 1 μg/mL was discontinued due to adverse events. No serious adverse events occurred.
Conclusion
There was no significant difference in the recurrence rate of MPO-AAV between treatment with versus without MZR.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anti-neutrophil cytoplasmic autoantibodies (ANCA)-associated vasculitis (AAV) is defined as necrotizing vasculitis with few or no immune deposits, predominantly affecting small blood vessels (i.e., capillaries, venules, arterioles, and small arteries), and it is associated with ANCAs that are specific for myeloperoxidase (MPO) or proteinase 3 (PR3) [1]. Many patients with AAV present rapidly progressive glomerulonephritis (RPGN), and untreated AAV has resulted in poor life and renal prognoses. AAV is classified into three categories: microscopic polyangiitis (MPA), granulomatosis with polyangiitis (GPA), and eosinophilic granulomatosis with polyangiitis (EGPA). PR3-ANCA is most commonly associated with GPA, whereas MPO-ANCA is more commonly associated with MPA.
The treatment of AAV [2, 3] can be divided into two phases: the induction of remission, and maintenance therapy. Induction therapy commonly comprises high-dose glucocorticoids together with a second agent, rituximab, or cyclophosphamide (CYC). The standard maintenance therapy has been rituximab or azathioprine (AZA) after the induction of remission. However, the use of immunosuppressive drugs poses a high risk of infection as a side effect.
Based on the findings of a nationwide survey of RPGN in Japan [4], we concluded that 64.7% of Japanese RPGN patients had ANCAs, and among ANCA-positive patients, approx. 90% had MPO-ANCA. Elderly Japanese AAV/RPGN patients have frequently died due to opportunistic infections during initial treatment, and thus the rate of treatment with corticosteroids alone for AAV has inevitably increased. However, there are many cases in which AAV recurs during maintenance therapy, eventually leading to renal death [5,6,7]. This is a major problem in RPGN treatment in AAV treatment in Japan. The importance of suppressing side effects and stabilizing renal function after an initial treatment for AAV has also been recognized.
Mizoribine (MZR) is a purine metabolism antagonist developed in Japan that is produced as an imidazole nucleic acid-related substance. MZR is an immunosuppressive agent for renal excretion that exerts an immunosuppressive effect in vivo by (1) specifically inhibiting inosine 5ʹ-monophosphate dehydrogenase (IMPDH), which is a rate-limiting enzyme in the de novo synthesis pathway of guanosine nucleotides, and (2) reducing the amount of intracellular guanosine triphosphate (GTP) [8, 9]. A study conducted in Japan reported that among the available immunosuppressive drugs, MZR has fewer side effects and was useful for patients with AAV [10]. However, MZR’s efficacy and optimal administration method and dose have not been established.
Measuring the blood concentrations of an immunosuppressive drug is known to be useful for the monitoring of both proper drug use and appropriate immunosuppression. It was reported that the change in the serum concentration of MZR measured by the population pharmacokinetics (PPK) method can be estimated using a nonlinear mixed effects model (NONMEM) program in healthy male volunteers [11] and adult recipients of renal transplantation [12]. Another investigation used this method to monitor the effects of MZR on idiopathic membranous nephropathy [13]. We conducted the present comparative study of AAV patients treated with MZR and a control AAV group in order to determine the usefulness and safety of MZR in remission maintenance therapy in AAV.
Patients and methods
This Study was entered in the University Hospital Medical Information Network-Clinical Trials Registry (UMIN-CTR) under trial identification no. UMIN 000,000,708.
Patients
Patients diagnosed with MPO-ANCA-associated vasculitis (MPO-AAV) who had achieved complete or incomplete remission after remission–induction therapy were recruited from 16 hospitals in Japan. The patients with MPO-AAV were defined as those who were positive for MPO-ANCA and presented with RPGN. Complete remission (CR) was defined as follows: the condition in which no newly active clinical symptoms of vasculitis are present and the Birmingham Vasculitis Activity Score (BVAS 2003) [14] is 0–1; the absence of deterioration of glomerulonephritis or renal function, and red blood cell cast has disappeared; and the patient's C-reactive protein (CRP) level is within the normal range. A BVAS of 0–1 means that there are no findings of new or worsening clinical symptoms due to vasculitis within the prior 4 weeks. Incomplete remission (ICR) was defined as having stable clinical symptoms, although the BVAS is > 1. Relapse was defined as the re-occurrence or new onset of disease attributable to active vasculitis.
The study’s inclusion criteria were patients who achieved a CR or ICR after remission–induction therapy for MPO-AAV, who provided written consent to participate in this study, and who did not meet any of the following exclusion criteria: age > 80 years at diagnosis, age ≤ 20 years, creatinine clearance < 20 mL/min or undergoing renal replacement therapy, severe hypersensitivity to MZR, a white blood cell (WBC) count < 3000/mm3, pregnancy or possible pregnancy, the use of an immunosuppressive agent or pretreatment with an immunosuppressive agent within the prior 4 weeks, and having been judged to be inappropriate by the patient's treating physician.
Interventions
We prospectively and randomly divided the patients into two groups: the MZR group and control group. The patients in the MZR group received 25–300 mg of MZR once daily before breakfast, depending on their creatinine clearance. The serum concentration of MZR was measured by high-performance liquid chromatography (HPLC) at Toyo Kensa Center (Shizuoka, Japan). Each patient's serum concentration of MZR was measured before (C0) and 3 h after (C3) he or she took the daily MZR, between 1 and 4 weeks after the start of the MZR regimen.
Patients whose C0 value of MZR was > 1 µg/mL at the initial measurement were excluded. We aimed for a C0 value that did not exceed 1 µg/mL and a C3 value at ≥ 3 µg/mL. When the C3 value did not reach 3 µg/mL, the dose of MZR was increased by 25 mg, and 4 weeks later, the serum MZR concentration was measured and adjusted to achieve the target. The patients in the control group did not receive MZR. The doses of corticosteroids were adjusted depending on the patients' symptoms. In principle, a concomitant use of other immunosuppressant agents was not permitted. The observation period was 12 months.
Data collection
During the trial, the patients’ clinical symptoms and laboratory test findings were examined at the start of the MZR regimen and 1, 3, 6, and 12 months later. Their height, weight, sitting blood pressure, presence/absence of edema, and other symptoms were checked; the daily urinary protein level, urinary creatinine concentration, urinary red blood cell count, complete blood count, blood biochemical data including total protein, albumin, total cholesterol, triglyceride, urea nitrogen, creatinine, electrolytes, uric acid, aspartate aminotransaminase, alanine aminotransferase, blood sugar, and CRP values were determined. The results of immunological tests including MPO-ANCA and immunoglobulin were obtained. Chest X-rays and the BVAS data were obtained at the start of the MZR regimen and 6 and 12 months later.
The primary endpoints of the study were the relapse rate, the length of time from remission to relapse, and the patient's BVAS throughout the study period. Secondary endpoints were the values of MPO-ANCA, CRP, and renal function as indicated by the creatinine clearance calculated by the Cockcroft–Gault formula (CLcr). Each item was evaluated at the start of the MZR regimen and 1, 3, 6, and 12 months later.
Estimation of the serum concentrations of MZR
Ishida et al. estimated the population pharmacokinetics (PPKs) of MZR by using a NONMEM program for 114 adult renal transplantation recipients who were treated with MZR [12]. Honda et al. described the PPKs of MZR by using a simple one-compartment model with first-order absorption [11]; their findings confirmed that renal function is the main factor responsible for the interindividual pharmacokinetic variability of MZR. They showed that the relationship between MZR oral clearance (CL/F) and creatinine clearance (CLcr), plus the relationship between MZR’s apparent volume of distribution (V/F) and body weight (WT) can be expressed as follows:
They identified the mean values for A, B, the absorption lag time (ALAG), and the absorption rate constant (ka).
We estimated the ka, CL/F, and V/F of each patient by using their MZR daily dosage and their values of C0, C3, CLcr, and WT by Bayesian inference based on the above-mentioned PPK parameters. When a drug is repeatedly administered at a dose of X0 and an administration interval of τ to reach a steady state, the blood concentration at time t after the administration of the drug is expressed as follows:
Css,t is the blood concentration (μg/mL) at time t after administration under the steady state, X0 is the dose (μg), ka is the absorption rate constant (1/hr), kel is the disappearance rate constant (1/hr), Vd is the volume of distribution (mL), F is the absorption rate, and τ is the dosing interval (hr). Using these data, we calculated the maximum drug concentration (Cmax), and the serum MZR concentration curves.
Statistical analyses
The results are expressed as the mean ± standard deviation. Differences between two groups were evaluated by the Mann–Whitney U test. Differences among four groups were evaluated by the Kruskal–Wallis test. The differences in ratios were tested with Fisher's exact test. Time-to-event analyses were performed using the Kaplan–Meier technique, and the curves were compared with the log-rank test. Probability (p) values < 0.05 were considered statistically significant. All statistical tests were two-sided. All analyses were performed with IBM SPSS Statistics ver. 27.
Results
Patients’ profiles
Between November 1, 2008 and December 31, 2011 a total of 58 patients with MPO-AAV were enrolled from 16 hospitals in this study. We randomly divided the 58 patients into two groups of 29 each, i.e., the MZR-treated group and the control (non-MZR-treated) group. In the MZR group, two patients withdrew their consent, and one patient withdrew due to a malignant tumor after providing study participation consent. One patient in the control group withdrew consent. Twenty-six patients; thus, received MZR, but one case was discontinued and excluded from the analysis because the patient’s C0 exceeded 1 μg/mL and the patient experienced an adverse event early in the treatment period. A final total of 53 patients were thus included in the analyses: 25 patients in the MZR group and 28 patients in the control group (Fig. 1). The baseline characteristics of the patients are summarized in (Table 1).
All 53 patients whose cases were analyzed were diagnosed with MPA. Nineteen of the 25 patients in the MZR group and 20 of the 28 patients in the control group were diagnosed with renal limited AAV. The average time from onset to the start of the observation period was 32.6 ± 45.4 months in the MZR group and 27.0 ± 25.1 months in the control group. As induction therapy, seven patients in the MZR group received CYC in combination (five of the seven patients received an oral administration of CYC and the other two patients received intravenous CYC pulse therapy), the other 18 patients in the MZR group received corticosteroids alone, three patients in the control group received intravenous CYC pulse therapy, and the other 25 patients in the control group received corticosteroids alone. At the start of the observation, 15 patients in the MZR group had achieved a CR, the remaining 10 patients in the MZR group had achieved an ICR, 18 patients in the control group had achieved a CR, and the remaining 10 patients in the control group had achieved an ICR. During the 12-month observation period, the mean dose of corticosteroids decreased from 12.1 mg to 7.5 mg in the MZR group and from 13.9 mg to 8.6 mg in the control group. There was no significant difference between the two groups in background, clinical symptoms, previous treatment, laboratory findings, or MPO-ANCA values.
Efficacy assessments
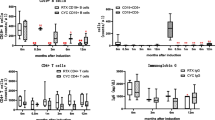
Ten patients (six of the 25 patients in the MZR group and four of 28 patients in the control group) relapsed during the 12 month observation period. Figure 2 depicts the two groups’ proportion of patients who survived without relapse during the observation period. There was no significant between-group difference in the relapse rate depending on the presence or absence of MZR treatment (p = 0.422). Table 2 provides the two groups’ mean values of CLcr, CRP, BVAS, and MPO-ANCA at baseline and at the final observation, divided into the relapsed patients and the nonrelapsed patients. There was no significant difference in any item at baseline between the relapsed and nonrelapsed groups.
The changes in serum MZR concentration
The daily dose of MZR in each patient adjusted for serum levels was 100–300 mg. Figure 3 illustrates the changes in serum MZR concentrations estimated by Bayesian inference based on the PPK parameters using the NONMEM program. The changes in serum MZR concentration could be estimated in 22 of the 26 patients in the MZR group. The serum concentration in four patients in the MZR group could not be used due to the lack of proper serum submission and deficient values. The MZR treatment of one patient with a C0 value > 1 μg/mL was discontinued because of adverse events (i.e., fever and eczema) and excluded from the further analyses. Two of the 10 patients (20%) who reached a Cmax of 3 μg/mL relapsed, whereas four of the 11 patients (36%) who did not reach this Cmax relapsed. This difference was not significant (p = 0.635). The suppression of the recurrence of MPO-AAV by an increased serum concentration of MZR was not examined in this study.
Adverse events
In one patient, anorexia, wheezing, fever and eczema appeared 2 weeks after the start of MZR treatment, and all symptoms disappeared approx. 1 week after the discontinuation of MZR. This case was excluded from the analyses. A total of 20 adverse events were reported in 13 patients (Table 3): 13 events among eight (32%) MZR patients and seven events among five (18%) control patients. There was no significant difference in the number of patients with adverse events between the two groups (p = 0.339). Another patient’s back pain was considered to be caused by a pulmonary nodular lesion due to a relapse of AAV. In that patient’s case, MZR was judged to be ineffective and was discontinued.
Five patients with herpes zoster and one patient with pulmonary tuberculosis were treated with a therapeutic agent for infection while continuing corticosteroids and MZR. All six patients recovered. Details of the other adverse events are as follows (Table 3): two patients in the MZR group presented with hyperglycemia, and one patient each in the MZR group had conjunctivitis, and anemia. One patient in the control group had fever, and another control patient’s alanine aminotransferase and aspartate aminotransferase values increased.
Discussion
We had speculated that (1) MZR can be used to suppress recurrence in MPO-AAV patients during their maintenance therapy after induction therapy, and (2) MZR would not cause severe adverse events. We thus conducted the present study to evaluate MZR treatment's recurrence-suppressing effect and its adverse events. Our additional hypothesis was that the administration of MZR can be effective and safe based on the monitoring of the serum concentration of MZR and the setting of both the appropriate trough concentration and the estimated serum peak concentration to a certain value or higher. Although our analyses revealed no significant difference in the recurrence rate of MPO-AAV between the use and nonuse of MZR, our findings demonstrated that it was possible to avoid serious bone marrow suppression by measuring the patients' serum MZR concentrations. It was not possible to establish MZR's ability to suppress recurrence by adjusting the MZR dose so that the peak of the estimated serum concentration of MZR was ≥ 3 μg/mL in this study.
An earlier investigation of the efficacy of MZR in patients with idiopathic membranous nephropathy with steroid-resistant nephrotic syndrome noted that a Cmax > 1.1 μg/mL is necessary for complete remission [13]. It was also reported that MZR showed a 50% inhibition of the human mixed-lymphocyte reaction (MLR) at a concentration of approx. 1 μg/mL [15]. Another study revealed that a peak serum MZR level (2 h post-dose) at ≥ 2.5–3.0 μg/mL was necessary to effectively treat pediatric patients with lupus nephritis [16]. From the above reports, we speculated that the Cmax of MZR should be 1–3 μg/mL in order to suppress the recurrence of MPO-AAV, and in this study we attempted to adjust the patients’ Cmax to ≥ 3 μg/mL. However, less than half of the patients reached the target Cmax of ≥ 3 μg/mL, and this number of patients was insufficient for the evaluation.
Only two of the 26 patients treated with MZR experienced a serious adverse event during the 12 month observation period. A similar frequency of infectious diseases occurred in the MZR and control groups, and in all cases, the infection could be controlled without discontinuing MZR. It has been reported that the use of rituximab or AZA recommended by the guidelines causes adverse events, such as severe infections [17] or skin carcinoma [18]; relapse was observed in approx. 50% of the patients with GPA or MPA with renal involvement [18]. MPO-AAV has a high recurrence rate and requires a long-term use of immunosuppressive drugs for maintenance therapy. Immunosuppressive drugs should not cause serious adverse events. Our present findings indicate that MZR is useful in that it is less likely to cause serious adverse events.
Our patients’ mean age (67.5 years) and male-to-female ratio (37.7%/63.3%) were similar to those of the previously reported MPO-AAV patients in Japan at 64.4 years and 42.6% [5]. Our patient series thus appears to reflect the population of MPO-AAV patients in Japan. However, because this study was aimed at patients who have achieved a CR or ICR after induction therapy, our findings may not be applicable to severe cases in which induction therapy has not been successful.
In conclusion, there was no significant difference in the recurrence rate of MPO-AAV between the use and nonuse of MZR. MZR may not be the first choice for immunosuppressive therapy in MPO-AAV maintenance therapy. However, if the appropriate doses and frequencies of administration can be identified, MZR may be an option when other immunosuppressive drugs cannot be used due to high risks of infectious diseases or allergies.
References
Jennette JC, Falk RJ, Bacon PA, et al. 2012 revised international chapel hill consensus conference nomenclature of vasculitides. Arthritis Rheum. 2013;65:1–11.
Chung SA, Langford CA, Maz M, et al. 2021 American college of rheumatology/vasculitis foundation guideline for the management of antineutrophil cytoplasmic antibody-associated vasculitis. Arthritis Rheum. 2021;73:1366–83.
Yates M, Watts RA, Bajeme IM, et al. EULAR/ERA-EDTA recommendations for the management of ANCA-associated vasculitis. Ann Rheum Dis. 2016;75:1583–94.
Koyama A, Yamagata K, Makino H, et al. Japan RPGN registry group. A nationwide survey of rapidly progressive glomerulonephritis in Japan: etiology, prognosis and treatment diversity. Clin Exp Nephrol. 2009;13:633–50.
Yamagata K, Usui J, Saito C, et al. ANCA-associated systemic vasculitis in Japan: clinical features and prognostic changes. Clin Exp Nephrol. 2012;16:580–8.
Yamagata K, Usui J, Sugiyama H, Maruyama S, Narita I. Temporal change in life and renal progressive glomerulonephritis in Japan via nationwide questionnaire survey. Clin Exp Nephrol. 2019;23:573–5.
Yamagata K, Usui J, Sugiyama H, Maruyama S, Narita I. Correction to: temporal change in life and renal progressive glomerulonephritis in Japan via nationwide questionnaire survey. Clin Exp Nephrol. 2020;24:976–7.
Mizuno K, Tsujino M, Takada M, Hayashi M, Atsumi K, Asano K, Matsuda T. Studies on bredinin. I. Isolation, characterization and biological properties. J Antibiot. 1974;27:775–82.
Yokota S. Mizoribine: mode of action and effects in clinical use. Pediatr Int. 2002;44:196–8.
Hirayama K, Kobayashi M, Hashimoto Y, et al. Treatment with the purine synthesis inhibitor mizoribine for ANCA-associated renal vasculitis. Am J Kidney Dis. 2004;44:57–63.
Honda M, Itoh H, Suzuki T, Hashimoto Y. Population pharmacokinetics of high-dose mizoribine in healthy male volunteers. Biol Pharm Bull. 2006;29:2460–4.
Ishida K, Okamoto M, Ishibashi M, Hashimoto Y. Population pharmacokinetics of mizoribine in adult recipients of renal transplantation. Clin Exp Nephrol. 2011;15:900–6.
Saito T, Iwano M, Matsumoto K, et al. The refractory nephrotic syndrome study group. Mizoribine therapy combined with steroids and mizoribine blood concentration monitoring for idiopathic membranous nephropathy with steroid-resistant nephrotic syndrome. Clin Exp Nephrol. 2017;21:961–70.
Flossmann O, Bacon P, de Groot K, et al. Development of comprehensive disease assessment in systemic vasculitis. Ann Rheum Dis. 2007;66:283–92.
Sonda K, Takahashi K, Tanabe K, et al. Clinical pharmacokinetic study of mizoribine in renal transplantation patients. Transplant Proc. 1996;28:3643–8.
Tanaka H, Tsugawa K, Nakahata T, Kudo M, Suzuki K, Ito E. Implication of the peak serum level of mizoribine for control of the serum anti-dsDNA antibody titer in patients with lupus nephritis. Clin Nephrol. 2005;63:417–22.
Smith RM, Jones RB, Specks U, et al. RITAZAREM coinvestigators. Rituximab as therapy to induce remission after relapse in ANCA-associated vasculitis. Ann Rheum Dis. 2020;79:1243–9.
Westman KWA, Bygren PG, Olsson H, Ranstam J, Wieslander J. Relapse rate, renal survival, and cancer morbidity in patients with Wegener’s granulomatosis or microscopic polyangiitis with renal involvement. J Am Soc Nephrol. 1998;9:842–52.
Acknowledgements
This study was supported in part by a Grant-in-Aid for Intractable Renal Diseases Research, Research on Rare and Intractable Diseases, and by Health and Labour Sciences Research Grants from the Ministry of Health, Labour and Welfare of Japan. We would like to express our sincere gratitude to Dr. Satoshi Horikoshi of Juntendo University and Dr. Yoshio Taguma of Sendai Shakaihoken Hospital for their valuable guidance in compiling this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Honoraria: TW (Kyowa Kirin Co. Ltd., Mitsubishi Tanabe Pharma Corp.), NH (Takeda Pharmaceutical Co., Ltd.), KY (Chugai, Daiichi-Sankyo, Kyowakirin, Mochida, Tanabe-Mitsubishi, Pfizer, Asteras). Research funding: TW (Shiseido Co., Ltd., Kyowa Kirin Co., Ltd.), YY (Baxter Ltd., Bayer Yakuhin, Ltd., Chugai Pharmaceutical Co., Ltd., Japan Tobacco Inc., Kyowa Kirin Co., Ltd., Ono Pharmaceutical Co., Ltd., Otsuka Pharmaceutical Co., Ltd., Sanofi Co., Ltd., Sumitomo Dainippon Pharma Co., Ltd., Torii Pharmaceutical Co., Ltd.), KY (Kyowakirin, Pfizer, Teijin-pharma, Daiichi-Sankyo, Dainihon-Sumitomo, Takeda, Tanabe-Mitsubishi, Asteras, Chugai). Subsidies or Donations: TW (Chugai Pharmaceutical Co., Ltd., Kyowa Kirin Co., Ltd., Mitsubishi Tanabe Pharma Corp., MSD K.K., GlaxoSmithKline K.K.).
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee at which the studies were conducted (IRB approval no.: University of Tsukuba Hospital, H18-117) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Mase, K., Saito, C., Usui, J. et al. The efficacy and safety of mizoribine for maintenance therapy in patients with myeloperoxidase anti-neutrophil cytoplasmic antibody (MPO-ANCA)-associated vasculitis: the usefulness of serum mizoribine monitoring. Clin Exp Nephrol 26, 1092–1099 (2022). https://doi.org/10.1007/s10157-022-02253-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-022-02253-6